Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices,
|
|
|
- Ruby Patterson
- 5 years ago
- Views:
Transcription
1 Original Research Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices, Daniel J. Pallin, MD, MPH Carlos A. Camargo Jr, MD, DrPH Jeremiah D. Schuur, MD, MHS Department of Emergency Medicine, Brigham and Women s Hospital, Boston, Massachusetts Supervising Section Editor: Robert Derlet, MD Submission history: Submitted April 23, 2013; Revision received July 15, 2013; Accepted August 26,2013 Electronically published January 6, 2014 Full text available through open access at DOI: /westjem Introduction: National guidelines suggest that most skin abscesses do not require antibiotics, and that cellulitis antibiotics should target streptococci, not community-associated MRSA (CA-MRSA). The objective of this study is to describe antimicrobial treatment of skin infections in U.S. emergency departments (EDs) and analyze potential quality measures. Methods: The National Hospital Ambulatory Medical Care Survey (NHAMCS) is a 4-stage probability sample of all non-federal U.S. ED visits. In 2007 NHAMCS started recording whether incision and drainage was performed at ED visits. We conducted a retrospective analysis, pooling data, identified skin infections using diagnostic codes, and identified abscesses by performance of incision and drainage. We generated national estimates and 95% confidence intervals using weighted analyses; quantified frequencies and proportions; and evaluated antibiotic prescribing practices. We evaluated 4 parameters that might serve as quality measures of antibiotic stewardship, and present 2 of them as potentially robust enough for implementation. Results: Of all ED visits, 3.2% (95% confidence interval %) were for skin infection, and 2.7% ( %) were first visits for skin infection, with no increase over time (p=0.80). However, anti-ca-mrsa antibiotic use increased, from 61% (56-66%) to 74% (71-78%) of antibiotic regimens (p<0.001). Twenty-two percent of visits were for abscess, with a non-significant increase (p=0.06). Potential quality measures: Among discharged abscess patients, 87% were prescribed antibiotics (84-90%, overuse). Among antibiotic regimens for abscess patients, 84% included anti-ca-mrsa agents (81-89%, underuse). Conclusion: From , use of anti-ca-mrsa agents for skin infections increased significantly, despite stable visit frequencies. Antibiotics were over-used for discharged abscess cases, and CA-MRSA-active antibiotics were underused among regimens when antibiotics were used for abscess. [West J Emerg Med. 2014;15(3): ] INTRODUCTION Skin infections are among the most common reasons for seeking medical care. Community-associated methicillinresistant Staphylococcus aureus (CA-MRSA) was first described in the mid-1990s. An epidemic of skin infections followed, and emergency department (ED) visits for skin infection nearly tripled from 1993 to In 2005, skin infections were diagnosed at 3.4 million ED visits and 7.7 million physician office visits in the United States (U.S.). 1,2 CA-MRSA became the most common pathogen isolated from purulent skin infections. 3 Surveillance has been limited by the absence of large studies capable of differentiating abscess from cellulitis. Most epidemiological studies have relied on diagnostic codes from the International Classification of Diseases, Clinical Modification, 9 th Edition (ICD9), which unfortunately groups these 2 conditions within a single category labeled Cellulitis and Abscess. 1,2 For example, ICD9 code 681 Western Journal of Emergency Medicine 282 Volume XV, NO. 3 : May 2014
2 Pallin et al indicates Cellulitis and abscess of finger, toe, or digit. In 2007, the National Hospital Ambulatory Medical Care Survey (NHAMCS) started tracking whether incision and drainage (I&D) was performed during an ED visit, allowing us to analyze nationwide antibiotic prescribing practices for abscess and cellulitis separately. Distinguishing abscess from cellulitis is clinically important because they are treated differently. Evidence-based guidelines recommend that most abscesses be treated with I&D, without antibiotics, and that most cases of cellulitis be treated with antibiotics targeting streptococci, not CA-MRSA. 4 The implication is that only a minority of skin infection patients treated as outpatients require coverage for CA- MRSA. Despite this, use of such antibiotics in this group has increased, reaching 38% of all antibiotic regimens among ED patients with skin infection by Overuse of antibiotics is an important public health and quality issue because it causes antimicrobial resistance, and adverse events such as Clostridium difficile colitis. 5 We analyzed NHAMCS data from , in order to describe antibiotic use at U.S. ED visits for abscess and cellulitis. We analyze 4 potential measures of quality of care regarding antibiotic use in skin infection cases. METHODS We conducted a retrospective analysis of NHAMCS data. NHAMCS is a 4-stage probability-weighted sample of ED visits in all 50 states and the District of Columbia, excluding federal, military, and Veterans Administration hospitals. Its methods have been detailed previously. 6 In brief, trained abstractors collect data on structured data entry forms. Data are subsequently validated and cleaned by staff at the Centers for Disease Control (CDC) and by outside consultants. Further details are available in CDC publications. 6 Since 2007, a specific data field indicates performance of I&D. Another field indicates whether the visit was the first visit for the complaint or a repeat visit. For this analysis, we pooled ED data from We included all observations in the database, without exclusions based on age, demographic characteristics or other characteristics. Skin infection visits were identified by the same ICD9 diagnostic codes used in prior investigations, i.e. cellulitis and abscess of finger (681.00); cellulitis and abscess of toe (681.10); other cellulitis and abscess ( , which includes head, neck, trunk, limbs, and buttocks); cellulitis digit NOS (681.90); felon (681.01); impetigo (684); hidradenitis (705.83); other specified diseases of the hair and hair follicle (i.e. folliculitis, 704.8); neonatal infective mastitis (771.5); nonpurulent mastitis (675.2); breast abscess (675.1); or carbuncle and furuncle ( ). We did not include: onychia, dental abscess, Bartholin s abscess, and pilonidal abscess, following prior investigations. 1 If the ED visit was not the first one for the index condition (i.e. was a follow-up visit), we excluded it from analysis. If I&D was Skin Infections as Targets for Antibiotic Stewardship performed, we classified the skin infection as an abscess. We classified antibiotics according to whether they were agents typically active against CA-MRSA (trimethoprimsulfamethoxazole, clindamycin, tetracyclines, rifampin, linezolid, or vancomycin). 3 We classified ED disposition as discharged or admitted (to intensive care unit, floor, operating room, observation unit, or to another hospital in transfer), and excluded patients who died in the ED or left before being seen or against medical advice. For individual years, , we report descriptive information on the frequency of visits and antibiotic prescribing practices. We also report the results for all years, stratified by region. We evaluated 4 potential quality measures: 1) Use of any antibiotic for discharged abscess patients, a measure of overuse. 4 2) Non-inclusion of agents with activity against CA-MRSA in antibiotic regimens for abscess patients, a measure of underuse. 4 We tested whether this measure would be affected by inclusion of fluoroquinolones in the definition of agents typically active against CA-MRSA, since they often do have such activity and might be chosen due to allergy to other agents, tolerability, desire for co-coverage of Gramnegative bacteria, or for other reasons. 3) Use of CA-MRSAactive agents for discharged cellulitis patients, a measure of overuse. Guidelines suggest that non-purulent cellulitis be treated with agents effective against streptococci, not CA- MRSA, and purulent cellulitis is uncommon. 3,4 4) Use of trimethoprim-sulfamethoxazole monotherapy for cellulitis patients, a measure of misuse. This is relevant because there is doubt about this antibiotic s effectiveness for streptococcal infections. 4 We conducted stratified analyses to determine whether any of the following factors were associated with adherence to these measures: age, sex, or geographic region. We used SAS 9.2 (SAS Institute, Cary, NC) for all analyses, analyzing data using recommended NHAMCS procedures. 6 For comparisons of proportions, we report relative risks and their 95% confidence intervals, and χ 2 testing. To assess trends over time and adjust for independent variables of interest, we used logistic regression, and report odds ratios and their 95% CIs. This study was exempted from review by our IRB. RESULTS Of all U.S. ED visits during , 3.2% included a diagnosis of skin infection (95% CI %). After exclusion of repeat skin infection visits, skin infection was diagnosed at 2.7% of all visits (Table 1). Repeat skin infection visits are excluded from further analyses. The frequency of skin infection visits relative to all other diagnoses did not change year to year (p=0.80). Among skin infection visits, I&D was noted at 22%, with a non-significant year-to-year increase (p=0.06). Antibiotics were prescribed at 83% of skin infection visits, without year-to-year change (p=0.66). An agent typically active against CA-MRSA was included in 68% of regimens when antibiotics were Volume XV, NO. 3 : May Western Journal of Emergency Medicine
3 Skin Infections as Targets for Antibiotic Stewardship Pallin et al Table 1. Skin infection visits, incision and drainage procedures, and antibiotic use, in United States emergency departments, by year, Size of sample and national visit estimates P for trend Number of observations in sample 35,490 34,134 34,942 34, ,502 n/a Estimated number of visits nationwide (thousands) 116, , , , , % confidence interval 101, , , , , , , , , ,738 Skin infection visits (excluding repeat skin infection visits) Estimated skin infection visits nationwide (thousands) 3,234 3,437 3,344 3,798 13, % confidence interval 2,729-3,738 2,975-3,898 2,735-3,953 3,211-4,385 12,231-15,393 Skin infection visits as proportion of all visits nationwide (%) % confidence interval % of skin infection visits with any antibiotic nationwide % confidence interval % of these antibiotic regimens covering CA-MRSA < % confidence interval % of antibiotic regimens with trimethoprimsulfamethoxazole monotherapy % confidence interval % of new skin infection visits with incision & drainage % confidence interval Skin infection visits with incision & drainage (excluding repeat skin infection visits) % of these visits with any antibiotic nationwide % confidence interval % of these antibiotic regimens covering CA-MRSA % confidence interval % of antibiotic regimens with trimethoprimsulfamethoxazole monotherapy % confidence interval Western Journal of Emergency Medicine 284 Volume XV, NO. 3 : May 2014
4 Pallin et al prescribed. From 2007 to 2010, there was a 13% increase in use of regimens active against CA-MRSA (61% in 2007 versus 74% in 2010, p for trend <0.001). Such an agent was used at 56% (95% confidence interval [CI] 54-58%) of all skin infection visits (as distinct from 68% of antibiotic regimens when antibiotics were prescribed). Table 2 shows results by region. All of the nationwide findings described above were accentuated in the South. Skin infections were more common, at 3.2% of all visits, versus in the other regions. I&D was performed at a higher proportion of skin infection visits (26% versus 11-22%), and antibiotics and anti-ca-mrsa antibiotics were used more often. (See Table 2). Our first quality analysis considered the use of antibiotics among visits with outpatient surgical treatment of abscess. Measure adherence was 13%, because antibiotics were used at 87% of these visits (Table 3). Among the covariates analyzed, this practice varied only by region, with the lowest adherence (i.e. most overuse) in the South, as detailed in Table 2. Our second analysis explored the underuse of agents effective against CA-MRSA among antibiotic regimens for abscess visits. As expected, among visits at which at least one antibiotic was prescribed, the probability of an antibiotic Skin Infections as Targets for Antibiotic Stewardship regimen containing an agent typically active against CA- MRSA was higher among abscess versus non-abscess visits (relative risk 2.39, 95% CI ). However, among abscess patients, only 84% of antibiotic regimens included an agent typically active against CA-MRSA (95% CI 81-88%); i.e. nearly 16% of regimens were guideline-non-concordant. When quinolones were included as CA-MRSA-active agents, this percentage was similar, at 86% (95% CI 82-89%). Among the potential covariates, only geographic region demonstrated heterogeneity, with the highest adherence in the South (i.e. least underuse), as detailed in Table 2. Our third analysis examined the use of CA-MRSA-active regimens among discharged patients with cellulitis, a measure of overuse. Among cellulitis visits, 63% of antibiotic regimens included an agent typically active against CA-MRSA (95% CI 60-65%).This increased from 56% (95% CI 50-61%) in 2007 to 68% (95% CI 63-73%) in 2010 (p=0.008). Among discharged cellulitis cases, 63% of regimens included such an agent (95% CI 60-66%). This was similar among admitted cases (62%, 95% CI 56-68%). Among the potential covariates, only geographic region demonstrated heterogeneity, with the most overuse in the South (Table 2). In our fourth analysis, we studied monotherapy with Table 2. Skin infection visits, incision and drainage procedures, and antibiotic use, in emergency departments, by United States region, Skin infection visits (excluding repeat skin infection visits) Northeast Midwest South West p-value* Estimated skin infection visits (thousands) 2,113 2,552 6,554 2,593 < % confidence interval 1,840-2,386 1,879-3,226 5,281-7,827 2,000-3,185 Skin infection visits as proportion of all visits (%) < % confidence interval % of skin infection visits with any antibiotic % confidence interval % of these antibiotic regimens covering CA-MRSA < % confidence interval % of antibiotic regimens with TS monotherapy < % confidence interval % of new skin infection visits with incision & drainage < % confidence interval Skin infection visits with incision & drainage (excluding repeat skin infection visits) % of these visits with any antibiotic nationwide % confidence interval % of these antibiotic regimens covering CA-MRSA % confidence interval % of antibiotic regimens with TS monotherapy % confidence interval CA-MRSA; community-associated methicillin-resistant Staphylococcus aureus; TS, trimethoprim-sulfamethoxazole *p-values are from chi-squared testing, and assess heterogeneity among the four geographic regions. Volume XV, NO. 3 : May Western Journal of Emergency Medicine
5 Skin Infections as Targets for Antibiotic Stewardship trimethoprim-sulfamethoxazole among cellulitis patients. Trimethoprim-sulfamethoxazole was used as the sole antibiotic at 23% of cellulitis visits (95% CI 21-26%), versus 44% of abscess visits (95% CI 39-49%), and in 29% of antibiotic regimens for cellulitis (95% CI 26-31%), versus 50% (95% CI 45-56%) of regimens for abscess. There was no association with patient age. The use of trimethoprimsulfamethoxazole monotherapy also varied regionally, with the most frequent misuse in the South, as detailed in Table 2. DISCUSSION Skin infection was diagnosed at 3.2% of U.S. ED visits during , with no increase during the period. A prior report found that 3.0% of ED visits were for skin infection in This echoes prior findings suggesting that the epidemic may have reached a plateau. 7 Pallin et al When we excluded repeat visits from the analysis, we found that skin infection was diagnosed at 2.7% of visits during , without an increase over time. We observed that 22% of new skin infection visits were for abscess (i.e. were treated with I&D). This is consistent with the results of a single-center study which also found that I&D was performed at 22% of skin infection visits. 8 Our analysis reveals substantial regional variation in the frequency of skin infection relative to other diagnoses, in the frequency of abscess among skin infection, and the likelihood of use of anti-ca-mrsa antibiotics, with the effects of the CA-MRSA epidemic most apparent in the South (Table 2). We have presented 4 potential metrics for assessment of quality of care, which we derived from evidence-based guidelines (Table 3). 4 We believe that 2 of them, one focusing on overuse and another on underuse, might be appropriate Table 3. Proposed quality measures of antibiotic use for skin infections, and performance in United States emergency departments (ED), Level of Performance % Metric name Measure description (domain) Numerator Denominator evidence x (95% CI) Measures with sufficient evidentiary support for implementation Use of antibiotics for outpatient treatment of abscesses Inclusion of CA- MRSA coverage* when using antibiotics for abscess treatment Proportion of discharged ED visits for skin infection undergoing I&D where antibiotics were prescribed (Efficiency; Overuse) Proportion of ED visits for skin infection undergoing I&D where antibiotics were prescribed, but did not include a CA-MRSA active antibiotic* (Effectiveness; Underuse). Denominator visits where antibiotics are given Denominator visits where CA- MRSA active antibiotics* were given ED initial visits for skin infection where I&D was performed and patient was discharged home ED initial visits for skin infection where I&D was performed and antibiotics were prescribed I.A. 87 (84-90) III.A. 84 (81-88) Measures requiring further research Use of CA-MRSA active antibiotics* for outpatient treatment of cellulitis Use of trimethoprimsulfamethoxazole as the only antibiotic for treatment of cellulitis Proportion of discharged ED visits for skin infection not undergoing I&D and receiving antibiotics where CA-MRSA active antibiotics* were used. (Efficiency; Overuse) Proportion of cellulitis patients who receive trimethoprimsulfamethoxazole and no other antibiotic (Effectiveness; Misuse) Denominator visits where CA- MRSA-active* antibiotics were given Denominator visits where trimethoprimsulfamethoxazole was the only antibiotic used ED initial visits for skin infection where I&D was not performed, antibiotics were prescribed, and patient was discharged home ED initial visits for skin infection where I&D was not performed, trimethoprimsulfamethoxazole was prescribed III.C. 63 (60-66) II.C. 23 (21-26) CA-MRSA; community-associated methicillin-resistant Staphylococcus aureus; I&D, incision and drainage *Antibiotics with CA-MRSA activity are defined here as: trimethoprim-sulfamethoxazole, clindamycin, tetracyclines, rifampin, linezolid, or vancomycin. However, fluoroquinolones often have such activity. As measures of overuse or misuse, lower performance is better. As a measure of underuse, a higher proportion is better. x Evidence grading classification detailed in reference [4]. Letter grades indicate strength of recommendation, with A indicating strong evidence, B indicating moderate evidence, and C indicating poor evidence. Roman numerals indicate quality of evidence, with I indicating 1 properly randomized trial, II indicating high-quality controlled observational studies or non-randomized trials, and III indicating expert opinion and case series. Western Journal of Emergency Medicine 286 Volume XV, NO. 3 : May 2014
6 Pallin et al measures for implementation in national quality programs, such as Medicare s Physician Quality Reporting System. 9 Our first proposed measure calculates the proportion of abscess visits ending in discharge at which an antibiotic is used. Multiple studies have shown that routine use of antibiotics for uncomplicated abscesses is not beneficial. 4 We suggest implementing this measure by designating as overuse any use of antibiotics for abscess treated with I&D and discharged from the ED or clinic, while providing an exception that allows the clinician to specify a reason for antibiotic use (such as immunosuppression, large area of surrounding cellulitis, or area difficult to drain). 4 We emphasize that it would never be correct to consider all antibiotic use inappropriate among discharged abscess patients, since there are accepted indications, as listed above. We suggest that this measure of overuse might be valuable as a relative measure, rather than an absolute measure. We found that 87% of discharged abscess patients were treated with antibiotics, suggesting widespread overuse of antibiotics for this common problem. This was most pronounced in the South, at 90%. Our second potential quality measure assesses failure to use agents active against CA-MRSA when using antibiotics to treat abscess patients. Although antibiotics are usually not indicated in the outpatient treatment of skin abscesses, when antibiotics are used, they should cover CA-MRSA. 3,4 We found that nearly 16% of antibiotic regimens prescribed at abscess visits did not include an agent typically active against CA-MRSA. This problem was least common in the South, at 12%. As discussed below, all aspects of performance in the South seem to be directed toward more CA-MRSA coverage, leading to more overuse and less underuse. This is interesting, given our observation that the epidemic appears to be affecting the South disproportionately. Our third analysis examined use of CA-MRSA-active antibiotics for outpatient treatment of cellulitis. We found that 63% of antibiotic regimens for cellulitis treated on the outpatient basis included an agent typically active against CA-MRSA (Table 3). This is not consistent with current IDSA guidelines, which suggest that non-purulent cellulitis be treated with antibiotics targeting streptococci, not CA- MRSA. 4 Purulent cellulitis is uncommon, accounting for only 8% of purulent skin infections. 3 Here again, the proper implementation of the quality measure would probably be to view use of anti-ca-mrsa antibiotics as overuse while allowing exceptions (such as failure of prior therapy or presence of purulence). 4 This and prior studies reveal that antibiotics targeting CA-MRSA are being used much more frequently, despite lack of evidence and guidelines that recommend otherwise. 1,4 Specifically, most cases of abscess do not require antibiotics at all, and most cases of cellulitis should be treated with agents targeting streptococci, not CA-MRSA. We suspect that as clinicians have seen a dramatic rise in the cases of CA-MRSA Skin Infections as Targets for Antibiotic Stewardship skin infections (i.e. abscesses), they have assumed that the same organism was responsible for other skin infections (i.e. cellulitis). Additionally, the presence of screening for MRSA carriage and computerized ED dashboards that display a patient s MRSA status, may lead clinicians to prescribe these antibiotics. However, while this national trend indicates an inappropriate response to the epidemic, there is a problem with applying this criterion to the practice of an individual clinician: clindamycin is a good first-line agent for CA- MRSA-associated infections, and is also a good first-line agent for non-purulent cellulitis, given its coverage of streptococci. 4 While many might view a beta lactam as a preferred first-line agent for non-purulent cellulitis, use of clindamycin would not rise to the level of poor quality care. Therefore, we consider monitoring of the use of anti-ca-mrsa agents for cellulitis to be a topic of epidemiological interest, but not sufficiently robust for evaluation of the quality of healthcare on a caseby-case basis. It also bears mentioning that providers may be skeptical of the IDSA guidelines recommendations for treatment of cellulitis, since they are not based on evidence from clinical trials and since microbiological proof of the etiology of cellulitis is usually impossible to obtain. 4,10 Lastly, we analyzed trimethoprim-sulfamethoxazole monotherapy among cellulitis patients as a potential quality measure. The inappropriateness of this practice would lie in the widely held belief that this antibiotic is not effective for streptococcal infections, leading to recommendations that all non-purulent skin infections be covered with beta lactams or other anti-streptococcal agents. 4 However, the evidence that this antibiotic is not effective for streptococcal infections is from small clinical trials that were done many years ago, and from in vitro studies that may have been influenced by inappropriately high concentrations of thymidine in culture media. 11 One clinical trial that uses trimethoprimsulfamethoxazole monotherapy for cellulitis is under way, and should shed light on this question (NCT ). Pending its publication, it remains prudent to recommend against trimethoprim-sulfamethoxazole monotherapy for streptococcal infections, but we believe that deeming such a practice poor quality would be inaccurate, and do not propose this as a quality measure at this time. In summary, we identified 2 reasonable measures for quality assessment: overuse of antibiotics among abscess patients treated as outpatients with I&D, and use of antibiotic regimens that fail to cover CA-MRSA when using antibiotics for treatment of abscesses. We present the last 2 of our 4 measures as important objects of further study. Evidence for or against the use of anti-ca-mrsa antibiotics in the treatment of cellulitis will come from three ongoing clinical trials (NCT , NCT , NCT ). Our regional analyses reveal interesting patterns of disease occurrence and medical practice. CA-MRSA appears to be causing more abscesses in the South, and prescribers in that region are responding by using more anti-ca-mrsa Volume XV, NO. 3 : May Western Journal of Emergency Medicine
7 Skin Infections as Targets for Antibiotic Stewardship agents. This includes both more overuse, and less underuse. This may be viewed as a well-intentioned but exaggerated response to the CA-MRSA epidemic. These findings mirror prior analyses of regional variation in appropriateness of antibiotic use in Medicare data, which found evidence of inappropriate use in the South. 12 Overall, these results provide clear evidence that the emergence of CA-MRSA continues to have a major impact on prescribing practices for skin infection patients in US EDs, while at the same time providing evidence that the epidemic may have reached a plateau. Before 2001, emergency clinicians almost never used anti-ca-mrsa regimens when treating skin infection patients. 1 But by 2005, 38% of antibiotic regimens for these patients included an agent typically active against CA-MRSA, and the current data show that by 2010, 74% of antibiotic regimens for skin infection patients targeted this organism. This dramatic increase is not justified by current evidence or national guidelines. LIMITATIONS The main limitations of our study are those common to all NHAMCS investigations. 13 Prior research has revealed that when analysis of NHAMCS data provides evidence of errors of omission in medical practice, such evidence should be viewed skeptically, because the data collectors sometimes miss data. 14 A case in point is our observation that only 81% of cellulitis patients received antibiotics. We are skeptical about this, and we assume that the true proportions were higher. We can only assume that many of the discharged patients got prescriptions that the NHAMCS data collectors did not see, or sought care after already receiving antibiotics from another provider. With regard to admitted patients, some of them may have received their antibiotics after they were sent from the ED to the ward. On the other hand, NHAMCS data are probably valid when they reveal errors of commission; there is no known mechanism by which errors of commission could erroneously appear. 14 All retrospective uncontrolled studies are vulnerable to information bias and other unknown threats to validity. A limitation particular to our study is use of I&D as a proxy for the diagnosis of abscess. Some procedures may not have been captured, and in some cases patients with cellulitis may have had I&D without identification of pus. Our prior research has suggested that billing data are specific but not sensitive for positive identification of abscesses among all skin infections. 8 Our first measure, overuse of antibiotics for discharged abscess patients, is caveated by the fact that in the present investigation we were unable to account for chronic comorbidities such as diabetes and immunosuppression. While there is no evidence that patients with these conditions benefit from antibiotics for uncomplicated skin abscesses, current guidelines do recommend that they receive antibiotic treatment as an adjunct to I&D. 4 Our second measure evaluated failure to include anti-ca-mrsa activity in Pallin et al antibiotic regimens for abscess patients. We found that about 16% of such regimens failed to include such agents. While it is conceivable that some of the 16% were data collection errors, our finding of statistically significant regional diversity, which was consistent with the other regional variations we observed, suggests that the data may be a valid measure of underuse we can think of no reason that NHAMCS data collectors would be less likely to miss anti-ca-mrsa antibiotics in the South. CONCLUSION While ED visit rates for skin infection increased from , this study suggests that the epidemic stabilized during The CA-MRSA epidemic has prompted major changes in antibiotic choices for these common infections, and use of anti-ca-mrsa agents continues to increase, despite lack of evidence to support their use in this setting. When treating abscesses, clinicians are using antibiotics too much. This is an appropriate target for quality improvement efforts and national quality metrics aimed at antimicrobial stewardship. When they do use antibiotics to treat abscesses, clinicians are often failing to include anti- CA-MRSA antibiotics. This is a reasonable target in efforts to improve care. When treating cellulitis, use of antibiotics effective against CA-MRSA is rising, despite lack of evidence and despite national guidelines. This may be a reasonable target for efforts to promote stewardship, with the caveats given above. Address for Correspondence: Daniel Pallin, MD, MPH. Brigham and Women s Hospital, 75 Francis St. Boston, MA dpallin@partners.org. Conflicts of Interest: By the WestJEM article submission agreement, all authors are required to disclose all affiliations, funding sources and financial or management relationships that could be perceived as potential sources of bias. The authors disclosed none. REFERENCES 1. Pallin DJ, Egan DJ, Pelletier AJ, et al. Increased US emergency department visits for skin and soft tissue infections, and changes in antibiotic choices, during the emergence of community-associated methicillin-resistant Staphylococcus aureus. Ann Emerg Med. 2008;51(3): Pallin DJ, Espinola JA, Leung DY, et al. Epidemiology of dermatitis and skin infections in United States physicians offices, Clin Infect Dis. 2009;49(6): Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. The N Engl J Med. Aug ;355(7): Western Journal of Emergency Medicine 288 Volume XV, NO. 3 : May 2014
8 Pallin et al Skin Infections as Targets for Antibiotic Stewardship 4. Liu C, Bayer A, Cosgrove SE, et al. Clinical practice guidelines by the infectious diseases society of america for the treatment of methicillinresistant Staphylococcus aureus infections in adults and children. Clin Infect Dis. 2011;52(3):e Bartlett JG. A call to arms: the imperative for antimicrobial stewardship. Clin Infect Dis. 2011;53 Suppl 1:S McCaig LF, McLemore T. Plan and operation of the National Hospital Ambulatory Medical Survey. Series 1: programs and collection procedures. Vital Health Stat (34): Ray GT, Suaya JA, Baxter R. Trends and characteristics of culture-confirmed Staphylococcus aureus infections in a large U.S. integrated health care organization. J Clin Microbiol. 2012;50(6): Qualls ML, Mooney MM, Camargo CA, Jr., et al. Emergency department visit rates for abscess versus other skin infections during the emergence of community-associated methicillin-resistant Staphylococcus aureus, Clin Infect Dis. 2012;55(1): Physicain Quality and Reporting System (formely PQRI). Avaliable at: Accessed 12/10/ Swartz MN. Clinical practice. Cellulitis. N Engl J Med. 2004;350(9): Bowen AC, Lilliebridge RA, Tong SY, et al. Is Streptococcus pyogenes Resistant or Susceptible to Trimethoprim- Sulfamethoxazole? J Clin Microbiol. 2012;50(12): Zhang Y, Steinman MA, Kaplan CM. Geographic Variation in Outpatient Antibiotic Prescribing Among Older Adults. Arch Intern Med. 2012;172(19): McCaig LF, Burt CW. Understanding and interpreting the national hospital ambulatory medical care survey: key questions and answers. Ann Emerg Med. 2012;60(6): e Cooper RJ. NHAMCS: Does It Hold Up to Scrutiny? Ann Emerg Med. 2012;60(6): Volume XV, NO. 3 : May Western Journal of Emergency Medicine
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments
 Original Research Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments Rakesh D. Mistry, MD, MS* Daniel J. Shapiro, BA Monika K. Goyal, MD Theoklis E. Zaoutis Jeffrey
Original Research Clinical Management of Skin and Soft Tissue Infections in the U.S. Emergency Departments Rakesh D. Mistry, MD, MS* Daniel J. Shapiro, BA Monika K. Goyal, MD Theoklis E. Zaoutis Jeffrey
All purulence is local - epidemiology and management of skin and soft tissue infections in three urban emergency departments
 University of Massachusetts Medical School escholarship@umms University of Massachusetts Medical School Faculty Publications 12-20-2013 All purulence is local - epidemiology and management of skin and
University of Massachusetts Medical School escholarship@umms University of Massachusetts Medical School Faculty Publications 12-20-2013 All purulence is local - epidemiology and management of skin and
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017
 Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
11/22/2016. Antimicrobial Stewardship Update Disclosures. Outline. No conflicts of interest to disclose
 Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP)
 IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Concise Antibiogram Toolkit Background
 Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016
 Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Physician Rating: ( 23 Votes ) Rate This Article:
 From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction
 Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
MDPH Antibiotic Resistance Program and the All-Payer Claims Data. Kerri Barton, MDPH Joy Vetter, Boston University, MDPH October 19, 2017
 MDPH Antibiotic Resistance Program and the All-Payer Claims Data Kerri Barton, MDPH Joy Vetter, Boston University, MDPH October 19, 2017 Outline Massachusetts DPH antibiotic resistance work The Massachusetts
MDPH Antibiotic Resistance Program and the All-Payer Claims Data Kerri Barton, MDPH Joy Vetter, Boston University, MDPH October 19, 2017 Outline Massachusetts DPH antibiotic resistance work The Massachusetts
Objective 1/20/2016. Expanding Antimicrobial Stewardship into the Outpatient Setting. Disclosure Statement of Financial Interest
 Expanding Antimicrobial Stewardship into the Outpatient Setting Michael E. Klepser, Pharm.D., FCCP Professor Pharmacy Practice Ferris State University College of Pharmacy Disclosure Statement of Financial
Expanding Antimicrobial Stewardship into the Outpatient Setting Michael E. Klepser, Pharm.D., FCCP Professor Pharmacy Practice Ferris State University College of Pharmacy Disclosure Statement of Financial
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs?
 Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings. Carlos Reyes Sacin, MD, AAHIVS
 Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
ANTIBIOTICS IN THE ER:
 ANTIBIOTICS IN THE ER: EXPLORING THE ROLE OF ANTIMICROBIAL STEWARDSHIP IN THE EMERGENCY DEPARTMENT ANGELINA DAVIS, PHARMD, MS, BCPS (AQ-ID) LIAISON CLINICAL PHARMACIST DUKE ANTIMICROBIAL STEWARDSHIP OUTREACH
ANTIBIOTICS IN THE ER: EXPLORING THE ROLE OF ANTIMICROBIAL STEWARDSHIP IN THE EMERGENCY DEPARTMENT ANGELINA DAVIS, PHARMD, MS, BCPS (AQ-ID) LIAISON CLINICAL PHARMACIST DUKE ANTIMICROBIAL STEWARDSHIP OUTREACH
Measure Information Form
 Release Notes: Measure Information Form Version 3.0b **NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE** Measure Set: Pneumonia (PN) Performance Measure Identifier: Measure Information Form
Release Notes: Measure Information Form Version 3.0b **NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE** Measure Set: Pneumonia (PN) Performance Measure Identifier: Measure Information Form
STAPHYLOCOCCUS AUREUS IS THE
 ORIGINAL INVESTIGATION National Trends in Ambulatory Visits and Antibiotic Prescribing for Skin and Soft-Tissue Infections Adam L. Hersh, MD, PhD; Henry F. Chambers, MD; Judith H. Maselli, MSPH; Ralph
ORIGINAL INVESTIGATION National Trends in Ambulatory Visits and Antibiotic Prescribing for Skin and Soft-Tissue Infections Adam L. Hersh, MD, PhD; Henry F. Chambers, MD; Judith H. Maselli, MSPH; Ralph
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM
 UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process High Priority
 Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction Meaningful Measure Area: Appropriate Use of Healthcare 2019 COLLECTION
Quality ID #66: Appropriate Testing for Children with Pharyngitis National Quality Strategy Domain: Efficiency and Cost Reduction Meaningful Measure Area: Appropriate Use of Healthcare 2019 COLLECTION
Challenges and opportunities for rapidly advancing reporting and improving inpatient antibiotic use in the U.S.
 Challenges and opportunities for rapidly advancing reporting and improving inpatient antibiotic use in the U.S. Overview of benchmarking Antibiotic Use Scott Fridkin, MD, Senior Advisor for Antimicrobial
Challenges and opportunities for rapidly advancing reporting and improving inpatient antibiotic use in the U.S. Overview of benchmarking Antibiotic Use Scott Fridkin, MD, Senior Advisor for Antimicrobial
Antibiotic Stewardship and Critical Access Hospitals. Robert White, BA, PT, CPHQ Program Manager TMF Quality Innovation Network
 Antibiotic Stewardship and Critical Access Hospitals Robert White, BA, PT, CPHQ Program Manager TMF Quality Innovation Network Antibiotic-Resistant Bacteria A serious threat to public health and the economy
Antibiotic Stewardship and Critical Access Hospitals Robert White, BA, PT, CPHQ Program Manager TMF Quality Innovation Network Antibiotic-Resistant Bacteria A serious threat to public health and the economy
Skin and Soft Tissue Infections Emerging Therapies and 5 things to know
 2011 MFMER slide-1 Skin and Soft Tissue Infections Emerging Therapies and 5 things to know Aaron Tande, MD Assistant Professor of Medicine October 27, 2017 Division of INFECTIOUS DISEASES 2011 MFMER slide-2
2011 MFMER slide-1 Skin and Soft Tissue Infections Emerging Therapies and 5 things to know Aaron Tande, MD Assistant Professor of Medicine October 27, 2017 Division of INFECTIOUS DISEASES 2011 MFMER slide-2
Mrsa abscess and cellulitis
 Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
Antibiotic stewardship in long term care
 Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Scottish Medicines Consortium
 Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources
 Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Combination vs Monotherapy for Gram Negative Septic Shock
 Combination vs Monotherapy for Gram Negative Septic Shock Critical Care Canada Forum November 8, 2018 Michael Klompas MD, MPH, FIDSA, FSHEA Professor, Harvard Medical School Hospital Epidemiologist, Brigham
Combination vs Monotherapy for Gram Negative Septic Shock Critical Care Canada Forum November 8, 2018 Michael Klompas MD, MPH, FIDSA, FSHEA Professor, Harvard Medical School Hospital Epidemiologist, Brigham
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare
 Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
S aureus infections: outpatient treatment. Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium
 S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
6/15/2017 PART 1: THE PROBLEM. Objectives. What is Antimicrobial Resistance? Conflicts of Interest Disclosure Statement
 Conflicts of Interest Disclosure Statement Getting a grasp on Antibiotic Use and Resistance: Principles of Antimicrobial Stewardship Speaker has nothing to disclose. Jacob M Kesner, PharmD UNMH PGY-2 Infectious
Conflicts of Interest Disclosure Statement Getting a grasp on Antibiotic Use and Resistance: Principles of Antimicrobial Stewardship Speaker has nothing to disclose. Jacob M Kesner, PharmD UNMH PGY-2 Infectious
Critical Appraisal Topic. Antibiotic Duration in Acute Otitis Media in Children. Carissa Schatz, BSN, RN, FNP-s. University of Mary
 Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
HEALTH SERVICES POLICY & PROCEDURE MANUAL
 PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
Replaces:04/14/16. Formulated: 1997 SKIN AND SOFT TISSUE INFECTION
 Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Predictors of the Diagnosis and Antibiotic Prescribing to Patients Presenting with Acute Respiratory Infections
 Predictors of the Diagnosis and Antibiotic Prescribing to Patients Presenting with Acute Respiratory Infections BY RYAN JOERRES CAPSTONE COMMITTEE MEMBERS: DENNIS J. BAUMGARDNER, MD, AJAY K. SETHI, PH.D.,
Predictors of the Diagnosis and Antibiotic Prescribing to Patients Presenting with Acute Respiratory Infections BY RYAN JOERRES CAPSTONE COMMITTEE MEMBERS: DENNIS J. BAUMGARDNER, MD, AJAY K. SETHI, PH.D.,
Objectives 4/26/2017. Co-Investigators Sadie Giuliani, PharmD, BCPS Claude Tonnerre, MD Jayme Hartzell, PharmD, MS, BCPS
 IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
Community-Associated C. difficile Infection: Think Outside the Hospital. Maria Bye, MPH Epidemiologist May 1, 2018
 Community-Associated C. difficile Infection: Think Outside the Hospital Maria Bye, MPH Epidemiologist Maria.Bye@state.mn.us 651-201-4085 May 1, 2018 Clostridium difficile Clostridium difficile Clostridium
Community-Associated C. difficile Infection: Think Outside the Hospital Maria Bye, MPH Epidemiologist Maria.Bye@state.mn.us 651-201-4085 May 1, 2018 Clostridium difficile Clostridium difficile Clostridium
Antimicrobial Stewardship in Ambulatory Care
 Antimicrobial Stewardship in Ambulatory Care Nila Suntharam, M.D. May 5, 2017 Dr. Suntharam indicated no potential conflict of interest to this presentation. She does not intend to discuss any unapproved/investigative
Antimicrobial Stewardship in Ambulatory Care Nila Suntharam, M.D. May 5, 2017 Dr. Suntharam indicated no potential conflict of interest to this presentation. She does not intend to discuss any unapproved/investigative
Burden of disease of antibiotic resistance The example of MRSA. Eva Melander Clinical Microbiology, Lund University Hospital
 Burden of disease of antibiotic resistance The example of MRSA Eva Melander Clinical Microbiology, Lund University Hospital Discovery of antibiotics Enormous medical gains Significantly reduced morbidity
Burden of disease of antibiotic resistance The example of MRSA Eva Melander Clinical Microbiology, Lund University Hospital Discovery of antibiotics Enormous medical gains Significantly reduced morbidity
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Treatment of Surgical Site Infection Meeting Quality Statement 6. Prof Peter Wilson University College London Hospitals
 Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process High Priority
 Quality ID #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction Meaningful Measure Area: Appropriate
Quality ID #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction Meaningful Measure Area: Appropriate
Core Elements of Antibiotic Stewardship for Nursing Homes
 Core Elements of Antibiotic Stewardship for Nursing Homes Nimalie D. Stone, MD, MS Medical Epidemiologist for LTC Division of Healthcare Quality Promotion Centers for Disease Control and Prevention Antimicrobial
Core Elements of Antibiotic Stewardship for Nursing Homes Nimalie D. Stone, MD, MS Medical Epidemiologist for LTC Division of Healthcare Quality Promotion Centers for Disease Control and Prevention Antimicrobial
Optimizing Antibiotic Stewardship in the ED
 Optimizing Antibiotic Stewardship in the ED Michael Pulia, MD MS FAAEM FACEP Director, UW EM Antibiotic Stewardship Research Program Chair, AAEM Antimicrobial Stewardship Task Force @DrMichaelPulia Learning
Optimizing Antibiotic Stewardship in the ED Michael Pulia, MD MS FAAEM FACEP Director, UW EM Antibiotic Stewardship Research Program Chair, AAEM Antimicrobial Stewardship Task Force @DrMichaelPulia Learning
FM - Male, 38YO. MRSA nasal swab (+) Due to positive MRSA nasal swab test, patient will be continued on Vancomycin 1500mg IV q12 for MRSA treatment...
 Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Preventing and Responding to Antibiotic Resistant Infections in New Hampshire
 Preventing and Responding to Antibiotic Resistant Infections in New Hampshire Benjamin P. Chan, MD, MPH NH Dept. of Health & Human Services Division of Public Health Services May 23, 2017 To bring a greater
Preventing and Responding to Antibiotic Resistant Infections in New Hampshire Benjamin P. Chan, MD, MPH NH Dept. of Health & Human Services Division of Public Health Services May 23, 2017 To bring a greater
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Antimicrobial Stewardship in the Hospital Setting
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
Cellulitis and Abscess: ED Phase v 1.1
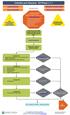 Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update
 EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Antimicrobial Stewardship:
 Antimicrobial Stewardship: Inpatient and Outpatient Elements Angela Perhac, PharmD afperhac@carilionclinic.org Disclosure I have no relevant finances to disclose. Objectives Review the core elements of
Antimicrobial Stewardship: Inpatient and Outpatient Elements Angela Perhac, PharmD afperhac@carilionclinic.org Disclosure I have no relevant finances to disclose. Objectives Review the core elements of
Hot Topics in Antimicrobial Stewardship. Meghan Brett, MD Medical Director, Antimicrobial Stewardship University of New Mexico Hospital
 Hot Topics in Antimicrobial Stewardship Meghan Brett, MD Medical Director, Antimicrobial Stewardship University of New Mexico Hospital Antimicrobial Stewardship Goals Primary Goal Optimize clinical outcomes
Hot Topics in Antimicrobial Stewardship Meghan Brett, MD Medical Director, Antimicrobial Stewardship University of New Mexico Hospital Antimicrobial Stewardship Goals Primary Goal Optimize clinical outcomes
3/1/2016. Antibiotics --When Less is More. Most Urgent Threats. Serious Threats
 Antibiotics --When Less is More Ralph Gonzales, MD, MSPH Associate Dean, Clinical Innovation School of Medicine VP, Clinical Innovation, UCSF Health Most Urgent Threats Serious Threats Multidrug-Resistant
Antibiotics --When Less is More Ralph Gonzales, MD, MSPH Associate Dean, Clinical Innovation School of Medicine VP, Clinical Innovation, UCSF Health Most Urgent Threats Serious Threats Multidrug-Resistant
Barriers to Intravenous Penicillin Use for Treatment of Nonmeningitis
 JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Schweizer et al. Antimicrobial Resistance and Infection Control 2013, 2:28
 Schweizer et al. Antimicrobial Resistance and Infection Control 2013, 2:28 RESEARCH Open Access Optimizing antimicrobial prescribing: Are clinicians following national trends in methicillin-resistant staphylococcus
Schweizer et al. Antimicrobial Resistance and Infection Control 2013, 2:28 RESEARCH Open Access Optimizing antimicrobial prescribing: Are clinicians following national trends in methicillin-resistant staphylococcus
The Core Elements of Antibiotic Stewardship for Nursing Homes
 The Core Elements of Antibiotic Stewardship for Nursing Homes APPENDIX B: Measures of Antibiotic Prescribing, Use and Outcomes National Center for Emerging and Zoonotic Infectious Diseases Division of
The Core Elements of Antibiotic Stewardship for Nursing Homes APPENDIX B: Measures of Antibiotic Prescribing, Use and Outcomes National Center for Emerging and Zoonotic Infectious Diseases Division of
Incidence of hospital-acquired Clostridium difficile infection in patients at risk
 Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 5-20-2016 Incidence of hospital-acquired Clostridium difficile infection in patients at risk Christine Ibarra
Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 5-20-2016 Incidence of hospital-acquired Clostridium difficile infection in patients at risk Christine Ibarra
2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY FINAL Working Group: E. Henderson, M. John, I. Davis, S. Dunford,
Canadian Nosocomial Infection Surveillance Program 2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY FINAL Working Group: E. Henderson, M. John, I. Davis, S. Dunford,
Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient
 PEDIATRICS/ORIGINAL RESEARCH Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient Myto Duong, MD, MS Stephen Markwell, MA John Peter,
PEDIATRICS/ORIGINAL RESEARCH Randomized, Controlled Trial of Antibiotics in the Management of Community-Acquired Skin Abscesses in the Pediatric Patient Myto Duong, MD, MS Stephen Markwell, MA John Peter,
Updates in Antimicrobial Stewardship
 Updates in Antimicrobial Stewardship Andrew Hunter, Pharm.D., BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center andrew.hunter@va.gov Disclosures No disclosures
Updates in Antimicrobial Stewardship Andrew Hunter, Pharm.D., BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center andrew.hunter@va.gov Disclosures No disclosures
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections
 Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Doxycycline staph aureus
 Search Search Doxycycline staph aureus Mercer infection is the one of the colloquial terms given for MRSA (Methicillin-Resistant Staphylococcus Aureus ) infection. Initially, Staphylococcal resistance
Search Search Doxycycline staph aureus Mercer infection is the one of the colloquial terms given for MRSA (Methicillin-Resistant Staphylococcus Aureus ) infection. Initially, Staphylococcal resistance
TREAT Steward. Antimicrobial Stewardship software with personalized decision support
 TREAT Steward TM Antimicrobial Stewardship software with personalized decision support ANTIMICROBIAL STEWARDSHIP - Interdisciplinary actions to improve patient care Quality Assurance The aim of antimicrobial
TREAT Steward TM Antimicrobial Stewardship software with personalized decision support ANTIMICROBIAL STEWARDSHIP - Interdisciplinary actions to improve patient care Quality Assurance The aim of antimicrobial
11-ID-10. Committee: Infectious Disease. Title: Creation of a National Campylobacteriosis Case Definition
 11-ID-10 Committee: Infectious Disease Title: Creation of a National Campylobacteriosis Case Definition I. Statement of the Problem Although campylobacteriosis is not nationally-notifiable, it is a disease
11-ID-10 Committee: Infectious Disease Title: Creation of a National Campylobacteriosis Case Definition I. Statement of the Problem Although campylobacteriosis is not nationally-notifiable, it is a disease
A Prospective Investigation of Nasal Mupirocin, Hexachlorophene Body Wash, and Systemic
 AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
ANTIBIOTIC STEWARDSHIP
 ANTIBIOTIC STEWARDSHIP S.A. Dehghan Manshadi M.D. Assistant Professor of Infectious Diseases and Tropical Medicine Tehran University of Medical Sciences Issues associated with use of antibiotics were recognized
ANTIBIOTIC STEWARDSHIP S.A. Dehghan Manshadi M.D. Assistant Professor of Infectious Diseases and Tropical Medicine Tehran University of Medical Sciences Issues associated with use of antibiotics were recognized
GUIDE TO INFECTION CONTROL IN THE HOSPITAL
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Compliance with antibiotic treatment guidelines in managed care patients with communityacquired pneumonia in ambulatory settings
 Compliance with antibiotic treatment guidelines in managed care patients with communityacquired pneumonia in ambulatory settings Jasmanda H. Wu, Ph.D., 1 David H. Howard, Ph.D., 2 John E. McGowan, Jr.,
Compliance with antibiotic treatment guidelines in managed care patients with communityacquired pneumonia in ambulatory settings Jasmanda H. Wu, Ph.D., 1 David H. Howard, Ph.D., 2 John E. McGowan, Jr.,
What is an Antibiotic Stewardship Program?
 What is an Antibiotic Stewardship Program? Jane Rogers, R.N. Anne Messer, MPH Learning Session #4 August 15, 2017 National Nursing Home Quality Care Collaborative Change Package Change Bundle: To prevent
What is an Antibiotic Stewardship Program? Jane Rogers, R.N. Anne Messer, MPH Learning Session #4 August 15, 2017 National Nursing Home Quality Care Collaborative Change Package Change Bundle: To prevent
Clinical Policy: Linezolid (Zyvox) Reference Number: CP.PMN.27 Effective Date: Last Review Date: Line of Business: HIM*, Medicaid
 Clinical Policy: (Zyvox) Reference Number: CP.PMN.27 Effective Date: 09.01.06 Last Review Date: 02.19 Line of Business: HIM*, Medicaid Coding Implications Revision Log See Important Reminder at the end
Clinical Policy: (Zyvox) Reference Number: CP.PMN.27 Effective Date: 09.01.06 Last Review Date: 02.19 Line of Business: HIM*, Medicaid Coding Implications Revision Log See Important Reminder at the end
Antibiotics in the trenches: An ER Doc s Perspective
 Antibiotics in the trenches: An ER Doc s Perspective Peter Currie, MD Medical Director for Quality Emergency Physicians Professional Association (EPPA) Agenda Emergency Medicine Specific Disease Processes
Antibiotics in the trenches: An ER Doc s Perspective Peter Currie, MD Medical Director for Quality Emergency Physicians Professional Association (EPPA) Agenda Emergency Medicine Specific Disease Processes
Bacterial skin infection
 D i v i s i o n o f P e d i a t r i c E m e r g e n c y M e d i c i n e P a g e 1 Bacterial skin infection Cellulitis w/o abscess Abscess Deep tissue involvement Multiple abscesses Perirectal Anterior
D i v i s i o n o f P e d i a t r i c E m e r g e n c y M e d i c i n e P a g e 1 Bacterial skin infection Cellulitis w/o abscess Abscess Deep tissue involvement Multiple abscesses Perirectal Anterior
Implementing Antibiotic Stewardship in Rural and Critical Access Hospitals
 National Center for Emerging and Zoonotic Infectious Diseases Implementing Antibiotic Stewardship in Rural and Critical Access Hospitals Denise Cardo, MD Director, Division of Healthcare Quality Promotion,
National Center for Emerging and Zoonotic Infectious Diseases Implementing Antibiotic Stewardship in Rural and Critical Access Hospitals Denise Cardo, MD Director, Division of Healthcare Quality Promotion,
Geriatric Mental Health Partnership
 Geriatric Mental Health Partnership September 8, 2017 First, let s test your knowledge about antibiotics http://www.cdc.gov/getsmart/community/about/quiz.html 2 Get Smart Antibiotics Quiz Antibiotics fight
Geriatric Mental Health Partnership September 8, 2017 First, let s test your knowledge about antibiotics http://www.cdc.gov/getsmart/community/about/quiz.html 2 Get Smart Antibiotics Quiz Antibiotics fight
4/3/2017 CLINICAL PEARLS: UPDATES IN THE MANAGEMENT OF NOSOCOMIAL PNEUMONIA DISCLOSURE LEARNING OBJECTIVES
 CLINICAL PEARLS: UPDATES IN THE MANAGEMENT OF NOSOCOMIAL PNEUMONIA BILLIE BARTEL, PHARMD, BCCCP APRIL 7 TH, 2017 DISCLOSURE I have had no financial relationship over the past 12 months with any commercial
CLINICAL PEARLS: UPDATES IN THE MANAGEMENT OF NOSOCOMIAL PNEUMONIA BILLIE BARTEL, PHARMD, BCCCP APRIL 7 TH, 2017 DISCLOSURE I have had no financial relationship over the past 12 months with any commercial
Antibiotic Stewardship in the LTC Setting
 Antibiotic Stewardship in the LTC Setting Joe Litsey, Director of Consulting Services Pharm.D., Board Certified Geriatric Pharmacist Thrifty White Pharmacy Objectives Describe the Antibiotic Stewardship
Antibiotic Stewardship in the LTC Setting Joe Litsey, Director of Consulting Services Pharm.D., Board Certified Geriatric Pharmacist Thrifty White Pharmacy Objectives Describe the Antibiotic Stewardship
IDSA GUIDELINES COMMUNITY ACQUIRED PNEUMONIA
 page 1 / 5 page 2 / 5 idsa guidelines community acquired pdf IDSA/ATS Guidelines for CAP in Adults CID 2007:44 (Suppl 2) S29 such as blood and sputum cultures. Conversely, these cultures may have a major
page 1 / 5 page 2 / 5 idsa guidelines community acquired pdf IDSA/ATS Guidelines for CAP in Adults CID 2007:44 (Suppl 2) S29 such as blood and sputum cultures. Conversely, these cultures may have a major
The Pennsylvania State University. The Graduate School. College of Medicine ASSESSING AND COMPARING ANTIBIOTIC THERAPY TRENDS FOR CHILDREN
 The Pennsylvania State University The Graduate School College of Medicine ASSESSING AND COMPARING ANTIBIOTIC THERAPY TRENDS FOR CHILDREN WITH ACUTE OTITIS MEDIA FROM 2005 TO 2014 IN U.S A Thesis in Public
The Pennsylvania State University The Graduate School College of Medicine ASSESSING AND COMPARING ANTIBIOTIC THERAPY TRENDS FOR CHILDREN WITH ACUTE OTITIS MEDIA FROM 2005 TO 2014 IN U.S A Thesis in Public
Study Protocol. Funding: German Center for Infection Research (TTU-HAARBI, Research Clinical Unit)
 Effectiveness of antibiotic stewardship interventions in reducing the rate of colonization and infections due to antibiotic resistant bacteria and Clostridium difficile in hospital patients a systematic
Effectiveness of antibiotic stewardship interventions in reducing the rate of colonization and infections due to antibiotic resistant bacteria and Clostridium difficile in hospital patients a systematic
Management of Skin and Soft-Tissue Infection
 Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
The Nevada Adult Outpatient Empiric Prescribing Guidelines (2017)
 The Nevada Adult Outpatient Empiric Prescribing Guidelines (2017) Background These empiric prescriber guidelines were produced by the AntiMicrobial Stewardship Summit (AMSS) series led by the University
The Nevada Adult Outpatient Empiric Prescribing Guidelines (2017) Background These empiric prescriber guidelines were produced by the AntiMicrobial Stewardship Summit (AMSS) series led by the University
POTENTIAL STRUCTURE INDICATORS FOR EVALUATING ANTIMICROBIAL STEWARDSHIP PROGRAMMES IN EUROPEAN HOSPITALS
 POTENTIAL STRUCTURE INDICATORS FOR EVALUATING ANTIMICROBIAL STEWARDSHIP PROGRAMMES IN EUROPEAN HOSPITALS Dirk VOGELAERS Department of General Internal Medicine, Infectious Diseases and Psychosomatic Medicine
POTENTIAL STRUCTURE INDICATORS FOR EVALUATING ANTIMICROBIAL STEWARDSHIP PROGRAMMES IN EUROPEAN HOSPITALS Dirk VOGELAERS Department of General Internal Medicine, Infectious Diseases and Psychosomatic Medicine
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form
 Last Updated: Version 3.2a NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Performance Measure Identifier: Measure Information Form Organization Set Measure ID#
Last Updated: Version 3.2a NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Performance Measure Identifier: Measure Information Form Organization Set Measure ID#
Update on CDC Antibiotic Stewardship Activities
 National Center for Emerging and Zoonotic Infectious Diseases Update on CDC Antibiotic Stewardship Activities CAPT Lauri Hicks, DO CAPT Arjun Srinivasan, MD Division of Healthcare Quality Promotion National
National Center for Emerging and Zoonotic Infectious Diseases Update on CDC Antibiotic Stewardship Activities CAPT Lauri Hicks, DO CAPT Arjun Srinivasan, MD Division of Healthcare Quality Promotion National
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies
 ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
Antimicrobial Stewardship in the Outpatient Setting. ELAINE LADD, PHARMD, ABAAHP, FAARFM OCTOBER 28th, 2016
 Antimicrobial Stewardship in the Outpatient Setting ELAINE LADD, PHARMD, ABAAHP, FAARFM OCTOBER 28th, 2016 Abbreviations AMS - Antimicrobial Stewardship Program OP - Outpatient OPS - Outpatient Setting
Antimicrobial Stewardship in the Outpatient Setting ELAINE LADD, PHARMD, ABAAHP, FAARFM OCTOBER 28th, 2016 Abbreviations AMS - Antimicrobial Stewardship Program OP - Outpatient OPS - Outpatient Setting
Antibacterial Resistance: Research Efforts. Henry F. Chambers, MD Professor of Medicine University of California San Francisco
 Antibacterial Resistance: Research Efforts Henry F. Chambers, MD Professor of Medicine University of California San Francisco Resistance Resistance Dose-Response Curve Antibiotic Exposure Anti-Resistance
Antibacterial Resistance: Research Efforts Henry F. Chambers, MD Professor of Medicine University of California San Francisco Resistance Resistance Dose-Response Curve Antibiotic Exposure Anti-Resistance
Study population The target population for the model were hospitalised patients with cellulitis.
 Comparison of linezolid with oxacillin or vancomycin in the empiric treatment of cellulitis in US hospitals Vinken A G, Li J Z, Balan D A, Rittenhouse B E, Willke R J, Goodman C Record Status This is a
Comparison of linezolid with oxacillin or vancomycin in the empiric treatment of cellulitis in US hospitals Vinken A G, Li J Z, Balan D A, Rittenhouse B E, Willke R J, Goodman C Record Status This is a
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Antimicrobial prophylaxis. Bs Lưu Hồ Thanh Lâm Bv Nhi Đồng 2
 Antimicrobial prophylaxis Bs Lưu Hồ Thanh Lâm Bv Nhi Đồng 2 Definition The United States Centers for Disease Control and Prevention (CDC) has developed criteria that define surgical site infection (SSI)
Antimicrobial prophylaxis Bs Lưu Hồ Thanh Lâm Bv Nhi Đồng 2 Definition The United States Centers for Disease Control and Prevention (CDC) has developed criteria that define surgical site infection (SSI)
Antimicrobial Stewardship
 Antimicrobial Stewardship Preventing the Spread of Antibiotic Resistance and Improving Patient Care (Adapted from the Centers for Disease Control and Prevention) What is Stewardship? Antimicrobial stewardship
Antimicrobial Stewardship Preventing the Spread of Antibiotic Resistance and Improving Patient Care (Adapted from the Centers for Disease Control and Prevention) What is Stewardship? Antimicrobial stewardship
Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts
 Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts Investigational Team: Diane Brideau-Laughlin BSc(Pharm),
Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts Investigational Team: Diane Brideau-Laughlin BSc(Pharm),
Staphylococcus Aureus
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
Antibiotic Stewardship Beyond Hospital Walls
 Antibiotic Stewardship Beyond Hospital Walls Katie Burenheide Foster, PharmD, MS, BCPS, FCCM Pharmacy Clinical Manager & PGY1 Pharmacy Residency Director OBJECTIVES 1. Review what Antibiotic Stewardship
Antibiotic Stewardship Beyond Hospital Walls Katie Burenheide Foster, PharmD, MS, BCPS, FCCM Pharmacy Clinical Manager & PGY1 Pharmacy Residency Director OBJECTIVES 1. Review what Antibiotic Stewardship
Clinical Policy: Clindamycin (Cleocin) Reference Number: CP.HNMC.08 Effective Date: Last Review Date: Line of Business: Medicaid - HNMC
 Clinical Policy: (Cleocin) Reference Number: CP.HNMC.08 Effective Date: 07.01.17 Last Review Date: 02.18 Line of Business: Medicaid - HNMC Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Cleocin) Reference Number: CP.HNMC.08 Effective Date: 07.01.17 Last Review Date: 02.18 Line of Business: Medicaid - HNMC Revision Log See Important Reminder at the end of this policy
Antimicrobial Stewardship Programs The Same, but Different. Sara Nausheen, MD Kevin Kern, PharmD
 Antimicrobial Stewardship Programs The Same, but Different Sara Nausheen, MD Kevin Kern, PharmD Antimicrobial Stewardship Programs The Same, but Different Objectives: Outline the overall function of an
Antimicrobial Stewardship Programs The Same, but Different Sara Nausheen, MD Kevin Kern, PharmD Antimicrobial Stewardship Programs The Same, but Different Objectives: Outline the overall function of an
ANTIMICROBIAL STEWARDSHIP: THE ROLE OF THE CLINICIAN SAM GUREVITZ PHARM D, CGP BUTLER UNIVERSITY COLLEGE OF PHARMACY AND HEALTH SCIENCES
 ANTIMICROBIAL STEWARDSHIP: THE ROLE OF THE CLINICIAN SAM GUREVITZ PHARM D, CGP BUTLER UNIVERSITY COLLEGE OF PHARMACY AND HEALTH SCIENCES 1 Crisis: Antibiotic Resistance Success Strategy 2 OBJECTIVES Discuss
ANTIMICROBIAL STEWARDSHIP: THE ROLE OF THE CLINICIAN SAM GUREVITZ PHARM D, CGP BUTLER UNIVERSITY COLLEGE OF PHARMACY AND HEALTH SCIENCES 1 Crisis: Antibiotic Resistance Success Strategy 2 OBJECTIVES Discuss
