MINOR PROCEDURES FOR ED/URGENT CARE
|
|
|
- Rosemary Parker
- 5 years ago
- Views:
Transcription
1 MINOR PROCEDURES FOR ED/URGENT CARE ELIZABETH BLUNT, RN, PHD, FNP -BC COLLEEN STELLABOTTE, RN, MSN, FNP -BC 1
2 Taser Removal 2
3 Taser Facts Brand name Electronic Control Weapon (ECW) Acronym from a 20 th century children s book Thomas A. Swift Electric Rifle Used to stun or incapacitate persons Provides a safer less than lethal force option 3
4 How Tasers Work Interferes with the ability of the brain to communicate with the muscles. Contacting the target on any body area leads to full incapacitation. Fires 2 small darts that act as electrodes Darts stay connected to the taser by thin conductive wires. When 2 darts stick a 5 second electrical charge is released. 4
5 Devices 5
6 Devices 6
7 7
8 How safe Extensive review of literature reveals injuries are associated with the fall and not from the electrical impulse. Do not cause cardiac arrhythmias when used appropriately and the exposure lasts for <15 seconds. High voltage with low wattage is the key to understanding the low electrical risk. Standard impulse setting is 5 seconds. Not risk free but a less lethal form of force. 8
9 Medical Considerations Threshold to induce ventricular fibrillation in a normal heart is joules. Most tasers fire at 0.5 joules or less. The most popular model fires at 0.3 joules, 30 times less than the threshold. High risk populations Pregnant women Elderly persons Young children Visibly frail Heart disease Medical/mental crisis Persons under the influence of alcohol/drugs 9
10 Assessment Confirm taser is off and cartridge is disconnected from the device. General survey of the patient addressing any serious injury from the fall. Evaluate the anatomical location of barbs. High risk zones Head Eyes Ears Nose Mouth Neck Genital Spine Hands, feet and joints 10
11 Barb Removal Universal precautions Local anesthetic Stabilize the skin surrounding the barb with your dominant using hemostats firmly grasp the barb with the notch facing up, jerk in a smooth quick motion Visually examine the barb to ensure it is fully intact Taser barb is considered a sharp, take all precautions to avoid accidental needle stick 11
12 Barb Removal Place barb in an appropriate container and return to law enforcement officer for evidence. Cleanse wound with antiseptic and dress. Up date tetanus immunization Instruct patient on basic wound care and signs and symptoms of infection. 12
13 Conclusion Current medical literature does not support the need for routine laboratory studies, electrocardiograms or prolonged ED observation after electrical exposure from a Electrical Control Device in an otherwise asymptomatic awake and alert individual. 13
14 ANIMAL BITE WOUNDS 14
15 EPIDEMIOLOGY Difficult to determine actual numbers because many are not reported CDC reports that an average of 4.5 million bites per year 885,000 require medical attention In 2006, 31,000 underwent reconstructive surgery Children are the most frequent victims 15
16 PRINCIPLES OF DISEASE Bites are traumatic injuries that cause damage to skin, muscle, nerves, blood vessels, tendons, joints and bones Wounds can be lacerations, contusions, scratches, tear or deep punctures Contamination with oral flora makes local wound infection the principle treatment concern along with rabies and tetanus immunization status Most US cities have animal bite reporting laws 16
17 CLINICAL MANAGEMENT Prevention and treatment of local bacterial infection and prevention, recognition and management of subsequent systemic illness Initial assessment for life threatening injury Meticulous exam and wound cleaning Special attention to wounds that involve joint space penetration 17
18 CLINICAL MANAGEMENT Facial, hands, and perineum wounds can be problematic due to the close proximity of delicate structures Image wounds if there is any suspicion of a foreign body Primary closure for cosmetic and functional issues Delayed primary closure is most successful Tetanus and Rabies immunization evaluation 18
19 HELICOPTER ACRONYM H E L I C O P T E R History Examination Liberal cleansing Irrigation Closure & culture consideration Operative cleansing and closure Prophylactic or therapeutic antimicrobial use Tetanus immunization status Elevation Rabies risk 19
20 TETANUS PROPHYLAXIS 20
21 RABIES PROPHYLAXIS Rare disease in developed countries Significant North American reservoirs of animal rabies exists in bats, skunks, raccoons and foxes. All carnivores and omnivores are potential vectors for updated information 21
22 RABIES PROPHYLAXIS DOG AND CAT BITES Condition of animal at time of attack Treatment of exposed person Healthy and available for 10 day observation No treatment unless animal develops rabies Rabid, suspected rabid, or escaped RIG and HDCV 22
23 RABIES PROPHYLAXIS Animal species Wild Skunk, bat, fox, raccoon, bobcat, and other carnivores Condition of animal at time of attack Regard as rabid Treatment of exposed person RIG and HDCV Bites from squirrels, hamsters, guinea pigs, gerbils, chipmunks, rats, mice, rabbits and hares almost never call for rabies prophylaxis. Consult local public health officials. 23
24 RABIES IMMUNOGLOBULIN (RIG) 20 IU/kg of body weight If anatomically feasible up to half the dose should be infiltrated around the wound and the rest administered in the gluteal area RIG should not be administered in the same syringe or into the same anatomic site as the vaccine because RIG may partially suppress active production of antibody 24
25 RABIES VACCINE (HDCV) HDCV 1 ml IM deltoid area on Day 0 Day 3 Day 7 Day 14 25
26 ANTIMICROBIAL TREATMENT All puncture wounds Bites involving hands, feet, face, or genital area Moderate or severe wounds All wounds in immunocompromised patients Bite wounds with signs of infection 26
27 PROPHYLACTIC ANTIBIOTICS Refer to the Sanford Guide to Antimicrobial Therapy or other source for specific bites Overall initial therapy for most bites and those not allergic to penicillin is Amoxicillin-Clavulanate Alternative combinations vary with specific animals 27
28 BATS Most recent human rabies has been caused by bats Contact with bats increases suspicion of rabies exposure Consult local health department and CDC Rabies is not transmitted by bat guano, urine or blood 28
29 DOG BITE 5-6 % become infected Pastaurella and anaerobes most common microorganism Capnocytophaga canimorsus rare but fulminant bacteremia following a dog bite 29
30 CAT BITES % become infected Narrow sharp teeth increase the susceptibility to deliver infectious agents through puncture wounds Pastaurella Multocida most common microorganism Cat scratch disease 7-12 days after bite or scratch 30
31 HUMAN BITES 31
32 HUMAN BITE WOUNDS AND CLOSED FIST INJURIES (CFI) Associated with a high incidence of infection, approximately 60%, especially with hand injuries Polymicrobial, staph and strept species Eikenella Corrodens common bacteria If blood involved hep B and HIV prophylaxis may be warranted CDC post exposure prophylaxis 24 hour hot line, for consultation 32
33 FERRET BITES 3rd most popular pet in the US Usually attack face and neck Little is known about the bacteriology of ferret bites CDC recommends management strategy similar to that for other domestic animals, 10 day observation. 33
34 DOMESTIC HERBIVORES 34
35 HORSES AND PIGS Pigs and horses can inflict serious injury with their powerful jaws and grinding teeth Usually require careful debridement and exploration High risk of infection Polymicrobial 35
36 RODENT BITES Usually trivial No rabies Rat bite fever- 2 similar febrile illnesses diagnosis confirmed by blood culture for streptobacillus moniliformis or spirillum minus rare Hantavirus is also rare transmission 36
37 OPHTHALMOLOGY Anatomy External Lid Eyelashes Internal Cornea Conjunctiva Iris Limbus Sclera 37
38 OPHTHALMOLOGIC EVALUATION History Traumatic Atraumatic Red Flags Pain Visual disturbance Vital sign of the eye Visual acuity Snellen chart pt stands 20 ft from chart Hand held 13 inches 38
39 OPHTHALMOSCOPE Filter dial Large, medium small Half light Red free Slit beam Blue light Focusing wheel Positive focuses objects that are close Negative wheel focuses objects that are far away 39
40 SLIT LAMP Illumination system Bio microscope Basic goals r/o globe rupture, corneal abrasion, ulcerations, and foreign bodies Provides superior magnification Tangential lighting assists in the diagnosis of uveitis and iritis 40
41 EYE PRESSURES Indications Eye pain Eye trauma mmhg normal Numerous tools 41
42 Tonopen Anesthetize the eye Apply latex cover Calibrate unit if not already done (every 24 hours) Press activation switch, ==== appears indicating ok to test Probe is held like a pen, briefly and lightly touched to the cornea Do 4 times After 4 valid readings a final beep will sound and display an averaged measurement 42
43 Tonopen 43
44 CHEMICAL BURNS Serious damage arises from strong basic and acidic compounds Severity is related to type of substance, volume, concentration, duration and mechanism Treatment goals- aggressive early management and close long term monitoring 44
45 Chemicals Acidic Battery acid (e.g., sulfuric acid) Bleach (e.g., sulfurous acid) Glass polish (e.g., hydrofluoric; behaves like alkali) Vinegar (e.g., acetic acid) Chromic acid (brown discoloration of conjunctiva) Nitric acid (yellow discoloration of conjunctiva Alkaline Cleaning products (e.g., ammonia) Fertilizers (e.g., ammonia) Drain cleaners (e.g., lye) Cement, plaster, mortar (e.g., lime) Airbag rupture (e.g., sodium hydroxide) Fireworks (e.g., magnesium hydroxide) Potash (e.g., potassium hydroxide) 45
46 MANAGEMENT Remove offending agent Irrigation Must contact ocular surface to be effective 1-2 liters Morgan lens Test ph Rx artificial tears Pain management Close ophthalmologic follow up 46
47 EYE FOREIGN BODY REMOVAL Topical anesthetic Measure visual acuity Inspect cornea If fb is visualized attempt removal with a moistened cotton-tip applicator If successful, fluorescein stain and inspect Evert upper lid to rule out pre-tarsal fb If unsuccessful refer to ophthalmology 47
48 EVERTING EYELID 48
49 FLUOROSCEIN STAINING Recommended for any red eye Procedure Grasp non-orange end Apply 1 drop of saline Gently place inside the lower lid Instruct pt to blink Use a wood lamp, blue filter on s slit lamp or a penlight with a blue filter 49
50 FLU0ROSCEIN STAINING 50
51 RING REMOVAL Remove all rings before edema!!!! Methods Lubrication String method Cut Consider anesthesia 51
52 RING CUTTER 52
53 STRING METHOD Wrap a Penrose drain circumferentially proximal to distal in piece of string Pass string under ring Wrap proximal to distal not allowing any skin to protrude Grasp proximal end, turn clockwise 53
54 FISHHOOK REMOVAL 54
55 The Problem is. 55
56 Fishhooks Variety of shapes and sizes Barb is a projection extending backward from the point of the hook. 56
57 Fish Hook Removal Several methods for successful removal Strategy depends primarily on the depth of the hook Caution to be taken for removal of a hook with multiple barbs Anesthetize the area either locally or by a digital block depending on location 57
58 Simple Retrograde Technique Press skin over tip of hook to disengage barb while apply pressure downward on shank Back the hook out of the skin Most simple but least effective 58
59 String Pull Method Variation of retrograde technique String is wrapped around the bend of the hook where it enters the skin End of the shank is depressed with one hand to disengage the barb. The other hand gives a quick pull on the string 59
60 Needle Cover Technique Requires dexterity 18g needle is inserted into the entrance wound along side of the shank Needle follows the hook until the lumen covers the barb The hook and needle are withdrawn from the wound as a unit 60
61 Advance & Cut Technique Useful for deep penetration and large hooks Tip is advanced through the skin Once exposed tip and barb are cut with wire cutters The remaining part is rotated back out of the wound 61
62 62
63 Incision Technique Modified needle cover technique Used for hooks embedded in dermis or in delicate areas Enlarge of wound with a #11 scalpel, follow the bend of the hook until the barb is disengaged from the tissue Withdraw hook through the wound 63
64 Arthrocentesis & Joint Injection The Basics
65 Arthrocentesis Aspiration of fluid from a joint space May be diagnostic or therapeutic Generally presents few complications Joint injection may occur after fluid removal or may be performed as a separate procedure
66 Indications Diagnosis of non-traumatic joint disease Relief of pain Removal of effusion Local infiltration of medication Diagnosis of bony or ligament injury Establishment of intra-articular fracture Obtain fluid for culture & cell study
67 Contraindication Absolute Overlying infection Cellulitis Abscess Suspected bacteremia Steroid injection Septic joint Relative Recent fracture Osteoporosis Anticoagulants Bleeding disorders
68 Requirements Always ensure complete H&P before procedure X-Rays? Check for allergies Previous joint aspirations or injections? Informed consent
69 Decisions Aspirate? Inject? Both?
70 Fluid Analysis Observation Chemical Analysis Microscopic Study Bacterial Culture Serologic Study Polarized Light Microscope
71 Synovial Fluid Analysis Fluid grossly assessed as clear, turbid or bloody Most important to distinguish between inflammatory and infectious causes Normal synovial fluid is Straw, clear enough to read newspaper Flows freely consistency of motor oil Gives positive string test
72 String Test Simple test for fluid viscosity Viscosity correlates with hyaluronate Inflammation degrades hyaluronate which becomes lowers viscosity Measure fluid string from falling drop of gloved finger Normal fluid = 5-10cm string Inflammation = short string or multiple drops
73
74 Specimen Collection Cell count and cytology lavender top tube (EDTA) Chemistries, serology and viscosity red top tube ( no additive) Crystals green top tube(sodium heparin) or immediate visualization under microscope
75 Specimen Collection GC culture medium, low oxygen level Culture appropriate medium
76 Synovial Fluid Analysis Indicator Normal Inflammatory Infectious Gross Appearance Clear Transparent Yellow Clear-slightly turbid Yellow Cloudy String Sign Normal Diminished Diminished WBC/mm3 <200 <200 >2000 Culture Negative Negative >50% positive Crystals Negative Positive Negative
77 Common Joint Injection Sites Knee* Hip Ankle Shoulder* Glenohumeral joint Acromioclavicular joint Elbow* Lateral epicondyle Medial epicondyle Hand and Wrist Thumb* Trigger finger* wrist
78 Steroid Injection and Doses Preparation Large Joint Small Joint Triamcinolone hexacetonide 20mg 2-6mg Triamcinolone acetonide 20mg 2-6mg Prednisolone terbutate 25mg mg Betamethasone sodium 1ml ml Phosphate/acetate Methylprednisolone 35mg mg Triamcinolone diacetate 20mg 2-6mg Prednisone acetate 30mg 3-9mg
79 Frequency of Injection 6 to 12 weeks between injection No more than 3 times per year for large or weight bearing joints Inject no more than 3 separate joints per month
80 Equipment Sterile gloves Skin prep Iodine & alcohol Sterile 4x4 s Sterile towels Vapor coolant 1% or 2% lidocaine Non lock syringes 2ml, 10ml, 30ml Needles 18, 22, 25 gauge Hemostat 3-way stopcock Specimen equipment Steroid injection Sterile dressing
81 Stop Cock
82 Procedure Thorough H & P Position patient optimally Knee fully extended with relaxed quadriceps Elbow flexed 90 degrees, forearm pronated, palm flat on table Spend time to find anatomical landmarks!!!!!!
83
84
85
86
87
88
89 Procedure Aseptic technique Clip thick hair Area thoroughly scrubbed Bactericidal agent x 3 Medial to lateral aspect in circular motion Allow to dry between scrubs Clean area with alcohol Sterile gloves and equipment
90 Procedure Anesthesia for Site Vapor coolant 1% or 2% Lidocaine (rapid onset; 1-2 hrs) OR Bupivacaine (5 minutes; 2-4 hrs) OR Diphenhydramine OR Ice
91 Procedure Identify Landmarks!! Use larges practical needle 18 gauge aspiration 25 gauge for injection Use appropriate syringe 30cc or 60cc for aspiration Insert needle, pull back on plunger, enter joint space
92 Procedure Withdraw all fluid Use hemostat or stopcock to change syringe Assess fluid and transfer into container Cell count, culture, slide, string test If injecting change syringe and inject Withdraw needle and apply dressing
93 Potential Complications Infection Introduction Masking with steroid Steroid arthropathy Post injection inflammation (steroid flare hours)
94 Potential Complications Bleeding and blood vessel trauma Peri-articular complications Tendon rupture Soft tissue atrophy Systemic responses Elevated BS Peripheral flushing
95 Follow-Up Band-Aid Rest, Ice, Elevation, Compression Limited weight bearing for 48 hours Consider knee immobilizer NSAID or other analgesic Instructions for signs of infection
96 Conclusions When performed correctly, arthrocentesis is a relatively safe procedure that is used to obtain valuable diagnostic information and provide therapy for acute joint disease. The key to success is strict adherence to sterile technique, observance of anatomic landmarks and proper preparation of synovial fluid for examination.
97 Musculoskeletal Injuries Extremity X-Rays Splinting 97
98 MUSCULOSKETAL EVALUATION History!!!!! Traumatic vs atraumatic Mechanism of injury Physical Exam Diagnostics X-ray CT MRI 98
99 CLASSIFICATION OF SPRAINS/STRAINS Sprain- injury to the ligament that connects a bone to another Strain-injury to the muscle fibers and to other fibers that attach to the muscle. 1 ST DEGREE 2 ND DEGREE 3 RD DEGREE 99
100 OTTAWA ANKLE RULES 100
101 TYPES OF FRACTURES 101
102 RADIOLOGY HAND WRIST ELBOW KNEE ANKLE FOOT 102
103 MANAGEMENT P Protect from further injury. R Restrict activity. I Apply Ice. C Apply Compression. E Elevate the injured area 103
104 SPLINT INDICATIONS Sprain/strains Fractures Lacerations Inflammatory processes Infection/cellulitis 104
105 SPLINT MATERIAL Pre-formed Plaster Fiberglass 105
106 SPLINTING Upper extremity Volar Long posterior Sugar tong Thumb Spica Ulna gutter Finger splint Lower extremity Knee immobilizer Posterior leg Long Short Stirrup Cam boot Hard shoe 106
107 VOLAR 107
108 SUGAR TONG 108
109 THUMB SPICA 109
110 ANKLE STIRRUP 110
111 POSTERIOR LEG 111
112 KNEE IMMOBILIZER 112
113 ANKLE AND FOOT 113
114 COMPLICATIONS Ischemia Heat injury plaster Pressure sores Infection Dermatitis 114
115 Let s Splint 115
SESSION 2 8:45 10am. In-office Procedures. Contraindications to Injection. Introduction Joint and Soft Tissue Injection. Learning Objective
 SESSION 2 8:45 10am Procedures You Can Do In Your Office SPEAKER Roger W. Bush, MD, MACP Presenter Disclosure Information The following relationships exist related to this presentation: Roger Bush, MD,
SESSION 2 8:45 10am Procedures You Can Do In Your Office SPEAKER Roger W. Bush, MD, MACP Presenter Disclosure Information The following relationships exist related to this presentation: Roger Bush, MD,
الكلب عضة = bite Dog Saturday, 09 October :56 - Last Updated Wednesday, 09 February :07
 Dog bite Almost 75 million dogs live in the United States, and since many victims of dog bites don't seek medical care or report the attack, it may be that the U.S. Center for Disease Control and Prevention
Dog bite Almost 75 million dogs live in the United States, and since many victims of dog bites don't seek medical care or report the attack, it may be that the U.S. Center for Disease Control and Prevention
Emergency Management of Life Threatening Problems
 The management of wounds constitutes a significant topic of Emergency Medicine and I will briefly discuss with you first the emergency management of life threatening problems followed by wound assessment
The management of wounds constitutes a significant topic of Emergency Medicine and I will briefly discuss with you first the emergency management of life threatening problems followed by wound assessment
COALINGA STATE HOSPITAL. NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF WOUNDS (FIRST AID) 1. PURPOSE: Proper
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF WOUNDS (FIRST AID) 1. PURPOSE: Proper
MANAGEMENT OF HUMAN EXPOSURES TO SUSPECT RABID ANIMALS A GUIDE FOR PHYSICIANS AND OTHER HEALTH CARE PROVIDERS. July 2010 Update
 MANAGEMENT OF HUMAN EXPOSURES TO SUSPECT RABID ANIMALS A GUIDE FOR PHYSICIANS AND OTHER HEALTH CARE PROVIDERS July 2010 Update DIVISION OF INFECTIOUS DISEASES & EPIDEMIOLOGY RABIES CONTROL PROGRAM Major
MANAGEMENT OF HUMAN EXPOSURES TO SUSPECT RABID ANIMALS A GUIDE FOR PHYSICIANS AND OTHER HEALTH CARE PROVIDERS July 2010 Update DIVISION OF INFECTIOUS DISEASES & EPIDEMIOLOGY RABIES CONTROL PROGRAM Major
Disclosures. Consider This Case. Objectives. Consequences of Bites. Animal Bites: What to Do and What to Avoid. Animal Bites: Epidemiology
 Animal Bites: What to Do and What to Avoid Meg Fisher, MD Medical Director Disclosures I have no disclosures I do not plan to discuss off label uses of drugs Objectives Manage a child who is bitten Discuss
Animal Bites: What to Do and What to Avoid Meg Fisher, MD Medical Director Disclosures I have no disclosures I do not plan to discuss off label uses of drugs Objectives Manage a child who is bitten Discuss
RABIES AND ITS PREVENTION. IAP UG Teaching Slides
 RABIES AND ITS PREVENTION 1 RABIES Etiology Rabies neurotropic virus, Lyssavirus genus Is a zoonotic disease Transmitted mainly by exposure to rabid animals (By bite, scratch, lick on damaged skin or intact
RABIES AND ITS PREVENTION 1 RABIES Etiology Rabies neurotropic virus, Lyssavirus genus Is a zoonotic disease Transmitted mainly by exposure to rabid animals (By bite, scratch, lick on damaged skin or intact
Dirty Wounds. Christopher M. Ziebell, MD, FACEP
 Dirty Wounds Christopher M. Ziebell, MD, FACEP Types Fresh Water Salt Water Bites Cats Humans Dogs and other mammals Freshwater Trauma Recognize this finger? Lindsey Lohan Microbiology Usual suspects:
Dirty Wounds Christopher M. Ziebell, MD, FACEP Types Fresh Water Salt Water Bites Cats Humans Dogs and other mammals Freshwater Trauma Recognize this finger? Lindsey Lohan Microbiology Usual suspects:
Intramuscular injections are administered according to established procedure in the adult patient.
 POLICY & PROCEDURE TITLE: IM Injection in Adult Patient Scope/Purpose: To document the standard of care in administering adult intramuscular injections in HealthPoint clinics. Division/Department: All
POLICY & PROCEDURE TITLE: IM Injection in Adult Patient Scope/Purpose: To document the standard of care in administering adult intramuscular injections in HealthPoint clinics. Division/Department: All
DISCUSS HAND HYGIENE AND PERFORM HAND ANTISEPSIS
 DISCUSS HAND HYGIENE AND PERFORM HAND ANTISEPSIS 1. TITLE SLIDE: DISCUSS HAND HYGIENE AND PERFORM HAND ANTISEPSIS. Hands are one of the most common sources of the spread of pathogenic microorganisms. Hand
DISCUSS HAND HYGIENE AND PERFORM HAND ANTISEPSIS 1. TITLE SLIDE: DISCUSS HAND HYGIENE AND PERFORM HAND ANTISEPSIS. Hands are one of the most common sources of the spread of pathogenic microorganisms. Hand
F1 IN THE NAME OF GOD
 F1 IN THE NAME OF GOD Slide 1 F1 FEIKO.IR.SOFT; 2011/07/06 Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion
F1 IN THE NAME OF GOD Slide 1 F1 FEIKO.IR.SOFT; 2011/07/06 Lid Laceration Conjunctival Hemorrhage a) No therapy is necessary b) Usually resolve in 7-12 days. Subconjunctival Hemorrhage Corneal Abrasion
EC-AH-011v1 January 2018 Page 1 of 5. Standard Operating Procedure Equine Center Clemson University
 EC-AH-011v1 January 2018 Page 1 of 5 Standard Operating Procedure Equine Center Clemson University SOP ID: EC-AH-011v1 January 2018 Title: Injection Techniques Author(s): Julia Tagher, CU Equine Center
EC-AH-011v1 January 2018 Page 1 of 5 Standard Operating Procedure Equine Center Clemson University SOP ID: EC-AH-011v1 January 2018 Title: Injection Techniques Author(s): Julia Tagher, CU Equine Center
EMERGENCIES When to Call the Vet And What to Do Until They Arrive
 EMERGENCIES When to Call the Vet And What to Do Until They Arrive By Dr. Jennifer Fowlie, DVM, MSc Board Certified Equine Surgeon (DACVS) As a horse owner or caretaker, it is very helpful to know how to
EMERGENCIES When to Call the Vet And What to Do Until They Arrive By Dr. Jennifer Fowlie, DVM, MSc Board Certified Equine Surgeon (DACVS) As a horse owner or caretaker, it is very helpful to know how to
Model Infection Control Plan for Veterinary Practices, 2010
 Model Infection Control Plan for Veterinary Practices, 2010 National Association of State Public Health Veterinarians (NASPHV) Veterinary Infection Control Committee (VICC) This plan should be adapted
Model Infection Control Plan for Veterinary Practices, 2010 National Association of State Public Health Veterinarians (NASPHV) Veterinary Infection Control Committee (VICC) This plan should be adapted
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare
 Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Patient Preparation. Surgical Team
 January 2019 www.nursingcenter.com Surgical Site Infection Prevention Surgical site infections (SSIs) are one of the most common and costly healthcare-associated infections in the United States (Smith
January 2019 www.nursingcenter.com Surgical Site Infection Prevention Surgical site infections (SSIs) are one of the most common and costly healthcare-associated infections in the United States (Smith
Regional and Local Anesthesia of the Wrist and Hand Aided by a Forearm Sterile Elastic Exsanguination Tourniquet - A Review
 H E M A C L E A R P R E S S A u g u s t 2 0 1 2 P a g e 1 Regional and Local Anesthesia of the Wrist and Hand Aided by a Forearm Sterile Elastic Exsanguination Tourniquet - A Review Noam Gavriely, MD,
H E M A C L E A R P R E S S A u g u s t 2 0 1 2 P a g e 1 Regional and Local Anesthesia of the Wrist and Hand Aided by a Forearm Sterile Elastic Exsanguination Tourniquet - A Review Noam Gavriely, MD,
2015 Vet Assisting CDE Prelim Exam
 Florida FFA Association ID: A 2015 Vet Assisting CDE Prelim Exam True/False Indicate whether the statement is true or false. Mark your answer choices on your answer form. 1 Hamsters may safely be picked
Florida FFA Association ID: A 2015 Vet Assisting CDE Prelim Exam True/False Indicate whether the statement is true or false. Mark your answer choices on your answer form. 1 Hamsters may safely be picked
Clinical Practice Guidelines
 Community Health Services Home 1 of 15 Population and Public Health Nov 2, Family Med/Primary Mental Health 1.0 PURPOSE 1.1 To provide timely public health investigation of individuals who have experienced
Community Health Services Home 1 of 15 Population and Public Health Nov 2, Family Med/Primary Mental Health 1.0 PURPOSE 1.1 To provide timely public health investigation of individuals who have experienced
Equine Emergencies. Identification and What to do Until the Vet Arrives Kathryn Krista, DVM, MS
 Equine Emergencies Identification and What to do Until the Vet Arrives Kathryn Krista, DVM, MS Common Equine Emergencies Cellulitis/lymphangitis Choke (esophageal obstruction) Colic Eye abnormalities Fever
Equine Emergencies Identification and What to do Until the Vet Arrives Kathryn Krista, DVM, MS Common Equine Emergencies Cellulitis/lymphangitis Choke (esophageal obstruction) Colic Eye abnormalities Fever
SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS
 SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if
SURGICAL ANTIBIOTIC PROPHYLAXIS GUIDELINES WITHIN ORTHOPAEDIC SURGERY FOR ADULT PATIENTS Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if
Proceeding of the SEVC Southern European Veterinary Conference
 www.ivis.org Proceeding of the SEVC Southern European Veterinary Conference Oct. 17-19, 2008 Barcelona, Spain http://www.sevc.info Reprinted in the IVIS website with the permission of the SEVC www.ivis.org
www.ivis.org Proceeding of the SEVC Southern European Veterinary Conference Oct. 17-19, 2008 Barcelona, Spain http://www.sevc.info Reprinted in the IVIS website with the permission of the SEVC www.ivis.org
Hand washing, Asepsis, Precautions and Infection Control
 Hand washing, Asepsis, Precautions and Infection Control FN Ch 12, NICS Ch4 Week 2 Lesa McArdle, MSN, RN Objectives Hand washing, Asepsis, Precautions & Infection Control Explain the chain of infection
Hand washing, Asepsis, Precautions and Infection Control FN Ch 12, NICS Ch4 Week 2 Lesa McArdle, MSN, RN Objectives Hand washing, Asepsis, Precautions & Infection Control Explain the chain of infection
Rabies Postexposure Treatment Recommendations. Jennifer House, DVM, MPH, DACVPM Veterinary Epidemiologist
 Rabies Postexposure Treatment Recommendations Jennifer House, DVM, MPH, DACVPM Veterinary Epidemiologist Bite Treatment Clean wound Use a virucidal agent Evaluate the need for antibiotics 2 Incubation
Rabies Postexposure Treatment Recommendations Jennifer House, DVM, MPH, DACVPM Veterinary Epidemiologist Bite Treatment Clean wound Use a virucidal agent Evaluate the need for antibiotics 2 Incubation
St George/Sutherland Hospitals And Health Services (SGSHHS)
 VASCATH INSTILLATION OF ANTICOAGULATION / ANTIBIOTIC LOCK Cross references (including NSW Health/ SESIAHS policy directives) NSW Health Policy for Medication Handling in NSW Public Hospitals PD207_007
VASCATH INSTILLATION OF ANTICOAGULATION / ANTIBIOTIC LOCK Cross references (including NSW Health/ SESIAHS policy directives) NSW Health Policy for Medication Handling in NSW Public Hospitals PD207_007
Surgical Site Infections (SSIs)
 Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Burn Infection & Laboratory Diagnosis
 Burn Infection & Laboratory Diagnosis Introduction Burns are one the most common forms of trauma. 2 million fires each years 1.2 million people with burn injuries 100000 hospitalization 5000 patients die
Burn Infection & Laboratory Diagnosis Introduction Burns are one the most common forms of trauma. 2 million fires each years 1.2 million people with burn injuries 100000 hospitalization 5000 patients die
Questions and Answers about Rabies
 Pets 1. Q: How can I protect my pet from rabies? A: There are several things you can do to protect your pet from rabies. First, visit your veterinarian with your pet on a regular basis and keep rabies
Pets 1. Q: How can I protect my pet from rabies? A: There are several things you can do to protect your pet from rabies. First, visit your veterinarian with your pet on a regular basis and keep rabies
Kristy Broaddus. Bite Wounds: Why are they so hard to manage? Bite Wounds 2/9/2016
 Kristy Broaddus Bite Wounds: Why are they so hard to manage? Kristy Broaddus, DVM, MS, DACVS VESC Richmond VA Michigan State DVM Auburn University internship and surgery residency Oklahoma State University
Kristy Broaddus Bite Wounds: Why are they so hard to manage? Kristy Broaddus, DVM, MS, DACVS VESC Richmond VA Michigan State DVM Auburn University internship and surgery residency Oklahoma State University
Illustrated Articles Northwestern Veterinary Hospital
 Page 1 of 5 First Aid in Cats Medical emergencies occur suddenly and without warning. It is important for all cat owners to have a basic understanding of common veterinary medical emergencies and basic
Page 1 of 5 First Aid in Cats Medical emergencies occur suddenly and without warning. It is important for all cat owners to have a basic understanding of common veterinary medical emergencies and basic
Providing Public Health Recommendations to Clinicians for Rabies Post Exposure Prophylaxis. Fall 2014
 Providing Public Health Recommendations to Clinicians for Rabies Post Exposure Prophylaxis Fall 2014 Which of the following describes how rabies virus is transmitted to people? (pick one) 1. Contact with
Providing Public Health Recommendations to Clinicians for Rabies Post Exposure Prophylaxis Fall 2014 Which of the following describes how rabies virus is transmitted to people? (pick one) 1. Contact with
How To Give Your Horse An Intramuscular Injection
 ANR-1018 A L A B A M A A & M A N D A U B U R N U N I V E R S I T I E S How To Give Your Horse An Intramuscular Injection Most horse owners occasionally must give their horse an injection. Fortunately,
ANR-1018 A L A B A M A A & M A N D A U B U R N U N I V E R S I T I E S How To Give Your Horse An Intramuscular Injection Most horse owners occasionally must give their horse an injection. Fortunately,
Each animal species exhibits different rabies symptoms.
 FLAGLER COUNTY SHERIFF S OFFICE Sheriff James L. Manfre Departmental Standards Directive TITLE: CONTROL OF ANIMALS SUSPECTED OF RABIES NUMBER: 41.19 EFFECTIVE: 1/3/07 RESCINDS/AMENDS: 12/01/03 STANDARDS:
FLAGLER COUNTY SHERIFF S OFFICE Sheriff James L. Manfre Departmental Standards Directive TITLE: CONTROL OF ANIMALS SUSPECTED OF RABIES NUMBER: 41.19 EFFECTIVE: 1/3/07 RESCINDS/AMENDS: 12/01/03 STANDARDS:
Animal Studies Committee Policy Rodent Survival Surgery
 Animal Studies Committee Policy Rodent Survival Surgery ASC Policy: To optimize animal health and well-being, survival surgery in rodents must be performed using sterile instruments, surgical gloves, masks
Animal Studies Committee Policy Rodent Survival Surgery ASC Policy: To optimize animal health and well-being, survival surgery in rodents must be performed using sterile instruments, surgical gloves, masks
CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II page 1
 CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II 1. What are the symptoms of an infected wound? a. Fever b. Edema c. Erythema d. Local pain and tenderness e. Induration of wound edge 2. A person with
CLPNA Pressure Ulcers ecourse: Module 5.6 Quiz II 1. What are the symptoms of an infected wound? a. Fever b. Edema c. Erythema d. Local pain and tenderness e. Induration of wound edge 2. A person with
Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site:
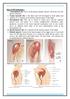 Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site: is the thick and well developed in both adults and children.
Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site: is the thick and well developed in both adults and children.
UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee
 UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee Policy: Surgical Guidelines EFFECTIVE ISSUE DATE: 2/21/2005 REVISION DATE(s): 2/14/15; 3/19/2018 SCOPE To describe guidelines and considerations
UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee Policy: Surgical Guidelines EFFECTIVE ISSUE DATE: 2/21/2005 REVISION DATE(s): 2/14/15; 3/19/2018 SCOPE To describe guidelines and considerations
Backcountry First Aid Prevention, Triage and
 Backcountry First Aid Prevention, Triage and Treatment Montana Equine Medical and Surgical Center Al Flint DVM, PhD Prior Planning Prevents. Prevention Trip Duration Trail Conditions Correct Fitting Tack
Backcountry First Aid Prevention, Triage and Treatment Montana Equine Medical and Surgical Center Al Flint DVM, PhD Prior Planning Prevents. Prevention Trip Duration Trail Conditions Correct Fitting Tack
ISPUB.COM. Animal Bites And Reconstruction. S Saraf INTRODUCTION PATIENTS AND METHODS
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 3 Number 1 S Saraf Citation S Saraf.. The Internet Journal of Plastic Surgery. 2006 Volume 3 Number 1. Abstract Animal bites resulting in significant
ISPUB.COM The Internet Journal of Plastic Surgery Volume 3 Number 1 S Saraf Citation S Saraf.. The Internet Journal of Plastic Surgery. 2006 Volume 3 Number 1. Abstract Animal bites resulting in significant
SOS EMERGENCY ANIMALS Please note that the following scenario(s) are generalized
 Suggested Tasks for Veterinary Students Volunteering at the VSPCA By Bosmat Gal, DVM Assistant to the President of the Animal Rescue League of Boston for International Programs Member of the VSPCA Advisory
Suggested Tasks for Veterinary Students Volunteering at the VSPCA By Bosmat Gal, DVM Assistant to the President of the Animal Rescue League of Boston for International Programs Member of the VSPCA Advisory
New Jersey Department of Health Rabies Background and Technical Information
 New Jersey Department of Health Rabies Background and Technical Information The History of Rabies Rabies is an ancient disease. It is well described in writings by Egyptians dating back to 2300 B.C. Rabies
New Jersey Department of Health Rabies Background and Technical Information The History of Rabies Rabies is an ancient disease. It is well described in writings by Egyptians dating back to 2300 B.C. Rabies
Animal Bites and Rabies
 Animal Bites and Rabies Animal bites Animal bites are not rare and can occur anywhere in the world. They can occur while: walking in the street jogging in the woods bicycle riding in the countryside or
Animal Bites and Rabies Animal bites Animal bites are not rare and can occur anywhere in the world. They can occur while: walking in the street jogging in the woods bicycle riding in the countryside or
Treatment of septic peritonitis
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
For use in beef cattle; dairy cattle; calves, including preruminating (veal) calves; and swine
 Liquamycin LA-200 (oxytetracycline injection) Antibiotic Each ml contains 200 mg of oxytetracycline base as oxytetracycline dihydrate. For use in beef cattle; dairy cattle; calves, including preruminating
Liquamycin LA-200 (oxytetracycline injection) Antibiotic Each ml contains 200 mg of oxytetracycline base as oxytetracycline dihydrate. For use in beef cattle; dairy cattle; calves, including preruminating
STANDARD OPERATING PROCEDURE #701 MACAQUE RELATED INJURY
 STANDARD OPERATING PROCEDURE #701 MACAQUE RELATED INJURY 1. PURPOSE This Standard Operating Procedure (SOP) describes the proper procedures for dealing with injuries sustained in the handling of macaques,
STANDARD OPERATING PROCEDURE #701 MACAQUE RELATED INJURY 1. PURPOSE This Standard Operating Procedure (SOP) describes the proper procedures for dealing with injuries sustained in the handling of macaques,
Wounds and skin injuries
 Wounds and skin injuries Overview Very minor wounds (cuts, grazes, burns, bites and bruises) often heal themselves. More serious wounds should always been seen by a vet. It s really important to stop your
Wounds and skin injuries Overview Very minor wounds (cuts, grazes, burns, bites and bruises) often heal themselves. More serious wounds should always been seen by a vet. It s really important to stop your
Investigation of potential rabies exposure situations
 Investigation of potential rabies exposure situations yond Sarah Scotland, MPH Epidemiologist Division of Epidemiology and Immunization Bureau of Infectious Disease and Laboratory Sciences Massachusetts
Investigation of potential rabies exposure situations yond Sarah Scotland, MPH Epidemiologist Division of Epidemiology and Immunization Bureau of Infectious Disease and Laboratory Sciences Massachusetts
The role of Infection Control Nurse in Prevention of Surgical Site Infection (SSI) April 2013
 The role of Infection Control Nurse in Prevention of Surgical Site Infection (SSI) April 2013 Impact of SSI 2 nd common health- care associated infection (HCAI) 14-16% of HCAI Post operation SSI prolong
The role of Infection Control Nurse in Prevention of Surgical Site Infection (SSI) April 2013 Impact of SSI 2 nd common health- care associated infection (HCAI) 14-16% of HCAI Post operation SSI prolong
SOP: Blood Collection in Swine
 SOP: Blood Collection in Swine These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during protocol
SOP: Blood Collection in Swine These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during protocol
Chapter 59 Wound Management Principles
 Chapter 59 Wound Management Principles Episode Overview: 1) List risk factors for wound infection 2) List the 5 stages of wound healing 3) List toxic doses of local anesthetics 4) List 3 types of wound
Chapter 59 Wound Management Principles Episode Overview: 1) List risk factors for wound infection 2) List the 5 stages of wound healing 3) List toxic doses of local anesthetics 4) List 3 types of wound
A Current Look at Navicular Syndrome. Patrick First, DVM
 A Current Look at Navicular Syndrome Patrick First, DVM Navicular syndrome is a broad term that is used to describe soreness or damage to the navicular bone and its surrounding structures in the equine
A Current Look at Navicular Syndrome Patrick First, DVM Navicular syndrome is a broad term that is used to describe soreness or damage to the navicular bone and its surrounding structures in the equine
Washington State University Institutional Animal Care and Use Committee
 1 Standard Operating Procedure #9 Title: Minor Medical Treatment of Rodents Washington State University Institutional Animal Care and Use Committee Purpose: Currently, the Office of the Campus Veterinarian
1 Standard Operating Procedure #9 Title: Minor Medical Treatment of Rodents Washington State University Institutional Animal Care and Use Committee Purpose: Currently, the Office of the Campus Veterinarian
Model Infection Control Plan for Veterinary Practices, 2015
 Appendix 4: Model Infection Control Plan 2015 Model Infection Control Plan for Veterinary Practices, 2015 National Association of State Public Health Veterinarians (NASPHV) Veterinary Infection Control
Appendix 4: Model Infection Control Plan 2015 Model Infection Control Plan for Veterinary Practices, 2015 National Association of State Public Health Veterinarians (NASPHV) Veterinary Infection Control
Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma
 Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma Lucio Petrizzi DVM DECVS Università degli Studi di Teramo Surgical site infections (SSI) Microbial contamination unavoidable Infection
Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma Lucio Petrizzi DVM DECVS Università degli Studi di Teramo Surgical site infections (SSI) Microbial contamination unavoidable Infection
Prescription Label. Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long):
 Prescription Label Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long): Prescribing Veterinarian's Name & Contact Information: Refills: [Content to be provided
Prescription Label Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long): Prescribing Veterinarian's Name & Contact Information: Refills: [Content to be provided
Gynaecological Surgery in Adults Surgical Antibiotic Prophylaxis
 Gynaecological Surgery in Adults Surgical Antibiotic Prophylaxis Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date
Gynaecological Surgery in Adults Surgical Antibiotic Prophylaxis Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date
Package leaflet: Information for the user. GENTAMICIN VISION 3 mg/ml eye drops, solution Gentamicin
 Package leaflet: Information for the user GENTAMICIN VISION 3 mg/ml eye drops, solution Gentamicin Read all of this leaflet carefully before you start taking this medicine because it contains important
Package leaflet: Information for the user GENTAMICIN VISION 3 mg/ml eye drops, solution Gentamicin Read all of this leaflet carefully before you start taking this medicine because it contains important
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients.
 Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Veterinary Ophthalmology
 Veterinary Ophthalmology Eyelids Protect the eye Provides part of and spreads the tear film Regulates the amount of light that enters the eye Clears foreign material Third Eyelid Protects the cornea by
Veterinary Ophthalmology Eyelids Protect the eye Provides part of and spreads the tear film Regulates the amount of light that enters the eye Clears foreign material Third Eyelid Protects the cornea by
STANDARD OPERATING PROCEDURE #110 MOUSE ANESTHESIA
 STANDARD OPERATING PROCEDURE #110 MOUSE ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing mice. 2. RESPONSIBILITY Principal Investigators (PIs) and their
STANDARD OPERATING PROCEDURE #110 MOUSE ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing mice. 2. RESPONSIBILITY Principal Investigators (PIs) and their
SOP: Blood Collection in the Horse
 SOP: Blood Collection in the Horse These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during
SOP: Blood Collection in the Horse These SOPs were developed by the Office of the University Veterinarian and reviewed by Virginia Tech IACUC to provide a reference and guidance to investigators during
Antimicrobial Prophylaxis in the Surgical Patient. M. J. Osgood
 Antimicrobial Prophylaxis in the Surgical Patient M. J. Osgood Outline Definitions surgical site infection (SSI) Risk factors Wound classification Microbiology of SSIs Strategies for prevention of SSIs
Antimicrobial Prophylaxis in the Surgical Patient M. J. Osgood Outline Definitions surgical site infection (SSI) Risk factors Wound classification Microbiology of SSIs Strategies for prevention of SSIs
Discovery. DIFFERENTIAL DIAGNOSES Septic joint or tendon sheath Abscess Vascular damage Fracture Tendon or ligament damage
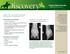 Discovery Applied Research for Today s Equine Athlete March 2012 Volume 3 Case File: Contrast-Enhanced Computed Tomography (CT) SIGNALMENT AND HISTORY 1-year-old Morgan colt January 1, 2011, Trooper was
Discovery Applied Research for Today s Equine Athlete March 2012 Volume 3 Case File: Contrast-Enhanced Computed Tomography (CT) SIGNALMENT AND HISTORY 1-year-old Morgan colt January 1, 2011, Trooper was
Rabies (Basic) Rabies is a deadly disease caused by a virus. It is the most serious zoonotic disease that you might encounter.
 This Chapter Covers: Introduction Animals That Contract Rabies Clinical Signs of Rabies Rabies Treatment Rabies Seasons and Cycles Animal Bites Rabies Quarantine Introduction Rabies is a deadly disease
This Chapter Covers: Introduction Animals That Contract Rabies Clinical Signs of Rabies Rabies Treatment Rabies Seasons and Cycles Animal Bites Rabies Quarantine Introduction Rabies is a deadly disease
STANDARD OPERATING PROCEDURE #111 RAT ANESTHESIA
 STANDARD OPERATING PROCEDURE #111 RAT ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing rats. 2. RESPONSIBILITY Principal Investigators (PIs) and their research
STANDARD OPERATING PROCEDURE #111 RAT ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing rats. 2. RESPONSIBILITY Principal Investigators (PIs) and their research
IN THE DAILY LIFE of a veterinarian or
 Administering Medication and Care IN THE DAILY LIFE of a veterinarian or veterinary technician, the majority of animal care involves administering medication to sick animals, giving vaccines for viruses,
Administering Medication and Care IN THE DAILY LIFE of a veterinarian or veterinary technician, the majority of animal care involves administering medication to sick animals, giving vaccines for viruses,
PRESCRIBING INFORMATION
 PRESCRIBING INFORMATION Pr PENTAMYCETIN Chloramphenicol Ophthalmic Solution USP 0.25%, 0.5% Chloramphenicol Ophthalmic Ointment USP 1% Antibiotic Pr PENTAMYCETIN/HC Chloramphenicol and Hydrocortisone Eye
PRESCRIBING INFORMATION Pr PENTAMYCETIN Chloramphenicol Ophthalmic Solution USP 0.25%, 0.5% Chloramphenicol Ophthalmic Ointment USP 1% Antibiotic Pr PENTAMYCETIN/HC Chloramphenicol and Hydrocortisone Eye
Standard Operating Procedure for Rabies. November Key facts
 Standard Operating Procedure for Rabies November 2011 Key facts Rabies occurs in more than 150 countries and territories. Dogs are the source of 99% of human rabies deaths. Worldwide, more than 55 000
Standard Operating Procedure for Rabies November 2011 Key facts Rabies occurs in more than 150 countries and territories. Dogs are the source of 99% of human rabies deaths. Worldwide, more than 55 000
Prescription Label. Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long):
 Prescription Label Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long): Prescribing Veterinarian's Name & Contact Information: Refills: [Content to be provided
Prescription Label Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long): Prescribing Veterinarian's Name & Contact Information: Refills: [Content to be provided
Wound types and healing part three: classification of injuries
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Wound types and healing part three: classification of injuries Author : Louise O Dwyer Categories : RVNs Date : July 1, 2010
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Wound types and healing part three: classification of injuries Author : Louise O Dwyer Categories : RVNs Date : July 1, 2010
Rabies spreads when an infected animal bites another animal or person, or if their saliva (spit) gets into a scratch or wound, eyes,
 Preventing Rabies What is rabies? Rabies is a very serious disease that affects the brain and spinal cord of mammals, such as cats, dogs, raccoons, coyotes, foxes, and occasionally people. Rabies is caused
Preventing Rabies What is rabies? Rabies is a very serious disease that affects the brain and spinal cord of mammals, such as cats, dogs, raccoons, coyotes, foxes, and occasionally people. Rabies is caused
Lameness Evaluation How to Spot It First Aid for Common Conditions When to Call the Vet. Ocean State Equine Associates
 Lameness Evaluation How to Spot It First Aid for Common Conditions When to Call the Vet Ocean State Equine Associates Lameness accounts for more losses in the equine industry than any other condition even
Lameness Evaluation How to Spot It First Aid for Common Conditions When to Call the Vet Ocean State Equine Associates Lameness accounts for more losses in the equine industry than any other condition even
Neurosurgery Antibiotic Prophylaxis Guideline
 Neurosurgery Antibiotic Prophylaxis Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version
Neurosurgery Antibiotic Prophylaxis Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version
NHS Dumfries And Galloway. Surgical Prophylaxis Guidelines
 NHS Dumfries And Galloway Surgical Prophylaxis Guidelines The aim of surgical prophylaxis is to reduce rates of surgical site and health-care associated infections and so reduce surgical morbidity and
NHS Dumfries And Galloway Surgical Prophylaxis Guidelines The aim of surgical prophylaxis is to reduce rates of surgical site and health-care associated infections and so reduce surgical morbidity and
ANIMALS AFFECTED WHAT IS RABIES? INCIDENCE AND DISTRIBUTION NEED TO KNOW INFORMATION FOR RABIES: AGRICULTURAL PRODUCERS
 Distributed by: Fact Sheet No. 19 Revised December 2013 THE AGRICULTURAL HEALTH & SAFETY NEED TO KNOW INFORMATION FOR RABIES: AGRICULTURAL PRODUCERS WHAT IS RABIES? Rabies is a disease caused by a virus
Distributed by: Fact Sheet No. 19 Revised December 2013 THE AGRICULTURAL HEALTH & SAFETY NEED TO KNOW INFORMATION FOR RABIES: AGRICULTURAL PRODUCERS WHAT IS RABIES? Rabies is a disease caused by a virus
DREXEL UNIVERSITY COLLEGE OF MEDICINE ANIMAL CARE AND USE COMMITTEE POLICY FOR PREOPERATIVE AND POSTOPERATIVE CARE FOR NON-RODENT MAMMALS
 DREXEL UNIVERSITY COLLEGE OF MEDICINE ANIMAL CARE AND USE COMMITTEE POLICY FOR PREOPERATIVE AND POSTOPERATIVE CARE FOR NON-RODENT MAMMALS OBJECTIVE: This policy is to ensure that appropriate provisions
DREXEL UNIVERSITY COLLEGE OF MEDICINE ANIMAL CARE AND USE COMMITTEE POLICY FOR PREOPERATIVE AND POSTOPERATIVE CARE FOR NON-RODENT MAMMALS OBJECTIVE: This policy is to ensure that appropriate provisions
RABIES CONTROL INTRODUCTION
 RABIES CONTROL INTRODUCTION Throughout human history, few illnesses have provoked as much anxiety as has rabies. Known as a distinct entity since at least 500 B.C., rabies has been the subject of myths
RABIES CONTROL INTRODUCTION Throughout human history, few illnesses have provoked as much anxiety as has rabies. Known as a distinct entity since at least 500 B.C., rabies has been the subject of myths
APPLICATION FOR LIVE ANIMAL USE IN TEACHING AT FAULKNER STATE COMMUNITY COLLEGE
 APPLICATION FOR LIVE ANIMAL USE IN TEACHING AT FAULKNER STATE COMMUNITY COLLEGE MARK WITH AN X IN THE BOX FOR ONE OF THE FOLLOWING AND TYPE YOUR CURRENT PROTOCOL NUMBER IF NEEDED: X New application Amendment
APPLICATION FOR LIVE ANIMAL USE IN TEACHING AT FAULKNER STATE COMMUNITY COLLEGE MARK WITH AN X IN THE BOX FOR ONE OF THE FOLLOWING AND TYPE YOUR CURRENT PROTOCOL NUMBER IF NEEDED: X New application Amendment
SPECIMEN COLLECTION FOR CULTURE OF BACTERIAL PATHOLOGENS QUICK REFERENCE
 1 Policy #: Subject: 611 (PLH-611-02) Effective Date: NA Reviewed Date: 2/1/2008 SPECIMEN COLLECTION FOR CULTURE OF BACTERIAL PATHOGENS QUICK REFERENCE Approved by: Laboratory Executive Director, Ed Hughes
1 Policy #: Subject: 611 (PLH-611-02) Effective Date: NA Reviewed Date: 2/1/2008 SPECIMEN COLLECTION FOR CULTURE OF BACTERIAL PATHOGENS QUICK REFERENCE Approved by: Laboratory Executive Director, Ed Hughes
FERAL CAT HOUSING AND HANDLING PROTOCOLS
 FERAL CAT HOUSING AND HANDLING PROTOCOLS For the safety of personnel and cats, the following protocols are to be used by all departments housing or caring for feral cats, semi-feral cats, or cats suspected
FERAL CAT HOUSING AND HANDLING PROTOCOLS For the safety of personnel and cats, the following protocols are to be used by all departments housing or caring for feral cats, semi-feral cats, or cats suspected
SURGICAL (SURVIVAL) OOCYTE COLLECTION FROM XENOUS LAEVIS
 UBC Animal Care Guidelines SOP: ACC 2013 01 Surgical Oocyte Collection from Xenopus Laevis Submitted by: Shelly McErlane Last Date Revised: Date Approved: January 28, 2013 SURGICAL (SURVIVAL) OOCYTE COLLECTION
UBC Animal Care Guidelines SOP: ACC 2013 01 Surgical Oocyte Collection from Xenopus Laevis Submitted by: Shelly McErlane Last Date Revised: Date Approved: January 28, 2013 SURGICAL (SURVIVAL) OOCYTE COLLECTION
Dry Eye Keratoconjunctivitis sicca (KCS)
 House Paws Home Veterinary Care (651) 283-7216 housepawsmn@gmail.com Dry Eye Keratoconjunctivitis sicca (KCS) Our veterinarian has diagnosed your dog with keratoconjunctivitis sicca (KCS), more simply
House Paws Home Veterinary Care (651) 283-7216 housepawsmn@gmail.com Dry Eye Keratoconjunctivitis sicca (KCS) Our veterinarian has diagnosed your dog with keratoconjunctivitis sicca (KCS), more simply
TRAINING BULLETIN #147
 TRAINING BULLETIN #147 COMBAT APPLICATION TOURNIQUET (C-A-T) I. Introduction The Combat Application Tourniquet (C-A-T) is a small, lightweight one-handed tourniquet that completely occludes arterial blood
TRAINING BULLETIN #147 COMBAT APPLICATION TOURNIQUET (C-A-T) I. Introduction The Combat Application Tourniquet (C-A-T) is a small, lightweight one-handed tourniquet that completely occludes arterial blood
Prescription Label. Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long):
 Prescription Label Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long): Prescribing Veterinarian's Name & Contact Information: Refills: [Content to be provided
Prescription Label Patient Name: Species: Drug Name & Strength: Directions (amount to give how often & for how long): Prescribing Veterinarian's Name & Contact Information: Refills: [Content to be provided
RabiesPostExposure Prophylaxis(PEP) GuidelinesforHuman HealthcareProviders
 RabiesPostExposure Prophylaxis(PEP) GuidelinesforHuman HealthcareProviders DC Department of Health Guidelines for Administering Rabies Post Exposure Prophylaxis (PEP): Human exposed to Domestic Animal
RabiesPostExposure Prophylaxis(PEP) GuidelinesforHuman HealthcareProviders DC Department of Health Guidelines for Administering Rabies Post Exposure Prophylaxis (PEP): Human exposed to Domestic Animal
Prince Edward Island Guidelines for the Management of Possible Rabies Exposure
 Prince Edward Island Guidelines for the Management of Possible Rabies Exposure October 2015 Table of Contents I INTRODUCTION... 3 II POST-EXPOSURE RABIES MANAGEMENT IN PEI... 4 III EPIDEMIOLOGY... 6 IV
Prince Edward Island Guidelines for the Management of Possible Rabies Exposure October 2015 Table of Contents I INTRODUCTION... 3 II POST-EXPOSURE RABIES MANAGEMENT IN PEI... 4 III EPIDEMIOLOGY... 6 IV
REPORT TO THE BOARDS OF HEALTH Jennifer Morse, M.D., Medical Director
 Ticks and Tick-borne illness REPORT TO THE BOARDS OF HEALTH Jennifer Morse, M.D., Medical Director District Health Department #10, Friday, May 19, 2017 Mid-Michigan District Health Department, Wednesday,
Ticks and Tick-borne illness REPORT TO THE BOARDS OF HEALTH Jennifer Morse, M.D., Medical Director District Health Department #10, Friday, May 19, 2017 Mid-Michigan District Health Department, Wednesday,
 Other vaccination recommendations will be determined on an individual basis after the risk assessment that reviews animal species, risk exposure, and personal health issues. The CMU consulting occupational
Other vaccination recommendations will be determined on an individual basis after the risk assessment that reviews animal species, risk exposure, and personal health issues. The CMU consulting occupational
Assuring Quality: A guide for youth livestock producers Activity for 2008
 Assuring Quality: A guide for youth livestock producers Activity for 2008 Daily Care and Management---Dairy Cow Activity 1: Proper Milking Procedures Resources Needed: Mud Bucket for water (ice cream pails
Assuring Quality: A guide for youth livestock producers Activity for 2008 Daily Care and Management---Dairy Cow Activity 1: Proper Milking Procedures Resources Needed: Mud Bucket for water (ice cream pails
Perioperative Care of Swine
 Swine are widely used in protocols that involve anesthesia and invasive surgical procedures. In order to ensure proper recovery of animals, preoperative, intraoperative and postoperative techniques specific
Swine are widely used in protocols that involve anesthesia and invasive surgical procedures. In order to ensure proper recovery of animals, preoperative, intraoperative and postoperative techniques specific
Animal, Plant & Soil Science
 Animal, Plant & Soil Science Lesson C5-9 Veterinary Terminology Interest Approach Gather some common veterinary tools (e.g., scissors, forceps, and scalpels). Ask the students what each item is and for
Animal, Plant & Soil Science Lesson C5-9 Veterinary Terminology Interest Approach Gather some common veterinary tools (e.g., scissors, forceps, and scalpels). Ask the students what each item is and for
Treatment Protocol. Diagnosis Clinical Signs Treatment Protocol and Dose Withdrawal. Period (slaughter)
 Treatment Protocol All IM injections given in the neck, with no me than 10 cc per site. Use 16 x 1 needles f IM injections; use 16 x ½ needles f SQ injections. Foot-rot Swelling above hooves (above both
Treatment Protocol All IM injections given in the neck, with no me than 10 cc per site. Use 16 x 1 needles f IM injections; use 16 x ½ needles f SQ injections. Foot-rot Swelling above hooves (above both
PACKAGE LEAFLET: INFORMATION FOR THE USER. GENTAMICIN VISION 3 mg/g eye ointment Gentamicin
 PACKAGE LEAFLET: INFORMATION FOR THE USER GENTAMICIN VISION 3 mg/g eye ointment Gentamicin Read all of this leaflet carefully before you start using this medicine. - Keep this leaflet. You may need to
PACKAGE LEAFLET: INFORMATION FOR THE USER GENTAMICIN VISION 3 mg/g eye ointment Gentamicin Read all of this leaflet carefully before you start using this medicine. - Keep this leaflet. You may need to
Examining and Medicating the Ears of Your Cat
 Examining and Medicating the Ears of Your Cat Source: Washington State University College of Veterinary Medicine https://www.vetmed.wsu.edu/outreach/pet Health Topics/categories/procedures/cats/examining
Examining and Medicating the Ears of Your Cat Source: Washington State University College of Veterinary Medicine https://www.vetmed.wsu.edu/outreach/pet Health Topics/categories/procedures/cats/examining
Mobility Issues and Arthritis
 Mobility Issues and Arthritis 1. Overview of end stage of the disease. Mobility issues are often attributed to normal aging by pet owners, and can have insidious symptoms as they may progress slowly without
Mobility Issues and Arthritis 1. Overview of end stage of the disease. Mobility issues are often attributed to normal aging by pet owners, and can have insidious symptoms as they may progress slowly without
March 2017 Animal Care Conference, Sacramento, CA
 Rabies Bats and Parvo Clusters: Helping the Community through Animal Disease Surveillance Emily Beeler DVM MPH, Veterinary Public Health Program, Los Angeles County Department of Public Health ebeeler@ph.lacounty.gov
Rabies Bats and Parvo Clusters: Helping the Community through Animal Disease Surveillance Emily Beeler DVM MPH, Veterinary Public Health Program, Los Angeles County Department of Public Health ebeeler@ph.lacounty.gov
acupressure for joint conditions
 The pet owner s guide to acupressure for joint conditions Dr Megan Kelly The pet owner s guide to acupressure for joint conditions onlinepethealth.com 1 Contents Introduction to acupressure 3 Acupressure
The pet owner s guide to acupressure for joint conditions Dr Megan Kelly The pet owner s guide to acupressure for joint conditions onlinepethealth.com 1 Contents Introduction to acupressure 3 Acupressure
Preparing for an AAALAC (and IACUC) Site Visit
 Preparing for an AAALAC (and IACUC) Site Visit Marcel Perret-Gentil, DVM, MS Neal Guentzel, PhD Updated 5/2013 About This Presentation Help you prepare for AAALAC site visit (as well as IACUC inspections)
Preparing for an AAALAC (and IACUC) Site Visit Marcel Perret-Gentil, DVM, MS Neal Guentzel, PhD Updated 5/2013 About This Presentation Help you prepare for AAALAC site visit (as well as IACUC inspections)
Stark County Rabies Prevention Information Manual
 Stark County Rabies Prevention Information Manual May 2012 Published by: Alliance City Health Department Canton City Health Department Massillon City Health Department Stark County Health Department Stark
Stark County Rabies Prevention Information Manual May 2012 Published by: Alliance City Health Department Canton City Health Department Massillon City Health Department Stark County Health Department Stark
Management of bite wounds and infection in primary care
 ANN T. KELLEHER, DO Dr. Kelleher has completed a fellowship in the Department of Infectious Disease at the Cleveland Clinic, and is a staff physician in the Department of Internal Medicine in the Cleveland
ANN T. KELLEHER, DO Dr. Kelleher has completed a fellowship in the Department of Infectious Disease at the Cleveland Clinic, and is a staff physician in the Department of Internal Medicine in the Cleveland
