Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient
|
|
|
- Myrtle Willis
- 5 years ago
- Views:
Transcription
1 PEDIATRICS/ORIGINAL RESEARCH Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient Myto Duong, MD, MS Stephen Markwell, MA John Peter, MD Stephen Barenkamp, MD From the Cardinal Glennon Children s Medical Center, Saint Louis University School of Medicine, Pediatric Emergency Medicine Department (Duong, Peter) and Pediatric Infectious Diseases Division, Department of Pediatrics (Barenkamp), Division of Pediatrics, St. Louis, MO; and the Southern Illinois University, School of Medicine, Division of Statistics and Research Consulting, Springfield, IL (Markwell). Dr. Duong is currently affiliated with Southern Illinois University, School of Medicine at St. John s Hospital, Springfield, IL. Study objective: Emergency department visits for skin and soft tissue infections are increasing with the discovery of community-acquired methicillin-resistant Staphylococcus aureus. Whether abscesses treated surgically also require antibiotics is controversial. There are no published pediatric randomized controlled trials evaluating the need for antibiotics in skin abscess management. We determine the benefits of antibiotics in surgically managed pediatric skin abscesses. Methods: This was a double-blind, randomized, controlled trial. Pediatric patients were randomized to receive 10 days of placebo or trimethoprim-sulfamethoxazole after incision and draining. Follow-up consisted of a visit/call at 10 to 14 days and a call at 90 days. Primary outcome was treatment failure at the 10-day follow-up. Secondary outcome was new lesion development at the 10- and 90-day follow-ups. Noninferiority of placebo relative to trimethoprim-sulfamethoxazole for primary and secondary outcomes was assessed. Results: One hundred sixty-one patients were enrolled, with 12 lost to follow-up. The failure rates were 5.3% (n 4/76) and 4.1% (n 3/73) in the placebo and antibiotic groups, respectively, yielding a difference of 1.2%, with a 1-sided 95% confidence interval (CI) ( to 6.8%). Noninferiority was established with an equivalence threshold of 7%. New lesions occurred at the 10-day follow-up: 19 on placebo (26.4%) and 9 on antibiotics (12.9%), yielding a difference of 13.5%, with 95% 1-sided CI ( to 24.3%). At the 3-month follow-up, 15 of 52 (28.8%) in the placebo group and 13 of 46 (28.3%) in the antibiotic group developed new lesions. The difference was 0.5%, with 95% 1-sided CI ( to 15.6%). Conclusion: Antibiotics are not required for pediatric skin abscess resolution. Antibiotics may help prevent new lesions in the short term, but further studies are required. [Ann Emerg Med. 2010;55: ] Please see page 402 for the Editor s Capsule Summary of this article. Provide feedback on this article at the journal s Web site, /$-see front matter Copyright 2009 by the American College of Emergency Physicians. doi: /j.annemergmed SEE EDITORIALS, P. 408 AND 412. INTRODUCTION The incidence of skin and soft tissue infections has increased markedly during the last decade. From 1993 to 2005, there was nearly a 3-fold increase in skin infections diagnosed by emergency physicians in the United States, from 1.2 to 3.4 million cases. 1 There are numerous reports indicating that this overall increase is primarily due to a dramatic increase in the number of infections caused by community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA), an organism that often presents with skin and soft tissue infections in the pediatric population. 2,3 In the past, surgical drainage of skin abscesses has been the accepted standard of care. With the emergence of CA-MRSA causing serious and even fatal infections in immunocompetent pediatric patients, many have recommended the addition of antibiotic therapy. 3-5 Several published studies have suggested that skin abscesses can be cured with adequate drainage alone, according to the finding that many patients improve despite receiving antibiotics to which their infecting organisms are not susceptible. 6-8 Rajendran et al 9 reported no benefit with the addition of cephalexin to the management of surgically drained CA-MRSA skin abscesses in adult patients, but a retrospective study by Ruhe et al 5 reported an association between delayed initiation of active antibiotic and treatment failure of CA-MRSA skin abscesses in adults. Volume 55, NO. 5 : May 2010 Annals of Emergency Medicine 401
2 Antibiotics for Skin Abscesses Editor s Capsule Summary What is already known on this topic With the increasing prevalence of methicillinresistant Staphylococcus aureus, there is concern that incision and draining may be insufficient treatment for skin abscesses. What question this study addressed This 149-child, double-blind, placebo-controlled trial compared incision and draining with incision and draining followed by a 10-day course of oral sulfamethoxazole/trimethoprim. What this study adds to our knowledge Placebo and sulfamethoxazole/trimethoprim groups fared equally well, though both had high rates of new lesions at 10 days and 3 months postincision and drainage. How this might change clinical practice Antibiotics should not be considered the standard of care in the treatment of skin abscesses in children. To our knowledge, there are no published randomized controlled studies evaluating the benefits of antibiotic treatment of adequately drained skin abscesses in the era of CA-MRSA, either in adults or in the pediatric population. The purpose of this study is to demonstrate noninferiority of placebo relative to antibiotic use in pediatric patients who undergo incision and drainage of acute skin abscesses. MATERIALS AND METHODS Setting This study was conducted in the emergency department (ED) at the Cardinal Glennon Children s Medical Center, Saint Louis University in St. Louis, MO, from July 2006 to February It is a Level I pediatric trauma center, with annual visits of 41,000 patients. Selection of Participants The study population consisted of pediatric patients aged 3 months to 18 years, who had skin abscesses and were nontoxic, with temperature less than 38.4 C (101.1 F). Skin abscesses were diagnosed clinically and by bedside ultrasonography, performed by emergency physicians, when available. Diagnostic criteria for skin abscess included the presence of all of the following features: (1) acute onset within 1 week, (2) fluctuance, (3) erythema, (4) induration, and (5) tenderness, with or without purulent drainage. Subjects who had skin abscesses and met the inclusion criteria were recruited by qualified pediatric emergency medicine attending physicians or fellows. Subjects or their parent or guardian had to be able to read and comprehend Duong et al English sufficiently to provide informed written consent (and assent when applicable). Children were excluded from the study if they had known chronic health problems, such as diabetes; were receiving immunosuppressive medications, such as oral steroids for asthma; had recent (within the last week) or current antibiotic usage; or had any contraindication to trimethoprimsulfamethoxazole, such as a history of hypersensitivity to sulfonamides or trimethoprim. Minor or superficial skin infections such as folliculitis were excluded because these infections tend to resolve spontaneously or with warm compresses or topical antibiotics, and surgical drainage is not required. Study Design, Interventions, and Data Collection and Processing This study was a double-blinded, prospective, randomized, controlled trial approved by the Institutional Review Board of Saint Louis University. Once written consent (or assent when applicable) was obtained, patient information (age, sex, race, history of skin abscesses, and family history of skin abscesses) and the largest diameter (in centimeters) of erythema and induration of the abscess were recorded. When ultrasonography was available, measurements were made in 2 dimensions, diameter and depth. Local anesthetic or procedural sedation was used at the discretion of the attending physician. The skin overlying all skin abscesses was cleansed with 10% povidoneiodine solution and then incised with a no. 11 blade, probed for loculations, and irrigated with normal saline solution. Abscess cultures obtained on Dacron swabs (Starplex Scientific Inc., Etobicoke, Ontario, Canada) were obtained immediately after surgical incision and sent for culture and antibiotic sensitivity testing. Antibiotic susceptibilities to S aureus isolates were performed at the microbiology laboratory at our institution. Isolates were tested with the Microscan systems by methods established by the Clinical and Laboratory Standards Institute for antibiotics, including amikacin, cefazolin, cefotaxime, ceftriaxone, chloramphenicol, gentamicin, penicillin, clindamycin, erythromycin, oxacillin, trimethoprimsulfamethoxazole, and vancomycin. Pathogens that were erythromycin resistant but clindamycin sensitive had a disk diffusion test (D-test) performed to evaluate the organism for inducible clindamycin resistance. 10 Decisions concerning the need for procedural sedation, the incision size, and 24-hour wound packing were physician dependent. With a computer randomization program, subjects were then randomized in permuted blocks of 50 to receive a 10-day course of placebo or trimethoprim-sulfamethoxazole. The placebo consisted of a Maalox and tonic water combination that resembled the antibiotic in color, texture, and taste. The antibiotic dose was a standard trimethoprim-sulfamethoxazole dose for mild bacterial infections (10-12 mg trimethoprim/kg/ day divided into 2 doses, with a maximum dose of 160 mg trimethoprim/dose). Only the liquid formulation of the antibiotic was used because teenagers could be persuaded to take 402 Annals of Emergency Medicine Volume 55, NO. 5 : May 2010
3 Duong et al liquids more readily than smaller children could be to take large tablets. The concentration of the antibiotic solution was 200 mg sulfamethoxazole/40 mg trimethoprim per 5 ml. The medications were prepared, stored, and dispensed by the inpatient pharmacist who also generated the randomization sequence and assigned the participants to their groups. The patient, parents, and clinician who assessed the clinical outcome were blinded to group assignment. Patients and their parents were asked to monitor study subjects for any adverse effects of the medication and to call if they had any questions or concerns. At home, they were instructed to remove and discard the gauze packing, if used, 24 hours after it was placed in the ED and to perform warm water soaks at least twice a day per standard of care. They were instructed to keep the wound clean and covered by a layer of gauze with taping around the edges and to avoid using topical antibiotic ointment/cream, hydrogen peroxide, alcohol, or Betadine to decrease the chance of confounding factors. Updated telephone numbers were verified before the patient s discharge on the initial and day 10 visits to increase the likelihood of a telephone follow-up at 2 to 3 days, 10 to 14 days, and 90 days later. With the 2- to 3-day follow-up call, patients were reminded to remove packing if present, to do warm soaks, and to take their medications. Any patient concerns were addressed at that time, and a 10- to 14-day follow-up appointment was set up. Compliance was evaluated by quantifying study medication that remained on the follow-up clinic visit or by parental report over the telephone. The participants were asked to bring their medicine and its container back at the 10-day follow-up visit. The remaining volume was recorded and categorized as 0%, 1% to 24%, 25% to 49%, 50% to 74%, and greater than 75% of medication remaining. Compliance was defined as greater than 50% of the medication taken by the patient. Patients and parents were also asked the number of days it took for them to notice healing of the wound at the 10-day follow-up visit or call. The 90-day telephone interview of the parent or guardian consisted of 2 questions: (1) whether there was there any recurrence of skin abscesses or spread to other body parts and (2) whether anyone else in the family developed skin abscesses. Methods of Measurements and Outcome Measures The primary outcome measure was clinical resolution or failure. Clinical resolution was defined as absence of erythema, warmth, induration, fluctuance, tenderness, and drainage at the 10-day follow-up. The secondary outcomes of interest included the development of new lesions at a different site ( 5 cm away from original skin abscess) on day 10 clinical follow-up or selfreport and 3-month telephone follow-up. Management of these new lesions was recorded. The spread to other family members (household contacts) by report at the 10-day and 3-month follow-up, as well as the presence of any adverse effects from the medications at the 10-day follow-up, was noted. Treatment failure was defined as the presence of any of the above signs or symptoms at the 10-day follow-up or worsening Antibiotics for Skin Abscesses signs or symptoms before the 10-day follow-up requiring further surgical drainage, change in medication, or hospital admission for intravenous antibiotics. New lesions within 5 cm of the original abscess site were also considered treatment failures. New lesions may consist of folliculitis, furuncles, carbuncles, or abscesses. Physicians involved in the enrollment and assessment of clinical outcome received training or education about the study design and protocol by the primary investigator. The study was approved by our institutional review board. A data and safety committee was formed to meet quarterly to monitor patient safety. More specifically, they reviewed the adverse effects of the medications, frequency of treatment failures, frequency of new lesion development, and subsequent managements and outcomes of these patients. Primary Data Analysis This was a noninferiority study. The sample size of 81 per group was calculated according to assumed treatment failure rate of 3.3% with antibiotics, an equivalence threshold of 7% (allowing up to 10.3% failure rate with placebo), to achieve a power of 0.80 ( 0.05), using nquery 7.0 Module PTE0. To assess noninferiority, a 95% 1-sided confidence interval (CI) was computed on the difference of the proportions between the 2 groups. If the upper limit of the CI was less than the equivalence threshold of 7%, then noninferiority could be inferred. Our definition for CA-MRSA is a methicillin-resistant S aureus isolate obtained from skin abscesses of patients from the community that is relatively susceptible to other antibiotics, including vancomycin, trimethoprim-sulfamethoxazole, tetracyclines, and clindamycin. Our definition is not based on molecular characterization of the isolates. RESULTS Characteristics of Study Subjects A total of 1,305 patients who presented to our ED were identified with the International Classification of Disease coding for cellulitis and skin abscesses during the study period. This was not a convenience sampling. Among this group of potential study subjects were 161 individuals who agreed to participate in the trial after the protocol was reviewed with them. These subjects were then randomly assigned treatment with either placebo or trimethoprim-sulfamethoxazole. Twelve subjects were lost to follow-up (8 from the placebo group and 4 from the trimethoprim-sulfamethoxazole group), resulting in a final cohort of 149 evaluable participants (Figure). The other potential study subjects were not enrolled because they did not meet inclusion criteria, refused to consent, or were not enrolled by the examining physician. No formal record was kept of the reasons for not enrolling the potential subjects who did not participate. Subjects in the 2 study groups were similar in baseline characteristics (Table 1). The patients in our study were primarily female (58%) black children (86%) younger than 5 Volume 55, NO. 5 : May 2010 Annals of Emergency Medicine 403
4 Antibiotics for Skin Abscesses Duong et al Figure. Study enrollment distribution. SSTI, Skin and soft tissue infections; TMP-SMX, trimethoprim-sulfamethoxazole. Table 1. Patient and abscess characteristics. Characteristics Placebo (%) (%) Total (%) Female 42/76 (55) 45/73 (61) 87/149 (58) Black 65/76 (86) 63/73 (86) 128/149 (86) 5 y 40/76 (53) 39/73 (53) 79/149 (53) History of skin 36/76 (47) 25/73 (34) 61/149 (41) abscess Family history of skin 33/76 (43) 37/73 (51) 70/149 (47) abscess Erythema diameter 26/52 (50) 26/52 (50) 52/149 (35) 4 cm Abscess induration 20/38 (53) 18/38 (47) 38/149 (26) 4 cm Ultrasonographic 53/58 (91) 43/45 (96) 96/149 (64) diameter result 5 cm Ultrasonographic depth 41/58 (71) 33/45 (73) 74/149 (50) result 2.5 cm Wound packing 50/71 (70) 58/71 (82) 108/149 (72) Procedural sedation 51/76 (67) 52/73 (71) 103/149 (69) years (53%), with a median age of 4 years and an interquartile range of 1 to 12 years. Forty-one percent of the patients had a history of skin abscesses and 47% had a family history of skin abscesses. The skin lesions were most often located in the diaper region: gluteus (43%), perineum/labia (5.4%), and inguinal (7.4%). Other locations for the skin abscesses included the upper leg (8.1%), lower leg (8.7%), axilla (13.4%), forearm (2.7%), abdomen (8.1%), and head (3.3%). The mean diameter of erythema and induration was cm and cm, respectively. There were 52 abscesses with erythema greater than or equal to 5 cm, 26 in the placebo group and 26 in the antibiotic group. For lesions measured by ultrasonography, the mean diameters were cm, and mean depth was Table 2. Medication adverse effects. Adverse Effects Placebo (%) (%) No adverse effects 67 (88.2) 59 (80.8) Rash 0 3 (4.1) Diarrhea 4 (5.3) 3 (4.1) Vomiting 1 (1.3) 1 (1.4) Vomiting and diarrhea 1 (1.3) 1 (1.4) Bad taste 1 (1.3) 5 (6.8) No documentation 2 (2.6) 1 (1.4) Total 76 (51) 73 (49) cm. Procedural sedation was performed in 69% of the patients and wound packing in 72%. There was no statistically significant difference between the 2 groups in terms of patient or abscess characteristics. Fifty-two percent of the patients received placebo (83) and 48% received trimethoprim-sulfamethoxazole (78). The overall compliance rate was 66%, 55% among subjects assigned to the placebo group and 46% among subjects assigned to the treatment group. Approximately 90% of the patients did not have any adverse effects. There were no reports of serious or potentially life-threatening adverse effects from the medications (Table 2). The bacterial pathogens isolated from the skin abscesses were primarily CA-MRSA (80%), with 18% clindamycin resistance but 100% trimethoprim-sulfamethoxazole and vancomycin sensitivity (Table 3). One hundred sixty-one subjects were enrolled, with 12 lost to follow-up. The patients who were lost to follow-up did not differ from the rest of study participants in terms of demographics or clinical presentation. For the patients who were lost to follow-up, 92% were black, with a mean age of 7 years. These patients had mean ultrasonogaphic diameter, 404 Annals of Emergency Medicine Volume 55, NO. 5 : May 2010
5 Duong et al Table 3. Skin abscess culture results. Culture Results Placebo (%) (%) Total (%) CA-MRSA 61 (81) 58 (79) 129 (80) MSSA 6 (8) 7 (10) 14 (9) Proteus mirabilis 4 (5) 2 (3) 6 (4) GAS 1 (1) 1 (1) 2 (1) Other 1 (1) 3 (4) 4 (3) No culture/growth 3 (4) 2 (3) 6 (3) MSSA, Methicillin sensitive S aureus; GAS, group A streptococcus. depth, erythema, and induration of cm, cm, cm, and cm, respectively. Twenty-five percent (3/12) of these patients lost to follow-up had a history of skin abscesses, and 50% of them had a family history of skin abscesses. Eight of these patients had been randomized to receive placebo, and 4 were randomized to receive trimethoprim-sulfamethoxazole. Of the 149 participants, the 10-day clinical follow-up occurred in 60% of the patients (90/149), with 40% requiring telephone follow-up. Sixty percent of the placebo group (46/76) and 60% (44/73) in the antibiotic group received clinical follow-ups. The 3-month telephone follow-up was 65% (98/ 149). The frequency of adverse effects was similar for the 2 treatment groups (Table 2). For clinical resolution, noninferiority was demonstrated for placebo relative to antibiotic. The failure rate was 5.3% (4 of 76) in the placebo group versus 4.1% (3 of 73) in the antibiotic group, yielding a difference of 1.2%, with a 1-sided 95% CI of to 6.8%. The upper limit (6.8%) of this CI for the difference in failure rate did not exceed the previously specified equivalence threshold of 7%. The treatment failures in the antibiotic groups had antibiotic change before the 10-day follow-up, which was not by design, and all investigators were blinded until the study end date. Of the 7 treatment failures, all had persistent purulent drainage, 2 had surgical reexploration for loculations and drainage, and none were hospitalized. They were all discharged home, receiving oral trimethoprim-sulfamethoxazole or clindamycin. Of the treatment failure patients, the pathogens were CA- MRSA (4) and Proteus mirabilis (3), which were all sensitive to trimethoprim-sulfamethoxazole. To address concerns that patients who are aged 14 years and older may respond better than patients younger than 14 years and thus bias our results, subanalysis of patients younger than 14 years was performed. Treatment failure was 2 of 58 (3.4%) in the placebo group and 1 of 62 (1.6%) in the antibiotic group, yielding a difference of 1.84%, with 95% CI ( to 6.5%). With the 7% margin, noninferiority was established for this subgroup analysis of patients younger than 14 years. Table 4. Management of new lesions at the 10-day follow-up. New Lesion Management Placebo Antibiotics for Skin Abscesses Medication Total Spontaneous drainage Incision and draining without antibiotic Incision and draining with antibiotic Bleach bath Intravenous antibiotic Expressed it Self-resolved Warm compresses Oral antibiotic Not applicable Total There was no statistically significant difference between placebo and antibiotic groups in new lesion development at the 3-month follow-up, but there was one at the 10-day follow-up. New lesions occurred in 28 patients (19%) at the 10-day follow-up: 19 in the placebo group (26.4%) and 9 in the antibiotics group (12.9%), yielding a difference of 13.5, with 95% 1-sided CI ( to 24.3%). Of the 28 patients with new lesion development at the 10- day follow-up, 8 required incision and draining (5 in the placebo and 3 in the antibiotic group), 1 in the placebo group was hospitalized for intravenous antibiotics, 4 began receiving oral antibiotics, 5 had spontaneous drainage, and 10 spontaneously resolved (Table 4). At 3 months, only 98 patients could be followed up (52 in the placebo and 46 in the antibiotic group): 28.8% of the patients in the placebo group and 28.3% in the antibiotics group developed new lesions, yielding a difference of 0.5%, with 95% 1-sided CI ( to 15.6%). LIMITATIONS Limitations to this study include possible selection bias, with a large proportion of potential patients not being enrolled from July 24, 2006, to February 2, 2008, by the examining physician. Another source of selection bias may come from the 12 participants (7%) who were lost to follow-up, but this is a relatively small number, and analysis of available data for them indicates similarity with the studied subjects. Forty percent of our follow-ups occurred by telephone calls, which is another source of bias with inaccurate data gathering and unreliable selfreporting. Because of the patient population who most often present to our ED (ie, lower social economic group with less stable living conditions), it was not surprising to find a larger loss in followup at 3 months (40%), which could have affected our interpretation of long-term skin abscess recurrence rate. Volume 55, NO. 5 : May 2010 Annals of Emergency Medicine 405
6 Antibiotics for Skin Abscesses No molecular studies were performed to verify that the methicillin-resistant S aureus were truly community acquired, as distinct from hospital-acquired methicillin-resistant S aureus. Our definition of CA-MRSA is based on clinical presentation of previously healthy pediatric patients to an outpatient setting (the ED) and the pathogen s antibiotic susceptibility pattern, but this is in compliance with the Centers for Disease Control and Prevention s (CDC s) definition of CA-MRSA. The CDC defines CA-MRSA as MRSA infections that are acquired by persons who have not been recently (within the past year) hospitalized or had a medical procedure (such as dialysis, surgery, catheters). 11 The compliance rate of 66% is poor but comparable to that of other clinical studies. Llera and Levy 8 reported a compliance rate of 68% in adults for a 7-day antibiotic course, but their definition of compliance was greater than 78% medication completion. The compliance rate in our study would be much lower if compliance were defined as greater than 75% medication completion as opposed to greater than 50%. The compliance rate might be higher if the duration of antibiotic therapy were reduced from 10 to 7 days. As mentioned above, further limitations include the unreliability of self-reporting of medication compliance in the patients who were followed up by telephone calls. The sample size was calculated according to a clinical tolerance of treatment failure rate of 7%, which some may find unacceptable. However, the treatment failures were not severe and required minimal change in management (such as receiving a susceptible oral antibiotic). It is impractical to conduct a study with a set clinical tolerance of treatment failure of 1%, which would require more than 4,500 patients. This study was conducted on previously healthy pediatric patients and may not be generalized to adults or pediatric patients who have comorbidities and present with skin abscesses. DISCUSSION Across the nation, there has been a dramatic increase in the diagnosis of skin and soft tissue infections. 1 There is no doubt that CA-MRSA has emerged as a common pathogen causing skin abscesses in adult and pediatric patients throughout the United States. Young 7 reported that 63% of skin abscess cultures in adults were CA-MRSA (median age 42 years; range 1 to 89 years). Moran et al 2 reported 76% CA-MRSA skin and soft tissue infections in adults, which is comparable to that in the pediatric population presented here, with CA-MRSA isolates of 80% from the skin abscesses. Geographic variation of antibiotic resistance is well established. California and Baltimore have reported 6% clindamycin resistance 12,13 and Detroit has reported 46% clindamycin resistance 14 among their CA-MRSA isolates. The proportion of CA-MRSA isolates that was clindamycin resistant in this study was 18%, which concurred with a retrospective Duong et al review at our institution in 2005, demonstrating a clindamycin resistance of 17% (unpublished data). The standard of care for the management of skin abscesses is incision and draining. Recommendations for the addition of antibiotics, which would be effective against CA-MRSA, in the management of skin abscesses stemmed from an increase in CA-MRSA skin and soft tissue infections and associated complications. In concordance with the articles written by Llera and Levy 8 and Rajendran et al, 9 our study demonstrated that antibiotics are not needed for skin abscess resolution after incision and draining. However, the treatment group in these other randomized control trials in the adult population used antibiotics (cephradine and cephalexin) that would not be active against CA-MRSA. Our results demonstrated no statistically significant difference in treatment failure rates of the primary lesions with or without antibiotics effective against CA-MRSA. No difference in treatment failure rates was found between the placebo and antibiotic groups in a subanalysis of data from skin abscesses caused by CA-MRSA. The current study suggests that systemic antibiotics are not required in the treatment of skin abscesses after incision and draining, even in the era of CA- MRSA. There were no correlations between treatment failure and other factors such as medical history or family history, use of wound packing, or use of procedural sedation for the incision and draining. In fact, the placebo group had more history of skin abscesses compared with the antibiotic group, which further supports our conclusion that antibiotic is not needed for skin abscess resolution. Lee et al 6 reported a treatment failure rate of 8%, with an increased risk of treatment failure in skin abscesses that were greater than 5 cm. On ultrasonography, our mean skin abscess diameter was only cm, which suggests that our skin abscesses may have been smaller than the ones reported by Lee et al, 6 with a selection bias for healing without antibiotics. Our treatment failure rate was slightly less, at 5%, but treatment failure did not correlate with clinical assessment of abscess size, erythema, or induration greater than or equal to 5 cm (Table 1). The presence of cellulitis with these skin abscesses did not correlate with treatment failure. There is a paucity of data on the usefulness of antibiotics in skin abscess management in terms of healing time or prevention of recurrence. In our patients, antibiotics decreased new lesion developments at the 10-day follow-up. There was no significant difference between the 2 groups in new lesion development at the 3-month follow-up. In the short term, antibiotics may be useful in preventing recurrent skin abscesses but provided no long-term benefits in terms of new lesion development. Further studies are required to further elucidate this issue. Despite the potential advantage of antibiotic use in the management of skin abscesses, with the continuing evolution of bacterial pathogens, poor patient compliance with medications, and increasing antibiotic resistance, it is prudent to minimize 406 Annals of Emergency Medicine Volume 55, NO. 5 : May 2010
7 Duong et al the use of antibiotics in this setting, given such low treatment failure rates. After incision and draining of skin abscesses in children, 95% of the skin abscesses demonstrated clinical resolution; therefore, antibiotics are not required. The potential benefit of preventing distal lesion development with the use of antibiotics will require further study and evaluation. By avoiding unnecessary antibiotic use, potential adverse effects, allergic reactions, and natural selection of more resistant organisms may be avoided. Furthermore, the cost saving of unnecessary antibiotic use is significant, considering the dramatic increase in skin abscess diagnoses. Supervising editor: Michael W. Shannon, MD; Steven M. Green, MD Author contributions: MD was the primary investigator and corresponding author. JP and SB designed the study. JP was involved in patient recruitment. SM conducted statistical analysis and provided graphical assistance. SB provided pediatric infectious disease expertise, with significant input in data analysis and article revision. MD takes responsibility for the paper as a whole. Funding and support: By Annals policy, all authors are required to disclose any and all commercial, financial, and other relationships in any way related to the subject of this article that might create any potential conflict of interest. See the Manuscript Submission Agreement in this issue for examples of specific conflicts covered by this statement. The authors were supported by a Fleur de Lis Award (intramural funding). This clinical trial was registered with the ClinicalTrials.gov Protocol Registration System. The registration/id number is NCT Publication dates: Received for publication November 3, Revisions received January 27, 2009, and February 19, Accepted for publication March 11, Available online April 30, Presented at the Pediatric Academic Society, May 2008, Honolulu, HI; and the Midwest Society of Pediatric Research, October 2008, Cleveland, OH. Address for reprints: Myto Duong, MD, MS, 800 East Carpenter St, St John s Hospital, Emergency Medicine Department, Springfield, IL 62702; , fax ; mduong@siumed.edu or myto_duong@yahoo.com.myto_duong@yahoo.com Antibiotics for Skin Abscesses REFERENCES 1. Pallin D, Egan J, Pelletier A, et al. Increased US emergency department visits for skin and soft tissue infections, and changes in antibiotic choices, during the emergence of communityassociated methicillin-resistant Staphylococcus aureus. Ann Emerg Med. 2008;51: Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant Staphylococcus aureus infections among patients in the emergency department. N Engl J Med. 2006;355: Kaplan S. Treatment of community-associated methicillin-resistant Staphylococcus aureus infections. Pediatr Infect Dis. 2005;24: Fergie J, Purcell K. Community-acquired methicillin-resistant Staphylococcus aureus infections in south Texas children. Pediatr Infect Dis. 2001;20: Ruhe J, Smith N, Bradsher R, et al. Community onset methicillinresistant Staphylococcus aureus skin and soft tissue infections: impact of antimicrobial therapy. Clin Infect Dis. 2007;44: Lee MC, Rios AM, Aten MF, et al. Management and outcome of children with skin and soft tissue abscesses caused by community-acquired methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis. 2004;23: Young GM. Incision and drainage of a cutaneous abscess. In: Henretig FM, King C, eds. Textbook of Pediatric Emergency Procedures. Baltimore, MD: Williams & Wilkins; 1997: Llera JL, Levy RC. Treatment of cutaneous abscess: a doubleblind clinical study. Ann Emerg Med. 1985;14: Rajendran P, Young D, Maurer T, et al. Randomized, double-blind, placebo-controlled trial of cephalexin for treatment of uncomplicated skin abscesses in a population at risk of community-acquired methicillin-resistant Staphylococcus aureus infection. Antimicrob Agents Chemother. 2007;55: Wilker MA, Cockerill FR, Craig WA, et al. Performance Standards for Antimicrobial Disk Susceptibility Tests: Approved Standard 9 th Edition. Wayne, PA: Clinical and Laboratory Standards Institute; Centers for Disease Control and Prevention. Communityassociated MRSA information for clinicians: questions and answers. Available at: ar_mrsa_ca_clinicians.html. Accessed March 23, Chen A, Goldstein M, Carroll K, et al. Evolving epidemiology of pediatric Staphylococcus aureus cutaneous infections in a Baltimore hospital. Pediatr Emerg Care. 2006;22: Frazee B, Lynn J, Charlebois E, et al. High prevalence of methicillin-resistant Staphylococcus aureus in emergency department skin and soft tissue infections. Ann Emerg Med. 2005;45: Davis S, Perri M, Donabedian S, et al. Epidemiology and outcomes of community-associated methicillin-resistant Staphylococcus aureus infection. J Clin Microbiol. 2007;45: Did you know? You can track the impact of your article with citation alerts that let you know when your article (or any article you d like to track) has been cited by another Elsevier-published journal. Visit today to see what else is new online! Volume 55, NO. 5 : May 2010 Annals of Emergency Medicine 407
INFECTIOUS DISEASE/ORIGINAL RESEARCH
 INFECTIOUS DISEASE/ORIGINAL RESEARCH Randomized Controlled Trial of Trimethoprim-Sulfamethoxazole for Uncomplicated Skin Abscesses in Patients at Risk for Community-Associated Methicillin-Resistant Staphylococcus
INFECTIOUS DISEASE/ORIGINAL RESEARCH Randomized Controlled Trial of Trimethoprim-Sulfamethoxazole for Uncomplicated Skin Abscesses in Patients at Risk for Community-Associated Methicillin-Resistant Staphylococcus
S aureus infections: outpatient treatment. Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium
 S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
HEALTH SERVICES POLICY & PROCEDURE MANUAL
 PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
Management of Skin and Soft-Tissue Infection
 Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices,
 Original Research Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices, 2007-2010 Daniel J. Pallin, MD, MPH Carlos A. Camargo Jr, MD, DrPH Jeremiah D. Schuur,
Original Research Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices, 2007-2010 Daniel J. Pallin, MD, MPH Carlos A. Camargo Jr, MD, DrPH Jeremiah D. Schuur,
Bacterial skin infection
 D i v i s i o n o f P e d i a t r i c E m e r g e n c y M e d i c i n e P a g e 1 Bacterial skin infection Cellulitis w/o abscess Abscess Deep tissue involvement Multiple abscesses Perirectal Anterior
D i v i s i o n o f P e d i a t r i c E m e r g e n c y M e d i c i n e P a g e 1 Bacterial skin infection Cellulitis w/o abscess Abscess Deep tissue involvement Multiple abscesses Perirectal Anterior
5/17/2012 DISCLOSURES OBJECTIVES CONTEMPORARY PEDIATRICS
 CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments
 Original Research Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments Rakesh D. Mistry, MD, MS* Daniel J. Shapiro, BA Monika K. Goyal, MD Theoklis E. Zaoutis Jeffrey
Original Research Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments Rakesh D. Mistry, MD, MS* Daniel J. Shapiro, BA Monika K. Goyal, MD Theoklis E. Zaoutis Jeffrey
Scottish Medicines Consortium
 Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Replaces:04/14/16. Formulated: 1997 SKIN AND SOFT TISSUE INFECTION
 Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
FM - Male, 38YO. MRSA nasal swab (+) Due to positive MRSA nasal swab test, patient will be continued on Vancomycin 1500mg IV q12 for MRSA treatment...
 Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Development of Drugs for Skin Infections
 EFPIA - Skin Infection comments 1 Development of Drugs for Skin Infections John H Rex, MD EFPIA - Skin Infection comments 2 Skin Infections Significant recent debate: Acceptable forms: A focus on fever
EFPIA - Skin Infection comments 1 Development of Drugs for Skin Infections John H Rex, MD EFPIA - Skin Infection comments 2 Skin Infections Significant recent debate: Acceptable forms: A focus on fever
Mrsa abscess and cellulitis
 Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY FINAL Working Group: E. Henderson, M. John, I. Davis, S. Dunford,
Canadian Nosocomial Infection Surveillance Program 2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY FINAL Working Group: E. Henderson, M. John, I. Davis, S. Dunford,
Skin and Soft Tissue Infections Emerging Therapies and 5 things to know
 2011 MFMER slide-1 Skin and Soft Tissue Infections Emerging Therapies and 5 things to know Aaron Tande, MD Assistant Professor of Medicine October 27, 2017 Division of INFECTIOUS DISEASES 2011 MFMER slide-2
2011 MFMER slide-1 Skin and Soft Tissue Infections Emerging Therapies and 5 things to know Aaron Tande, MD Assistant Professor of Medicine October 27, 2017 Division of INFECTIOUS DISEASES 2011 MFMER slide-2
CA-MRSA lesions: What works, what doesn t
 For mass reproduction, content licensing and permissions contact Dowden Health Media. FAMILY David McBride, MD University Student Health Services and the Department of Family Medicine, Boston University
For mass reproduction, content licensing and permissions contact Dowden Health Media. FAMILY David McBride, MD University Student Health Services and the Department of Family Medicine, Boston University
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Scottish Medicines Consortium
 Scottish Medicines Consortium daptomycin 350mg powder for concentrate for solution for infusion (Cubicin ) Chiron Corporation Limited No. (248/06) 10 March 2006 The Scottish Medicines Consortium (SMC)
Scottish Medicines Consortium daptomycin 350mg powder for concentrate for solution for infusion (Cubicin ) Chiron Corporation Limited No. (248/06) 10 March 2006 The Scottish Medicines Consortium (SMC)
11/10/2016. Skin and Soft Tissue Infections. Disclosures. Educational Need/Practice Gap. Objectives. Case #1
 Disclosures Selecting Antimicrobials for Common Infections in Children FMR-Contemporary Pediatrics 11/2016 Sean McTigue, MD Assistant Professor of Pediatrics, Pediatric Infectious Diseases Medical Director
Disclosures Selecting Antimicrobials for Common Infections in Children FMR-Contemporary Pediatrics 11/2016 Sean McTigue, MD Assistant Professor of Pediatrics, Pediatric Infectious Diseases Medical Director
Perichondritis: Source: UpToDate Ciprofloxacin 10 mg/kg/dose PO (max 500 mg/dose) BID Inpatient: Ceftazidime 50 mg/kg/dose q8 hours IV
 Empiric Antibiotics for Pediatric Infections Seen in ED NOTE: Choice of empiric antibiotic therapy must take into account local pathogen frequency and resistance patterns, individual patient characteristics,
Empiric Antibiotics for Pediatric Infections Seen in ED NOTE: Choice of empiric antibiotic therapy must take into account local pathogen frequency and resistance patterns, individual patient characteristics,
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health
 UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Management of Pediatric Skin Abscesses in Pediatric, General Academic and Community Emergency Departments
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Management of Pediatric Skin Abscesses in Pediatric, General Academic and Community Emergency Departments
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections. Skin & Soft Tissue Infections (SSTI)
 Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections 2007 Abscess Cellulitis Bradley W Frazee, MD, FACEP Dept of Emergency Medicine Alameda County Medical Center - Highland Hospital Associate
Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections 2007 Abscess Cellulitis Bradley W Frazee, MD, FACEP Dept of Emergency Medicine Alameda County Medical Center - Highland Hospital Associate
Breastfeeding Challenges - Mastitis & Breast Abscess -
 CLINICAL PRACTICE GUIDELINE Breastfeeding Challenges - Mastitis & Breast Abscess - SCOPE (Area): Maternity Unit, Emergency Department, Paediatrics SCOPE (Staff): Medical, Midwifery & Nursing DESIRED OUTCOME/OBJECTIVE
CLINICAL PRACTICE GUIDELINE Breastfeeding Challenges - Mastitis & Breast Abscess - SCOPE (Area): Maternity Unit, Emergency Department, Paediatrics SCOPE (Staff): Medical, Midwifery & Nursing DESIRED OUTCOME/OBJECTIVE
Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CONTROLLED DOCUMENT
 CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections
 Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Safety of an Out-Patient Intravenous Antibiotics Programme
 Safety of an Out-Patient Intravenous Antibiotics Programme Chan VL, Tang ESK, Leung WS, Wong L, Cheung PS, Chu CM Department of Medicine & Geriatrics United Christian Hospital Outpatient Parental Antimicrobial
Safety of an Out-Patient Intravenous Antibiotics Programme Chan VL, Tang ESK, Leung WS, Wong L, Cheung PS, Chu CM Department of Medicine & Geriatrics United Christian Hospital Outpatient Parental Antimicrobial
Cellulitis and Abscess: ED Phase v 1.1
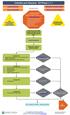 Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
Lyme disease: diagnosis and management
 National Institute for Health and Care Excellence Final Lyme disease: diagnosis and management [D] Evidence review for the management of erythema migrans NICE guideline 95 Evidence review April 2018 Final
National Institute for Health and Care Excellence Final Lyme disease: diagnosis and management [D] Evidence review for the management of erythema migrans NICE guideline 95 Evidence review April 2018 Final
Reduce the risk of recurrence Clear bacterial infections fast and thoroughly
 Reduce the risk of recurrence Clear bacterial infections fast and thoroughly Clearly advanced 140916_Print-Detailer_Englisch_V2_BAH-05-01-14-003_RZ.indd 1 23.09.14 16:59 In bacterial infections, bacteriological
Reduce the risk of recurrence Clear bacterial infections fast and thoroughly Clearly advanced 140916_Print-Detailer_Englisch_V2_BAH-05-01-14-003_RZ.indd 1 23.09.14 16:59 In bacterial infections, bacteriological
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction
 Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
Trimethoprim Sulfamethoxazole versus Placebo for Uncomplicated Skin Abscess
 The new england journal of medicine Original Article Trimethoprim Sulfamethoxazole versus Placebo for Uncomplicated Skin Abscess David A. Talan, M.D., William R. Mower, M.D., Ph.D., Anusha Krishnadasan,
The new england journal of medicine Original Article Trimethoprim Sulfamethoxazole versus Placebo for Uncomplicated Skin Abscess David A. Talan, M.D., William R. Mower, M.D., Ph.D., Anusha Krishnadasan,
ANTIBIOTICS IN THE ER:
 ANTIBIOTICS IN THE ER: EXPLORING THE ROLE OF ANTIMICROBIAL STEWARDSHIP IN THE EMERGENCY DEPARTMENT ANGELINA DAVIS, PHARMD, MS, BCPS (AQ-ID) LIAISON CLINICAL PHARMACIST DUKE ANTIMICROBIAL STEWARDSHIP OUTREACH
ANTIBIOTICS IN THE ER: EXPLORING THE ROLE OF ANTIMICROBIAL STEWARDSHIP IN THE EMERGENCY DEPARTMENT ANGELINA DAVIS, PHARMD, MS, BCPS (AQ-ID) LIAISON CLINICAL PHARMACIST DUKE ANTIMICROBIAL STEWARDSHIP OUTREACH
Infections caused by Methicillin-Resistant Staphylococcus
 MRSA infections are no longer limited to hospitals. An infectious disease specialist offers insight on what this means for dermatologists. By Robert S. Jones, DO, Reading, PA Infections caused by Methicillin-Resistant
MRSA infections are no longer limited to hospitals. An infectious disease specialist offers insight on what this means for dermatologists. By Robert S. Jones, DO, Reading, PA Infections caused by Methicillin-Resistant
Diagnosis and Management of Skin and Soft-tissue Infections
 Diagnosis and Management of Skin and Soft-tissue Infections Skin and soft tissue infections (SSTIs), are referred as skin and skin structure infections. These infections also represent a group of infections
Diagnosis and Management of Skin and Soft-tissue Infections Skin and soft tissue infections (SSTIs), are referred as skin and skin structure infections. These infections also represent a group of infections
Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome
 MAJOR ARTICLE Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome Jörg J. Ruhe, 1,2 Nathaniel Smith, 1,3 Robert W. Bradsher,
MAJOR ARTICLE Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome Jörg J. Ruhe, 1,2 Nathaniel Smith, 1,3 Robert W. Bradsher,
A Placebo-Controlled Trial of Antibiotics for Smaller Skin Abscesses
 Original Article A Placebo-Controlled Trial of Antibiotics for Smaller Skin Abscesses Robert S. Daum, M.D., C.M., Loren G. Miller, M.D., M.P.H., Lilly Immergluck, M.D., Stephanie Fritz, M.D., M.S.C.I.,
Original Article A Placebo-Controlled Trial of Antibiotics for Smaller Skin Abscesses Robert S. Daum, M.D., C.M., Loren G. Miller, M.D., M.P.H., Lilly Immergluck, M.D., Stephanie Fritz, M.D., M.S.C.I.,
amoxycillin/clavulanate vs placebo in the prevention of infection after animal
 Archives of Emergency Medicine, 1989, 6, 251-256 A comparative double blind study of amoxycillin/clavulanate vs placebo in the prevention of infection after animal bites P. H. BRAKENBURY & C. MUWANGA Accident
Archives of Emergency Medicine, 1989, 6, 251-256 A comparative double blind study of amoxycillin/clavulanate vs placebo in the prevention of infection after animal bites P. H. BRAKENBURY & C. MUWANGA Accident
Methicillin Resistant Staphylococcus aureus:
 Methicillin Resistant Staphylococcus aureus: Action-Oriented Guidance for Community-Based Prevention Jackie Dawson, PhD Public Health Epidemiologist Chelan, Douglas, Grant, Kittitas, & Okanogan Counties
Methicillin Resistant Staphylococcus aureus: Action-Oriented Guidance for Community-Based Prevention Jackie Dawson, PhD Public Health Epidemiologist Chelan, Douglas, Grant, Kittitas, & Okanogan Counties
Impact of Systemic Antibiotics on Staphylococcus aureus Colonization and Recurrent Skin Infection
 Clinical Infectious Diseases MAJOR ARTICLE Impact of Systemic Antibiotics on Staphylococcus aureus Colonization and Recurrent Skin Infection Patrick G. Hogan, 1 Marcela Rodriguez, 2 Allison M. Spenner,
Clinical Infectious Diseases MAJOR ARTICLE Impact of Systemic Antibiotics on Staphylococcus aureus Colonization and Recurrent Skin Infection Patrick G. Hogan, 1 Marcela Rodriguez, 2 Allison M. Spenner,
Cefazolin vs. Antistaphyloccal Penicillins: The Great Debate
 Cefazolin vs. Antistaphyloccal Penicillins: The Great Debate Annie Heble, PharmD PGY2 Pediatric Pharmacy Resident Children s Hospital Colorado Microbiology Rounds March 22, 2017 Image Source: Buck cartoons
Cefazolin vs. Antistaphyloccal Penicillins: The Great Debate Annie Heble, PharmD PGY2 Pediatric Pharmacy Resident Children s Hospital Colorado Microbiology Rounds March 22, 2017 Image Source: Buck cartoons
Suitability of Antibiotic Treatment for CAP (CAPTIME) The duration of antibiotic treatment in community acquired pneumonia (CAP)
 STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
Period of study: 12 Nov 2002 to 08 Apr 2004 (first subject s first visit to last subject s last visit)
 Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Antibiotic Abyss. Discussion Points. MRSA Treatment Guidelines
 Antibiotic Abyss Fredrick M. Abrahamian, D.O., FACEP, FIDSA Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical Center Sylmar, California
Antibiotic Abyss Fredrick M. Abrahamian, D.O., FACEP, FIDSA Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical Center Sylmar, California
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
moxifloxacin intravenous, 400mg/250mL, solution for infusion (Avelox ) SMC No. (650/10) Bayer Schering
 moxifloxacin intravenous, 400mg/250mL, solution for infusion (Avelox ) SMC No. (650/10) Bayer Schering 05 November 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
moxifloxacin intravenous, 400mg/250mL, solution for infusion (Avelox ) SMC No. (650/10) Bayer Schering 05 November 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
Prophylactic antibiotic timing and dosage. Dr. Sanjeev Singh AIMS, Kochi
 Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Evaluation of Physician Prescribing Patterns For Antibiotics in the Treatment of Nonnecrotizing Skin and Soft Tissue Infections
 Evaluation of Physician Prescribing Patterns For Antibiotics in the Treatment of Nonnecrotizing Skin and Soft Tissue Infections Michael C. Ezebuenyi, PharmD, BCPS; Fatima Brakta, PharmD, BCPS, AQ-ID; Ifeanyichukwu
Evaluation of Physician Prescribing Patterns For Antibiotics in the Treatment of Nonnecrotizing Skin and Soft Tissue Infections Michael C. Ezebuenyi, PharmD, BCPS; Fatima Brakta, PharmD, BCPS, AQ-ID; Ifeanyichukwu
Author - Dr. Josie Traub-Dargatz
 Author - Dr. Josie Traub-Dargatz Dr. Josie Traub-Dargatz is a professor of equine medicine at Colorado State University (CSU) College of Veterinary Medicine and Biomedical Sciences. She began her veterinary
Author - Dr. Josie Traub-Dargatz Dr. Josie Traub-Dargatz is a professor of equine medicine at Colorado State University (CSU) College of Veterinary Medicine and Biomedical Sciences. She began her veterinary
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process High Priority
 Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction Meaningful Measure Area: Appropriate Use of Healthcare 2019 COLLECTION
Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction Meaningful Measure Area: Appropriate Use of Healthcare 2019 COLLECTION
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #407: Appropriate Treatment of Methicillin-Susceptible Staphylococcus Aureus (MSSA) Bacteremia National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #407: Appropriate Treatment of Methicillin-Susceptible Staphylococcus Aureus (MSSA) Bacteremia National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Antibiotic Stewardship Program (ASP) CHRISTUS SETX
 Antibiotic Stewardship Program (ASP) CHRISTUS SETX Program Goals I. Judicious use of antibiotics Decrease use of broad spectrum antibiotics and deescalate use based on clinical symptoms Therapeutic duplication:
Antibiotic Stewardship Program (ASP) CHRISTUS SETX Program Goals I. Judicious use of antibiotics Decrease use of broad spectrum antibiotics and deescalate use based on clinical symptoms Therapeutic duplication:
Critical Appraisal Topic. Antibiotic Duration in Acute Otitis Media in Children. Carissa Schatz, BSN, RN, FNP-s. University of Mary
 Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
POTENTIAL STRUCTURE INDICATORS FOR EVALUATING ANTIMICROBIAL STEWARDSHIP PROGRAMMES IN EUROPEAN HOSPITALS
 POTENTIAL STRUCTURE INDICATORS FOR EVALUATING ANTIMICROBIAL STEWARDSHIP PROGRAMMES IN EUROPEAN HOSPITALS Dirk VOGELAERS Department of General Internal Medicine, Infectious Diseases and Psychosomatic Medicine
POTENTIAL STRUCTURE INDICATORS FOR EVALUATING ANTIMICROBIAL STEWARDSHIP PROGRAMMES IN EUROPEAN HOSPITALS Dirk VOGELAERS Department of General Internal Medicine, Infectious Diseases and Psychosomatic Medicine
Barriers to Intravenous Penicillin Use for Treatment of Nonmeningitis
 JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Cellulitis. Assoc Prof Mark Thomas. Conference for General Practice Auckland Saturday 28 July 2018
 Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
SKIN AND SOFT TISSUE INFECTIONS OCTOBER 3-4, 2015
 SKIN AND SOFT TISSUE INFECTIONS OCTOBER 3-4, 2015 Disclosures I have no financial conflicts of interest to disclose or report. Steven Tran, PharmD NEFSHP Fall Meeting 2015 Objectives for Pharmacists Review
SKIN AND SOFT TISSUE INFECTIONS OCTOBER 3-4, 2015 Disclosures I have no financial conflicts of interest to disclose or report. Steven Tran, PharmD NEFSHP Fall Meeting 2015 Objectives for Pharmacists Review
Optimizing Antibiotic Stewardship in the ED
 Optimizing Antibiotic Stewardship in the ED Michael Pulia, MD MS FAAEM FACEP Director, UW EM Antibiotic Stewardship Research Program Chair, AAEM Antimicrobial Stewardship Task Force @DrMichaelPulia Learning
Optimizing Antibiotic Stewardship in the ED Michael Pulia, MD MS FAAEM FACEP Director, UW EM Antibiotic Stewardship Research Program Chair, AAEM Antimicrobial Stewardship Task Force @DrMichaelPulia Learning
Surveillance of Multi-Drug Resistant Organisms
 Surveillance of Multi-Drug Resistant Organisms Karen Hoffmann, RN, MS, CIC Associate Director Statewide Program for Infection Control and Epidemiology (SPICE) University of North Carolina School of Medicine
Surveillance of Multi-Drug Resistant Organisms Karen Hoffmann, RN, MS, CIC Associate Director Statewide Program for Infection Control and Epidemiology (SPICE) University of North Carolina School of Medicine
Diabetic Foot Infection. Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals
 Diabetic Foot Infection Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals History of previous amputation [odds ratio (OR)=19.9, P=.01], Peripheral vascular disease (OR=5.5, P=.007)
Diabetic Foot Infection Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals History of previous amputation [odds ratio (OR)=19.9, P=.01], Peripheral vascular disease (OR=5.5, P=.007)
Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days
 Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days Executive Summary National consensus guidelines created jointly by the Infectious Diseases Society of
Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days Executive Summary National consensus guidelines created jointly by the Infectious Diseases Society of
A Prospective Investigation of Nasal Mupirocin, Hexachlorophene Body Wash, and Systemic
 AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
Clinical Policy: Linezolid (Zyvox) Reference Number: CP.PMN.27 Effective Date: Last Review Date: Line of Business: HIM*, Medicaid
 Clinical Policy: (Zyvox) Reference Number: CP.PMN.27 Effective Date: 09.01.06 Last Review Date: 02.19 Line of Business: HIM*, Medicaid Coding Implications Revision Log See Important Reminder at the end
Clinical Policy: (Zyvox) Reference Number: CP.PMN.27 Effective Date: 09.01.06 Last Review Date: 02.19 Line of Business: HIM*, Medicaid Coding Implications Revision Log See Important Reminder at the end
Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children
 Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children Prescribing Antimicrobials for Common Illnesses When treating common illnesses such as ear infections and strep throat,
Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children Prescribing Antimicrobials for Common Illnesses When treating common illnesses such as ear infections and strep throat,
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
 http://dx.doi.org/10.1016/j.jemermed.2015.06.028 The Journal of Emergency Medicine, Vol. 49, No. 6, pp. 998 1003, 2015 Copyright Ó 2015 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/$
http://dx.doi.org/10.1016/j.jemermed.2015.06.028 The Journal of Emergency Medicine, Vol. 49, No. 6, pp. 998 1003, 2015 Copyright Ó 2015 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/$
SESSION 2 8:45 10am. In-office Procedures. Contraindications to Injection. Introduction Joint and Soft Tissue Injection. Learning Objective
 SESSION 2 8:45 10am Procedures You Can Do In Your Office SPEAKER Roger W. Bush, MD, MACP Presenter Disclosure Information The following relationships exist related to this presentation: Roger Bush, MD,
SESSION 2 8:45 10am Procedures You Can Do In Your Office SPEAKER Roger W. Bush, MD, MACP Presenter Disclosure Information The following relationships exist related to this presentation: Roger Bush, MD,
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update
 EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
Why Antimicrobial Stewardship?
 Antimicrobial Stewardship: Why and How CAPT Arjun Srinivasan, MD Associate Director for Healthcare Associated Infection Prevention Programs Division of Healthcare Quality Promotion Why Antimicrobial Stewardship?
Antimicrobial Stewardship: Why and How CAPT Arjun Srinivasan, MD Associate Director for Healthcare Associated Infection Prevention Programs Division of Healthcare Quality Promotion Why Antimicrobial Stewardship?
Risk factors? Insect bites? Hygiene? Household crowding Health literacy
 Recurrent boils Commonest sites face, neck, armpits, shoulders, and buttocks (bottom) infection of the hair root or sweat pore Occur in otherwise healthy people (higher rates in diabetics, eczema, iron
Recurrent boils Commonest sites face, neck, armpits, shoulders, and buttocks (bottom) infection of the hair root or sweat pore Occur in otherwise healthy people (higher rates in diabetics, eczema, iron
Antimicrobial Stewardship Strategy: Antibiograms
 Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Treatment of Surgical Site Infection Meeting Quality Statement 6. Prof Peter Wilson University College London Hospitals
 Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
8/17/2016 ABOUT US REDUCTION OF CLOSTRIDIUM DIFFICILE THROUGH THE USE OF AN ANTIMICROBIAL STEWARDSHIP PROGRAM
 Mary Moore, MS CIC MT (ASCP) Infection Prevention Coordinator Great River Medical Center, West Burlington REDUCTION OF CLOSTRIDIUM DIFFICILE THROUGH THE USE OF AN ANTIMICROBIAL STEWARDSHIP PROGRAM ABOUT
Mary Moore, MS CIC MT (ASCP) Infection Prevention Coordinator Great River Medical Center, West Burlington REDUCTION OF CLOSTRIDIUM DIFFICILE THROUGH THE USE OF AN ANTIMICROBIAL STEWARDSHIP PROGRAM ABOUT
General Approach to Infectious Diseases
 General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus
 Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Treating Rosacea in the Era of Bacterial Resistance. This presentation is sponsored by Galderma Laboratories, L.P.
 Treating Rosacea in the Era of Bacterial Resistance This presentation is sponsored by Galderma Laboratories, L.P. Lecture Discuss rosacea as an inflammatory condition Assess the psychosocial impact of
Treating Rosacea in the Era of Bacterial Resistance This presentation is sponsored by Galderma Laboratories, L.P. Lecture Discuss rosacea as an inflammatory condition Assess the psychosocial impact of
Simplicef is Used to Treat Animals with Skin Infections
 Simplicef is Used to Treat Animals with Skin Infections PRODUCT INFO Simplicef tablets are a semi-synthetic cephalosporin antibiotic cefpodoxime proxetil used to cure infections caused by the susceptible
Simplicef is Used to Treat Animals with Skin Infections PRODUCT INFO Simplicef tablets are a semi-synthetic cephalosporin antibiotic cefpodoxime proxetil used to cure infections caused by the susceptible
Infectious Disease 101: Helping the Consultant Pharmacist with Stewardship Principles
 Infectious Disease 101: Helping the Consultant Pharmacist with Stewardship Principles Conflicts of Interest None at this time May be discussing off-label indications KALIN M. CLIFFORD, PHARM.D., BCPS,
Infectious Disease 101: Helping the Consultant Pharmacist with Stewardship Principles Conflicts of Interest None at this time May be discussing off-label indications KALIN M. CLIFFORD, PHARM.D., BCPS,
Bacterial skin and soft tissues infections (SSTI) are one of the most common 1. infections among different age groups
 Bacterial skin and soft tissues infections (SSTI) are one of the most common 1 infections among different age groups Gram-positive bacteria are the most frequently isolated pathogens from SSTI, with a
Bacterial skin and soft tissues infections (SSTI) are one of the most common 1 infections among different age groups Gram-positive bacteria are the most frequently isolated pathogens from SSTI, with a
Misericordia Community Hospital (MCH) Antimicrobial Stewardship Report. July December 2013 Second and Third Quarters 2014
 H e a l i n g t h e B o d y E n r i c h i n g t h e M i n d N u r t u r i n g t h e S o u l Misericordia Community Hospital (MCH) Antimicrobial Stewardship Report July December 213 Second and Third Quarters
H e a l i n g t h e B o d y E n r i c h i n g t h e M i n d N u r t u r i n g t h e S o u l Misericordia Community Hospital (MCH) Antimicrobial Stewardship Report July December 213 Second and Third Quarters
Potential Conflicts of Interest. Schematic. Reporting AST. Clinically-Oriented AST Reporting & Antimicrobial Stewardship
 Potential Conflicts of Interest Clinically-Oriented AST Reporting & Antimicrobial Stewardship Hsu Li Yang 27 th September 2013 Research Funding: Pfizer Singapore AstraZeneca Janssen-Cilag Merck, Sharpe
Potential Conflicts of Interest Clinically-Oriented AST Reporting & Antimicrobial Stewardship Hsu Li Yang 27 th September 2013 Research Funding: Pfizer Singapore AstraZeneca Janssen-Cilag Merck, Sharpe
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings. Carlos Reyes Sacin, MD, AAHIVS
 Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Study population The target population for the model were hospitalised patients with cellulitis.
 Comparison of linezolid with oxacillin or vancomycin in the empiric treatment of cellulitis in US hospitals Vinken A G, Li J Z, Balan D A, Rittenhouse B E, Willke R J, Goodman C Record Status This is a
Comparison of linezolid with oxacillin or vancomycin in the empiric treatment of cellulitis in US hospitals Vinken A G, Li J Z, Balan D A, Rittenhouse B E, Willke R J, Goodman C Record Status This is a
a. 379 laboratories provided quantitative results, e.g (DD method) to 35.4% (MIC method) of all participants; see Table 2.
 AND QUANTITATIVE PRECISION (SAMPLE UR-01, 2017) Background and Plan of Analysis Sample UR-01 (2017) was sent to API participants as a simulated urine culture for recognition of a significant pathogen colony
AND QUANTITATIVE PRECISION (SAMPLE UR-01, 2017) Background and Plan of Analysis Sample UR-01 (2017) was sent to API participants as a simulated urine culture for recognition of a significant pathogen colony
Received 20 March 2007/Returned for modification 10 July 2007/Accepted 27 August 2007
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
Interventions for children with ear discharge occurring at least two weeks following grommet(ventilation tube) insertion(review)
 Cochrane Database of Systematic Reviews Interventions for children with ear discharge occurring at least two weeks following grommet(ventilation tube) insertion(review) Venekamp RP, Javed F, van Dongen
Cochrane Database of Systematic Reviews Interventions for children with ear discharge occurring at least two weeks following grommet(ventilation tube) insertion(review) Venekamp RP, Javed F, van Dongen
GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS
 Version 3.1 GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS Date ratified June 2008 Updated March 2009 Review date June 2010 Ratified by Authors Consultation Evidence base Changes
Version 3.1 GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS Date ratified June 2008 Updated March 2009 Review date June 2010 Ratified by Authors Consultation Evidence base Changes
Submission for Reclassification
 Submission for Reclassification Fucithalmic (Fusidic Acid 1% Eye Drops) From Prescription Medicine to Restricted Medicine (Pharmacist Only Medicine) CSL Biotherapies (NZ) Limited 666 Great South Road Penrose
Submission for Reclassification Fucithalmic (Fusidic Acid 1% Eye Drops) From Prescription Medicine to Restricted Medicine (Pharmacist Only Medicine) CSL Biotherapies (NZ) Limited 666 Great South Road Penrose
Antimicrobial Stewardship:
 Antimicrobial Stewardship: Inpatient and Outpatient Elements Angela Perhac, PharmD afperhac@carilionclinic.org Disclosure I have no relevant finances to disclose. Objectives Review the core elements of
Antimicrobial Stewardship: Inpatient and Outpatient Elements Angela Perhac, PharmD afperhac@carilionclinic.org Disclosure I have no relevant finances to disclose. Objectives Review the core elements of
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources
 Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Appropriate Management of Common Pediatric Infections. Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases
 Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
