A review of neglected tropical diseases: filariasis
|
|
|
- Gary Jason Floyd
- 5 years ago
- Views:
Transcription
1 Asian Pacific Journal of Tropical Medicine (2011) Contents lists available at ScienceDirect Asian Pacific Journal of Tropical Medicine journal homepage: Document heading doi: A review of neglected tropical diseases: filariasis Anish Chandy 1*, Alok Singh Thakur 1, Mukesh Pratap Singh 1, Ashish Manigauha 2 1 School of Pharmacy, Chouksey Engineering College, Bilaspur, Chattishgarh, India 2 NRI College of Pharmacy, Bhopal, India ARTICLE INFO Article history: Received 11 February 2011 Received in revised form 11 April 2011 Accepted 15 June 2011 Available online 20 July 2011 Keywords: Filariasis Parasite Treatment Pathophysiology Drugs Ivermectin ABSTRACT Filariasis is result of parasitic infection caused by three specific kinds of round worm. Lymphatic filariasis is found in under developed region of South America, Central Africa, pacific and Caribbian. It has been found for centuries, with main symptoms as elephant like swelling of the arms, legs and genitals. It is estimate that 120 millions peoples in the world have lymphatic filariasis. The spread of diseases and the challenge encountered in its management are discussed along with a review on drugs against filariasis in this article. Detail on clinical effect of drugs on the infection, safety profile, status in clinical practices and drug resistances are also covered. 1. Introduction Filariasis is a disease caused by parasitic worms called filariae. Filariae are microscopic roundworms that dwell in the blood and tissues of humans. The most important filarial diseases for humans are lymphatic filariases, in which the adult worms are found in the lymphatic system. The lymphatic form of filariasis will be the focus of the site. Lymphatic is also referred to sometimes as elephantiasis. Elephantiasis is actually an extreme clinical feature of filariasis[1]. 2. History of filariasis[2,3] Due to the fact that there is no reliable written record of lymphatic filariasis before the 16th century, ancient historical evidence of lymphatic filariasis cannot be confirmed. It is known that lymphatic filariasis occured in the Nile region, and ancient artifacts suggest that *Corresponding author: Anish Chandy, School of Pharmacy, Chouksey Engineering College, Bilaspur, Chattishgarh, India. Tel: anishpharma@gmail.com the disease may have been found as early as 2000BC. A statue of Pharaoh Mentuhotep 栻 depicts swollen limbs, a characteristic of elephantiasis, which is a symptom of heavy lymphatic filariasis infection. Artifacts from the Nok civilization in West Africa also show scrotal swelling, another characteristic of elephantiasis. The Nok artifacts date much later than the Egyptian artifacts, from about 500AD. The first written account of lymphatic filariasis comes from the ancient Greek and Roman civilizations. In these civilizations, symptoms of leprosy and lymphatic filariasis are differentiated, and leprosy is described as elephantiasis graecorum while lymphatic filariasis as elephantiasis arabum [4]. The first reliable documentation of lymphatic filariasis symptoms is from an exploration of Goa between 1588 and 1592[5]. During this trip, Jan Huygen Linschoten wrote that inhabitants were all born with one of their legs and one foot from the knee downwards as thick as an elephant s leg[4]. More documentations appeared in parts of Africa and Asia soon after. In 1849, William Prout documented a common condition common of lymphatic filariasis called chyluria firstly. This occurs with the passage of lymph in the urine so it appears milky. Such a description is from Prout s book entitled On the nature and treatment of stomach and renal diseases. In 1863, French surgeon
2 582 Anish Chandy et al./asian Pacific Journal of Tropical Medicine (2011) Jean-Nicolas Demarquay recorded the observation of microfilariae in fluid extracted from a hydrocoele (another common symptom of lymphatic filariasis) firstly. Three years later, Otto Henry Wucherer discovered microfilariae in urine in Brazil. However, the connection between these two discoveries was not found until Timothy Lewis noted the occurrence of microfilariae in both blood and urine. Lewis also proposed the association between these microfilariae and elephantiasis firstly. Soon after the discovery of microfilariae, the adult worm was discovered by Joseph Bancroft. This species was later named after Bancroft, and was recognized as Wuchereria Bancroft (W. bancroft). Perhaps the most important discovery related to lymphatic filariasis is found by Patrick Manson in Manson looked for an intermediate host for lymphatic filariasis microfilariae. In 1877, he was finally able to pinpoint the microfilariae in mosquitoes. This discovery was later applied to other tropical diseases such as malaria, and was the first discovery of an arthropod as a vector. However, Manson incorrectly hypothesized that the transmission occurred when the mosquito deposited the filaria in water that then infected humans through ingestion of contaminated water or direct skin penetration. In 1900, George Carmichael Low discovered microfilariae in the proboscis of mosquitoes, and finally pinpointed the true mechanism of transmission, which is attributed to infective bite from a mosquito vector. As researches on lymphatic filariasis continue, the focuses are on prevalence, treatment, prevention, transmission cycles, and even new species. However, current information on lymphatic filariasis is not complete, and further researches are still needed. 3. Epidemiology of disease Due to its alarmingly high prevalence in developing countries, lymphatic filariasis remains one of the most important infectious diseases worldwide. Lymphatic filariasis comprises most of the world s filarial infection. One hundred and twenty million people in at least eighty countries are infected with the parasites associated with lymphatic filariasis. 90% of this infection is caused by W. bancrofti. Most of the remaining cases are due to Brugia malayi (B. malayi). In addition, one billion people (20% of the world s population) are estimated to be at risk for infection[6, 7]. Although 80 countries are known to be endemic areas, about 70% of infected cases are in India, Nigeria[8], Bangladesh and Indonesia. Lymphatic filariasis is endemic in 32 of the world s 38 least developed countries[9-11]. Usually it takes several months to develope filariasis. People that live or stay in endemic tropical or sub-tropical areas for a long time are at the greatest risk. These regions include central Africa, the Nile delta, Madagascar, Turkey, the Middle East, India, Pakistan, Sri Lanka, Myanmar, Thailand, Malaysia, Vietnam, South Korea, Indonesia, the Philipines, Timor, Southern China, Haiti, Dominican Republic, Guyana, French Guinea, and Costal Brazil. And Short-term tourists are at a very low risk[10,11]. 4. Etiology Filariasis in India is caused by the helminths W. bancrofti and B. malayi[13]. Macaques and leaf monkeys are reservoirs in some parts of the world. Acute infection is caused by the microfilariae, which are the larval forms and are transmitted by mosquitoes of various species. Chronic filarial lymphoedema is caused by the adult worms which deposit in, and block the lymphatics. Experimental evidence suggests that unless associated inflammation, simple lymphatic occlusion may not cause lymphoedema. Occluded lymph vessels are greatly prone to attacks of lymphangitis followed by edema. Fibrosis block becomes thick and hard with excrescences in the end, which is known as elephantiasis. Lymphoedema and elephantiasis are common in the lower limb, followed by the genitalia[14], the upper extremity, breast and other areas. The commonest manifestation of filariasis is, however, hydrocele. Lymphatic blockage of and around the cysterna chyli may result in retrograde flow and consequent leakage of chyle through the pelvi-calyceal system (chyluria), the intestines (chylous diarrhoea), the skin-generally around the groin (chylorrhagia), the mediastinum (chylothorax), and the peritoneum (chylous ascites)[1,4]. The male: female ratio is 10:1. This may be because women s mode of dress are more covered. About 50% of the patients are in their 3rd or 4th decades of life, though no age is exempt. Most patients are from the lower socioeconomic groups. The incubation period from mosquito bite to clinical manifestation may be as short as 4 weeks but is generally 8-16 months, or even longer. Attacks last 3-15 days and reoccurrence is common. Asymptomatic infection may occur and may last for life. Acute manifestations of lymphatic filariasis are episodic attacks of lymphadenitis and lymphangitis (fever, pain in the affected part, tender red streaks) along with fever and malaise. Over 90% of cases with chronic manifestations will give a history of acute attacks. Occasionally the adult worms and their associated granulomatous reaction are manifested as lumps in the subcutaneous tissue, breasts or testicles[1, 4, 14]. On the basis of spices of microorganisms, vector etc, it is classified in to four types Lymphatic filariasis Mosquitoes of the genera Aedes, Anopheles, Culex, or Mansonia are the intermediate hosts and vectors of lymphatic filariasis[15-17]. Acute lymphatic filariasis is related to larval molting and adult maturation to fifth-stage larvae. Adult worms are found in lymph nodes and lymphatic vessels distal to the
3 Anish Chandy et al./asian Pacific Journal of Tropical Medicine (2011) nodes. Females measure mm in length and males are 40 mm. The most commonly affected nodes are in the femoral and epitrochlear regions. Abscess formation may occur at the nodes or anywhere along the distal vessel. Infection with Brugia timori (B. timori) appears to result in more abscesses than infection with B. malayi[13] or W. bancrofti[8]. Cellular invasion, with plasma cells, eosinophils, and macrophages, together with hyperplasia of the lymphatic endothelium, occurs with repeated inflammatory episodes. The consequence is lymphatic damage and chronic leakage of protein-rich lymph in the tissues, thickening and verrucous changes of the skin, and chronic streptococcal and fungal infections, which all contribute to the appearance of elephantiasis. B. malayi elephantiasis is more likely to affect the upper and lower limbs, with genital pathology and chyluria being rare Occult filariasis Occult filariasis referes filarial infection in which microfilariae are not observed in the blood but may be found in other body fluids and/or tissues. The occult syndromes are tropical pulmonary eosinophilia (TPE), Dirofilaria immitis (D. immitis) or Dirofilaria repens infection, filarial arthritis, filarial breast abscess, and filarial-associated immunecomplex glomerulonephritis. TPE most likely results from a hyperresponsiveness to W. bancrofti or B. malayi antigen. Human infection with D. immitis may result in pulmonary lesions of immature Dirofilaria worms in the lung periphery. If D. immitis larvae lodge in branches of the pulmonary arteries, they can cause pulmonary infarcts Onchocerciasis Microfilariae from the skin are ingested by the Simulium species of blackflies. Chronic onchocerciasis cases are hyporesponsive to parasite antigen with increased eosinophilia, and result in the presence of high levels of serum immunoglobulin E (IgE). Patterns of onchocercal eye disease also are associated with parasite strain differences at the DNA level Loaiasis Mango flies or deerflies of Chrysops transmit loaiasis. Response to Loa loa (L. loa) infection appears to differ between residents and nonresidents in endemic areas. Nonresidents with infection appear to be more prone to symptoms than residents, despite lower levels of microfilaremia. Eosinophil, serum IgE, and antibody levels also are higher in nonresidents with infection[18]. 5. Symptoms Symptoms of lymphatic filariasis can be divided into asymptomatic, chronic, and acute manifestations: At least half of all patients with lymphatic filariasis appear clinically asymptomatic. This asymptomatic presentation exists despite the presence of microfilariae in their blood and hidden damage to their lymphatics. The length of this asymptomatic period is directly linked to the quality of the patient s immune response[1, 19]. Acute filariasis is characterized by episodic occurrence of inflammation of the lymph glands (lymphadenitis), inflammation of the lymph channels (lymphangitis) and subsequent swelling of the limbs or scrotum (lymphedema). These symptoms are typically accompanied by pulmonary eosinophilia, fever and malaise. Filariatic fever is often seen with headache and chills, and will usually occur at the same time as lymphangitis. Lymphadenitis and lymphangitis are characteristic of both the W. bancrofti and B. malayi forms[8]. In lymphadenitis, the parasite essentially takes over lymph nodes in the body, causing immune reaction and inflammation. Blockage and stretching of the lymph vessels by the adult worms make it difficult for lymph to flow out of the lymphatics and back into the blood stream. Inflammation of the lymph channels and lymph nodes along with a decreased draining efficiency leads to lymphedema. Lymphatic trunks become very painful and the skin on the arms and legs is covered in red streaks. The distal end of the affected limb becomes swollen during the attack and remains swollen for several days. Usually the swelling is limited to a single limb. Tropical pulmonary eosinophilia is an extreme immune response to filarial infection. It is characterized by high eosinophilia levels, asthma-like symptoms and restrictive lung disease. This manifestation occurs with low frequency in endemic areas. In addition to the concurrent exhibition of these symptoms, a patient may suffer from extreme pain in the genital area and may develop filarial abscesses. These pus-filled nodules swell until rupturing when they discharge bacteria and dead adult worms. 6. Pathogenisis Periodicity refers to the time of day when microfilariae are most prevalent in the blood. This corresponds directly to the feeding habits of the various mosquito species. Most species propagating lymphatic filariasis feed at night with the exception of Aedes polynesiensis, a vector of W. bancrofti. There is no known natural animal reservoir for lymphatic filariasis. W. bancrofti has a curvature of its anterior end and is thinner by comparison to the Brugian microfilaria. The microfilaria of B. malayi is easily identifiable[20]. During a blood meal, an infected mosquito introduces infective larvae onto the skin of a human host. The larvae then enter the host s body through the bite wound, at which point they migrate to the lymphatics and develop to maturity. This can be a slow process, taking between six and twelve
4 584 Anish Chandy et al./asian Pacific Journal of Tropical Medicine (2011) months. Adult filariae can live for upto 15 years. At the lymphatics, sexual reproduction between male and female adult nematodes results in the production of sheathed eggs known as microfilariae. Female filariae can release microfilariae for up to five years and the microfilariae can live for a year and a half. The microfilariae travel through the lymphatic channels into the blood stream where they are again taken up by the mosquito through a blood meal. Within one to two weeks after uptake by the mosquito, the microfilariae lose their sheath, bore through the stomach wall and enter the mosquitos thoracic cavity where they develop into infective third-stage filariform larvae. The filariform larvae migrate to the mosquito s proboscis from which they are deposited during the mosquito s next blood meal. The larvae penetrate the skin of the vertebrate host and the cycle continues. 7. Diagnosis The first step towards developing a diagnosis of lymphatic filariasis is to establish a history of exposure in endemic areas. Laboratory tests can follow this basic clinical procedure[2,2-23]. These tests may include: 1) Basic serology testing of peripheral blood for microfilariae detection, keeping the periodicity of the microfilariae in mind[21]; 2)A skin biopsy can also be performed, but this test is generally reserved for the infection by tissue-dwelling nematodes (Onchocerca volvulus); 3)Recently, ultrasonography using a 7.5 or 10 MHz probe has helped to locate and visualise the movements of living adult filarial worms of W. bancrofti in the scrotal lymphatics of asymptomatic males with microfilaraemia[22, 24]; 4)New techniques for antigen detection represent the highest quality lab test for diagnosing infection by W. bancrofti. PCR tests are of high specificity and sensitivity, and detect parasite DNA in humans as well as vectors in both bancroftian and brugian filariasis[21]; 5)Lymphoscintigraphy has shown that even in the early, clinically asymptomatic stage of the disease, there are lymphatic abnormalities in the affected limbs of people harboring microfilaria[19]; 6)Immunochromatographic test which are highly sensitive and specific filarial antigen detection assays, are available for the diagnosis of W. bancrofti infection[2]. With this test, the parasite antigens can be detected independent of the microfilariae s periodicity. It is rapid (1-10 minutes), and no such test exists for B. filariasis. 8. Therapy for lymphatic filariasis 8.1. Drugs for filariasis Ivermectin and suramin are extremely potent semi synthetic derivatives of the antinematodal principle obtained from Streptomyces avermitilis. Nematodes develop tonic paralysis when they are exposed to ivermectin or suramin. It acts aspecial type of glutamate gated CI channel only in invertebrates. Such channels are not involved in the motor control of flukes and tape worms, which are unaffected by ivermectin. Potentiation of GABAergic transmission in the worm has been observed. The lack of GABA related actions in man could be due to its low affinity for mammalian GABA receptors and its exclusion from the brain, probably by p- glyco protein mediated efflux at the blood-brain-barrier. Adult dose of ivermectin is mcg/kg/d po., and suramin is 66.7 mg/kg/d[25-28]. In 2010 Turner and coworkers proved the microfilaricidal activity of doxycycline against Onchocerca volvulus(o. volvulus) in area of L. loa co-endemicity[18]. Mebendazole and flubendazole irreversibly blocks the uptake of exogenous glucose by nematodes, leading to glycogen depletion and reduced generation of ATP required for survival. Due to this the parasites die, or are slowly immobilized and cleared from the gut gradually. It does not affect blood glucose levels in humans. Mebendazole is poorly absorbed from the gut, and peak plasma levels are reached in 2 or 4 hours. The drug is excreted in the urine unchanged or as its metabolites. It causes worm death by selectively and irreversibly blocking uptake of glucose and other nutrients in susceptible adult intestine where helminths dwell. Adult dose of mebendazole and flubendazole are 100 mg po. bid for 3 d, second course if patient not cured in three week[3,23,26-28]. Diethylcarbmazine(DEC) has a highly selective effect on the micro filariae. The most important action of DEC appears to be alteration of micro filariae[23], which are readily phagocytosed by tissue fixed monocytes, but not by circulating phagocytes. It also has an effect on the muscular. Activity of the microfilariae and adult worms causing hyperpolarization due to the piperazine moiety so that they are disloged. To decrease risk of adverse effects, low doses (approximately 2-3 mg/kg/d) usually are recommended for the first 3 d of treatment. Higher doses (9 mg/kg/d) are recommended for L. loa from days Concurrent administration of corticosteroids should be considered with DEC treatment to minimize the allergic manifestations secondary to the disintegration of microfilariae, particularly O. volvulus and L. loa infections. To avoid adverse effects, doses for the treatment of onchocerciasis and loaiasis start at 50 mg and are increased slowly in frequency and amount[2]. The precise mechanism of action of albendazole is not properly understood. However, it seems to afford its primary anthelmintic effect by binding to the free 3-tubulin present in the parasite cells, thereby causing a more or less selective inhibition of parasite micotubule polymerization, and inhibition of micotubule-dependent glucose-up-take significantly. Besides, the effective inhibition of parasite b-tubulin usually takes place at rather lower strengths of the drug than those that are normally needed to check and suppress human microtube polymerization. Decreases
5 Anish Chandy et al./asian Pacific Journal of Tropical Medicine (2011) ATP production in worms, causes energy depletion, immobilization and finally death. Adult dose is 400 mg po.[27,29] Surgical treatment Hydrocele is treated by traditional procedures like excision/eversion. Excision of overlying elephantiasis skin is frequently necessary. Thorough cleaning of the skin is recommended along with peri-operative antibiotic cover as the infection rate is excessive. Surgery for lymphoedema of the limb can be classified into two main types:drainage procedures and excisional procedures. Drainage procedures are essentially designed to improve lymph flows by either bypassing the block e.g. lympho venous anastomosis or creating additional lymph channels eg. omental transposition. Excisional procedures are debulking procedures where the extra large limb volume is trimmed. The procedures differ in the site and type of incision, the way of skin cover and the staging of operations. In Homan s procedure the entire circumference of the leg is cleared in 2-4 stages, while other operations have tried to combine the two Thermal treatment The Chinese have devised a new method of treatment of lymphoedema by alternatively heating and cooling the leg in an oven. This method is reported to be very effective though cumbersome. Use of a microwave oven has been found to be better Herbal treatments There are several herbs that have been prescribed by Ayurveda for the treatment of elephantiasis for centuries. The following are some of the herbs reported as having antifilarial activities ie. Vitex negundo L. (roots)[30], Butea monosperma L. (roots and leaves)[30], Ricinus communis L.(leaves)[30], Aegle marmelos Corr. (leaves)[30], Canthium mannii (Rubiaceae)[31], Boerhaavia diffusa L.(whole plant)[32]. 9. Discussion True elephantiasis is the result of a parasitic infection caused by three specific kinds of round worms. The long, threadlike worms block the body s lymphatic system-a network of channels, lymph nodes, and organs that help maintain proper fluid levels in the body by draining lymph from tissues into the bloodstream. This blockage causes fluids to collect in the tissues, which can lead to great swelling, called lymphedema. Limbs can swell so enormously that they resemble an elephant s foreleg in size, texture, and color. This is the severely disfiguring and disabling condition of elephantiasis. There are a few different causes of elephantiasis, but the agents responsible for most of the elephantiasis in the world are filarial worms: white, slender round worms found in most tropical and subtropical places. They are transmitted by particular kinds (species) of mosquitoes, that is, bloodsucking insects. Infection with these worms is called lymphatic filariasis and over a long period of time can cause elephantiasis. Lymphatic filariasis is a disease of underdeveloped regions found in South America, Central Africa, Asia, the Pacific Islands, and the Caribbean. It is a disease that has been present for centuries, as ancient Persian and Indian writings clearly described elephant-like swellings of the arms, legs, and genitals. It is estimated that 120 million people in the world have lymphatic filariasis. The disease appears to be spreading, in spite of decades of research in this area. Other terms for elephantiasis are Barbados leg, elephant leg, morbus herculeus, mal de Cayenne, and myelolymphangioma. Other situations that can lead to elephantiasis are protozoan disease called leishmaniasis, repeated streptococcal infection, the surgical removal of lymph nodes (usually to prevent the spread of cancer) and hereditary birth defect. If this regime of therapy works, which includes elevation, movement and skin care, it is likely to be of benefit in the management of many other important diseases. This includes management of the skin of patients with AIDS, or for the management of breaks in the surface continuity of epithelium that are highly prevalent in the tropics and in metabolic diseases such as diabetes mellitus or in vulnerable groups such as the bedridden elderly. It requires recognition that the grotesque changes that occur in the most severe cases of lymphoedema are not merely a consequence of lymphatic failure alone. There is in all cases a strong component of both venous and epidermal failure, which responds to therapies specifically targeting at the veins and epidermis. Conflict of interest statement We declare that we have no conflict of interest. References [1] Kabatereine NB, Malecela M, Lado M, Zaramba S, Amiel O, Kolaczinski JH. How to (or not to) integrate vertical programmes for the control of major neglected tropical diseases in sub-saharan Africa. PLoS Negl Trop Dis 2010; 4(6): e755. [2] Weil G, Lammie PJ, Weiss N. The ICT filariasis test: A rapid format antigen test for diagnosis of bancrofitian flariasis. Parasitol Today 1997; 13: [3] Andrade LA, Medeiros Z, Pires ML, Pimentel A, Rocha A, Figuerado-Silva J, et al. Comparative efficacy of three different diethylcarbamazine reigmens in lymphatic filariasis. Trans Royal Soc Trop Med Hyg 1995; 89:
6 586 Anish Chandy et al./asian Pacific Journal of Tropical Medicine (2011) [4] Addiss DG. Global elimination of lymphatic filariasis: addressing the public health problem. PLoS Negl Trop Dis 2010; 4(6): e741. [5] Narain JP, Dash AP, Parnell B, Bhattacharya SK, Barua S, Bhatia R, et al. Elimination of neglected tropical diseases in the South- East Asia Region of the World Health Organization. Bull World Health Organ 2010; 88(3): [6] Leite AB, Lima AR, Leite RB, Santos RV, Gonà alves JE, Rocha EM, et al. Assessment of family and neighbors of an individual infected with Wuchereria bancrofti from a non-endemic area in the city of Maceió, Brazil. Braz J Infect Dis 2010; 14(2): [7] Addiss DG, Louis-Charles J, Roberts J, Leconte F, Wendt JM, Milord MD, et al. Feasibility and effectiveness of basic lymphedema management in Leogane, Haiti, an area endemic for Bancroftian filariasis. PLoS Negl Trop Dis 2010; 4(4): e668. [8] Okon OE, Iboh CI, Opara KN. Bancroftian filariasis among the Mbembe people of Cross River state, Nigeria. J Vector Borne Dis 2010; 47(2): [9] Chu BK, Hooper PJ, Bradley MH, McFarland DA, Ottesen EA. The economic benefits resulting from the first 8 years of the Global Programme to Eliminate Lymphatic Filariasis ( ). PLoS Negl Trop Dis 2010; 4(6): e708. [10] Hotez PJ, Ehrenberg JP. Escalating the global fight against neglected tropical diseases through interventions in the Asia Pacific Region. Adv Parasitol 2010; 72C: [11] Utzinger J, Bergquist R, Olveda R, Zhou XN. Important helminth infections in Southeast Asia diversity, potential for control and prospects for elimination. Adv Parasitol 2010; 72C: [12] Sudomo M, Chayabejara S, Duong S, Hernandez L, Wu WP, Bergquist R. Elimination of lymphatic filariasis in Southeast Asia. Adv Parasitol 2010; 72: [13] Edeson JF.The epidemiology and treatment of infection due to Brugia malayi. Bull World Health Organ 1962; 27(4-5): [14] Al-Shaham AA, Sood S. Recurrent furunculosis as a cause of isolated penile lymphedema: a case report. J Med Case Reports 2010; 4: 196. [15] Kaliwal MB, Kumar A, Shanbhag AB, Dash AP, Javali SB. Spatiotemporal variations in adult density, abdominal status & indoor resting pattern of Culex quinquefasciatus Say in Panaji, Goa, India. Indian J Med Res 2010; 131: [16] Barbosa RM, Regis L, Vasconcelos R, Leal WS. Culex mosquitoes (Diptera: Culicidae) egg laying in traps loaded with Bacillus thuringiensis variety israelensis and baited with skatole. J Med Entomol 2010; 47(3): [17] Stoops CA, Gionar YR, Rusmiarto S, Susapto D, Andris H, Elyazar IR, et al. Laboratory and field testing of bednet traps for mosquito (Diptera: Culicidae) sampling in West Java, Indonesia. J Vector Ecol 2010; 35(1): [18] Turner JD, Tendongfor N, Esum M, Johnston KL, Langley RS, Ford L, et al. Macrofilaricidal activity after doxycycline only treatment of Onchocerca volvulus in an area of Loa loa coendemicity: a randomized controlled trial. PLoS Negl Trop Dis 2010; 4(4): 660. [19] Freedman DO, de Almeoda Filho PJ, Besh S. Lymphoscintraphic analysis of lymphatic abnormalities in symptomatic and asymptomatic human filariasis. J Inf Dis 1994; 170: [20] Castro MC, Kanamori S, Kannady K, Mkude S, Killeen GF, Fillinger U. The importance of drains for the larval development of lymphatic filariasis and malaria vectors in Dar es Salaam, United Republic of Tanzania. PLoS Negl Trop Dis 2010; 4(5): e693. [21] McCarthy J. Diagnosis of lymphatic filarial infection. In: Nutman TB. Lymphatic filariasis. London: Imperial College Press; 2000,p [22] Amaral F, Dreyer G, Figueredo-Silva J. Live adult worms detected by ultrasonography in human bancroftian filariasis. Am J Trop Med Hyg 1994; 50: [23] Noroes J, Dreyer G, Santos A, e Noroes J, Cavalcanti A, Samico SC, et al. Assessment of efficacy of diethylcarbamazine on adult Wuchereria bancrofti in vivo. Trans Roy Soc Trop Med 1997; 91: [24] Anitha, K Shenoy RK. Treatment of lymphatic filariasis. Curr Trends Continuing Medical Education 2001: 67(2): [25] Dreyer G, Addiss D, Noroes J, Amaral F, Rocha A, Coutinho A. Ultrasonographic direct assessment of the adulticidal efficacy of repeat high-dose invermectin in bancrofitian filariasis. Trop Med Int Health 1996; 1: [26] Shenoy RK, Suma TK, Rajan K, Kumaraswami V. Prevention of acute adenolymphangitis in brugian filariasis: comparison of the efficacy of ivermectin and diethylcarbamazine, each combined with local treatment of the affected limb. Ann Med Parasitol 1998; 92: [27] Shenoy RK, John A, Babu BS, Suma TK, Kumaraswami V. Two-year follow-up of the microflaraemia of asymptomatic Brugian filariasis, after treatment with two, annual, single doses of invermectin, diethylcarbamazine or albendazole in various combinations. Ann Trop Med Parasitol 2000; 94: [28] El-Shahawi GA, Abdel-Latif M, Saad AH, Bahgat M. Setaria equina: In vivo effect of diethylcarbamazine citrate on microfilariae in albino rats. Exp Parasitol 2010; 126: [29] Simonsen PE, Pedersen EM, Rwegoshora RT, Malecela MN, Derua YA, Magesa SM. Lymphatic filariasis control in Tanzania: effect of repeated mass drug administration with ivermectin and albendazole on infection and transmission. PLoS Negl Trop Dis 2010; 4(6): e696. [30] Sahare KN, Anandharaman V, Meshram VG, Meshram SU, Gajalakshmi D,Goswami K, et al. In vitro effect of four herbal plants on the motility of Brugia malayi microfilariae. Indian J Med Res 2008; 127: [31] Wabo Pone J, Bilong Bilong CF, Mpoame M. In vitro nematicidal activity of extracts of Canthium mannii (Rubiaceae), on different life-cycle stages of Heligmosomoides polygyrus (Nematoda, Heligmosomatidae). J Helminthol 2009; [32] Jain SP, Singh J. Traditional medicinal practice among the tribal people of raigarh (Chattishgarh), India. Ind J Nat Product Resources 2010; 1:
Drug therapy of Filariasis. Dr. Shareef sm Asst. professor pharmacology
 Drug therapy of Filariasis Dr. Shareef sm Asst. professor pharmacology Signs and symptoms Lymphatic filariasis Fever Inguinal or axillary lymphadenopathy Testicular and/or inguinal pain Skin exfoliation
Drug therapy of Filariasis Dr. Shareef sm Asst. professor pharmacology Signs and symptoms Lymphatic filariasis Fever Inguinal or axillary lymphadenopathy Testicular and/or inguinal pain Skin exfoliation
A review of Filariasis
 International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Review Article Volume 5, Issue 2-2019 DOI: http://dx.doi.org/10.22192/ijcrms.2019.05.02.005
International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Review Article Volume 5, Issue 2-2019 DOI: http://dx.doi.org/10.22192/ijcrms.2019.05.02.005
TISSUE NEMATODES MODULE 49.1 INTODUCTION OBJECTIVES 49.2 FILARIASIS. Notes
 MODULE Tissue Nematodes 49 TISSUE NEMATODES 49.1 INTODUCTION Some nematodes cause infection in the tissues and may be found in the blood or lymphatics as well as in the muscle and other advetitious tissue.
MODULE Tissue Nematodes 49 TISSUE NEMATODES 49.1 INTODUCTION Some nematodes cause infection in the tissues and may be found in the blood or lymphatics as well as in the muscle and other advetitious tissue.
M Correia, D Amonkar, P Audi, C Bhat, P Cruz, N Mitta, A Pednekar, P Kurane
 ISPUB.COM The Internet Journal of Surgery Volume 25 Number 2 Filariasis In The Arm A Diagnostic Enigma! M Correia, D Amonkar, P Audi, C Bhat, P Cruz, N Mitta, A Pednekar, P Kurane Citation M Correia, D
ISPUB.COM The Internet Journal of Surgery Volume 25 Number 2 Filariasis In The Arm A Diagnostic Enigma! M Correia, D Amonkar, P Audi, C Bhat, P Cruz, N Mitta, A Pednekar, P Kurane Citation M Correia, D
RECENT TRENDS IN TREATMENT AND MANAGEMENT OF FILARIASIS
 ISSN: 0975-8232 IJPSR (2010), Vol. 1, Issue 8 (Review Article) Received on 26 March, 2010; received in revised form 28 June, 2010; accepted 17 July, 2010 RECENT TRENDS IN TREATMENT AND MANAGEMENT OF FILARIASIS
ISSN: 0975-8232 IJPSR (2010), Vol. 1, Issue 8 (Review Article) Received on 26 March, 2010; received in revised form 28 June, 2010; accepted 17 July, 2010 RECENT TRENDS IN TREATMENT AND MANAGEMENT OF FILARIASIS
Elephantiasis. C h r i s t i a n H e s s. N u t r i t i o n R o n V e r n o n
 Elephantiasis C h r i s t i a n H e s s N u t r i t i o n 1 0 2 0 R o n V e r n o n 11-29-11 Elephantiasis Elephantiasis or Lymphatic Filariasis is defined by The Journal of Veterinary Medicine Series,
Elephantiasis C h r i s t i a n H e s s N u t r i t i o n 1 0 2 0 R o n V e r n o n 11-29-11 Elephantiasis Elephantiasis or Lymphatic Filariasis is defined by The Journal of Veterinary Medicine Series,
BIO 221 Invertebrate Zoology I Spring Ancylostoma caninum. Ancylostoma caninum cuticular larval migrans. Lecture 23
 BIO 221 Invertebrate Zoology I Spring 2010 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 23 Ancylostoma caninum Ancylostoma caninum cuticular larval migrans Order Ascarida
BIO 221 Invertebrate Zoology I Spring 2010 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 23 Ancylostoma caninum Ancylostoma caninum cuticular larval migrans Order Ascarida
Albendazole for the control and elimination of lymphatic filariasis: systematic review
 Tropical Medicine and International Health volume 10 no 9 pp 818 825 september 2005 Albendazole for the control and elimination of lymphatic filariasis: systematic review Julia Critchley 1, David Addiss
Tropical Medicine and International Health volume 10 no 9 pp 818 825 september 2005 Albendazole for the control and elimination of lymphatic filariasis: systematic review Julia Critchley 1, David Addiss
Department of Microbio
 Fila riae National Institutes t of Health Edward Mitre, MD Department of Microbio ology and Immunology Uniformed Services University of the Health Sciences Februar ry 2011 National Institute of llergy
Fila riae National Institutes t of Health Edward Mitre, MD Department of Microbio ology and Immunology Uniformed Services University of the Health Sciences Februar ry 2011 National Institute of llergy
Mosquito-borne Dog Heartworm Disease 1
 ENY-628 Mosquito-borne Dog Heartworm Disease 1 J. K. Nayar and C. Roxanne Rutledge 2 Each year thousands of dogs become disabled or die from lung, heart or circulatory problems caused by heartworm disease.
ENY-628 Mosquito-borne Dog Heartworm Disease 1 J. K. Nayar and C. Roxanne Rutledge 2 Each year thousands of dogs become disabled or die from lung, heart or circulatory problems caused by heartworm disease.
Tissue and Blood Residing Nematodes
 Tissue and Blood Residing Nematodes Filarial worm Trichina worm Lecture 6 Medical Parasitology Course (MLAB 362) Dr. Mohamed A. El-Sakhawy 1 Common Characteristics Biohelminth Need intermediate host Location
Tissue and Blood Residing Nematodes Filarial worm Trichina worm Lecture 6 Medical Parasitology Course (MLAB 362) Dr. Mohamed A. El-Sakhawy 1 Common Characteristics Biohelminth Need intermediate host Location
Drug Discovery: Supporting development of new drugs to treat global parasitic diseases
 Drug Discovery: Supporting development of new drugs to treat global parasitic diseases UC Santa Cruz Bio 117 Feb. 23, 2016 Judy Sakanari Center for Parasitic Diseases UC San Francisco Parasitic Diseases,
Drug Discovery: Supporting development of new drugs to treat global parasitic diseases UC Santa Cruz Bio 117 Feb. 23, 2016 Judy Sakanari Center for Parasitic Diseases UC San Francisco Parasitic Diseases,
WHO/FIU Distr.: Limited English only
 WHO/FIU98.194 Distr.: Limited English only WHO/FIL/98.194 English only This document is not issued to the general public, and all rights are reserved by the World Health Organization (WHO). The document
WHO/FIU98.194 Distr.: Limited English only WHO/FIL/98.194 English only This document is not issued to the general public, and all rights are reserved by the World Health Organization (WHO). The document
Evidence of continued transmission of Wuchereria bancrofti
 Evidence of continued transmission of Wuchereria bancrofti and associated factors despite nine rounds of ivermectin and albendazole mass drug administration in Rufiji district, Tanzania CLARER JONES 1,
Evidence of continued transmission of Wuchereria bancrofti and associated factors despite nine rounds of ivermectin and albendazole mass drug administration in Rufiji district, Tanzania CLARER JONES 1,
 Kraichat.tan@mahidol.ac.th 1 Outline Vector Borne Disease The linkage of CC&VBD VBD Climate Change and VBD Adaptation for risk minimization Adaptation Acknowledgement: data supported from WHO//www.who.org
Kraichat.tan@mahidol.ac.th 1 Outline Vector Borne Disease The linkage of CC&VBD VBD Climate Change and VBD Adaptation for risk minimization Adaptation Acknowledgement: data supported from WHO//www.who.org
Lymphatic Filariasis Elimination Programme
 Lymphatic Filariasis Elimination Programme training module for drug distributors in countries where lymphatic filariasis is not co-endemic with onchocerciasis World Health Organization Part 1. Lymphatic
Lymphatic Filariasis Elimination Programme training module for drug distributors in countries where lymphatic filariasis is not co-endemic with onchocerciasis World Health Organization Part 1. Lymphatic
THE CONTROL AND SURVEILLANCE OF FILARIASIS IN HAINAN PROVINCE, CHINA
 FILARIASIS IN HAINAN, PR CHINA THE CONTROL AND SURVEILLANCE OF FILARIASIS IN HAINAN PROVINCE, CHINA Hu Xi-min, Wang Shan-qing, Huang Jie-min, Lin Shaoxiong, Tong Chongjin, Li Shanwen and Zhen Wen Hainan
FILARIASIS IN HAINAN, PR CHINA THE CONTROL AND SURVEILLANCE OF FILARIASIS IN HAINAN PROVINCE, CHINA Hu Xi-min, Wang Shan-qing, Huang Jie-min, Lin Shaoxiong, Tong Chongjin, Li Shanwen and Zhen Wen Hainan
BIO Parasitology Spring Trichostrongylines. Lecture 20. Hairworms in Horses. Stephen M. Shuster Northern Arizona University
 BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 20 Trichostrongylines Hairworms in Horses Eggs hatch when eaten by the horse. Larvae
BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 20 Trichostrongylines Hairworms in Horses Eggs hatch when eaten by the horse. Larvae
What causes heartworm disease?
 Heartworm Disease: What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs and cats. It is caused by a blood-borne parasite called Dirofilaria
Heartworm Disease: What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs and cats. It is caused by a blood-borne parasite called Dirofilaria
Aquaculture and human health
 Aquaculture and human health Jimmy Turnbull Institute of Aquaculture University of Stirling Scotland UK 1 Introduction zoonosis The transmission of a disease from an animal or nonhuman species to humans.
Aquaculture and human health Jimmy Turnbull Institute of Aquaculture University of Stirling Scotland UK 1 Introduction zoonosis The transmission of a disease from an animal or nonhuman species to humans.
HOOKWORM FAQ SHEET (rev ) Adapted from the CDC Fact Sheet
 HOOKWORM FAQ SHEET (rev 3-1-10) Adapted from the CDC Fact Sheet Hookworm Infection FAQ Sheet Contents What is hookworm? Where are hookworms commonly found? How do I get a hookworm infection? Who is at
HOOKWORM FAQ SHEET (rev 3-1-10) Adapted from the CDC Fact Sheet Hookworm Infection FAQ Sheet Contents What is hookworm? Where are hookworms commonly found? How do I get a hookworm infection? Who is at
Module 1. Introduction to Targeted Neglected Tropical Diseases (NTDs)
 TARGETED FOR CONTROL OR Module 1. Introduction to Targeted Neglected Tropical Diseases (NTDs) Overview Road map to NTDs targeted for Preventive Chemotherapy (PC) Disease specific epidemiology and control
TARGETED FOR CONTROL OR Module 1. Introduction to Targeted Neglected Tropical Diseases (NTDs) Overview Road map to NTDs targeted for Preventive Chemotherapy (PC) Disease specific epidemiology and control
Feline and Canine Internal Parasites
 Feline and Canine Internal Parasites Internal parasites are a very common problem among dogs. Almost all puppies are already infected with roundworm when still in the uterus, or get the infection immediately
Feline and Canine Internal Parasites Internal parasites are a very common problem among dogs. Almost all puppies are already infected with roundworm when still in the uterus, or get the infection immediately
Schistosoma mansoni, S. japonicum, S. haematobium
 Schistosoma mansoni, S. japonicum, S. haematobium The Organisms More than 200 million people are infected worldwide with Schistosoma species. The adult worms are long and slender (males are 6 12 mm in
Schistosoma mansoni, S. japonicum, S. haematobium The Organisms More than 200 million people are infected worldwide with Schistosoma species. The adult worms are long and slender (males are 6 12 mm in
Peter J. Weina, PhD, MD, FACP, FIDSA Colonel, Medical Corps, US Army Deputy Commander, WRAIR
 Peter J. Weina, PhD, MD, FACP, FIDSA Colonel, Medical Corps, US Army Deputy Commander, WRAIR Patrick Manson -Born Scotland, worked in China for 23 yrs - Pioneer in tropical medicine - Posted to Formosa
Peter J. Weina, PhD, MD, FACP, FIDSA Colonel, Medical Corps, US Army Deputy Commander, WRAIR Patrick Manson -Born Scotland, worked in China for 23 yrs - Pioneer in tropical medicine - Posted to Formosa
ECHINOCOCCOSIS. By Dr. Ameer kadhim Hussein. M.B.Ch.B. FICMS (Community Medicine).
 ECHINOCOCCOSIS By Dr. Ameer kadhim Hussein. M.B.Ch.B. FICMS (Community Medicine). INTRODUCTION Species under genus Echinococcus are small tapeworms of carnivores with larval stages known as hydatids proliferating
ECHINOCOCCOSIS By Dr. Ameer kadhim Hussein. M.B.Ch.B. FICMS (Community Medicine). INTRODUCTION Species under genus Echinococcus are small tapeworms of carnivores with larval stages known as hydatids proliferating
Cases and Developments of Filariasis Disease and Its Caused in Indonesia. Mettison Markus Silitonga* Doli Situmeang*
 Cases and Developments of Filariasis Disease and Its Caused in Indonesia Mettison Markus Silitonga* Doli Situmeang* * Faculty of Science Universitas Advent Indonesia e-mail: mettison@gmail.com Abstract
Cases and Developments of Filariasis Disease and Its Caused in Indonesia Mettison Markus Silitonga* Doli Situmeang* * Faculty of Science Universitas Advent Indonesia e-mail: mettison@gmail.com Abstract
CANINE HEARTWORM DISEASE
 ! CANINE HEARTWORM DISEASE What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs. It is caused by a blood-borne parasite called Dirofilaria
! CANINE HEARTWORM DISEASE What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs. It is caused by a blood-borne parasite called Dirofilaria
Antihelminthic Trematodes (flukes): Cestodes (tapeworms): Nematodes (roundworms, pinworm, whipworms and hookworms):
 Antihelminthic Drugs used to treat parasitic worm infections: helminthic infections Unlike protozoa, helminthes are large and have complex cellular structures It is very important to identify the causative
Antihelminthic Drugs used to treat parasitic worm infections: helminthic infections Unlike protozoa, helminthes are large and have complex cellular structures It is very important to identify the causative
Onchocerciasis & Lymphatic Filariasis Global Health & Disasters Course UCHSC
 Onchocerciasis & Lymphatic Filariasis Global Health & Disasters Course UCHSC Paul Pottinger, MD, DTM&H University of Washington November 2012 Tissue Nematodes: Goals Refresh your understanding of important
Onchocerciasis & Lymphatic Filariasis Global Health & Disasters Course UCHSC Paul Pottinger, MD, DTM&H University of Washington November 2012 Tissue Nematodes: Goals Refresh your understanding of important
WUCHERERIA BANCROFTI ANTIGENAEMIA AMONG SCHOOL CHILDREN:
 KWAME NKRUMAH UNIVERSITY OF SCIENCE AND TECHNOLOGY, KUMASI COLLEGE OF HEALTH SCIENCES SCHOOL OF MEDICAL SCIENCES, DEPARTMENT OF CLINICAL MICROBIOLOGY WUCHERERIA BANCROFTI ANTIGENAEMIA AMONG SCHOOL CHILDREN:
KWAME NKRUMAH UNIVERSITY OF SCIENCE AND TECHNOLOGY, KUMASI COLLEGE OF HEALTH SCIENCES SCHOOL OF MEDICAL SCIENCES, DEPARTMENT OF CLINICAL MICROBIOLOGY WUCHERERIA BANCROFTI ANTIGENAEMIA AMONG SCHOOL CHILDREN:
Biology and Control of Insects and Rodents Workshop Vector Borne Diseases of Public Health Importance
 Vector-Borne Diseases of Public Health Importance Rudy Bueno, Jr., Ph.D. Director Components in the Disease Transmission Cycle Pathogen Agent that is responsible for disease Vector An arthropod that transmits
Vector-Borne Diseases of Public Health Importance Rudy Bueno, Jr., Ph.D. Director Components in the Disease Transmission Cycle Pathogen Agent that is responsible for disease Vector An arthropod that transmits
Management And Treatment Of Tropical Diseases By B. G. Maegraith
 Management And Treatment Of Tropical Diseases By B. G. Maegraith If you are searching for a ebook Management and Treatment of Tropical Diseases by B. G. Maegraith in pdf form, then you have come on to
Management And Treatment Of Tropical Diseases By B. G. Maegraith If you are searching for a ebook Management and Treatment of Tropical Diseases by B. G. Maegraith in pdf form, then you have come on to
Mosquito Control Matters
 Mosquito Control Matters Community Presentation: FIGHT THE BITE Mosquitoes and West Nile Virus Prevention Luz Maria Robles Public Information Officer Sacramento Yolo Mosquito & Vector Control District
Mosquito Control Matters Community Presentation: FIGHT THE BITE Mosquitoes and West Nile Virus Prevention Luz Maria Robles Public Information Officer Sacramento Yolo Mosquito & Vector Control District
Helminth Infections. Pinworms
 Helminth Infections Pinworms Helminths Worm classified as a parasite Contaminate food, water, air, feces, pets, wild animals, toilet seats and door handles Prevention: Frequent hand washing Frequent cleaning
Helminth Infections Pinworms Helminths Worm classified as a parasite Contaminate food, water, air, feces, pets, wild animals, toilet seats and door handles Prevention: Frequent hand washing Frequent cleaning
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan. Associate Consultant Infectious Disease Centre, PMH
 Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
Canine Anaplasmosis Anaplasma phagocytophilum Anaplasma platys
 Canine Anaplasmosis Anaplasma phagocytophilum Anaplasma platys It takes just hours for an infected tick to transmit Anaplasma organisms to a dog. What is canine anaplasmosis? Canine anaplasmosis is a disease
Canine Anaplasmosis Anaplasma phagocytophilum Anaplasma platys It takes just hours for an infected tick to transmit Anaplasma organisms to a dog. What is canine anaplasmosis? Canine anaplasmosis is a disease
Heartworm Disease in Dogs
 Kingsbrook Animal Hospital 5322 New Design Road, Frederick, MD, 21703 Phone: (301) 631-6900 Website: KingsbrookVet.com What causes heartworm disease? Heartworm Disease in Dogs Heartworm disease or dirofilariasis
Kingsbrook Animal Hospital 5322 New Design Road, Frederick, MD, 21703 Phone: (301) 631-6900 Website: KingsbrookVet.com What causes heartworm disease? Heartworm Disease in Dogs Heartworm disease or dirofilariasis
Hydatid Cyst Dr. Nora L. El-Tantawy
 Hydatid Cyst Dr. Nora L. El-Tantawy Ass. Prof. of Parasitology Faculty of Medicine, Mansoura university, Egypt Echinococcus granulosus Geographical Distribution: cosmopolitan especially in sheep raising
Hydatid Cyst Dr. Nora L. El-Tantawy Ass. Prof. of Parasitology Faculty of Medicine, Mansoura university, Egypt Echinococcus granulosus Geographical Distribution: cosmopolitan especially in sheep raising
Symptoms of cellulitis (n=396) %
 Cellulitis and lymphoedema Vaughan Keeley May 2012 What is cellulitis? - also called erysipelas, acute inflammatory episodes etc. - bacterial infection of skin + subcutaneous tissues - more common in people
Cellulitis and lymphoedema Vaughan Keeley May 2012 What is cellulitis? - also called erysipelas, acute inflammatory episodes etc. - bacterial infection of skin + subcutaneous tissues - more common in people
Update of Oncho Program Status. Kofi Marfo
 Update of Oncho Program Status Kofi Marfo Presentation Outline Introduction Progress of Activities Achievements Challenges Way Forward NTDs A group of about 17 infectious diseases which affect over a billion
Update of Oncho Program Status Kofi Marfo Presentation Outline Introduction Progress of Activities Achievements Challenges Way Forward NTDs A group of about 17 infectious diseases which affect over a billion
General introduction
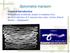 Spirometra mansoni General introduction Distributed worldwide, mainly in southeast Asia. Larval infection of S. mansoni may cause serious clinical disease ---Sparganosis Morphology Adult worm measures
Spirometra mansoni General introduction Distributed worldwide, mainly in southeast Asia. Larval infection of S. mansoni may cause serious clinical disease ---Sparganosis Morphology Adult worm measures
HEARTWORM DISEASE AND THE DAMAGE DONE
 HEARTWORM DISEASE AND THE DAMAGE DONE Stephen Jones, DVM There are now more months of the year where environmental conditions favor mosquito survival and reproduction. Warmer temperatures Indoor environments
HEARTWORM DISEASE AND THE DAMAGE DONE Stephen Jones, DVM There are now more months of the year where environmental conditions favor mosquito survival and reproduction. Warmer temperatures Indoor environments
From macrocyclic lactones back to tetracyclines: new targets for the antiparasitic treatment in animals and humans
 From macrocyclic lactones back to tetracyclines: new targets for the antiparasitic treatment in animals and humans Claudio Genchi Ordinario di Malattie Parassitarie Università degli Studi di Milano Medicinal
From macrocyclic lactones back to tetracyclines: new targets for the antiparasitic treatment in animals and humans Claudio Genchi Ordinario di Malattie Parassitarie Università degli Studi di Milano Medicinal
Israel Journal of Entomology Vol. XXIII(1989) pp
 Israel Journal of Entomology Vol. XXIII(1989) pp. 51-57 THE PROSPECT OF BACILLUS THURINGIENSIS VAR. ISRAELENSIS AND BACILLUS SPHAERICUS IN MOSQUITO CONTROL IN THAILAND SOMSAK PANTUWATANA Department of
Israel Journal of Entomology Vol. XXIII(1989) pp. 51-57 THE PROSPECT OF BACILLUS THURINGIENSIS VAR. ISRAELENSIS AND BACILLUS SPHAERICUS IN MOSQUITO CONTROL IN THAILAND SOMSAK PANTUWATANA Department of
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 A randomized clinical trial comparing single- and multi-dose combination therapy with diethylcarbamazine and
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 A randomized clinical trial comparing single- and multi-dose combination therapy with diethylcarbamazine and
LYMPHATIC FILARIASIS WORLD HEALTH ORGANIZATION GLOBAL PROGRAMME TO ELIMINATE LYMPHATIC FILARIASIS. A HanDbook for national elimination programmes
 WORLD HEALTH ORGANIZATION GLOBAL PROGRAMME TO ELIMINATE LYMPHATIC FILARIASIS Lymphatic filariasis: PRACTICAL ENTOMOLOGY LYMPHATIC FILARIASIS A HanDbook for national elimination programmes WORLD HEALTH
WORLD HEALTH ORGANIZATION GLOBAL PROGRAMME TO ELIMINATE LYMPHATIC FILARIASIS Lymphatic filariasis: PRACTICAL ENTOMOLOGY LYMPHATIC FILARIASIS A HanDbook for national elimination programmes WORLD HEALTH
Aquaculture and human health
 Aquaculture and human health Jimmy Turnbull Institute of Aquaculture University of Stirling Scotland UK 1 Introduction zoonosis The transmission of a disease from an animal or nonhuman species to humans.
Aquaculture and human health Jimmy Turnbull Institute of Aquaculture University of Stirling Scotland UK 1 Introduction zoonosis The transmission of a disease from an animal or nonhuman species to humans.
HYDATID CYST DISEASE
 HYDATID CYST DISEASE Hydatid disease, also called hydatidosis or echinococcosis, is a cystforming disease resulting from an infection with the metacestode, or larval form, of parasitic dog tapeworms from
HYDATID CYST DISEASE Hydatid disease, also called hydatidosis or echinococcosis, is a cystforming disease resulting from an infection with the metacestode, or larval form, of parasitic dog tapeworms from
Lymphatic Filariasis: Transmission, Treatment and Elimination. Wilma Stolk
 Lymphatic Filariasis: Transmission, Treatment and Elimination Wilma Stolk Lymphatic Filariasis: Transmission, Treatment and Elimination Lymfatische Filariasis: Transmissie, Behandeling en Eliminatie Proefschrift
Lymphatic Filariasis: Transmission, Treatment and Elimination Wilma Stolk Lymphatic Filariasis: Transmission, Treatment and Elimination Lymfatische Filariasis: Transmissie, Behandeling en Eliminatie Proefschrift
The Effect of Compliance on the Impact of Mass Drug Administration for Elimination of Lymphatic Filariasis in Egypt
 Am. J. Trop. Med. Hyg., 77(6), 2007, pp. 1069 1073 Copyright 2007 by The American Society of Tropical Medicine and Hygiene The Effect of Compliance on the Impact of Mass Drug Administration for Elimination
Am. J. Trop. Med. Hyg., 77(6), 2007, pp. 1069 1073 Copyright 2007 by The American Society of Tropical Medicine and Hygiene The Effect of Compliance on the Impact of Mass Drug Administration for Elimination
Hydatid Disease. Overview
 Hydatid Disease Overview Hydatid disease in man is caused principally by infection with the larval stage of the dog tapeworm Echinococcus granulosus. It is an important pathogenic zoonotic parasitic infection
Hydatid Disease Overview Hydatid disease in man is caused principally by infection with the larval stage of the dog tapeworm Echinococcus granulosus. It is an important pathogenic zoonotic parasitic infection
Public Health Problem Related to Mosquito
 Public Health Problem Related to Mosquito Goutam Chandra Ph.D., D.Sc. Professor of Zoology Mosquito, Microbiology and Nanotechnology Research Units Parasitology Laboratory The University of Burdwan West
Public Health Problem Related to Mosquito Goutam Chandra Ph.D., D.Sc. Professor of Zoology Mosquito, Microbiology and Nanotechnology Research Units Parasitology Laboratory The University of Burdwan West
Diurnal variation in microfilaremia in cats experimentally infected with larvae of
 Hayasaki et al., Page 1 Short Communication Diurnal variation in microfilaremia in cats experimentally infected with larvae of Dirofilaria immitis M. Hayasaki a,*, J. Okajima b, K.H. Song a, K. Shiramizu
Hayasaki et al., Page 1 Short Communication Diurnal variation in microfilaremia in cats experimentally infected with larvae of Dirofilaria immitis M. Hayasaki a,*, J. Okajima b, K.H. Song a, K. Shiramizu
Effectiveness of a triple-drug regimen for global elimination of lymphatic filariasis: a modelling study
 Effectiveness of a triple-drug regimen for global elimination of lymphatic filariasis: a modelling study Michael A Irvine, Wilma A Stolk, Morgan E Smith, Swaminathan Subramanian, Brajendra K Singh, Gary
Effectiveness of a triple-drug regimen for global elimination of lymphatic filariasis: a modelling study Michael A Irvine, Wilma A Stolk, Morgan E Smith, Swaminathan Subramanian, Brajendra K Singh, Gary
DEWORMING PROCESS KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE , INDIA
 DEWORMING PROCESS KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE-560008, INDIA Email: sales@srisaiagro.com Www.srisaiagro.com INSTRODUCTION According
DEWORMING PROCESS KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE-560008, INDIA Email: sales@srisaiagro.com Www.srisaiagro.com INSTRODUCTION According
Mosquitoes & Diseases. Maxwell Lea, Jr. DVM State Veterinarian Louisiana Dept. of Agriculture and Forestry Department of Animal Health Services
 Mosquitoes & Diseases Maxwell Lea, Jr. DVM State Veterinarian Louisiana Dept. of Agriculture and Forestry Department of Animal Health Services Canine Heartworm Disease Eastern Equine Encephalomyelitis
Mosquitoes & Diseases Maxwell Lea, Jr. DVM State Veterinarian Louisiana Dept. of Agriculture and Forestry Department of Animal Health Services Canine Heartworm Disease Eastern Equine Encephalomyelitis
Taking your pets abroad
 Taking your pets abroad Your guide to diseases encountered abroad Produced by the BVA Animal Welfare Foundation www.bva-awf.org.uk BVA AWF is a registered charity (287118) Prevention is better than cure!
Taking your pets abroad Your guide to diseases encountered abroad Produced by the BVA Animal Welfare Foundation www.bva-awf.org.uk BVA AWF is a registered charity (287118) Prevention is better than cure!
Blood protozoan: Plasmodium
 Blood protozoan: Plasmodium Dr. Hala Al Daghistani The causative agent of including Plasmodium vivax P. falciparum P. malariae P. ovale. malaria in humans: four species are associated The Plasmodium spp.
Blood protozoan: Plasmodium Dr. Hala Al Daghistani The causative agent of including Plasmodium vivax P. falciparum P. malariae P. ovale. malaria in humans: four species are associated The Plasmodium spp.
Blood protozoan: Plasmodium
 Blood protozoan: Plasmodium The causative agent of including Plasmodium vivax P. falciparum P. malariae P. ovale. malaria in humans:four species are associated The Plasmodium spp. life cycle can be divided
Blood protozoan: Plasmodium The causative agent of including Plasmodium vivax P. falciparum P. malariae P. ovale. malaria in humans:four species are associated The Plasmodium spp. life cycle can be divided
Efficacies of fenbendazole and albendazole in the treatment of commercial turkeys artificially infected with Ascaridia dissimilis
 Efficacies of fenbendazole and albendazole in the treatment of commercial turkeys artificially infected with Ascaridia dissimilis Jessica Perkins, Thomas Yazwinski, Chris Tucker Abstract The goal of this
Efficacies of fenbendazole and albendazole in the treatment of commercial turkeys artificially infected with Ascaridia dissimilis Jessica Perkins, Thomas Yazwinski, Chris Tucker Abstract The goal of this
UNDERSTANDING HEARTWORMS 4-Pets
 Oklahoma 4-H 4H SMAN 503 UNDERSTANDING HEARTWORMS 4-Pets WHAT IS A HEARTWORM Heartworms are internal parasites that can infect your dog or cat. Parasites live on the inside (internal) or on the outside
Oklahoma 4-H 4H SMAN 503 UNDERSTANDING HEARTWORMS 4-Pets WHAT IS A HEARTWORM Heartworms are internal parasites that can infect your dog or cat. Parasites live on the inside (internal) or on the outside
BITING DENSITY, BEHAVIOR AND AGE DISTRIBUTION OF CULEX QUINQUEFASCIA TUS, SAY IN MYSORE CITY, INDIA
 BITING DENSITY, BEHAVIOR AND AGE DISTRIBUTION OF CULEX QUINQUEFASCIA TUS, SAY IN MYSORE CITY, INDIA N Ninge Gowda and VA Vijayan Department of Studies in Zoology, University of Mysore, Manasa Gangotri,
BITING DENSITY, BEHAVIOR AND AGE DISTRIBUTION OF CULEX QUINQUEFASCIA TUS, SAY IN MYSORE CITY, INDIA N Ninge Gowda and VA Vijayan Department of Studies in Zoology, University of Mysore, Manasa Gangotri,
Heartworm Disease in Dogs
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Heartworm Disease in Dogs Basics OVERVIEW Disease caused by infestation with heartworms
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Heartworm Disease in Dogs Basics OVERVIEW Disease caused by infestation with heartworms
Changing Trends and Issues in Canine and Feline Heartworm Infections
 Changing Trends and Issues in Canine and Feline Heartworm Infections Byron L. Blagburn College of Veterinary Medicine Auburn University Canine and feline heartworm diagnostic, treatment and prevention
Changing Trends and Issues in Canine and Feline Heartworm Infections Byron L. Blagburn College of Veterinary Medicine Auburn University Canine and feline heartworm diagnostic, treatment and prevention
ANIMAL RABIES IN NEPAL AND RACCOON RABIES IN ALBANY COUNTY, NEW YORK
 ANIMAL RABIES IN NEPAL AND RACCOON RABIES IN ALBANY COUNTY, NEW YORK SHANKAR YADAV MPH Report/Capstone Project Presentation 07/19/2012 CHAPTER 1: FIELD EXPERIENCE AT KANSAS STATE UNIVERSITY RABIES LABORATORY
ANIMAL RABIES IN NEPAL AND RACCOON RABIES IN ALBANY COUNTY, NEW YORK SHANKAR YADAV MPH Report/Capstone Project Presentation 07/19/2012 CHAPTER 1: FIELD EXPERIENCE AT KANSAS STATE UNIVERSITY RABIES LABORATORY
Chapter 9. General discussion
 Chapter 9 General discussion Chapter 9 General Discussion Ever since the inception of research into human oesophagostomiasis in northern Ghana and Togo just over two decades ago, Oesophagostomum infection
Chapter 9 General discussion Chapter 9 General Discussion Ever since the inception of research into human oesophagostomiasis in northern Ghana and Togo just over two decades ago, Oesophagostomum infection
HUSK, LUNGWORMS AND CATTLE
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk HUSK, LUNGWORMS AND CATTLE Author : Alastair Hayton Categories : Vets Date : July 20, 2009 Alastair Hayton discusses how best
Vet Times The website for the veterinary profession https://www.vettimes.co.uk HUSK, LUNGWORMS AND CATTLE Author : Alastair Hayton Categories : Vets Date : July 20, 2009 Alastair Hayton discusses how best
Mosquito Reference Document
 INTRODUCTION Insects (class Insecta) are highly diverse and one of the most successful groups of animals. They live in almost every region of the world: at high elevation, in freshwater, in oceans, and
INTRODUCTION Insects (class Insecta) are highly diverse and one of the most successful groups of animals. They live in almost every region of the world: at high elevation, in freshwater, in oceans, and
Summary of the Eighteenth Meeting of the International Task Force for Disease Eradication (II) April 6, 2011
 Summary of the Eighteenth Meeting of the International Task Force for Disease Eradication (II) April 6, 2011 The Eighteenth Meeting of the International Task Force for Disease Eradication (ITFDE) was convened
Summary of the Eighteenth Meeting of the International Task Force for Disease Eradication (II) April 6, 2011 The Eighteenth Meeting of the International Task Force for Disease Eradication (ITFDE) was convened
Breastfeeding Challenges - Mastitis & Breast Abscess -
 CLINICAL PRACTICE GUIDELINE Breastfeeding Challenges - Mastitis & Breast Abscess - SCOPE (Area): Maternity Unit, Emergency Department, Paediatrics SCOPE (Staff): Medical, Midwifery & Nursing DESIRED OUTCOME/OBJECTIVE
CLINICAL PRACTICE GUIDELINE Breastfeeding Challenges - Mastitis & Breast Abscess - SCOPE (Area): Maternity Unit, Emergency Department, Paediatrics SCOPE (Staff): Medical, Midwifery & Nursing DESIRED OUTCOME/OBJECTIVE
MALARIA A disease of the developing world
 MALARIA A disease of the developing world Introduction Malaria is an infectious disease and is found mainly in the world s poorest tropical areas, such as Africa, South America and South East Asia. The
MALARIA A disease of the developing world Introduction Malaria is an infectious disease and is found mainly in the world s poorest tropical areas, such as Africa, South America and South East Asia. The
The Rat Lungworm Lifecycle
 Hawaii Island Rat Lungworm Working Group Daniel K. Inouye College of Pharmacy University of Hawaii, Hilo The Rat Lungworm Lifecycle Rat Lungworm IPM RLWL-3 It is important to understand the lifecycle of
Hawaii Island Rat Lungworm Working Group Daniel K. Inouye College of Pharmacy University of Hawaii, Hilo The Rat Lungworm Lifecycle Rat Lungworm IPM RLWL-3 It is important to understand the lifecycle of
SUMMARY. Mosquitoes are surviving on earth since millions of years. They are the
 SUMMARY Mosquitoes are surviving on earth since millions of years. They are the important carriers of various diseases like malaria, dengue, filaria, Japanese encephalitis, west nile virus and chikun gunia.
SUMMARY Mosquitoes are surviving on earth since millions of years. They are the important carriers of various diseases like malaria, dengue, filaria, Japanese encephalitis, west nile virus and chikun gunia.
Seroprevalence of Dengue in Antenatal and Paediatric Patients - In a Tertiary Care Hospital, Puducherry
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.077
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 06 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.706.077
Introduction to Helminthology
 Introduction to Helminthology HELMINTHES (WORMS) - Characteristics Eukaryotic, multicellular animals that usually have digestive, circulatory, nervous, excretory, and reproductive systems. Worms with bilateral
Introduction to Helminthology HELMINTHES (WORMS) - Characteristics Eukaryotic, multicellular animals that usually have digestive, circulatory, nervous, excretory, and reproductive systems. Worms with bilateral
How to talk to clients about heartworm disease
 Client Communication How to talk to clients about heartworm disease Detecting heartworm infection early generally allows for a faster and more effective response to treatment. Answers to pet owners most
Client Communication How to talk to clients about heartworm disease Detecting heartworm infection early generally allows for a faster and more effective response to treatment. Answers to pet owners most
Intestinal parasitic infections are a serious
 Paediatrica Indonesiana VOLUME 54 March NUMBER 2 Original Article Albendazole alone vs. albendazole and diethylcarbamazine combination therapy for trichuriasis Windya Sari Nasution, Muhammad Ali, Ayodhia
Paediatrica Indonesiana VOLUME 54 March NUMBER 2 Original Article Albendazole alone vs. albendazole and diethylcarbamazine combination therapy for trichuriasis Windya Sari Nasution, Muhammad Ali, Ayodhia
Guard against intestinal worms with Palatable All-wormer
 Guard against intestinal worms with Palatable All-wormer WHIPWORMS HOOKWORMS TAPEWORMS ROUNDWORMS Palatable All-wormer, for superior, flexible protection of dogs and cats. GENTLE ON PETS, TOUGH ON WORMS.
Guard against intestinal worms with Palatable All-wormer WHIPWORMS HOOKWORMS TAPEWORMS ROUNDWORMS Palatable All-wormer, for superior, flexible protection of dogs and cats. GENTLE ON PETS, TOUGH ON WORMS.
Situation update of dengue in the SEA Region, 2010
 Situation update of dengue in the SEA Region, 21 The global situation of Dengue It is estimated that nearly 5 million dengue infections occur annually in the world. Although dengue has a global distribution,
Situation update of dengue in the SEA Region, 21 The global situation of Dengue It is estimated that nearly 5 million dengue infections occur annually in the world. Although dengue has a global distribution,
h e a l t h l i n e ISSN X Volume 1 Issue 1 July-December 2010 Pages 16-20
 h e a l t h l i n e ISSN 2229-337X Volume 1 Issue 1 July-December 2010 Pages 16-20 Original Article Awareness and practice about preventive method against mosquito bite in Gujarat Niraj Pandit 1, Yogesh
h e a l t h l i n e ISSN 2229-337X Volume 1 Issue 1 July-December 2010 Pages 16-20 Original Article Awareness and practice about preventive method against mosquito bite in Gujarat Niraj Pandit 1, Yogesh
Farm Newsletter - February 2017
 Farm Newsletter - February 2017 Lung Worm in Cattle The disease is caused by the worm Dictyocaulus viviparus. Adult worms live in the animal s lungs where they produce eggs which hatch quickly. The first
Farm Newsletter - February 2017 Lung Worm in Cattle The disease is caused by the worm Dictyocaulus viviparus. Adult worms live in the animal s lungs where they produce eggs which hatch quickly. The first
Awareness, knowledge and practices about mosquito borne diseases in patients of tertiary care hospital in Navi Mumbai
 International Journal of Community Medicine and Public Health Wasnik S et al. Int J Community Med Public Health. 2017 Oct;4(10):3673-3677 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original
International Journal of Community Medicine and Public Health Wasnik S et al. Int J Community Med Public Health. 2017 Oct;4(10):3673-3677 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original
WORLD HEATH ORGANIZATION GLOBAL PROGRAMME TO ELIMINATE LYMPHATIC FILARIASIS
 WORLD HEATH ORGANIZATION GLOBAL PROGRAMME TO ELIMINATE LYMPHATIC FILARIASIS NTD-STAG M&E SUB-WORKING GROUP ON DISEASE SPECIFIC INDICATORS MEETING REPORT 2012 LYMPHATIC FILARIASIS THE TASK FORCE FOR GLOBAL
WORLD HEATH ORGANIZATION GLOBAL PROGRAMME TO ELIMINATE LYMPHATIC FILARIASIS NTD-STAG M&E SUB-WORKING GROUP ON DISEASE SPECIFIC INDICATORS MEETING REPORT 2012 LYMPHATIC FILARIASIS THE TASK FORCE FOR GLOBAL
Understanding Epidemics Section 3: Malaria & Modelling
 Understanding Epidemics Section 3: Malaria & Modelling PART B: Biology Contents: Vector and parasite Biology of the malaria parasite Biology of the anopheles mosquito life cycle Vector and parasite Malaria
Understanding Epidemics Section 3: Malaria & Modelling PART B: Biology Contents: Vector and parasite Biology of the malaria parasite Biology of the anopheles mosquito life cycle Vector and parasite Malaria
A:Malaria (Plasmodium species) Plasmodium falciparum causes malignant tertian malaria P. malariae: causes Quartan malaria P. vivax: causes benign
 A:Malaria (Plasmodium species) Plasmodium falciparum causes malignant tertian malaria P. malariae: causes Quartan malaria P. vivax: causes benign tertian malaria P. ovale: causes benign tertian malaria
A:Malaria (Plasmodium species) Plasmodium falciparum causes malignant tertian malaria P. malariae: causes Quartan malaria P. vivax: causes benign tertian malaria P. ovale: causes benign tertian malaria
Feline Immunodeficiency Virus (FIV)
 Virus (FeLV) FIV and FeLV are both viruses within the same family of retroviruses, but they are in different groups within that family: FIV is in one group called lentiviruses these cause lifelong infections
Virus (FeLV) FIV and FeLV are both viruses within the same family of retroviruses, but they are in different groups within that family: FIV is in one group called lentiviruses these cause lifelong infections
Corallopyronin A: a new anti-filarial drug. Kenneth Pfarr Institute for Medical Microbiology, Immunology and Parasitology
 Corallopyronin A: a new anti-filarial drug Kenneth Pfarr Institute for Medical Microbiology, Immunology and Parasitology PEG, Weimar, 17 th October, 2014 Filariasis ~150 million people infected >1.3 billion
Corallopyronin A: a new anti-filarial drug Kenneth Pfarr Institute for Medical Microbiology, Immunology and Parasitology PEG, Weimar, 17 th October, 2014 Filariasis ~150 million people infected >1.3 billion
2. LITERATURE REVIEW 2.1 Lymphatic filariasis Epidemiology Geographical distribution
 2. LITERATURE REVIEW 2.1 Lymphatic filariasis Lymphatic filariasis is an inflammatory parasitic infection of lymphatic vessels caused by the filarial roundworms Wuchereria bancrofti, Brugia malayi, and
2. LITERATURE REVIEW 2.1 Lymphatic filariasis Lymphatic filariasis is an inflammatory parasitic infection of lymphatic vessels caused by the filarial roundworms Wuchereria bancrofti, Brugia malayi, and
Update on Fluoroquinolones. Charles Krasner, M.D. June 16, 2016 Antibiotic Stewardship Program -ECHO
 Update on Fluoroquinolones Charles Krasner, M.D. June 16, 2016 Antibiotic Stewardship Program -ECHO Potential fluoroquinolone side-effects Increased risk, greater than with most other antibiotics, for
Update on Fluoroquinolones Charles Krasner, M.D. June 16, 2016 Antibiotic Stewardship Program -ECHO Potential fluoroquinolone side-effects Increased risk, greater than with most other antibiotics, for
A. Effect upon human culture 1. Control of malaria has contributed to world=s population explosion 2. Africans brought to U.S.
 VI. Malaria A. Effect upon human culture 1. Control of malaria has contributed to world=s population explosion 2. Africans brought to U.S. because they were resistant to malaria & other diseases 3. Many
VI. Malaria A. Effect upon human culture 1. Control of malaria has contributed to world=s population explosion 2. Africans brought to U.S. because they were resistant to malaria & other diseases 3. Many
June, 2004 Journal of Vector Ecology 101
 June, 2004 Journal of Vector Ecology 101 The in vitro effect of albendazole, ivermectin, diethylcarbamazine, and their combinations against infective third-stage larvae of nocturnally subperiodic Brugia
June, 2004 Journal of Vector Ecology 101 The in vitro effect of albendazole, ivermectin, diethylcarbamazine, and their combinations against infective third-stage larvae of nocturnally subperiodic Brugia
BRUCELLOSIS. Morning report 7/11/05 Andy Bomback
 BRUCELLOSIS Morning report 7/11/05 Andy Bomback Also called undulant, Mediterranean, or Mata fever, brucellosis is an acute and chronic infection of the reticuloendothelial system gram negative facultative
BRUCELLOSIS Morning report 7/11/05 Andy Bomback Also called undulant, Mediterranean, or Mata fever, brucellosis is an acute and chronic infection of the reticuloendothelial system gram negative facultative
Vector Control in emergencies
 OBJECTIVE Kenya WASH Cluster Training for Emergencies Oct 2008 3.06 - Vector Control in emergencies To provide practical guidance and an overview of vector control in emergency situations It will introduce
OBJECTIVE Kenya WASH Cluster Training for Emergencies Oct 2008 3.06 - Vector Control in emergencies To provide practical guidance and an overview of vector control in emergency situations It will introduce
Chapter 5: Aquatic Plants, Mosquitoes and Public Health
 Chapter 5: Aquatic Plants, Mosquitoes and Public Health James P. Cuda: University of Florida, Gainesville FL; jcuda@ufl.edu Introduction Approximately 200 species of aquatic plants are classified as weeds
Chapter 5: Aquatic Plants, Mosquitoes and Public Health James P. Cuda: University of Florida, Gainesville FL; jcuda@ufl.edu Introduction Approximately 200 species of aquatic plants are classified as weeds
Rapid Diagnostic Test for pet
 In vitro Diagnostic Rapid Diagnostic Test for pet Canine / Feline Rapid Test offers highly sensitive and specificity for the detection of antigen and antibody from various kinds of easily obtainable specimen.
In vitro Diagnostic Rapid Diagnostic Test for pet Canine / Feline Rapid Test offers highly sensitive and specificity for the detection of antigen and antibody from various kinds of easily obtainable specimen.
Clarer Jones 1*, Billy Ngasala 1,2, Yahya A. Derua 3, Donath Tarimo 1, Lisa Reimer 4, Moses Bockarie 5 and Mwelecele N. Malecela 6
 Jones et al. Parasites & Vectors (2018) 11:588 https://doi.org/10.1186/s13071-018-3156-2 RESEARCH Open Access Lymphatic filariasis transmission in Rufiji District, southeastern Tanzania: infection status
Jones et al. Parasites & Vectors (2018) 11:588 https://doi.org/10.1186/s13071-018-3156-2 RESEARCH Open Access Lymphatic filariasis transmission in Rufiji District, southeastern Tanzania: infection status
Equine Diseases. Dr. Kashif Ishaq. Disease Management
 Equine Diseases Dr. Kashif Ishaq Disease Management Prevention is the singularly most important aspect Vaccinate regularly Keep horse areas cleaned up and sanitized Proper feeds and feeding management
Equine Diseases Dr. Kashif Ishaq Disease Management Prevention is the singularly most important aspect Vaccinate regularly Keep horse areas cleaned up and sanitized Proper feeds and feeding management
Fight The Bite. Mosquito Control on Woodlots. Introduction and Overview. History. Vector. Mosquitoes and Flies
 Fight The Bite Mosquito Control on Woodlots Introduction and Overview Josh Jacobson Assistant Biologist Theresa Micallef Overview District Background/History Mosquito Biology What We Do West Nile Virus
Fight The Bite Mosquito Control on Woodlots Introduction and Overview Josh Jacobson Assistant Biologist Theresa Micallef Overview District Background/History Mosquito Biology What We Do West Nile Virus
Rabbits, companion animals and arthropod-borne diseases
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Rabbits, companion animals and arthropod-borne diseases Author : Glen Cousquer Categories : RVNs Date : December 1, 2013 Glen
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Rabbits, companion animals and arthropod-borne diseases Author : Glen Cousquer Categories : RVNs Date : December 1, 2013 Glen
