Comparison of subsequent infection in. nasal carriers between ST72 communitygenotype and hospital genotypes: a retrospective cohort study
|
|
|
- Hortense Goodman
- 5 years ago
- Views:
Transcription
1 Park et al. Antimicrobial Resistance and Infection Control (2017) 6:60 DOI /s RESEARCH Comparison of subsequent infection in methicillin-resistant Staphylococcus aureus nasal carriers between ST72 communitygenotype and hospital genotypes: a retrospective cohort study Open Access So Yeon Park 1,4, Doo Ryeon Chung 1,2,3*, Yu Ri Kang 1,3, So Hyun Kim 1,3, Sun Young Cho 1,2, Young Eun Ha 1, Cheol-In Kang 1, Kyong Ran Peck 1 and Jae-Hoon Song 1,3 Abstract Background: Carriage of methicillin-resistant Staphylococcus aureus (MRSA) is an important risk factor of subsequent infection. The purpose of our study was to compare the rates of subsequent infection among newly-admitted patients carrying MRSA between community-genotype and hospital-genotypes Methods: In this retrospective cohort study, we compared the rates of subsequent MRSA infection, time to subsequent infection and mortality in the following 6 months between the community-genotype ST72 MRSA cohort and the hospital-genotypes ST5 / ST239 MRSA cohort. Results: We identified 198 patients carrying ST72 and 156 patients carrying ST5 or ST239. There was no difference in the rates of subsequent infection between ST72 cohort and ST5 / ST239 cohort (13.1% vs. 12.8%; P = 0.931). The median time to development of subsequent infection was not significantly different (27 days vs. 88 days; P = ). The Kaplan-Meier method showed no difference in the cumulative rate of being free of subsequent infection between the cohorts (P = ). Overall mortality rates at 6 months did not differ (1.5% vs. 1.9%; P =1.000) Conclusions: We found no evidence that rates of subsequent MRSA infection were different between newly-admitted patients carrying community-genotype ST72 MRSA and those whom carrying hospital-genotypes ST5 or ST239 MRSA. Keywords: Genotype, Kaplan-meier estimate, Methicillin-resistant Staphylococcus aureus, Cohort study, Carrier state Background Methicillin-resistant Staphylococcus aureus (MRSA) infections have imposed a high burden on healthcare resources as well as significant morbidity and mortality, and a recent emergence of community-associated MRSA (CA-MRSA) worldwide has added another concern. MRSA carriage has been identified as a strong risk factor for subsequent infection [1, 2]. Approximately 11% - * Correspondence: iddrchung@gmail.com 1 Division of Infectious Diseases, Department of Internal Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, 81 Irwon-ro, Gangnam-gu, Seoul 06351, Republic of Korea 2 Center for Infection Prevention and Control, Samsung Medical Center, Seoul, South Korea Full list of author information is available at the end of the article 25% of patients who newly acquired MRSA were reported to develop subsequent infection during hospitalization [3, 4]. Although several CA-MRSA clones have emerged as important pathogens both in the community and the hospitals worldwide [5 7] and have shown different characteristics in the pattern of colonization and infection from the hospital-genotype MRSA clones [7, 8], there has been no study comparing the rates of subsequent MRSA infection in hospitalized patients carrying MRSA between the communitygenotype and hospital-genotype strains. In Korea, dominant MRSA clones endemic in the hospitals have been sequence type 5 (ST5) and ST239 clones, while ST72 clone has emerged in the community The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
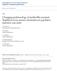
2 Park et al. Antimicrobial Resistance and Infection Control (2017) 6:60 Page 2 of 7 and has spread into the hospitals [9 11]. A recent single center study from Korea showed that the most frequent genotype in newly-admitted patients carrying MRSA was ST72, followed by ST5 and ST239 [12]. In this study, we compared the rates of subsequent MRSA infection among newly-detected hospitalized patients carrying MRSA between the community-genotype and the hospital-genotype cohort. Methods Study design and study participants A retrospective cohort study was performed at Samsung Medical Center (Seoul, Republic of Korea), a universityaffiliated tertiary care hospital with 1983 patient beds. We identified patients who were newly-detected MRSA nasal carriers between January 1, 2007 and March 31, 2010 from the previous study [12]. MRSA nasal screening was performed in selected newly-admitted patients according to the active surveillance policy for infection prevention purpose of the hospital. The indications for screening included the referral patients from the other hospitals or the chronic care facilities, the patients scheduled for operations in the departments of orthopedic surgery, neurosurgery, thoracic surgery and general surgery, the patients receiving hemodialysis or peritoneal dialysis, MRSA isolation from clinical specimens and carriage of vancomycinresistant Enterococcus (VRE). Conventional culture methods were used for screening and confirmation of nasal carrier status of MRSA. The MRSA isolates were collected and stocked in the Asian Bacterial Bank (Seoul, Republic of Korea). Patients were excluded from the study if nasal MRSA carriage had been already known prior to the study period. The patients carrying MRSA belonging to the sequence types other than ST72, ST5 and ST239 were excluded. We also excluded the patients who could not be followed up at least 6 months and had not developed subsequent MRSA infection until that time point (Fig. 1). Cohort 1 included the patients carrying MRSA with community-genotype, ST72, and cohort 2 included those who carried MRSA with hospital-genotypes, ST5 or ST239. If the patients developed MRSA infection multiple times, the first episode was only included in the analysis. This study was approved by the Institute Review Board of Samsung Medical Center. Data collection Demographic and clinical characteristics, laboratory data, and outcome data were collected from the electronic medical records. The McCabe classification was used to categorize the severity of the underlying medical condition as non-fatal, ultimately fatal, or rapidly fatal [13]. Outcome variables included the rates of subsequent MRSA infection within six months after new detection of MRSA nasal colonization, overall mortality rates at six months, and time to development of subsequent MRSA infection. The type of infections was also described. Microbiological and molecular characterization The Vitek 2 automated system (biomerieux, Marcy l Etoile, France) was used for microbiological identification and antimicrobial susceptibility testing. The MICs Fig. 1 Flow chart summarizing identification of study cohorts
3 Park et al. Antimicrobial Resistance and Infection Control (2017) 6:60 Page 3 of 7 were determined according to the standards established by the Clinical and Laboratory Standards Institute (CLSI) [14]. Multilocus sequence typing (MLST) was carried out using PCR amplification and sequencing of seven housekeeping genes (arcc, aroe, glpf, gmk, pta, tpi, and yqil), as previously described [15]. The allelic profiles and sequence types (STs) were assigned according to the MLST web site (http//saureus.mlst.net/). Statistical analysis All tests of significance were two-tailed. P-values <0.05 were considered statistically significant. Categorical variables were compared between the groups using Chi-square test or Fisher s exact test. Continuous variables were compared using the Mann Whitney U test. Multivariate logistic regression analysis was used to determine the risk factors of subsequent MRSA infection. Stepwise model comparison was used to determine the best model using the PASW version 18.0 (SPSS Inc., Chicago, IL, USA). Times to development of subsequent MRSA infection during the follow-up period were calculated by the Kaplan-Meier method and compared between the cohorts using the log-rank test. Stata version 11.2 (StataCorp, College Station, TX, USA) was used for this analysis. Results Study population We identified 1118 patients with nasal MRSA colonization during the study period. Among those patients, 592 known MRSA carriers revisiting the hospital were excluded. The patients carrying MRSA strains belonging to ST72, ST5 or ST239 who were followed up for at least 6 months were included in this study. A total of 354 patients carrying MRSA were included (Fig. 1). Among those MRSA isolates, the most frequent sequence type was ST72 (55.9%). ST5 and ST239 accounted for 23.8% and 5.4%, respectively. The most frequent reasons for nasal MRSA screening were transfer from other hospital (36.2%) and pre-operative screening (33.6%). Other reasons included MRSA isolation from clinical specimens (9.0%), carriage of VRE (6.5%), and undergoing hemodialysis or continuous ambulatory peritoneal dialysis (CAPD) (4.2%). Among the MRSA isolates from nasal carriers who were screened for preoperative screening, ST72 (67.2%) was more frequent than ST5 or ST239 (Table 1). Comparison of characteristics of MRSA carriers between ST72 cohort and ST5 / ST239 cohort The demographic and clinical characteristics of MRSA nasal carriers were compared between ST72 cohort and ST5 / ST239 cohort (Table 1). The most frequent comorbidity in ST72 cohort was solid tumor (24.2%), followed by cardiovascular disease, diabetes mellitus, liver disease, neurologic disease, and chronic kidney disease. Solid tumor was more frequent in ST72 cohort than in ST5 / ST239 cohort, whereas hematologic malignancy was more frequent in ST5 / ST239 cohort. Subsequent MRSA infection The median duration of follow-up after detection of nasal MRSA carriage was 1058 days (range days) in ST72 cohort and days (range days) in ST5 / ST239 cohort (P = 0.555). Among MRSA carriers of ST72 cohort, 13.1% developed subsequent MRSA infection similar to the rate in ST5 / ST239 cohort (12.8%) (P = 0.931). The median time to development of subsequent MRSA infection following new detection of nasal carriage was 27 days in ST72 cohort, which was not a statistically significant difference compared to ST5 / ST239 cohort (88 days). The Kaplan- Meier method was used to calculate the cumulative rate of being free of subsequent MRSA infection, and no significant difference was observed between two cohorts (P = ) (Fig. 2). Overall mortality rates did not differ between two cohorts (1.5% vs. 1.9%) (P = 1.000). The most frequent type of subsequent MRSA infections was pneumonia (50%), followed by urinary tract infection (13.0%), primary bacteremia (10.9%), surgical site infection (8.7%), intra-abdominal infection (8.7%), and skin and soft tissue infection (6.5%). There was no difference in distribution of infection types between two cohorts. Among 26 cases of subsequent MRSA infections in ST72 cohort, 19 (73.1%) were hospital-onset. Risk factors for subsequent MRSA infection in MRSA nasal carrier cohorts Multivariate analysis showed that the nasal carriers who also had MRSA isolated from culture of clinical specimens had 33-fold increased risk of subsequent MRSA infection (Table 2). Chronic lung disease and transfer from another hospital were also the risk factors for subsequent MRSA infection (O.R and O.R , respectively). Predictive factors for ST72 MRSA nasal carriage Multivariate analysis showed that predictive factors for ST72 MRSA among MRSA nasal carriage were preoperative screening for MRSA nasal carriage (odds ratio 1.828; 95% CI ; P = 0.015) and solid tumor (odds ratio 1.747; 95% CI ; P = 0.048). Discussion We found no evidence that rates of subsequent MRSA infection were different between community-genotype ST72 MRSA nasal carrier cohort and hospital-genotype ST5 / ST239 cohort. Comparison of the cumulative rates of being free of subsequent MRSA infection using the Kaplan-Meier method also revealed no significant
4 Park et al. Antimicrobial Resistance and Infection Control (2017) 6:60 Page 4 of 7 Table 1 Comparison of demographic and clinical characteristics of the patients colonized with methicillin-resistant Staphylococcus aureus between ST72 and ST5 / ST239 cohorts Variable No. (%) P value Community-genotype ST72 MRSA cohort (n = 198) Hospital-genotype ST5 / ST239 MRSA cohort (n = 156) Female gender 77 (38.9) 61 (39.1) Age, median (IQR) 53.0 ( ) 65.5 ( ) Reason for nasal MRSA screening Transfer from other hospital 68 (34.3) 60 (38.5) Pre-operative screening 80 (40.4) 39 (25.0) MRSA isolated from clinical specimens 22 (11.1) 10 (6.4) Carriage of vancomycin-resistant Enterococcus 10 (5.1) 13 (8.3) Undergoing HD or CAPD 9 (4.5) 6 (3.8) Location before admission Tertiary hospital 141 (71.2) 113 (72.4) Home 34 (17.2) 26 (16.7) General hospital 19 (9.6) 11 (7.1) Chronic care facility 4 (2.0) 6 (3.8) Admission due to infection other than MRSA infection 32 (16.2) 39 (25.0) Comorbidity Solid tumor 48 (24.2) 24 (15.4) Cardiovascular disease 40 (20.2) 33 (21.2) Diabetes mellitus 26 (13.1) 32 (20.5) Liver disease 21 (10.6) 14 (9.0) Neurologic disease 20 (10.1) 24 (15.4) Chronic kidney disease 19 (9.6) 21 (13.5) Solid organ transplantation 7 (3.5) 3 (1.9) Chronic lung disease 5 (2.5) 10 (6.4) Hematologic malignancy 4 (2.0) 11 (7.1) CAPD 0 (0.0) 3 (1.9) HSCT 0 (0.0) 1 (0.6) Severity of underlying disease Rapidly fatal 9 (4.6) 5 (3.2) Ultimately fatal 102 (51.5) 76 (48.7) Nonfatal 87 (43.9) 75 (48.7) ST sequence type, IQR Interquartile range, HD hemodialysis, CAPD Continuous ambulatory peritoneal dialysis, HSCT hematopoietic stem cell transplantation difference between two cohorts. In most previous reports studying subsequent MRSA infection rates among MRSA carriers, the difference of infection rates according to the genotype was not studied. Our study is unique in this regard because we compared the subsequent MRSA infection rates between hospital-endemic MRSA clones and CA-MRSA clone highly prevalent in Korea. A retrospective cohort study in the US tertiary care medical center showed that 33% of MRSA carriers developed MRSA infections in the following year [16]. Another retrospective cohort study in the US hospitals showed that persistent MRSA colonizers had an increased risk of death (HR 2.58) and MRSA infection (HR 10.89) [17]. A retrospective cohort study conducted in Alaska aiming to determine if carriage of CA-MRSA increased the risk for subsequent soft tissue infection revealed nasal MRSA carriage to be a significant risk factor for skin infections in the first year when compared with MSSA and non S. aureus carriers [18]. In contrast, the study from the Asian countries is sparse. The report
5 Park et al. Antimicrobial Resistance and Infection Control (2017) 6:60 Page 5 of 7 Fig. 2 Kaplan-Meier curves for the cumulative risk of subsequent MRSA infection from the single center in Singapore showed that 14.4% of the MRSA carriers developed MRSA infection with median time to infection of 22 days [19]. It is interesting that ST72 MRSA cohort tended to have a shorter duration until developing subsequent MRSA infection compared to ST5 / ST239 cohort. A study from Singapore showed that risk of infection was much higher shortly after the initial acquisition; however the genotypes of MRSA were not determined [19]. In the retrospective cohort study from the US tertiary care medical center which also provided no information on genotypes showed that infection occurred a median of 56 days post-detection [16]. Higher virulence potential of CA-MRSA has been suggested in various communitygenotype MRSA clones. USA300 clone is well known to be highly virulent [20]. Enhanced virulence of ST59 CA- MRSA over hospital-associated lineages was also demonstrated [21]. However, the virulence of ST72 MRSA needs to be more elucidated. Two studies comparing the virulence of ST72 MRSA with that of ST5 revealed lower virulence of ST72 MRSA strains [22, 23]. Several genes associated with adhesion and virulence were absent or rarely found in ST72 isolates. Our study has demonstrated that isolation of MRSA from culture of clinical specimens was the most significant risk factor for subsequent MRSA infection in nasal carrier cohorts using the multivariate analysis. Although anterior nares are the most frequent carriage sites for S. aureus, multiple body sites can be colonized and CA-MRSA appears to be different in the distribution of colonization sites [7, 24]. As for USA300 strains, perirectal and inguinal area were common sites of colonization following the nares [25]. The frequencies of colonization in those areas were higher compared to non-usa300 strains. There are some limitations in our study. First, this study focused on screening the nasal MRSA carriers according to the infection prevention and control policy of the hospital, and screening for the MRSA carriage at other body sites was not routinely performed. The MRSA surveillance study from the hospitals in Taiwan, in which majority of the isolates were clonotypes belonging to ST239, showed that nares cultures alone detected only 72.5% % of all colonized patients [26]. As CA-MRSA strains are known to colonize various body sites rather than the nares frequently, the carriers who have a higher potential to develop subsequent MRSA infection could be excluded, affecting the results. Second, this was a retrospective design, and so many patients whose follow-up period less than 6 months were excluded from the analysis. It could affect the results. Third, the genotypes of MRSA isolates from subsequent infection were unknown, and so the relationship of MRSA isolates between the colonizing strains and the strains causing subsequent infection were not determined. Lastly, this is a single center study and caution should be exercised in generalizing our results. Conclusions In conclusion, we found no evidence that rates of subsequent MRSA infection were different between newly-
6 Park et al. Antimicrobial Resistance and Infection Control (2017) 6:60 Page 6 of 7 Table 2 Risk factors for subsequent MRSA infection in MRSA nasal carrier cohorts Variable No. (%) P Adjusted OR (95% CI) P Patients with subsequent MRSA infection (n = 46) Patients with no subsequent MRSA infection (n = 308) Female gender 16 (34.8) 122 (39.6) Age, median (IQR) 57.5 ( ) 52.5 ( ) ST72 MRSA 26 (56.5) 172 (55.8) Reason for nasal MRSA screening Transfer from other hospital 24 (52.2) 104 (33.8) ( Pre-operative screening 11 (23.9) 108 (35.1) MRSA isolated from clinical specimens 23 (50.0) 9 (2.9) < ( ) <0.001 Carriage of VRE 2 (4.3) 21 (6.8) Undergoing HD or CAPD 3 (6.5) 12 (3.9) Admission due to infection other than MRSA infection Comorbidity 17 (37.0) 54 (17.5) ( ) Solid tumor 9 (16.9) 63 (20.5) Cardiovascular 10 (21.7) 63 (20.5) Diabetes mellitus 11 (23.9) 47 (15.3) Liver disease 6 (13.0) 29 (9.4) Neurologic disease 4 (8.7) 40 (13.0) Chronic kidney disease 8 (17.4) 32 (10.4) Solid organ transplantation 2 (4.3) 8 (2.6) Chronic lung disease 7 (15.2) 8 (2.6) ( ) Hematologic malignancy 3 (6.5) 12 (3.9) CAPD 0 (0.0) 3 (1.0) HSCT 0 (0.0) 1 (0.3) Severity of underlying disease Rapidly fatal 3 (6.5) 11 (3.6) Ultimately fatal 26 (56.5) 152 (49.4) Nonfatal 17 (37.0) 145 (47.1) MRSA methicillin-resistant Staphylococcus aureus, OR odds ratio, IQR Interquartile range, ST sequence type, VRE vancomycin-resistant Enterococcus, HD hemodialysis, CAPD continuous ambulatory peritoneal dialysis, HSCT hematopoietic stem cell transplantation admitted patients carrying community-genotype ST72 MRSA and those whom carrying hospital-genotypes ST5 or ST239 MRSA in the following 6 months. This study also suggests the importance of post-discharge surveillance in determining the incidence of healthcareassociated infections due to MRSA, considering that infections occur after a considerable period of time after becoming a carrier. Acknowledgements Not applicable. Funding This work was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education, Science and Technology (NRF-2016M3A9B ) and by a grant from the Korean Health Technology R&D Project, Ministry of Health & Welfare, Republic of Korea (HI12C0756). Availability of data and materials The datasets generated and/or analysed during the current study are not publicly available but are available from the corresponding author on reasonable request. Authors contributions SYP performed the data collection. YRK and SHK performed the laboratory experiments. SYP, YRK, SYC, and DRC performed the analysis. SYP, YEH, CIK, KRP, JHS and DRC conceived the study, participated in its design and drafted the manuscript. All authors read and approved the final manuscript. Competing interests The authors declare that they have no competing interests. Consent for publication Not applicable. Ethics approval and consent to participate The Institute Review Board of Samsung Medical Center approved this study and a waiver of the informed consent ( ).
7 Park et al. Antimicrobial Resistance and Infection Control (2017) 6:60 Page 7 of 7 Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Division of Infectious Diseases, Department of Internal Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, 81 Irwon-ro, Gangnam-gu, Seoul 06351, Republic of Korea. 2 Center for Infection Prevention and Control, Samsung Medical Center, Seoul, South Korea. 3 Asia Pacific Foundation for Infectious Diseases, Seoul, South Korea. 4 Present address: Division of Infectious Diseases, Kangdong Sacred Heart Hospital, Hallym University College of Medicine, Seoul, South Korea. Received: 2 April 2017 Accepted: 5 June 2017 References 1. von Eiff C, Becker K, Machka K, Stammer H, Peters G. Nasal carriage as a source of Staphylococcus aureus bacteremia. Study group. N Engl J Med. 2001;344: Wertheim HFL, Vos MC, Ott A, van Belkum A, Voss A, Kluytmans JAJW, et al. Risk and outcome of nosocomial Staphylococcus aureus bacteraemia in nasal carriers versus non-carriers. Lancet. 2004;364: Coello R, Glynn JR, Gaspar C, Picazo JJ, Fereres J. Risk factors for developing clinical infection with methicillin-resistant Staphylococcus aureus (MRSA) amongst hospital patients initially only colonized with MRSA. J Hosp Infect. 1997;37: Davis KA, Stewart JJ, Crouch HK, Florez CE, Hospenthal DR. Methicillinresistant Staphylococcus aureus (MRSA) nares colonization at hospital admission and its effect on subsequent MRSA infection. Clin Infect Dis. 2004;39: Moran GJ, Krishnadasan A, Gorwitz RJ, Fosheim GE, McDougal LK, Carey RB, Talan DA, Group EMINS. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med. 2006;355: Maree CL, Daum RS, Boyle-Vavra S, Matayoshi K, Miller LG. Communityassociated methicillin-resistant Staphylococcus aureus isolates causing healthcare-associated infections. Emerg Infect Dis. 2007;13: DeLeo FR, Otto M, Kreiswirth BN, Chambers HF. Community-associated meticillin-resistant Staphylococcus aureus. Lancet. 2010;375: Naimi TS, LeDell KH, Como-Sabetti K, Borchardt SM, Boxrud DJ, Etienne J, et al. Comparison of community- and health care-associated methicillinresistant Staphylococcus aureus infection. JAMA. 2003;290: Kim ES, Song JS, Lee HJ, Choe PG, Park KH, Cho JH, et al. A survey of community-associated methicillin-resistant Staphylococcus aureus in Korea. J Antimicrob Chemother. 2007;60: Song JH, Hsueh PR, Chung DR, Ko KS, Kang CI, Peck KR, et al. Spread of methicillin-resistant Staphylococcus aureus between the community and the hospitals in Asian countries: an ANSORP study. J Antimicrob Chemother. 2011;66: Joo EJ, Chung DR, Ha YE, Park SY, Kang SJ, Kim SH, et al. Communityassociated Panton-valentine leukocidin-negative meticillin-resistant Staphylococcus aureus clone (ST72-MRSA-IV) causing healthcare-associated pneumonia and surgical site infection in Korea. J Hosp Infect. 2012;81: Park SY, Chung DR, Yoo JR, Baek JY, Kim SH, Ha YE, et al. Sequence type 72 community-associated meticillin-resistant Staphylococcus aureus emerged as a predominant clone of nasal colonization in newly admitted patients. J Hosp Infect. 2016;93: McCabe W, Jackson G. Gram-negative bacteremia: I. Etiology and ecology. Arch Intern Med. 1962;110: Clinical and Laboratory Standards Institute. Performance standards for antimicrobial susceptibility testing; Twenty-First Informational Supplement M100-S21. Wayne, PA; Enright MC, Day NP, Davies CE, Peacock SJ, Spratt BG. Multilocus sequence typing for characterization of methicillin-resistant and methicillin-susceptible clones of Staphylococcus aureus. J Clin Microbiol. 2000;38: Huang SS, Hinrichsen VL, Datta R, Spurchise L, Miroshnik I, Nelson K, et al. Methicillin-resistant Staphylococcus aureus infection and hospitalization in high-risk patients in the year following detection. PLoS One. 2011;6:e Gupta K, Martinello RA, Young M, Strymish J, Cho K, Lawler E. MRSA nasal carriage patterns and the subsequent risk of conversion between patterns, infection, and death. PLoS One. 2013;8:e Stevens AM, Hennessy T, Baggett HC, Bruden D, Parks D, Klejka J. Methicillin-resistant Staphylococcus aureus carriage and risk factors for skin infections, southwestern Alaska. USA Emerg Infect Dis. 2010;16: Balm MN, Lover AA, Salmon S, Tambyah PA, Fisher DA. Progression from new methicillin-resistant Staphylococcus aureus colonisation to infection: an observational study in a hospital cohort. BMC Infect Dis. 2013;13: Li M, Diep BA, Villaruz AE, Braughton KR, Jiang X, DeLeo FR, et al. Evolution of virulence in epidemic community-associated methicillin-resistant Staphylococcus aureus. Proc Natl Acad Sci U S A. 2009;106: Li M, Dai Y, Zhu Y, Fu CL, Tan VY, Wang Y, et al. Virulence determinants associated with the Asian community-associated methicillin-resistant Staphylococcus aureus lineage ST59. Sci Rep. 2016;6: Joo EJ, Choi JY, Chung DR, Song JH, Ko KS. Characteristics of the community-genotype sequence type 72 methicillin-resistant Staphylococcus aureus isolates that underlie their persistence in hospitals. J Microbiol. 2016;54: Park KH, Chong YP, Kim SH, Lee SO, Choi SH, Lee MS, et al. Communityassociated MRSA strain ST72-SCCmecIV causing bloodstream infections: clinical outcomes and bacterial virulence factors. J Antimicrob Chemother. 2015;70: Wertheim HF, Melles DC, Vos MC, van Leeuwen W, van Belkum A, Verbrugh HA, et al. The role of nasal carriage in Staphylococcus aureus infections. Lancet Infect Dis. 2005;5: Popovich KJ, Aroutcheva A, Hota B, Beavis KG, Hayden MK, Weinstein RA. Anatomic sites of colonization with community-associated methicillinresistant Staphylococcus aureus. Infect Control Hosp Epidemiol. 2014l35: Lauderdale TL, Wang JT, Lee WS, Huang JH, McDonald LC, Huang IW, et al. Carriage rates of methicillin-resistant Staphylococcus aureus (MRSA) depend on anatomic location, the number of sites cultured, culture methods, and the distribution of clonotypes. Eur J Clin Microbiol Infect Dis. 2010;29: Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
FM - Male, 38YO. MRSA nasal swab (+) Due to positive MRSA nasal swab test, patient will be continued on Vancomycin 1500mg IV q12 for MRSA treatment...
 Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Hong-Kai Wang 1, Chun-Yen Huang 1 and Yhu-Chering Huang 1,2*
 Wang et al. BMC Infectious Diseases (2017) 17:470 DOI 10.1186/s12879-017-2560-0 RESEARCH ARTICLE Open Access Clinical features and molecular characteristics of childhood communityassociated methicillin-resistant
Wang et al. BMC Infectious Diseases (2017) 17:470 DOI 10.1186/s12879-017-2560-0 RESEARCH ARTICLE Open Access Clinical features and molecular characteristics of childhood communityassociated methicillin-resistant
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs?
 Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Principles of Antimicrobial Therapy
 Principles of Antimicrobial Therapy Doo Ryeon Chung, MD, PhD Professor of Medicine, Division of Infectious Diseases Director, Infection Control Office SUNGKYUNKWAN UNIVERSITY SCHOOL OF MEDICINE CASE 1
Principles of Antimicrobial Therapy Doo Ryeon Chung, MD, PhD Professor of Medicine, Division of Infectious Diseases Director, Infection Control Office SUNGKYUNKWAN UNIVERSITY SCHOOL OF MEDICINE CASE 1
Is Cefazolin Inferior to Nafcillin for Treatment of Methicillin-Susceptible Staphylococcus aureus Bacteremia?
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2011, p. 5122 5126 Vol. 55, No. 11 0066-4804/11/$12.00 doi:10.1128/aac.00485-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Is Cefazolin
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2011, p. 5122 5126 Vol. 55, No. 11 0066-4804/11/$12.00 doi:10.1128/aac.00485-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Is Cefazolin
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
2016/LSIF/FOR/007 Improving Antimicrobial Use and Awareness in Korea
 2016/LSIF/FOR/007 Improving Antimicrobial Use and Awareness in Korea Submitted by: Asia Pacific Foundation for Infectious Diseases Policy Forum on Strengthening Surveillance and Laboratory Capacity to
2016/LSIF/FOR/007 Improving Antimicrobial Use and Awareness in Korea Submitted by: Asia Pacific Foundation for Infectious Diseases Policy Forum on Strengthening Surveillance and Laboratory Capacity to
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Risk Factors for Persistent MRSA Colonization in Children with Multiple Intensive Care Unit Admissions
 University of Massachusetts Amherst From the SelectedWorks of Nicholas G Reich July, 2013 Risk Factors for Persistent MRSA Colonization in Children with Multiple Intensive Care Unit Admissions Victor O.
University of Massachusetts Amherst From the SelectedWorks of Nicholas G Reich July, 2013 Risk Factors for Persistent MRSA Colonization in Children with Multiple Intensive Care Unit Admissions Victor O.
The importance of infection control in the era of multi drug resistance
 Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
Prevalence and Molecular Characteristics of Methicillin-resistant Staphylococcus aureus Isolates in a Neonatal Intensive Care Unit
 Journal of Bacteriology and Virology 2016. Vol. 46, No. 2 p.99 103 http://dx.doi.org/10.4167/jbv.2016.46.2.99 Communication Prevalence and Molecular Characteristics of Methicillin-resistant Staphylococcus
Journal of Bacteriology and Virology 2016. Vol. 46, No. 2 p.99 103 http://dx.doi.org/10.4167/jbv.2016.46.2.99 Communication Prevalence and Molecular Characteristics of Methicillin-resistant Staphylococcus
Healthcare-associated Infections Annual Report March 2015
 March 2015 Healthcare-associated Infections Annual Report 2009-2014 TABLE OF CONTENTS SUMMARY... 1 MRSA SURVEILLANCE RESULTS... 1 CDI SURVEILLANCE RESULTS... 1 INTRODUCTION... 2 METHICILLIN-RESISTANT
March 2015 Healthcare-associated Infections Annual Report 2009-2014 TABLE OF CONTENTS SUMMARY... 1 MRSA SURVEILLANCE RESULTS... 1 CDI SURVEILLANCE RESULTS... 1 INTRODUCTION... 2 METHICILLIN-RESISTANT
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Why should we care about multi-resistant bacteria? Clinical impact and
 Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
Changing trends in clinical characteristics and antibiotic susceptibility of Klebsiella pneumoniae bacteremia
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:595-603 Changing trends in clinical characteristics and antibiotic susceptibility of Klebsiella pneumoniae Miri Hyun, Chang In Noh, Seong Yeol Ryu, and Hyun
ORIGINAL ARTICLE Korean J Intern Med 2018;33:595-603 Changing trends in clinical characteristics and antibiotic susceptibility of Klebsiella pneumoniae Miri Hyun, Chang In Noh, Seong Yeol Ryu, and Hyun
Nosocomial Infections: What Are the Unmet Needs
 Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Division of Infectious Diseases, Department of Internal Medicine, Soonchunhyang University Hospital, Seoul, Korea
 Original Article http://dx.doi.org/10.3947/ic.2014.46.3.172 Infect Chemother 2014;46(3):172-181 pissn 2093-2340 eissn 2092-6448 Infection & Chemotherapy Oral Antimicrobial Therapy: Efficacy and Safety
Original Article http://dx.doi.org/10.3947/ic.2014.46.3.172 Infect Chemother 2014;46(3):172-181 pissn 2093-2340 eissn 2092-6448 Infection & Chemotherapy Oral Antimicrobial Therapy: Efficacy and Safety
Analysis of community- and hospital-acquired bacteraemia during a recent 5-year period
 Journal of Medical Microbiology (2014), 63, 421 426 DOI 10.1099/jmm.0.069054-0 Analysis of community- and hospital-acquired bacteraemia during a recent 5-year period Hee-Won Moon, Young Jin Ko, Seungman
Journal of Medical Microbiology (2014), 63, 421 426 DOI 10.1099/jmm.0.069054-0 Analysis of community- and hospital-acquired bacteraemia during a recent 5-year period Hee-Won Moon, Young Jin Ko, Seungman
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Risk of organism acquisition from prior room occupants: A systematic review and meta analysis
 Risk of organism acquisition from prior room occupants: A systematic review and meta analysis A/Professor Brett Mitchell 1-2 Dr Stephanie Dancer 3 Dr Malcolm Anderson 1 Emily Dehn 1 1 Avondale College;
Risk of organism acquisition from prior room occupants: A systematic review and meta analysis A/Professor Brett Mitchell 1-2 Dr Stephanie Dancer 3 Dr Malcolm Anderson 1 Emily Dehn 1 1 Avondale College;
Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
 Infect Dis Ther (2014) 3:55 59 DOI 10.1007/s40121-014-0028-8 BRIEF REPORT Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
Infect Dis Ther (2014) 3:55 59 DOI 10.1007/s40121-014-0028-8 BRIEF REPORT Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
Screening programmes for Hospital Acquired Infections
 Screening programmes for Hospital Acquired Infections European Diagnostic Manufacturers Association In Vitro Diagnostics Making a real difference in health & life quality June 2007 HAI Facts Every year,
Screening programmes for Hospital Acquired Infections European Diagnostic Manufacturers Association In Vitro Diagnostics Making a real difference in health & life quality June 2007 HAI Facts Every year,
HEALTHCARE-ACQUIRED INFECTIONS AND ANTIMICROBIAL RESISTANCE
 Universidade de São Paulo Departamento de Moléstias Infecciosas e Parasitárias HEALTHCARE-ACQUIRED INFECTIONS AND ANTIMICROBIAL RESISTANCE Anna S. Levin 4 main lines! Epidemiology of HAS and resistance!
Universidade de São Paulo Departamento de Moléstias Infecciosas e Parasitárias HEALTHCARE-ACQUIRED INFECTIONS AND ANTIMICROBIAL RESISTANCE Anna S. Levin 4 main lines! Epidemiology of HAS and resistance!
ACCEPTED. Division of pediatric infectious diseases, Chang Gung Children s Hospital and Chang
 JCM Accepts, published online ahead of print on 1 October 00 J. Clin. Microbiol. doi:./jcm.0-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on 1 October 00 J. Clin. Microbiol. doi:./jcm.0-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
The CARI Guidelines Caring for Australians with Renal Impairment. 8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter
 8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: February 2003 Final submission: May 2004 Guidelines (Include recommendations based on level I or II evidence) Antibiotic
8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: February 2003 Final submission: May 2004 Guidelines (Include recommendations based on level I or II evidence) Antibiotic
(DRAFT) RECOMMENDATIONS FOR THE CONTROL OF MULTI-DRUG RESISTANT GRAM-NEGATIVES: CARBAPENEM RESISTANT ENTEROBACTERIACEAE
 (DRAFT) RECOMMENDATIONS FOR THE CONTROL OF MULTI-DRUG RESISTANT GRAM-NEGATIVES: CARBAPENEM RESISTANT ENTEROBACTERIACEAE John Ferguson (Hunter New England, NSW) on behalf of MRGN Task Force Acknowledgement
(DRAFT) RECOMMENDATIONS FOR THE CONTROL OF MULTI-DRUG RESISTANT GRAM-NEGATIVES: CARBAPENEM RESISTANT ENTEROBACTERIACEAE John Ferguson (Hunter New England, NSW) on behalf of MRGN Task Force Acknowledgement
Risk Factors Associated with Methicillin Resistance among Staphylococcus aureus Infections in Veterans
 infection control and hospital epidemiology january 2010, vol. 31, no. 1 original article Risk Factors Associated with Methicillin Resistance among Staphylococcus aureus s in Veterans Natalie L. McCarthy,
infection control and hospital epidemiology january 2010, vol. 31, no. 1 original article Risk Factors Associated with Methicillin Resistance among Staphylococcus aureus s in Veterans Natalie L. McCarthy,
*Corresponding Author:
 Original Research Article DOI: 10.18231/2394-5478.2017.0098 Prevalence and factors associated with the nasal colonization of Staphylococcus aureus and Methicillin-Resistant Staphylococcus aureus among
Original Research Article DOI: 10.18231/2394-5478.2017.0098 Prevalence and factors associated with the nasal colonization of Staphylococcus aureus and Methicillin-Resistant Staphylococcus aureus among
Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care units
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
REVISIONE CRITICA sulla VALIDITA delle COMUNI MISURE per la PREVENZIONE delle INFEZIONI CORRELATE a CATETERE INTRAVASCOLARE
 Le Malattie infettive del terzo millennio - dall isolamento all integrazione Paestum 13-15 maggio 2004 REVISIONE CRITICA sulla VALIDITA delle COMUNI MISURE per la PREVENZIONE delle INFEZIONI CORRELATE
Le Malattie infettive del terzo millennio - dall isolamento all integrazione Paestum 13-15 maggio 2004 REVISIONE CRITICA sulla VALIDITA delle COMUNI MISURE per la PREVENZIONE delle INFEZIONI CORRELATE
Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives
 Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives John Jernigan, MD, MS Alex Kallen, MD, MPH Division of Healthcare Quality Promotion Centers for Disease
Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives John Jernigan, MD, MS Alex Kallen, MD, MPH Division of Healthcare Quality Promotion Centers for Disease
Epidemiology of early-onset bloodstream infection and implications for treatment
 Epidemiology of early-onset bloodstream infection and implications for treatment Richard S. Johannes, MD, MS Marlborough, Massachusetts Health care-associated infections: For over 35 years, infections
Epidemiology of early-onset bloodstream infection and implications for treatment Richard S. Johannes, MD, MS Marlborough, Massachusetts Health care-associated infections: For over 35 years, infections
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Surveillance of Multi-Drug Resistant Organisms
 Surveillance of Multi-Drug Resistant Organisms Karen Hoffmann, RN, MS, CIC Associate Director Statewide Program for Infection Control and Epidemiology (SPICE) University of North Carolina School of Medicine
Surveillance of Multi-Drug Resistant Organisms Karen Hoffmann, RN, MS, CIC Associate Director Statewide Program for Infection Control and Epidemiology (SPICE) University of North Carolina School of Medicine
Burden of disease of antibiotic resistance The example of MRSA. Eva Melander Clinical Microbiology, Lund University Hospital
 Burden of disease of antibiotic resistance The example of MRSA Eva Melander Clinical Microbiology, Lund University Hospital Discovery of antibiotics Enormous medical gains Significantly reduced morbidity
Burden of disease of antibiotic resistance The example of MRSA Eva Melander Clinical Microbiology, Lund University Hospital Discovery of antibiotics Enormous medical gains Significantly reduced morbidity
Risk factors for methicillin-resistant Staphylococcus aureus bacteraemia differ depending on the control group chosen
 Epidemiol. Infect. (2013), 141, 2376 2383. Cambridge University Press 2013 doi:10.1017/s0950268813000174 Risk factors for methicillin-resistant Staphylococcus aureus bacteraemia differ depending on the
Epidemiol. Infect. (2013), 141, 2376 2383. Cambridge University Press 2013 doi:10.1017/s0950268813000174 Risk factors for methicillin-resistant Staphylococcus aureus bacteraemia differ depending on the
Horizontal vs Vertical Infection Control Strategies
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL Chapter 14 Horizontal vs Vertical Infection Control Strategies Author Salma Abbas, MBBS Michael Stevens, MD, MPH Chapter Editor Shaheen Mehtar, MBBS. FRC Path,
GUIDE TO INFECTION CONTROL IN THE HOSPITAL Chapter 14 Horizontal vs Vertical Infection Control Strategies Author Salma Abbas, MBBS Michael Stevens, MD, MPH Chapter Editor Shaheen Mehtar, MBBS. FRC Path,
Approval Signature: Original signed by Dr. Michel Tetreault Date of Approval: July Review Date: July 2017
 WRHA Infection Prevention and Control Program Operational Directives Admission Screening for Antibiotic Resistant Organisms (AROs): Methicillin Resistant Staphylococcus aureus (MRSA) and Vancomycin Resistant
WRHA Infection Prevention and Control Program Operational Directives Admission Screening for Antibiotic Resistant Organisms (AROs): Methicillin Resistant Staphylococcus aureus (MRSA) and Vancomycin Resistant
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017
 Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
Appropriate antimicrobial therapy in HAP: What does this mean?
 Appropriate antimicrobial therapy in HAP: What does this mean? Jaehee Lee, M.D. Kyungpook National University Hospital, Korea KNUH since 1907 Presentation outline Empiric antimicrobial choice: right spectrum,
Appropriate antimicrobial therapy in HAP: What does this mean? Jaehee Lee, M.D. Kyungpook National University Hospital, Korea KNUH since 1907 Presentation outline Empiric antimicrobial choice: right spectrum,
Success for a MRSA Reduction Program: Role of Surveillance and Testing
 Success for a MRSA Reduction Program: Role of Surveillance and Testing Singapore July 13, 2009 Lance R. Peterson, MD Director of Microbiology and Infectious Disease Research Associate Epidemiologist, NorthShore
Success for a MRSA Reduction Program: Role of Surveillance and Testing Singapore July 13, 2009 Lance R. Peterson, MD Director of Microbiology and Infectious Disease Research Associate Epidemiologist, NorthShore
GUIDE TO INFECTION CONTROL IN THE HOSPITAL
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
Lindsay E. Nicolle University of Manitoba Winnipeg, CANADA
 Lindsay E. Nicolle University of Manitoba Winnipeg, CANADA Long Term Care Facilities: Spectrum low acuity assisted living mobile independent Not LTAC high acuity complete functional disability dialysis
Lindsay E. Nicolle University of Manitoba Winnipeg, CANADA Long Term Care Facilities: Spectrum low acuity assisted living mobile independent Not LTAC high acuity complete functional disability dialysis
Prevalence and Risk Factor Analysis for Methicillin-Resistant Staphylococcus aureus Nasal Colonization in Children Attending Child Care Centers
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1041 1047 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.02235-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Prevalence
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1041 1047 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.02235-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Prevalence
Methicillin resistant Staphylococcus aureus (MRSA) in pigs, the Spanish experience
 Methicillin resistant Staphylococcus aureus (MRSA) in pigs, the Spanish experience M. Concepción Porrero, José-Francisco Fernández- Garayzabal, Ana Mateos and Lucas Domínguez cporrero@visavet.ucm.es Food-borne
Methicillin resistant Staphylococcus aureus (MRSA) in pigs, the Spanish experience M. Concepción Porrero, José-Francisco Fernández- Garayzabal, Ana Mateos and Lucas Domínguez cporrero@visavet.ucm.es Food-borne
Staphylococcus Aureus
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
ACCEPTED. Association between staphylococcal PVL gene and a lower inhospital. survival in Pulmonary Patients. Spain. Científicas (CSIC), Madrid, Spain
 JCM Accepts, published online ahead of print on 8 November 006 J. Clin. Microbiol. doi:10.118/jcm.003-06 Copyright 006, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 8 November 006 J. Clin. Microbiol. doi:10.118/jcm.003-06 Copyright 006, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
A Prospective Investigation of Nasal Mupirocin, Hexachlorophene Body Wash, and Systemic
 AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
Prevalence and molecular characteristics of MRSA colonization among adult
 Prevalence and molecular characteristics of MRSA colonization among adult patients visiting emergency department in a medical center in northern Taiwan Sheng-Yun Lu 1, Fang-Yu Chang 1, Ching-Chung Cheng
Prevalence and molecular characteristics of MRSA colonization among adult patients visiting emergency department in a medical center in northern Taiwan Sheng-Yun Lu 1, Fang-Yu Chang 1, Ching-Chung Cheng
Surgical prophylaxis for Gram +ve & Gram ve infection
 Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Community-associated methicillin-resistant Staphylococcus aureus infections
 British Medical Bulletin Advance Access published April 1, 2010 Community-associated methicillin-resistant Staphylococcus aureus infections Fiona J. Cooke and Nicholas M. Brown * Clinical Microbiology
British Medical Bulletin Advance Access published April 1, 2010 Community-associated methicillin-resistant Staphylococcus aureus infections Fiona J. Cooke and Nicholas M. Brown * Clinical Microbiology
Can we trust the Xpert?
 Can we trust the Xpert? An evaluation of the Xpert MRSA/SA BC System and an assessment of potential clinical impact Dr Kessendri Reddy Division of Medical Microbiology, NHLS Tygerberg Fakulteit Geneeskunde
Can we trust the Xpert? An evaluation of the Xpert MRSA/SA BC System and an assessment of potential clinical impact Dr Kessendri Reddy Division of Medical Microbiology, NHLS Tygerberg Fakulteit Geneeskunde
Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome
 MAJOR ARTICLE Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome Jörg J. Ruhe, 1,2 Nathaniel Smith, 1,3 Robert W. Bradsher,
MAJOR ARTICLE Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome Jörg J. Ruhe, 1,2 Nathaniel Smith, 1,3 Robert W. Bradsher,
Ann Dermatol Vol. 27, No. 4,
 MY Jung, et al Ann Dermatol Vol. 27, No. 4, 2015 http://dx.doi.org/10.5021/ad.2015.27.4.398 ORIGINAL ARTICLE Antibiotic Susceptibility of Staphylococcus aureus in Atopic Dermatitis: Current Prevalence
MY Jung, et al Ann Dermatol Vol. 27, No. 4, 2015 http://dx.doi.org/10.5021/ad.2015.27.4.398 ORIGINAL ARTICLE Antibiotic Susceptibility of Staphylococcus aureus in Atopic Dermatitis: Current Prevalence
ESBL Positive E. coli and K. pneumoneae are Emerging as Major Pathogens for Urinary Tract Infection
 ESBL Positive E. coli and K. pneumoneae are Emerging as Major Pathogens for Urinary Tract Infection Muhammad Abdur Rahim*, Palash Mitra*. Tabassum Samad*. Tufayel Ahmed Chowdhury*. Mehruba Alam Ananna*.
ESBL Positive E. coli and K. pneumoneae are Emerging as Major Pathogens for Urinary Tract Infection Muhammad Abdur Rahim*, Palash Mitra*. Tabassum Samad*. Tufayel Ahmed Chowdhury*. Mehruba Alam Ananna*.
The past decade has seen a large increase in infections
 Community-associated Methicillin- Resistant Staphylococcus aureus in Outpatients, United States, 1999 2006 Eili Klein, David L. Smith, and Ramanan Laxminarayan CME ACTIVITY MedscapeCME is pleased to provide
Community-associated Methicillin- Resistant Staphylococcus aureus in Outpatients, United States, 1999 2006 Eili Klein, David L. Smith, and Ramanan Laxminarayan CME ACTIVITY MedscapeCME is pleased to provide
Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital
 Epidemiology J Microbiol Immunol of MRSA Infect. bacteremia 2007;40:310-316 Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital Chih-Yu
Epidemiology J Microbiol Immunol of MRSA Infect. bacteremia 2007;40:310-316 Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital Chih-Yu
03/09/2014. Infection Prevention and Control A Foundation Course. Talk outline
 Infection Prevention and Control A Foundation Course 2014 What is healthcare-associated infection (HCAI), antimicrobial resistance (AMR) and multi-drug resistant organisms (MDROs)? Why we should be worried?
Infection Prevention and Control A Foundation Course 2014 What is healthcare-associated infection (HCAI), antimicrobial resistance (AMR) and multi-drug resistant organisms (MDROs)? Why we should be worried?
Nasal carriage rate and molecular epidemiology of methicillin-resistant Staphylococcus aureus among. medical students in a Taiwanese university
 Nasal carriage rate and molecular epidemiology of methicillin-resistant Staphylococcus aureus among medical students in a Taiwanese university Chang -Sheng Chen 1, Chao-Yu Chen 1, Yhu-Chering Huang 1,2
Nasal carriage rate and molecular epidemiology of methicillin-resistant Staphylococcus aureus among medical students in a Taiwanese university Chang -Sheng Chen 1, Chao-Yu Chen 1, Yhu-Chering Huang 1,2
MRSA in the United Kingdom status quo and future developments
 MRSA in the United Kingdom status quo and future developments Dietrich Mack Chair of Medical Microbiology and Infectious Diseases The School of Medicine - University of Wales Swansea P R I F Y S G O L
MRSA in the United Kingdom status quo and future developments Dietrich Mack Chair of Medical Microbiology and Infectious Diseases The School of Medicine - University of Wales Swansea P R I F Y S G O L
Acinetobacter sp. isolates from emergency departments in two hospitals of South Korea
 Journal of Medical Microbiology (2014), 63, 1363 1368 DOI 10.1099/jmm.0.075325-0 Acinetobacter sp. isolates from emergency departments in two hospitals of South Korea Ji-Young Choi, 1 3 Eun Ah Ko, 2 3
Journal of Medical Microbiology (2014), 63, 1363 1368 DOI 10.1099/jmm.0.075325-0 Acinetobacter sp. isolates from emergency departments in two hospitals of South Korea Ji-Young Choi, 1 3 Eun Ah Ko, 2 3
Correspondence should be addressed to Jun Yong Choi; and Dongeun Yong;
 BioMed Research International Volume 2015, Article ID 831074, 8 pages http://dx.doi.org/10.1155/2015/831074 Research Article Clinical Usefulness of the 2010 Clinical and Laboratory Standards Institute
BioMed Research International Volume 2015, Article ID 831074, 8 pages http://dx.doi.org/10.1155/2015/831074 Research Article Clinical Usefulness of the 2010 Clinical and Laboratory Standards Institute
Prevalence & Risk Factors For MRSA. For Vets
 For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
Antibacterials. Recent data on linezolid and daptomycin
 Antibacterials Recent data on linezolid and daptomycin Patricia Muñoz, MD. Ph.D. (pmunoz@micro.hggm.es) Hospital General Universitario Gregorio Marañón Universidad Complutense de Madrid. 1 GESITRA Reasons
Antibacterials Recent data on linezolid and daptomycin Patricia Muñoz, MD. Ph.D. (pmunoz@micro.hggm.es) Hospital General Universitario Gregorio Marañón Universidad Complutense de Madrid. 1 GESITRA Reasons
Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1
 Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Konsequenzen für Bevölkerung und Gesundheitssysteme. Stephan Harbarth Infection Control Program
 Konsequenzen für Bevölkerung und Gesundheitssysteme Stephan Harbarth Infection Control Program University of Geneva Hospitals Outline Introduction What data sources are available? AMR-associated outcomes
Konsequenzen für Bevölkerung und Gesundheitssysteme Stephan Harbarth Infection Control Program University of Geneva Hospitals Outline Introduction What data sources are available? AMR-associated outcomes
Summary of the latest data on antibiotic resistance in the European Union
 Summary of the latest data on antibiotic resistance in the European Union EARS-Net surveillance data November 2017 For most bacteria reported to the European Antimicrobial Resistance Surveillance Network
Summary of the latest data on antibiotic resistance in the European Union EARS-Net surveillance data November 2017 For most bacteria reported to the European Antimicrobial Resistance Surveillance Network
GUIDE TO INFECTION CONTROL IN THE HOSPITAL. Enterococcal Species
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 44 Enterococcal Species Authors Jacob Pierce, MD, Michael Edmond, MD, MPH, MPA Michael P. Stevens, MD, MPH Chapter Editor Victor D. Rosenthal, MD, CIC,
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 44 Enterococcal Species Authors Jacob Pierce, MD, Michael Edmond, MD, MPH, MPA Michael P. Stevens, MD, MPH Chapter Editor Victor D. Rosenthal, MD, CIC,
Contrasting Pediatric and Adult Methicillin-resistant Staphylococcus aureus Isolates
 Contrasting Pediatric and Adult Methicillin-resistant Staphylococcus aureus Isolates Michael Z. David,* Susan E. Crawford,* Susan Boyle-Vavra,* Mark A. Hostetler,* Daniel C. Kim,* and Robert S. Daum* We
Contrasting Pediatric and Adult Methicillin-resistant Staphylococcus aureus Isolates Michael Z. David,* Susan E. Crawford,* Susan Boyle-Vavra,* Mark A. Hostetler,* Daniel C. Kim,* and Robert S. Daum* We
Empiric antimicrobial use in the treatment of dialysis related infections in RIPAS Hospital
 Original Article Brunei Int Med J. 2013; 9 (6): 372-377 Empiric antimicrobial use in the treatment of dialysis related infections in RIPAS Hospital Lah Kheng CHUA, Department of Pharmacy, RIPAS Hospital,
Original Article Brunei Int Med J. 2013; 9 (6): 372-377 Empiric antimicrobial use in the treatment of dialysis related infections in RIPAS Hospital Lah Kheng CHUA, Department of Pharmacy, RIPAS Hospital,
UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients
 Background/methods: UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients This guideline establishes evidence-based consensus standards for management
Background/methods: UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients This guideline establishes evidence-based consensus standards for management
original article infection control and hospital epidemiology october 2009, vol. 30, no. 10
 infection control and hospital epidemiology october 2009, vol. 30, no. 10 original article 5 Years of Experience Implementing a Methicillin-Resistant Staphylococcus aureus Search and Destroy Policy at
infection control and hospital epidemiology october 2009, vol. 30, no. 10 original article 5 Years of Experience Implementing a Methicillin-Resistant Staphylococcus aureus Search and Destroy Policy at
Antimicrobial Cycling. Donald E Low University of Toronto
 Antimicrobial Cycling Donald E Low University of Toronto Bad Bugs, No Drugs 1 The Antimicrobial Availability Task Force of the IDSA 1 identified as particularly problematic pathogens A. baumannii and
Antimicrobial Cycling Donald E Low University of Toronto Bad Bugs, No Drugs 1 The Antimicrobial Availability Task Force of the IDSA 1 identified as particularly problematic pathogens A. baumannii and
Safe Patient Care Keeping our Residents Safe Use Standard Precautions for ALL Residents at ALL times
 Safe Patient Care Keeping our Residents Safe 2016 Use Standard Precautions for ALL Residents at ALL times #safepatientcare Do bugs need drugs? Dr Deirdre O Brien Consultant Microbiologist Mercy University
Safe Patient Care Keeping our Residents Safe 2016 Use Standard Precautions for ALL Residents at ALL times #safepatientcare Do bugs need drugs? Dr Deirdre O Brien Consultant Microbiologist Mercy University
Genetic Lineages of Methicillin-Resistant Staphylococcus aureus Acquired during Admission to an Intensive Care Unit of a General Hospital
 Original Paper Received: April 10, 2016 Accepted: November 8, 2016 Published online: November 8, 2016 Genetic Lineages of Methicillin-Resistant Staphylococcus aureus Acquired during Admission to an Intensive
Original Paper Received: April 10, 2016 Accepted: November 8, 2016 Published online: November 8, 2016 Genetic Lineages of Methicillin-Resistant Staphylococcus aureus Acquired during Admission to an Intensive
Research Article Risk Factors Associated with Vancomycin-Resistant Enterococcus in Intensive Care Unit Settings in Saudi Arabia
 Interdisciplinary Perspectives on Infectious Diseases Volume 2013, Article ID 369674, 4 pages http://dx.doi.org/10.1155/2013/369674 Research Article Risk Factors Associated with Vancomycin-Resistant Enterococcus
Interdisciplinary Perspectives on Infectious Diseases Volume 2013, Article ID 369674, 4 pages http://dx.doi.org/10.1155/2013/369674 Research Article Risk Factors Associated with Vancomycin-Resistant Enterococcus
Follow this and additional works at:
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses Dissertations and Theses 2014 Penicillin Use and Duration of Bacteremia, Length of Stay, and 30-day Readmission in Hospitalized
University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses Dissertations and Theses 2014 Penicillin Use and Duration of Bacteremia, Length of Stay, and 30-day Readmission in Hospitalized
NEONATAL Point Prevalence Survey. Ward Form
 Appendix 2 NEONATAL Point Prevalence Survey Ward Form Please fill in one form for each ward included in PPS Date of survey Person completing form (Auditor code) Hospital Name Department/Ward Neonatal departments
Appendix 2 NEONATAL Point Prevalence Survey Ward Form Please fill in one form for each ward included in PPS Date of survey Person completing form (Auditor code) Hospital Name Department/Ward Neonatal departments
Antimicrobial stewardship: Quick, don t just do something! Stand there!
 Antimicrobial stewardship: Quick, don t just do something! Stand there! Stanley I. Martin, MD, FACP, FIDSA Director, Division of Infectious Diseases Director, Antimicrobial Stewardship Program Geisinger
Antimicrobial stewardship: Quick, don t just do something! Stand there! Stanley I. Martin, MD, FACP, FIDSA Director, Division of Infectious Diseases Director, Antimicrobial Stewardship Program Geisinger
Preventing Multi-Drug Resistant Organism (MDRO) Infections. For National Patient Safety Goal
 Preventing Multi-Drug Resistant Organism (MDRO) Infections For National Patient Safety Goal 07.03.01 2009 Methicillin Resistant Staphlococcus aureus (MRSA) About 3-8% of the population at large is a carrier
Preventing Multi-Drug Resistant Organism (MDRO) Infections For National Patient Safety Goal 07.03.01 2009 Methicillin Resistant Staphlococcus aureus (MRSA) About 3-8% of the population at large is a carrier
Received 23 May 2004/Returned for modification 31 August 2004/Accepted 11 October 2004
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2005, p. 760 766 Vol. 49, No. 2 0066-4804/05/$08.00 0 doi:10.1128/aac.49.2.760 766.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2005, p. 760 766 Vol. 49, No. 2 0066-4804/05/$08.00 0 doi:10.1128/aac.49.2.760 766.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
FREQUENCY OF METHICILLIN RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COLONIZATION AMONGST HOSPITAL STAFF IN TEACHING HOSPITALS OF PESHAWAR
 Original Article ABSTRACT FREQUENCY OF METHICILLIN RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COLONIZATION AMONGST HOSPITAL STAFF IN TEACHING HOSPITALS OF PESHAWAR Muhammad Asghar 1, Naheed Asghar 2, Shahina
Original Article ABSTRACT FREQUENCY OF METHICILLIN RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COLONIZATION AMONGST HOSPITAL STAFF IN TEACHING HOSPITALS OF PESHAWAR Muhammad Asghar 1, Naheed Asghar 2, Shahina
MDRO in LTCF: Forming Networks to Control the Problem
 MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
Impact of Postoperative Antibiotic Prophylaxis Duration on Surgical Site Infections in Autologous Breast Reconstruction
 Impact of Postoperative Antibiotic Prophylaxis Duration on Surgical Site Infections in Autologous Breast Reconstruction Kerry E. Drury, BA 1 ; Steven T. Lanier, MD 1 ; Nima Khavanin, BS 1 ; Keith M. Hume,
Impact of Postoperative Antibiotic Prophylaxis Duration on Surgical Site Infections in Autologous Breast Reconstruction Kerry E. Drury, BA 1 ; Steven T. Lanier, MD 1 ; Nima Khavanin, BS 1 ; Keith M. Hume,
Randomized Controlled Trial on Adjunctive Lavage for Severe Peritoneal Dialysis- Related Peritonitis
 Randomized Controlled Trial on Adjunctive Lavage for Severe Peritoneal Dialysis- Related Peritonitis Steve SM Wong Alice Ho Miu Ling Nethersole Hospital Background PD peritonitis is a major cause of PD
Randomized Controlled Trial on Adjunctive Lavage for Severe Peritoneal Dialysis- Related Peritonitis Steve SM Wong Alice Ho Miu Ling Nethersole Hospital Background PD peritonitis is a major cause of PD
TACKLING THE MRSA EPIDEMIC
 TACKLING THE MRSA EPIDEMIC Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine MRSA Trend (HA + CA) in US TSN Database USA (1993-2003) % of MRSA among S. aureus
TACKLING THE MRSA EPIDEMIC Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine MRSA Trend (HA + CA) in US TSN Database USA (1993-2003) % of MRSA among S. aureus
Healthcare-associated Infections Annual Report
 September 2014 Healthcare-associated Infections Annual Report 2009-2013 Summary Provincial Infection Control Newfoundland Labrador (PIC-NL) has collected data on inpatients and outpatients with healthcare-associated
September 2014 Healthcare-associated Infections Annual Report 2009-2013 Summary Provincial Infection Control Newfoundland Labrador (PIC-NL) has collected data on inpatients and outpatients with healthcare-associated
IJETST- Vol. 03 Issue 07 Pages July ISSN
 International Journal of Emerging Trends in Science and Technology Impact Factor: 2.838 DOI: http://dx.doi.org/10.18535/ijetst/v3i07.13 A surveillance of MRSA nasal carriage in Community and Health Care
International Journal of Emerging Trends in Science and Technology Impact Factor: 2.838 DOI: http://dx.doi.org/10.18535/ijetst/v3i07.13 A surveillance of MRSA nasal carriage in Community and Health Care
OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS
 HTIDE CONFERENCE 2018 OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS FEDERICO PEA INSTITUTE OF CLINICAL PHARMACOLOGY DEPARTMENT OF MEDICINE, UNIVERSITY OF UDINE, ITALY SANTA
HTIDE CONFERENCE 2018 OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS FEDERICO PEA INSTITUTE OF CLINICAL PHARMACOLOGY DEPARTMENT OF MEDICINE, UNIVERSITY OF UDINE, ITALY SANTA
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016
 Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Int.J.Curr.Microbiol.App.Sci (2017) 6(3):
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 3 (2017) pp. 891-895 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.603.104
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 3 (2017) pp. 891-895 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.603.104
Summary Report Relating to a Pilot Program to Require Reporting of Methicillin-resistant Staphylococcus aureus
 Summary Report Relating to a Pilot Program to Require Reporting of Methicillin-resistant Staphylococcus aureus Prepared by the Texas Department of State Health Services as required by House Bill 1082,
Summary Report Relating to a Pilot Program to Require Reporting of Methicillin-resistant Staphylococcus aureus Prepared by the Texas Department of State Health Services as required by House Bill 1082,
Fifteen-Year Study of the Changing Epidemiology of Methicillin-Resistant Staphylococcus aureus
 The American Journal of Medicine (2006) 119, 943-951 CLINICAL RESEARCH STUDY AJM Theme Issue: Infectious Disease Fifteen-Year Study of the Changing Epidemiology of Methicillin-Resistant Staphylococcus
The American Journal of Medicine (2006) 119, 943-951 CLINICAL RESEARCH STUDY AJM Theme Issue: Infectious Disease Fifteen-Year Study of the Changing Epidemiology of Methicillin-Resistant Staphylococcus
Community-associated meticillin-resistant Staphylococcus aureus: the case for a genotypic definition
 Journal of Hospital Infection 81 (2012) 143e148 Available online at www.sciencedirect.com Journal of Hospital Infection journal homepage: www.elsevierhealth.com/journals/jhin Review Community-associated
Journal of Hospital Infection 81 (2012) 143e148 Available online at www.sciencedirect.com Journal of Hospital Infection journal homepage: www.elsevierhealth.com/journals/jhin Review Community-associated
Staphylococcus aureus nasal carriage in diabetic patients in a tertiary care hospital
 Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 15, 7 (7):23-28 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-5071 USA CODEN: DPLEB4 Staphylococcus
Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 15, 7 (7):23-28 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-5071 USA CODEN: DPLEB4 Staphylococcus
Preventing Surgical Site Infections. Edward L. Goodman, MD September 16, 2013
 Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
MRSA Control : Belgian policy
 MRSA Control : Belgian policy PEN ERY CLI DOT GEN KAN SXT CIP MIN RIF FUC MUP OXA Marc Struelens Service de microbiologie & unité d épidémiologie des maladies infectieuses Université Libre de Bruxelles
MRSA Control : Belgian policy PEN ERY CLI DOT GEN KAN SXT CIP MIN RIF FUC MUP OXA Marc Struelens Service de microbiologie & unité d épidémiologie des maladies infectieuses Université Libre de Bruxelles
Deborah A. Williamson 1,2,3 *, Sally A. Roberts 2, Stephen R. Ritchie 1, Geoffrey W. Coombs 4,5, John D. Fraser 1, Helen Heffernan 3.
 Clinical and Molecular Epidemiology of Methicillin- Resistant Staphylococcus aureus in New Zealand: Rapid Emergence of Sequence Type 5 (ST5)-SCCmec-IV as the Dominant Community-Associated MRSA Clone Deborah
Clinical and Molecular Epidemiology of Methicillin- Resistant Staphylococcus aureus in New Zealand: Rapid Emergence of Sequence Type 5 (ST5)-SCCmec-IV as the Dominant Community-Associated MRSA Clone Deborah
