Highly Effective Regimen for Decolonization of Methicillin-Resistant Staphylococcus aureus Carriers
|
|
|
- Bruce Curtis
- 6 years ago
- Views:
Transcription
1 infection control and hospital epidemiology june 2008, vol. 29, no. 6 original article Highly Effective Regimen for Decolonization of Methicillin-Resistant Staphylococcus aureus Carriers M. Buehlmann, MD; R. Frei, MD; L. Fenner, MD; M. Dangel, MPH; U. Fluckiger, MD; A. F. Widmer, MD, MS objective. To evaluate the efficacy of a standardized regimen for decolonization of methicillin-resistant Staphylococcus aureus (MRSA) carriers and to identify factors influencing decolonization treatment failure. design. Prospective cohort study from January 2002 to April 2007, with a mean follow-up period of 36 months. setting. University hospital with 750 beds and 27,000 admissions/year. patients. Of 94 consecutive hospitalized patients with MRSA colonization or infection, 32 were excluded because of spontaneous loss of MRSA, contraindications, death, or refusal to participate. In 62 patients, decolonization treatment was completed. At least 6 body sites were screened for MRSA (including by use of rectal swabs) before the start of treatment. interventions. Standardized decolonization treatment consisted of mupirocin nasal ointment, chlorhexidine mouth rinse, and full-body wash with chlorhexidine soap for 5 days. Intestinal and urinary-tract colonization were treated with oral vancomycin and cotrimoxazole, respectively. Vaginal colonization was treated with povidone-iodine or, alternatively, with chlorhexidine ovula or octenidine solution. Other antibiotics were added to the regimen if treatment failed. Successful decolonization was considered to have been achieved if results were negative for 3 consecutive sets of cultures of more than 6 screening sites. results. The mean age ( standard deviation [SD]) age of the 62 patients was years. The most frequent locations of MRSA colonization were the nose (42 patients [68%]), the throat (33 [53%]), perianal area (33 [53%]), rectum (36 [58%]), and inguinal area (30 [49%]). Decolonization was completed in 87% of patients after a mean ( SD) of decolonization cycles (range, 1-10 cycles). Sixty-five percent of patients ultimately required peroral antibiotic treatment (vancomycin, 52%; cotrimoxazole, 27%; rifampin and fusidic acid, 18%). Decolonization was successful in 54 (87%) of the patients in the intent-to-treat analysis and in 51 (98%) of 52 patients in the on-treatment analysis. conclusion. This standardized regimen for MRSA decolonization was highly effective in patients who completed the full decolonization treatment course. Infect Control Hosp Epidemiol 2008; 29: In past decades, methicillin-resistant Staphylococcus aureus (MRSA) has become the most important multidrug-resistant pathogen worldwide, causing significant morbidity and increased healthcare costs. 1,2 MRSA colonization precedes MRSA infection, which occurs in 20% 60% of colonized patients in acute-care facilities and in 3% 15% of those in long-term-care facilities. 3 The rate of nosocomial transmission of MRSA in healthcare facilities can be reduced by the use of strict infection-control measures, such as establishment of MRSA surveillance; early identification of carriers; isolation of colonized or infected patients; use of barrier precautions, such as use of gloves, gowns, and masks, for patient care; use of strict hand hygiene with alcohol-based hand rubs; and careful environmental cleaning in patient rooms. 3,4 Recently, community-associated strains of MRSA have begun to spread in the community, causing intrafamily clusters of infection and outbreaks among injection drug abusers, prisoners, homeless individuals, sports teams, and children in day care centers. 5,6 Studies of surgical patients colonized with methicillinsusceptible S. aureus have demonstrated that decolonization treatment for example, with mupirocin can reduce the incidence of subsequent infection. 7 In addition, most authorities recommend that MRSA carriers be decolonized in outbreak situations. MRSA decolonization may reduce the risk of MRSA infection in individual carriers and could prevent MRSA spread in healthcare facilities and in the community by eliminating a reservoir for the organism. Several topical and systemic antimicrobial agents have been used for MRSA decolonization, with limited success rates However, most of the studies are limited by the selection of patients (such as when patients with From the Division of Infectious Diseases and Hospital Epidemiology (M.B., M.D., U.F., A.F.W.) and Microbiology Laboratory (R.F., L.F.), University Hospital Basel, Basel, Switzerland. Received January 6, 2008; accepted March 12, 2008; electronically published May 30, by The Society for Healthcare Epidemiology of America. All rights reserved X/2008/ $ DOI: /588201
2 effective decolonization of mrsa carriers 511 MRSA infection are excluded), small sample sizes, and methodological flaws. 8 Therefore, the effectiveness of MRSA decolonization is still controversial, and it is not routinely recommended. The present study was performed to evaluate the efficacy of a standardized MRSA decolonization treatment regimen for MRSA-colonized and MRSA-infected patients and to identify factors influencing the failure of the decolonization program. methods Setting The University Hospital Basel is a primary- and tertiary-care center with 750 beds and 27,000 admissions/year. Since 1993, data on all patients colonized or infected with MRSA have been prospectively collected by use of case report forms and entered into a database. The local prevalence of methicillin resistance among S. aureus isolates has remained low (less than 5%) during the past decade. 12 Screening for MRSA by analysis of nose and throat swab samples is routinely performed for patients who (1) are transferred from areas with MRSA endemicity, (2) have a history of MRSA colonization, (3) have a history of injection drug use, or (4) have been in contact with a known MRSA carrier. Study Design and Definitions We conducted a prospective cohort study from January 1, 2002, to April 30, All patients admitted to the University Hospital who were colonized or infected with MRSA were eligible for decolonization treatment. Patients who were unable or failed to attend follow-up visits were excluded from the analysis. For the purpose of the present study, MRSA colonization was defined as being present in any patient from whom MRSA was cultured from any body site (from routine screening or clinical specimens). MRSA infections were defined by use of the criteria of the Centers for Disease Control and Prevention. 13 In an adaptation of the Centers for Disease Control and Prevention definition, a case of MRSA colonization was defined as community acquired if the patient had (1) no history of MRSA colonization; (2) no history of hospitalization, surgery, or hemodialysis in the previous 12 months; and (3) an MRSA strain that was not epidemiologically linked to the hospital strains. A case was defined as healthcare associated if the patient (1) underwent hospitalization in an acute-care or longterm-care facility, hemodialysis, or any surgery in the previous 12 months and (2) had an MRSA strain that was epidemiologically not linked to the hospital strains. A case was defined as nosocomial if the patient had MRSA colonization diagnosed more than 48 hours after hospital admission, 30 days after an operation, or 1 year after implantation of persistent foreign body material (eg, a joint prosthesis). Decolonization Before initiation of decolonization treatment, all patients with MRSA colonization underwent standardized screening, using samples collected by use of polyester fiber tipped swabs from the following body sites: the nose, throat, inguinal area, perineal area, rectum, vagina (in women), wounds, and insertion sites of catheters. In addition, urine culture for MRSA was performed for patients with urinary catheters or urinary-tract infection. Decolonization treatment was offered to all patients. It consisted of a 5-day standard regimen of application of mupirocin ointment (Bactroban; GlaxoSmithKline) twice daily, oral rinsing with 0.2% chlorhexidine solution (Dentohexin; Streuli Pharma) 3 times daily, and daily body washing with 4% chlorhexidine soap (Lifoscrub; B. Braun). In addition, specific decolonization treatment was administered for urogenital and gastrointestinal colonization: for patients with MRSA colonization of the urine, cotrimoxazole (800/160 mg twice daily) was administered for 5 days, if the strain was susceptible. For gastrointestinal colonization (indicated by an MRSA-positive rectal swab sample), oral vancomycin (1 g twice daily) was administered for 5 days. Vaginal colonization was treated with a povidone-iodine ovula (Betadine; Mundipharma Medical Company) administered once daily for 5 days as a first choice or, alternatively, a hexetidine ovula (Vagi-Hex; Drossapharm) administered twice daily for 6 days or octenidine solution (Octenisept; Schülke & Mayr) twice daily for 6 days for patients who did not tolerate or had contraindications for the use of a povidone-iodine ovula. If a first cycle of decolonization treatment failed, the management of treatment was evaluated for potential obstacles to success for example, noncompliance. Thereafter, a second cycle was started with the same regimen as described above. Systemic antibiotic treatment was recommended for patients whose conditions did not respond to 2 full cycles of decolonization treatment. Such patients were treated with fusidic acid (500 mg 3 times daily) and rifampin (450 mg twice daily) for 5 days. Other antibiotics were chosen on an individual basis for patients colonized with MRSA strains resistant to fusidic acid or rifampin. MRSA decolonization was considered to be successful if there was no growth in 3 sets of surveillance cultures of samples (from the nose, throat, inguinal area, perianal area, rectum, vagina [in women], wounds, insertion sites, or urine [for patients with urinary-tract colonization]) obtained at least 2-3 days after completion of decolonization treatment at intervals of 2-3 days. After successful MRSA decolonization, follow-up cultures (of nose and throat samples) were performed at every subsequent hospital admission. All patients ever colonized with MRSA are labeled in the hospital mainframe system, and an alarm is sent to the department of hospital epidemiology within minutes after admission.
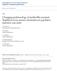
3 512 infection control and hospital epidemiology june 2008, vol. 29, no. 6 figure 1. Diagram summarizing inclusion and exclusion of patients in the study. MRSA, methicillin-resistant Staphylococcus aureus. Identification of MRSA and Molecular Typing MRSA screening was performed by means of culture in a highly selective enrichment broth, as described elsewhere. 12 At the University Hospital Basel, each nonrepetitive clinical MRSA isolate has been typed by pulsed-field gel electrophoresis (PFGE) since 1993 and saved at 70 C. In addition, strains have been typed by polymerase chain reaction (PCR) 14 and, more recently, by spa typing. 15 For the present study, MRSA isolates were thawed from frozen storage and subcultured twice. DNA was extracted by use of the LC MagnaPure system (Roche Diagnostics), in accordance with the manufacturer s instructions. Genes for Panton-Valentine leukocidin (pvl); toxic shock syndrome toxin (tsst); exfoliative toxins A, B, and D (eta, etb, and etd); and methicillin resistance (meca) were detected by PCR, as described elsewhere The polymorphic X region of the spa gene was amplified using primers spa-1113f and spa-1514r and sequenced as described elsewhere. 15 Sequences were analyzed by use of StaphType software, version 1.5.4, and SpaServer (both Ridom). 20 Analysis of clustering into spa clonal complexes (spaccs) was done using default parameters. Susceptibility to mupirocin was determined by E-test (AB Biodisk) and interpreted according to the commonly used definition (minimum inhibitory concentration for low-level resistance, g/ml; minimum inhibitory concentration for high-level resistance, more than 512 g/ml). 21,22 Statistical Analysis Data were analyzed with SPSS version for Windows (SPSS). Kaplan-Meier curves were used to describe the probability of decolonization success; covariates were compared using the log rank test. P.05 was considered to be significant. results During the study period, 94 cases of MRSA colonization or infection in hospitalized patients were identified, corresponding to prevalences of 0.1 cases per 100 patients discharged and 1.2 cases per 10,000 patient-days. Thirty-two cases were excluded from the analysis (Figure 1). For 11 patients, MRSA did not grow in screening cultures at the time when additional cultures were performed before decolonization was initiated, and all 11 patients had negative results for 3 sets of screening cultures at follow-up. The most common sites of MRSA colonization were the nose and throat (Table 1), and 36 patients (58%) had gastrointestinal MRSA colonization (positive rectal cultures). However, no patients were found to have MRSA colonization by rectal culture only. In addition, 6 (26%) of 23 women had vaginal colonization. Seventeen (27%) of the patients presented with MRSA infection (Table 1). A minority of patients had community-acquired MRSA colonization (Table 1).
4 effective decolonization of mrsa carriers 513 table 1. Demographic and Clinical Characteristics of Patients Colonized or Infected with Methicillin-Resistant Staphylococcus aureus (MRSA) Characteristic Value No. of patients 62 Male sex 39 (62.9) Age, years, mean SD Type of MRSA colonization Nosocomial 28 (45.2) Healthcare associated 27 (43.5) Community acquired 7 (11.3) spa type of colonizing strain (n 56 a ) t (25) t (21.4) t002 7 (12.5) t032 5 (8.9) t030 2 (3.6) Other b 16 (28.6) Site of colonization Nose 42 (67.7) Throat 33 (53.2) Inguinal area 30 (48.8) Perianal area 33 (53.2) Rectum 36 (58.1) Wound 27 (43.5) Urine 13 (21.0) Vagina c 6 (26) Other d 19 (30.6) Risk factors for colonization Foreign-body implantation 19 (30.6) Chronic skin ulcer 12 (19.3) Diabetes mellitus 8 (12.9) Immunosuppression 5 (8.1) Hemodialysis 2 (3.2) Chronic skin disease 1 (1.6) None 15 (24.1) Site of MRSA infection Osteomyelitis or spondylodiscitis 3 (4.8) Bloodstream infection 3 (4.8) Skin and soft-tissue infection 3 (4.8) Pulmonary infection 2 (3.2) Other e 6 (9.7) Total no. of infections 17 (27.4) note. Data are no. (%) of patients, unless otherwise indicated. a Six isolates were not available for spa typing. b Other spa types included t001, t016, t024, t025, t026, t037, t046, t074, t1508, t1594, t230, t266, t355, t391, and t548. c Percentage of positive vaginal cultures among women only (6 of 23). d Insertion sites, 5 patients; blood, 4; sputum, 4; tracheobronchial secretions, 1; tracheostoma, 1; abdomen, 1; penis, 1; subretinal fluid, 1; nasolacrimal duct, 1. e Prosthetic valve endocarditis, 1 patient; abdominal abscess, 1; urinary tract infection, 1; dacryocystitis, 1; endophthalmitis, 1; foreignbody infection, 1 (Tenkhoff catheter). Three isolates (5%) were positive for the community-acquired MRSA marker Panton-Valentine leukocidin, whereas the gene for toxic-shock syndrome toxin 1 was found in 3 other isolates. No isolate was positive for the exfoliative toxin gene. figure 2. Number of decolonization courses needed for successful methicillin-resistant Staphylococcus aureus (MRSA) eradication, overall (bold line) and stratified according to number of sites initially colonized by MRSA (P.004). Overall, 54 of the patients (87%) were successfully decolonized (intent-to-treat analysis). Of the 8 patients with decolonization failure, 7 did not complete the decolonization treatment course according to the protocol, because of noncompliance (3 patients) or sociomedical reasons (4 patients). The patient for whom decolonization failed despite completion of the decolonization treatment course was a young man who had been transferred to our hospital from Brazil after a car accident. After treatment of an open fracture, he developed a chronic osteomyelitis caused by multidrug-resistant Pseudomonas aeruginosa and was found to be colonized with MRSA (MRSA was not found in the bone biopsy). Treatment of osteomyelitis failed, as did decolonization after completion of 6 decolonization treatment cycles. It was therefore decided to postpone further decolonization treatment until the osteomyelitis was under control. Treatment was successful in 51 (98%) of 52 (on-treatment analysis) of the patients who completed the full decolonization treatment cycle. For 29 (46.7%) of 62 of the patients, MRSA eradication was achieved after 1 decolonization course (Figure 2). A minority of patients (10 [16%]) underwent more than 3 decolonization courses. Patients with MRSA colonization at a single body site required significantly fewer decolonization courses for successful eradication than did those with colonization at multiple sites (eradication rate after 1 course, 76.9% of patients with 1 site colonized and 38.7% of patients with multiple sites colonized; P.004) (Figure 2). MRSA colonization persisted longer in patients with throat colonization than in patients with colonization of other sites (Figure 3). Decolonization was not successful in 23.5% of MRSA-infected patients, compared with 8.8% of colonized patients. Decolonization in patients with MRSA spa type t041 was more difficult to achieve than was decolonization in patients with other spa
5 514 infection control and hospital epidemiology june 2008, vol. 29, no. 6 figure 3. Number of patients colonized after each decolonization course (Deco), by methicillin-resistant Staphylococcus aureus colonization site (colonization of multiple sites was possible). types (eradication rate after 1 course, 26.6% and 51.2%, respectively); however, the difference was not statistically significant (P.20). After successful decolonization, recolonization with MRSA occurred in 10 patients, after a mean interval of 240 days (range, days). The recolonization isolate from 1 patient was not available for typing. One patient was colonized with a new MRSA type, confirmed by the presence of a new spa type (t008 and t032). In 8 patients, the recolonization strains were indistinguishable from the previous isolates by PFGE, a finding possibly indicating decolonization failure or recolonization by the identical strain. However, the long-term eradication rate was still 72.6%, under the assumption that all patients mentioned above are considered to have decolonization failure. A mean of 4 control screening cultures were available after successful decolonization during a median follow-up period of 34 months (range, 0-72 months). Mupirocin resistance was rare (Table 2). There was no mupirocin resistance observed in strains of MRSA from patients who were recolonized. Rates of susceptibility to rifampin, fusidic acid, and cotrimoxazole were 92%, 83%, and 89%, respectively. No glycopeptideresistant MRSA strains were found. Of 62 isolates, 56 were available for spa typing. Of these, 40 (71.4%) belonged to 5 widely distributed epidemic spa types that are circulating throughout Europe (Table 1). discussion Eradication of MRSA carriage may reduce the risk of infection in MRSA-colonized patients and prevent MRSA crosstransmission to other individuals. However, the efficacy of MRSA decolonization treatment still remains controversial. 8,9 Our study demonstrates that MRSA decolonization with a combination of topical and systemic antimicrobial agents is highly effective for patients completing the full decolonization treatment course. Our decolonization success rate of 87% is higher than most rates that have been reported elsewhere in the literature None of the previous studies defined decolonization success as rigorously as ours: at least 6 body sites, some of them almost never screened in published studies (eg, the vagina), had to test negative by use of state-of-the-art selective enrichment broth methods. 12 There are several possible reasons for the high efficacy of our MRSA decolonization strategy. First, several other trials evaluated the efficacy of MRSA decoltable 2. Characteristics of Methicillin-Resistant Staphylococcus aureus Decolonization in 94 Patients Characteristic Value Decolonization cycles required for successful decolonization, mean SD (range), no. per patient (1-10) Time from diagnosis to start of first decolonization course, median (range), days 13 (0-687) Time to successful decolonization, median (range), days a 65 (14-559) Colonization with a mupirocin-resistant strain Low-level resistance (MIC, g/ml) 2 (3.6) High-level resistance (MIC 512 g/ml) 1 (1.8) Decolonization regimen Standardized regimen without antibiotics b 22 (35.5) Vancomycin by mouth 32 (51.6) Cotrimoxazole 17 (27.4) Rifampin plus fusidic acid 11 (17.7) Rifampin plus other antibiotic c 3 (4.8) Other d 4 (6.4) Decolonization treatment result Successful decolonization 54 (87.1) Decolonization regimen not completed e 7 (11.3) Unsuccessful decolonization 1 (1.6) Follow-up period for successful decolonization, median (range), months 34 (0-72) note. Data are no. (%) of patients, unless otherwise indicated. MIC, minimum inhibitory concentration. a Decolonization success was defined as 3 sets of negative culture results from swab samples from the following body sites: nose, throat, inguinal area, rectum, perianal area, urine, wounds, and vagina (in women). b Application of mupirocin ointment twice daily, oral rinsing with chlorhexidine 0.2% 3 times daily, and washing with chlorhexidine soap once daily for 5 days. c Teicoplanine and rifampin, 1 patient; vancomycin and rifampin, 2 [1 of the 2 courses was followed by treatment with cotrimoxazole and rifampin]. d Clindamycin, 1 patient; fusidic acid, 1; doxycyline, 1; linezolid, 1. e Interruption because of noncompliance for 3 patients and because of sociomedical reasons for 4 patients.
6 effective decolonization of mrsa carriers 515 onization on the basis of a single decolonization course. However, in our study, decolonization treatment was repeated if it was not successful at the first attempt, and possible reasons were evaluated, resulting in a mean of 2 courses per patient, with 16% of patients undergoing more than 3 decolonization courses. MRSA eradication after a single decolonization course was achieved in 46.7% of patients, which is comparable to rates in the literature. 10,11,23,24 In pediatric patients with cystic fibrosis, a 3-step protocol with topical mupirocin, chlorhexidine for washing, and a 5-day course of rifampin and fusidic acid has been evaluated; MRSA eradication was achieved in 16 (94%) of 17 patients 8 (47%) after 1 decolonization course and 8 (47%) after 2 or 3 decolonization courses. 25 Maraha et al. 26 found the rate of MRSA elimination to be 100% after a mean of 1.6 courses of treatment with enteral vancomycin and topical antimicrobials during an outbreak; decolonization was achieved after 1 course in 69% of patients. Second, decolonization failure has been reported in patients colonized with MRSA strains with low-level mupirocin resistance. 23 In our study, the rate of low-level mupirocin resistance was low. Of 3 patients colonized with strains with low-level mupirocin resistance, 2 did not undergo decolonization because of noncompliance, and 1 patient was successfully decolonized. The only patient colonized with a strain with high-level mupirocin resistance did not complete decolonization because of noncompliance. In addition, decolonization failure or MRSA recolonization during follow-up was not associated with mupirocin resistance. Third, previous studies have revealed that the gastrointestinal tract is an important MRSA reservoir in colonized patients. 27,28 In our study, more than half of the patients had MRSA colonization of the gastrointestinal tract, as indicated by positive rectal cultures. Decolonization procedures using topical antimicrobial agents focus on eradication of MRSA on nares, skin, and, less frequently, the throat. However, treatment is not targeted at gastrointestinal colonization, facilitating recolonization of other body sites. Silvestri et al. 29 found eradication of MRSA gut carriage by treatment with enteral vancomycin to be effective in the reduction of the rate of MRSA colonization and infection in an outbreak among patients receiving mechanical ventilation in intensive care units. Maraha et al. 26 reported a 100% success rate for MRSA decolonization with enteral vancomycin and topical antimicrobial treatment during an outbreak in a urological unit. In our study, elimination of gut carriage could have minimized the rate of decolonization failure and the risk of recolonization in our population. Recent studies have shown that the throat is an important site for MRSA colonization that can persist for years. 12,30 Our data suggest that throat colonization is more difficult to eradicate than is colonization of other sites. One possible reason for this could be the insufficient levels of antiseptics that are achieved in the crypts of the tonsils with topical treatment. In addition, S. aureus can be internalized by human cells and can survive intracellularly. 31 Systemic antibiotics, especially rifampin and cotrimoxazole, may achieve better tissue and intracellular levels, 32 leading to higher MRSA eradication rates. However, this has to be confirmed in further studies. Countries such as The Netherlands also routinely decolonize MRSA carriers. They report low prevalences of MRSA carriage, similar to those observed in our institution. We speculate that routine decolonization, which has been underestimated in the past as a strategy to control the spread of MRSA, may contribute to the low prevalence. Our study has several limitations. It was not a randomized controlled trial; therefore, there was no appropriate control group. The study population consisted of a selected group of patients, 34% of whom did not meet inclusion criteria. This could have led to overestimation of the decolonization success. However, 27% of the patients were not only colonized but also infected with MRSA, which added obstacles to successful decolonization. The number of cases was small because of a low local MRSA prevalence. In fact, Switzerland has a very low rate of antibiotic use, 33 leading to low selection pressure and potentially allowing MRSA to escape detection by screening culture. Finally, although the study design was prospective, with standardized protocols, PCR for the pvl and tsst genes and the additional method of spa typing were introduced during the study period. However, PFGE was used throughout the study. In conclusion, this standardized regimen including a combination of topical and systemic antimicrobial agents was highly effective for MRSA decolonization in colonized and infected individuals. The majority of patients were successfully decolonized with 2 or 3 decolonization courses. Decolonization of patients with throat carriage seems to be more difficult to achieve than decolonization of patients with carriage at other sites, and systemic antibiotics may be necessary in the treatment of patients whose conditions do not respond to topical therapy. Specific treatment of gastrointestinal and urogenital MRSA reservoirs may improve the rate of successful decolonization. However, the evolution of other antibiotic-resistant organisms, such as vancomycin-resistant enterococci, needs to be carefully monitored. acknowledgments We thank M. Battegay, for his helpful comments, and the infection control team of the University Hospital Basel, for their help in data collection. Financial support. The study was supported in part by the Swiss National Science Foundation (3200BO ) and the hospital research fund. Potential conflicts of interest. All authors report no conflicts of interest relevant to this article. Address reprint requests to Andreas F. Widmer, MD, MS, Division of Infectious Diseases and Hospital Epidemiology, University Hospital Basel, Petersgraben 4, CH Basel, Switzerland (awidmer@uhbs.ch). Presented in part: 47th Interscience Conference on Antimicrobial Agents and Chemotherapy; Chicago, Illinois; Sept 17-20, 2007.
7 516 infection control and hospital epidemiology june 2008, vol. 29, no. 6 references 1. Lowy FD. Staphylococcus aureus infections. N Engl J Med 1998;339: Gould IM. The clinical significance of methicillin-resistant Staphylococcus aureus. J Hosp Infect 2005;61: Rubinovitch B, Pittet D. Screening for methicillin-resistant Staphylococcus aureus in the endemic hospital: what have we learned? J Hosp Infect 2001; 47: Pittet D, Hugonnet S, Harbarth S, et al. Effectiveness of a hospital-wide programme to improve compliance of hand-hygiene. Lancet 2000;356: Gilbert M, MacDonald J, Gregson D, et al. Outbreak in Alberta of community-acquired (USA300) methicillin-resistant Staphylococcus aureus in people with a history of drug use, homelessness or incarceration. CMAJ 2006;175: Weber JT. Community-associated methicillin-resistant Staphylococcus aureus. Clin Infect Dis 2005;41(Suppl 4):S Perl TM, Cullen JJ, Wenzel RP, et al. Intranasal mupirocin to prevent postoperative Staphylococcus aureus infections. N Engl J Med 2002;346: Loeb M, Main C, Walker-Dilks C, et al. Antimicrobial drugs for treating methicillin-resistant Staphylococcus aureus colonization. Cochrane Database Syst Rev 2003;(4). 9. Loveday HP, Pellowe CM, Jones SRLJ, et al. A systematic review of the evidence for interventions for the prevention and control of methicillinresistant Staphylococcus aureus ( ): report to the Joint MRSA Working Party (Subgroup A). J Hosp Infect 2006;63:S45-S Walsh TJ, Standiford HC, Reboli AC, et al. Randomized double-blinded trial of rifampin with either novobiocin or trimethoprim-sulfamethoxazole against methicillin-resistant Staphylococcus aureus colonization: prevention of antimicrobial resistance and effect of host factors on outcome. Antimicrob Agents Chemother 1993;37: Simor AE, Phillips E, McGeer A, et al. Randomized controlled trial of chlorhexidine gluconate for washing, intranasal mupirocin, and rifampin and doxycycline versus no treatment for the eradication of methicillinresistant Staphylococcus aureus colonization. Clin Infect Dis 2007;44: Mertz D, Frei R, Jaussi B, et al. Throat swabs are necessary to reliably detect carriers of Staphylococcus aureus. Clin Infect Dis 2007;45: In: Mayhall CG, Horan TC, Gaynes RP, eds. Hospital Epidemiology and Infection Control: Surveillance of Nosocomial Infections. 3rd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004: Strandén AM, Frei R, Widmer AF. Molecular typing of methicillinresistant S. aureus (MRSA): can PCR replace pulsed-field gel electrophoresis. J Clin Microbiol 2003;41: Strommenger B, Kettlitz C, Weniger T, et al. Assignment of Staphylococcus isolates to groups by spa typing, SmaI macrorestriction analysis, and multilocus sequence typing. J Clin Microbiol 2006;44: Lina G, Piemont Y, Godail-Gamot F, et al. Involvement of Panton- Valentine leukocidin producing Staphylococcus aureus in primary skin infections and pneumonia. Clin Infect Dis 1999;29: Yamasaki O, Tristan A, Yamaguchi T, et al. Distribution of the exfoliative toxin D gene in clinical Staphylococcus aureus isolates in France. Clin Microbiol Infect 2006;12: Mehrotra M, Wang G, Johnson WM. Multiplex PCR for detection of genes for Staphylococcus aureus enterotoxins, exfoliative toxins, toxic shock syndrome toxin 1, and methicillin resistance. J Clin Microbiol 2000; 38: Murakami K, Minamide W, Wada K, et al. Identification of methicillinresistant strains of staphylococci by polymerase chain reaction. J Clin Microbiol 1991;29: Ridom SpaServer. Available at: Accessed February 20, MacGowan AP, Wise R. Establishing MIC breakpoints and the interpretation of in vitro susceptibility tests. J Antimicrob Chemother 2001;48: Simor AE, Stuart TL, Louie L, et al. Mupirocin-resistant, methicillinresistant Staphylococcus aureus strains in Canadian hospitals. Antimicrob Agents Chemother 2007;51: Harbarth S, Dharan S, Liassine N, et al. Randomized, placebo-controlled, double-blind trial to evaluate the efficacy of mupirocin for eradicating carriage of methicillin-resistant Staphylococcus aureus. Antimicrob Agents Chemother 1999;43: Muder RR. A controlled trial of rifampicin, minocycline and rifampicin plus minocycline for eradication of methicillin-resistant Staphylococcus aureus in long-term care patients. J Antimicrob Chemother 1994;34: Macfarlane M, Leavy A, McVaughan J, et al. Successful decolonization of methicillin-resistant Staphylococcus aureus in paediatric patients with cystic fibrosis using a three-step protocol. J Hosp Infect 2007;65: Maraha B, Van Halteren J, Verzijl JM, et al. Decolonization of methicillinresistant Staphylococcus aureus using oral vancomcyin and topical mupirocin. Clin Microbiol Infect 2002;8: Klotz M, Zimmermann S, Opper S, et al. Possible risk for re-colonization with methicillin-resistant Staphylococcus aureus (MRSA) by faecal transmission. Int J Hyg Environ Health 2005;208: Boyce JM, Havill NL, Maria B. Frequency and possible infection control implications of gastrointestinal colonization with methicillin-resistant Staphylococcus aureus. J Clin Microbiol 2005;43: Silvestri L, Milanese M, Oblach L, et al. Enteral vancomycin to control methicillin-resistant Staphylococcus aureus outbreak in mechanically ventilated patients. Am J Infect Control 2002;30: Ringberg H, Petersson AC, Walder M, et al. The throat: an important site for MRSA colonization. Scand J Infect Dis 2006;38: Garzoni C, Francois P, Huyghe A, et al. A global view of Staphylococcus aureus whole genome expression upon internalization in human epithelial cells. BMC Genomics 2007;8: Yamaoka T. The bactericidal effects of anti-mrsa agents with rifampicin and sulfamethoxazole-trimethoprim against intracellular phagocytized MRSA. J Infect Chemother 2007;13: Filippini M, Masiero G, Moschetti K. Socioeconomic determinants of regional differences in outpatient antibiotic consumption: evidence from Switzerland. Health Policy 2006;78:77-92.
Highly Effective Regimen for Decolonization of Methicillin-Resistant Staphylococcus aureus Carriers
 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY JUNE 2008, VOL. 29, NO. 6 ORIGINAL ARTICLE Highly Effective Regimen for Decolonization of Methicillin-Resistant Staphylococcus aureus Carriers M. Buehlmann,
INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY JUNE 2008, VOL. 29, NO. 6 ORIGINAL ARTICLE Highly Effective Regimen for Decolonization of Methicillin-Resistant Staphylococcus aureus Carriers M. Buehlmann,
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
North West Neonatal Operational Delivery Network Working together to provide the highest standard of care for babies and families
 Document Title and Reference : Guideline for the management of multi-drug resistant organisms (MDRO) Main Author (s) Simon Power Ratified by: GM NSG Date Ratified: February 2012 Review Date: March 2017
Document Title and Reference : Guideline for the management of multi-drug resistant organisms (MDRO) Main Author (s) Simon Power Ratified by: GM NSG Date Ratified: February 2012 Review Date: March 2017
Horizontal vs Vertical Infection Control Strategies
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL Chapter 14 Horizontal vs Vertical Infection Control Strategies Author Salma Abbas, MBBS Michael Stevens, MD, MPH Chapter Editor Shaheen Mehtar, MBBS. FRC Path,
GUIDE TO INFECTION CONTROL IN THE HOSPITAL Chapter 14 Horizontal vs Vertical Infection Control Strategies Author Salma Abbas, MBBS Michael Stevens, MD, MPH Chapter Editor Shaheen Mehtar, MBBS. FRC Path,
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs?
 Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Prevalence & Risk Factors For MRSA. For Vets
 For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
Staphylococcus Aureus
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
Preventing Multi-Drug Resistant Organism (MDRO) Infections. For National Patient Safety Goal
 Preventing Multi-Drug Resistant Organism (MDRO) Infections For National Patient Safety Goal 07.03.01 2009 Methicillin Resistant Staphlococcus aureus (MRSA) About 3-8% of the population at large is a carrier
Preventing Multi-Drug Resistant Organism (MDRO) Infections For National Patient Safety Goal 07.03.01 2009 Methicillin Resistant Staphlococcus aureus (MRSA) About 3-8% of the population at large is a carrier
Successful Treatment for Carriage of Methicillin-Resistant Staphylococcus aureus and Importance of Follow-Up
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2010, p. 4020 4025 Vol. 54, No. 9 0066-4804/10/$12.00 doi:10.1128/aac.01240-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Successful
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2010, p. 4020 4025 Vol. 54, No. 9 0066-4804/10/$12.00 doi:10.1128/aac.01240-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Successful
FM - Male, 38YO. MRSA nasal swab (+) Due to positive MRSA nasal swab test, patient will be continued on Vancomycin 1500mg IV q12 for MRSA treatment...
 Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Screening programmes for Hospital Acquired Infections
 Screening programmes for Hospital Acquired Infections European Diagnostic Manufacturers Association In Vitro Diagnostics Making a real difference in health & life quality June 2007 HAI Facts Every year,
Screening programmes for Hospital Acquired Infections European Diagnostic Manufacturers Association In Vitro Diagnostics Making a real difference in health & life quality June 2007 HAI Facts Every year,
Hosted by Dr. Jon Otter, Guys & St. Thomas Hospital, King s College, London A Webber Training Teleclass 1
 Andreas Voss, MD, PhD Professor of Infection Control Radboud University Nijmegen Medical Centre & Canisius-Wilhelmina Hospital Nijmegen, Netherlands Hosted by Dr. Jon O0er Guys & St. Thomas NHS Founda
Andreas Voss, MD, PhD Professor of Infection Control Radboud University Nijmegen Medical Centre & Canisius-Wilhelmina Hospital Nijmegen, Netherlands Hosted by Dr. Jon O0er Guys & St. Thomas NHS Founda
Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives
 Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives John Jernigan, MD, MS Alex Kallen, MD, MPH Division of Healthcare Quality Promotion Centers for Disease
Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives John Jernigan, MD, MS Alex Kallen, MD, MPH Division of Healthcare Quality Promotion Centers for Disease
LINEE GUIDA: VALORI E LIMITI
 Ferrara 28 novembre 2014 LINEE GUIDA: VALORI E LIMITI Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi EVIDENCE BIASED GERIATRIC MEDICINE Older patients with comorbid conditions
Ferrara 28 novembre 2014 LINEE GUIDA: VALORI E LIMITI Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi EVIDENCE BIASED GERIATRIC MEDICINE Older patients with comorbid conditions
Surgical prophylaxis for Gram +ve & Gram ve infection
 Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Preventing Surgical Site Infections. Edward L. Goodman, MD September 16, 2013
 Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Other Enterobacteriaceae
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 50: Other Enterobacteriaceae Author Kalisvar Marimuthu, MD Chapter Editor Michelle Doll, MD, MPH Topic Outline Topic outline - Key Issues Known
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 50: Other Enterobacteriaceae Author Kalisvar Marimuthu, MD Chapter Editor Michelle Doll, MD, MPH Topic Outline Topic outline - Key Issues Known
Surveillance of Multi-Drug Resistant Organisms
 Surveillance of Multi-Drug Resistant Organisms Karen Hoffmann, RN, MS, CIC Associate Director Statewide Program for Infection Control and Epidemiology (SPICE) University of North Carolina School of Medicine
Surveillance of Multi-Drug Resistant Organisms Karen Hoffmann, RN, MS, CIC Associate Director Statewide Program for Infection Control and Epidemiology (SPICE) University of North Carolina School of Medicine
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Safe Patient Care Keeping our Residents Safe Use Standard Precautions for ALL Residents at ALL times
 Safe Patient Care Keeping our Residents Safe 2016 Use Standard Precautions for ALL Residents at ALL times #safepatientcare Do bugs need drugs? Dr Deirdre O Brien Consultant Microbiologist Mercy University
Safe Patient Care Keeping our Residents Safe 2016 Use Standard Precautions for ALL Residents at ALL times #safepatientcare Do bugs need drugs? Dr Deirdre O Brien Consultant Microbiologist Mercy University
Responders as percent of overall members in each category: Practice: Adult 490 (49% of 1009 members) 57 (54% of 106 members)
 Infectious Diseases Society of America Emerging Infections Network 6/2/10 Report for Query: Perioperative Staphylococcus aureus Screening and Decolonization Overall response rate: 674/1339 (50.3%) physicians
Infectious Diseases Society of America Emerging Infections Network 6/2/10 Report for Query: Perioperative Staphylococcus aureus Screening and Decolonization Overall response rate: 674/1339 (50.3%) physicians
Risk Factors for Persistent MRSA Colonization in Children with Multiple Intensive Care Unit Admissions
 University of Massachusetts Amherst From the SelectedWorks of Nicholas G Reich July, 2013 Risk Factors for Persistent MRSA Colonization in Children with Multiple Intensive Care Unit Admissions Victor O.
University of Massachusetts Amherst From the SelectedWorks of Nicholas G Reich July, 2013 Risk Factors for Persistent MRSA Colonization in Children with Multiple Intensive Care Unit Admissions Victor O.
Is biocide resistance already a clinical problem?
 Is biocide resistance already a clinical problem? Stephan Harbarth, MD MS University of Geneva Hospitals and Faculty of Medicine, Geneva, Switzerland Important points Biocide resistance exists Antibiotic
Is biocide resistance already a clinical problem? Stephan Harbarth, MD MS University of Geneva Hospitals and Faculty of Medicine, Geneva, Switzerland Important points Biocide resistance exists Antibiotic
Antibiotic Prophylaxis Update
 Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
MDR Acinetobacter baumannii. Has the post antibiotic era arrived? Dr. Michael A. Borg Infection Control Dept Mater Dei Hospital Malta
 MDR Acinetobacter baumannii Has the post antibiotic era arrived? Dr. Michael A. Borg Infection Control Dept Mater Dei Hospital Malta 1 The Armageddon recipe Transmissible organism with prolonged environmental
MDR Acinetobacter baumannii Has the post antibiotic era arrived? Dr. Michael A. Borg Infection Control Dept Mater Dei Hospital Malta 1 The Armageddon recipe Transmissible organism with prolonged environmental
Methicillin-Resistant Staphylococcus aureus
 Methicillin-Resistant Staphylococcus aureus By Karla Givens Means of Transmission and Usual Reservoirs Staphylococcus aureus is part of normal flora and can be found on the skin and in the noses of one
Methicillin-Resistant Staphylococcus aureus By Karla Givens Means of Transmission and Usual Reservoirs Staphylococcus aureus is part of normal flora and can be found on the skin and in the noses of one
Multi-Drug Resistant Organisms (MDRO)
 Multi-Drug Resistant Organisms (MDRO) 2016 What are MDROs? Multi-drug resistant organisms, or MDROs, are bacteria resistant to current antibiotic therapy and therefore difficult to treat. MDROs can cause
Multi-Drug Resistant Organisms (MDRO) 2016 What are MDROs? Multi-drug resistant organisms, or MDROs, are bacteria resistant to current antibiotic therapy and therefore difficult to treat. MDROs can cause
Ca-MRSA Update- Hand Infections. Washington Hand Society September 19, 2007
 Ca-MRSA Update- Hand Infections Washington Hand Society September 19, 2007 Resistant Staph. Aureus Late 1940 s -50% S.Aureus resistant to PCN 1957-80/81 strain- of S.A. highly virulent and easily transmissible
Ca-MRSA Update- Hand Infections Washington Hand Society September 19, 2007 Resistant Staph. Aureus Late 1940 s -50% S.Aureus resistant to PCN 1957-80/81 strain- of S.A. highly virulent and easily transmissible
CONCISE COMMUNICATION
 CONCISE COMMUNICATION Decolonization of methicillin-resistant Staphylococcus aureus using oral vancomycin and topical mupirocin B. Maraha 1, J. van Halteren 2, J. M. Verzijl 3, R. G. F. Wintermans 4 and
CONCISE COMMUNICATION Decolonization of methicillin-resistant Staphylococcus aureus using oral vancomycin and topical mupirocin B. Maraha 1, J. van Halteren 2, J. M. Verzijl 3, R. G. F. Wintermans 4 and
SCOTTISH MRSA REFERENCE LABORATORY
 Title SCOTTISH MRSA REFERENCE LABORATORY LABORATORY PROCEDURE NUMBER / VERSION User Manual DATE OF ISSUE 20/01/2017 REVIEW INTERVAL AUTHORISED BY AUTHOR 1 Year Dr. B. Jones Dr E. Dickson COPY 1 of 1 Master
Title SCOTTISH MRSA REFERENCE LABORATORY LABORATORY PROCEDURE NUMBER / VERSION User Manual DATE OF ISSUE 20/01/2017 REVIEW INTERVAL AUTHORISED BY AUTHOR 1 Year Dr. B. Jones Dr E. Dickson COPY 1 of 1 Master
Approval Signature: Original signed by Dr. Michel Tetreault Date of Approval: July Review Date: July 2017
 WRHA Infection Prevention and Control Program Operational Directives Admission Screening for Antibiotic Resistant Organisms (AROs): Methicillin Resistant Staphylococcus aureus (MRSA) and Vancomycin Resistant
WRHA Infection Prevention and Control Program Operational Directives Admission Screening for Antibiotic Resistant Organisms (AROs): Methicillin Resistant Staphylococcus aureus (MRSA) and Vancomycin Resistant
MRSA CROSS INFECTION RISK: IS YOUR PRACTICE CLEAN ENOUGH?
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk MRSA CROSS INFECTION RISK: IS YOUR PRACTICE CLEAN ENOUGH? Author : CATHERINE F LE BARS Categories : Vets Date : February 25,
Vet Times The website for the veterinary profession https://www.vettimes.co.uk MRSA CROSS INFECTION RISK: IS YOUR PRACTICE CLEAN ENOUGH? Author : CATHERINE F LE BARS Categories : Vets Date : February 25,
BMC Infectious Diseases
 BMC Infectious Diseases This Provisional PDF corresponds to the article as it appeared upon acceptance. Copyedited and fully formatted PDF and full text (HTML) versions will be made available soon. Staphylococcus
BMC Infectious Diseases This Provisional PDF corresponds to the article as it appeared upon acceptance. Copyedited and fully formatted PDF and full text (HTML) versions will be made available soon. Staphylococcus
HOSPITAL-ACQUIRED INFECTION/MRSA EYERUSALEM KIFLE AND GIFT IMUETINYAN OMOBOGBE PNURSS15
 HOSPITAL-ACQUIRED INFECTION/MRSA EYERUSALEM KIFLE AND GIFT IMUETINYAN OMOBOGBE PNURSS15 INTRODUCTION DEFINITIONS SIGNS AND SYMPTOMS RISK FACTORS DIAGNOSIS COMPLICATIONS PREVENTIONS TREATMENT PATIENT EDUCATION
HOSPITAL-ACQUIRED INFECTION/MRSA EYERUSALEM KIFLE AND GIFT IMUETINYAN OMOBOGBE PNURSS15 INTRODUCTION DEFINITIONS SIGNS AND SYMPTOMS RISK FACTORS DIAGNOSIS COMPLICATIONS PREVENTIONS TREATMENT PATIENT EDUCATION
Success for a MRSA Reduction Program: Role of Surveillance and Testing
 Success for a MRSA Reduction Program: Role of Surveillance and Testing Singapore July 13, 2009 Lance R. Peterson, MD Director of Microbiology and Infectious Disease Research Associate Epidemiologist, NorthShore
Success for a MRSA Reduction Program: Role of Surveillance and Testing Singapore July 13, 2009 Lance R. Peterson, MD Director of Microbiology and Infectious Disease Research Associate Epidemiologist, NorthShore
Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care units
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Today s Agenda: 9/30/14
 Today s Agenda: 9/30/14 1. Students will take C List Medical Abbreviation Quiz. 2. TO: Discuss MRSA. MRSA MRSA Methicillin Resistant Staphylococcus Aureus Methicillin Resistant Staphylococcus Aureus What
Today s Agenda: 9/30/14 1. Students will take C List Medical Abbreviation Quiz. 2. TO: Discuss MRSA. MRSA MRSA Methicillin Resistant Staphylococcus Aureus Methicillin Resistant Staphylococcus Aureus What
Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1
 Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Development of Drugs for Eradication of Nasal Carriage of S. aureus to Reduce S. aureus Infections in Vulnerable Surgical Patients
 Development of Drugs for Eradication of Nasal Carriage of S. aureus to Reduce S. aureus Infections in Vulnerable Surgical Patients Richard Bax Transcrip Partners Bax - Eradication of carriage - EMA 25-26
Development of Drugs for Eradication of Nasal Carriage of S. aureus to Reduce S. aureus Infections in Vulnerable Surgical Patients Richard Bax Transcrip Partners Bax - Eradication of carriage - EMA 25-26
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Cellulitis. Assoc Prof Mark Thomas. Conference for General Practice Auckland Saturday 28 July 2018
 Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust
 PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust Neonatal Case History Neonate born at 26 +2 gestation Spontaneous onset of
PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust Neonatal Case History Neonate born at 26 +2 gestation Spontaneous onset of
In-Service Training Program. Managing Drug-Resistant Organisms in Long-Term Care
 In-Service Training Program Managing Drug-Resistant Organisms in Long-Term Care OBJECTIVES 1. Define the term antibiotic resistance. 2. Explain the difference between colonization and infection. 3. Identify
In-Service Training Program Managing Drug-Resistant Organisms in Long-Term Care OBJECTIVES 1. Define the term antibiotic resistance. 2. Explain the difference between colonization and infection. 3. Identify
Glycopeptide Resistant Enterococci (GRE) Policy IC/292/10
 BASINGSTOKE AND NORTH HAMPSHIRE NHS FOUNDATION TRUST Glycopeptide Resistant Enterococci (GRE) Policy IC/292/10 Supersedes: IC/292/07 Owner Name Dr Nicki Hutchinson Job Title Consultant Microbiologist,
BASINGSTOKE AND NORTH HAMPSHIRE NHS FOUNDATION TRUST Glycopeptide Resistant Enterococci (GRE) Policy IC/292/10 Supersedes: IC/292/07 Owner Name Dr Nicki Hutchinson Job Title Consultant Microbiologist,
MDRO in LTCF: Forming Networks to Control the Problem
 MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
MRSA Outbreak in Firefighters
 MRSA Outbreak in Firefighters Angie Carranza Munger, MD Resident, Occupational and Environmental Medicine The University of Colorado, Denver and National Jewish Health Candidate, Masters of Public Health
MRSA Outbreak in Firefighters Angie Carranza Munger, MD Resident, Occupational and Environmental Medicine The University of Colorado, Denver and National Jewish Health Candidate, Masters of Public Health
REVISIONE CRITICA sulla VALIDITA delle COMUNI MISURE per la PREVENZIONE delle INFEZIONI CORRELATE a CATETERE INTRAVASCOLARE
 Le Malattie infettive del terzo millennio - dall isolamento all integrazione Paestum 13-15 maggio 2004 REVISIONE CRITICA sulla VALIDITA delle COMUNI MISURE per la PREVENZIONE delle INFEZIONI CORRELATE
Le Malattie infettive del terzo millennio - dall isolamento all integrazione Paestum 13-15 maggio 2004 REVISIONE CRITICA sulla VALIDITA delle COMUNI MISURE per la PREVENZIONE delle INFEZIONI CORRELATE
MRSA Control : Belgian policy
 MRSA Control : Belgian policy PEN ERY CLI DOT GEN KAN SXT CIP MIN RIF FUC MUP OXA Marc Struelens Service de microbiologie & unité d épidémiologie des maladies infectieuses Université Libre de Bruxelles
MRSA Control : Belgian policy PEN ERY CLI DOT GEN KAN SXT CIP MIN RIF FUC MUP OXA Marc Struelens Service de microbiologie & unité d épidémiologie des maladies infectieuses Université Libre de Bruxelles
Infection Control Manual Residential Care Part 3 Infection Control Standards IC7: 0100 Methicillin Resistant Staphylococcus aureus
 Infection Control Manual Residential Care Part 3 Infection Control Standards IC7: 0100 Methicillin Resistant Staphylococcus aureus IC7: 0100 MRSA 1. Purpose To outline the assessment, management, room
Infection Control Manual Residential Care Part 3 Infection Control Standards IC7: 0100 Methicillin Resistant Staphylococcus aureus IC7: 0100 MRSA 1. Purpose To outline the assessment, management, room
DR. MICHAEL A. BORG DIRECTOR OF INFECTION PREVENTION & CONTROL MATER DEI HOSPITAL - MALTA
 DR. MICHAEL A. BORG DIRECTOR OF INFECTION PREVENTION & CONTROL MATER DEI HOSPITAL - MALTA The good old days The dread (of) infections that used to rage through the whole communities is muted Their retreat
DR. MICHAEL A. BORG DIRECTOR OF INFECTION PREVENTION & CONTROL MATER DEI HOSPITAL - MALTA The good old days The dread (of) infections that used to rage through the whole communities is muted Their retreat
Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CONTROLLED DOCUMENT
 CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings?
 An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings? Dr. Andrew Morris Antimicrobial Stewardship ProgramMt. Sinai Hospital University Health Network amorris@mtsinai.on.ca andrew.morris@uhn.ca
An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings? Dr. Andrew Morris Antimicrobial Stewardship ProgramMt. Sinai Hospital University Health Network amorris@mtsinai.on.ca andrew.morris@uhn.ca
GUIDE TO INFECTION CONTROL IN THE HOSPITAL. Enterococcal Species
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 44 Enterococcal Species Authors Jacob Pierce, MD, Michael Edmond, MD, MPH, MPA Michael P. Stevens, MD, MPH Chapter Editor Victor D. Rosenthal, MD, CIC,
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 44 Enterococcal Species Authors Jacob Pierce, MD, Michael Edmond, MD, MPH, MPA Michael P. Stevens, MD, MPH Chapter Editor Victor D. Rosenthal, MD, CIC,
HEALTHCARE-ACQUIRED INFECTIONS AND ANTIMICROBIAL RESISTANCE
 Universidade de São Paulo Departamento de Moléstias Infecciosas e Parasitárias HEALTHCARE-ACQUIRED INFECTIONS AND ANTIMICROBIAL RESISTANCE Anna S. Levin 4 main lines! Epidemiology of HAS and resistance!
Universidade de São Paulo Departamento de Moléstias Infecciosas e Parasitárias HEALTHCARE-ACQUIRED INFECTIONS AND ANTIMICROBIAL RESISTANCE Anna S. Levin 4 main lines! Epidemiology of HAS and resistance!
A Prospective Investigation of Nasal Mupirocin, Hexachlorophene Body Wash, and Systemic
 AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
MRSA in the United Kingdom status quo and future developments
 MRSA in the United Kingdom status quo and future developments Dietrich Mack Chair of Medical Microbiology and Infectious Diseases The School of Medicine - University of Wales Swansea P R I F Y S G O L
MRSA in the United Kingdom status quo and future developments Dietrich Mack Chair of Medical Microbiology and Infectious Diseases The School of Medicine - University of Wales Swansea P R I F Y S G O L
Nosocomial Infections: What Are the Unmet Needs
 Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
original article infection control and hospital epidemiology october 2009, vol. 30, no. 10
 infection control and hospital epidemiology october 2009, vol. 30, no. 10 original article 5 Years of Experience Implementing a Methicillin-Resistant Staphylococcus aureus Search and Destroy Policy at
infection control and hospital epidemiology october 2009, vol. 30, no. 10 original article 5 Years of Experience Implementing a Methicillin-Resistant Staphylococcus aureus Search and Destroy Policy at
(DRAFT) RECOMMENDATIONS FOR THE CONTROL OF MULTI-DRUG RESISTANT GRAM-NEGATIVES: CARBAPENEM RESISTANT ENTEROBACTERIACEAE
 (DRAFT) RECOMMENDATIONS FOR THE CONTROL OF MULTI-DRUG RESISTANT GRAM-NEGATIVES: CARBAPENEM RESISTANT ENTEROBACTERIACEAE John Ferguson (Hunter New England, NSW) on behalf of MRGN Task Force Acknowledgement
(DRAFT) RECOMMENDATIONS FOR THE CONTROL OF MULTI-DRUG RESISTANT GRAM-NEGATIVES: CARBAPENEM RESISTANT ENTEROBACTERIACEAE John Ferguson (Hunter New England, NSW) on behalf of MRGN Task Force Acknowledgement
 1) Mangram AJ,Horan TC,Pearson ML, et al:guideline for Prevention of Surgical Site Infection.Infect Control Hosp Epidemiol 1999;20:247-278. 1a) Perl TM, Cullen JJ, Wenzel RP, et al.: Intranasal mupirocin
1) Mangram AJ,Horan TC,Pearson ML, et al:guideline for Prevention of Surgical Site Infection.Infect Control Hosp Epidemiol 1999;20:247-278. 1a) Perl TM, Cullen JJ, Wenzel RP, et al.: Intranasal mupirocin
National MRSA Reference Laboratory
 Author: Gráinne Brennan Date: 23/02/2017 Date of Issue: 23/02/2017 National MRSA Reference Laboratory User s Manual NMRSARL Users Manual Page 1 of 12 Table of Contents Page 1. Location... 3 2. Contact
Author: Gráinne Brennan Date: 23/02/2017 Date of Issue: 23/02/2017 National MRSA Reference Laboratory User s Manual NMRSARL Users Manual Page 1 of 12 Table of Contents Page 1. Location... 3 2. Contact
Screening and Decolonization: Does Methicillin-Susceptible Staphylococcus aureus Hold Lessons for Methicillin-Resistant S. aureus?
 INVITED ARTICLE HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor Screening and Decolonization: Does Methicillin-Susceptible Staphylococcus aureus Hold Lessons for Methicillin-Resistant S. aureus?
INVITED ARTICLE HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor Screening and Decolonization: Does Methicillin-Susceptible Staphylococcus aureus Hold Lessons for Methicillin-Resistant S. aureus?
SCOTTISH MRSA REFERENCE LABORATORY
 Title SCOTTISH MRSA REFERENCE LABORATORY LABORATORY PROCEDURE NUMBER / VERSION User Manual DATE OF ISSUE 17/05/2014 REVIEW INTERVAL AUTHORISED BY AUTHOR 2 Years Dr. B. Jones B. Cosgrove COPY 1 of 1 Master
Title SCOTTISH MRSA REFERENCE LABORATORY LABORATORY PROCEDURE NUMBER / VERSION User Manual DATE OF ISSUE 17/05/2014 REVIEW INTERVAL AUTHORISED BY AUTHOR 2 Years Dr. B. Jones B. Cosgrove COPY 1 of 1 Master
MRSA eradication of newly acquired lower respiratory tract infection in cystic fibrosis
 MRSA eradication of newly acquired lower respiratory tract infection in cystic fibrosis Vallières, E., Rendall, J. C., Moore, J. E., McCaughan, J., Hoeritzauer, A. I., Tunney, M. M.,... Downey, D. G. (2016).
MRSA eradication of newly acquired lower respiratory tract infection in cystic fibrosis Vallières, E., Rendall, J. C., Moore, J. E., McCaughan, J., Hoeritzauer, A. I., Tunney, M. M.,... Downey, D. G. (2016).
Methicillin Resistant Staphylococcus Aureus (MRSA) The drug resistant `Superbug that won t die
 Methicillin Resistant Staphylococcus Aureus (MRSA) The drug resistant `Superbug that won t die Michael A. Miller, MD Assistant Professor of Pediatrics -Jacksonville OBJECTIVES 1. Understand the basic microbiology
Methicillin Resistant Staphylococcus Aureus (MRSA) The drug resistant `Superbug that won t die Michael A. Miller, MD Assistant Professor of Pediatrics -Jacksonville OBJECTIVES 1. Understand the basic microbiology
Infection Control Priorities for Antibiotics Resistance - The Search and Destroy Strategy. WH Seto Hong Kong China
 Infection Control Priorities for Antibiotics Resistance - The Search and Destroy Strategy WH Seto Hong Kong China WHD 2011 slogan Tier 1 Education Surveillance Environment Administration Usage IC isolation
Infection Control Priorities for Antibiotics Resistance - The Search and Destroy Strategy WH Seto Hong Kong China WHD 2011 slogan Tier 1 Education Surveillance Environment Administration Usage IC isolation
Int.J.Curr.Microbiol.App.Sci (2018) 7(8):
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 08 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.708.378
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 08 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.708.378
TACKLING THE MRSA EPIDEMIC
 TACKLING THE MRSA EPIDEMIC Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine MRSA Trend (HA + CA) in US TSN Database USA (1993-2003) % of MRSA among S. aureus
TACKLING THE MRSA EPIDEMIC Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine MRSA Trend (HA + CA) in US TSN Database USA (1993-2003) % of MRSA among S. aureus
Multi-Drug Resistant Gram Negative Organisms POLICY REVIEW DATE EXTENDED Printed copies must not be considered the definitive version
 Multi-Drug Resistant Gram Negative Organisms POLICY REVIEW DATE EXTENDED 2018 Printed copies must not be considered the definitive version DOCUMENT CONTROL POLICY NO. IC-122 Policy Group Infection Control
Multi-Drug Resistant Gram Negative Organisms POLICY REVIEW DATE EXTENDED 2018 Printed copies must not be considered the definitive version DOCUMENT CONTROL POLICY NO. IC-122 Policy Group Infection Control
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update
 EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
So Why All the Fuss About Hand Hygiene?
 CARING PROFESSIONAL SERVICES, INC. HAND HYGIENE In-Service So Why All the Fuss About Hand Hygiene? Most common mode of transmission of pathogens is via hands! Infections acquired in healthcare Spread of
CARING PROFESSIONAL SERVICES, INC. HAND HYGIENE In-Service So Why All the Fuss About Hand Hygiene? Most common mode of transmission of pathogens is via hands! Infections acquired in healthcare Spread of
Bacterial whole genome sequencing in clinical microbiology, infection control and public health. Julian Parkhill. FIS, Birmingham, November 2013
 Bacterial whole genome sequencing in clinical microbiology, infection control and public health Julian Parkhill FIS, Birmingham, November 2013 Falling costs of genomics 2003 Cost/genome Throughput 60,000
Bacterial whole genome sequencing in clinical microbiology, infection control and public health Julian Parkhill FIS, Birmingham, November 2013 Falling costs of genomics 2003 Cost/genome Throughput 60,000
Conflict of interest: We have no conflict of interest to report on this topic of SSI reduction for total knees.
 Reducing SSI- Knees TIFFANY KENNERK MBA, MSN, RN, NE -BC, ONC CYNTHIA SEAMAN BSN, RN, ONC, CMSRN ~COMMUNITY HOSPITALS AND WELLNESS CENTERS~ Conflict of interest: We have no conflict of interest to report
Reducing SSI- Knees TIFFANY KENNERK MBA, MSN, RN, NE -BC, ONC CYNTHIA SEAMAN BSN, RN, ONC, CMSRN ~COMMUNITY HOSPITALS AND WELLNESS CENTERS~ Conflict of interest: We have no conflict of interest to report
MRSA Screening (Elective Patients)
 What is MRSA? MRSA stands for Meticillin resistant Staphylococcus aureus. It is a type of Staphylococcus aureus bacteria (germ) that is very resistant to antibiotics so infections due to MRSA can be quite
What is MRSA? MRSA stands for Meticillin resistant Staphylococcus aureus. It is a type of Staphylococcus aureus bacteria (germ) that is very resistant to antibiotics so infections due to MRSA can be quite
MAJOR ARTICLE. Andrew E. Simor, 1,2 Elizabeth Phillips, 5 Allison McGeer, 1,3 Ana Konvalinka, 1 Mark Loeb, 6 H. Rosalyn Devlin, 1,4 and Alex Kiss 2
 MAJOR ARTICLE Randomized Controlled Trial of Chlorhexidine Gluconate for Washing, Intranasal Mupirocin, and Rifampin and Doxycycline Versus No Treatment for the Eradication of Methicillin-Resistant Staphylococcus
MAJOR ARTICLE Randomized Controlled Trial of Chlorhexidine Gluconate for Washing, Intranasal Mupirocin, and Rifampin and Doxycycline Versus No Treatment for the Eradication of Methicillin-Resistant Staphylococcus
Optimalization of the antibiotic policy in the Netherlands XI : SWAB Guidelines for the Treatment of MRSA Carriage
 SWAB: Dutch Working Party on Antibiotic Policy Optimalization of the antibiotic policy in the Netherlands XI : SWAB Guidelines for the Treatment of MRSA Carriage SWAB, March 2007 Preparatory Committee:
SWAB: Dutch Working Party on Antibiotic Policy Optimalization of the antibiotic policy in the Netherlands XI : SWAB Guidelines for the Treatment of MRSA Carriage SWAB, March 2007 Preparatory Committee:
UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients
 Background/methods: UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients This guideline establishes evidence-based consensus standards for management
Background/methods: UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients This guideline establishes evidence-based consensus standards for management
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS
 VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
HEALTH SERVICES POLICY & PROCEDURE MANUAL
 PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
New Antibiotics for MRSA
 New Antibiotics for MRSA Faculty Warren S. Joseph, DPM, FIDSA Consultant, Lower Extremity Infectious Diseases Roxborough Memorial Hospital Philadelphia, Pennsylvania Faculty Disclosure Dr. Joseph: Speaker
New Antibiotics for MRSA Faculty Warren S. Joseph, DPM, FIDSA Consultant, Lower Extremity Infectious Diseases Roxborough Memorial Hospital Philadelphia, Pennsylvania Faculty Disclosure Dr. Joseph: Speaker
Appropriate Antimicrobial Therapy for Treatment of
 Appropriate Antimicrobial Therapy for Treatment of Staphylococcus aureus infections ( MRSA ) By : A. Bojdi MD Assistant Professor Inf. Dis. Dep. Imam Reza Hosp. MUMS Antibiotics Still Miracle Drugs Paul
Appropriate Antimicrobial Therapy for Treatment of Staphylococcus aureus infections ( MRSA ) By : A. Bojdi MD Assistant Professor Inf. Dis. Dep. Imam Reza Hosp. MUMS Antibiotics Still Miracle Drugs Paul
The importance of infection control in the era of multi drug resistance
 Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
MRSA What We Need to Know Sharon Pearce, CRNA, MSN Carolina Anesthesia Associates
 MRSA What We Need to Know Sharon Pearce, CRNA, MSN Carolina Anesthesia Associates What is MRSA? Methicillin-resistant Staphylococus aureus This hardy bacterium has developed resistance to every antibiotic
MRSA What We Need to Know Sharon Pearce, CRNA, MSN Carolina Anesthesia Associates What is MRSA? Methicillin-resistant Staphylococus aureus This hardy bacterium has developed resistance to every antibiotic
Staphylococcus aureus
 Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins
 Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Methicillin-resistant Staphylococcus aureus (MRSA) on Belgian pig farms
 Methicillinresistant Staphylococcus aureus (MRSA) on Belgian pig farms Dewaele I., De Man I., Stael A., Delputte P., Butaye P., Vlaemynck G., Herman L., Heyndrickx M., Rasschaert G. 1 ILVO: Institute for
Methicillinresistant Staphylococcus aureus (MRSA) on Belgian pig farms Dewaele I., De Man I., Stael A., Delputte P., Butaye P., Vlaemynck G., Herman L., Heyndrickx M., Rasschaert G. 1 ILVO: Institute for
MRSA surveillance 2014: Poultry
 Vicky Jasson MRSA surveillance 2014: Poultry 1. Introduction In the framework of the FASFC surveillance, a surveillance of MRSA in poultry has been executed in order to determine the prevalence and diversity
Vicky Jasson MRSA surveillance 2014: Poultry 1. Introduction In the framework of the FASFC surveillance, a surveillance of MRSA in poultry has been executed in order to determine the prevalence and diversity
Prophylactic antibiotic timing and dosage. Dr. Sanjeev Singh AIMS, Kochi
 Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Community-Associated Methicillin-Resistant Staphylococcus aureus: Review of an Emerging Public Health Concern
 Community-Associated Methicillin-Resistant Staphylococcus aureus: Review of an Emerging Public Health Concern Timothy D. Drews, MD; Jonathan L. Temte, MD, PhD; Barry C. Fox, MD ABSTRACT Methicillin-resistant
Community-Associated Methicillin-Resistant Staphylococcus aureus: Review of an Emerging Public Health Concern Timothy D. Drews, MD; Jonathan L. Temte, MD, PhD; Barry C. Fox, MD ABSTRACT Methicillin-resistant
Lindsay E. Nicolle University of Manitoba Winnipeg, CANADA
 Lindsay E. Nicolle University of Manitoba Winnipeg, CANADA Long Term Care Facilities: Spectrum low acuity assisted living mobile independent Not LTAC high acuity complete functional disability dialysis
Lindsay E. Nicolle University of Manitoba Winnipeg, CANADA Long Term Care Facilities: Spectrum low acuity assisted living mobile independent Not LTAC high acuity complete functional disability dialysis
Carbapenemase-Producing Enterobacteriaceae (CPE)
 Carbapenemase-Producing Enterobacteriaceae (CPE) September 21, 2017 Maryam Khan Peel Public Health Madeleine Ashcroft Public Health Ontario Objectives Differentiate the acronyms related to CPE (CPE,CPO,CRE,CRO)
Carbapenemase-Producing Enterobacteriaceae (CPE) September 21, 2017 Maryam Khan Peel Public Health Madeleine Ashcroft Public Health Ontario Objectives Differentiate the acronyms related to CPE (CPE,CPO,CRE,CRO)
Eradiaction of Resistant Organisms:
 Eradiaction of Resistant Organisms: Can we do it and does it help? Noah Lechtzin, MD; MHS Director, Adult CF Program Outline Evidence resistant organisms are bad MRSA, B cepacia, Pseudomonas, Fungal infections
Eradiaction of Resistant Organisms: Can we do it and does it help? Noah Lechtzin, MD; MHS Director, Adult CF Program Outline Evidence resistant organisms are bad MRSA, B cepacia, Pseudomonas, Fungal infections
Impact of Antimicrobial Resistance on Human Health. Robert Cunney HSE HCAI/AMR Programme and Temple Street Children s University Hospital
 Impact of Antimicrobial Resistance on Human Health Robert Cunney HSE HCAI/AMR Programme and Temple Street Children s University Hospital AMR in Foodchain Conference, UCD, Dec 2014 Sir Patrick Dun s Hospital
Impact of Antimicrobial Resistance on Human Health Robert Cunney HSE HCAI/AMR Programme and Temple Street Children s University Hospital AMR in Foodchain Conference, UCD, Dec 2014 Sir Patrick Dun s Hospital
Global Status of Antimicrobial Resistance with a Focus on Nepal
 Global Status of Antimicrobial Resistance with a Focus on Nepal John Ferguson, John Hunter Hospital, University of Newcastle, NSW, Australia Infectious Diseases Physician and Medical Microbiologist SIMON
Global Status of Antimicrobial Resistance with a Focus on Nepal John Ferguson, John Hunter Hospital, University of Newcastle, NSW, Australia Infectious Diseases Physician and Medical Microbiologist SIMON
A hypothetical case of nasal microbiome transplantation
 A hypothetical case of nasal microbiome transplantation Katherine P. Lemon, MD, PhD Institute & Boston Children s Hospital Mary-Claire Roghmann, MD, MS University of Maryland Microbiota-transplantation
A hypothetical case of nasal microbiome transplantation Katherine P. Lemon, MD, PhD Institute & Boston Children s Hospital Mary-Claire Roghmann, MD, MS University of Maryland Microbiota-transplantation
