Antibiotic guidelines for SKIN AND SOFT TISSUE INFECTIONS
|
|
|
- Samuel Flynn
- 6 years ago
- Views:
Transcription
1 CLINICAL USEFUL INFORMATION RECOMMENDATIONS ALTERNATIVE Impetigo erythematous papules vesicles and pustules honey-colored crusts on an erythematous base Gram stain and culture of the pus or exudates from skin lesions Bullous and non-bullous impetigo can be treated with oral or topical antimicrobials, but oral therapy is recommended for patients with numerous lesions or in outbreaks affecting several people to help decrease transmission of infection. Hygiene measures are important to aid healing and stop the infection spreading to other sites on the body and to other people; advise patient appropriately. Management of the underlying cause (if applicable) is recommended e.g. atopic eczema, scabies, or head lice. Topical Fusidic acid 6-8 hourly Flucloxacillin 1g 6 hourly PO Clarithromycin 500mg 12 hourly PO 7 days Erysipelas Acute onset of symptoms e.g. cutaneous redness, warmth, tenderness Systemic symptoms e.g. fever Cultures of blood, pus, or bullae in patients with systemic toxicity Elevate affected extremity. Identify and manage any underlying risk factors such as eczema, tinea pedis, lymphoedema, leg ulceration, varicella and bites. Benzylpenicillin 1.2g 4 If no response within 48hrs or acute deterioration add: Clindamycin 900mg 8 (if >65yrs, discuss with microbiology) Clarithromycin 500mg 12 If no response within 48hrs or acute deterioration switch to: Clindamycin 900mg 8 (if >65yrs, discuss with microbiology) 5-10 days depending on clinical response; if >7 days, discuss with microbiology.
2 CLINICAL USEFUL INFORMATION RECOMMENDATIONS ALTERNATIVE Bites (Dog, cat and human) Bite injury which is either infected or at risk of becoming infected. Xray in clenched fist/crush injuries to exclude the presence of teeth or dental fragments, rule out bone damage etc. If infected, send pus or a deep wound swab for culture, before cleaning the wound Blood cultures where indicated Surgical evaluation where indicated 80% of cat bites and 5% of dog bites become infected. Cleanse wound thoroughly. Assess tetanus and rabies risk; for tetanus prone wound, give human tetanus immunoglobulin with absorbed diphtheria (low dose) vaccine if necessary, according to immunization history. Assess HIV, hepatitis B & C risk in the case of human bites. Cat bite wounds tend to penetrate deeply, with higher risk of associated osteomyelitis, tenosynovitis, and septic arthritis. Prophylaxis with antibiotic therapy recommended for: o All human bite wounds <72 hrs old o All cat bites o Animal bites to hand, foot, or face. o Puncture wounds o Wounds requiring surgical debridement o Wounds involving joints, tendons, ligaments, or suspected fractures o Animal bites < 48hrs where the risk of infection is high o Immuno-compromised, diabetic, elderly or asplenic patients. Patients require review at 24 and 48hrs with primary care if minor wound or ED if more significant. Co-amoxiclav 625mg 8 hourly PO or 1.2g 8 depending on severity Doxycycline 100mg 12 hourly PO Metronidazole 400mg 8 hourly PO or Clindamycin 900mg 8 Ciprofloxacin 400mg 12 depending on severity. Prophylaxis: 3-5 days Treatment: 7 days
3 USEFUL INFORMATION RECOMMENDATIONS ALTERNATIVE (suitable in penicillin allergy/ MRSA) Cellulitis cutaneous redness, warmth, tenderness Systemic symptoms e.g. fever Take blood culture and wound swab or pus for culture. Contact microbiology immediately if: o Rapidly spreading cellulitis (Group A Strep) o Panton-Valentine Leukocidin (PVL) positive S. aureus strains suspected; generally affects previously healthy young children and young adults. Risk factors include recurrent abscess/ssti and close contact/crowding. o Necrotising fasciitis, Fourniers or gas gangrene Elevate affected extremity. Identify and manage any underlying risk factors (e.g. eczema, tinea pedis, lymphoedema, leg ulceration, varicella and bites) or co-morbidities (such as diabetes mellitus or alcohol misuse) that may cause the cellulitis to spread rapidly, or delay healing. Class 1: no signs of systemic toxicity, and no significant comorbidity. Class 2: systemically well, but with a co-morbidity e.g. PVD, chronic venous insufficiency or morbid obesity which may complicate or delay resolution of their infection OR systemically unwell. Class 3-4: have severe sepsis syndrome with organ failure or severe life threatening infection e.g. necrotising fasciitis (see separate section). Daptomycin: monitor creatinine kinase before treatment and then weekly (more frequently if receiving another drug known to cause myopathy-preferably avoid concomitant use).if weight > 87kg confirm dose with pharmacy or microbiology between 9am and 5pm day 1/ 2 of treatment. Class 1: Flucloxacillin 1g 6 hourly PO Class 2: Flucloxacillin 2g 6 hourly IV +/- Benzylpenicillin 1.2g 4 depending on severity. Class 3-4: See severe soft tissue infection Class 1 penicillin allergic or MRSA: Doxycycline 100mg 12 hourly PO Class 2 <65: Clindamycin 900mg 8 Class 2 65 or MRSA (all ages): Daptomycin 6mg/kg 24 Class 3-4: See severe soft tissue infection Class 1: 7days Class 2: 7-14 days
4 CLINICAL USEFUL INFORMATION RECOMMENDATIONS ALTERNATIVE Severe Soft Tissue Infection necrotizing fasciitis Fournier s gangrene gas gangrene evidence of toxic shock Five clinical features suggest the presence of a deep and severe infection of skin and its deeper tissue: o severe, constant pain o bullous lesions o gas in the soft tissues o systemic toxicity o rapid spread centrally along fascial planes. Take blood culture and send wound swab, debrided tissue/ pus for culture to microbiology. CT/MRI when indicated These are acute, rapidly developing infections of deep fascia which are life threatening. Urgent surgical and microbiology input is required. Treatment includes early surgical debridement and high dose antibiotic therapy directed at the pathogens. If necrotising fasciitis or Fournier s gangrene suspected, isolate patient with appropriate contact/droplet precautions and discuss with IPCT. Daptomycin: If creatinine kinase elevated before treatment contact microbiology for advice. o Monitor creatinine kinase before treatment and then weekly (more frequently if receiving another drug known to cause myopathy-preferably avoid concomitant use). o If >83kg confirm dose with pharmacy or microbiology between 9am and 5pm day 1 or 2 of treatment. Piperacillin/Tazobactam 4.5g 6 plus Clindamycin 1.2g 6 hourly IV. If known MRSA add: Daptomycin 6mg/kg 24 Clindamycin 1.2g 6 plus Ciprofloxacin 600mg 12 plus Metronidazole 500mg 8 If known MRSA add: Daptomycin 6mg/kg days
5 Preseptal cellulitis eyelid swelling with or without erythema ocular pain Blood cultures Consider CT Preseptal cellulitis: o No proptosis o No impairment of ocular motility o Normal optic nerve function If concerns of progression to orbital cellulitis, or not improving, treat as orbital cellulitis and contact microbiology. Daptomycin: monitor creatinine kinase before treatment and then weekly (more frequently if receiving another drug known to cause myopathy-preferably avoid concomitant use).if weight > 87kg confirm dose with pharmacy or microbiology between 9am and 5pm day 1/ 2 of treatment. Flucloxacillin 2g 6 Benzylpenicillin 1.2g 4 Metronidazole 500mg 8 <65 yrs Clindamycin 900mg 8 65 yrs Daptomycin 6mg/kg 24 Metronidazole 500mg days Treatment should be continued until the erythema and swelling have resolved or nearly resolved Orbital cellulitis as above + ophthalmoplegia proptosis Conjunctival swelling Fever Blood cultures CT/MRI Ophthalmologist, ENT and microbiology referral required. Most patients with uncomplicated orbital cellulitis can be treated with antibiotics alone. Complications include subperiosteal abscess, orbital abscess, visual loss, and intracranial extension. The main indications for surgery are a poor response to antibiotic treatment, worsening visual acuity or pupillary changes, evidence of an abscess (especially a large abscess (>10 mm in diameter) or one that fails to respond promptly to antibiotic treatment). In some cases, drainage of affected sinuses is also required to control the infection. The results of cultures and susceptibility testing from samples obtained during surgery can be used to tailor therapy. Cefotaxime 2g 6 hourly IV Vancomycin IV Metronidazole 500mg 8 Contact microbiology for PO switch when suitable. If true anaphylaxis to penicillin, contact microbiology days Treatment should be continued until all signs resolved.
6 Leg Ulcers (Non-Diabetic) Enlarging ulcer. Increased exudate. Increased pain. Pyrexia. Foul odour. Cellulitis specimens obtained by curettage. Leg ulcers ccasionally become infected, but are invariably colonised by two or more different bacterial species. The predominant pathogens are S.aureus, beta-haemolytic streptococci and anaerobes. If the ulcer has an unpleasant odour, anaerobes are present, irrespective of whether or not they have been isolated. Organisms which commonly COLONISE (but rarely infect) ulcers include: coliforms (especially Proteus species), Pseudomonas aeruginosa and enterococci. Clinically non-infected ulcers should not be cultured. Infected leg ulcers do not normally require urgent treatment and it is often possible to await the results of cultures, when optimal therapy can be initiated. Manage associated oedema, pain, and dermatitis. Treatment should be reviewed with culture results. For Diabetic Foot Infections see relevant guidelines Flucloxacillin 2g 6 +/- Metronidazole 500mg 8 Clarithromycin 500mg 12 +/- Metronidazole 500mg 8 7 days May be extended if slow response; contact microbiology Infected insect/ tick bites or stings local reactions papular urticarial systemic allergic reaction Erythema migrans rash Most local reactions to insect/tick bites or stings can be managed symptomatically; only treat with antibiotics if infected. If a tick is still attached, remove it. Tick bites: Consider micro/id consultation and advise review by a doctor for consideration of antibiotics if they develop any symptoms of Lyme disease. For people who do not have an erythema migrans rash but have symptoms suggestive of Lyme disease and a recent history of a tick bite or possible exposure to ticks, test for antibodies to Borrelia burgdorferi. Doxycycline 100mg 12hourly PO Infected insect bite: 7 days Infected tick bite/ erythema migrans rash: days
7 Superficial abscesses, boils and carbuncles Painful, tender, and fluctuant red nodules, often surmounted by a pustule and encircled by a rim of erythematous swelling. Gram stain and culture of pus from carbuncles and abscesses are recommended Treat with Incision and drainage as soon as possible. The decision to administer antibiotics as an adjunct to incision and drainage should be made based on if: o Severe or rapidly progressive infections o The presence of extensive associated cellulitis o symptoms of systemic illness o Associated septic phlebitis o Diabetes or other immune suppression o Advanced age o Location of the abscess in an area where complete drainage is difficult (e.g. face, genitalia) o Lack of response to incision and drainage alone A recurrent abscess at a site of previous infection should prompt a search for local causes such as a pilonidal cyst, hidradenitis suppurativa, or foreign material. Flucloxacillin 1g 6 hourly PO Clarithromycin 500mg 12 hourly PO Continue antibiotics until drained.
8 Surgical wound infections pain, swelling, erythema, and purulent drainage Send blood and culture of the exudate if patient is febrile. Wound infections associated with cellulitis alone (i.e., no fluctuance) can be treated with a course of antibiotics without open drainage. Suture removal plus incision and drainage should be performed for surgical site infections Adjunctive systemic antimicrobial therapy is not routinely indicated, but in conjunction with incision and drainage may be beneficial for surgical site infections associated with a significant systemic response, such as erythema and induration extending >5 cm from the wound edge, temperature 38.5 C, heart rate >110 beats/minute, or white blood cell (WBC) count >12 Addition of metronidazole is recommended for infections following operations on the axilla, gastrointestinal tract, perineum, or female genital tract Superficial infections: treat as cellulitis guidelines Deeper infections: e.g. suspected collection/abscess, treat as per Intraabdominal sepsis +/- collections guidelines under The Trust Antibiotic Guidelines for GASTRO-INTESTINAL INFECTIONS Burn wound infections Blood cultures when indicated Swabs Treatment not recommended for colonisation, only if burn wound cellulitis or sepsis. Discuss with microbiology when swab results available. Piperacillin/Tazobactam 4.5g 8 If MRSA add: IV Teicoplanin as prescription chart IV Teicoplanin as prescription chart Ciprofloxacin 600mg 12 Metronidazole 500mg days
9 Tissue infection in IV drug abusers Blood cultures when indicated Swabs Blood borne viruses If abscess, requires incision and drainage. Consider anthrax in any drug user who presents with: o Severe soft tissue infection, particularly if associated with tissue oedema (often marked). This can present as a compartment syndrome. o Signs of severe sepsis even without evidence of soft tissue infection o Meningitis (particularly haemorrhagic meningitis). Also be suspicious if drug users present/ have CT evidence suggestive of subarachnoid haemorrhage/ intracranial bleed) o symptoms of inhalational anthrax Flu-like illness, progressing to severe respiratory difficulties and shock CXR signs Progressively enlarging haemorrhagic pleural effusions are a consistent feature Respiratory symptoms may also be accompanied by signs and symptoms suggesting meningitis or intracranial bleeding in the rapidly advancing stages of the disease process due to haematogenous spread Cases of disseminated anthrax may present with a variety of symptoms such as abdominal pain, nausea, D&V, GI haemorrhage, ascites etc., suggestive of either GI involvement or actual GI anthrax. Assess tetanus risk and manage appropriately. If pyomyositis or severe-contact microbiology. Flucloxacillin 1g 6 hourly PO Metronidazole 400mg 8 hourly PO If suspected anthraxcontact microbiology for advice. Doxycycline 100mg 12 hourly PO Metronidazole 400mg 8 hourly PO If suspected anthrax-contact microbiology for advice days
10 Puncture wound Or Contaminated wound Surgical specimens for culture Marine Infection A careful history is required to manage the patient and to identify risk factors for complications of the puncture injury. Cleanse thoroughly and evaluate wound for the presence of foreign bodies. Surgical debridement or abscess drainage is an important component of treatment of infected puncture wounds. For tetanus prone wound, give human tetanus immunoglobulin with absorbed diphtheria (low dose) and tetanus vaccine, according to immunization history. Following puncture injury antibiotic prophylaxis can be administered in high risk patients e.g. Forefoot injury, Wearing shoes at the time of the injury, Diabetes mellitus. Many more potential pathogens compared to nonmarine injury including Aeromonas, Edwardsiella tarda, Erysipelothrix rhusiopathiae, Vibrio vulnificus, Mycobacterium marinum Empiric antibiotic coverage does not include coverage for M. marinum infection, since the presentation is subacute and without associated Co-amoxiclav 625mg 8 hourly PO Or 1.2g 8 If plantar puncture wound, ear cartilage wound, farmyard injury or not settling within 48hrs: Piperacillin/Tazobactam 4.5g 8 Cephalexin 500 mg 6 hourly PO OR Cefazolin 1g 8 Levofloxacin 750 mg once daily PO/IV Co-trimoxazole 960mg PO (960mg-1.44g IV) 12 hourly Metronidazole 400mg PO ( 500mg IV) 8 hourly If plantar puncture wound, ear cartilage wound, farmyard injury or not settling within 48hrs: IV Teicoplanin as prescription chart Ciprofloxacin 600mg 12 Metronidazole 500mg 8 Clindamycin 300mg 6 hourly PO OR 600mg 8 Levofloxacin 750 mg once daily PO/IV Prophylaxis: 3-5 days Treatment of contaminate d wound: 7-14 days days For Mycobacteri um marinum d/w ID/respirator y
11 systemic toxicity. A specimen (e.g. lesion aspirate, biopsy) should be obtained and the microbiology laboratory notified that M. marinum is suspected so that appropriate culture conditions will be included. If acid-fast staining is positive or if the exposure history and physical examination findings suggest M. marinum infection (e.g. laceration from an aquarium), then we suggest that specific treatment for M. marinum infection should be initiated. Metronidazole 500 mg 6 hourly PO/IV (if exposure to sewagecontaminated water or if soil-contaminated wound) OR Doxycycline 100 mg 12 hourly PO for coverage of Vibrio species if seawater exposure Doxycycline 100 mg 12 hourly PO for coverage of Vibrio species if seawater exposure For tetanus prone wound, give human tetanus immunoglobulin with absorbed diphtheria (low dose) and tetanus vaccine, according to immunization history.
12 Associated underlying/ open fracture See Surgical Prophylaxis guidelines
13 Title: Author: CLINICAL GUIDELINES ID TAG Antibiotic Guidelines for Skin and Soft tissue Infection Dr M Brown, Mrs A McCorry Speciality / Division: Directorate: Microbiology, Pharmacy, MUSC Acute Date Uploaded: 21 st August 2017 Review Date September 2018 Clinical Guideline ID CG0477 References: 1. Practice Guidelines for the Diagnosis and Management of Skin and Soft Tissue Infections: 2014 Update by the Infectious Diseases Society of America. June NICE Cellulitis - Scenario: Management of acute cellulitis. 3. NICE Impetigo - Scenario: Management of impetigo. 4. Diagnosis and Treatment of Impetigo. Am Fam Physician Mar 15;75(6): Accessed June NICE Bites - human and animal. Assessing a bite/managing a human bite/ 7. NICE Leg ulcer - Scenario: Infected venous leg ulcer. 8. NICE Lyme disease-scenario: Management of Lyme Disease. 9. NICE Insect bites and stings-scenario: Infection Accessed July 2017.
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Diabetic Foot Infection. Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals
 Diabetic Foot Infection Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals History of previous amputation [odds ratio (OR)=19.9, P=.01], Peripheral vascular disease (OR=5.5, P=.007)
Diabetic Foot Infection Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals History of previous amputation [odds ratio (OR)=19.9, P=.01], Peripheral vascular disease (OR=5.5, P=.007)
CELLULITIS / SKIN INFECTIONS
 Skin Infections Assessment Investigations Cellulitis Management Abscess Management Infection Control Antibiotic Choice Education Recurrent Infections Referral to Community Nursing References Skin Infections
Skin Infections Assessment Investigations Cellulitis Management Abscess Management Infection Control Antibiotic Choice Education Recurrent Infections Referral to Community Nursing References Skin Infections
Author s: Clinical Standards Group and Effectiveness Sub-Board
 Trust Antibiotic Policy for the Management of Common Infections in Accident and Emergency and Cromer Minor Injuries Unit (Paediatrics) Accident and Emergency, Norfolk and Norwich and For Use in: Cromer
Trust Antibiotic Policy for the Management of Common Infections in Accident and Emergency and Cromer Minor Injuries Unit (Paediatrics) Accident and Emergency, Norfolk and Norwich and For Use in: Cromer
Dirty Wounds. Christopher M. Ziebell, MD, FACEP
 Dirty Wounds Christopher M. Ziebell, MD, FACEP Types Fresh Water Salt Water Bites Cats Humans Dogs and other mammals Freshwater Trauma Recognize this finger? Lindsey Lohan Microbiology Usual suspects:
Dirty Wounds Christopher M. Ziebell, MD, FACEP Types Fresh Water Salt Water Bites Cats Humans Dogs and other mammals Freshwater Trauma Recognize this finger? Lindsey Lohan Microbiology Usual suspects:
INFECTIONS IN CHILDREN-ANTIMICROBIAL MANAGEMENT
 INFECTIONS IN CHILDREN-ANTIMICROBIAL MANAGEMENT Name & Title Of Authors: Dr M Milupi, Consultant Microbiologist Dr N Rao,Consultant Paediatrician Dr V Desai Consultant Paediatrician Date Revised: DEC 2015
INFECTIONS IN CHILDREN-ANTIMICROBIAL MANAGEMENT Name & Title Of Authors: Dr M Milupi, Consultant Microbiologist Dr N Rao,Consultant Paediatrician Dr V Desai Consultant Paediatrician Date Revised: DEC 2015
INFECTIONS IN CHILDREN-ANTIMICROBIAL MANAGEMENT
 INFECTIONS IN CHILDREN-ANTIMICROBIAL MANAGEMENT Name & Title Of Authors: Dr M Milupi, Consultant Microbiologist Dr N Rao,Consultant Paediatrician Dr V Desai Consultant Paediatrician Date Revised: APRIL
INFECTIONS IN CHILDREN-ANTIMICROBIAL MANAGEMENT Name & Title Of Authors: Dr M Milupi, Consultant Microbiologist Dr N Rao,Consultant Paediatrician Dr V Desai Consultant Paediatrician Date Revised: APRIL
Perichondritis: Source: UpToDate Ciprofloxacin 10 mg/kg/dose PO (max 500 mg/dose) BID Inpatient: Ceftazidime 50 mg/kg/dose q8 hours IV
 Empiric Antibiotics for Pediatric Infections Seen in ED NOTE: Choice of empiric antibiotic therapy must take into account local pathogen frequency and resistance patterns, individual patient characteristics,
Empiric Antibiotics for Pediatric Infections Seen in ED NOTE: Choice of empiric antibiotic therapy must take into account local pathogen frequency and resistance patterns, individual patient characteristics,
DRAFT DRAFT. Paediatric Antibiotic Prescribing Guideline. May
 Paediatric Antibiotic Prescribing Guideline www.oxfdahsn.g/children Magdalen Centre Nth, 1 Robert Robinson Avenue, Oxfd Science Park, OX4 4GA, United Kingdom t: +44(0) 1865 784944 e: info@oxfdahsn.g Follow
Paediatric Antibiotic Prescribing Guideline www.oxfdahsn.g/children Magdalen Centre Nth, 1 Robert Robinson Avenue, Oxfd Science Park, OX4 4GA, United Kingdom t: +44(0) 1865 784944 e: info@oxfdahsn.g Follow
Symptoms of cellulitis (n=396) %
 Cellulitis and lymphoedema Vaughan Keeley May 2012 What is cellulitis? - also called erysipelas, acute inflammatory episodes etc. - bacterial infection of skin + subcutaneous tissues - more common in people
Cellulitis and lymphoedema Vaughan Keeley May 2012 What is cellulitis? - also called erysipelas, acute inflammatory episodes etc. - bacterial infection of skin + subcutaneous tissues - more common in people
Necrotizing Soft Tissue Infections: Emerging Bacterial Resistance
 Necrotizing Soft Tissue Infections: Emerging Bacterial Resistance Eileen M. Bulger, MD Professor of Surgery Harborview Medical Center University of Washington Objectives Review definition & diagnostic
Necrotizing Soft Tissue Infections: Emerging Bacterial Resistance Eileen M. Bulger, MD Professor of Surgery Harborview Medical Center University of Washington Objectives Review definition & diagnostic
PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust
 PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust Neonatal Case History Neonate born at 26 +2 gestation Spontaneous onset of
PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust Neonatal Case History Neonate born at 26 +2 gestation Spontaneous onset of
Guidelines for the Empirical Treatment of Sepsis in Adults (excluding Neutropenic Sepsis)
 Guidelines for the Empirical Treatment of Sepsis in Adults (excluding Neutropenic Sepsis) Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state
Guidelines for the Empirical Treatment of Sepsis in Adults (excluding Neutropenic Sepsis) Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state
CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II page 1
 CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II 1. What are the symptoms of an infected wound? a. Fever b. Edema c. Erythema d. Local pain and tenderness e. Induration of wound edge 2. A person with
CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II 1. What are the symptoms of an infected wound? a. Fever b. Edema c. Erythema d. Local pain and tenderness e. Induration of wound edge 2. A person with
Treatment of Surgical Site Infection Meeting Quality Statement 6. Prof Peter Wilson University College London Hospitals
 Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Surgical Site Infections (SSIs)
 Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Cellulitis. Assoc Prof Mark Thomas. Conference for General Practice Auckland Saturday 28 July 2018
 Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Guidelines for the Medical management of Diabetic Foot Infection
 Guidelines for the Medical management of Diabetic Foot Infection Introduction and summary points - Foot infections in diabetic patients usually begin with skin ulceration - However, skin wounds with no
Guidelines for the Medical management of Diabetic Foot Infection Introduction and summary points - Foot infections in diabetic patients usually begin with skin ulceration - However, skin wounds with no
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT DRAFT AS CURRENTLY OUT FOR CONSULTATION BUT CAN BE UTILISED IN PRESENT FORMAT Name & Title Of Author: Date Revised: Approved by Committee/Group:
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT DRAFT AS CURRENTLY OUT FOR CONSULTATION BUT CAN BE UTILISED IN PRESENT FORMAT Name & Title Of Author: Date Revised: Approved by Committee/Group:
Skin and Soft Tissue Infections (SSTI) Antibiotic Guidelines (Adult) Contents. Section
 Antibiotic Guidelines (Adult) Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine Unique ID: 144TD(C)25(B3) Issue
Antibiotic Guidelines (Adult) Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine Unique ID: 144TD(C)25(B3) Issue
S aureus infections: outpatient treatment. Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium
 S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children
 Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children Prescribing Antimicrobials for Common Illnesses When treating common illnesses such as ear infections and strep throat,
Prescribing Guidelines for Outpatient Antimicrobials in Otherwise Healthy Children Prescribing Antimicrobials for Common Illnesses When treating common illnesses such as ear infections and strep throat,
Antibiotic Prophylaxis in Spinal Surgery Antibiotic Guidelines. Contents
 Antibiotic Prophylaxis in Spinal Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine Unique
Antibiotic Prophylaxis in Spinal Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine Unique
Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CONTROLLED DOCUMENT
 CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
IAEM Clinical Guideline 6 Bite Wound Management in Adults and Children Version 1 July 2016
 IAEM Clinical Guideline 6 Bite Wound Management in Adults and Children Version 1 July 2016 Authors: Dr Sinead Ni Bhraonain, Dr Jessica Pflipsen, Dr Éanna Mac Suibhne Guideline lead: Dr Termizi Hassan,
IAEM Clinical Guideline 6 Bite Wound Management in Adults and Children Version 1 July 2016 Authors: Dr Sinead Ni Bhraonain, Dr Jessica Pflipsen, Dr Éanna Mac Suibhne Guideline lead: Dr Termizi Hassan,
Who should read this document? 2. Key practice points 2. Background/ Scope/ Definitions 2. What is new in this version? 3
 Neurosurgical infections (adult only) Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): as above Authors Division: DCSS & Tertiary
Neurosurgical infections (adult only) Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): as above Authors Division: DCSS & Tertiary
GUIDELINE FOR ANTIMICROBIAL USE IN THE ORTHOPAEDIC AND TRAUMA DEPARTMENT
 GUIDELINE FOR ANTIMICROBIAL USE IN THE ORTHOPAEDIC AND TRAUMA DEPARTMENT Written by: Dr Ken. N. Agwuh, Consultant Microbiologist Mr Roger Helm, Consultant Orthopaedic Surgeon Mr T Kumar, Consultant Orthopaedic
GUIDELINE FOR ANTIMICROBIAL USE IN THE ORTHOPAEDIC AND TRAUMA DEPARTMENT Written by: Dr Ken. N. Agwuh, Consultant Microbiologist Mr Roger Helm, Consultant Orthopaedic Surgeon Mr T Kumar, Consultant Orthopaedic
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare
 Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults)
 Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults) Community Acquired Pneumonia Community Acquired Pneumonia 1) Is it pneumonia? ie new symptoms and signs of
Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults) Community Acquired Pneumonia Community Acquired Pneumonia 1) Is it pneumonia? ie new symptoms and signs of
Replaces:04/14/16. Formulated: 1997 SKIN AND SOFT TISSUE INFECTION
 Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Mrsa abscess and cellulitis
 Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
Search Mrsa abscess and cellulitis An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The. Staph
Provincial Drugs & Therapeutics Committee Memorandum Version 2
 Provincial Drugs & Therapeutics Committee Memorandum Version 2 16 Garfield Street 16, rue Garfield PO Box 2000, Charlottetown C.P. 2000, Charlottetown Prince Edward Island Île-du-Prince-Édouard Canada
Provincial Drugs & Therapeutics Committee Memorandum Version 2 16 Garfield Street 16, rue Garfield PO Box 2000, Charlottetown C.P. 2000, Charlottetown Prince Edward Island Île-du-Prince-Édouard Canada
Health PEI: Provincial Antibiotic Advisory Team Empiric Antibiotic Treatment Guidelines for Sepsis Syndromes in Adults
 Health PEI: Provincial Antibiotic Advisory Team Empiric Antibiotic Treatment Guidelines for Sepsis Syndromes in Adults COMMUNITY-ACQUIRED PNEUMONIA HEALTHCARE-ASSOCIATED PNEUMONIA INTRA-ABDOMINAL INFECTION
Health PEI: Provincial Antibiotic Advisory Team Empiric Antibiotic Treatment Guidelines for Sepsis Syndromes in Adults COMMUNITY-ACQUIRED PNEUMONIA HEALTHCARE-ASSOCIATED PNEUMONIA INTRA-ABDOMINAL INFECTION
ANTIBIOTIC PRESCRIBING POLICY FOR DIABETIC FOOT DISEASE IN SECONDARY CARE
 ANTIBIOTIC PRESCRIBING POLICY FOR DIABETIC FOOT DISEASE IN SECONDARY CARE Version 1.0 Date ratified June 2009 Review date June 2011 Ratified by Authors Consultation Nottingham Antibiotic Guidelines Committee
ANTIBIOTIC PRESCRIBING POLICY FOR DIABETIC FOOT DISEASE IN SECONDARY CARE Version 1.0 Date ratified June 2009 Review date June 2011 Ratified by Authors Consultation Nottingham Antibiotic Guidelines Committee
Invasive Group A Streptococcus (GAS)
 Invasive Group A Streptococcus (GAS) Cause caused by a bacterium commonly found on the skin and in the throat transmitted by direct, indirect or droplet contact with secretions from the nose, and throat
Invasive Group A Streptococcus (GAS) Cause caused by a bacterium commonly found on the skin and in the throat transmitted by direct, indirect or droplet contact with secretions from the nose, and throat
Diagnosis and Management of Skin and Soft-tissue Infections
 Diagnosis and Management of Skin and Soft-tissue Infections Skin and soft tissue infections (SSTIs), are referred as skin and skin structure infections. These infections also represent a group of infections
Diagnosis and Management of Skin and Soft-tissue Infections Skin and soft tissue infections (SSTIs), are referred as skin and skin structure infections. These infections also represent a group of infections
Central Nervous System Infections
 Central Nervous System Infections Meningitis Treatment Bacterial meningitis is a MEDICAL EMERGENCY. ANTIBIOTICS SHOULD BE STARTED AS SOON AS THE POSSIBILITY OF BACTERIAL MENINGITIS BECOMES EVIDENT, IDEALLY
Central Nervous System Infections Meningitis Treatment Bacterial meningitis is a MEDICAL EMERGENCY. ANTIBIOTICS SHOULD BE STARTED AS SOON AS THE POSSIBILITY OF BACTERIAL MENINGITIS BECOMES EVIDENT, IDEALLY
10/13/14. Low: not well absorbed. Good: [blood and tissue] < than if given IV. High: > 90% absorption orally
![10/13/14. Low: not well absorbed. Good: [blood and tissue] < than if given IV. High: > 90% absorption orally 10/13/14. Low: not well absorbed. Good: [blood and tissue] < than if given IV. High: > 90% absorption orally](/thumbs/79/80222162.jpg) Low: not well absorbed PO agent not for serious infection nitrofurantoin Good: [blood and tissue] < than if given IV [Therapeutic] in excess of [effective] eg. cephalexin High: > 90% absorption orally
Low: not well absorbed PO agent not for serious infection nitrofurantoin Good: [blood and tissue] < than if given IV [Therapeutic] in excess of [effective] eg. cephalexin High: > 90% absorption orally
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Women s Antimicrobial Guidelines Summary
 Women s Antimicrobial Guidelines Summary 1. Introduction and Who Guideline applies to This guideline has been developed to deliver safe and appropriate empirical use of antibiotics for patients at University
Women s Antimicrobial Guidelines Summary 1. Introduction and Who Guideline applies to This guideline has been developed to deliver safe and appropriate empirical use of antibiotics for patients at University
Septicaemia Definitions 1
 Septicaemia Definitions 1 Term Definition Bacteraemia Systemic Inflammatory response (SIRS) Sepsis Bacteria that can be cultured from the blood stream The systemic response to a wide range of stresses.
Septicaemia Definitions 1 Term Definition Bacteraemia Systemic Inflammatory response (SIRS) Sepsis Bacteria that can be cultured from the blood stream The systemic response to a wide range of stresses.
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Infection Comments First Line Agents Penicillin Allergy History of multiresistant. line treatment: persist for >7 days they may be
 Gastrointestinal Infections Infection Comments First Line Agents Penicillin Allergy History of multiresistant Campylobacter Antibiotics not recommended. Erythromycin 250mg PO 6 Alternative to first N/A
Gastrointestinal Infections Infection Comments First Line Agents Penicillin Allergy History of multiresistant Campylobacter Antibiotics not recommended. Erythromycin 250mg PO 6 Alternative to first N/A
Copyright 2012 Diabetes In Control, Inc. For permission to reprint, please contact Heather Moran, Production Editor, at
 Malignant Otitis Externa Inflammation and damage at the base of the skull due to an untreated outer ear P. aeruginosa most common organism Yellow-green drainage from the ear Odor Fever Deep inner ear pain
Malignant Otitis Externa Inflammation and damage at the base of the skull due to an untreated outer ear P. aeruginosa most common organism Yellow-green drainage from the ear Odor Fever Deep inner ear pain
Infection/Wound & Dressings
 Infection/Wound & Dressings Wendy McInnes ; Vascular Nurse Practitioner The Lyell McEwin Hospital, Adelaide, South Australia wendy.mcinnes@sa,gov.au 0447 051 036 WIFi Foot Infection Clinical Manifestation
Infection/Wound & Dressings Wendy McInnes ; Vascular Nurse Practitioner The Lyell McEwin Hospital, Adelaide, South Australia wendy.mcinnes@sa,gov.au 0447 051 036 WIFi Foot Infection Clinical Manifestation
Full Title of Guideline. Author: Contact Name and Job Title. Division & Speciality. Review date December 2020
 Full Title of Guideline Author: Contact Name and Job Title Division & Speciality Guideline for the treatment of prosthetic joint infections in adults Mr Peter James - Consultant Orthopaedic Surgeon Dr
Full Title of Guideline Author: Contact Name and Job Title Division & Speciality Guideline for the treatment of prosthetic joint infections in adults Mr Peter James - Consultant Orthopaedic Surgeon Dr
Skin and Soft Tissue Infections
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 28: Skin and Soft Tissue Infections Author Antoni Trilla, MD, PhD, MSc Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Topic Outline Staphylococcal Skin
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 28: Skin and Soft Tissue Infections Author Antoni Trilla, MD, PhD, MSc Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Topic Outline Staphylococcal Skin
Similar to Penicillins: -Chemically. -Mechanism of action. -Toxicity.
 Similar to Penicillins: -Chemically. -Mechanism of action. -Toxicity. Cephalosporins are divided into Generations: -First generation have better activity against gram positive organisms. -Later compounds
Similar to Penicillins: -Chemically. -Mechanism of action. -Toxicity. Cephalosporins are divided into Generations: -First generation have better activity against gram positive organisms. -Later compounds
SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS
 SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if
SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if
your hospitals, your health, our priority PARC (Policy Approval and Ratification Committee) STANDARD OPERATING PROCEDURE:
 STANDARD OPERATING PROCEDURE: TRUST ANTIBIOTIC TREATMENT SOP SOP NO: TW10/136 SOP 1 VERSION NO: VERSION 6.1 (JANUARY 2013) APPROVING COMMITTEE: INFECTION PREVENTION AND CONTROL COMMITTEE DATE THIS VERSION
STANDARD OPERATING PROCEDURE: TRUST ANTIBIOTIC TREATMENT SOP SOP NO: TW10/136 SOP 1 VERSION NO: VERSION 6.1 (JANUARY 2013) APPROVING COMMITTEE: INFECTION PREVENTION AND CONTROL COMMITTEE DATE THIS VERSION
11/10/2016. Skin and Soft Tissue Infections. Disclosures. Educational Need/Practice Gap. Objectives. Case #1
 Disclosures Selecting Antimicrobials for Common Infections in Children FMR-Contemporary Pediatrics 11/2016 Sean McTigue, MD Assistant Professor of Pediatrics, Pediatric Infectious Diseases Medical Director
Disclosures Selecting Antimicrobials for Common Infections in Children FMR-Contemporary Pediatrics 11/2016 Sean McTigue, MD Assistant Professor of Pediatrics, Pediatric Infectious Diseases Medical Director
PRACTIC GUIDELINES for APPROPRIATE ANTIBIOTICS USE
 PRACTIC GUIDELINES for APPROPRIATE ANTIBIOTICS USE Global Alliance for Infection in Surgery World Society of Emergency Surgery (WSES) and not only!! Aims - 1 Rationalize the risk of antibiotics overuse
PRACTIC GUIDELINES for APPROPRIATE ANTIBIOTICS USE Global Alliance for Infection in Surgery World Society of Emergency Surgery (WSES) and not only!! Aims - 1 Rationalize the risk of antibiotics overuse
HEALTH SERVICES POLICY & PROCEDURE MANUAL
 PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
PAGE 1 of 3 PURPOSE To assure that DOP inmates with Soft Tissue Infections are receiving high quality Primary Care for their infections and that the risk of infecting other inmates or staff is minimized.
Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults)
 Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults) Community Acquired Community Acquired 1) Is it pneumonia? ie new symptoms and signs of a lower respiratory
Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults) Community Acquired Community Acquired 1) Is it pneumonia? ie new symptoms and signs of a lower respiratory
PIPERACILLIN- TAZOBACTAM INJECTION - SUPPLY PROBLEMS
 PIPERACILLIN- TAZOBACTAM INJECTION - SUPPLY PROBLEMS The current supply of piperacillin- tazobactam should be reserved f Microbiology / Infectious Diseases approval and f neutropenic sepsis, severe sepsis
PIPERACILLIN- TAZOBACTAM INJECTION - SUPPLY PROBLEMS The current supply of piperacillin- tazobactam should be reserved f Microbiology / Infectious Diseases approval and f neutropenic sepsis, severe sepsis
Tropical infections caused by Staphylococcus aureus
 Tropical infections caused by Staphylococcus aureus Michael Ellis, MD Infectious Diseases Division Uniformed Services University of the Health Sciences February 2015 Introduction Tropical Pyomyositis Cutaneous
Tropical infections caused by Staphylococcus aureus Michael Ellis, MD Infectious Diseases Division Uniformed Services University of the Health Sciences February 2015 Introduction Tropical Pyomyositis Cutaneous
Antimicrobial Update. Alison MacDonald Area Antimicrobial Pharmacist NHS Highland April 2018
 Antimicrobial Update Alison MacDonald Area Antimicrobial Pharmacist NHS Highland alisonc.macdonald@nhs.net April 2018 Starter Questions Setting the scene... What if antibiotics were no longer effective?
Antimicrobial Update Alison MacDonald Area Antimicrobial Pharmacist NHS Highland alisonc.macdonald@nhs.net April 2018 Starter Questions Setting the scene... What if antibiotics were no longer effective?
Antibiotic Abyss. Discussion Points. MRSA Treatment Guidelines
 Antibiotic Abyss Fredrick M. Abrahamian, D.O., FACEP, FIDSA Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical Center Sylmar, California
Antibiotic Abyss Fredrick M. Abrahamian, D.O., FACEP, FIDSA Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical Center Sylmar, California
Rational management of community acquired infections
 Rational management of community acquired infections Dr Tanu Singhal MD, MSc Consultant Pediatrics and Infectious Disease Kokilaben Dhirubhai Ambani Hospital, Mumbai Why is rational management needed?
Rational management of community acquired infections Dr Tanu Singhal MD, MSc Consultant Pediatrics and Infectious Disease Kokilaben Dhirubhai Ambani Hospital, Mumbai Why is rational management needed?
Antimicrobial Prophylaxis in the Surgical Patient. M. J. Osgood
 Antimicrobial Prophylaxis in the Surgical Patient M. J. Osgood Outline Definitions surgical site infection (SSI) Risk factors Wound classification Microbiology of SSIs Strategies for prevention of SSIs
Antimicrobial Prophylaxis in the Surgical Patient M. J. Osgood Outline Definitions surgical site infection (SSI) Risk factors Wound classification Microbiology of SSIs Strategies for prevention of SSIs
Who should read this document 2. Key practice points 2. Background/ Scope/ Definitions 2. What is new in this version 3. Policy/Procedure/Guideline 3
 Antibiotic Prophylaxis in Cranial Neurosurgery Antibiotic Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): as above Authors Division: DCSS & Tertiary
Antibiotic Prophylaxis in Cranial Neurosurgery Antibiotic Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): as above Authors Division: DCSS & Tertiary
COALINGA STATE HOSPITAL. NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF WOUNDS (FIRST AID) 1. PURPOSE: Proper
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF WOUNDS (FIRST AID) 1. PURPOSE: Proper
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS
 VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
Scottish Medicines Consortium
 Scottish Medicines Consortium daptomycin 350mg powder for concentrate for solution for infusion (Cubicin ) Chiron Corporation Limited No. (248/06) 10 March 2006 The Scottish Medicines Consortium (SMC)
Scottish Medicines Consortium daptomycin 350mg powder for concentrate for solution for infusion (Cubicin ) Chiron Corporation Limited No. (248/06) 10 March 2006 The Scottish Medicines Consortium (SMC)
5/17/2012 DISCLOSURES OBJECTIVES CONTEMPORARY PEDIATRICS
 CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
Skin & Soft Tissue Infections (SSTIs)
 Skin & Soft Tissue Infections (SSTIs) Marnie Peterson, Pharm.D., Ph.D. College of Pharmacy peter377@umn.edu (612) 626-4388 SSTIs Objectives To classify types of skin infections To present a case of cellulitis
Skin & Soft Tissue Infections (SSTIs) Marnie Peterson, Pharm.D., Ph.D. College of Pharmacy peter377@umn.edu (612) 626-4388 SSTIs Objectives To classify types of skin infections To present a case of cellulitis
Appropriate Management of Common Pediatric Infections. Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases
 Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
Paediatric Empirical Antimicrobial Guidance for Infections in Hospital
 Paediatric Empirical Antimicrobial Guidance for Infections in Hospital This guidance is for empirical treatment. Alternative antibiotics may be required if specific pathogens are identified or there is
Paediatric Empirical Antimicrobial Guidance for Infections in Hospital This guidance is for empirical treatment. Alternative antibiotics may be required if specific pathogens are identified or there is
CLINICAL USE OF BETA-LACTAMS
 CLINICAL USE OF BETA-LACTAMS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu WHY IS INFECTIOUS DISEASE PHARMACOTHERAPY SO CONFUSING? Microbial
CLINICAL USE OF BETA-LACTAMS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu WHY IS INFECTIOUS DISEASE PHARMACOTHERAPY SO CONFUSING? Microbial
21 st Expert Committee on Selection and Use of Essential Medicines Peer Review Report Antibiotics Review
 (1) Have all important studies/evidence of which you are aware been included in the application? Yes No Please provide brief comments on any relevant studies that have not been included: (2) For each of
(1) Have all important studies/evidence of which you are aware been included in the application? Yes No Please provide brief comments on any relevant studies that have not been included: (2) For each of
Overview Management of Skin and Soft Tissue Infections in the MRSA Era
 Overview Management of Skin and Soft Tissue Infections in the MRSA Era April 2011 2011 IDSA MRSA Treatment Guidelines Skin and soft tissue infections (SSTIs) Management of Recurrent SSTIs Necrotizing soft
Overview Management of Skin and Soft Tissue Infections in the MRSA Era April 2011 2011 IDSA MRSA Treatment Guidelines Skin and soft tissue infections (SSTIs) Management of Recurrent SSTIs Necrotizing soft
Remember: AIEs are painful: analgesics should be prescribed regularly and p.r.n. palliativedrugs.com November/December newsletter
 ACUTE INFLAMMATORY EPISODES IN A LYMPHOEDEMATOUS LIMB Acute inflammatory episodes (AIEs), often called cellulitis, are common in lymphoedema: mild: pain, increased swelling, erythema (well-defined or blotchy)
ACUTE INFLAMMATORY EPISODES IN A LYMPHOEDEMATOUS LIMB Acute inflammatory episodes (AIEs), often called cellulitis, are common in lymphoedema: mild: pain, increased swelling, erythema (well-defined or blotchy)
General Approach to Infectious Diseases
 General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
General Approach to Infectious Diseases 2 The pharmacotherapy of infectious diseases is unique. To treat most diseases with drugs, we give drugs that have some desired pharmacologic action at some receptor
Delayed Prescribing for Minor Infections Resource Pack for Prescribers
 Delayed Prescribing for Minor Infections Resource Pack for Prescribers Background: Antibiotic resistance is an alarming threat to modern healthcare, and infectious illness remains a major global threat
Delayed Prescribing for Minor Infections Resource Pack for Prescribers Background: Antibiotic resistance is an alarming threat to modern healthcare, and infectious illness remains a major global threat
Risk factors? Insect bites? Hygiene? Household crowding Health literacy
 Recurrent boils Commonest sites face, neck, armpits, shoulders, and buttocks (bottom) infection of the hair root or sweat pore Occur in otherwise healthy people (higher rates in diabetics, eczema, iron
Recurrent boils Commonest sites face, neck, armpits, shoulders, and buttocks (bottom) infection of the hair root or sweat pore Occur in otherwise healthy people (higher rates in diabetics, eczema, iron
THERAPY OF ANAEROBIC INFECTIONS LUNG ABSCESS BRAIN ABSCESS
 THERAPY OF ANAEROBIC INFECTIONS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu LUNG ABSCESS A lung abscess is a localized pus cavity in
THERAPY OF ANAEROBIC INFECTIONS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu LUNG ABSCESS A lung abscess is a localized pus cavity in
Antimicrobial Update Stewardship in Primary Care. Clare Colligan Antimicrobial Pharmacist NHS Forth Valley
 Antimicrobial Update Stewardship in Primary Care Clare Colligan Antimicrobial Pharmacist NHS Forth Valley Setting the Scene! Consequences of Antibiotic Use? Resistance For an individual patient with
Antimicrobial Update Stewardship in Primary Care Clare Colligan Antimicrobial Pharmacist NHS Forth Valley Setting the Scene! Consequences of Antibiotic Use? Resistance For an individual patient with
Antibiotic stewardship in long term care
 Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Cellulitis and Abscess: ED Phase v 1.1
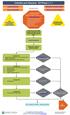 Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
Cellulitis and Abscess: ED Phase v 1.1 Executive Summary Test Your Knowledge PHASE I (E.D.) Explanation of Evidence Ratings Summary of Version Changes! Labs if systemic illness or necrotizing fasciitis
Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS
 Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care Dell Seton Medical Center at the University of Texas and Seton Healthcare Family Clinical
Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care Dell Seton Medical Center at the University of Texas and Seton Healthcare Family Clinical
Disclosures. Consider This Case. Objectives. Consequences of Bites. Animal Bites: What to Do and What to Avoid. Animal Bites: Epidemiology
 Animal Bites: What to Do and What to Avoid Meg Fisher, MD Medical Director Disclosures I have no disclosures I do not plan to discuss off label uses of drugs Objectives Manage a child who is bitten Discuss
Animal Bites: What to Do and What to Avoid Meg Fisher, MD Medical Director Disclosures I have no disclosures I do not plan to discuss off label uses of drugs Objectives Manage a child who is bitten Discuss
COMMUNITY ASSOCIATED METHICILLIN-RESISTANT STAPHLOCOCCUS AUREUS A PRACTICAL GUIDE FOR PRIMARY CARE PRACTITIONERS
 COMMUNITY ASSOCIATED METHICILLIN-RESISTANT STAPHLOCOCCUS AUREUS A PRACTICAL GUIDE FOR PRIMARY CARE PRACTITIONERS December 21, 2010 Background Since it was first described in 1961 methicillin resistant
COMMUNITY ASSOCIATED METHICILLIN-RESISTANT STAPHLOCOCCUS AUREUS A PRACTICAL GUIDE FOR PRIMARY CARE PRACTITIONERS December 21, 2010 Background Since it was first described in 1961 methicillin resistant
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan. Associate Consultant Infectious Disease Centre, PMH
 Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
Infections caused by Methicillin-Resistant Staphylococcus
 MRSA infections are no longer limited to hospitals. An infectious disease specialist offers insight on what this means for dermatologists. By Robert S. Jones, DO, Reading, PA Infections caused by Methicillin-Resistant
MRSA infections are no longer limited to hospitals. An infectious disease specialist offers insight on what this means for dermatologists. By Robert S. Jones, DO, Reading, PA Infections caused by Methicillin-Resistant
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS
 Version 3.1 GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS Date ratified June 2008 Updated March 2009 Review date June 2010 Ratified by Authors Consultation Evidence base Changes
Version 3.1 GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED PNEUMONIA IN ADULTS Date ratified June 2008 Updated March 2009 Review date June 2010 Ratified by Authors Consultation Evidence base Changes
Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC
 Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC APPROVED BY: Policy and Guidelines Committee TRUST REFERENCE: B9/2009 AWP Ref: AWP61 Date (approved): July 2008 REVIEW
Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC APPROVED BY: Policy and Guidelines Committee TRUST REFERENCE: B9/2009 AWP Ref: AWP61 Date (approved): July 2008 REVIEW
Treatment of septic peritonitis
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance
 Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Intra-Abdominal Infections. Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018
 Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Volume. December Infection. Notes. length of. cases as 90% 1 week. tonsillitis. First Line. sore throat / daily for 5 days. quinsy >4000.
 Volume 8; Number 22 LINCOLNSHIRE GUIDELINES FOR THE TREATMENT OF COMMONLYY OCCURRING INFECTIONS IN PRIMARY CARE: WINTER 2014/15 In this issue of the PACE Bulletin we present an update of our Guidelines
Volume 8; Number 22 LINCOLNSHIRE GUIDELINES FOR THE TREATMENT OF COMMONLYY OCCURRING INFECTIONS IN PRIMARY CARE: WINTER 2014/15 In this issue of the PACE Bulletin we present an update of our Guidelines
Antibiotic Prophylaxis Update
 Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
Approach to pediatric Antibiotics
 Approach to pediatric Antibiotics Gassem Gohal FAAP FRCPC Assistant professor of Pediatrics objectives To be familiar with common pediatric antibiotics o Classification o Action o Adverse effect To discus
Approach to pediatric Antibiotics Gassem Gohal FAAP FRCPC Assistant professor of Pediatrics objectives To be familiar with common pediatric antibiotics o Classification o Action o Adverse effect To discus
Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections. Skin & Soft Tissue Infections (SSTI)
 Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections 2007 Abscess Cellulitis Bradley W Frazee, MD, FACEP Dept of Emergency Medicine Alameda County Medical Center - Highland Hospital Associate
Skin & Soft Tissue Infections (SSTI) Skin & Soft Tissue Infections 2007 Abscess Cellulitis Bradley W Frazee, MD, FACEP Dept of Emergency Medicine Alameda County Medical Center - Highland Hospital Associate
Role of the nurse in diagnosing infection: The right sample, every time
 BROUGHT TO YOU BY Role of the nurse in diagnosing infection: The right sample, every time The module has been written by Shanika Anne-Marie Crusz and Amelia Joseph Authors affiliation: Department of Clinical
BROUGHT TO YOU BY Role of the nurse in diagnosing infection: The right sample, every time The module has been written by Shanika Anne-Marie Crusz and Amelia Joseph Authors affiliation: Department of Clinical
Rational use of antibiotics
 Rational use of antibiotics Uga Dumpis MD, PhD,, DTM Stradins University Hospital Riga, Latvia ugadumpis@stradini.lv BALTICCARE CONFERENCE, PSKOV, 16-18.03, 18.03, 2006 Why to use antibiotics? Prophylaxis
Rational use of antibiotics Uga Dumpis MD, PhD,, DTM Stradins University Hospital Riga, Latvia ugadumpis@stradini.lv BALTICCARE CONFERENCE, PSKOV, 16-18.03, 18.03, 2006 Why to use antibiotics? Prophylaxis
Subacute Adenitis. Ann M. Loeffler, MD
 Subacute Adenitis Ann M. Loeffler, MD Lymphadenitis Swelling and hyperplasia of sinusoidal lining cells Infiltration of leukocytes +/- abscess formation Granulomatous or non-granulomatous Pyogenic adenitis
Subacute Adenitis Ann M. Loeffler, MD Lymphadenitis Swelling and hyperplasia of sinusoidal lining cells Infiltration of leukocytes +/- abscess formation Granulomatous or non-granulomatous Pyogenic adenitis
Can levaquin treat group b strep
 Can levaquin treat group b strep The Borg System is 100 % Can levaquin treat group b strep IBS - Symptoms, Diet and Treatment. IBS, is the common slang term or abbreviation for Irritable Bowel Syndrome
Can levaquin treat group b strep The Borg System is 100 % Can levaquin treat group b strep IBS - Symptoms, Diet and Treatment. IBS, is the common slang term or abbreviation for Irritable Bowel Syndrome
General Surgery Small Group Activity (Facilitator Notes) Curriculum for Antimicrobial Stewardship
 General Surgery Small Group Activity (Facilitator Notes) Curriculum for Antimicrobial Stewardship Facilitator instructions: Read through the facilitator notes and make note of discussion points for each
General Surgery Small Group Activity (Facilitator Notes) Curriculum for Antimicrobial Stewardship Facilitator instructions: Read through the facilitator notes and make note of discussion points for each
The Bug Stops Here: Treating Resistant Staph Infections Holly Roberts, DVM, MS, DACVD Blue Pearl Veterinary Specialists San Antonio, TX
 The Bug Stops Here: Treating Resistant Staph Infections Holly Roberts, DVM, MS, DACVD Blue Pearl Veterinary Specialists San Antonio, TX 1. Staphylococcus bacteria a. Gram positive b. Opportunistic pathogens
The Bug Stops Here: Treating Resistant Staph Infections Holly Roberts, DVM, MS, DACVD Blue Pearl Veterinary Specialists San Antonio, TX 1. Staphylococcus bacteria a. Gram positive b. Opportunistic pathogens
