INFECTIOUS DISEASE/ORIGINAL RESEARCH
|
|
|
- Eleanor Gibson
- 6 years ago
- Views:
Transcription
1 INFECTIOUS DISEASE/ORIGINAL RESEARCH Randomized Controlled Trial of Trimethoprim-Sulfamethoxazole for Uncomplicated Skin Abscesses in Patients at Risk for Community-Associated Methicillin-Resistant Staphylococcus aureus Infection Gillian R. Schmitz, MD, David Bruner, MD, Rebecca Pitotti, RN, BSN, Cameron Olderog, MD, Timothy Livengood, MD, Justin Williams, MD, Kermit Huebner, MD, Jeffrey Lightfoot, MD, Brandon Ritz, MD, Christopher Bates, MD, Matthew Schmitz, MD, Mihriye Mete, PhD, Gregory Deye, MD From the Department of Emergency Medicine, Washington Hospital Center, Washington, DC (G. R. Schmitz); the Department of Emergency Medicine, Naval Medical Center, Portsmouth, VA (Bruner, Lightfoot); the Department of Emergency Medicine (Pitotti, Bates) and Department of Orthopaedic Surgery (M. Schmitz), Wilford Hall Medical Center, Lackland Air Force Base, TX; the Department of Emergency Medicine, Brooke Army Medical Center, Ft. Sam Houston, TX (Olderog, Livengood, Williams); the Department of Emergency Medicine, Darnall Army Medical Center, Ft. Hood, TX (Huebner, Ritz); Departments of Epidemiology and Statistics, Medstar Research Institute, Hyattsville, MD (Mete); and the Department of Clinical Pharmacology, Walter Reed Army Institute of Research, Silver Spring, MD (Deye). The opinions expressed in this document are solely those of the authors and do not represent an endorsement by or the views of the United States Air Force, the Department of Defense, or the United States Government. Study objective: Community-associated methicillin-resistant Staphylococcus aureus is now the leading cause of uncomplicated skin abscesses in the United States, and the role of antibiotics is controversial. We evaluate whether trimethoprim-sulfamethoxazole reduces the rate of treatment failures during the 7 days after incision and drainage and whether it reduces new lesion formation within 30 days. Methods: In this multicenter, double-blind, randomized, placebo-controlled trial, we randomized adults to oral trimethoprimsulfamethoxazole or placebo after uncomplicated abscess incision and drainage. Using emergency department rechecks at 2 and 7 days and telephone follow-up, we assessed treatment failure within 7 days, and using clinical follow-up, telephone follow-up, and medical record review, we recorded the development of new lesions within 30 days. Results: We randomized 212 patients, and 190 (90%) were available for 7-day follow-up. We observed a statistically similar incidence of treatment failure in patients receiving trimethoprim-sulfamethoxazole (15/88; 17%) versus placebo (27/102; 26%), difference 9%, 95% confidence interval 2% to 21%; P.12. On 30-day follow-up (successful in 69% of patients), we observed fewer new lesions in the antibiotic (4/46; 9%) versus placebo (14/50; 28%) groups, difference 19%, 95% confidence interval 4% to 34%, P.02. Conclusion: After the incision and drainage of uncomplicated abscesses in adults, treatment with trimethoprimsulfamethoxazole does not reduce treatment failure but may decrease the formation of subsequent lesions. [Ann Emerg Med. 2010;56: ] Please see page 284 for the Editor s Capsule Summary of this article. Provide feedback on this article at the journal s Web site, /$-see front matter Copyright 2010 by the American College of Emergency Physicians. doi: /j.annemergmed INTRODUCTION Background and Importance Skin and soft tissue infections caused by community-associated (CA) methicillin-resistant Staphylococcus aureus (MRSA) pose a clinical challenge because of their increasing incidence, as well as uncertain optimal medical management. CA-MRSA infections have been reported to account for more than 50% of skin and soft tissue infections observed at major medical centers in the United States. 1 CA-MRSA is resistant to cephalexin that had previously been a mainstay of treatment for skin infections. Although prescribing antibiotics with activity against CA- MRSA for skin and soft tissue infections has become increasingly common, 2,3 it remains unclear whether they benefit uncomplicated CA-MRSA abscesses after drainage. High cure rates (91%) have been observed without antibiotics. 4 To our knowledge, there are no previous controlled trials in adults to Volume 56, NO. 3 : September 2010 Annals of Emergency Medicine 283
2 Trimethoprim-Sulfamethoxazole for Skin Abscesses Schmitz et al Editor s Capsule Summary What is already known on this topic With the increasing prevalence of methicillinresistant Staphylococcus aureus, there is concern that incision and drainage may be insufficient treatment for skin abscesses. What question this study addressed After drainage of uncomplicated skin abscesses, does treatment with oral trimethoprim-sulfamethoxazole reduce treatment failure at 7 days? What this study adds to our knowledge This 212-adult, double-blind, randomized, controlled trial found similar rates of treatment failure in patients receiving antibiotics and placebo. How this might change clinical practice Antibiotics are unnecessary after abscess incision and drainage. evaluate antibiotics with activity against CA-MRSA in an emergency department (ED) setting, but trimethoprimsulfamethoxazole did not reduce treatment failure in a recent study of ED children. 5 Goals of This Investigation In ED adults with soft tissue abscesses, we evaluated whether trimethoprim-sulfamethoxazole reduced the rate of treatment failure by 15% relative to placebo during the 7 days after incision and drainage. Secondarily, we assessed the rate of new lesion formation within 30 days. MATERIALS AND METHODS Study Design We conducted a multicenter, double-blind, randomized, placebo-controlled trial (registered under identifiers NCT and NCT at clinicaltrials.gov). The study was approved by the institutional review board at each site, with written informed consent. Setting This study was conducted at 4 military EDs that treat both civilians and military patients: Wilford Hall Medical Center (50,000 visits/year), Brooke Army Medical Center (50,000 visits/year), Darnall Medical Center (43,000 visits/year), and Portsmouth Medical Center (75,000 visits/year). Selection of Participants We enrolled a convenience sample of adults (aged 16 years or older) with uncomplicated skin abscesses requiring incision and drainage between November 20, 2007, and June 1, 2009 Figure. Study enrollment distribution. TMP-SMX, Trimethoprim-sulfamethoxazole. (Figure). We excluded patients who were immunocompromised (eg, diabetes, HIV, cancer), were pregnant or breast feeding, were allergic to sulfa drugs, had associated fever or signs of systemic illness, had received antibiotics in the previous week, or had been hospitalized in the previous month. We excluded abscesses on the face and known or suspected tracts or fistulas to deeper structures, or abscesses requiring operating room drainage. Data Collection and Processing Treating physicians enrolled patients 7 days a week, 24 hours a day, and completed a standard data collection form detailing age, sex, race, and location of abscess. Location of abscess was categorized into head and neck, trunk, axilla, extremity, or groin/buttock. The largest diameter of the abscesses and areas of cellulitis were measured with a standardized ruler in each enrollment packet. Interventions Abscesses were drained and packed with gauze according to standard practice, with incision length, irrigation, and use of ultrasonography at each physician s discretion. Cavity wound cultures were obtained and sent for aerobic and anaerobic culture and antimicrobial susceptibility testing. A block randomization scheme was prepared by the pharmacy, with allocation to each group achieved by opening sequentially numbered, sealed envelopes. Patients assigned to the antibiotic treatment group received trimethoprimsulfamethoxazole (160 mg/800 mg), and those assigned to the control group received identical-appearing placebo capsules, both with instructions to take 2 pills orally twice daily for 7 days. Thus, patients and physicians were blinded to treatment arm. Subjects were asked to return to the ED in 2 days and 7 days for wound rechecks, with repacking and additional visits as clinically appropriate. A study investigator blinded to treatment 284 Annals of Emergency Medicine Volume 56, NO. 3 : September 2010
3 Schmitz et al arm telephoned patients as needed to remind them to return for wound rechecks, inquire about potential medication-related adverse effects, and assess for presence of fever, worsening cellulitis, or new lesions if the patients did not return for follow-up. Methods of Measurement Our primary outcome was treatment failure within 7 days, defined as no improvement after 2 days, development of a new separate lesion within 7 days, or worsening infection within 7 days, leading to an intervention (ie, further antibiotic administration, additional incision and drainage, surgical debridement, or hospital admission). A worsening infection required evidence of an increased diameter of abscess or cellulitis, or the presence of fever or systemic response. Recheck physicians blinded to study arm recorded these outcomes and the supporting clinical findings on a standardized recheck form. Culture results and sensitivities were available if a patient failed treatment to guide therapy. Our secondary outcome was the development of new lesions, abscess or pustule, within 30 days of enrollment. Hence, patients with a primary outcome treatment failure based on a new lesion within 7 days were also classified according to this secondary outcome. One of the 4 study sites (Portsmouth Medical Center) did not collect data on this secondary outcome, and thus its subjects were excluded from this analysis. The secondary outcome was assessed through telephone calls from a study investigator (blinded to treatment arm), any return visits to the ED within 30 days, and review of all further treatment recorded in the medical records. Primary Data Analysis We selected a 15% difference in treatment failure as clinically important, as did a previous similar study. 4 Assuming a 2-sided comparison,.05, and.20, we calculated that 88 patients were needed in each treatment arm. Anticipating that some patients would be lost to follow-up, we intentionally enrolled more subjects than calculated. We analyzed our outcomes with 2 or the Fisher s exact test, using Intercooled Stata 9.2 (StataCorp, College Station, TX). Trimethoprim-Sulfamethoxazole for Skin Abscesses Table 1. Baseline characteristics of the participants. Characteristics Placebo (%) Trimethoprim- Sulfamethoxazole (%) Male 72/116 (62) 68/96 (71) White 62/108 (57) 47/91 (52) Abscess(es) 5 cm 12/116 (10) 6/96 (6) Culture results MRSA 47/100 (47) 50/84 (60) MSSA 22/100 (22) 13/84 (15) Coag neg staph 10/100 (10) 8/84 (10) S viridans 5/100 (5) 1/84 (1) No growth 8/100 (8) 2/84 (2) Other 8/100 (8) 10/84 (12) Abscess location Trunk 21/116 (18) 14/96 (15) Extremity 55/116 (47) 47/96 (49) Groin/buttock 20/116 (17) 20/96 (21) Axilla 14/116 (12) 5/96 (5) Head and neck 6/116 (5) 10/96 (10) Age, y (n 212) n 116 n 96 Median (IQR) 27 (21 38) 28 (21 38) Range Cellulitis, cm (n 212) n 116 n 96 Median (IQR) 5 (0.5 7) 4.5 (2 8) Range Abscess size, cm (n 212) n 116 n 96 Median (IQR) 2.8 ( ) 2.5 (2 3) Range MSSA, Methicillin-sensitive Staphylococcus aureus; IQR, interquartile range. RESULTS Characteristics of Study Subjects We assessed 220 patients for enrollment in the study, with trial flow shown in the Figure. We did not collect information on potential subjects who were not enrolled. Baseline characteristics were similar between the 96 subjects randomized to trimethoprimsulfamethoxazole and the 116 randomized to placebo (Table 1). No patients with abscesses associated with foreign bodies, infected sutures, or bites were enrolled. MRSA was cultured from 53% of subjects overall, with similar rates at the 4 study sites. All isolates were sensitive to trimethoprimsulfamethoxazole. For 7-day follow-up, 190 of 212 (90%) subjects were evaluable. We observed statistically similar rates of 7-day treatment failure between those receiving trimethoprimsulfamethoxazole and placebo (Table 2), and our observed 9% effect size was less than the 15% we predefined as clinically important. For the 3 sites collecting 30-day follow-up data, 43 subjects could not be contacted and were lost to follow-up, leaving 96 of 139 (69%) evaluable. We observed fewer abscesses within 30 days in the trimethoprim-sulfamethoxazole group (Table 3). Post hoc sensitivity analyses assuming extreme opposite outcomes for patients lost to follow-up would change the statistical significance of both primary and secondary outcomes. Ten patients receiving trimethoprim-sulfamethoxazole reported adverse effects: nausea (4), drowsy/dizzy (3), headache and night sweats (1), vaginal yeast infection (1), and a mild allergic reaction (1). One patient receiving placebo reported an adverse effect, ie, feeling drowsy. LIMITATIONS The principal limitation of this study was the loss to followup. Unequal outcome differences in those not returning or unable to be contacted could have altered our outcomes, particularly the 30-day evaluation. Our study is also limited in that it included a convenience sample, although we have no reason to believe that enrolled subjects systematically differed from those not enrolled. We studied only healthy adults, and thus our findings cannot apply to children or the immunocompromised. Finally, we did not standardize the Volume 56, NO. 3 : September 2010 Annals of Emergency Medicine 285
4 Trimethoprim-Sulfamethoxazole for Skin Abscesses Schmitz et al Table 2. Treatment failure at 7 days. Treatment Failure at 7 Days Placebo (n 102) Trimethoprim-Sulfamethoxazole (n 88) Difference, % (95% CI) P Value Total 27 (26%) 15 (17%) 9 ( 2 to 21).12 Nature of treatment failures n 27 n 15 Worsening infection* 15 9 New lesion 8 4 Not clinically improved 4 2 Intervention for treatment failures n 27 n 15 Admitted for IV antibiotics 5 2 IV antibiotics in ED only 3 1 Re-I&D only 3 2 Sent home with antibiotic 9 5 Both re-i&d and sent home with antibiotic 7 5 CI, Confidence interval; IV, intravenous; I&D, incision and drainage. *A worsening infection required evidence of an increased diameter of abscess or cellulitis, or the presence of fever or systemic response. Table 3. Development of new lesions within 30 days. New Lesions Within 30 Days Placebo (n 50) Trimethoprim-Sulfamethoxazole (n 46) Difference, % (95% CI) P Value Total 14 (28%) 4 (9%) 19 (4 34).02 Timing of new lesions, days n 14 n Location of new lesion n 14 n 4 Same limb or body part 11 2 Elsewhere 3 2 incision and drainage technique, but rather left clinicians to use their standard practice. DISCUSSION Although a number of previous studies have evaluated abscess and wound healing, 4-11 to our knowledge we report the first randomized, double-blinded, placebo-controlled trial of trimethoprim-sulfamethoxazole in adults. MRSA has been cultured from 51% 1 to 80% 5 of patients with skin and soft tissue infections, and our rate (53%) was similar. Like those previously reported, 5 our isolates were uniformly sensitive to trimethoprim-sulfamethoxazole. Previous research of antibiotics for CA-MRSA abscesses has been mixed, with results both against 4,6,7 and for 8,9 such therapy. Most do not assess subsequent rates of new lesion development. 5,10,11 Before ours, 2 prospective randomized controlled trials have compared antibiotics versus placebo after abscess incision and drainage. Rajendran et al 4 found no improvement with cephalexin at 7 days, with 84% of patients cured with antibiotics and 91% without. Duong et al 5 also observed similar improvement between trimethoprim-sulfamethoxazole and placebo in ED children, with treatment failure in 4% of patients with antibiotics and 5% without. They also found significantly more new lesions in the placebo group at 10 days (26% versus 13%) but no such difference at 3 months. Our results confirm these 2 previous negative results, and together our trials support the contention that, despite the high frequency of CA-MRSA, antibiotics are not required after incision and drainage of uncomplicated abscesses. We did observe a nonsignificant trend toward efficacy; however, our study was not powered to identify treatment effects of less than 15%. Our findings support those of Duong et al 5 in that trimethoprimsulfamethoxazole may decrease the development of subsequent new lesions. However, this latter analysis is not as robust as our primary outcome because of the large number of subjects lost to follow-up and should be interpreted with caution. In conclusion, the addition of trimethoprim-sulfamethoxazole (160/800) to incision and drainage did not decrease rates of failure by 15% or more by 7 days compared with placebo. However, it may decrease new lesion development within 30 days. The authors thank the Emergency Medicine Foundation and the Surgeon General s Office for funding this study. The authors also thank James Barker, MD, and Vik Bebarta, MD, for their support and mentorship and Mihriye Mete, PhD, and Anneke Bush, PhD, for their assistance with data and statistical analysis. Supervising editor: Steven M. Green, MD Author contributions: GRS and DB conceived the study, designed the trial, and performed the majority of data collection. GRS obtained research funding and drafted the 286 Annals of Emergency Medicine Volume 56, NO. 3 : September 2010
5 Schmitz et al Trimethoprim-Sulfamethoxazole for Skin Abscesses article. GRS, DB, JW, and KH were the primary investigators at each of the 4 study sites and oversaw the conduct of the trial. RP enrolled many of the patients and updated and maintained the databases. RP, CO, TL, JL, BR, and CB made follow-up telephone calls. CO, TL, JL, BR, and CB helped collect data and maintain the study at each site. MS assisted with editing, background research, and writing the article. MM performed the statistical analysis. GD provided feedback for the grant and assisted with editing and writing the article. All authors contributed to revision of the article. GRS takes responsibility for the paper as a whole. Funding and support: By Annals policy, all authors are required to disclose any and all commercial, financial, and other relationships in any way related to the subject of this article that might create any potential conflict of interest. See the Manuscript Submission Agreement in this issue for examples of specific conflicts covered by this statement. This research was funded by EMF EMBRS grant and the Surgeon General s Office. Publication dates: Received for publication January 20, Revision received February 11, Accepted for publication March 1, Available online March 26, Presented as an abstract at the Society of Air Force Clinical Surgeons, April 2009, Denver, CO; the Leadership and Advocacy Conference, April 2009, Washington, DC; and the Scientific Assembly, ACEP Research Forum, October 2009, Boston, MA. Address for correspondence: Gillian R. Schmitz, MD, 714 Carpenter Rd, Alexandria, VA 22314; , fax ; GillianMD@gmail.com. REFERENCES 1. Frazee BW, Lynn J, Charlebois ED, et al. High prevalence of methicillin-resistant Staphylococcus aureus in emergency department skin and soft tissue infections. Ann Emerg Med. 2005;4: Hersh AL, Chambers HF, Maselli JH, et al. National trends in ambulatory visits and antibiotic prescribing for skin and soft tissue infections. Arch Intern Med. 2008;168: LoVecchio F, Perera N, Cassanova L, et al. Board-certified emergency physicians treatment of skin and soft tissue infections in the community-acquired methicillin-resistant Staphylococcus aureus era. Am J Emerg Med. 2009;27: Rajendran PM, Young D, Maurer T, et al. Randomized, double blind, placebo-controlled trial of cephalexin for treatment of uncomplicated skin abscesses in a population at risk for methicillin resistant Staphylococcus aureus. Antimicrob Agents Chemother. 2007;5: Duong M, Markwell S, Peter J, et al. Randomized, controlled trial of antibiotics in the management of community-acquired skin abscesses in the pediatric patient. Ann Emerg Med Lee MC, Rios AM, Aten MF, et al. Management and outcome of children with skin and soft tissue abscesses caused by community-acquired methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis J. 2004;2: Paydar KZ, Hansen SL, Charlebois ED, et al. Inappropriate antibiotic use in soft tissue infections. Arch Surg. 2006;141: Ruhe JJ, Smith N, Bradsher RW, et al. Community-onset methicillin-resistant Staphylococcus aureus skin and soft tissue infections: impact of antimicrobial therapy on outcome. Clin Infect Dis. 2007;44: Szumowski JD, Cohen DE, Kanaya F, et al. Treatment and outcomes of infections by methicillin-resistant Staphylococcus aureus at an ambulatory clinic. Antimicrob Agents Chemother. 2007;51: Macfie J, Harvey J. The treatment of acute superficial abscesses: a prospective clinical trial. Br J Surg. 1977;64: Barnes EV, Dooley DP, Hepburn MJ, et al. Outcomes of community-acquired, methicillin-resistant Staphylococcus aureus, soft tissue infections treated with antibiotics other than vancomycin. Mil Med. 2006;171: Did you know? You can save your online searches and get the results by . Visit today to see what else is new online! Volume 56, NO. 3 : September 2010 Annals of Emergency Medicine 287
Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient
 PEDIATRICS/ORIGINAL RESEARCH Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient Myto Duong, MD, MS Stephen Markwell, MA John Peter,
PEDIATRICS/ORIGINAL RESEARCH Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient Myto Duong, MD, MS Stephen Markwell, MA John Peter,
Management of Skin and Soft-Tissue Infection
 Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments
 Original Research Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments Rakesh D. Mistry, MD, MS* Daniel J. Shapiro, BA Monika K. Goyal, MD Theoklis E. Zaoutis Jeffrey
Original Research Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments Rakesh D. Mistry, MD, MS* Daniel J. Shapiro, BA Monika K. Goyal, MD Theoklis E. Zaoutis Jeffrey
Mrsa abscess and cellulitis
 Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Skin and Soft Tissue Infections Emerging Therapies and 5 things to know
 2011 MFMER slide-1 Skin and Soft Tissue Infections Emerging Therapies and 5 things to know Aaron Tande, MD Assistant Professor of Medicine October 27, 2017 Division of INFECTIOUS DISEASES 2011 MFMER slide-2
2011 MFMER slide-1 Skin and Soft Tissue Infections Emerging Therapies and 5 things to know Aaron Tande, MD Assistant Professor of Medicine October 27, 2017 Division of INFECTIOUS DISEASES 2011 MFMER slide-2
11/10/2016. Skin and Soft Tissue Infections. Disclosures. Educational Need/Practice Gap. Objectives. Case #1
 Disclosures Selecting Antimicrobials for Common Infections in Children FMR-Contemporary Pediatrics 11/2016 Sean McTigue, MD Assistant Professor of Pediatrics, Pediatric Infectious Diseases Medical Director
Disclosures Selecting Antimicrobials for Common Infections in Children FMR-Contemporary Pediatrics 11/2016 Sean McTigue, MD Assistant Professor of Pediatrics, Pediatric Infectious Diseases Medical Director
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections
 Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Scottish Medicines Consortium
 Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
FM - Male, 38YO. MRSA nasal swab (+) Due to positive MRSA nasal swab test, patient will be continued on Vancomycin 1500mg IV q12 for MRSA treatment...
 Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
A Prospective Investigation of Nasal Mupirocin, Hexachlorophene Body Wash, and Systemic
 AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
S aureus infections: outpatient treatment. Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium
 S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Scottish Medicines Consortium
 Scottish Medicines Consortium daptomycin 350mg powder for concentrate for solution for infusion (Cubicin ) Chiron Corporation Limited No. (248/06) 10 March 2006 The Scottish Medicines Consortium (SMC)
Scottish Medicines Consortium daptomycin 350mg powder for concentrate for solution for infusion (Cubicin ) Chiron Corporation Limited No. (248/06) 10 March 2006 The Scottish Medicines Consortium (SMC)
Development of Drugs for Skin Infections
 EFPIA - Skin Infection comments 1 Development of Drugs for Skin Infections John H Rex, MD EFPIA - Skin Infection comments 2 Skin Infections Significant recent debate: Acceptable forms: A focus on fever
EFPIA - Skin Infection comments 1 Development of Drugs for Skin Infections John H Rex, MD EFPIA - Skin Infection comments 2 Skin Infections Significant recent debate: Acceptable forms: A focus on fever
CA-MRSA lesions: What works, what doesn t
 For mass reproduction, content licensing and permissions contact Dowden Health Media. FAMILY David McBride, MD University Student Health Services and the Department of Family Medicine, Boston University
For mass reproduction, content licensing and permissions contact Dowden Health Media. FAMILY David McBride, MD University Student Health Services and the Department of Family Medicine, Boston University
Bacterial skin infection
 D i v i s i o n o f P e d i a t r i c E m e r g e n c y M e d i c i n e P a g e 1 Bacterial skin infection Cellulitis w/o abscess Abscess Deep tissue involvement Multiple abscesses Perirectal Anterior
D i v i s i o n o f P e d i a t r i c E m e r g e n c y M e d i c i n e P a g e 1 Bacterial skin infection Cellulitis w/o abscess Abscess Deep tissue involvement Multiple abscesses Perirectal Anterior
Trimethoprim Sulfamethoxazole versus Placebo for Uncomplicated Skin Abscess
 The new england journal of medicine Original Article Trimethoprim Sulfamethoxazole versus Placebo for Uncomplicated Skin Abscess David A. Talan, M.D., William R. Mower, M.D., Ph.D., Anusha Krishnadasan,
The new england journal of medicine Original Article Trimethoprim Sulfamethoxazole versus Placebo for Uncomplicated Skin Abscess David A. Talan, M.D., William R. Mower, M.D., Ph.D., Anusha Krishnadasan,
amoxycillin/clavulanate vs placebo in the prevention of infection after animal
 Archives of Emergency Medicine, 1989, 6, 251-256 A comparative double blind study of amoxycillin/clavulanate vs placebo in the prevention of infection after animal bites P. H. BRAKENBURY & C. MUWANGA Accident
Archives of Emergency Medicine, 1989, 6, 251-256 A comparative double blind study of amoxycillin/clavulanate vs placebo in the prevention of infection after animal bites P. H. BRAKENBURY & C. MUWANGA Accident
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health
 UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Management of Pediatric Skin Abscesses in Pediatric, General Academic and Community Emergency Departments
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Management of Pediatric Skin Abscesses in Pediatric, General Academic and Community Emergency Departments
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Intra-Abdominal Infections. Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018
 Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices,
 Original Research Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices, 2007-2010 Daniel J. Pallin, MD, MPH Carlos A. Camargo Jr, MD, DrPH Jeremiah D. Schuur,
Original Research Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices, 2007-2010 Daniel J. Pallin, MD, MPH Carlos A. Camargo Jr, MD, DrPH Jeremiah D. Schuur,
MRSA Background. New Challenges From an Old Foe. MRSA Demographics. Comparison of Types of MRSA CA-MRSA HA-MRSA
 Winter Clinical 2017 : MRSA Update Whitney A. High, MD, JD, Meng whitney.high@ucdenver.edu Associate Professor, Dermatology & Pathology Director of Dermatopathology University of Colorado School of Medicine
Winter Clinical 2017 : MRSA Update Whitney A. High, MD, JD, Meng whitney.high@ucdenver.edu Associate Professor, Dermatology & Pathology Director of Dermatopathology University of Colorado School of Medicine
Tandan, Meera; Duane, Sinead; Vellinga, Akke.
 Provided by the author(s) and NUI Galway in accordance with publisher policies. Please cite the published version when available. Title Do general practitioners prescribe more antimicrobials when the weekend
Provided by the author(s) and NUI Galway in accordance with publisher policies. Please cite the published version when available. Title Do general practitioners prescribe more antimicrobials when the weekend
ANTIBIOTICS IN THE ER:
 ANTIBIOTICS IN THE ER: EXPLORING THE ROLE OF ANTIMICROBIAL STEWARDSHIP IN THE EMERGENCY DEPARTMENT ANGELINA DAVIS, PHARMD, MS, BCPS (AQ-ID) LIAISON CLINICAL PHARMACIST DUKE ANTIMICROBIAL STEWARDSHIP OUTREACH
ANTIBIOTICS IN THE ER: EXPLORING THE ROLE OF ANTIMICROBIAL STEWARDSHIP IN THE EMERGENCY DEPARTMENT ANGELINA DAVIS, PHARMD, MS, BCPS (AQ-ID) LIAISON CLINICAL PHARMACIST DUKE ANTIMICROBIAL STEWARDSHIP OUTREACH
HEALTH SERVICES POLICY & PROCEDURE MANUAL
 PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
Surgical prophylaxis for Gram +ve & Gram ve infection
 Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs?
 Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
SKIN AND SOFT TISSUE INFECTIONS OCTOBER 3-4, 2015
 SKIN AND SOFT TISSUE INFECTIONS OCTOBER 3-4, 2015 Disclosures I have no financial conflicts of interest to disclose or report. Steven Tran, PharmD NEFSHP Fall Meeting 2015 Objectives for Pharmacists Review
SKIN AND SOFT TISSUE INFECTIONS OCTOBER 3-4, 2015 Disclosures I have no financial conflicts of interest to disclose or report. Steven Tran, PharmD NEFSHP Fall Meeting 2015 Objectives for Pharmacists Review
Can you treat mrsa with amoxicillin
 Can you treat mrsa with amoxicillin 15-8-2017 Community-associated MRSA You can pick up MRSA outside the hospital, especially if you :. (a related drug developed to treat these germs). Amoxicillin and
Can you treat mrsa with amoxicillin 15-8-2017 Community-associated MRSA You can pick up MRSA outside the hospital, especially if you :. (a related drug developed to treat these germs). Amoxicillin and
Replaces:04/14/16. Formulated: 1997 SKIN AND SOFT TISSUE INFECTION
 Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
ABSTRACT ORIGINAL RESEARCH. Li Wen Loo. Yi Xin Liew. Winnie Lee. Piotr Chlebicki. Andrea Lay-Hoon Kwa
 DOI 10.1007/s40121-015-0085-7 ORIGINAL RESEARCH Impact of Antimicrobial Stewardship Program (ASP) on Outcomes in Patients with Acute Bacterial Skin and Skin Structure Infections (ABSSSIs) in an Acute-
DOI 10.1007/s40121-015-0085-7 ORIGINAL RESEARCH Impact of Antimicrobial Stewardship Program (ASP) on Outcomes in Patients with Acute Bacterial Skin and Skin Structure Infections (ABSSSIs) in an Acute-
Bacterial skin and soft tissues infections (SSTI) are one of the most common 1. infections among different age groups
 Bacterial skin and soft tissues infections (SSTI) are one of the most common 1 infections among different age groups Gram-positive bacteria are the most frequently isolated pathogens from SSTI, with a
Bacterial skin and soft tissues infections (SSTI) are one of the most common 1 infections among different age groups Gram-positive bacteria are the most frequently isolated pathogens from SSTI, with a
A Placebo-Controlled Trial of Antibiotics for Smaller Skin Abscesses
 Original Article A Placebo-Controlled Trial of Antibiotics for Smaller Skin Abscesses Robert S. Daum, M.D., C.M., Loren G. Miller, M.D., M.P.H., Lilly Immergluck, M.D., Stephanie Fritz, M.D., M.S.C.I.,
Original Article A Placebo-Controlled Trial of Antibiotics for Smaller Skin Abscesses Robert S. Daum, M.D., C.M., Loren G. Miller, M.D., M.P.H., Lilly Immergluck, M.D., Stephanie Fritz, M.D., M.S.C.I.,
Infectious Disease Update 2017
 Infectious Disease Update 2017 Greg Moran, MD, FACEP, FIDSA Professor of Clinical Emergency Medicine Geffen School of Medicine at UCLA Dept. of Emergency Medicine and Division of Infectious Diseases Olive
Infectious Disease Update 2017 Greg Moran, MD, FACEP, FIDSA Professor of Clinical Emergency Medicine Geffen School of Medicine at UCLA Dept. of Emergency Medicine and Division of Infectious Diseases Olive
The Impact of meca Gene Testing and Infectious Diseases Pharmacists. Intervention on the Time to Optimal Antimicrobial Therapy for ACCEPTED
 JCM Accepts, published online ahead of print on 7 May 2008 J. Clin. Microbiol. doi:10.1128/jcm.00801-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 7 May 2008 J. Clin. Microbiol. doi:10.1128/jcm.00801-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Impact of Systemic Antibiotics on Staphylococcus aureus Colonization and Recurrent Skin Infection
 Clinical Infectious Diseases MAJOR ARTICLE Impact of Systemic Antibiotics on Staphylococcus aureus Colonization and Recurrent Skin Infection Patrick G. Hogan, 1 Marcela Rodriguez, 2 Allison M. Spenner,
Clinical Infectious Diseases MAJOR ARTICLE Impact of Systemic Antibiotics on Staphylococcus aureus Colonization and Recurrent Skin Infection Patrick G. Hogan, 1 Marcela Rodriguez, 2 Allison M. Spenner,
Suitability of Antibiotic Treatment for CAP (CAPTIME) The duration of antibiotic treatment in community acquired pneumonia (CAP)
 STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts
 Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts Investigational Team: Diane Brideau-Laughlin BSc(Pharm),
Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts Investigational Team: Diane Brideau-Laughlin BSc(Pharm),
Cellulitis and Abscess: ED Phase v 1.1
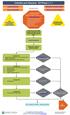 Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
Antimicrobial Stewardship in the Hospital Setting
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
Disclosures. Consider This Case. Objectives. Consequences of Bites. Animal Bites: What to Do and What to Avoid. Animal Bites: Epidemiology
 Animal Bites: What to Do and What to Avoid Meg Fisher, MD Medical Director Disclosures I have no disclosures I do not plan to discuss off label uses of drugs Objectives Manage a child who is bitten Discuss
Animal Bites: What to Do and What to Avoid Meg Fisher, MD Medical Director Disclosures I have no disclosures I do not plan to discuss off label uses of drugs Objectives Manage a child who is bitten Discuss
Treatment and Outcomes of Infections by Methicillin-Resistant Staphylococcus aureus at an Ambulatory Clinic
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2007, p. 423 428 Vol. 51, No. 2 0066-4804/07/$08.00 0 doi:10.1128/aac.01244-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Treatment
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2007, p. 423 428 Vol. 51, No. 2 0066-4804/07/$08.00 0 doi:10.1128/aac.01244-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Treatment
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #464 (NQF 0657): Otitis Media with Effusion: Systemic Antimicrobials - Avoidance of Inappropriate Use National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #464 (NQF 0657): Otitis Media with Effusion: Systemic Antimicrobials - Avoidance of Inappropriate Use National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
MAJOR ARTICLE. identifiable cause of purulent skin infections, that is, abscess and purulent cellulitis [1, 2]. The frequency of
![MAJOR ARTICLE. identifiable cause of purulent skin infections, that is, abscess and purulent cellulitis [1, 2]. The frequency of MAJOR ARTICLE. identifiable cause of purulent skin infections, that is, abscess and purulent cellulitis [1, 2]. The frequency of](/thumbs/72/67424591.jpg) MAJOR ARTICLE Clinical Trial: Comparative Effectiveness of Cephalexin Plus Trimethoprim- Sulfamethoxazole Versus Cephalexin Alone for Treatment of Uncomplicated Cellulitis: A Randomized Controlled Trial
MAJOR ARTICLE Clinical Trial: Comparative Effectiveness of Cephalexin Plus Trimethoprim- Sulfamethoxazole Versus Cephalexin Alone for Treatment of Uncomplicated Cellulitis: A Randomized Controlled Trial
moxifloxacin intravenous, 400mg/250mL, solution for infusion (Avelox ) SMC No. (650/10) Bayer Schering
 moxifloxacin intravenous, 400mg/250mL, solution for infusion (Avelox ) SMC No. (650/10) Bayer Schering 05 November 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
moxifloxacin intravenous, 400mg/250mL, solution for infusion (Avelox ) SMC No. (650/10) Bayer Schering 05 November 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
Breastfeeding Challenges - Mastitis & Breast Abscess -
 CLINICAL PRACTICE GUIDELINE Breastfeeding Challenges - Mastitis & Breast Abscess - SCOPE (Area): Maternity Unit, Emergency Department, Paediatrics SCOPE (Staff): Medical, Midwifery & Nursing DESIRED OUTCOME/OBJECTIVE
CLINICAL PRACTICE GUIDELINE Breastfeeding Challenges - Mastitis & Breast Abscess - SCOPE (Area): Maternity Unit, Emergency Department, Paediatrics SCOPE (Staff): Medical, Midwifery & Nursing DESIRED OUTCOME/OBJECTIVE
Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections. Skin & Soft Tissue Infections (SSTI)
 Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections 2007 Abscess Cellulitis Bradley W Frazee, MD, FACEP Dept of Emergency Medicine Alameda County Medical Center - Highland Hospital Associate
Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections 2007 Abscess Cellulitis Bradley W Frazee, MD, FACEP Dept of Emergency Medicine Alameda County Medical Center - Highland Hospital Associate
Class Update with New Drug Evaluation: Ototopical Antibiotics
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Why Antimicrobial Stewardship?
 Antimicrobial Stewardship: Why and How CAPT Arjun Srinivasan, MD Associate Director for Healthcare Associated Infection Prevention Programs Division of Healthcare Quality Promotion Why Antimicrobial Stewardship?
Antimicrobial Stewardship: Why and How CAPT Arjun Srinivasan, MD Associate Director for Healthcare Associated Infection Prevention Programs Division of Healthcare Quality Promotion Why Antimicrobial Stewardship?
The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection
 THE IRAQI POSTGRADUATE MEDICAL JOURNAL PROPHYLACTIC ANTIBIOTICS ON SURGICAL WOUND INFECTION The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection Ahmed Hamid Jasim*, Nabeel
THE IRAQI POSTGRADUATE MEDICAL JOURNAL PROPHYLACTIC ANTIBIOTICS ON SURGICAL WOUND INFECTION The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection Ahmed Hamid Jasim*, Nabeel
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016
 Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process High Priority
 Quality ID #464 (NQF 0657): Otitis Media with Effusion: Systemic Antimicrobials - Avoidance of Inappropriate Use National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Appropriate
Quality ID #464 (NQF 0657): Otitis Media with Effusion: Systemic Antimicrobials - Avoidance of Inappropriate Use National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Appropriate
Antibiotics in the trenches: An ER Doc s Perspective
 Antibiotics in the trenches: An ER Doc s Perspective Peter Currie, MD Medical Director for Quality Emergency Physicians Professional Association (EPPA) Agenda Emergency Medicine Specific Disease Processes
Antibiotics in the trenches: An ER Doc s Perspective Peter Currie, MD Medical Director for Quality Emergency Physicians Professional Association (EPPA) Agenda Emergency Medicine Specific Disease Processes
All purulence is local - epidemiology and management of skin and soft tissue infections in three urban emergency departments
 University of Massachusetts Medical School escholarship@umms University of Massachusetts Medical School Faculty Publications 12-20-2013 All purulence is local - epidemiology and management of skin and
University of Massachusetts Medical School escholarship@umms University of Massachusetts Medical School Faculty Publications 12-20-2013 All purulence is local - epidemiology and management of skin and
Barriers to Intravenous Penicillin Use for Treatment of Nonmeningitis
 JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM
 UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
Cephalosporins, Quinolones and Co-amoxiclav Prescribing Audit
 Cephalosporins, Quinolones and Co-amoxiclav Prescribing Audit Executive Summary Background Antibiotic resistance poses a significant threat to public health, as antibiotics underpin routine medical practice.
Cephalosporins, Quinolones and Co-amoxiclav Prescribing Audit Executive Summary Background Antibiotic resistance poses a significant threat to public health, as antibiotics underpin routine medical practice.
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #407: Appropriate Treatment of Methicillin-Susceptible Staphylococcus Aureus (MSSA) Bacteremia National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #407: Appropriate Treatment of Methicillin-Susceptible Staphylococcus Aureus (MSSA) Bacteremia National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
General Approach to Infectious Diseases
 General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days
 Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days Executive Summary National consensus guidelines created jointly by the Infectious Diseases Society of
Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days Executive Summary National consensus guidelines created jointly by the Infectious Diseases Society of
Critical Appraisal Topic. Antibiotic Duration in Acute Otitis Media in Children. Carissa Schatz, BSN, RN, FNP-s. University of Mary
 Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Quality Improvement Case Study Don Buckingham, MBOE Senior Quality Improvement Service Line Coordinator
 Quality Improvement Case Study Don Buckingham, MBOE Senior Quality Improvement Service Line Coordinator Began my QI Journey not quite 10 years ago Capstone Project as EVP Marketing Distribution Submitted
Quality Improvement Case Study Don Buckingham, MBOE Senior Quality Improvement Service Line Coordinator Began my QI Journey not quite 10 years ago Capstone Project as EVP Marketing Distribution Submitted
Outpatient Antimicrobial Stewardship. Jeffrey S Gerber, MD, PhD Division of Infectious Diseases The Children s Hospital of Philadelphia
 Outpatient Antimicrobial Stewardship Jeffrey S Gerber, MD, PhD Division of Infectious Diseases The Children s Hospital of Philadelphia Overview The case for outpatient antimicrobial stewardship Interventions
Outpatient Antimicrobial Stewardship Jeffrey S Gerber, MD, PhD Division of Infectious Diseases The Children s Hospital of Philadelphia Overview The case for outpatient antimicrobial stewardship Interventions
Impact of Postoperative Antibiotic Prophylaxis Duration on Surgical Site Infections in Autologous Breast Reconstruction
 Impact of Postoperative Antibiotic Prophylaxis Duration on Surgical Site Infections in Autologous Breast Reconstruction Kerry E. Drury, BA 1 ; Steven T. Lanier, MD 1 ; Nima Khavanin, BS 1 ; Keith M. Hume,
Impact of Postoperative Antibiotic Prophylaxis Duration on Surgical Site Infections in Autologous Breast Reconstruction Kerry E. Drury, BA 1 ; Steven T. Lanier, MD 1 ; Nima Khavanin, BS 1 ; Keith M. Hume,
Cellulitis. Assoc Prof Mark Thomas. Conference for General Practice Auckland Saturday 28 July 2018
 Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
MDRO in LTCF: Forming Networks to Control the Problem
 MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Treatment of Surgical Site Infection Meeting Quality Statement 6. Prof Peter Wilson University College London Hospitals
 Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
11/22/2016. Antimicrobial Stewardship Update Disclosures. Outline. No conflicts of interest to disclose
 Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus
 Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
 http://dx.doi.org/10.1016/j.jemermed.2015.06.028 The Journal of Emergency Medicine, Vol. 49, No. 6, pp. 998 1003, 2015 Copyright Ó 2015 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/$
http://dx.doi.org/10.1016/j.jemermed.2015.06.028 The Journal of Emergency Medicine, Vol. 49, No. 6, pp. 998 1003, 2015 Copyright Ó 2015 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/$
STAPHYLOCOCCUS AUREUS IS THE
 ORIGINAL INVESTIGATION National Trends in Ambulatory Visits and Antibiotic Prescribing for Skin and Soft-Tissue Infections Adam L. Hersh, MD, PhD; Henry F. Chambers, MD; Judith H. Maselli, MSPH; Ralph
ORIGINAL INVESTIGATION National Trends in Ambulatory Visits and Antibiotic Prescribing for Skin and Soft-Tissue Infections Adam L. Hersh, MD, PhD; Henry F. Chambers, MD; Judith H. Maselli, MSPH; Ralph
ANTIBIOTIC STEWARDSHIP
 ANTIBIOTIC STEWARDSHIP S.A. Dehghan Manshadi M.D. Assistant Professor of Infectious Diseases and Tropical Medicine Tehran University of Medical Sciences Issues associated with use of antibiotics were recognized
ANTIBIOTIC STEWARDSHIP S.A. Dehghan Manshadi M.D. Assistant Professor of Infectious Diseases and Tropical Medicine Tehran University of Medical Sciences Issues associated with use of antibiotics were recognized
Implementing Antibiotic Stewardship in Rural and Critical Access Hospitals
 National Center for Emerging and Zoonotic Infectious Diseases Implementing Antibiotic Stewardship in Rural and Critical Access Hospitals Denise Cardo, MD Director, Division of Healthcare Quality Promotion,
National Center for Emerging and Zoonotic Infectious Diseases Implementing Antibiotic Stewardship in Rural and Critical Access Hospitals Denise Cardo, MD Director, Division of Healthcare Quality Promotion,
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017
 Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
ISPUB.COM. Animal Bites And Reconstruction. S Saraf INTRODUCTION PATIENTS AND METHODS
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 3 Number 1 S Saraf Citation S Saraf.. The Internet Journal of Plastic Surgery. 2006 Volume 3 Number 1. Abstract Animal bites resulting in significant
ISPUB.COM The Internet Journal of Plastic Surgery Volume 3 Number 1 S Saraf Citation S Saraf.. The Internet Journal of Plastic Surgery. 2006 Volume 3 Number 1. Abstract Animal bites resulting in significant
Optimizing Antibiotic Stewardship in the ED
 Optimizing Antibiotic Stewardship in the ED Michael Pulia, MD MS FAAEM FACEP Director, UW EM Antibiotic Stewardship Research Program Chair, AAEM Antimicrobial Stewardship Task Force @DrMichaelPulia Learning
Optimizing Antibiotic Stewardship in the ED Michael Pulia, MD MS FAAEM FACEP Director, UW EM Antibiotic Stewardship Research Program Chair, AAEM Antimicrobial Stewardship Task Force @DrMichaelPulia Learning
TITLE: NICU Late-Onset Sepsis Antibiotic Practice Guideline
 Site: Saint Joseph Hospital - NICU Original Effective Date: 6/1/2016 Next Review Date: 6/1/2019 TITLE: Practice Guideline Purpose: Timely and appropriate treatment of late-onset sepsis with antibiotic
Site: Saint Joseph Hospital - NICU Original Effective Date: 6/1/2016 Next Review Date: 6/1/2019 TITLE: Practice Guideline Purpose: Timely and appropriate treatment of late-onset sepsis with antibiotic
New Antibiotics for MRSA
 New Antibiotics for MRSA Faculty Warren S. Joseph, DPM, FIDSA Consultant, Lower Extremity Infectious Diseases Roxborough Memorial Hospital Philadelphia, Pennsylvania Faculty Disclosure Dr. Joseph: Speaker
New Antibiotics for MRSA Faculty Warren S. Joseph, DPM, FIDSA Consultant, Lower Extremity Infectious Diseases Roxborough Memorial Hospital Philadelphia, Pennsylvania Faculty Disclosure Dr. Joseph: Speaker
Advancing Antimicrobial Stewardship in Community and Rural Hospitals
 Advancing Antimicrobial Stewardship in Community and Rural Hospitals Whitney Buckel, PharmD, BCPS Infectious Diseases Clinical Pharmacist Intermountain Medical Center Disclosures The SCORE study was supported
Advancing Antimicrobial Stewardship in Community and Rural Hospitals Whitney Buckel, PharmD, BCPS Infectious Diseases Clinical Pharmacist Intermountain Medical Center Disclosures The SCORE study was supported
TITLE: Antibacterial Sutures for Wound Closure after Surgery: A Review of the Clinical Effectiveness and Long-Term Adverse Effects
 TITLE: Antibacterial Sutures for Wound Closure after Surgery: A Review of the Clinical Effectiveness and Long-Term Adverse Effects DATE: 17 September 2008 CONTEXT AND POLICY ISSUES: Surgical site infections
TITLE: Antibacterial Sutures for Wound Closure after Surgery: A Review of the Clinical Effectiveness and Long-Term Adverse Effects DATE: 17 September 2008 CONTEXT AND POLICY ISSUES: Surgical site infections
Treating Rosacea in the Era of Bacterial Resistance. This presentation is sponsored by Galderma Laboratories, L.P.
 Treating Rosacea in the Era of Bacterial Resistance This presentation is sponsored by Galderma Laboratories, L.P. Lecture Discuss rosacea as an inflammatory condition Assess the psychosocial impact of
Treating Rosacea in the Era of Bacterial Resistance This presentation is sponsored by Galderma Laboratories, L.P. Lecture Discuss rosacea as an inflammatory condition Assess the psychosocial impact of
Preventing Surgical Site Infections. Edward L. Goodman, MD September 16, 2013
 Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources
 Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Community Methicillin- Resistant Staphylococcus aureus. Sixth Plague of Egypt. Epidemiology
 Community Methicillin- Resistant Staphylococcus aureus Henry F. Chambers, M.D. University of California San Francisco San Francisco General Hospital Sixth Plague of Egypt (~ 1200 BCE) So they took soot
Community Methicillin- Resistant Staphylococcus aureus Henry F. Chambers, M.D. University of California San Francisco San Francisco General Hospital Sixth Plague of Egypt (~ 1200 BCE) So they took soot
The Three R s Rethink..Reduce..Rocephin
 The Three R s Rethink..Reduce..Rocephin By: Alisa Cuff RN,BN,CIC and John Bautista B.Sc. (Chem), B.Sc.Pharm, M.Sc.Pharm IPAC National Conference 2017 Newfoundland and Labrador Regional Health Authorities
The Three R s Rethink..Reduce..Rocephin By: Alisa Cuff RN,BN,CIC and John Bautista B.Sc. (Chem), B.Sc.Pharm, M.Sc.Pharm IPAC National Conference 2017 Newfoundland and Labrador Regional Health Authorities
NUOVE IPOTESI e MODELLI di STEWARDSHIP
 Esperienze di successo di antimicrobial stewardship Bologna, 18 novembre 2014 NUOVE IPOTESI e MODELLI di STEWARDSHIP Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Interventions
Esperienze di successo di antimicrobial stewardship Bologna, 18 novembre 2014 NUOVE IPOTESI e MODELLI di STEWARDSHIP Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Interventions
5/17/2012 DISCLOSURES OBJECTIVES CONTEMPORARY PEDIATRICS
 CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare
 Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Period of study: 12 Nov 2002 to 08 Apr 2004 (first subject s first visit to last subject s last visit)
 Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Clinical and Economic Impact of Urinary Tract Infections Caused by Escherichia coli Resistant Isolates
 Clinical and Economic Impact of Urinary Tract Infections Caused by Escherichia coli Resistant Isolates Katia A. ISKANDAR Pharm.D, MHS, AMES, PhD candidate Disclosure Katia A. ISKANDAR declare to meeting
Clinical and Economic Impact of Urinary Tract Infections Caused by Escherichia coli Resistant Isolates Katia A. ISKANDAR Pharm.D, MHS, AMES, PhD candidate Disclosure Katia A. ISKANDAR declare to meeting
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies
 ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
