Clinical Presentation of Nipah Virus Infection in Bangladesh
|
|
|
- Chloe Sparks
- 5 years ago
- Views:
Transcription
1 MAJOR ARTICLE Clinical Presentation of Nipah Virus Infection in Bangladesh M. Jahangir Hossain, 1 Emily S. Gurley, 1 Joel M. Montgomery, 4 Michael Bell, 4 Darin S. Carroll, 4 Vincent P. Hsu, 4 P. Formenty, 5 A. Croisier, 5 E. Bertherat, 5 M. A. Faiz, 2 Abul Kalam Azad, 3 Rafiqul Islam, 3 M. Abdur Rahim Molla, 3 Thomas G. Ksiazek, 4 Paul A. Rota, 4 James A. Comer, 4 Pierre E. Rollin, 4 Stephen P. Luby, 1 and Robert F. Breiman 1 1 International Centre for Diarrhoeal Disease Research and 2 Dhaka Medical College Hospital, Dhaka, and 3 Institute of Epidemiology, Disease Control and Research, Ministry of Health and Family Welfare, Government of Bangladesh, Bangladesh; 4 Centers for Disease Control and Prevention, Atlanta, Georgia; and 5 World Health Organization, Geneva, Switzerland Background. In Bangladesh, 4 outbreaks of Nipah virus infection were identified during the period Methods. We characterized the clinical features of Nipah virus infected individuals affected by these outbreaks. We classified patients as having confirmed cases of Nipah virus infection if they had antibodies reactive with Nipah virus antigen. Patients were considered to have probable cases of Nipah virus infection if they had symptoms consistent with Nipah virus infection during the same time and in the same community as patients with confirmed cases. Results. We identified 92 patients with Nipah virus infection, 67 (73%) of whom died. Although all age groups were affected, 2 outbreaks principally affected young persons (median age, 12 years); 62% of the affected persons were male. Fever, altered mental status, headache, cough, respiratory difficulty, vomiting, and convulsions were the most common signs and symptoms; clinical and radiographic features of acute respiratory distress syndrome of Nipah illness were identified during the fourth outbreak. Among those who died, death occurred a median of 6 days (range, 2 36 days) after the onset of illness. Patients who died were more likely than survivors to have a temperature C, altered mental status, difficulty breathing, and abnormal plantar reflexes. Among patients with Nipah virus infection who had well-defined exposure to another patient infected with Nipah virus, the median incubation period was 9 days (range, 6 11 days). Conclusions. Nipah virus infection produced rapidly progressive severe illness affecting the central nervous and respiratory systems. Clinical characteristics of Nipah virus infection in Bangladesh, including a severe respiratory component, appear distinct from clinical characteristics reported during earlier outbreaks in other countries. Nipah virus is a recently identified paramyxovirus that is closely related to Hendra virus [1]. The first recognized outbreaks of Nipah virus illness in humans occurred in Malaysia and Singapore from September 1998 through June 1999; 283 persons, mostly pig farm and abattoir workers were infected through contact with sick pigs [2 6]. A case-fatality rate of 40% was observed in Malaysia and Singapore; patients presented primarily with CNS symptoms [2, 7, 8]. A second outbreak of Received 8 July 2007; accepted 19 November 2007; electronically published 27 February Reprints or correspondence: Dr. M. Jahangir Hossain, Clinical Sciences Div., ICDDR,B, 68 Shaheed Tajuddin Ahmed Sarani, Mohakhali, Dhaka 1212, Bangladesh (jhossain@icddrb.org). Clinical Infectious Diseases 2008; 46: by the Infectious Diseases Society of America. All rights reserved /2008/ $15.00 DOI: / Nipah virus infection, with a case-fatality rate of 68%, occurred from January through February 2001 in Siliguri, India, a town close to the northern border of Bangladesh. Patients affected by this outbreak presented with both encephalitis and respiratory symptoms [9]. In Bangladesh, 7 outbreaks of Nipah virus infection were identified during the period In Bangladesh, Nipah virus infection was associated with contact with a sick cow, consumption of fresh date palm sap (potentially contaminated with pteropid bat saliva), and person-to-person transmission [10 12]. The Malaysian outbreak was associated with a single strain [13]. By contrast, viruses isolated in Bangladesh represent diverse strains [14]. Hypothetically, a single strain of Nipah virus could result in a narrower range of clinical presentations than those found during epidemics associated with genetically diverse strains. Thus, Nipah virus illnesses occurring in Bangladesh potentially pro- Clinical Presentation of Nipah Virus CID 2008:46 (1 April) 977
2 Table 1. Clinical characteristics of Nipah virus infection during different outbreaks in Bangladesh. Characteristic Age, years Meherpur, 2001 (n p 13) Naogaon, 2003 (n p 12) Outbreak Rajbari, 2004 (n p 31) Faridpur, 2004 (n p 36) All (n p 92) Mean SD Median (range) 38 (4 60) 12 (4 42) 12 (2 50) 35 (5 60) 26 (2 60) Fever 13/13 (100) 12/12 (100) 31/31 (100) 36/36 (100) 92/92 (100) Altered mental status a 13/13 (100) 10/12 (83) 30/30 (100) 29/36 (81) 82/91 (90) Unconsciousness b 3/13 (23) 9/12 (75) 28/30 (93) 27/36 (75) 67/91 (74) Headache 8/13 (62) 10/12 (83) 16/27 (59) 30/36 (83) 64/88 (73) Severe weakness NC 3/12 (25) 23/28 (82) 25/36 (69) 51/76 (67) Cough and/or cold 10/13 (77) 6/12 (50) 14/29 (48) 26/36 (72) 56/90 (62) Respiratory difficulty 9/13 (69) 7/12 (58) 19/29 (66) 27/36 (75) 62/90 (69) Vomiting 7/13 (54) 6/12 (50) 20/30 (67) 20/36 (56) 53/91 (58) Diarrhea 2/13 (15) 1/12 (8) 8/29 (28) 15/36 (42) 26/90 (29) Convulsion 3/13 (23) 3/12 (25) 14/30 (47) 1/36 (3) 21/91 (23) Planter reflex Absent ND ND 1/12 (8) 0/5 (0) 1/17 (6) Equivocal ND ND 2/12 (17) 2/5 (40) 4/17 (24) Extensor ND ND 6/12 (50) 0/5 (0) 6/17 (35) Flexor ND ND 3/12 (25) 0/5 (0) 3/17 (35) Deep tendon reflex Absent ND ND 4/11 (36) 0/3 (0) 4/14 (29) Diminished ND ND 5/11 (45) 0/3 (0) 5/14 (36) Exaggerated ND ND 0/11 (0) 0/3 (0) 0/14 (0) Normal ND ND 2/11 (18) 3/3 (100) 5/14 (36) Case fatality 9/13 (69) 8/12 (67) 23/31 (74) 27/36 (75) 67/92 (73) NOTE. Data are proportion (%) of patients, unless otherwise indicated. NC, not collected; ND, not done. a Altered mental status was defined as lack of orientation to time, place, and person. Unconsciousness was included as altered mental status. b Unconsciousness was defined as inability to give meaningful response to any stimuli. vide insight into broader clinical manifestations of Nipah virus infection. We describe the clinical presentation of 92 Nipah virus infected patients identified during the first 4 outbreaks in Bangladesh during the period METHODS We investigated cases of Nipah virus infection from 4 outbreaks in the following regions: Meherpur District (from April through May 2001), Naogaon District (in January 2003), Rajbari (Goalanda subdistrict) and 7 other northwestern districts (from January through April 2004), and Faridpur District (from February through April 2004) [10, 11, 15 20]. The investigations for the first and second outbreaks, in Mehepur and Naogaon, took place after the outbreaks occurred. Because of increased awareness of Nipah virus among health officials, the third and fourth outbreaks, in Rajbari and Faridpur, were reported to authorities and investigated while the outbreaks were ongoing. Therefore, the case definitions and case detection methods differed slightly because of differences in the timing of investigations. Outbreaks of Nipah virus infection in Meherpur and Naogaon. The investigation of the Meherpur outbreak was conducted 2 years after the outbreak, and the investigation of the Naogaon outbreak was performed 2 months after the outbreak. Patients with suspected cases of Nipah virus infection were persons residing in the outbreak areas who experienced fever with either headache or altered mental status during the time of the outbreak [11]. Field research assistants identified patients with suspected cases during house to-house case-finding efforts. Study physicians collected illness histories from either patients with suspected cases or their caregivers (when the patients were minors or decedents) using a standardized case report form. We also collected information from hospital records, if available. A 5-mL blood specimen was collected from each living patient with a suspected case, and the serum was transported to the International Centre for Diarrhoeal Disease Research, Bangladesh (Dhaka), on ice for storage at 70 C. Serum samples were then shipped to the Centers for Disease Control and Prevention (Atlanta, GA) for Nipah virus serologic 978 CID 2008:46 (1 April) Hossain et al.
3 Table 2. Relationship between onset of Nipah virus illness and seroconversion in patients with acute Nipah virus infection. No. of days after onset of Nipah virus illness Total collected No. of specimens IgM antibody positive IgG antibody positive years testing. Patients with suspected cases of Nipah virus infection who survived and had evidence of the infection, demonstrated by the presence of either IgM or IgG antibodies, were considered to have laboratory-confirmed cases. Patients with suspected cases who died during the outbreak, experienced fever with altered mental status, and were linked to patients with laboratory-confirmed cases by place of residence and timing of symptom onset were considered to have had probable cases of Nipah virus infection. Outbreaks of Nipah virus infection in Rajbari and Faridpur. The Rajbari and Faridpur cases were investigated while the outbreaks were ongoing. A similar definition for a suspected case (fever and headache or altered mental status) was used during these investigations. However, because many severely ill patients with suspected cases also presented with respiratory symptoms, patients with a history of cough and fever were also considered to have suspected cases. Patients with suspected cases of Nipah virus infection were identified by house-to-house and hospital visits in the affected area. Physicians working with the investigation team collected illness histories from patients with suspected cases or their caregivers (when the patients were minors, decedents, or unable to provide personal histories because of altered mental status) using a standardized case report form. They verified clinical information by physical examination of the surviving patients (when possible) and by reviewing hospital records (when available). Case-finding efforts were expanded to 7 northwestern districts from January through April Tertiary care hospitals in the region were visited, and all patients hospitalized with fever and altered mental status during this period were investigated. We identified 19 additional cases of Nipah virus infection during this effort; some were clustered, and some were isolated. We included these 19 cases with the cases identified in Rajbari District for this report, because the cases were identified beginning with the Rajbari outbreak in January. We obtained acute serum samples from all living patients with suspected Nipah virus infection and convalescent serum samples at least 10 days after onset of illness from patients surviving acute illness. In addition to blood samples, we obtained throat swab, urine, and when possible, CSF samples from hospitalized patients with altered mental status. Serum and CSF samples were assayed for the presence or absence of Nipah virus specific IgM and IgG antibodies, as described elsewhere [21]. CSF and throat swab specimens were tested for presence of Nipah virus RNA by RT-PCR using a primer set to detect the nucleocapsid gene, as described elsewhere [7]. Attempts were also made to isolate virus from CSF, throat swab, and urine specimens by placing 100 ul of specimen in cell culture, according to methods described elsewhere [7, 22]. The samples were transported and stored in the same manner as in the first 2 outbreaks. Patients with suspected cases who had evidence of Nipah Table 3. Analysis of CSF specimens from 6 patients with laboratory-confirmed Nipah virus infection in Patient Age, years WBC count, cells/mm 3 RBC count, cells/mm 3 Glucose level, a mmol/l Protein level, b mg/dl Culture result Outcome 1 10 c 1 2 No growth Died No growth Survived 3 35 d No growth Survived Not done Died 5 10 e No growth Survived 6 18 f 2500 Moderate No growth Died a Normal glucose level range, mmol/l. b Normal protein level range, mg/dl. c Virus isolated from a CSF specimen. d Virus isolated from a urine specimen. e Results of PCR of throat and CSF specimens were positive. f Results of PCR of urine and CSF specimens were positive. Clinical Presentation of Nipah Virus CID 2008:46 (1 April) 979
4 Table 4. Clinical features of Nipah virus infection in patients who died, compared with those who survived. Characteristic Age, years Patients who died a (n p 67) Patients who survived a (n p 25) OR (95% CI) P Mean SD b Median (range) 28 (2 60) 15 (4 50) Male sex 44/67 (66) 13/25 (52) 1.8 ( ).232 Altered mental status c 64/66 (97) 18/25 (72) 12.4 ( )!.001 Unconscious d 55/66 (83) 12/25 (48) 5.4 ( )!.001 Cough 44/65 (68) 12/25 (48) 2.3 ( ).084 Respiratory difficulty 52/65 (80) 10/25 (40) 6.0 ( )!.001 Vomiting 39/66 (59) 14/25 (56) 1.1 ( ).791 Convulsion 14/66 (21) 7/25 (28) 0.7 ( ).493 Headache 48/64 (75) 16/24 (67) 1.5 ( ).434 Severe weakness 38/55 (69) 13/21 (62) 1.4 ( ).551 Temperature C 27/30 (90) 4/9 (44) 11.2 ( ).003 Abnormal plantar response (diminished, extensor, or equivocal) 8/8 (100) 3/9 (50) Undefined (NA).004 Deep tendon reflex (absent or diminished) 3/5 (60) 6/9 (67) 0.75 ( ).803 NOTE. Data are proportion (%) of patients, unless otherwise indicated. NA, not applicable. a Difference in size of denominator is because of missing information or because the information was unknown or not collected. b P value by Mann-Whitney U test. c Altered mental status was defined as lack of orientation to time, place, and person. Unconsciousness was included as altered mental status. d Unconsciousness was defined as inability to give meaningful response to any stimuli. virus infection, demonstrated by the presence of Nipah virus IgM antibodies or by isolation of Nipah virus, were considered to have laboratory-confirmed cases [21]. Although other laboratory tests were performed, they were not considered to be reliable enough to use for the case definition. Patients with probable cases were those who had fever with altered mental status or breathing difficulty and whose cases were part of a cluster of laboratory-confirmed cases in the outbreak region; adequate specimens (including convalescent-phase specimens) for detection of Nipah virus antibodies could not be obtained from these patients because of fatal outcomes. Those with specimens (including convalescent-phase serum specimens) shown to be Nipah virus negative using all Nipah virus tests were considered to not be infected with Nipah virus. Statistical analysis. Clinical findings were contrasted between patients with fatal outcomes and patients who survived. Pearson s x 2 test or Fisher s exact test and univariate logistic regression were performed to determine ORs. Normally distributed continuous variables were analyzed using Student s t test, and nonnormally distributed continuous variables were analyzed using the Mann-Whitney U test. Associations were considered to be statistically significant at P!.05. Stata, version 8.0 (Stata), was used for statistical analysis. RESULTS We identified 92 patients with confirmed and probable cases of Nipah virus infection, including 13 patients in Meherpur, 12 in Naogaon, 31 in Rajbari (and other districts), and 36 in Faridpur. Forty-seven patients (51%) had laboratory-confirmed cases, 5 (5%; 4 from Meherpur and 1 from Naogaon) of whom were IgG positive only; all other patients with laboratory-confirmed cases ( n p 42) were IgM positive. Nipah virus was iso- lated from 4 patients (all of whom had detectable IgM antibodies to Nipah virus), and each isolate was identified by indirect fluorescent study test with Nipah virus antibodies and by RT-PCR [14]. Nipah virus was isolated from 2 patients associated with the third outbreak in Rajbari and 1 patient infected during the fourth outbreak in Faridpur; the fourth isolate was from a patient with an isolated case identified from Rajshahi District. Among 15 patients, all of whom had IgM antibodies, PCR results were positive for 8 throat swab, 6 urine, 5 CSF, and 4 saliva samples. Twenty-two (47%) of 47 laboratory confirmed-cases resulted in death. Of the 45 patients (49%) with probable cases, 41 (91%) died before collection of any specimens. Four patients had 1 specimen obtained during the early phase of illness (median time after onset of illness, 3.5 days; range, 2 5 days), and each patient had negative results of tests for Nipah virus and died before additional, potentially confirmatory specimens could be obtained. The age distribution of patients varied between outbreaks. The outbreaks in Naogaon (median patient age, 12 years; range, 4 42 years) and Rajbari (median patient age, 12 years; range, 2 50 years) occurred primarily among younger patients, com- 980 CID 2008:46 (1 April) Hossain et al.
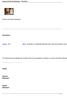
5 Figure 1. Chest radiographs for 4 patients, showing diffuse bilateral opacities covering majority of the lung fields, consistent with acute respiratory distress syndrome. pared with the outbreaks in Meherpur (median patient age, 38 years; range, 4 60 years) and Faridpur (median patient age, 35 years; range, 5 60 years). Fifty-seven (62%) patients were male; however, the proportion of male patients varied from 46% to 74% during the various outbreaks. Fever, required as part of the probable case definition, was universally (100%) present, followed by altered mental status (90%), headache (73%), severe weakness (67%), cough (62%), difficult breathing (69%), diarrhea (29%), and seizures (23%) (table 1). The clinical presentation started with mild-to-severe fever, followed by altered mental status (median time after onset of illness, 4 days; range, 0 10 days) or cough with respiratory difficulty (median time after onset of illness, 4 days; range, 0 13 days). Compared with the other outbreaks, during the Faridpur outbreak, respiratory difficulty was more common (75%) and seizures were less common (3%). The case-fatality rate was high (73%; range, 69% 75%). Most patients who died did so shortly after onset of illness (mean duration SD from onset of illness to death, days; median, 6 days; range, 2 36 days). In the Faridpur outbreak, during which most persons became infected through person-to-person transmission [19], a short, specific period of exposure could be determined for 11 patients who were exposed to only 1 infected patient for defined periods. Seven patients had a single close exposure (touched or were in the same room with an infected patient for at least 10 min) Clinical Presentation of Nipah Virus CID 2008:46 (1 April) 981
6 over the course of 1 day, and 4 had close exposures with a patient with Nipah virus infection during 2 consecutive days. On the basis of the exposure histories of these 11 patients, the median incubation period was 9 days (range, 6 11 days). During all 4 outbreaks, a total of 64 serum specimens were obtained from 51 patients. Two specimens were obtained from 13 patients; 23 patients died before a second sample could be obtained, and the remaining patients had only 1 specimen obtained after illness. We used antibody test results from all patients to assess the relationship between onset of symptoms and seroconversion (table 2). During the first 5 days of illness, 6 (66%) of 9 patients were IgM positive, and only 2 were IgG positive. By 2 weeks after symptom onset, all patients were IgM positive, and after 2 weeks, all patients were still IgG positive. Between 2 and 3 months after symptom onset, IgM antibody levels began to decrease, and after 2 years, no survivors were IgM positive, but 100% remained IgG positive. In total, 5 patients who were Nipah antibody negative when the first specimens were tested had detectable IgM antibodies in specimens obtained at least 2 weeks after the onset of illness. CSF specimens from 6 patients with confirmed Nipah virus infection were analyzed; 3 (50%) had a WBC count!5 cells/ mm 3. CSF glucose levels were within normal limits, and CSF protein levels were elevated in all patients except 1, who had normal levels. There was no bacterial growth yielded by any of the CSF cultures (table 3). Patients who died were significantly older (median age, 28 years; range, 2 60 years) than those who survived (median age, 15 years; range, 4 50 years; P p.018 ). Patients who died were more likely than survivors to have altered mental status (OR, 12.4; 95% CI, ), difficulty breathing (OR, 6.0; 95% CI, ), documented temperature C (OR, 11.2; 95% CI, ), and abnormal (diminished or extensor) planter reflexes (undefined OR; P p.004) (table 4). All surviving patients had laboratory-confirmed cases by definition, compared with 22 (33%) of 67 patients who died ( P!.001). Chest radiographs were performed for 5 patients from the Faridpur outbreak; all had a history of cough and difficulty breathing, and radiographic findings for all 5 were consistent with acute respiratory distress syndrome (figure 1). In patients with chest radiograph confirmed acute respiratory distress syndrome, respiratory symptoms (cough and difficulty breathing) started within 2 5 days after the onset of fever. All 5 patients with acute respiratory distress syndrome died. Only 1 patient who had severe respiratory difficulty received mechanical ventilation; a chest radiograph was not performed for this patient, and the patient died on day 17 of his illness. DISCUSSION There are important differences between the clinical descriptions of Nipah virus illness in Bangladesh and those from Malaysia. Cough or breathing difficulties were common during all of the first 4 outbreaks in Bangladesh and were particularly pronounced during the Faridpur outbreak. In the Faridpur outbreak, additional patients had respiratory symptoms similar to those experienced by the patients with documented acute respiratory distress syndrome, but chest radiographs were not performed because of the lack of facilities at treatment centers. In Malaysia and Singapore, respiratory symptoms were reported less frequently. Only 14% of Malaysian patients had a history of nonproductive cough [8], and 3 (27%) of 11 patients in Singapore had atypical pneumonia, along with abnormal chest radiographic findings [3, 4, 6, 23]. Respiratory symptoms were also common in patients during the outbreak in Siliguri, India in 2001, providing further evidence of a clinical presentation of Nipah virus infection in the southern Asian region that was different from the clinical presentation described in Malaysia [9]. Person-to-person transmission was documented during 1 outbreak in Faridpur [19] and was suggested in the Meherpur outbreak in Bangladesh [11]. Health care workers and hospital visitors were infected after exposure to hospitalized patients during the outbreak of Nipah virus infection in Siliguri, India, also suggesting person-to-person transmission [9]. The high prevalence of respiratory symptoms, especially cough, may have contributed to the transmissibility of Nipah virus infection from person to person that was observed in Bangladesh and Siliguri but not in Malaysia [5, 24, 25]. Coinfections with other respiratory pathogens have not been documented and were not systematically investigated. Genetic differences in Nipah virus strains between those isolated in Malaysia and those isolated in Bangladesh could explain the differences in clinical presentation observed, specifically the importance of respiratory symptoms in Bangladeshi patients [13, 26]. Because Nipah virus has been isolated from respiratory secretions of humans [27] and commonly causes pulmonary symptoms in other animals [28 30], it is plausible that some strains cause pulmonary symptoms in humans. Comparing sequence differences between patients with and without severe respiratory manifestations would help to evaluate this hypothesis. The case-fatality rate was higher in Bangladesh and Siliguri than in Malaysia. We found that clinical features, including respiratory symptoms, fever, and absence of plantar reflexes, were associated with death. In Bangladesh, the higher casefatality rate could be related to suboptimal health care. Diagnostic and supportive care facilities were limited in the areas affected by the outbreaks in Bangladesh. Other factors contributing to a higher case-fatality rate in Bangladesh may include any or a combination of the following: a more virulent Nipah virus genotype, exposure to secretions and/or excretions of patients with extremely high viral loads, and suppressed 982 CID 2008:46 (1 April) Hossain et al.
7 immunity, perhaps because of malnutrition (commonly seen in Bangladesh). WBC counts in CSF specimens were not elevated in 3 of 6 patients with Nipah virus infection, a finding similar to that for the Malaysian patients [8]. These findings suggest that normal WBC count and normal chemical parameters in CSF do not rule out Nipah virus infection in patients with encephalitis. There are several limitations to our study. The context of an investigation of an outbreak of Nipah virus infection in Bangladesh is challenging because of the quick progression from symptom onset to death, coupled with reluctance of sick patients to seek care and inadequate diagnostic infrastructure in health care facilities. For these reasons, many infected patients in Bangladesh were not hospitalized, and clinical evaluations were not performed. Even when hospital records were available, they were often incomplete. These challenges also produce delays in identification and investigation of outbreaks, which contributes to incomplete recall or recall bias by patients and/or relatives. This might have resulted in underreporting of some symptoms, especially when the recall time was long, as was the case for the Meherpur outbreak. In addition, because of delays in outbreak detection, the confirmed case definitions from the first and second outbreaks in Meherpur and Naogaon were based on the presence of IgG (rather than IgM) antibody to Nipah virus antigen. A case definition based on the presence of IgG antibody is reasonable, even if suboptimal, because all patients from these 2 outbreaks experienced encephalitis during a very specific period and in a specific geographic location. Although our case definition was based on the presence of IgG antibody, 3 of 4 patients with laboratory-confirmed cases who lived in Naogaon also had IgM antibodies, providing further evidence that presence of IgG antibodies is a reasonable indicator of past infection. In addition, there has been no evidence of another outbreak with similar impact in the area in the recent or more remote past; thus, previous exposure was unlikely. A third limitation is that our series may be biased toward more-severe cases, considering our reliance on hospital surveillance for case detection in many areas. However, door-todoor visits in areas where outbreaks occurred limited the effect of this bias. Asymptomatic infection was reported in 8% of patients with laboratory-confirmed cases in Malaysia [25]; however, there is no evidence of asymptomatic Nipah virus infection in Bangladesh during outbreaks, although cases of mild illness were identified. The findings of our investigation suggest that Nipah virus infections occurred in all age groups and that fever, altered mental status, cough, and respiratory symptoms were the most common symptoms among those infected in Bangladesh. Severe neurologic manifestations are consistently the most substantial and severe components of Nipah virus infection. Severe chronic sequelae occur in many survivors, adding to the significant public health burden of Nipah virus associated disease [31]. Future priorities should include ongoing surveillance and investigation of outbreaks of Nipah virus infection, identification and evaluation of strategies to prevent Nipah virus transmission, and improvement of clinical management of cases in resource-poor settings. Acknowledgments We thank the Centers for Disease Control and Prevention; World Health Organization; Institute of Epidemiology Disease Control and Research; Ministry of Health and Family Welfare, Bangladesh; Dr. Abu Taher Azad, Dr. Sultana Monira Hossain, and Dr. A. K. M. Saifuddin Ekram, for assistance in data collection; the study participants and their relatives; Mr. Milton Quiah, for administrative support; the Director and staff of the Dhaka, Faridpur, and Rajshahi Medical College Hospitals; and Dr. M. A. Salam, for his critical review of the manuscript. Financial support. Centers for Disease Control and Prevention, World Health Organization, and Ministry of Health and Family Welfare, Bangladesh. Potential conflicts of interest. All authors: no conflicts. References 1. Harcourt BH, Tamin A, Halpin K, et al. Molecular characterization of the polymerase gene and genomic termini of Nipah virus. Virology 2001; 287: Update: outbreak of Nipah virus Malaysia and Singapore, MMWR Morb Mortal Wkly Rep 1999; 48: Chew MH, Arguin PM, Shay DK, et al. Risk factors for Nipah virus infection among abattoir workers in Singapore. J Infect Dis 2000; 181: Chua KB. A novel approach for collecting samples from fruit bats for isolation of infectious agents. Microbes Infect 2003; 5: Parashar UD, Sunn LM, Ong F, et al. Case-control study of risk factors for human infection with a new zoonotic paramyxovirus, Nipah virus, during a outbreak of severe encephalitis in Malaysia. J Infect Dis 2000; 181: Chan KP, Rollin PE, Ksiazek TG, et al. A survey of Nipah virus infection among various risk groups in Singapore. Epidemiol Infect 2002; 128: Chua KB, Bellini WJ, Rota PA, et al. Nipah virus: a recently emergent deadly paramyxovirus. Science 2000; 288: Goh KJ, Tan CT, Chew NK, et al. Clinical features of Nipah virus encephalitis among pig farmers in Malaysia. N Engl J Med 2000; 342: Harit AK, Ichhpujani RL, Gupta S, et al. Nipah/Hendra virus outbreak in Siliguri, West Bengal, India in Indian J Med Res 2006; 123: Gurley ES, Montgomery JM, Hossain MJ, et al. Risk of nosocomial transmission of nipah virus in a Bangladesh hospital. Infect Control Hosp Epidemiol 2007; 28: Hsu VP, Hossain MJ, Parashar UD, et al. Nipah virus encephalitis reemergence, Bangladesh. Emerg Infect Dis 2004; 10: Luby SP, Rahman M, Hossain MJ, et al. Foodborne transmission of Nipah virus, Bangladesh. Emerg Infect Dis 2006; 12: AbuBakar S, Chang LY, Ali AR, Sharifah SH, Yusoff K, Zamrod Z. Isolation and molecular identification of Nipah virus from pigs. Emerg Infect Dis 2004; 10: Bellini WJ, Harcourt BH, Bowden N, Rota PA. Nipah virus: an emergent paramyxovirus causing severe encephalitis in humans. J Neurovirol 2005; 11: World Health Organization. Nipah virus. Wkly Epidemiol Rec 2002; 77: Clinical Presentation of Nipah Virus CID 2008:46 (1 April) 983
8 16. Nipah virus outbreak(s) in Bangladesh, January-April Wkly Epidemiol Rec 2004; 79: World Health Organization. Nipah-like virus, Bangladesh. Wkly Epidemiol Rec 2004; 79: ICDDR,B. Nipah encephalitis outbreak over wide area of western Bangladesh, Health and Science Bulletin 2004; 2: Gurley ES, Montgomery JM, Hossain MJ, et al. Person-to-person transmission of Nipah virus in a Bangladeshi community. Emerg Infect Dis 2007; 13: Quddus R, Alam S, Majumdar MA, et al. A report of 4 patients with Nipah encephalitis from Rajbari district, Bangladesh in the January 2004 outbreak. Neurol Asia 2004; 9: Daniels P, Ksiazek T, Eaton BT. Laboratory diagnosis of Nipah and Hendra virus infections. Microbes Infect 2001; 3: Chan YP, Chua KB, Koh CL, Lim ME, Lam SK. Complete nucleotide sequences of Nipah virus isolates from Malaysia. J Gen Virol 2001; 82: Lee KE, Umapathi T, Tan CB, et al. The neurological manifestations of Nipah virus encephalitis, a novel paramyxovirus. Ann Neurol 1999; 46: Mounts AW, Kaur H, Parashar UD, et al. A cohort study of health care workers to assess nosocomial transmissibility of Nipah virus, Malaysia, J Infect Dis 2001; 183: Tan KS, Tan CT, Goh KJ. Epidemiological aspects of Nipah virus infection. Neurol J Southeast Asia 1999; 4: Harcourt BH, Lowe L, Tamin A, et al. Genetic characterization of Nipah virus, Bangladesh, Emerg Infect Dis 2005; 11: Chua KB, Lam SK, Goh KJ, et al. The presence of Nipah virus in respiratory secretions and urine of patients during an outbreak of Nipah virus encephalitis in Malaysia. J Infect 2001; 42: Murray K, Selleck P, Hooper P, et al. A morbillivirus that caused fatal disease in horses and humans. Science 1995; 268: Selvey LA, Wells RM, McCormack JG, et al. Infection of humans and horses by a newly described morbillivirus. Med J Aust 1995; 162: Mohd Nor MN, Gan CH, Ong BL. Nipah virus infection of pigs in peninsular Malaysia. Rev Sci Tech 2000; 19: Sejvar JJ, Hossain J, Saha SK, et al. Long-term neurological and functional outcome in Nipah virus infection. Ann Neurol 2007; 62: CID 2008:46 (1 April) Hossain et al.
Patients with asymptomatic Nipah virus infection may have abnormal cerebral MR imaging
 Neurol J Southeast Asia 2000; 5 : 69 73 Patients with asymptomatic Nipah virus infection may have abnormal cerebral MR imaging Kay-Sin TAN, *Sazilah AHMAD SARJI, Chong-Tin TAN, *Basri Johan Jeet ABDULLAH,
Neurol J Southeast Asia 2000; 5 : 69 73 Patients with asymptomatic Nipah virus infection may have abnormal cerebral MR imaging Kay-Sin TAN, *Sazilah AHMAD SARJI, Chong-Tin TAN, *Basri Johan Jeet ABDULLAH,
Ten year clinical and serological outcomes of Nipah virus infection
 Neurology Asia 2009; 14 : 53 58 Ten year clinical and serological outcomes of Nipah virus infection SR Siva, HT Chong, CT Tan Division of Neurology, Faculty of Medicine, University of Malaya, Kuala Lumpur,
Neurology Asia 2009; 14 : 53 58 Ten year clinical and serological outcomes of Nipah virus infection SR Siva, HT Chong, CT Tan Division of Neurology, Faculty of Medicine, University of Malaya, Kuala Lumpur,
Nipah Virus outbreak in the World
 International Journal of Advanced Research in Biological Sciences ISSN: 2348-8069 www.ijarbs.com DOI: 10.22192/ijarbs Coden: IJARQG(USA) Volume 5, Issue 9-2018 Review Article DOI: http://dx.doi.org/10.22192/ijarbs.2018.05.09.013
International Journal of Advanced Research in Biological Sciences ISSN: 2348-8069 www.ijarbs.com DOI: 10.22192/ijarbs Coden: IJARQG(USA) Volume 5, Issue 9-2018 Review Article DOI: http://dx.doi.org/10.22192/ijarbs.2018.05.09.013
Statistical Analysis of Nipah Virus Using R
 RESEARCH ARTICLE Statistical Analysis of Nipah Virus Using R Roopa Sri Paladugu 1, Sruthi Chilukuri 2, Dr.Sangeetha Yalamanchili 3 1(Department of IT, V.R.Siddhartha Engineering College, and Vijayawada)
RESEARCH ARTICLE Statistical Analysis of Nipah Virus Using R Roopa Sri Paladugu 1, Sruthi Chilukuri 2, Dr.Sangeetha Yalamanchili 3 1(Department of IT, V.R.Siddhartha Engineering College, and Vijayawada)
EFFECTS OF NIPAH VIRUS IN TODAY S WORLD
 EFFECTS OF NIPAH VIRUS IN TODAY S WORLD Available online at www.ijistweb.com REVIEW ARTICLE Dhiraj Kumar Singh*, Rakhi Ahuja, Nagendra Kumar Singh Delhi Pharmaceutical Sciences and Research University,
EFFECTS OF NIPAH VIRUS IN TODAY S WORLD Available online at www.ijistweb.com REVIEW ARTICLE Dhiraj Kumar Singh*, Rakhi Ahuja, Nagendra Kumar Singh Delhi Pharmaceutical Sciences and Research University,
EMERGING DISEASES ASSOCIATED WITH FLYING FOXES HOST MANAGEMENT STRATEGIES
 EMERGING DISEASES ASSOCIATED WITH FLYING FOXES HOST MANAGEMENT STRATEGIES Hume Field Department of Primary Industries & Fisheries Queensland Email: hume.field@dpi.qld.gov.au Introduction Several novel
EMERGING DISEASES ASSOCIATED WITH FLYING FOXES HOST MANAGEMENT STRATEGIES Hume Field Department of Primary Industries & Fisheries Queensland Email: hume.field@dpi.qld.gov.au Introduction Several novel
Hendra virus: Important information for all horse owners. An update on Hendra virus The Hendra vaccine
 Hendra virus: Important information for all horse owners An update on Hendra virus The Hendra vaccine HENDRA VIRUS Welcome to the Hendra virus information update The aim of this update is to provide information
Hendra virus: Important information for all horse owners An update on Hendra virus The Hendra vaccine HENDRA VIRUS Welcome to the Hendra virus information update The aim of this update is to provide information
Jones & Bartlett Learning, LLC. NOT FOR SALE OR DISTRIBUTION
 Chapter 8 Every culture has its own customs, recreational activities, crafts, and cuisine. In this viral encounter, a local delicacy becomes contaminated with a new and deadly virus that emerged from Malaysia.
Chapter 8 Every culture has its own customs, recreational activities, crafts, and cuisine. In this viral encounter, a local delicacy becomes contaminated with a new and deadly virus that emerged from Malaysia.
The Prevalence of Nelson Bay Virus in Humans and Bats and its Significance within the Framework of Conservation Medicine
 Georgia State University ScholarWorks @ Georgia State University Public Health Theses School of Public Health 7-23-2007 The Prevalence of Nelson Bay Virus in Humans and Bats and its Significance within
Georgia State University ScholarWorks @ Georgia State University Public Health Theses School of Public Health 7-23-2007 The Prevalence of Nelson Bay Virus in Humans and Bats and its Significance within
Surveillance of animal brucellosis
 Surveillance of animal brucellosis Assoc.Prof.Dr. Theera Rukkwamsuk Department of large Animal and Wildlife Clinical Science Faculty of Veterinary Medicine Kasetsart University Review of the epidemiology
Surveillance of animal brucellosis Assoc.Prof.Dr. Theera Rukkwamsuk Department of large Animal and Wildlife Clinical Science Faculty of Veterinary Medicine Kasetsart University Review of the epidemiology
Nipah Virus Infection
 Nipah Virus Infection Porcine Respiratory and Encephalitis Syndrome, Porcine Respiratory and Neurologic Syndrome, Barking Pig Syndrome Last Updated: November 9, 2007 Importance Nipah virus infection is
Nipah Virus Infection Porcine Respiratory and Encephalitis Syndrome, Porcine Respiratory and Neurologic Syndrome, Barking Pig Syndrome Last Updated: November 9, 2007 Importance Nipah virus infection is
Nipah Encephalitis An Update
 Sherrini Bazir Ahmad, MRCP, Chong Tin Tan, FRCP Neurology, Department of Medicine, University of Malaya, Kuala Lumpur, Malaysia. SUMMARY Between September 1998 to May 1999, Malaysia and Singapore were
Sherrini Bazir Ahmad, MRCP, Chong Tin Tan, FRCP Neurology, Department of Medicine, University of Malaya, Kuala Lumpur, Malaysia. SUMMARY Between September 1998 to May 1999, Malaysia and Singapore were
Animal reservoirs for Nipah virus
 Animal reservoirs for Nipah virus Dr. D. T. Mourya ICMR-National Institute of Virology Pune 411021, INDIA Tracing the source of Infection ICMR-NIV, Pune has team of scientific experts and trained field
Animal reservoirs for Nipah virus Dr. D. T. Mourya ICMR-National Institute of Virology Pune 411021, INDIA Tracing the source of Infection ICMR-NIV, Pune has team of scientific experts and trained field
Chanchal et al., IJPSR, 2018; Vol. 9(8): E-ISSN: ; P-ISSN:
 IJPSR (208), Volume 9, Issue 8 (Review Article) Received on 27 November, 207; received in revised form, 3 February, 208; accepted, 2 June, 208; published 0 August, 208 NIPAH: SILENTLY RISING INFECTION
IJPSR (208), Volume 9, Issue 8 (Review Article) Received on 27 November, 207; received in revised form, 3 February, 208; accepted, 2 June, 208; published 0 August, 208 NIPAH: SILENTLY RISING INFECTION
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan. Associate Consultant Infectious Disease Centre, PMH
 Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
Does history-taking help predict rabies diagnosis in dogs?
 Asian Biomedicine Vol. 4 No. 5 October 2010; 811-815 Brief communication (original) Does history-taking help predict rabies diagnosis in dogs? Veera Tepsumethanon, Boonlert Lumlertdacha, Channarong Mitmoonpitak
Asian Biomedicine Vol. 4 No. 5 October 2010; 811-815 Brief communication (original) Does history-taking help predict rabies diagnosis in dogs? Veera Tepsumethanon, Boonlert Lumlertdacha, Channarong Mitmoonpitak
GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS
 Version 3.1 GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS Date ratified June 2008 Updated March 2009 Review date June 2010 Ratified by Authors Consultation Evidence base Changes
Version 3.1 GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS Date ratified June 2008 Updated March 2009 Review date June 2010 Ratified by Authors Consultation Evidence base Changes
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Brucellosis in Kyrgyzstan
 Centers for Disease Control and Prevention Case Studies in Applied Epidemiology No. 053-D11 Brucellosis in Kyrgyzstan Participant's Guide Learning Objectives After completing this case study, the participant
Centers for Disease Control and Prevention Case Studies in Applied Epidemiology No. 053-D11 Brucellosis in Kyrgyzstan Participant's Guide Learning Objectives After completing this case study, the participant
Standard Operating Procedure for Rabies. November Key facts
 Standard Operating Procedure for Rabies November 2011 Key facts Rabies occurs in more than 150 countries and territories. Dogs are the source of 99% of human rabies deaths. Worldwide, more than 55 000
Standard Operating Procedure for Rabies November 2011 Key facts Rabies occurs in more than 150 countries and territories. Dogs are the source of 99% of human rabies deaths. Worldwide, more than 55 000
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Nipah Virus Research: A Scientometric Assessment of Global Publications Output during
 Int J Med. Public Health. 2018; 8(2):48-55 A Multifaceted Peer Reviewed Journal in the field of Medicine and Public Health www.ijmedph.org www.journalonweb.com/ijmedph Invited Article Nipah Virus Research:
Int J Med. Public Health. 2018; 8(2):48-55 A Multifaceted Peer Reviewed Journal in the field of Medicine and Public Health www.ijmedph.org www.journalonweb.com/ijmedph Invited Article Nipah Virus Research:
P<0.05 ٢٠٠٧ ٣ ﺩﺪﻌﻟﺍ ﺮﺸﻋ ﺚﻟﺎﺜﻟﺍ ﺪﻠﺠﳌﺍ ﺔﻴﳌﺎﻌﻟﺍ ﺔﺤﺼﻟﺍ ﺔﻤﻈﻨﻣ ﻂﺳﻮﺘﳌﺍ ﻕﺮﺸﻟ ﺔﻴﺤﺼﻟﺍ ﺔﻠﺠﳌﺍ
 72 144 P
72 144 P
Nipah Virus Outbreak Investigation in Kerala, India
 Nipah Virus Outbreak Investigation in Kerala, India 1 Introduction Nipah virus infection was first identified in Sept, 1998 in Ipoh, Malaysia In Malaysia & Singapore, most cases were in individuals handling
Nipah Virus Outbreak Investigation in Kerala, India 1 Introduction Nipah virus infection was first identified in Sept, 1998 in Ipoh, Malaysia In Malaysia & Singapore, most cases were in individuals handling
Defense Technical Information Center
 UNCLASSIFIED Defense Technical Information Center Compilation Part Notice ADP013384 TITLE: Evaluation of Nipah Virus as a Human and Animal Biological Terrorism and Warfare Agent DISTRIBUTION: Approved
UNCLASSIFIED Defense Technical Information Center Compilation Part Notice ADP013384 TITLE: Evaluation of Nipah Virus as a Human and Animal Biological Terrorism and Warfare Agent DISTRIBUTION: Approved
Canine and Feline Distemper. Description. The following chart indicates the animals which are susceptible to infection by canine and feline distemp
 Canine and Feline Distemper Description Canine and feline distemper are diseases affecting many wild and domestic carnivo The following chart indicates the animals which are susceptible to infection by
Canine and Feline Distemper Description Canine and feline distemper are diseases affecting many wild and domestic carnivo The following chart indicates the animals which are susceptible to infection by
ESBL Positive E. coli and K. pneumoneae are Emerging as Major Pathogens for Urinary Tract Infection
 ESBL Positive E. coli and K. pneumoneae are Emerging as Major Pathogens for Urinary Tract Infection Muhammad Abdur Rahim*, Palash Mitra*. Tabassum Samad*. Tufayel Ahmed Chowdhury*. Mehruba Alam Ananna*.
ESBL Positive E. coli and K. pneumoneae are Emerging as Major Pathogens for Urinary Tract Infection Muhammad Abdur Rahim*, Palash Mitra*. Tabassum Samad*. Tufayel Ahmed Chowdhury*. Mehruba Alam Ananna*.
Suggested vector-borne disease screening guidelines
 Suggested vector-borne disease screening guidelines SNAP Dx Test Screen your dog every year with the SNAP Dx Test to detect exposure to pathogens that cause heartworm disease, ehrlichiosis, Lyme disease
Suggested vector-borne disease screening guidelines SNAP Dx Test Screen your dog every year with the SNAP Dx Test to detect exposure to pathogens that cause heartworm disease, ehrlichiosis, Lyme disease
Bacterial Pneumonia in Sheep, The Domestic Bighorn Sheep Interface, and Research at ADRU
 Bacterial Pneumonia in Sheep, The Domestic Bighorn Sheep Interface, and Research at ADRU USAHA Committee on Sheep and Goats Providence, RI October 27, 2015 PLC M. A. Highland, DVM, DACVP, PhD candidate
Bacterial Pneumonia in Sheep, The Domestic Bighorn Sheep Interface, and Research at ADRU USAHA Committee on Sheep and Goats Providence, RI October 27, 2015 PLC M. A. Highland, DVM, DACVP, PhD candidate
Hendra virus: what do we know?
 Hendra virus: what do we know? Isabel M. R. Hess A,E, Peter D. Massey B, Belinda Walker C, Deborah J. Middleton D and Therese M. Wright C A NSW Public Health Officer Training Program, NSW Department of
Hendra virus: what do we know? Isabel M. R. Hess A,E, Peter D. Massey B, Belinda Walker C, Deborah J. Middleton D and Therese M. Wright C A NSW Public Health Officer Training Program, NSW Department of
International Contribution to Nipah Virus Research
 Malaysian Journal of Library & Information Science, Vol. 17, no. 3, December 2012: 35-47 International Contribution to Nipah Virus Research 1999-2010 H. Safahieh 1, S.A. Sanni 1, A.N. Zainab 1,2 1 Department
Malaysian Journal of Library & Information Science, Vol. 17, no. 3, December 2012: 35-47 International Contribution to Nipah Virus Research 1999-2010 H. Safahieh 1, S.A. Sanni 1, A.N. Zainab 1,2 1 Department
Animal Bites and Rabies
 Animal Bites and Rabies Animal bites Animal bites are not rare and can occur anywhere in the world. They can occur while: walking in the street jogging in the woods bicycle riding in the countryside or
Animal Bites and Rabies Animal bites Animal bites are not rare and can occur anywhere in the world. They can occur while: walking in the street jogging in the woods bicycle riding in the countryside or
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Veterinary Epidemiology Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2016 Veterinary Epidemiology Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2016 Veterinary Epidemiology Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal
Guidance Document. Pig Semen PIGSEMEN.GEN. [Document Date] A guidance document issued by the Ministry for Primary Industries
![Guidance Document. Pig Semen PIGSEMEN.GEN. [Document Date] A guidance document issued by the Ministry for Primary Industries Guidance Document. Pig Semen PIGSEMEN.GEN. [Document Date] A guidance document issued by the Ministry for Primary Industries](/thumbs/95/122495953.jpg) Guidance Document Pig Semen PIGSEMEN.GEN A guidance document issued by the Ministry for Primary Industries Title About this document This guidance document contains information about acceptable ways of
Guidance Document Pig Semen PIGSEMEN.GEN A guidance document issued by the Ministry for Primary Industries Title About this document This guidance document contains information about acceptable ways of
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal viscera, examination of, in investigation of emerging infectious diseases of food animals, 6 American Veterinary Medical Association,
Index Note: Page numbers of article titles are in boldface type. A Abdominal viscera, examination of, in investigation of emerging infectious diseases of food animals, 6 American Veterinary Medical Association,
INFECTIOUS HEPATITIS, PARVOVIRUS & DISTEMPER
 Canine VacciCheck INFECTIOUS HEPATITIS, PARVOVIRUS & DISTEMPER IgG ANTIBODY TEST KIT INSTRUCTION MANUAL Sufficient for 12/120 assays 13 JUL 2015 Biogal Galed Laboratories Acs. Ltd., tel: 972-4-9898605.
Canine VacciCheck INFECTIOUS HEPATITIS, PARVOVIRUS & DISTEMPER IgG ANTIBODY TEST KIT INSTRUCTION MANUAL Sufficient for 12/120 assays 13 JUL 2015 Biogal Galed Laboratories Acs. Ltd., tel: 972-4-9898605.
Final 2009 West Nile Virus Activity in the United States
 Final West Nile Virus Activity in the United s Washington West Nile Virus Activity in the United s West Nile Virus Activity in the United s Final West Nile Virus Activity in the United s Delaware Rhode
Final West Nile Virus Activity in the United s Washington West Nile Virus Activity in the United s West Nile Virus Activity in the United s Final West Nile Virus Activity in the United s Delaware Rhode
OIE Collaborating Centres Reports Activities
 OIE Collaborating Centres Reports Activities Activities in 2015 This report has been submitted : 2016-03-24 20:54:12 Title of collaborating centre: Emerging and Re-Emerging Zoonotic Diseases Address of
OIE Collaborating Centres Reports Activities Activities in 2015 This report has been submitted : 2016-03-24 20:54:12 Title of collaborating centre: Emerging and Re-Emerging Zoonotic Diseases Address of
Three patients with fever and rash after a stay in Morocco: infection with Rickettsia conorii
 Three patients with fever and rash after a stay in Morocco: infection with Rickettsia conorii Stylemans D 1, Mertens R 1, Seyler L 1, Piérard D 2, Lacor P 1 1. Department of Internal Medicine, UZ Brussel
Three patients with fever and rash after a stay in Morocco: infection with Rickettsia conorii Stylemans D 1, Mertens R 1, Seyler L 1, Piérard D 2, Lacor P 1 1. Department of Internal Medicine, UZ Brussel
EPIDEMIOLOGY OF CAMPYLOBACTER IN IRELAND
 EPIDEMIOLOGY OF CAMPYLOBACTER IN IRELAND Table of Contents Acknowledgements 3 Summary 4 Introduction 5 Case Definitions 6 Materials and Methods 7 Results 8 Discussion 13 References 14 Epidemiology of Campylobacteriosis
EPIDEMIOLOGY OF CAMPYLOBACTER IN IRELAND Table of Contents Acknowledgements 3 Summary 4 Introduction 5 Case Definitions 6 Materials and Methods 7 Results 8 Discussion 13 References 14 Epidemiology of Campylobacteriosis
Review Article Pathology of Acute Henipavirus Infection in Humans and Animals
 SAGE-Hindawi Access to Research Pathology Research International Volume 2011, Article ID 567248, 12 pages doi:10.4061/2011/567248 Review Article Pathology of Acute Henipavirus Infection in Humans and Animals
SAGE-Hindawi Access to Research Pathology Research International Volume 2011, Article ID 567248, 12 pages doi:10.4061/2011/567248 Review Article Pathology of Acute Henipavirus Infection in Humans and Animals
READER S DIGEST OVERVIEW: BIGHORN SHEEP. Peregrine Wolff, DVM
 READER S DIGEST OVERVIEW: RESPIRATORY DISEASE IN BIGHORN SHEEP Peregrine Wolff, DVM Nevada Department of Wildlife During the Lewis & Clark expedition (1804 1806) There may have been 2 million bighorn sheep
READER S DIGEST OVERVIEW: RESPIRATORY DISEASE IN BIGHORN SHEEP Peregrine Wolff, DVM Nevada Department of Wildlife During the Lewis & Clark expedition (1804 1806) There may have been 2 million bighorn sheep
WHO Guideline for Management of Possible Serious Bacterial Infection (PSBI) in neonates and young infants where referral is not feasible
 WHO Guideline for Management of Possible Serious Bacterial Infection (PSBI) in neonates and young infants where referral is not feasible Department of Maternal, Newborn, Child & Adolescent Health Newborn
WHO Guideline for Management of Possible Serious Bacterial Infection (PSBI) in neonates and young infants where referral is not feasible Department of Maternal, Newborn, Child & Adolescent Health Newborn
Coccidioidomycosis Nothing to disclose
 Coccidioidomycosis Nothing to disclose Disclosure Greg Melcher, M.D. Professor of Clinical Medicine Division of HIV, ID and Global Medicine Zuckerman San Francisco General Hospital University of California,
Coccidioidomycosis Nothing to disclose Disclosure Greg Melcher, M.D. Professor of Clinical Medicine Division of HIV, ID and Global Medicine Zuckerman San Francisco General Hospital University of California,
MANAGEMENT OF DOMESTIC ANIMAL RABIES EXPOSURES NEW JERSEY DEPARTMENT OF HEALTH March 2016
 MANAGEMENT OF DOMESTIC ANIMAL RABIES EXPOSURES NEW JERSEY DEPARTMENT OF HEALTH March 2016 Authority: New Jersey law requires that whenever a dog, cat, or other animal has been known or suspected to have
MANAGEMENT OF DOMESTIC ANIMAL RABIES EXPOSURES NEW JERSEY DEPARTMENT OF HEALTH March 2016 Authority: New Jersey law requires that whenever a dog, cat, or other animal has been known or suspected to have
ANIMALS AFFECTED WHAT IS RABIES? INCIDENCE AND DISTRIBUTION NEED TO KNOW INFORMATION FOR RABIES: AGRICULTURAL PRODUCERS
 Distributed by: Fact Sheet No. 19 Revised December 2013 THE AGRICULTURAL HEALTH & SAFETY NEED TO KNOW INFORMATION FOR RABIES: AGRICULTURAL PRODUCERS WHAT IS RABIES? Rabies is a disease caused by a virus
Distributed by: Fact Sheet No. 19 Revised December 2013 THE AGRICULTURAL HEALTH & SAFETY NEED TO KNOW INFORMATION FOR RABIES: AGRICULTURAL PRODUCERS WHAT IS RABIES? Rabies is a disease caused by a virus
Asian Journal of Medical and Biological Research ISSN (Print) (Online)
 Asian J. Med. Biol. Res. 2015, 1 (2), 350-358; doi: 10.3329/ajmbr.v1i2.25629 Asian Journal of Medical and Biological Research ISSN 2411-4472 (Print) 2412-5571 (Online) www.ebupress.com/journal/ajmbr Article
Asian J. Med. Biol. Res. 2015, 1 (2), 350-358; doi: 10.3329/ajmbr.v1i2.25629 Asian Journal of Medical and Biological Research ISSN 2411-4472 (Print) 2412-5571 (Online) www.ebupress.com/journal/ajmbr Article
Typhoid fever - priorities for research and development of new treatments
 Typhoid fever - priorities for research and development of new treatments Isabela Ribeiro, Manica Balasegaram, Christopher Parry October 2017 Enteric infections Enteric infections vary in symptoms and
Typhoid fever - priorities for research and development of new treatments Isabela Ribeiro, Manica Balasegaram, Christopher Parry October 2017 Enteric infections Enteric infections vary in symptoms and
Parvovirus Type 2c An Emerging Pathogen in Dogs. Sanjay Kapil, DVM, MS, PhD Professor Center for Veterinary Health Sciences OADDL Stillwater, OK
 Parvovirus Type 2c An Emerging Pathogen in Dogs Sanjay Kapil, DVM, MS, PhD Professor Center for Veterinary Health Sciences OADDL Stillwater, OK Properties of Canine Parvovirus Single-stranded DNA virus
Parvovirus Type 2c An Emerging Pathogen in Dogs Sanjay Kapil, DVM, MS, PhD Professor Center for Veterinary Health Sciences OADDL Stillwater, OK Properties of Canine Parvovirus Single-stranded DNA virus
ANTHRAX. INHALATION, INTESTINAL and CUTANEOUS ANTHRAX
 INHALATION, INTESTINAL and CUTANEOUS ANTHRAX CPMP/4048/01, rev. 3 1/7 General points on treatment Anthrax is an acute infectious disease caused by Bacillus anthracis, that may be infecting man via cutaneous
INHALATION, INTESTINAL and CUTANEOUS ANTHRAX CPMP/4048/01, rev. 3 1/7 General points on treatment Anthrax is an acute infectious disease caused by Bacillus anthracis, that may be infecting man via cutaneous
Henipavirus: A Review of Laboratory Animal Pathology
 Special Focus: Research Challenges and Animal Models in Biological Defense Henipavirus: A Review of Laboratory Animal Pathology Veterinary Pathology 47(5) 871-880 ª The American College of Veterinary Pathologists
Special Focus: Research Challenges and Animal Models in Biological Defense Henipavirus: A Review of Laboratory Animal Pathology Veterinary Pathology 47(5) 871-880 ª The American College of Veterinary Pathologists
Antibiotic stewardship in long term care
 Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Zoonotic Diseases. Risks of working with wildlife. Maria Baron Palamar, Wildlife Veterinarian
 Zoonotic Diseases Risks of working with wildlife www.cdc.gov Definition Zoonoses: infectious diseases of vertebrate animals that can be naturally transmitted to humans Health vs. Disease Transmission -
Zoonotic Diseases Risks of working with wildlife www.cdc.gov Definition Zoonoses: infectious diseases of vertebrate animals that can be naturally transmitted to humans Health vs. Disease Transmission -
Canine Distemper Virus
 Photo: LE Carmichael, MJ Appel Photo: LE Carmichael, MJ Appel Photo: LE Carmichael, MJ Appel Canine Distemper Virus Canine Distemper (CD) is a highly contagious infectious disease of dogs worldwide caused
Photo: LE Carmichael, MJ Appel Photo: LE Carmichael, MJ Appel Photo: LE Carmichael, MJ Appel Canine Distemper Virus Canine Distemper (CD) is a highly contagious infectious disease of dogs worldwide caused
Taking the Teeth Out of Canine Distemper Virus July 21, 2016
 Taking the Teeth Out of Canine Distemper Virus Sandra Newbury, DVM Director University of Wisconsin-Madison Shelter Medicine Program UW School of Veterinary Medicine www.uwsheltermedicine.com Many thanks
Taking the Teeth Out of Canine Distemper Virus Sandra Newbury, DVM Director University of Wisconsin-Madison Shelter Medicine Program UW School of Veterinary Medicine www.uwsheltermedicine.com Many thanks
11-ID-10. Committee: Infectious Disease. Title: Creation of a National Campylobacteriosis Case Definition
 11-ID-10 Committee: Infectious Disease Title: Creation of a National Campylobacteriosis Case Definition I. Statement of the Problem Although campylobacteriosis is not nationally-notifiable, it is a disease
11-ID-10 Committee: Infectious Disease Title: Creation of a National Campylobacteriosis Case Definition I. Statement of the Problem Although campylobacteriosis is not nationally-notifiable, it is a disease
Outlines. Introduction Prevalence Resistance Clinical presentation Diagnosis Management Prevention Case presentation Achievements
 Amal Meas Al-Anizi, PharmD Candidate KSU, Infectious Disease Rotation 2014 Outlines Introduction Prevalence Resistance Clinical presentation Diagnosis Management Prevention Case presentation Achievements
Amal Meas Al-Anizi, PharmD Candidate KSU, Infectious Disease Rotation 2014 Outlines Introduction Prevalence Resistance Clinical presentation Diagnosis Management Prevention Case presentation Achievements
Central Nervous System Infections
 Central Nervous System Infections Meningitis Treatment Bacterial meningitis is a MEDICAL EMERGENCY. ANTIBIOTICS SHOULD BE STARTED AS SOON AS THE POSSIBILITY OF BACTERIAL MENINGITIS BECOMES EVIDENT, IDEALLY
Central Nervous System Infections Meningitis Treatment Bacterial meningitis is a MEDICAL EMERGENCY. ANTIBIOTICS SHOULD BE STARTED AS SOON AS THE POSSIBILITY OF BACTERIAL MENINGITIS BECOMES EVIDENT, IDEALLY
Epidemiological profile of Bite Cases Admitted at a 50 bedded Community Health Centre of Himachal Pradesh, India
 ISPUB.COM The Internet Journal of Health Volume 7 Number 1 Epidemiological profile of Bite Cases Admitted at a 50 bedded Community Health Centre of Himachal Pradesh, India S Goel, H Gupta, S Mazta Citation
ISPUB.COM The Internet Journal of Health Volume 7 Number 1 Epidemiological profile of Bite Cases Admitted at a 50 bedded Community Health Centre of Himachal Pradesh, India S Goel, H Gupta, S Mazta Citation
Outbreaks Due to Unpasteurized Dairy Products in the United States
 Outbreaks Due to Unpasteurized Dairy Products in the United States Casey Barton Behravesh, DVM, DrPH, DACVPM LCDR, US Public Health Service Enteric Diseases Epidemiology Branch National Center for Zoonotic,
Outbreaks Due to Unpasteurized Dairy Products in the United States Casey Barton Behravesh, DVM, DrPH, DACVPM LCDR, US Public Health Service Enteric Diseases Epidemiology Branch National Center for Zoonotic,
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC
 Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC APPROVED BY: Policy and Guidelines Committee TRUST REFERENCE: B9/2009 AWP Ref: AWP61 Date (approved): July 2008 REVIEW
Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC APPROVED BY: Policy and Guidelines Committee TRUST REFERENCE: B9/2009 AWP Ref: AWP61 Date (approved): July 2008 REVIEW
Human Rabies Post-Exposure Prophylaxis and Animal Rabies in Ontario,
 Human Rabies Post-Exposure Prophylaxis and Animal Rabies in Ontario, 2001 2012 PHO Grand Rounds Tuesday April 21, 2015 Dean Middleton Enteric, Zoonotic and Vector-Borne Diseases Unit Outline Introduction
Human Rabies Post-Exposure Prophylaxis and Animal Rabies in Ontario, 2001 2012 PHO Grand Rounds Tuesday April 21, 2015 Dean Middleton Enteric, Zoonotic and Vector-Borne Diseases Unit Outline Introduction
SURVEILLANCE IN ACTION: Introduction, Techniques and Strategies
 SURVEILLANCE IN ACTION: Introduction, Techniques and Strategies Dr. Scott McBurney Wildlife Pathologist, Canadian Cooperative Wildlife Health Centre Training Workshop for OIE National Focal Points for
SURVEILLANCE IN ACTION: Introduction, Techniques and Strategies Dr. Scott McBurney Wildlife Pathologist, Canadian Cooperative Wildlife Health Centre Training Workshop for OIE National Focal Points for
Informing Public Policy on Agricultural Use of Antimicrobials in the United States: Strategies Developed by an NGO
 Informing Public Policy on Agricultural Use of Antimicrobials in the United States: Strategies Developed by an NGO Stephen J. DeVincent, DVM, MA Director, Ecology Program Alliance for the Prudent Use of
Informing Public Policy on Agricultural Use of Antimicrobials in the United States: Strategies Developed by an NGO Stephen J. DeVincent, DVM, MA Director, Ecology Program Alliance for the Prudent Use of
OIE RL for Rabies in China: Activities and Challenges
 OIE RL for Rabies in China: Activities and Challenges Email: changchun_tu@hotmail.com http://cvrirabies.bmi.ac.cn Diagnostic Laboratory on Rabies and Wildlife Associated Zoonoses (DLR), Chinese Ministry
OIE RL for Rabies in China: Activities and Challenges Email: changchun_tu@hotmail.com http://cvrirabies.bmi.ac.cn Diagnostic Laboratory on Rabies and Wildlife Associated Zoonoses (DLR), Chinese Ministry
Infection Control and Standard Precautions
 Home Care Aide Training Guide Infection Control and Standard Precautions Pre-Service Training Course #1 Home Care Aide Orientation Training Manual: Infection Control & Standard Precautions Page 2 Table
Home Care Aide Training Guide Infection Control and Standard Precautions Pre-Service Training Course #1 Home Care Aide Orientation Training Manual: Infection Control & Standard Precautions Page 2 Table
BOVINE RESPIRATORY DISEASE COMPLEX. Kristen Mierzwiak LCS 630
 BOVINE RESPIRATORY DISEASE COMPLEX Kristen Mierzwiak LCS 630 Ring... You are called out to the farm of one of your regular dairy clients because some of the replacement heifers they bought at a public
BOVINE RESPIRATORY DISEASE COMPLEX Kristen Mierzwiak LCS 630 Ring... You are called out to the farm of one of your regular dairy clients because some of the replacement heifers they bought at a public
Global Perspective of Rabies. Alexander I. Wandeler CFIA Scientist Emeritus
 Global Perspective of Rabies Alexander I. Wandeler CFIA Scientist Emeritus Topics general review of global situation of rabies general problems and basic epidemiology of rabies why do we need to focus
Global Perspective of Rabies Alexander I. Wandeler CFIA Scientist Emeritus Topics general review of global situation of rabies general problems and basic epidemiology of rabies why do we need to focus
RABIES EPIDEMIOLOGY, PREVENTION AND CONTROL. John R. Dunn, DVM, PhD Deputy State Epidemiologist State Public Health Veterinarian
 RABIES EPIDEMIOLOGY, PREVENTION AND CONTROL John R. Dunn, DVM, PhD Deputy State Epidemiologist State Public Health Veterinarian https://tn.gov/assets/entities/health/attachments/rabiesmanual2016.pdf Rabies
RABIES EPIDEMIOLOGY, PREVENTION AND CONTROL John R. Dunn, DVM, PhD Deputy State Epidemiologist State Public Health Veterinarian https://tn.gov/assets/entities/health/attachments/rabiesmanual2016.pdf Rabies
Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children
 Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children Prescribing Antimicrobials for Common Illnesses When treating common illnesses such as ear infections and strep throat,
Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children Prescribing Antimicrobials for Common Illnesses When treating common illnesses such as ear infections and strep throat,
One Health: What Does Occupational and Environmental Medicine Have To Do With It?
 One Health: What Does Occupational and Environmental Medicine Have To Do With It? Peter M. Rabinowitz, MD, MPH University of Washington Center for One Health Research Seattle, WA USA NAOEM Conference September
One Health: What Does Occupational and Environmental Medicine Have To Do With It? Peter M. Rabinowitz, MD, MPH University of Washington Center for One Health Research Seattle, WA USA NAOEM Conference September
Biology and Control of Insects and Rodents Workshop Vector Borne Diseases of Public Health Importance
 Vector-Borne Diseases of Public Health Importance Rudy Bueno, Jr., Ph.D. Director Components in the Disease Transmission Cycle Pathogen Agent that is responsible for disease Vector An arthropod that transmits
Vector-Borne Diseases of Public Health Importance Rudy Bueno, Jr., Ph.D. Director Components in the Disease Transmission Cycle Pathogen Agent that is responsible for disease Vector An arthropod that transmits
Drd. OBADĂ MIHAI DORU. PhD THESIS ABSTRACT
 UNIVERSITY OF AGRICULTURAL SCIENCES AND VETERINARY MEDICINE ION IONESCU DE LA BRAD IAŞI FACULTY OF VETERINARY MEDICINE SPECIALIZATION MICROBIOLOGY- IMUNOLOGY Drd. OBADĂ MIHAI DORU PhD THESIS ABSTRACT RESEARCHES
UNIVERSITY OF AGRICULTURAL SCIENCES AND VETERINARY MEDICINE ION IONESCU DE LA BRAD IAŞI FACULTY OF VETERINARY MEDICINE SPECIALIZATION MICROBIOLOGY- IMUNOLOGY Drd. OBADĂ MIHAI DORU PhD THESIS ABSTRACT RESEARCHES
CHAPTER 1 INTRODUCTION
 1 CHAPTER 1 INTRODUCTION The Staphylococci are a group of Gram-positive bacteria, 14 species are known to cause human infections but the vast majority of infections are caused by only three of them. They
1 CHAPTER 1 INTRODUCTION The Staphylococci are a group of Gram-positive bacteria, 14 species are known to cause human infections but the vast majority of infections are caused by only three of them. They
ENVIRACOR J-5 aids in the control of clinical signs associated with Escherichia coli (E. coli) mastitis
 GDR11136 ENVIRACOR J-5 aids in the control of clinical signs associated with Escherichia coli (E. coli) mastitis February 2012 Summary The challenge data presented in this technical bulletin was completed
GDR11136 ENVIRACOR J-5 aids in the control of clinical signs associated with Escherichia coli (E. coli) mastitis February 2012 Summary The challenge data presented in this technical bulletin was completed
Dr Sumathy Puvanendiran, BVSc,M.Phil,PhD(USA) Veterinary Research Officer Dept of Animal Production & Health Sri Lanka
 Dr Sumathy Puvanendiran, BVSc,M.Phil,PhD(USA) Veterinary Research Officer Dept of Animal Production & Health Sri Lanka Sri Lanka Island in Indian Ocean, land extent-64,000sq km, 9 provinces and 25 districts
Dr Sumathy Puvanendiran, BVSc,M.Phil,PhD(USA) Veterinary Research Officer Dept of Animal Production & Health Sri Lanka Sri Lanka Island in Indian Ocean, land extent-64,000sq km, 9 provinces and 25 districts
Objective 1/20/2016. Expanding Antimicrobial Stewardship into the Outpatient Setting. Disclosure Statement of Financial Interest
 Expanding Antimicrobial Stewardship into the Outpatient Setting Michael E. Klepser, Pharm.D., FCCP Professor Pharmacy Practice Ferris State University College of Pharmacy Disclosure Statement of Financial
Expanding Antimicrobial Stewardship into the Outpatient Setting Michael E. Klepser, Pharm.D., FCCP Professor Pharmacy Practice Ferris State University College of Pharmacy Disclosure Statement of Financial
AKC Canine Health Foundation Grant Updates: Research Currently Being Sponsored By The Vizsla Club of America Welfare Foundation
 AKC Canine Health Foundation Grant Updates: Research Currently Being Sponsored By The Vizsla Club of America Welfare Foundation GRANT PROGRESS REPORT REVIEW Grant: 00748: SNP Association Mapping for Canine
AKC Canine Health Foundation Grant Updates: Research Currently Being Sponsored By The Vizsla Club of America Welfare Foundation GRANT PROGRESS REPORT REVIEW Grant: 00748: SNP Association Mapping for Canine
Feline Vaccines: Benefits and Risks
 Feline Vaccines: Benefits and Risks Deciding which vaccines your cat should receive requires that you have a complete understanding of the benefits and risks of the procedure. For this reason, it is extremely
Feline Vaccines: Benefits and Risks Deciding which vaccines your cat should receive requires that you have a complete understanding of the benefits and risks of the procedure. For this reason, it is extremely
Critical Appraisal Topic. Antibiotic Duration in Acute Otitis Media in Children. Carissa Schatz, BSN, RN, FNP-s. University of Mary
 Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Why should we care about multi-resistant bacteria? Clinical impact and
 Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
The natural history of Hendra and Nipah viruses
 Microbes and Infection, 3, 2001, 307 314 2001 Éditions scientifiques et médicales Elsevier SAS. All rights reserved S1286457901013843/REV The natural history of Hendra and Nipah viruses Hume Field a *,
Microbes and Infection, 3, 2001, 307 314 2001 Éditions scientifiques et médicales Elsevier SAS. All rights reserved S1286457901013843/REV The natural history of Hendra and Nipah viruses Hume Field a *,
The importance of infection control in the era of multi drug resistance
 Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
Appropriate Management of Common Pediatric Infections. Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases
 Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
General Approach to Infectious Diseases
 General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
An Overview of the Ontario Wildlife Rabies Control Program
 An Overview of the Ontario Wildlife Rabies Control Program Presentation to the Centre for Public Health and Zoonoses May 5, 2009 Lucille Brown Research Biologist Ontario Ministry of Natural Resources Rabies
An Overview of the Ontario Wildlife Rabies Control Program Presentation to the Centre for Public Health and Zoonoses May 5, 2009 Lucille Brown Research Biologist Ontario Ministry of Natural Resources Rabies
An Outbreak of Brucella melitensis among Goat Farmers in Thailand, December 2009
 An Outbreak of Brucella melitensis among Goat Farmers in Thailand, December 29 Vilaiporn Wongphruksasoong 1,*, Santayakorn S 1, Sitthi W 1, Chuxnum T 1, Pipatjaturong N 2, Kunthu A 3, Phuyathon B 4, Prasert
An Outbreak of Brucella melitensis among Goat Farmers in Thailand, December 29 Vilaiporn Wongphruksasoong 1,*, Santayakorn S 1, Sitthi W 1, Chuxnum T 1, Pipatjaturong N 2, Kunthu A 3, Phuyathon B 4, Prasert
Terrestrial and Aquatic Manuals and the mechanism of standard adoption
 Dr Patrick Bastiaensen Programme Officer OIE Sub-Regional Representation for Eastern Africa Terrestrial and Aquatic Manuals and the mechanism of standard adoption Presented during the Regional Workshop
Dr Patrick Bastiaensen Programme Officer OIE Sub-Regional Representation for Eastern Africa Terrestrial and Aquatic Manuals and the mechanism of standard adoption Presented during the Regional Workshop
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Physician Rating: ( 23 Votes ) Rate This Article:
 From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
Presentation of Quiz #85
 Presentation of Quiz #85 ***Reminder: Slides are copyrighted and cannot be copied for publication. A 36 year old male from Columbia was admitted to the hospital with seizures. This patient had previously
Presentation of Quiz #85 ***Reminder: Slides are copyrighted and cannot be copied for publication. A 36 year old male from Columbia was admitted to the hospital with seizures. This patient had previously
PILOT STUDY OF THE ANTIMICROBIAL SUSCEPTIBILITY OF SHIGELLA IN NEW ZEALAND IN 1996
 PILOT STUDY OF THE ANTIMICROBIAL SUSCEPTIBILITY OF SHIGELLA IN NEW ZEALAND IN 996 November 996 by Maggie Brett Antibiotic Reference Laboratory ESR Communicable Disease Centre Porirua CONTENTS Page SUMMARY
PILOT STUDY OF THE ANTIMICROBIAL SUSCEPTIBILITY OF SHIGELLA IN NEW ZEALAND IN 996 November 996 by Maggie Brett Antibiotic Reference Laboratory ESR Communicable Disease Centre Porirua CONTENTS Page SUMMARY
Antibiotics & Common Infections: Stewardship, Effectiveness, Safety & Clinical Pearls. Welcome We will begin shortly.
 Antibiotics & Common Infections: Stewardship, Effectiveness, Safety & Clinical Pearls Welcome We will begin shortly. The Canadian Pharmacists Association is pleased to be collaborating with the following
Antibiotics & Common Infections: Stewardship, Effectiveness, Safety & Clinical Pearls Welcome We will begin shortly. The Canadian Pharmacists Association is pleased to be collaborating with the following
Update on diagnosis of feline infectious peritonitis (FIP)
 Update on diagnosis of feline infectious peritonitis (FIP) Séverine Tasker RCVS Specialist in Feline Medicine The Feline Centre Langford Veterinary Services University of Bristol http://www.felinecentre.co.uk/
Update on diagnosis of feline infectious peritonitis (FIP) Séverine Tasker RCVS Specialist in Feline Medicine The Feline Centre Langford Veterinary Services University of Bristol http://www.felinecentre.co.uk/
Originally posted February 13, Update: March 26, 2018
 UPDATED: FDA Investigates Pattern of Contamination in Certain Raw Pet Foods Made by Arrow Reliance Inc., Including Darwin s Natural Pet Products and ZooLogics Pet Food Originally posted February 13, 2018
UPDATED: FDA Investigates Pattern of Contamination in Certain Raw Pet Foods Made by Arrow Reliance Inc., Including Darwin s Natural Pet Products and ZooLogics Pet Food Originally posted February 13, 2018
Canine Distemper Virus
 Canine Distemper Virus Sandra Newbury, DVM National Shelter Medicine Extension Veterinarian Koret Shelter Medicine Program Center for Companion Animal Health U C Davis School of Veterinary Medicine www.sheltermedicine.com
Canine Distemper Virus Sandra Newbury, DVM National Shelter Medicine Extension Veterinarian Koret Shelter Medicine Program Center for Companion Animal Health U C Davis School of Veterinary Medicine www.sheltermedicine.com
New Jersey Department of Health Rabies Background and Technical Information
 New Jersey Department of Health Rabies Background and Technical Information The History of Rabies Rabies is an ancient disease. It is well described in writings by Egyptians dating back to 2300 B.C. Rabies
New Jersey Department of Health Rabies Background and Technical Information The History of Rabies Rabies is an ancient disease. It is well described in writings by Egyptians dating back to 2300 B.C. Rabies
DEWORMING PROCESS KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE , INDIA
 DEWORMING PROCESS KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE-560008, INDIA Email: sales@srisaiagro.com Www.srisaiagro.com INSTRODUCTION According
DEWORMING PROCESS KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE-560008, INDIA Email: sales@srisaiagro.com Www.srisaiagro.com INSTRODUCTION According
