Surgical site infection (SSI) continues to be the source
|
|
|
- Morgan Barton
- 6 years ago
- Views:
Transcription
1 SURGICAL INFECTIONS Volume 17, Number 5, 2016 ª Mary Ann Liebert, Inc. DOI: /sur Topical Antimicrobials and the Open Surgical Wound Donald E. Fry Abstract Background: Topical antiseptic and antibiotic agents have been used for the prevention of surgical site infections since Joseph Lister s original research on this subject. Although these agents are used extensively in clinical practice, evidence to support the use of topical antimicrobial agents remains limited. Patients and Methods: The world literature on the use of antiseptic and antibiotic agents was evaluated to determine the current status of evidence to support the use of topical antimicrobial agents in the prevention of surgical site infections. Results: Although several techniques of using topical antibiotic solutions, powders, antibiotic gauzes, and beads have some evidence for validation, there are equal numbers of reports that have failed to show benefit. There is little evidence to support the use of antiseptic solutions in the prevention of infections at the surgical site. Conclusions: Additional clinical trials are necessary to provide evidence to support any of the methods for using topical antimicrobial agents to present surgical site infections. Dilute antiseptic agents should be considered in future trials when antimicrobial activity can be identified without local toxicity. Surgical site infection (SSI) continues to be the source of complications after all operative procedures. Numerous preventive strategies are used to prevent SSI, because there are a variety of potential sources of bacterial contamination and there are an abundance of clinical risk factors that will enhance the virulence of micro-organisms that are present at the surgical site [1]. The prevalence of bacteria from patients, the operating team, and the environment means that all surgical sites have organisms that can be cultured at the end of the procedure. It has always seemed logical that the introduction of antimicrobial agents into the wound at the completion of the operation ought to be of benefit in the reduction of infection post-operatively. The French barber surgeon, Ambroise Paré ( ) [2], used topical egg yolk, oil of roses, and turpentine as an alternative to boiling oil for the management of open traumatic wounds. Numerous alternative agents have been used both to create and prevent laudable pus in surgical and traumatic wounds well before the germ theory of disease evolved. With the evidence by Pasteur and others of the role of microbes in infection [3], it was Joseph Lister who introduced topical antiseptics (carbolic acid) as a method to reduce infections in the open surgical incision. As was identified by Lister [4] in one of his last publications, however, the benefits of antiseptics in the open wound were offset in part by the caustic action which I knew must occur. Nevertheless, the early benefits for the reduction of SSI rates with the use of carbolic acid in preparation of the skin and sterilization of instruments led to the expectation that clinical benefit could be derived from the introduction of topical antimicrobial agents into the open incision and that these benefits might override potential local tissue toxicity. Potential Topical Antiseptics The potential topical antiseptic agents that have been proposed for use in the open surgical incision or traumatic wound for the prevention of infection are identified in Table 1. The advantage of the topical application of an antiseptic agent is the achievement of high concentrations of the agent at the site of bacterial contamination. As a group, the antiseptic agents have rapid and bactericidal effects on most potential bacterial pathogens that will contaminate the open incision. Antiseptic agents have multiple mechanisms of action on the bacterial cell, which gives them a broad spectrum of antimicrobial activity and also makes the emergence of resistant strains uncommon. As a group, the antiseptic agents are chemicals, not of biologic origin, and tend to be hypoallergenic. In addition to the use of antiseptic agents for the prevention of infections in open incisions, many of the agents in Table 1 have been used Departments of Surgery, Northwestern University Feinberg School of Medicine, Chicago, Illinois, and the University of New Mexico School of Medicine, Albuquerque, New Mexico. 520
2 TOPICAL ANTIMICROBIAL AGENTS 521 Table 1. Antiseptic Agents Applied to Open Surgical Incisions that Have Been Used to Prevent or Manage Post-Operative Surgical Site Infection Antiseptic choice Acetic acid solution Alcohols Boric acid Chlorhexidine Chlorine compounds Hydrogen peroxide Iodine compounds Silver compounds Triclocarban Triclosan Comments Dilute (0.25%) solutions have been used in incisions without any evidence to support use. Higher concentrations are associated with tissue injury. The solution has been used in bladder irrigation and for otitis externa management. Isopropyl alcohol is most commonly used for topical skin application. Rapidly bactericidal. Desiccates open incisions and is tissue toxic; painful in most concentrations. Not recommended for use in open incisions. Used as eye irrigation for its antimicrobial effects, it is not recommended for use in open incisions. The most common antiseptic in skin preparations, it is generally not recommended at conventional concentrations of 2% 4% in open incisions. Buffered sodium hypochlorite solution; used at 0.25% 0.5% solution; action from oxidative injury of bacterial membranes and enzymes. A common household remedy for cuts and abrasions, it is generally tissue-toxic for application in open incisions for prevention. Tincture of iodine has largely disappeared for any application in operations. Iodophors are less toxic. Iodophors have been used clinically for topical application in open incisions but have not been subject to clinical evaluation for efficacy. Silver nitrate and silver sulfadiazine have been extensively used in burns and selectively in open infected soft tissue incisions. Various slow-release topical preparations are available but are not used commonly in open incisions for prevention. A common antiseptic in commercial soaps; there are no data to evaluate its use in open incisions. Common antiseptic in cosmetics and used in the coating for selected surgical sutures. No data on use in open incisions. extensively in chronic or actively infected soft tissue wounds (e.g., Dakin solution). The randomized clinical evidence to document clinical effectiveness is lacking, however, and continued practice in using these topical agents in the chronic wound is largely based on testimonials and anecdotes. The antiseptic agents collectively are viewed with negative features that have been deterrents for their use in the acute surgical incision for prevention. As was noted by Joseph Lister, the antiseptics have a concentration-dependent tissue toxicity. Antiseptic agents commonly contain detergents that may contribute to local toxicity in the tissue. There is a considerable volume of literature that speaks to the issue of tissue cytotoxicity [5,6] and inhibition of wound healing [7]. Finally, there are limited data that would support the use of topical antiseptic agents in the incision for the prevention of SSI. Randomized trials are rare and usually underpowered. In the era of systemic antibiotic agents, there has been very limited interest in pursuing clinical trials to evaluate specific antiseptic agents that are introduced into the incision for the prevention of infection in surgical incisions or traumatic wounds. The role of antiseptic agents has largely been relegated to the preparation of the skin before the surgical incision or placement of a percutaneous device. Topical Antibiotics With the discovery of sulfa and penicillin, many clinicians viewed the topical application of these agents as potentially of benefit in the prevention of SSI. Topical antibiotics permit concentrations of the drug in the incision that would be much greater than systemic administration. The topical use avoids or markedly limits any systemic exposure of the drug and has the promise of not creating resistance problems that are associated with parenteral use. The problems of topical antibiotic application in the open incision are several. First, there is no convincing evidence that topical antibiotics improve on the benefits that are observed with the appropriate use of systemic preventive antibiotic agents. Second, because high concentrations are used with topical application, there are the usual concerns about potential toxicity and inhibition of wound healing. Finally, the application of topical antibiotic agents has usually been performed by adding the drug to a volume of saline irrigation and then applying the antibiotic solution to the incision. Customarily, this is performed with the dwell time of the antibiotic-laden irrigation only a brief period (15 30 sec) at which point the solution is suctioned from the area. Unlike antiseptics, the contact of the antibiotic with the bacterial target necessitates a time for biologic effect that is far greater than the dwell time that is commonly used. Thus, it is unlikely that the antibiotic irrigation solution has much of an effect on the microbial inoculum in large part because of the methods of delivery that have been used in clinical practice. A scenario that attempted to address this shortcoming of topical antibiotic solutions was that of Lord et al. [8] in which the antibiotic was applied every 10 minutes during the operative procedure. This later scenario was viewed as logistically not practical during a long operation and was not evaluated against appropriate systemic antibiotics in a controlled clinical trial. Alternative Topical Delivery Systems The problems of topical delivery of antibiotics to achieve a sustained concentration of the drug to optimize the opportunity for prevention at the surgical site have led to several alternative methods other than simple incision irrigation. An innovative method for delivery of an antibiotic solution for
3 522 FRY prevention of SSI has been proposed by Alexander et al. [9] in patients undergoing open gastric bypass operations. Closed suction catheters are introduced by separate stab incisions and are placed in a dependent position within the surgical incision space after fascial closure. The skin of the incision is then closed in a watertight fashion. Kanamycin irrigation solution (0.1%, or 1,000 mcg/ml) is then introduced through the suction catheters to create a liquid environment of concentrated antibiotic within the space. The irrigation solution remains for 2 hours and then is suctioned out. This technique has the promise of overcoming the transient antibiotic exposure of the contaminating bacteria that occurs with conventional irrigation and suctioning at the end of the operation but before wound closure. Results of the alternative irrigation tactic in more than 800 patients with an average body mass index >50 have demonstrated reduced SSI rates (<0.25%) in this high-risk population of patients undergoing a bariatric procedure compared with historical control groups. This methodology may well have merit in those patients undergoing laparotomy with substantial depth of subcutaneous adipose tissue but would likely be of limited value in thin patients. Additional studies are necessary to evaluate this method, the length of time that would be best for achievement of optimal outcomes, and which antibiotic would be best suited for topical delivery. Instead of using an antibiotic irrigation solution, some have used undissolved antibiotic powder and directly introduced it into the incision at the time of closure. Andersen et al. [10] introduced ampicillin powder into the incision after surgical removal of non-perforated appendices and reported a dramatic reduction in SSI rates compared with patients treated with incision closure alone. Andersen et al. [11] similarly reported a dramatic reduction in SSI rates after colorectal surgery with the use of ampicillin powder in the incision at closure. Raahave et al. [12], however, reported no benefit in the prevention of SSI in patients undergoing colon resection using the same application of topical ampicillin powder. The use of antibiotic powder continues to be discussed, but convincing evidence for using such a tactic in high-risk surgical incisions (e.g., colon resections) is not available. Antibiotic-impregnated sponges and fleeces that are made of biodegradable collagen have been introduced into the surgical incision at closure in the hope of achieving a sustained release of drug into the incision interface. In a randomized trial of 221 patients who were undergoing elective colorectal surgery, the use of the gentamicin-impregnated sponge reduced SSI rates to 5.6% compared with patients without the sponge (18.4%; p < 0.01) [13]. Greussner et al. [14] found a reduction in perineal SSIs in patients undergoing abdominoperineal resection when an antibiotic-impregnated fleece was place in the incision at primary closure. In another randomized clinical trial by Bennett-Guerrero et al. [15] of 602 patients undergoing colorectal procedures, the gentamicin sponge was identified with an increased SSI rate of 30% compared with no sponge placement of 20.9% (p = 0.01). In a study of nearly 2,000 patients undergoing cardiac operations, the use of the gentamicin sponge was reported by Friberg et al. [16] to dramatically reduce surgical SSIs. Schimmer et al. [17], who studied more than 700 patients who were randomized to receive a gentamicin sponge behind the sternum at closure compared with no sponge, noted a reduction of deep sternal incision infections from 3.5% to 0.6%. A study by Bennett-Guerrero et al. [18] of 1,500 patients undergoing cardiac surgery identified no reduction in SSI rates with the use of the gentamicin-impregnated sponge. Eklund et al. [19] found no reduction of SSI in a study of 542 cardiac surgery patients who were randomized to the gentamicin sponge versus standard closure. Thus, there are conflicting data on the utility of the gentamicin-impregnated collagen sponges/fleeces into the surgical incision to prevent SSIs. There is certainly variability in the methods used for placing the collagen matrix in the incision, and this may account for some differences in results. The foreign body effect could create an adjuvant effect to enhance infection rates. The inflammatory response surrounding the biodegradation of the collagen material combined with a variable inoculum of bacteria can lead to exudative discharge from the closed incision that may or may not be clinical infection. The collagen material may potentially create a sustained dead space in the wound after closure. Creanor et al. [20] found insufficient evidence to support the use of gentamicin sponges for cardiac operations in a metaanalysis of clinical trials. Overall, the current evidence does not support using this method. Antibiotic-impregnated cement has been evaluated in multiple studies of total joint replacement. Parvizi et al. [21] evaluated seven studies by meta-analysis in which antibioticimpregnated cement was used and identified a significant reduction (p < 0.001) in SSI. Gentamicin was the predominant antibiotic agent used. Others have reported no benefit with this method in a study of 3,000 patients in which erythromycin and colistin-impregnated cement was used [22]. Antibiotic-impregnated cement is used in practice, but additional studies are necessary to evaluate the correct formulation of the antibiotic agent employed and the concentration to optimize outcomes. Antibiotic-impregnated beads are used by selected orthopedic surgeons for the prevention of SSI in open fractures. The beads are made with methylmethacrylate and have impregnated aminoglycoside or other antibiotic agents. Combination drugs are often used. The beads are placed into the incision and the antibiotic agent diffuses out of the beads and into the adjacent tissue giving a sustained release over time. The beads are then removed once healing is complete. The beads are used for open fractures, management of osteomyelitis, and for management of dead space in orthopedic procedures. Ostermann et al. [23] reported a reduction in SSI from 12% to 3.7% with the antibiotic beads in open fractures. Moehring et al. [24], however, found no benefit from using antibiotic beads in the prevention of infection in open fractures. Bioabsorbable beads are now being evaluated [25]. In a review of using antibiotic-impregnated beads in open fractures, Hauser et al [26] concluded that there was insufficient evidence to support the routine use of antibiotic-impregnated beads as prophylaxis in open fracture surgery. There are many published and unpublished methods that have been used for the delivery of antibiotic agents into the open surgical incision to prevent infection. The collective data remain inconclusive to use any method. The problem remains that many different antibiotic agents are used, and all have their peculiar method for drug delivery. Studies that
4 TOPICAL ANTIMICROBIAL AGENTS 523 report benefit have high infection rates in the control groups, and many of those reporting no differences in infection rates often are underpowered. Several of these methods may ultimately prove to be of benefit. Huiras et al. [27] and McHugh et al. [28] have concluded that evidence is insufficient to support any topical used of antibiotics to prevent infection. Systemic antibiotics remain the preferred choice for prophylaxis of SSI. Antiseptics Revisited The search for an effective topical antimicrobial tactic has struggled with insufficient evidence to justify any use [29]. The problem of topical antiseptics has been the local tissue and phagocytic cell toxicity of the agents that have been used. An area that has been ignored largely is whether an antiseptic concentration can be identified that has potent antimicrobial activity but does not have clinically significant local tissue or host response injury. Chlorhexidine solution is the topical antiseptic that is generally used for skin preparation of surgical sites and for insertion of intravascular devices. The conventional preparations are 2% or 4% solutions. Dental mouthwashes have only a 0.12% concentration and appear to have antimicrobial effect but without adverse effects on mucous membranes. Edmiston et al. [30] evaluated the in vitro antibacterial effects of 0.05% chlorhexidine solution on multiple bacterial strains. The authors identified a five-log 10 reduction in bacterial colony-forming units when a /ml concentration of Staphylococcus and Escherichia coli was exposed to 0.05% chlorhexidine. These observations pose an interesting question for the topical use of this antiseptic at a concentration that is not recognized as having local tissue toxicity. Yet another feature of chlorhexidine is the binding of the antiseptic agent to soft tissue. Chlorhexidine binds to epidermal, mucous, and subcutaneous tissues after topical application. The bound chlorhexidine has antiseptic effects that continue after the tissue binding, and it is unaffected by the local presence of blood [31]. As a dilute irrigation solution of open wounds and soft tissue infections, it can be anticipated that antiseptic effects will continue after application. To explore these potential advantages in the prevention of SSI, a clinical trial is being conducted to test whether 0.05% chlorhexidine applied by a unique application to the open surgical incision will reduce SSI rates. The study is being performed with the IrriSept Ò system for topical administration [32]. This system contains 450 ml of 0.05% chlorhexidine in water. The delivery system consists of a hand-held compressible bottle that allows delivery of the antiseptic irrigant under pressure to provide both the antiseptic but a pressure-lavage effect on the wound surface. The pressure-lavage effect offers a debriding effect on the wound surface, but at a lower pressure than is observed with conventional pulsed-lavage systems. This lower pressure lavage affords removal of the contaminated fibrin surface of the wound but avoids the pressure-associated tissue injury that has been observed with high-pressure irrigation systems. The low pressure administration permits tissue penetration of the dilute antiseptic that may have merit for both the prevention and management of soft tissue infection. In the current trial, patients presenting with emergency trauma and those undergoing emergency open laparotomy will be enrolled and randomized. These operations are chosen because SSI rates can be anticipated to be 20% when the surgical incision is closed primarily. This trial of open contaminated emergency laparotomy incisions will test the hypothesis of reducing SSI rates with the IrriSept irrigation system versus conventional irrigation and incision management. Patients in both arms of the trial will receive appropriate pre-operative systemic antibiotic agents, and systemic antibiotic therapy will be discontinued within 24 hours of the procedure. The study will have a total of 600 patients randomized to either the IrriSept or conventional (pour/bulb syringe) application. Each patient in the trial will have irrigation of the incision at two standardized times. The initial irrigation will be after the incision is made but before the abdominal fascia is opened. A 60-second dwell time will be required after this initial irrigation. This initial irrigation will test the hypothesis of whether tissue penetration and tissue binding of the Irri- Sept system is superior to conventional irrigation. At the conclusion of the operative procedure, the fascia will be closed by the standard method of the operating surgeon and either the IrriSept or standard irrigation will be conducted a second time. A dwell time of 60 seconds will again be used after the second irrigation. Comprehensive clinical data including pre-operative laboratory data will be obtained to permit risk adjustment of the patient population. There will be study centers. SSI of the incision is the primary evaluation end point at 30 days after the operation. An initial analysis by an independent contractor will be performed after a total of 350 cases have been randomized and evaluated. Conclusion Although the benefits of preventive systemic antibiotics are well accepted, it is generally perceived that better outcomes can possibly be achieved by the addition of topical antimicrobial agents at the surgical site. Studies to validate the added benefit of topical agents have been inconsistent and generally viewed as not being conclusive in their results. The failure of topical antimicrobial agents to augment systemic antibiotic agents may well be shortcomings of the delivery system. Better clinical trials that are adequately powered, that examine different delivery systems, and examine drug dosage and exposure are necessary to find a topical antimicrobial tactic that will improve outcomes. Author Disclosure Statement Dr. Fry declares a consulting relationship with IrriMax Corp. and Prescient Surgical, and is on the Speakers Bureau of Merck and CareFusion. References 1. Fry DE. Fifty ways to cause surgical site infections. Surg Infect 2011;12: Kocher MS. Early limb salvage: open tibia fractures of Ambroise Paré ( ) and Percivall Pott ( ). World J Surg 1997;21: Fry DE. In vino veritas. Surg Infect 2001;2:
5 524 FRY 4. Lister J. Remarks on some points in the history of antiseptic surgery. Br Med J 1908;1: Muller G, Kramer A. Biocompatibility index of antiseptic agents by parallel assessment of antimicrobial activity and cellular toxicity. J Antimicrob Chemother 2008;61: Lineaweaver W, Howard R, Soucy D, et al. Topical antimicrobial toxicity. Arch Surg 1985;120: Thomas GW, Rael LT, Bar-Or R, et al. Mechanisms of delayed wound healing by commonly used antiseptics. J Trauma 2009;66: Lord JW, Rossi G, Daliana M. Intraoperative antibiotic wound lavage: An attempt to eliminate postoperative infection in arterial and clean general surgical procedures. Ann Surg 1977;185: Alexander JW, Rahn R, Goodman HR. Prevention of surgical site infections by an infusion of topical antibiotic in morbidly obese patients. Surg Infect 2009;10: Andersen B, Bendtsen A, Holbraad L, Schantz A. Wound infections after appendicectomy. I. A controlled trial on the prophylactic efficacy of topical ampicillin in non-perforated appendicitis. II. A controlled trial on the prophylactic efficacy of delayed primary suture and topical ampicillin in perforated appendicitis. Acta Chir Scand 1972;138: Andersen B, Korner B, Ostergaard AH. Topical ampicillin against wound infection after colorectal surgery. Ann Surg 1972;176: Raahave D, Hesselfeldt P, Pedersen T, et al. No effect of topical ampicillin prophylaxis in elective operations of the colon or rectum. Surg Gynecol Obstet 1989;168: Rutten HJ, Nijhuis PH. Prevention of wound infection in elective colorectal surgery by local application of a gentamicin-containing collagen sponge. Eur J Surg Suppl 1997;578: Gruessner U, Clemens M, Pahlplatz PV, et al. Improvement of perineal wound healing by local administration of gentamicinimpregnated collagen fleeces after abdominoperineal excision of rectal cancer. Am J Surg 2001;182: Bennett-Guerrero E, Pappas TN, Koltun WA, et al. Gentamicincollagen sponge for infection prophylaxis in colorectal surgery. N Engl J Med 2010;363: Friberg O, Svedjeholm R, Söderquist B, et al. Local gentamicin reduces sternal wound infections after cardiac surgery: A randomized controlled trial. Ann Thorac Surg 2005;79: Schimmer C, Özkur M, Sinha B, et al. Gentamicin-collagen sponge reduces sternal wound complications after heart surgery: A controlled, prospectively randomized, doubleblind study. J Thorac Cardiovasc Surg 2012;143: Bennett-Guerrero E, Ferguson TB Jr, Lin M, et al. Effect of an implantable gentamicin-collagen sponge on sternal wound infections following cardiac surgery: A randomized trial. JAMA 2010;304: Eklund AM, Valtonen M, Werkkala KA. Prophylaxis of sternal wound infections with gentamicin-collagen implant: Randomized controlled study in cardiac surgery. J Hosp Infect 2005;59: Creanor S, Barton A, Marchbank A. Effectiveness of a gentamicin impregnated collagen sponge on reducing sternal wound infections following cardiac surgery: A metaanalysis of randomised controlled trials. Ann R Coll Surg Engl 2012;94: Parvizi J, Saleh KJ, Ragland PS, et al. Efficacy of antibioticimpregnated cement in total hip replacement. Acta Orthop 2008;79: Hinarejos P, Guirro P, Leal J, et al. The use of erythromycin and colistin-loaded cement in total knee arthroplasty does not reduce the incidence of infection: A prospective randomized study in 3000 knees. J Bone Joint Surg Am 2013;95: Ostermann PA, Seligson D, Henry SL. Local antibiotic therapy for severe open fractures. A review of 1085 consecutive cases. J Bone Joint Surg Br 1995;77: Moehring HD, Gravel C, Chapman MW, Olson SA. Comparison of antibiotic beads and intravenous antibiotics in open fractures. Clin Orthop Relat Res 2000;372: Ueng SW, Lin SS, Wang IC, et al. Efficacy of vancomycinreleasing biodegradable poly(lactide-co-glycolide) antibiotics beads for treatment of experimental bone infection due to Staphylococcus aureus. J Orthop Surg Res 2016; 11: Hauser CJ, Adams CA, Eachempati SR. Surgical Infection Society guideline: Prophylactic antibiotic use in open fractures: An evidence-based guideline. Surg Infect 2006;7: Huiras P, Logan JK, Papadopoulos S, Whitney D. Local antimicrobial administration for prophylaxis of surgical site infections. Pharmacotherapy 2012;32: McHugh SM, Collins CJ, Corrigan MA, et al. The role of topical antibiotics used as prophylaxis in surgical site infection prevention. J Antimicrob Chemother 2011; Barnes S, Spencer M, Graham D, Johnson HB. Surgical wound irrigation: A call for evidence-based standardization of practice. Am J Infect Control 2014;42: Edmiston CE Jr, Bruden B, Rucinski MC, et al. Reducing the risk of surgical site infections: Does chlorhexidine gluconate provide a risk reduction benefit? Am J Infect Control 2013;41:S49 S Edmiston DE Jr, Seabrook GR, Johnson CP, et al. Comparison of a new and innovative 2% chlorhexidine gluconateimpregnated cloth with 4% chlorhexidine gluconate as a topical antiseptic for preparation of skin prior to surgery. Am J Infect Control 2007;35: IrriseptÒ. Last accessed May 27, Address correspondence to: Dr. Donald E. Fry MPA Healthcare Solutions 1 East Wacker Drive, Suite 1210 Chicago, IL dfry@consultmpa.com
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bennett-Guerrero E, Pappas TN, Koltun WA, et al. Gentamicin
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bennett-Guerrero E, Pappas TN, Koltun WA, et al. Gentamicin
Patient Preparation. Surgical Team
 January 2019 www.nursingcenter.com Surgical Site Infection Prevention Surgical site infections (SSIs) are one of the most common and costly healthcare-associated infections in the United States (Smith
January 2019 www.nursingcenter.com Surgical Site Infection Prevention Surgical site infections (SSIs) are one of the most common and costly healthcare-associated infections in the United States (Smith
Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma
 Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma Lucio Petrizzi DVM DECVS Università degli Studi di Teramo Surgical site infections (SSI) Microbial contamination unavoidable Infection
Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma Lucio Petrizzi DVM DECVS Università degli Studi di Teramo Surgical site infections (SSI) Microbial contamination unavoidable Infection
Surgical prophylaxis for Gram +ve & Gram ve infection
 Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Redefining Infection Management. Proven Clinical Outcomes
 Proven Clinical Outcomes Proof of Bacteria-Binding1 In the first 30 seconds, 1 square centimeter of Cutimed Sorbact binds wound bacteria - after 2 hours, the amount of bacteria bound are more than would
Proven Clinical Outcomes Proof of Bacteria-Binding1 In the first 30 seconds, 1 square centimeter of Cutimed Sorbact binds wound bacteria - after 2 hours, the amount of bacteria bound are more than would
Reducing Infections in Surgical Practice. Fred A Sweet, MD Rockford Spine Center Illinois, USA
 Reducing Infections in Surgical Practice Fred A Sweet, MD Rockford Spine Center Illinois, USA Introduction: How bacteria get in The Host The Surgeon The Procedure The STAFF Skin PREP Prophylactic Antibiotics
Reducing Infections in Surgical Practice Fred A Sweet, MD Rockford Spine Center Illinois, USA Introduction: How bacteria get in The Host The Surgeon The Procedure The STAFF Skin PREP Prophylactic Antibiotics
Antimicrobial Prophylaxis in Digestive Surgery
 Antimicrobial Prophylaxis in Digestive Surgery Toar JM. Lalisang, MD, PhD Digestive Surgery Division Cipto Mangunkusumo Hospital Medical Faculty Universitas Indonesia Antibiotic must be present before
Antimicrobial Prophylaxis in Digestive Surgery Toar JM. Lalisang, MD, PhD Digestive Surgery Division Cipto Mangunkusumo Hospital Medical Faculty Universitas Indonesia Antibiotic must be present before
CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II page 1
 CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II 1. What are the symptoms of an infected wound? a. Fever b. Edema c. Erythema d. Local pain and tenderness e. Induration of wound edge 2. A person with
CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II 1. What are the symptoms of an infected wound? a. Fever b. Edema c. Erythema d. Local pain and tenderness e. Induration of wound edge 2. A person with
 1) Mangram AJ,Horan TC,Pearson ML, et al:guideline for Prevention of Surgical Site Infection.Infect Control Hosp Epidemiol 1999;20:247-278. 1a) Perl TM, Cullen JJ, Wenzel RP, et al.: Intranasal mupirocin
1) Mangram AJ,Horan TC,Pearson ML, et al:guideline for Prevention of Surgical Site Infection.Infect Control Hosp Epidemiol 1999;20:247-278. 1a) Perl TM, Cullen JJ, Wenzel RP, et al.: Intranasal mupirocin
Introduction to Chemotherapeutic Agents. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The university of Jordan November 2018
 Introduction to Chemotherapeutic Agents Munir Gharaibeh MD, PhD, MHPE School of Medicine, The university of Jordan November 2018 Antimicrobial Agents Substances that kill bacteria without harming the host.
Introduction to Chemotherapeutic Agents Munir Gharaibeh MD, PhD, MHPE School of Medicine, The university of Jordan November 2018 Antimicrobial Agents Substances that kill bacteria without harming the host.
Antimicrobial Prophylaxis in the Surgical Patient. M. J. Osgood
 Antimicrobial Prophylaxis in the Surgical Patient M. J. Osgood Outline Definitions surgical site infection (SSI) Risk factors Wound classification Microbiology of SSIs Strategies for prevention of SSIs
Antimicrobial Prophylaxis in the Surgical Patient M. J. Osgood Outline Definitions surgical site infection (SSI) Risk factors Wound classification Microbiology of SSIs Strategies for prevention of SSIs
SSI PREVENTION - CORRECT AND SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS
 SSI PREVENTION - CORRECT AN SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS Things you should know! There is wide consensus on specific procedures that warrant antibiotic prophylaxis as well as in which procedures
SSI PREVENTION - CORRECT AN SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS Things you should know! There is wide consensus on specific procedures that warrant antibiotic prophylaxis as well as in which procedures
No-leaching. No-resistance. No-toxicity. >99.999% Introducing BIOGUARD. Best-in-class dressings for your infection control program
 Introducing BIOGUARD No-leaching. >99.999% No-resistance. No-toxicity. Just cost-efficient, broad-spectrum, rapid effectiveness you can rely on. Best-in-class dressings for your infection control program
Introducing BIOGUARD No-leaching. >99.999% No-resistance. No-toxicity. Just cost-efficient, broad-spectrum, rapid effectiveness you can rely on. Best-in-class dressings for your infection control program
Prevention of Surgical Site Infections
 Prevention of Surgical Site Infections A Review of Recent Evidence and Guidelines Dale W. Bratzler, DO, MPH, MACOI, FIDSA Professor and Associate Dean, College of Public Health Professor, College of Medicine
Prevention of Surgical Site Infections A Review of Recent Evidence and Guidelines Dale W. Bratzler, DO, MPH, MACOI, FIDSA Professor and Associate Dean, College of Public Health Professor, College of Medicine
GUIDELINE FOR ANTIMICROBIAL USE IN THE ORTHOPAEDIC AND TRAUMA DEPARTMENT
 GUIDELINE FOR ANTIMICROBIAL USE IN THE ORTHOPAEDIC AND TRAUMA DEPARTMENT Written by: Dr Ken. N. Agwuh, Consultant Microbiologist Mr Roger Helm, Consultant Orthopaedic Surgeon Mr T Kumar, Consultant Orthopaedic
GUIDELINE FOR ANTIMICROBIAL USE IN THE ORTHOPAEDIC AND TRAUMA DEPARTMENT Written by: Dr Ken. N. Agwuh, Consultant Microbiologist Mr Roger Helm, Consultant Orthopaedic Surgeon Mr T Kumar, Consultant Orthopaedic
Preventing Surgical Site Infections. Edward L. Goodman, MD September 16, 2013
 Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Prophylactic antibiotic timing and dosage. Dr. Sanjeev Singh AIMS, Kochi
 Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection
 THE IRAQI POSTGRADUATE MEDICAL JOURNAL PROPHYLACTIC ANTIBIOTICS ON SURGICAL WOUND INFECTION The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection Ahmed Hamid Jasim*, Nabeel
THE IRAQI POSTGRADUATE MEDICAL JOURNAL PROPHYLACTIC ANTIBIOTICS ON SURGICAL WOUND INFECTION The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection Ahmed Hamid Jasim*, Nabeel
Antibiotic Prophylaxis Update
 Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
Antibacterial Agents & Conditions. Stijn van der Veen
 Antibacterial Agents & Conditions Stijn van der Veen Antibacterial agents & conditions Antibacterial agents Disinfectants: Non-selective antimicrobial substances that kill a wide range of bacteria. Only
Antibacterial Agents & Conditions Stijn van der Veen Antibacterial agents & conditions Antibacterial agents Disinfectants: Non-selective antimicrobial substances that kill a wide range of bacteria. Only
The role of Infection Control Nurse in Prevention of Surgical Site Infection (SSI) April 2013
 The role of Infection Control Nurse in Prevention of Surgical Site Infection (SSI) April 2013 Impact of SSI 2 nd common health- care associated infection (HCAI) 14-16% of HCAI Post operation SSI prolong
The role of Infection Control Nurse in Prevention of Surgical Site Infection (SSI) April 2013 Impact of SSI 2 nd common health- care associated infection (HCAI) 14-16% of HCAI Post operation SSI prolong
Drug resistance in relation to use of silver sulphadiazine cream in a burns unit
 J. clin. Path., 1977, 30, 160-164 Drug resistance in relation to use of silver sulphadiazine cream in a burns unit KIM BRIDGES AND E. J. L. LOWBURY From the MRC Industrial Injuries and Burns Unit, Birmingham
J. clin. Path., 1977, 30, 160-164 Drug resistance in relation to use of silver sulphadiazine cream in a burns unit KIM BRIDGES AND E. J. L. LOWBURY From the MRC Industrial Injuries and Burns Unit, Birmingham
Emergency Management of Life Threatening Problems
 The management of wounds constitutes a significant topic of Emergency Medicine and I will briefly discuss with you first the emergency management of life threatening problems followed by wound assessment
The management of wounds constitutes a significant topic of Emergency Medicine and I will briefly discuss with you first the emergency management of life threatening problems followed by wound assessment
Other Beta - lactam Antibiotics
 Other Beta - lactam Antibiotics Assistant Professor Dr. Naza M. Ali Lec 5 8 Nov 2017 Lecture outlines Other beta lactam antibiotics Other inhibitors of cell wall synthesis Other beta-lactam Antibiotics
Other Beta - lactam Antibiotics Assistant Professor Dr. Naza M. Ali Lec 5 8 Nov 2017 Lecture outlines Other beta lactam antibiotics Other inhibitors of cell wall synthesis Other beta-lactam Antibiotics
Dual Antibiotic Delivery from Chitosan Sponges Prevents In Vivo Polymicrobial Biofilm Infections
 Dual Antibiotic Delivery from Chitosan Sponges Prevents In Vivo Polymicrobial Biofilm Infections Ashley Parker, MS 1, James Smith, MS 1, Karen Beenken, PhD 2, Jessica Amber Jennings, PhD 3, Mark Smeltzer,
Dual Antibiotic Delivery from Chitosan Sponges Prevents In Vivo Polymicrobial Biofilm Infections Ashley Parker, MS 1, James Smith, MS 1, Karen Beenken, PhD 2, Jessica Amber Jennings, PhD 3, Mark Smeltzer,
The Choice. V e r s a t i l i t y. S t r e n g t h. F l e x i b i l i t y. of surgeons for half a century
 The Choice of surgeons for half a century V e r s a t i l i t y S t r e n g t h F l e x i b i l i t y S t o p b l e e d i n g f a s t w i t h t h r e e p r o v e n p e r f o r m e r s SURGICEL Absorbable
The Choice of surgeons for half a century V e r s a t i l i t y S t r e n g t h F l e x i b i l i t y S t o p b l e e d i n g f a s t w i t h t h r e e p r o v e n p e r f o r m e r s SURGICEL Absorbable
Prevention of Perioperative Surgical Infections
 Prevention of Perioperative Surgical Infections Michael A. West, MD, PhD, FACS Department of Surgery University California San Francisco San Francisco, CA, USA Surgical Site Infections (SSI) 2-5% of operated
Prevention of Perioperative Surgical Infections Michael A. West, MD, PhD, FACS Department of Surgery University California San Francisco San Francisco, CA, USA Surgical Site Infections (SSI) 2-5% of operated
NHS Dumfries And Galloway. Surgical Prophylaxis Guidelines
 NHS Dumfries And Galloway Surgical Prophylaxis Guidelines The aim of surgical prophylaxis is to reduce rates of surgical site and health-care associated infections and so reduce surgical morbidity and
NHS Dumfries And Galloway Surgical Prophylaxis Guidelines The aim of surgical prophylaxis is to reduce rates of surgical site and health-care associated infections and so reduce surgical morbidity and
Treatment of Surgical Site Infection Meeting Quality Statement 6. Prof Peter Wilson University College London Hospitals
 Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
The CARI Guidelines Caring for Australians with Renal Impairment. 8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter
 8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: February 2003 Final submission: May 2004 Guidelines (Include recommendations based on level I or II evidence) Antibiotic
8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: February 2003 Final submission: May 2004 Guidelines (Include recommendations based on level I or II evidence) Antibiotic
Overview of Infection Control and Prevention
 Overview of Infection Control and Prevention Review of the Cesarean-section Antibiotic Prophylaxis Program in Jordan and Workshop on Rational Medicine Use and Infection Control Terry Green and Salah Gammouh
Overview of Infection Control and Prevention Review of the Cesarean-section Antibiotic Prophylaxis Program in Jordan and Workshop on Rational Medicine Use and Infection Control Terry Green and Salah Gammouh
Use And Misuse Of Antibiotics In Neurosurgery
 Use And Misuse Of Antibiotics In Neurosurgery CSF infection in the United States after neurosurgery from 1992 to 2003 0.86% to 2.32% * *National Nosocomial Infections Surveillance System: National Nosocomial
Use And Misuse Of Antibiotics In Neurosurgery CSF infection in the United States after neurosurgery from 1992 to 2003 0.86% to 2.32% * *National Nosocomial Infections Surveillance System: National Nosocomial
Prevention of surgical site infections (SSI) nosocomial infection * - Lead to prolonged hospital stay and increased coasts
 Antibiotic Prophylaxis in Surgery Birgit Ross, MD Dep. of Hospital Hygiene University Hospital and Clinics, Essen Prevention of surgical site infections (SSI) - Surgical site infections account for approximately
Antibiotic Prophylaxis in Surgery Birgit Ross, MD Dep. of Hospital Hygiene University Hospital and Clinics, Essen Prevention of surgical site infections (SSI) - Surgical site infections account for approximately
Systemic Antimicrobial Prophylaxis Issues
 Systemic Antimicrobial Prophylaxis Issues Pierre Moine Department of Anesthesiology University of Colorado Denver 3 rd International Conference on Surgery and Anesthesia OMICs Group Conference The Surgical
Systemic Antimicrobial Prophylaxis Issues Pierre Moine Department of Anesthesiology University of Colorado Denver 3 rd International Conference on Surgery and Anesthesia OMICs Group Conference The Surgical
International Journal for Pharmaceutical Research Scholars (IJPRS)
 International Journal for Pharmaceutical Research Scholars (IJPRS) V-3, I-2, 2014 ISSN No: 2277-7873 CASE STUDY Acute Kidney Injury Following Antibiotic Spacer Placement for Two-Stage Arthroplasty Gregory
International Journal for Pharmaceutical Research Scholars (IJPRS) V-3, I-2, 2014 ISSN No: 2277-7873 CASE STUDY Acute Kidney Injury Following Antibiotic Spacer Placement for Two-Stage Arthroplasty Gregory
Antibiotic Prophylaxis in Adult Orthopaedic Surgery. Formulary/prescribing guideline
 Document type: Antibiotic Prophylaxis in Adult Orthopaedic Surgery Version: 2.0 Author (name): Author (designation): Validated by Formulary/prescribing guideline Dr Celia Chu, Dr Katy Edwards, Dr Pradeep
Document type: Antibiotic Prophylaxis in Adult Orthopaedic Surgery Version: 2.0 Author (name): Author (designation): Validated by Formulary/prescribing guideline Dr Celia Chu, Dr Katy Edwards, Dr Pradeep
Surgical Site Infections (SSIs)
 Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
In 2002, surgical site infections (SSI) were noted by. Antimicrobial Formulation and Delivery in the Prevention of Surgical Site Infection
 SURGICAL INFECTIONS Volume 17, Number 3, 2016 ª Mary Ann Liebert, Inc. DOI: 10.1089/sur.2015.272 Antimicrobial Formulation and Delivery in the Prevention of Surgical Site Infection Patrick B. O Neal 1,2
SURGICAL INFECTIONS Volume 17, Number 3, 2016 ª Mary Ann Liebert, Inc. DOI: 10.1089/sur.2015.272 Antimicrobial Formulation and Delivery in the Prevention of Surgical Site Infection Patrick B. O Neal 1,2
TITLE: Antibacterial Sutures for Wound Closure after Surgery: A Review of the Clinical Effectiveness and Long-Term Adverse Effects
 TITLE: Antibacterial Sutures for Wound Closure after Surgery: A Review of the Clinical Effectiveness and Long-Term Adverse Effects DATE: 17 September 2008 CONTEXT AND POLICY ISSUES: Surgical site infections
TITLE: Antibacterial Sutures for Wound Closure after Surgery: A Review of the Clinical Effectiveness and Long-Term Adverse Effects DATE: 17 September 2008 CONTEXT AND POLICY ISSUES: Surgical site infections
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Voluntary Only
 Last Updated: Version 4.4a NQF-ENORSE VOLUNTARY CONSENSUS STANARS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Voluntary Only Measure Set: Surgical Care Improvement Project (SCIP) Set
Last Updated: Version 4.4a NQF-ENORSE VOLUNTARY CONSENSUS STANARS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Voluntary Only Measure Set: Surgical Care Improvement Project (SCIP) Set
TEAT DIP- POST DIP- PRE DIP- STRIPING
 TEAT DIP- POST DIP- PRE DIP- STRIPING KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE-560008, INDIA Email: sales@srisaiagro.com Www.srisaiagro.com
TEAT DIP- POST DIP- PRE DIP- STRIPING KRISHIMATE AGRO AND DAIRY PVT LTD NO.1176, 1ST CROSS, 12TH B MAIN, H A L 2ND STAGE, INDIRANAGAR BANGALORE-560008, INDIA Email: sales@srisaiagro.com Www.srisaiagro.com
In an effort to help reduce surgical site infections, Surgical Services associates will be expected to observe the following guidelines:
 To: Dept. of Surgery Associates From: Gloria Karr, Dir. Infection Prevention Date: May, 2012 Re: Guidelines for Infection Control in In an effort to help reduce surgical site infections, Surgical Services
To: Dept. of Surgery Associates From: Gloria Karr, Dir. Infection Prevention Date: May, 2012 Re: Guidelines for Infection Control in In an effort to help reduce surgical site infections, Surgical Services
During the second half of the 19th century many operations were developed after anesthesia
 Continuing Education Column Surgical Site Infection and Surveillance Tae Jin Lim, MD Department of Surgery, Keimyung University College of Medicine E mail : tjlim@dsmc.or.kr J Korean Med Assoc 2007; 50(10):
Continuing Education Column Surgical Site Infection and Surveillance Tae Jin Lim, MD Department of Surgery, Keimyung University College of Medicine E mail : tjlim@dsmc.or.kr J Korean Med Assoc 2007; 50(10):
Gynaecological Surgery in Adults Surgical Antibiotic Prophylaxis
 Gynaecological Surgery in Adults Surgical Antibiotic Prophylaxis Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date
Gynaecological Surgery in Adults Surgical Antibiotic Prophylaxis Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date
IACUC POLICY Rodent Survival Surgery
 BACKGROUND The University of Rhode Island s Institutional Animal Care and Use Committee (IACUC) is charged with ensuring that all surgical facilities and procedures meet the criteria set by the federal
BACKGROUND The University of Rhode Island s Institutional Animal Care and Use Committee (IACUC) is charged with ensuring that all surgical facilities and procedures meet the criteria set by the federal
This is the use of antibiotics before, during and after a diagnostic, therapeutic or surgical procedure to prevent infectious complications.
 Antibiotic prophylaxis in surgery CSu2 Policy Antimicrobial prophylaxis is used to reduce the incidence of post operative wound infection; patients undergoing procedures associated with high infection
Antibiotic prophylaxis in surgery CSu2 Policy Antimicrobial prophylaxis is used to reduce the incidence of post operative wound infection; patients undergoing procedures associated with high infection
General Rules Topicals for Skin Infections Topicals for Allergic Skin Disease Topicals for Seborrhea
 Douglas J. DeBoer, D.V.M., Diplomate A.C.V.D. School of Veterinary Medicine University of Wisconsin-Madison General Rules Topicals for Skin Infections Topicals for Allergic Skin Disease Topicals for Seborrhea
Douglas J. DeBoer, D.V.M., Diplomate A.C.V.D. School of Veterinary Medicine University of Wisconsin-Madison General Rules Topicals for Skin Infections Topicals for Allergic Skin Disease Topicals for Seborrhea
The role of topical antibiotics used as prophylaxis in surgical site infection prevention
 J Antimicrob Chemother 2011; 66: 693 701 doi:10.1093/jac/dkr009 Advance Access publication 3 February 2011 The role of topical antibiotics used as prophylaxis in surgical site infection prevention S. M.
J Antimicrob Chemother 2011; 66: 693 701 doi:10.1093/jac/dkr009 Advance Access publication 3 February 2011 The role of topical antibiotics used as prophylaxis in surgical site infection prevention S. M.
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients.
 Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Conflict of interest: We have no conflict of interest to report on this topic of SSI reduction for total knees.
 Reducing SSI- Knees TIFFANY KENNERK MBA, MSN, RN, NE -BC, ONC CYNTHIA SEAMAN BSN, RN, ONC, CMSRN ~COMMUNITY HOSPITALS AND WELLNESS CENTERS~ Conflict of interest: We have no conflict of interest to report
Reducing SSI- Knees TIFFANY KENNERK MBA, MSN, RN, NE -BC, ONC CYNTHIA SEAMAN BSN, RN, ONC, CMSRN ~COMMUNITY HOSPITALS AND WELLNESS CENTERS~ Conflict of interest: We have no conflict of interest to report
SHC Surgical Antimicrobial Prophylaxis Guidelines
 SHC Surgical Antimicrobial Prophylaxis Guidelines I. Purpose/Background This document is based upon the 2013 consensus guidelines from American Society of Health-System Pharmacists (ASHP), the Infectious
SHC Surgical Antimicrobial Prophylaxis Guidelines I. Purpose/Background This document is based upon the 2013 consensus guidelines from American Society of Health-System Pharmacists (ASHP), the Infectious
Treatment of septic peritonitis
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Scottish Medicines Consortium
 Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Antimicrobial prophylaxis. Bs Lưu Hồ Thanh Lâm Bv Nhi Đồng 2
 Antimicrobial prophylaxis Bs Lưu Hồ Thanh Lâm Bv Nhi Đồng 2 Definition The United States Centers for Disease Control and Prevention (CDC) has developed criteria that define surgical site infection (SSI)
Antimicrobial prophylaxis Bs Lưu Hồ Thanh Lâm Bv Nhi Đồng 2 Definition The United States Centers for Disease Control and Prevention (CDC) has developed criteria that define surgical site infection (SSI)
Burton's Microbiology for the Health Sciences. Chapter 9. Controlling Microbial Growth in Vivo Using Antimicrobial Agents
 Burton's Microbiology for the Health Sciences Chapter 9. Controlling Microbial Growth in Vivo Using Antimicrobial Agents Chapter 9 Outline Introduction Characteristics of an Ideal Antimicrobial Agent How
Burton's Microbiology for the Health Sciences Chapter 9. Controlling Microbial Growth in Vivo Using Antimicrobial Agents Chapter 9 Outline Introduction Characteristics of an Ideal Antimicrobial Agent How
STERILIZATION, DESINFECTION PREVENTION OF SURGICAL SITE INFECTION (SSI)
 Semmelweis University Faculty of Medicine Department of Surgical Research and Techniques OPERATING ROOM (OR) - STRUCTURE, EQUIPMENTS STERILIZATION, DESINFECTION PREVENTION OF SURGICAL SITE INFECTION (SSI)
Semmelweis University Faculty of Medicine Department of Surgical Research and Techniques OPERATING ROOM (OR) - STRUCTURE, EQUIPMENTS STERILIZATION, DESINFECTION PREVENTION OF SURGICAL SITE INFECTION (SSI)
SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS
 SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if
SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if
Intra-Abdominal Infections. Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018
 Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS
 RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS I. Purpose/Scope These guidelines apply to all surgical procedures performed on animals at Mississippi State University in which the animals
RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS I. Purpose/Scope These guidelines apply to all surgical procedures performed on animals at Mississippi State University in which the animals
Cefuroxime 1.5gm IV and Metronidazole 500mg IV. Metronidazole 500mg IV/Ampicillin-sulbactam e 3g/Ceftriaxone 2gm. +Metronidazole 500mg/Ertapenem 1gm
 SURGICAL ANTIBIOTIC PROPHYLAXIS GENERAL SURGERY* PROCEDURE RECOMMENDED AGENTS a,b Clean None None ALTERNATIVE AGENTS (If allergic to penicillin or colonized/infected with MRSA at any site) Clean with potential
SURGICAL ANTIBIOTIC PROPHYLAXIS GENERAL SURGERY* PROCEDURE RECOMMENDED AGENTS a,b Clean None None ALTERNATIVE AGENTS (If allergic to penicillin or colonized/infected with MRSA at any site) Clean with potential
MANAGEMENT OF TOTAL JOINT ARTHROPLASTY INFECTIONS
 MANAGEMENT OF TOTAL JOINT ARTHROPLASTY INFECTIONS Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine TOTAL JOINT ARTHROPLASTIES In 2009: 1 million THA and TKA By 2030,
MANAGEMENT OF TOTAL JOINT ARTHROPLASTY INFECTIONS Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine TOTAL JOINT ARTHROPLASTIES In 2009: 1 million THA and TKA By 2030,
Measure Information Form
 Release Notes: Measure Information Form Version 2.4 **NQF-NORS VOLUNTARY CONSNSUS STANARS FOR HOSPITAL CAR** Measure Information Form Measure Set: Surgical Care Improvement Project (SCIP) Set Measure I
Release Notes: Measure Information Form Version 2.4 **NQF-NORS VOLUNTARY CONSNSUS STANARS FOR HOSPITAL CAR** Measure Information Form Measure Set: Surgical Care Improvement Project (SCIP) Set Measure I
3M Health Care Academy Managing the Risk of SSI: Sterile Surface
 SM 3M Health Care Academy Managing the Risk of SSI: Sterile Surface February 28, 2017 Kimberly Prinsen Karen Neis House Keeping From the GoToWebinar page: Click on the orange box with a white arrow to
SM 3M Health Care Academy Managing the Risk of SSI: Sterile Surface February 28, 2017 Kimberly Prinsen Karen Neis House Keeping From the GoToWebinar page: Click on the orange box with a white arrow to
Beyond SCIP: Leading the Way to SSI Reduction. House Keeping. House Keeping. Questions. Dianne Rawson, RN, MA Hugo, MN May 14, 2013
 3M Learning Connection 5/7/2013 3M Infection Prevention Solutions Learning Connection Beyond SCIP: Leading the Way to SSI Reduction Dianne Rawson, RN, MA Hugo, MN May 14, 2013 2012. All Rights Reserved.
3M Learning Connection 5/7/2013 3M Infection Prevention Solutions Learning Connection Beyond SCIP: Leading the Way to SSI Reduction Dianne Rawson, RN, MA Hugo, MN May 14, 2013 2012. All Rights Reserved.
How to Use Delayed Closure for Limb Wound Management
 How to Use Delayed Closure for Limb Wound Management Richard P. Hackett, DVM, MS, Diplomate ACVS Author s address: Department of Clinical Sciences, College of Veterinary Medicine, Cornell University, Ithaca,
How to Use Delayed Closure for Limb Wound Management Richard P. Hackett, DVM, MS, Diplomate ACVS Author s address: Department of Clinical Sciences, College of Veterinary Medicine, Cornell University, Ithaca,
Wound Management. Elof Eriksson MD PhD Professor Emeritus, Harvard Medical School Chief Medical Officer, Applied Tissue Technologies LLC
 Wound Management The use of a Platform Wound Device for Topical Treatment of Infections and for Delivery of Negative Pressure Elof Eriksson MD PhD Professor Emeritus, Harvard Medical School Chief Medical
Wound Management The use of a Platform Wound Device for Topical Treatment of Infections and for Delivery of Negative Pressure Elof Eriksson MD PhD Professor Emeritus, Harvard Medical School Chief Medical
The Infected Implant in Orthopaedic Reconstruction: An Update on the Clinical and Molecular Approaches to Prevention and Diagnosis
 The Infected Implant in Orthopaedic Reconstruction: An Update on the Clinical and Molecular Approaches to Prevention and Diagnosis (Organized by the Musculoskeletal Tumor Society (MSTS) and ORS) Organizers:
The Infected Implant in Orthopaedic Reconstruction: An Update on the Clinical and Molecular Approaches to Prevention and Diagnosis (Organized by the Musculoskeletal Tumor Society (MSTS) and ORS) Organizers:
مادة االدوية المرحلة الثالثة م. غدير حاتم محمد
 م. مادة االدوية المرحلة الثالثة م. غدير حاتم محمد 2017-2016 ANTIMICROBIAL DRUGS Antimicrobial drugs Lecture 1 Antimicrobial Drugs Chemotherapy: The use of drugs to treat a disease. Antimicrobial drugs:
م. مادة االدوية المرحلة الثالثة م. غدير حاتم محمد 2017-2016 ANTIMICROBIAL DRUGS Antimicrobial drugs Lecture 1 Antimicrobial Drugs Chemotherapy: The use of drugs to treat a disease. Antimicrobial drugs:
Post-operative surgical wound infection
 Med. J. Malaysia Vol. 45 No. 4 December 1990 Post-operative surgical wound infection Yasmin Abu Hanifah, MBBS, MSc. (London) Lecturer Department of Medical Microbiology, Faculty of Medicine, University
Med. J. Malaysia Vol. 45 No. 4 December 1990 Post-operative surgical wound infection Yasmin Abu Hanifah, MBBS, MSc. (London) Lecturer Department of Medical Microbiology, Faculty of Medicine, University
Scottish Surveillance of Healthcare Infection Programme (SSHAIP) Health Protection Scotland SSI Surveillance Protocol 7th Edition 2017 Question &
 Contents General... 4 Pre-op... 4 Peri-op... 5 Post-op... 8 Caesarean Section... 12 Orthopaedics... 14 Large Bowel:... 15 Vascular... 17 General Pre-op Q: If a patient is an emergency admission is the
Contents General... 4 Pre-op... 4 Peri-op... 5 Post-op... 8 Caesarean Section... 12 Orthopaedics... 14 Large Bowel:... 15 Vascular... 17 General Pre-op Q: If a patient is an emergency admission is the
American Association of Feline Practitioners American Animal Hospital Association
 American Association of Feline Practitioners American Animal Hospital Association Basic Guidelines of Judicious Therapeutic Use of Antimicrobials August 1, 2006 Introduction The Basic Guidelines to Judicious
American Association of Feline Practitioners American Animal Hospital Association Basic Guidelines of Judicious Therapeutic Use of Antimicrobials August 1, 2006 Introduction The Basic Guidelines to Judicious
An Evidence Based Approach to Antibiotic Prophylaxis in Oral Surgery
 An Evidence Based Approach to Antibiotic Prophylaxis in Oral Surgery Nicholas Makhoul DMD. MD. FRCD(C). Dip ABOMS. FACS. Director, Division of Oral and Maxillofacial Surgery Assistant Professor McGill
An Evidence Based Approach to Antibiotic Prophylaxis in Oral Surgery Nicholas Makhoul DMD. MD. FRCD(C). Dip ABOMS. FACS. Director, Division of Oral and Maxillofacial Surgery Assistant Professor McGill
Antimicrobial Selection to Combat Resistance
 Antimicrobial Selection to Combat Resistance (Dead Bugs Don t Mutate!) Shelley C Rankin PhD Associate Professor CE Microbiology Head of Diagnostic Services & Chief of Clinical Microbiology Ryan Veterinary
Antimicrobial Selection to Combat Resistance (Dead Bugs Don t Mutate!) Shelley C Rankin PhD Associate Professor CE Microbiology Head of Diagnostic Services & Chief of Clinical Microbiology Ryan Veterinary
PREVENTION OF SURGICAL SITE INFECTION
 PREVENTION OF SURGICAL SITE INFECTION Montreal, March 29 2011 Chantal Bellerose P. Dt., BScHN, M.Sc. Adm Claude Laflamme MD, FRCPC, MHSC(c) Sandra Savery BScN, M.Sc.Adm Disclosure Financial disclosure:
PREVENTION OF SURGICAL SITE INFECTION Montreal, March 29 2011 Chantal Bellerose P. Dt., BScHN, M.Sc. Adm Claude Laflamme MD, FRCPC, MHSC(c) Sandra Savery BScN, M.Sc.Adm Disclosure Financial disclosure:
EcoHydra Antimicrobial Handwash. Product Overview. Physical Properties. Product Description. Regulatory Compliance. Key Features and Benefits
 EcoHydra Antimicrobial Handwash Product Overview Product Description The EcoHydra Antimicrobial Handwash is a liquid soap substitute for the wet method of washing and disinfecting to remove dirt and kill
EcoHydra Antimicrobial Handwash Product Overview Product Description The EcoHydra Antimicrobial Handwash is a liquid soap substitute for the wet method of washing and disinfecting to remove dirt and kill
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS
 VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
Burn Infection & Laboratory Diagnosis
 Burn Infection & Laboratory Diagnosis Introduction Burns are one the most common forms of trauma. 2 million fires each years 1.2 million people with burn injuries 100000 hospitalization 5000 patients die
Burn Infection & Laboratory Diagnosis Introduction Burns are one the most common forms of trauma. 2 million fires each years 1.2 million people with burn injuries 100000 hospitalization 5000 patients die
Approach to Antibiotics in Obstetrics: Surgical Prophylaxis for Cesareans
 Approach to Antibiotics in Obstetrics: Surgical Prophylaxis for Cesareans Amy Murtha, MD Associate Professor Vice Chair for Research Department of Ob/Gyn Objectives Review antibiotic prophylaxis for
Approach to Antibiotics in Obstetrics: Surgical Prophylaxis for Cesareans Amy Murtha, MD Associate Professor Vice Chair for Research Department of Ob/Gyn Objectives Review antibiotic prophylaxis for
Antimicrobial Prophylaxis for Surgical and Non-surgical Procedures
 Antimicrobial Prophylaxis for Surgical and Non-surgical Procedures Written by: Dr Linda Jewes, Consultant Microbiologist Date: April 2016 Approved by: Drugs & Therapeutics Committee Date: September 2016
Antimicrobial Prophylaxis for Surgical and Non-surgical Procedures Written by: Dr Linda Jewes, Consultant Microbiologist Date: April 2016 Approved by: Drugs & Therapeutics Committee Date: September 2016
Performing Rodent Survival Surgery
 University of Louisville Institutional Animal Care and Use Committee Policies and Procedures Performing Rodent Survival Surgery Policy: Survival surgical procedures in rodents requires aseptic techniques
University of Louisville Institutional Animal Care and Use Committee Policies and Procedures Performing Rodent Survival Surgery Policy: Survival surgical procedures in rodents requires aseptic techniques
Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS
 Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care Dell Seton Medical Center at the University of Texas and Seton Healthcare Family Clinical
Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care Dell Seton Medical Center at the University of Texas and Seton Healthcare Family Clinical
Surgical Cross Coder. Essential links from CPT codes to ICD-9-CM and HCPCS codes
 Essential links from CPT codes to ICD-9-CM and HCPCS codes 2016 Contents Introduction... iii Cardiovascular System...527 Digestive System...707 General...1 Integumentary System...9 Musculoskeletal System...173
Essential links from CPT codes to ICD-9-CM and HCPCS codes 2016 Contents Introduction... iii Cardiovascular System...527 Digestive System...707 General...1 Integumentary System...9 Musculoskeletal System...173
Top Ten Articles Infection Prevention and Control
 Top Ten Articles Infection Prevention and Control 2017-2018 John M Conly MD Chingiz Amirov Just wash em! May 2018 Objectives Research or evidence-based guidelines in IPC Critique strengths and weaknesses
Top Ten Articles Infection Prevention and Control 2017-2018 John M Conly MD Chingiz Amirov Just wash em! May 2018 Objectives Research or evidence-based guidelines in IPC Critique strengths and weaknesses
Institute of Surgical Research
 Institute of Surgical Research Surgical techniques A5 Practical Module. A1. MODUL - Asepsis and the surgeon A2. MODUL Surgical instrumentation A3. MODUL Operations A4. MODUL Bleedings A5. MODUL sterile
Institute of Surgical Research Surgical techniques A5 Practical Module. A1. MODUL - Asepsis and the surgeon A2. MODUL Surgical instrumentation A3. MODUL Operations A4. MODUL Bleedings A5. MODUL sterile
Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site:
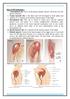 Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site: is the thick and well developed in both adults and children.
Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site: is the thick and well developed in both adults and children.
Antimicrobial Stewardship. We cannot afford to go back
 Antimicrobial Stewardship We cannot afford to go back Objectives What is antimicrobial stewardship? Why the concern over antibiotic resistance? Discuss the role and use of antibacterial medical devices
Antimicrobial Stewardship We cannot afford to go back Objectives What is antimicrobial stewardship? Why the concern over antibiotic resistance? Discuss the role and use of antibacterial medical devices
Clinical Study of Surgical Site Infection
 Clinical Study of Surgical Site Infection Dr. Balaji Prabhakaran, Dr. Mohamed Afjal, Dr. Saptarshi Paul Abstract: Background and objective: Study most common organisms encountered and their sensitivity
Clinical Study of Surgical Site Infection Dr. Balaji Prabhakaran, Dr. Mohamed Afjal, Dr. Saptarshi Paul Abstract: Background and objective: Study most common organisms encountered and their sensitivity
Surgical Site Infection (SSI) Prevention: The Latest, Greatest and Unanswered Questions
 Surgical Site Infection (SSI) Prevention: The Latest, Greatest and Unanswered Questions Keith S. Kaye, MD, MPH Corporate Vice President of Quality and Patient Safety Corporate Medical Director, Infection
Surgical Site Infection (SSI) Prevention: The Latest, Greatest and Unanswered Questions Keith S. Kaye, MD, MPH Corporate Vice President of Quality and Patient Safety Corporate Medical Director, Infection
Surgical Wound Management in Dogs using an Improved Stable Chlorine Dioxide Antiseptic Solution.
 Case Report Surgical Wound Management in Dogs using an Improved Stable Chlorine Dioxide Antiseptic Solution. Chapnick A 1 and Wilkins RJ *2 Journal of Veterinary Science & Animal Husbandry Volume 1 Issue
Case Report Surgical Wound Management in Dogs using an Improved Stable Chlorine Dioxide Antiseptic Solution. Chapnick A 1 and Wilkins RJ *2 Journal of Veterinary Science & Animal Husbandry Volume 1 Issue
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Measure #20 (NQF 0270): Perioperative Care: Timing of Prophylactic Parenteral Antibiotic Ordering Physician
 Measure #20 (NQF 0270): Perioperative Care: Timing of Prophylactic Parenteral Antibiotic Ordering Physician 2014 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage of surgical
Measure #20 (NQF 0270): Perioperative Care: Timing of Prophylactic Parenteral Antibiotic Ordering Physician 2014 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage of surgical
Author - Dr. Josie Traub-Dargatz
 Author - Dr. Josie Traub-Dargatz Dr. Josie Traub-Dargatz is a professor of equine medicine at Colorado State University (CSU) College of Veterinary Medicine and Biomedical Sciences. She began her veterinary
Author - Dr. Josie Traub-Dargatz Dr. Josie Traub-Dargatz is a professor of equine medicine at Colorado State University (CSU) College of Veterinary Medicine and Biomedical Sciences. She began her veterinary
Diabetic Foot Infection. Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals
 Diabetic Foot Infection Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals History of previous amputation [odds ratio (OR)=19.9, P=.01], Peripheral vascular disease (OR=5.5, P=.007)
Diabetic Foot Infection Dr David Orr Consultant Microbiologist Lancashire Teaching Hospitals History of previous amputation [odds ratio (OR)=19.9, P=.01], Peripheral vascular disease (OR=5.5, P=.007)
So Why All the Fuss About Hand Hygiene?
 CARING PROFESSIONAL SERVICES, INC. HAND HYGIENE In-Service So Why All the Fuss About Hand Hygiene? Most common mode of transmission of pathogens is via hands! Infections acquired in healthcare Spread of
CARING PROFESSIONAL SERVICES, INC. HAND HYGIENE In-Service So Why All the Fuss About Hand Hygiene? Most common mode of transmission of pathogens is via hands! Infections acquired in healthcare Spread of
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance
 Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Schimmelbusch 1886 sterilization of instruments using soda lye rubber glowes and surgical gowns
 Surgical asepsis and antisepsis Prof. MVDr. Alois Nečas, PhD, MBA Development of Surgery 1. Discovery of the anesthesia 2. Development of antiseptic metods Infection of the surgical wound - complication
Surgical asepsis and antisepsis Prof. MVDr. Alois Nečas, PhD, MBA Development of Surgery 1. Discovery of the anesthesia 2. Development of antiseptic metods Infection of the surgical wound - complication
Is biocide resistance already a clinical problem?
 Is biocide resistance already a clinical problem? Stephan Harbarth, MD MS University of Geneva Hospitals and Faculty of Medicine, Geneva, Switzerland Important points Biocide resistance exists Antibiotic
Is biocide resistance already a clinical problem? Stephan Harbarth, MD MS University of Geneva Hospitals and Faculty of Medicine, Geneva, Switzerland Important points Biocide resistance exists Antibiotic
UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee
 UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee Policy: Surgical Guidelines EFFECTIVE ISSUE DATE: 2/21/2005 REVISION DATE(s): 2/14/15; 3/19/2018 SCOPE To describe guidelines and considerations
UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee Policy: Surgical Guidelines EFFECTIVE ISSUE DATE: 2/21/2005 REVISION DATE(s): 2/14/15; 3/19/2018 SCOPE To describe guidelines and considerations
Anti-infective Studies
 Anti-infective Studies Blast-related Polytraumatic Extremity Wounds and Infectious Outcomes: Trauma Infectious Disease Outcomes Study and Trauma-associated Osteomyelitis Trauma Infectious Disease Outcomes
Anti-infective Studies Blast-related Polytraumatic Extremity Wounds and Infectious Outcomes: Trauma Infectious Disease Outcomes Study and Trauma-associated Osteomyelitis Trauma Infectious Disease Outcomes
UDC: : :579.22/ :615.28
 www.imiamn.org.ua /journal.htm 8 UDC: 6.33:61.017.1:579./.841.9:6.8 SUBSTANTIATION OF OVERCOMING OF ANTIBIOTIC RESISTANCE IN ACINETOBACTER BAUMANNII CLINICAL STRAINS BY USAGE OF DECAMETHOXINUM Nazarchuk
www.imiamn.org.ua /journal.htm 8 UDC: 6.33:61.017.1:579./.841.9:6.8 SUBSTANTIATION OF OVERCOMING OF ANTIBIOTIC RESISTANCE IN ACINETOBACTER BAUMANNII CLINICAL STRAINS BY USAGE OF DECAMETHOXINUM Nazarchuk
