In the past few decades, methicillin-resistant Staphylococcus aureus (MRSA) has
|
|
|
- Lynne Blankenship
- 6 years ago
- Views:
Transcription
1 The evolution of methicillin-resistant Staphylococcus aureus in Canadian hospitals: 5 years of national surveillance Research Recherche Andrew E. Simor, * Marianna Ofner-Agostini, Elizabeth Bryce, Karen Green, ** Allison McGeer, ** Michael Mulvey, Shirley Paton, and the Canadian Nosocomial Infection Surveillance Program, Health Canada Abstract Background: To better understand the epidemiology of methicillin-resistant Staphylococcus aureus (MRSA) in Canadian hospitals, surveillance has been conducted in sentinel hospitals across the country since We report the results of the first 5 years of the program. Methods: For each newly identified inpatient with MRSA, medical records were reviewed for demographic and clinical data. Isolates were subjected to susceptibility testing and molecular typing by pulsed-field gel electrophoresis. Results: A total of 4507 patients infected or colonized with MRSA were identified between January 1995 and December The rate of MRSA increased each year from a mean of 0.95 per 100 S. aureus isolates in 1995 to 5.97 per 100 isolates in 1999 (0.46 per 1000 admissions in 1995 to 4.12 per 1000 admissions in 1999) (p < 0.05). Most of the increase in MRSA occurred in Ontario, Quebec and the western provinces. Of the 3009 cases for which the site of MRSA acquisition could be determined, 86% were acquired in a hospital, 8% were acquired in a long-term care facility and 6% were acquired in the community. A total of 1603 patients (36%) were infected with MRSA. The most common sites of infection were skin or soft tissue (25% of MRSA infections), pulmonary tissues (24%) and surgical sites (23%); 13% of the patients were bacteremic. An epidemiologic link with a previously identified MRSA patient was suspected in 53% of the cases. Molecular typing indicated that most (81%) of the isolates could be classified as related to 1 of the 4 Canadian epidemic strains of MRSA. Interpretation: There has been a significant increase in the rate of isolating MRSA in many Canadian hospitals, related to the transmission of a relatively small number of MRSA strains. From the *Department of Microbiology, Sunnybrook and Women s College Health Sciences Centre, Toronto, Ont.; the Department of Laboratory Medicine and Pathobiology, University of Toronto, Toronto, Ont.; the Division of Nosocomial and Occupational Infections, Centre for Infectious Disease Prevention and Control, Health Canada, Ottawa, Ont.; the Department of Public Health Sciences, University of Toronto, Toronto, Ont., the Department of Pathology, Vancouver General Hospital, Vancouver, BC; the **Department of Microbiology, Mount Sinai Hospital, Toronto, Ont. This article has been peer reviewed. CMAJ 2001;165(1):21-6 ß See related article page 31 In the past few decades, methicillin-resistant Staphylococcus aureus (MRSA) has been recognized as an important nosocomial pathogen worldwide. 1 5 The emergence and rapid spread of this organism has created important new challenges for infection prevention and control services in hospitals and other health care facilities. Interestingly, there appears to be significant variability in the epidemiology and prevalence of MRSA in different parts of the world and even in different regions of a country. 3 MRSA was first reported in Canada in Since then, the organism has been identified in many Canadian health care facilities, 7 9 and one report has documented the rapid interprovincial spread of a single clone of MRSA. 10 Community-acquired MRSA has also been described, particularly for Aboriginal communities in the Prairie provinces. 11,12 However, nationwide data describing the incidence and epidemiology of MRSA in Canada were not available before In that year, national surveillance for MRSA was started in sentinel hospitals participating in the CMAJ JULY 10, 2001; 165 (1) Canadian Medical Association or its licensors
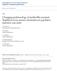
2 Simor et al Canadian Nosocomial Infection Surveillance Program (CNISP). Preliminary results of this surveillance have indicated a significant increase in the number of patients infected or colonized with MRSA in each of the past few years. 13,14 This report summarizes the results of the first 5 years of surveillance (1995 to 1999). The CNISP is a collaborative effort involving sentinel hospitals across the country, which participate as members of the Canadian Hospital Epidemiology Committee (a subcommittee of the Canadian Infectious Diseases Society), and the Centre for Infectious Disease Prevention and Control, Health Canada. Surveillance for MRSA started in January 1995 and is continuing. From 1995 to 1999 the number of participating sites increased from 22 to 34, with widespread geographic representation. Hospital sites in every province except Prince Edward Island participate in the surveillance. Most (30 [88%]) of the hospital sites are tertiary care teaching hospitals, representing 90% of the university-affiliated teaching medical centres in the country. Twelve hospitals are also affiliated with long-term care facilities, and 5 are pediatric hospitals. Methods Surveillance for MRSA was based on laboratory testing. When MRSA was isolated from an inpatient for the first time, the hospital s infection control practitioner reviewed the patient s medical records to obtain demographic and clinical information, including age, sex, prior admissions to hospital in the previous year, hospital service at the time the MRSA was first detected, and the reason for which the culture that yielded MRSA was obtained. All sites and tissues from which MRSA was isolated were recorded. The presence of infection caused by MRSA was determined according to standard definitions used in infection surveillance. 15 MRSA colonization was defined as the presence of MRSA without any clinical signs or symptoms of infection. An attempt was made to determine whether the MRSA had been acquired in a hospital, a long-term care facility or the community, according to the infection control practitioner s best judgement. For MRSA colonization or infection to be defined as having been acquired in hospital, there had to be no evidence that the organism was likely to have been present at the time of admission, or there had to be evidence that it was likely to have been acquired during a previous admission. For those cases in which colonization or infection was thought to have been acquired in hospital, an attempt was made to determine whether there was an epidemiologic link with any other known MRSA patients in the facility (e.g., roommate, patients who had undergone the same procedures as the affected patient, or health care workers). MRSA isolates were sent to a central laboratory, where the identity of the organism was confirmed according to standard procedures. Resistance to oxacillin was confirmed by growth on an oxacillin agar screening plate (Mueller-Hinton agar supplemented with 4% sodium chloride and oxacillin 6 µg/ml) incubated at 35 C for 24 hours. 16 Additional antimicrobial susceptibility testing was done by broth microdilution in accordance with the guidelines of the National Committee for Clinical Laboratory Standards. 16 All isolates were confirmed as MRSA by detection of the meca gene by polymerase chain reaction, as previously described. 17 Isolates were typed by pulsed-field gel electrophoresis after extraction of DNA and digestion of the extract with SmaI. Electrophoretically generated DNA profiles were digitized into the GelCompar computer software program for analysis. Cluster analysis was performed by the unweighted pair-group method on the basis of arithmetic averages, and DNA relatedness was calculated on the basis of the Dice coefficient. 18,19 Isolates were considered to be genetically related if their macrorestriction DNA patterns differed by fewer than 7 bands and the Dice coefficient of correlation was 75% or greater. 18,19 Categorical variables were compared with either the Fisher exact test or the χ 2 test. The extended Mantel-Haenszel χ 2 test for trend was used to determine changes in proportion over time. Differences for which p was less than 0.05 were considered statistically significant. Results During the 5 years of surveillance, a total of 4507 new patients with MRSA were identified in the participating hospitals. Of these, 36% (1603) were infected with MRSA. The mean incidence rate of MRSA increased in each of the surveillance years, rising from 0.46 cases per 1000 admissions in 1995 to 4.12 per 1000 admissions in 1999 (range of rates in participating hospitals over the surveillance period 0.1 to 16.3 per 1000 admissions) (p = 0.002) (Table 1). MRSA infection rates also increased, from 0.25 infections per 1000 admissions in 1995 to 1.11 infections per 1000 admissions in 1999 (p < 0.001). Most of the increase in MRSA cases occurred in Ontario and Quebec, although there was also a significant increase in the country s western provinces (Fig. 1). The rates increased from 0.6 to 6.5 per 1000 admissions in Ontario (p = 0.003) and from 0.2 to 4.9 per 1000 admissions in Quebec (p = 0.008). Overall, 59% (2667 of 4507) of the patients were male. The median age was 71 years (range less than 1 to 101 years). In 63% of cases (2797 of 4507), the patients were 65 years of age or older, whereas in only 4% (193 of 4507) were the patients less than 20 years of age. Patients 21 to 64 years of age were more likely to have had an MRSA infection than were those over 65 years of age (relative risk [RR] 2.7, 95% confidence interval [CI] ; p < 0.001); conversely, patients over 65 years of age were more likely to have been colonized without infection (RR 1.9, 95% CI ; p < 0.001). In 3% of cases (144) the patients were of Aboriginal origin; 105 (73%) of these people resided on reserves, particularly in the western provinces of Manitoba, Alberta, and British Columbia. In 1995, 71% (135) of the 191 cultures that eventually yielded MRSA were obtained for clinical indications (i.e., an infection was suspected), 20% (39) were obtained as part of MRSA screening or surveillance, and 9% (17) were obtained as part of outbreak investigation. However, by 1999, the initial culture yielding MRSA was obtained for a clinical indication in only 37% (718) of the 1939 cases (p < 0.001), whereas specimens were obtained for screening and 22 JAMC 10 JUILL. 2001; 165 (1)
3 Methicillin-resistant Staphylococcus aureus in Canadian hospitals outbreak investigation in 54% (1039) and 9% (182) of cases respectively. The most common sites from which MRSA was recovered in colonized and infected patients are summarized in Table 2. A determination of where the MRSA had been acquired was made in 78% of the cases (3515 of 4507) cases. MRSA was thought to have been acquired in hospital in 86% of these cases (3008 of 3515), in a long-term care facility in 8% (288) and in the community in 6% (219). Cases from Alberta and Manitoba were more likely to have been acquired in the community than were cases from other provinces (RR 4.9, 95% CI ; p < 0.001). Of the 3008 cases thought to have been acquired in hospital, 23% (692) were thought to have been acquired on a surgical service, 22% (662) on a medical service and 13% (391) in a critical care unit. Patients in a critical care unit were more likely to have had an MRSA infection (RR 1.5, 95% CI ; p < 0.001) than were patients elsewhere in the hospital. The proportion of hospital-acquired cases thought to have been acquired in the index hospital (i.e., the hospital that initially identified the patient with MRSA) was 86% (2587 of 3008). The rate of cases thought to have been acquired in the index hospital increased from 0.91 per 1000 admissions in 1997 to 2.81 per 1000 admissions in 1999 (p = 0.02). An epidemiologic link between the index case and another patient in the hospital was identified for slightly more than half (53%) of the hospital-acquired cases (1594 of 3008). In most of the epidemiologically linked cases (88%; 1403 of 1594), the identified link was a stay in the same hospital room or on the same nursing unit. An epidemiologic link was more likely to be identified in 1999 than in 1995 (960 of 1844 [52%] v. 76 of 187 [41%]; RR 1.6, 95% CI ; p < 0.001). Antimicrobial susceptibility testing of 2663 MRSA isolates from across the country revealed uniform resistance to the β-lactam antibiotics. Resistance rates for other antimicrobial agents were as follows: erythromycin and clindamycin, 94% each; ciprofloxacin, 89%; trimethoprim-sulfamethoxazole, 56%; tetracycline, 33%; rifampin, 3%; fusidic acid, 3%; and mupirocin, 2%. None of the isolates were found to have reduced susceptibility to vancomycin. Isolates recovered from patients in provinces west of Ontario were more likely to be resistant to tetracycline than were those recovered in Ontario, Quebec or the Atlantic provinces (72% v. 11%; p < 0.01). No other regional differences in susceptibility profiles were identified. There were also no temporal changes in antibiotic susceptibility profiles over the 5 years. A total of 1831 isolates, consisting of all of those from the period 1995 to 1997 and a subset of those from 1998 and 1999, were typed by pulsed-field gel electrophoresis. Fifty-six distinct DNA profiles were obtained. However, MRSA, no. per 1000 admissions Western Canada Ontario Quebec Eastern Canada Fig. 1: Rates of methicillin-resistant Staphylococcus aureus (number per 1000 admissions) in hospitals participating in the Canadian Nosocomial Infection Surveillance Program from 1995 to Table 1: Incidence of methicillin-resistant Staphylococcus aureus (MRSA) in sentinel Canadian hospitals, Year No. of patients with MRSA No. per 1000 admissions No. per patient-days No. per 100 S. aureus isolates All cases of MRSA* Overall MRSA infections Overall *Infections and colonizations. CMAJ JULY 10, 2001; 165 (1) 23
4 Simor et al most of the isolates (81%; 1483 of 1831) could be grouped into 1 of 4 epidemic strains of MRSA, which have previously been designated as Canadian epidemic strains (CMRSA-1, CMRSA-2, CMRSA-3 and CMRSA-4). 14 Each of these MRSA clones could be distinguished by its electrophoretic DNA profile and caused significant disease in patients from numerous hospital sites in 3 or more geographic regions of the country. CMRSA-1 was the most prevalent strain in Ontario, CMRSA-2 was the most prevalent strain in Quebec and CMRSA-3 was the most prevalent strain in provinces of western Canada. The DNA profiles were not associated with colonization or infection status, site of MRSA acquisition or antimicrobial susceptibility profile. Interpretation Since MRSA was first identified nearly 40 years ago, this organism has become prevalent in many countries around the world. However, for most of the past 2 decades, the epidemiology of MRSA in Canadian hospitals has been different from that described in the United States and many European countries. In the United States, for example, MRSA became endemic in many hospitals throughout the 1980s and early 1990s, with rates as high as 40% of all S. aureus isolates. 2 In contrast, until relatively recently, MRSA was not thought to be endemic in any Canadian health care facility. This study describes the results of a prospective nationwide surveillance program for MRSA in a large sample of Canadian hospitals. The results indicate a significant increase in MRSA rates in many parts of the country over the 5-year period 1995 to The largest increase occurred in hospitals in Ontario and British Columbia, but there have also been substantial increases in Alberta and Quebec. Part of this increase may be related to more frequent screening for asymptomatic MRSA in high-risk patients. 20 However, it is important to note that there has also been a fourfold increase in MRSA infection rates, in addition to the increase in identification of MRSA colonized patients. In this study most of the patients with MRSA were older Table 2: Sites of MRSA infection and colonization No. (and %) of cases* Site Infection Colonization Nose (43) Surgical site 431 (23) 168 (4) Other skin or soft tissue 474 (25) 1517 (34) Respiratory tract 454 (24) 467 (11) Urinary tract 177 (9) 254 (6) Bloodstream 250 (13) 0 Other 122 (6) 106 (2) *Some patients had MRSA at more than one site; each site of infection or colonization was counted as a separate case. Other sites of infection or colonization included catheter exit site (49 patients), intravascular catheter tip (49), conjunctiva (32), bone (9), cerebrospinal fluid (9) and pleural fluid (1). adults receiving care on medical or surgical units. Our surveillance was not designed to identify risk factors for MRSA acquisition, but risk factors that have previously been associated with acquisition of MRSA in hospitals have included prolonged stay, broad-spectrum antimicrobial therapy, admission to an intensive care unit, older age and proximity to other patients with MRSA Although there have been recent reports indicating an increase in community-acquired MRSA in the United States, 24,25 our data suggest that MRSA remains largely a hospital-acquired pathogen in Canada. Less than 15% of cases were thought to have been acquired outside of a hospital setting, and the rate of community-acquired MRSA did not change during the 5 years of surveillance (data not shown). Neither age nor infection or colonization status was associated with whether MRSA was nosocomial or acquired in the community (data not shown). However, cases from Manitoba and Alberta were more likely to have been acquired in the community than were cases from other provinces. Many of these patients were Aboriginals, which concurs with previously reported findings. 8,11,12 The frequent identification of an epidemiologic link between cases and the results of molecular typing by pulsedfield gel electrophoresis indicate that acquisition and transmission of MRSA were common occurrences in the participating hospitals. These surveillance results also indicate that MRSA has spread between institutions, with transmission of certain strains to several hospitals in geographically separate regions of the country. Such rapid, widespread dissemination within Canada of an epidemic strain of MRSA has previously been described. 10 However, in the absence of an outbreak, the spread of multiple clones of MRSA has been reported more often. 7,26 It is therefore remarkable that 81% of the Canadian MRSA isolates belonged to 1 of only 4 DNA types (designated Canadian epidemic MRSA strains). 14 It is not known what factors determine the ease of transmission of different strains of MRSA, but several phenotypic and genotypic properties have been associated with epidemic strains of MRSA. 27 Because a substantial number of hospitals participated in the surveillance and because most of the teaching medical centres in the country were represented, we believe that the results of this study are an accurate indication of MRSA in Canadian tertiary care hospitals. Moreover, the results obtained from Ontario CNISP hospitals are consistent with those from all Ontario hospitals, as reported by the province s Laboratory Proficiency Testing Program, 20 which indicates that CNISP results may also reflect the epidemiology of MRSA in many nonteaching hospitals in Canada. However, more broadly based surveillance with a representative sample of health care facilities would be necessary to obtain results that could be generalized to nonteaching hospitals in all regions of the country. Patients, physicians and hospital administrators should be concerned about increases in illness and death associated with MRSA, as well as the organism s impact on health care 24 JAMC 10 JUILL. 2001; 165 (1)
5 Methicillin-resistant Staphylococcus aureus in Canadian hospitals costs and the risks of emergence of further antibiotic resistance. MRSA strains are virulent and capable of causing serious disease. It has been reported that among hospital inpatients colonized with MRSA, 30% to 60% will eventually experience a significant MRSA infection, such as a wound infection, pneumonia or bacteremia. 22 In this surveillance project, slightly more than one-third of the patients had an MRSA infection, including 13% who were bacteremic. Several studies have documented that MRSA infections are associated with greater mortality rate and length of hospital stay, and that after adjustment for comorbidities methicillin resistance is a significant independent risk factor for death. 29,30 MRSA is typically resistant to multiple classes of antibiotics. Therefore, treatment options for the management of serious MRSA infections are limited. The current medication of choice is vancomycin. Higher rates of MRSA in Canadian health care facilities would lead to increased use of vancomycin, which is in turn associated with the emergence of vancomycin resistance in enterococci and MRSA Although S. aureus with reduced susceptibility to vancomycin has not yet been identified in Canada, it is likely just a matter of time before this occurs. Higher rates of MRSA and a concomitant increase in the use of vancomycin would promote earlier emergence of vancomycin resistance. The continued spread of MRSA in health care settings poses a serious risk to the health of patients. The associated costs of treating MRSA infections and of controlling outbreaks present an enormous burden on health care resources. Epidemic modelling has indicated that, if little is done now, MRSA rates will continue to rise exponentially in Canadian hospitals during the next 5 to 10 years. 36 The results of our study suggest an urgent need to implement better infection prevention and control measures to limit transmission of MRSA in hospital settings in Canada. Hospitals and countries that have implemented stringent infection control measures have been successful in limiting the spread of MRSA. 3,37,38 We believe there is currently an opportunity to effectively intervene and limit further spread of MRSA in Canadian health care facilities, but this opportunity will not exist indefinitely. Competing interests: None declared. Contributors: Dr. Simor participated in developing the initial study concept and design, supervised the conduct of the study, participated in data analysis and was the primary author of the manuscript. Ms. Ofner-Agostini participated in study design and data analysis and contributed to writing the manuscript. Dr. Bryce participated in study design and contributed to writing the manuscript. Ms. Green participated in study design and revision of the manuscript. Dr. McGeer participated in developing the initial study concept and design, participated in the conduct of the study and data analysis and contributed to writing the manuscript. Dr. Mulvey participated in the conduct of the study, reviewed the laboratory results and contributed to writing the manuscript. Ms. Paton participated in developing the initial study concept and design, helped to coordinate the conduct of the study and participated in analyzing the data and revising the manuscript. Acknowledgments: We thank the infection control practitioners and laboratory personnel of all the hospitals in the Canadian Nosocomial Infection Surveillance Program for their invaluable assistance in data collection. References 1. Townsend DE, Ashdown N, Bolton S, Bradley J, Duckworth G, Moorhouse EC, et al. The international spread of methicillin-resistant Staphylococcus aureus. J Hosp Infect 1987;9: Panlilio AL, Culver DH, Gaynes RP, Banerjee S, Henderson TS, Tolson JS, et al, and the National Nosocomial Infections Surveillance System. Methicillin-resistant Staphylococcus aureus in U.S. hospitals, Infect Control Hosp Epidemiol 1992;13: Voss A, Milatovic D, Wallrauch-Schwarz C, Rosdahl VT, Braveny I. Methicillin-resistant Staphylococcus aureus in Europe. Eur J Clin Microbiol Infect Dis 1994;13: Riley TV, Pearman JW, Rouse IL. Changing epidemiology of methicillin-resistant Staphylococcus aureus in Western Australia. Med J Aust 1995;163: Cox RA, Conquest C, Mallaghan C, Marples RR. A major outbreak of methicillin-resistant Staphylococcus aureus caused by a new phage-type (EMRSA-16). J Hosp Infect 1995;29: Low DE, Garcia M, Callery S, Milne P, Devlin HR, Campbell I, et al. Methicillin-resistant Staphylococcus aureus Ontario. Can Dis Wkly Rep 1981;7: Nicolle LE, Bialkowska-Hobrzanska H, Romance L, Harry VS, Parker S. Clonal diversity of methicillin-resistant Staphylococcus aureus in an acute-care institution. Infect Control Hosp Epidemiol 1992;13: Embil J, Ramotar K, Romance L, Alfa M, Conly J, Cronk S, et al. Methicillin-resistant Staphylococcus aureus in tertiary care institutions on the Canadian Prairies Infect Control Hosp Epidemiol 1994;15: Suh K, Toye B, Jessamine P, Chan F, Ramotar K. Epidemiology of methicillin-resistant Staphylococcus aureus in three Canadian tertiary-care centers. Infect Control Hosp Epidemiol 1998;19: Roman RS, Smith J, Walker M, Byrne S, Ramotar K, Dyck B, et al. Rapid geographic spread of a methicillin-resistant Staphylococcus aureus strain. Clin Infect Dis 1997;25: Dammann TA, Wiens RM, Taylor GD. Methicillin-resistant Staphylococcus aureus: identification of a community outbreak by monitoring of hospital isolates. Can J Public Health 1988;79: Taylor G, Kirkland T, Kowalewska-Grochowska K, Wang Y. A multistrain cluster of methicillin-resistant Staphylococcus aureus based in a native community. Can J Infect Dis 1990;1: Simor A, Ofner-Agostini M, Paton S, Canadian Nosocomial Infection Surveillance Program. The Canadian Nosocomial Infection Surveillance Program: results of the first 18 months of surveillance for methicillin-resistant Staphylococcus aureus in Canadian hospitals. Can Commun Dis Rep 1997;23: Simor AE, Boyd D, Louie L, McGeer A, Mulvey M, Willey BM, Canadian Hospital Epidemiology Committee, Canadian Nosocomial Infection Surveillance Program. Characterization and proposed nomenclature of epidemic strains of MRSA in Canada. Can J Infect Dis 1999;10: Garner JS, Jarvis WR, Emori TG, Horan TC, Hughes JM. CDC definitions for nosocomial infections, Am J Infect Control 1988;16: National Committee for Clinical Laboratory Standards. Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically [approved standard M7-A5]. 5th ed. Wayne (PA): The Committee; Murakami K, Minamide W, Wada K, Nakamura E, Teraoka H, Watanabe S. Identification of methicillin-resistant strains of staphylococci by polymerase chain reaction. J Clin Microbiol 1991;29: Bannerman TL, Hancock GA, Tenover FC, Miller JM. Pulsed-field gel electrophoresis as a replacement for bacteriophage typing of Staphylococcus aureus. J Clin Microbiol 1995;33: Tenover FC, Arbeit RD, Goering RV, Mickelsen PA, Murray BE, Persing DH, et al. Interpreting chromosomal DNA restriction patterns produced by pulsed-field gel electrophoresis: criteria for bacterial strain typing. J Clin Microbiol 1995;33: McGeer A, Saginur M, Green K, Fleming CA, Low DE. MRSA and VRE in Ontario Still room for optimism! Lab Proficiency Test Program Newslett 1999;258: Thompson RL, Cabezudo I, Wenzel RP. Epidemiology of nosocomial infections caused by methicillin-resistant Staphylococcus aureus. Ann Intern Med 1982;97: Boyce JM, Jackson MM, Pugliese G, Batt MD, Fleming D, Garner JS, et al. Methicillin-resistant Staphylococcus aureus (MRSA): a briefing for acute care hospitals and nursing facilities. Infect Control Hosp Epidemiol 1994;15: Monnet DL. Methicillin-resistant Staphylococcus aureus and its relationship to antimicrobial use: possible implications for control. Infect Control Hosp Epidemiol 1998;19: Herold BC, Immergluck LC, Maranan M, Lauderdale DS, Gaskin RE, Boyle- Vavra S, et al. Community-acquired methicillin-resistant Staphylococcus aureus in children with no identified predisposing risk. JAMA 1998;279: Gorak EJ, Yamada SM, Brown JD. Community-acquired methicillin-resistant Staphylococcus aureus in hospitalized adults and children without known risk factors. Clin Infect Dis 1999;29: Roberts RB, de Lencastre A, Eisner W, Severina EP, Shopsin B, Kreiswirth BN, et al. Molecular epidemiology of methicillin-resistant Staphylococcus aureus in 12 New York hospitals. J Infect Dis 1998;178: CMAJ JULY 10, 2001; 165 (1) 25
6 Simor et al 27. Papakyriacou H, Vaz D, Simor AE, Louie M, McGavin MJ. Molecular analysis of the accessory gene regulator (agr) locus and balance of virulence factor expression in epidemic methicillin-resistant Staphylococcus aureus. J Infect Dis 2000;181: Wakefield DS, Helms CM, Massanari RM, Mori M, Pfaller M. Cost of nosocomial infection: relative contributions of laboratory, antibiotic, and per diem costs in serious Staphylococcus aureus infections. Am J Infect Control 1988;16: Romero-Vivas J, Rubio M, Fernandez C, Picazo JJ. Mortality associated with nosocomial bacteremia due to methicillin-resistant Staphylococcus aureus. Clin Infect Dis 1995;21: Conterno LO, Wey SB, Castelo A. Risk factors for mortality in Staphylococcus aureus bacteremia. Infect Control Hosp Epidemiol 1998;19: Ibelings MMS, Bruining HA. Methicillin-resistant Staphylococcus aureus: acquisition and risk of death in patients in the intensive care unit. Eur J Surg 1998;164: Abramson MA, Sexton DJ. Nosocomial methicillin-resistant and methicillinsusceptible Staphylococcus aureus primary bacteremia: At what costs? Infect Control Hosp Epidemiol 1999;20: Murray BE. Vancomycin-resistant enterococcal infections. N Engl J Med 2000; 342: Hiramatsu K, Aritaka N, Hanaki H, Kawasaki S, Hosoda Y, Hori S, et al. Dissemination in Japanese hospitals of strains of Staphylococcus aureus heterogeneously resistant to vancomycin. Lancet 1997;350: Smith TL, Pearson ML, Wilcox KR, Cruz PHC, Lancaster MV, Robinson- Dunn B, et al. Emergence of vancomycin resistance in Staphylococcus aureus. N Engl J Med 1999;340: Ofner ME, Palmer RWH, Simor AE, Paton S, Canadian Hospital Epidemiology Committee. Epidemic modeling of methicillin-resistant Staphylococcus aureus infection in Canadian hospitals participating in the Canadian Nosocomial Infection Surveillance Program [abstract]. Infect Control Hosp Epidemiol 1999;20: Rosdahl VT, Knudesn AM. The decline of methicillin resistance among Danish Staphylococcus aureus strains. Infect Control Hosp Epidemiol 1991;12: Verhoef J, Beaujean D, Blok H, Baars A, Meyler A, van der Werken C, et al. A Dutch approach to methicillin-resistant Staphylococcus aureus. Eur J Clin Microbiol Infect Dis 1999;18: Correspondence to: Dr. Andrew E. Simor, Department of Microbiology, Sunnybrook and Women s College Health Sciences Centre, B Bayview Ave., North York ON M4N 3M5; fax ; andrew.simor@swchsc.on.ca Members of the Canadian Nosocomial Infection Surveillance Program (CNISP): Dr. Elizabeth Bryce, Vancouver General Hospital, Vancouver, BC; Dr. John Conly, University Health Network, Toronto, Ont.; Dr. John Embil, Health Sciences Centre, Winnipeg, Man.; Dr. Marie Gourdeau, Hôpital de l Enfant-Jésus, Quebec City, Que.; Ms. Karen Green, Community and Hospital Infection Control Association-Canada; Dr. Dan Gregson, St. Joseph s Health Centre, London, Ont.; Dr. Betty-Ann Henderson, Peter Lougheed Centre, Calgary, Alta.; Dr. James Hutchinson, Health Sciences Centre, St. John s, Nfld.; Dr. Magued Ishak, Centre hospitalier Angrignon, Verdun, Que.; Dr. Peter Jessamine, The Ottawa Hospital, Ottawa, Ont.; Dr. Lynne Johnston, Queen Elizabeth II Health Sciences Centre, Halifax, NS; Dr. Joanne Langley, I.W.K. Grace Health Science Centre, Halifax, NS; Dr. Mark Loeb, Hamilton Health Sciences Corp., Hamilton, Ont.; Dr. Anne Matlow, Hospital for Sick Children, Toronto, Ont.; Dr. Allison McGeer, Mount Sinai Hospital, Toronto, Ont.; Dr. Mark Miller, Jewish General Hospital, Montreal, Que.; Dr. Dorothy Moore, Montreal Children s Hospital, Montreal, Que.; Dr. Michael Mulvey, Canadian Science Centre for Human and Animal Health, Health Canada; Ms. Marianna Ofner-Agostini, Centre for Infectious Disease Prevention and Control, Health Canada; Ms. Shirley Paton, Centre for Infectious Disease Prevention and Control, Health Canada; Dr. Andrew Simor, Sunnybrook and Women s College Health Sciences Centre, Toronto, Ont.; Dr. Geoffrey Taylor, University of Alberta, Edmonton, Alta.; Dr. William Thompson, The Moncton Hospital, Moncton, NB; Dr. Mary Vearncombe, Sunnybrook and Women s College Health Sciences Centre, Toronto, Ont.; Dr. Alice Wong, Royal University Hospital, Saskatoon, Sask.; Dr. Dick Zoutman, Kingston General Hospital, Kingston, Ont. Essential reading in Canadian medicine The CMA s expanding family of medical journals offers new sources of reliable information to Canada s doctors. The coverage is current, the debate lively and the issues fascinating. Call us today to start your subscription! For information on a subscription package, call the Member Service Centre (outside Ottawa) (Ottawa and area) x2307 cmamsc@cma.ca Canadian Journal of Surgery Clinical and Investigative Medicine Journal of Psychiatry & Neuroscience Canadian Association of Radiologists Journal CJEM Canadian Journal of Rural Medicine Canadian Medical Association Journal 26 JAMC 10 JUILL. 2001; 165 (1)
Annual Report: Table 1. Antimicrobial Susceptibility Results for 2,488 Isolates of S. pneumoniae Collected Nationally, 2005 MIC (µg/ml)
 Streptococcus pneumoniae Annual Report: 5 In 5, a total of, isolates of pneumococci were collected from 59 clinical microbiology laboratories across Canada. Of these, 733 (9.5%) were isolated from blood
Streptococcus pneumoniae Annual Report: 5 In 5, a total of, isolates of pneumococci were collected from 59 clinical microbiology laboratories across Canada. Of these, 733 (9.5%) were isolated from blood
Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1
 Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Healthcare-associated Infections Annual Report
 September 2014 Healthcare-associated Infections Annual Report 2009-2013 Summary Provincial Infection Control Newfoundland Labrador (PIC-NL) has collected data on inpatients and outpatients with healthcare-associated
September 2014 Healthcare-associated Infections Annual Report 2009-2013 Summary Provincial Infection Control Newfoundland Labrador (PIC-NL) has collected data on inpatients and outpatients with healthcare-associated
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs?
 Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Tariq A. Madani, MD; Nabeela A. Al-Abdullah, RN; Ali A. Al-Sanousi, MD; Tawfik M. Ghabrah, MD; Shadia Z. Afandi, MD; Huda A. Bajunid, MD METHODS
 Vol. 22 No. 4 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY 211 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN TWO TERTIARY-CARE CENTERS IN JEDDAH, SAUDI ARABIA Tariq A. Madani, MD; Nabeela A. Al-Abdullah,
Vol. 22 No. 4 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY 211 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN TWO TERTIARY-CARE CENTERS IN JEDDAH, SAUDI ARABIA Tariq A. Madani, MD; Nabeela A. Al-Abdullah,
Healthcare-associated Infections Annual Report March 2015
 March 2015 Healthcare-associated Infections Annual Report 2009-2014 TABLE OF CONTENTS SUMMARY... 1 MRSA SURVEILLANCE RESULTS... 1 CDI SURVEILLANCE RESULTS... 1 INTRODUCTION... 2 METHICILLIN-RESISTANT
March 2015 Healthcare-associated Infections Annual Report 2009-2014 TABLE OF CONTENTS SUMMARY... 1 MRSA SURVEILLANCE RESULTS... 1 CDI SURVEILLANCE RESULTS... 1 INTRODUCTION... 2 METHICILLIN-RESISTANT
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update
 EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Methicillin-Resistant Staphylococcus aureus
 Methicillin-Resistant Staphylococcus aureus By Karla Givens Means of Transmission and Usual Reservoirs Staphylococcus aureus is part of normal flora and can be found on the skin and in the noses of one
Methicillin-Resistant Staphylococcus aureus By Karla Givens Means of Transmission and Usual Reservoirs Staphylococcus aureus is part of normal flora and can be found on the skin and in the noses of one
Consequences of Antimicrobial Resistant Bacteria. Antimicrobial Resistance. Molecular Genetics of Antimicrobial Resistance. Topics to be Covered
 Antimicrobial Resistance Consequences of Antimicrobial Resistant Bacteria Change in the approach to the administration of empiric antimicrobial therapy Increased number of hospitalizations Increased length
Antimicrobial Resistance Consequences of Antimicrobial Resistant Bacteria Change in the approach to the administration of empiric antimicrobial therapy Increased number of hospitalizations Increased length
MID 23. Antimicrobial Resistance. Consequences of Antimicrobial Resistant Bacteria. Molecular Genetics of Antimicrobial Resistance
 Antimicrobial Resistance Molecular Genetics of Antimicrobial Resistance Micro evolutionary change - point mutations Beta-lactamase mutation extends spectrum of the enzyme rpob gene (RNA polymerase) mutation
Antimicrobial Resistance Molecular Genetics of Antimicrobial Resistance Micro evolutionary change - point mutations Beta-lactamase mutation extends spectrum of the enzyme rpob gene (RNA polymerase) mutation
SUPPLEMENT ARTICLE. S114 CID 2001:32 (Suppl 2) Diekema et al.
 SUPPLEMENT ARTICLE Survey of Infections Due to Staphylococcus Species: Frequency of Occurrence and Antimicrobial Susceptibility of Isolates Collected in the United States, Canada, Latin America, Europe,
SUPPLEMENT ARTICLE Survey of Infections Due to Staphylococcus Species: Frequency of Occurrence and Antimicrobial Susceptibility of Isolates Collected in the United States, Canada, Latin America, Europe,
Brief Report THE DEVELOPMENT OF VANCOMYCIN RESISTANCE IN A PATIENT WITH METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS INFECTION
 Brief Report THE DEVELOPMENT OF VANCOMYCIN RESISTANCE IN A PATIENT WITH METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS INFECTION KRZYSZTOF SIERADZKI, PH.D., RICHARD B. ROBERTS, M.D., STUART W. HABER, M.D.,
Brief Report THE DEVELOPMENT OF VANCOMYCIN RESISTANCE IN A PATIENT WITH METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS INFECTION KRZYSZTOF SIERADZKI, PH.D., RICHARD B. ROBERTS, M.D., STUART W. HABER, M.D.,
Healthcare-associated infections surveillance report
 Healthcare-associated infections surveillance report Methicillin-resistant Staphylococcus aureus (MRSA) Update, Q4 2015/16 Summary Table Q4 2015/2016 Previous quarter (Q3 2015/16) Same quarter of previous
Healthcare-associated infections surveillance report Methicillin-resistant Staphylococcus aureus (MRSA) Update, Q4 2015/16 Summary Table Q4 2015/2016 Previous quarter (Q3 2015/16) Same quarter of previous
Antimicrobial Resistance
 Antimicrobial Resistance Consequences of Antimicrobial Resistant Bacteria Change in the approach to the administration of empiric antimicrobial therapy Increased number of hospitalizations Increased length
Antimicrobial Resistance Consequences of Antimicrobial Resistant Bacteria Change in the approach to the administration of empiric antimicrobial therapy Increased number of hospitalizations Increased length
Antimicrobial Resistance Acquisition of Foreign DNA
 Antimicrobial Resistance Acquisition of Foreign DNA Levy, Scientific American Horizontal gene transfer is common, even between Gram positive and negative bacteria Plasmid - transfer of single or multiple
Antimicrobial Resistance Acquisition of Foreign DNA Levy, Scientific American Horizontal gene transfer is common, even between Gram positive and negative bacteria Plasmid - transfer of single or multiple
Prevalence & Risk Factors For MRSA. For Vets
 For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
FM - Male, 38YO. MRSA nasal swab (+) Due to positive MRSA nasal swab test, patient will be continued on Vancomycin 1500mg IV q12 for MRSA treatment...
 Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Antimicrobial Stewardship Strategy: Antibiograms
 Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Healthcare-associated Infections Annual Report December 2018
 December 2018 Healthcare-associated Infections Annual Report 2011-2017 TABLE OF CONTENTS INTRODUCTION... 1 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS INFECTIONS... 2 MRSA SURVEILLANCE... 3 CLOSTRIDIUM
December 2018 Healthcare-associated Infections Annual Report 2011-2017 TABLE OF CONTENTS INTRODUCTION... 1 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS INFECTIONS... 2 MRSA SURVEILLANCE... 3 CLOSTRIDIUM
Healthcare-associated infections surveillance report
 Healthcare-associated infections surveillance report Methicillin-resistant Staphylococcus aureus (MRSA) Update, Q3 of 2017/18 Summary Table Q3 2017/18 Previous quarter (Q2 2017/18) Same quarter of previous
Healthcare-associated infections surveillance report Methicillin-resistant Staphylococcus aureus (MRSA) Update, Q3 of 2017/18 Summary Table Q3 2017/18 Previous quarter (Q2 2017/18) Same quarter of previous
Antibiotic usage in nosocomial infections in hospitals. Dr. Birgit Ross Hospital Hygiene University Hospital Essen
 Antibiotic usage in nosocomial infections in hospitals Dr. Birgit Ross Hospital Hygiene University Hospital Essen Infection control in healthcare settings - Isolation - Hand Hygiene - Environmental Hygiene
Antibiotic usage in nosocomial infections in hospitals Dr. Birgit Ross Hospital Hygiene University Hospital Essen Infection control in healthcare settings - Isolation - Hand Hygiene - Environmental Hygiene
Safe Patient Care Keeping our Residents Safe Use Standard Precautions for ALL Residents at ALL times
 Safe Patient Care Keeping our Residents Safe 2016 Use Standard Precautions for ALL Residents at ALL times #safepatientcare Do bugs need drugs? Dr Deirdre O Brien Consultant Microbiologist Mercy University
Safe Patient Care Keeping our Residents Safe 2016 Use Standard Precautions for ALL Residents at ALL times #safepatientcare Do bugs need drugs? Dr Deirdre O Brien Consultant Microbiologist Mercy University
CHAPTER 1 INTRODUCTION
 1 CHAPTER 1 INTRODUCTION The Staphylococci are a group of Gram-positive bacteria, 14 species are known to cause human infections but the vast majority of infections are caused by only three of them. They
1 CHAPTER 1 INTRODUCTION The Staphylococci are a group of Gram-positive bacteria, 14 species are known to cause human infections but the vast majority of infections are caused by only three of them. They
Failure of Cloxacillin in a Patient with BORSA Endocarditis ACCEPTED
 JCM Accepts, published online ahead of print on 30 December 2008 J. Clin. Microbiol. doi:10.1128/jcm.00571-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All
JCM Accepts, published online ahead of print on 30 December 2008 J. Clin. Microbiol. doi:10.1128/jcm.00571-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Clostridium difficile Surveillance Report 2016
 Clostridium difficile Surveillance Report 2016 EMERGING INFECTIONS PROGRAM Clostridium difficile Surveillance Report 2016 Minnesota Department of Health Emerging Infections Program PO Box 64882, St. Paul,
Clostridium difficile Surveillance Report 2016 EMERGING INFECTIONS PROGRAM Clostridium difficile Surveillance Report 2016 Minnesota Department of Health Emerging Infections Program PO Box 64882, St. Paul,
An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings?
 An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings? Dr. Andrew Morris Antimicrobial Stewardship ProgramMt. Sinai Hospital University Health Network amorris@mtsinai.on.ca andrew.morris@uhn.ca
An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings? Dr. Andrew Morris Antimicrobial Stewardship ProgramMt. Sinai Hospital University Health Network amorris@mtsinai.on.ca andrew.morris@uhn.ca
(Accepted 27 November 2009; first published online 22 January 2010)
 Epidemiol. Infect. (2010), 138, 730 737. f Crown Copyright. Published by Cambridge University Press 2010 doi:10.1017/s0950268809991488 A comparison of risk factors associated with community-associated
Epidemiol. Infect. (2010), 138, 730 737. f Crown Copyright. Published by Cambridge University Press 2010 doi:10.1017/s0950268809991488 A comparison of risk factors associated with community-associated
Decrease of vancomycin resistance in Enterococcus faecium from bloodstream infections in
 AAC Accepted Manuscript Posted Online 30 March 2015 Antimicrob. Agents Chemother. doi:10.1128/aac.00513-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 Decrease of vancomycin
AAC Accepted Manuscript Posted Online 30 March 2015 Antimicrob. Agents Chemother. doi:10.1128/aac.00513-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 Decrease of vancomycin
Antimicrobial Resistance and Molecular Epidemiology of Staphylococcus aureus in Ghana
 Antimicrobial Resistance and Molecular Epidemiology of Staphylococcus aureus in Ghana Beverly Egyir, PhD Noguchi Memorial Institute for Medical Research Bacteriology Department, University of Ghana Background
Antimicrobial Resistance and Molecular Epidemiology of Staphylococcus aureus in Ghana Beverly Egyir, PhD Noguchi Memorial Institute for Medical Research Bacteriology Department, University of Ghana Background
ORIGINAL ARTICLE. and 6 Institut für Mikrobiologie, Zürich, Switzerland. Epidemic, molecular typing, MRSA, sporadic
 ORIGINAL ARTICLE Molecular epidemiology of predominant clones and sporadic strains of methicillin resistant Staphylococcus aureus in Switzerland and comparison with European epidemic clones D. S. Blanc
ORIGINAL ARTICLE Molecular epidemiology of predominant clones and sporadic strains of methicillin resistant Staphylococcus aureus in Switzerland and comparison with European epidemic clones D. S. Blanc
Antimicrobial Resistance
 Antimicrobial Resistance Consequences of Antimicrobial Resistant Bacteria Change in the approach to the administration of Change in the approach to the administration of empiric antimicrobial therapy Increased
Antimicrobial Resistance Consequences of Antimicrobial Resistant Bacteria Change in the approach to the administration of Change in the approach to the administration of empiric antimicrobial therapy Increased
Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital
 Epidemiology J Microbiol Immunol of MRSA Infect. bacteremia 2007;40:310-316 Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital Chih-Yu
Epidemiology J Microbiol Immunol of MRSA Infect. bacteremia 2007;40:310-316 Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital Chih-Yu
Nosocomial Infections: What Are the Unmet Needs
 Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Burden of disease of antibiotic resistance The example of MRSA. Eva Melander Clinical Microbiology, Lund University Hospital
 Burden of disease of antibiotic resistance The example of MRSA Eva Melander Clinical Microbiology, Lund University Hospital Discovery of antibiotics Enormous medical gains Significantly reduced morbidity
Burden of disease of antibiotic resistance The example of MRSA Eva Melander Clinical Microbiology, Lund University Hospital Discovery of antibiotics Enormous medical gains Significantly reduced morbidity
03/09/2014. Infection Prevention and Control A Foundation Course. Talk outline
 Infection Prevention and Control A Foundation Course 2014 What is healthcare-associated infection (HCAI), antimicrobial resistance (AMR) and multi-drug resistant organisms (MDROs)? Why we should be worried?
Infection Prevention and Control A Foundation Course 2014 What is healthcare-associated infection (HCAI), antimicrobial resistance (AMR) and multi-drug resistant organisms (MDROs)? Why we should be worried?
3/1/2016. Antibiotics --When Less is More. Most Urgent Threats. Serious Threats
 Antibiotics --When Less is More Ralph Gonzales, MD, MSPH Associate Dean, Clinical Innovation School of Medicine VP, Clinical Innovation, UCSF Health Most Urgent Threats Serious Threats Multidrug-Resistant
Antibiotics --When Less is More Ralph Gonzales, MD, MSPH Associate Dean, Clinical Innovation School of Medicine VP, Clinical Innovation, UCSF Health Most Urgent Threats Serious Threats Multidrug-Resistant
Microbiological Surveillance of Methicillin Resistant Staphylococcus aureus (MRSA) in Belgian Hospitals in 2003
 Microbiological Surveillance of Methicillin Resistant Staphylococcus aureus (MRSA) in Belgian Hospitals in 3 Final report Olivier Denis and Marc J. Struelens Reference Laboratory for Staphylococci Department
Microbiological Surveillance of Methicillin Resistant Staphylococcus aureus (MRSA) in Belgian Hospitals in 3 Final report Olivier Denis and Marc J. Struelens Reference Laboratory for Staphylococci Department
Horizontal vs Vertical Infection Control Strategies
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL Chapter 14 Horizontal vs Vertical Infection Control Strategies Author Salma Abbas, MBBS Michael Stevens, MD, MPH Chapter Editor Shaheen Mehtar, MBBS. FRC Path,
GUIDE TO INFECTION CONTROL IN THE HOSPITAL Chapter 14 Horizontal vs Vertical Infection Control Strategies Author Salma Abbas, MBBS Michael Stevens, MD, MPH Chapter Editor Shaheen Mehtar, MBBS. FRC Path,
Reportable Disease Surveillance & Antibiotic Resistant Bacteria
 Reportable Disease Surveillance & Antibiotic Resistant Bacteria Kevin T. Kavanagh, MD, MS Health Watch USA December 16, 2015 This presentation is the express opinion of Kevin T. Kavanagh, MD, MS The Crisis
Reportable Disease Surveillance & Antibiotic Resistant Bacteria Kevin T. Kavanagh, MD, MS Health Watch USA December 16, 2015 This presentation is the express opinion of Kevin T. Kavanagh, MD, MS The Crisis
Optimal Use Report CADTH. Canadian Agency for Drugs and Technologies in Health. Agence canadienne des médicaments et des technologies de la santé
 Canadian Agency for Drugs and Technologies in Health Agence canadienne des médicaments et des technologies de la santé Optimal Use Report CADTH Volume 2, Issue 2A April 2012 Screening, Isolation, and Decolonization
Canadian Agency for Drugs and Technologies in Health Agence canadienne des médicaments et des technologies de la santé Optimal Use Report CADTH Volume 2, Issue 2A April 2012 Screening, Isolation, and Decolonization
Antimicrobial stewardship: Quick, don t just do something! Stand there!
 Antimicrobial stewardship: Quick, don t just do something! Stand there! Stanley I. Martin, MD, FACP, FIDSA Director, Division of Infectious Diseases Director, Antimicrobial Stewardship Program Geisinger
Antimicrobial stewardship: Quick, don t just do something! Stand there! Stanley I. Martin, MD, FACP, FIDSA Director, Division of Infectious Diseases Director, Antimicrobial Stewardship Program Geisinger
Epidemiology and Clinical Features of Methicillin-Resistant Staphylococcus Aureus (MRSA) at the University Hospital, Jeddah, Saudi Arabia
 Epidemiology J KAU: and Med. Clinical Sci., Vol. Features 10, pp. of 3-12 Methicillin-Resistant (1422 A.H. / 2002 Staphylococcus A.D.) aureus... 3 Epidemiology and Clinical Features of Methicillin-Resistant
Epidemiology J KAU: and Med. Clinical Sci., Vol. Features 10, pp. of 3-12 Methicillin-Resistant (1422 A.H. / 2002 Staphylococcus A.D.) aureus... 3 Epidemiology and Clinical Features of Methicillin-Resistant
Staphylococcus aureus Bacteremia: Comparison of Two Periods and a Predictive Model of Mortality
 288 BJID 2002; 6 (December) Staphylococcus aureus Bacteremia: Comparison of Two Periods and a Predictive Model of Mortality Lucieni de Oliveira Conterno, Sérgio Barsanti Wey and Adauto Castelo Division
288 BJID 2002; 6 (December) Staphylococcus aureus Bacteremia: Comparison of Two Periods and a Predictive Model of Mortality Lucieni de Oliveira Conterno, Sérgio Barsanti Wey and Adauto Castelo Division
Preventing Multi-Drug Resistant Organism (MDRO) Infections. For National Patient Safety Goal
 Preventing Multi-Drug Resistant Organism (MDRO) Infections For National Patient Safety Goal 07.03.01 2009 Methicillin Resistant Staphlococcus aureus (MRSA) About 3-8% of the population at large is a carrier
Preventing Multi-Drug Resistant Organism (MDRO) Infections For National Patient Safety Goal 07.03.01 2009 Methicillin Resistant Staphlococcus aureus (MRSA) About 3-8% of the population at large is a carrier
MRSA Outbreak in Firefighters
 MRSA Outbreak in Firefighters Angie Carranza Munger, MD Resident, Occupational and Environmental Medicine The University of Colorado, Denver and National Jewish Health Candidate, Masters of Public Health
MRSA Outbreak in Firefighters Angie Carranza Munger, MD Resident, Occupational and Environmental Medicine The University of Colorado, Denver and National Jewish Health Candidate, Masters of Public Health
Infection Control Manual Residential Care Part 3 Infection Control Standards IC7: 0100 Methicillin Resistant Staphylococcus aureus
 Infection Control Manual Residential Care Part 3 Infection Control Standards IC7: 0100 Methicillin Resistant Staphylococcus aureus IC7: 0100 MRSA 1. Purpose To outline the assessment, management, room
Infection Control Manual Residential Care Part 3 Infection Control Standards IC7: 0100 Methicillin Resistant Staphylococcus aureus IC7: 0100 MRSA 1. Purpose To outline the assessment, management, room
North West Neonatal Operational Delivery Network Working together to provide the highest standard of care for babies and families
 Document Title and Reference : Guideline for the management of multi-drug resistant organisms (MDRO) Main Author (s) Simon Power Ratified by: GM NSG Date Ratified: February 2012 Review Date: March 2017
Document Title and Reference : Guideline for the management of multi-drug resistant organisms (MDRO) Main Author (s) Simon Power Ratified by: GM NSG Date Ratified: February 2012 Review Date: March 2017
Overview of Nosocomial Infections Caused by Gram-Negative Bacilli
 HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor INVITED ARTICLE Overview of Nosocomial Infections Caused by Gram-Negative Bacilli Robert Gaynes, Jonathan R. Edwards, and the National Nosocomial
HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor INVITED ARTICLE Overview of Nosocomial Infections Caused by Gram-Negative Bacilli Robert Gaynes, Jonathan R. Edwards, and the National Nosocomial
MRSA in the Northwest Territories. Wanda White Manager of Health protection Unit Department of Health & Social Services March 23, 2012
 MRSA in the Northwest Territories Wanda White Manager of Health protection Unit Department of Health & Social Services March 23, 2012 Outbreak setting Northwest Territories Large, sparsely populated (43
MRSA in the Northwest Territories Wanda White Manager of Health protection Unit Department of Health & Social Services March 23, 2012 Outbreak setting Northwest Territories Large, sparsely populated (43
CANADIAN NOSOCOMIAL INFECTION SURVEILLANCE PROGRAM (CNISP): Summary Report of Healthcare Associated Infection (HAI), Antimicrobial Resistance (AMR)
 CANADIAN NOSOCOMIAL INFECTION SURVEILLANCE PROGRAM (CNISP): Summary Report of Healthcare Associated Infection (HAI), Antimicrobial Resistance (AMR) and Antimicrobial Use (AMU) Surveillance Data from January
CANADIAN NOSOCOMIAL INFECTION SURVEILLANCE PROGRAM (CNISP): Summary Report of Healthcare Associated Infection (HAI), Antimicrobial Resistance (AMR) and Antimicrobial Use (AMU) Surveillance Data from January
RESISTANCE OF STAPHYLOCOCCUS AUREUS TO VANCOMYCIN IN ZARQA, JORDAN
 RESISTANCE OF STAPHYLOCOCCUS AUREUS TO VANCOMYCIN IN ZARQA, JORDAN Hussein Azzam Bataineh 1 ABSTRACT Background: Vancomycin has been widely used in the treatment of infections caused by Methicillin-Resistant
RESISTANCE OF STAPHYLOCOCCUS AUREUS TO VANCOMYCIN IN ZARQA, JORDAN Hussein Azzam Bataineh 1 ABSTRACT Background: Vancomycin has been widely used in the treatment of infections caused by Methicillin-Resistant
Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives
 Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives John Jernigan, MD, MS Alex Kallen, MD, MPH Division of Healthcare Quality Promotion Centers for Disease
Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Activity C: ELC Prevention Collaboratives John Jernigan, MD, MS Alex Kallen, MD, MPH Division of Healthcare Quality Promotion Centers for Disease
Hong-Kai Wang 1, Chun-Yen Huang 1 and Yhu-Chering Huang 1,2*
 Wang et al. BMC Infectious Diseases (2017) 17:470 DOI 10.1186/s12879-017-2560-0 RESEARCH ARTICLE Open Access Clinical features and molecular characteristics of childhood communityassociated methicillin-resistant
Wang et al. BMC Infectious Diseases (2017) 17:470 DOI 10.1186/s12879-017-2560-0 RESEARCH ARTICLE Open Access Clinical features and molecular characteristics of childhood communityassociated methicillin-resistant
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN U.S. HOSPITALS,
 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN U.S. HOSPITALS, 1975-1991 Adelisa L. Panlilio, MD, MPH; David H. Culver, PhD; Robert P. Gaynes, MD; Shailen Banerjee, PhD; Tonya S. Henderson, BS; James S.
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN U.S. HOSPITALS, 1975-1991 Adelisa L. Panlilio, MD, MPH; David H. Culver, PhD; Robert P. Gaynes, MD; Shailen Banerjee, PhD; Tonya S. Henderson, BS; James S.
Success for a MRSA Reduction Program: Role of Surveillance and Testing
 Success for a MRSA Reduction Program: Role of Surveillance and Testing Singapore July 13, 2009 Lance R. Peterson, MD Director of Microbiology and Infectious Disease Research Associate Epidemiologist, NorthShore
Success for a MRSA Reduction Program: Role of Surveillance and Testing Singapore July 13, 2009 Lance R. Peterson, MD Director of Microbiology and Infectious Disease Research Associate Epidemiologist, NorthShore
MRSA surveillance 2014: Poultry
 Vicky Jasson MRSA surveillance 2014: Poultry 1. Introduction In the framework of the FASFC surveillance, a surveillance of MRSA in poultry has been executed in order to determine the prevalence and diversity
Vicky Jasson MRSA surveillance 2014: Poultry 1. Introduction In the framework of the FASFC surveillance, a surveillance of MRSA in poultry has been executed in order to determine the prevalence and diversity
Detection and Quantitation of the Etiologic Agents of Ventilator Associated Pneumonia in Endotracheal Tube Aspirates From Patients in Iran
 Letter to the Editor Detection and Quantitation of the Etiologic Agents of Ventilator Associated Pneumonia in Endotracheal Tube Aspirates From Patients in Iran Mohammad Rahbar, PhD; Massoud Hajia, PhD
Letter to the Editor Detection and Quantitation of the Etiologic Agents of Ventilator Associated Pneumonia in Endotracheal Tube Aspirates From Patients in Iran Mohammad Rahbar, PhD; Massoud Hajia, PhD
Ca-MRSA Update- Hand Infections. Washington Hand Society September 19, 2007
 Ca-MRSA Update- Hand Infections Washington Hand Society September 19, 2007 Resistant Staph. Aureus Late 1940 s -50% S.Aureus resistant to PCN 1957-80/81 strain- of S.A. highly virulent and easily transmissible
Ca-MRSA Update- Hand Infections Washington Hand Society September 19, 2007 Resistant Staph. Aureus Late 1940 s -50% S.Aureus resistant to PCN 1957-80/81 strain- of S.A. highly virulent and easily transmissible
Hosted by Dr. Jon Otter, Guys & St. Thomas Hospital, King s College, London A Webber Training Teleclass 1
 Andreas Voss, MD, PhD Professor of Infection Control Radboud University Nijmegen Medical Centre & Canisius-Wilhelmina Hospital Nijmegen, Netherlands Hosted by Dr. Jon O0er Guys & St. Thomas NHS Founda
Andreas Voss, MD, PhD Professor of Infection Control Radboud University Nijmegen Medical Centre & Canisius-Wilhelmina Hospital Nijmegen, Netherlands Hosted by Dr. Jon O0er Guys & St. Thomas NHS Founda
original article Prevalence of antimicrobial use in a network of Canadian hospitals in 2002 and 2009
 Prevalence of antimicrobial use in a network of Canadian hospitals in 2002 and 2009 Geoffrey Taylor MD 1, Denise Gravel MSc 2, Lynora Saxinger MD 1, Kathryn Bush MSc 3, Kimberley Simmonds MSc 4, Anne Matlow
Prevalence of antimicrobial use in a network of Canadian hospitals in 2002 and 2009 Geoffrey Taylor MD 1, Denise Gravel MSc 2, Lynora Saxinger MD 1, Kathryn Bush MSc 3, Kimberley Simmonds MSc 4, Anne Matlow
Evaluation of a computerized antimicrobial susceptibility system with bacteria isolated from animals
 J Vet Diagn Invest :164 168 (1998) Evaluation of a computerized antimicrobial susceptibility system with bacteria isolated from animals Susannah K. Hubert, Phouc Dinh Nguyen, Robert D. Walker Abstract.
J Vet Diagn Invest :164 168 (1998) Evaluation of a computerized antimicrobial susceptibility system with bacteria isolated from animals Susannah K. Hubert, Phouc Dinh Nguyen, Robert D. Walker Abstract.
During the second half of the 19th century many operations were developed after anesthesia
 Continuing Education Column Surgical Site Infection and Surveillance Tae Jin Lim, MD Department of Surgery, Keimyung University College of Medicine E mail : tjlim@dsmc.or.kr J Korean Med Assoc 2007; 50(10):
Continuing Education Column Surgical Site Infection and Surveillance Tae Jin Lim, MD Department of Surgery, Keimyung University College of Medicine E mail : tjlim@dsmc.or.kr J Korean Med Assoc 2007; 50(10):
IDSA GUIDELINES COMMUNITY ACQUIRED PNEUMONIA
 page 1 / 5 page 2 / 5 idsa guidelines community acquired pdf IDSA/ATS Guidelines for CAP in Adults CID 2007:44 (Suppl 2) S29 such as blood and sputum cultures. Conversely, these cultures may have a major
page 1 / 5 page 2 / 5 idsa guidelines community acquired pdf IDSA/ATS Guidelines for CAP in Adults CID 2007:44 (Suppl 2) S29 such as blood and sputum cultures. Conversely, these cultures may have a major
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016
 Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Int.J.Curr.Microbiol.App.Sci (2018) 7(8):
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 08 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.708.378
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 08 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.708.378
Concise Antibiogram Toolkit Background
 Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Antimicrobial Stewardship. October 2012
 Antimicrobial Stewardship October 2012 Rising Antimicrobial Resistance Methicillin resistant staphylococcus aureus (MRSA) Vancomycin resistant enterococci (VRE) MDR and extremely drug resistant (XDR TB)
Antimicrobial Stewardship October 2012 Rising Antimicrobial Resistance Methicillin resistant staphylococcus aureus (MRSA) Vancomycin resistant enterococci (VRE) MDR and extremely drug resistant (XDR TB)
Antimicrobial Resistance Trends in the Province of British Columbia. August Epidemiology Services British Columbia Centre for Disease Control
 Antimicrobial Resistance Trends in the Province of British Columbia August 2008 Epidemiology Services British Columbia Centre for Disease Control 5 Table of Contents Executive Summary...5 Objective...6
Antimicrobial Resistance Trends in the Province of British Columbia August 2008 Epidemiology Services British Columbia Centre for Disease Control 5 Table of Contents Executive Summary...5 Objective...6
The importance of infection control in the era of multi drug resistance
 Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
Dr. Kumar Consultant Infectious Diseases Physician Hospital Sungai buloh The importance of infection control in the era of multi drug resistance Nosocomial infections In Australian acute hospitals 200,000
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE FOR HEALTHCARE ACQUIRED CEREBROSPINAL FLUID SHUNT ASSOCIATED INFECTIONS
 Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE FOR HEALTHCARE ACQUIRED CEREBROSPINAL FLUID SHUNT ASSOCIATED INFECTIONS FINAL November 29, 2017 Working Group: Joanne Langley (Chair),
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE FOR HEALTHCARE ACQUIRED CEREBROSPINAL FLUID SHUNT ASSOCIATED INFECTIONS FINAL November 29, 2017 Working Group: Joanne Langley (Chair),
Epidemiology and Susceptibility of 3,051 Staphylococcus aureus Isolates from 25 University Hospitals Participating in the European SENTRY Study
 JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2001, p. 3727 3732 Vol. 39, No. 10 0095-1137/01/$04.00 0 DOI: 10.1128/JCM.39.10.3727 3732.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2001, p. 3727 3732 Vol. 39, No. 10 0095-1137/01/$04.00 0 DOI: 10.1128/JCM.39.10.3727 3732.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved.
Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care units
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
Preventing Clostridium difficile Infection (CDI)
 1 Preventing Clostridium difficile Infection (CDI) All Hands on Deck to Reduce CDI Skill Nursing Facility Conference July 28, 2017 Idamae Kennedy, MPH,BSN,RN,CIC Liaison Infection Preventionist Healthcare
1 Preventing Clostridium difficile Infection (CDI) All Hands on Deck to Reduce CDI Skill Nursing Facility Conference July 28, 2017 Idamae Kennedy, MPH,BSN,RN,CIC Liaison Infection Preventionist Healthcare
Why should we care about multi-resistant bacteria? Clinical impact and
 Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
Multi-Drug Resistant Gram Negative Organisms POLICY REVIEW DATE EXTENDED Printed copies must not be considered the definitive version
 Multi-Drug Resistant Gram Negative Organisms POLICY REVIEW DATE EXTENDED 2018 Printed copies must not be considered the definitive version DOCUMENT CONTROL POLICY NO. IC-122 Policy Group Infection Control
Multi-Drug Resistant Gram Negative Organisms POLICY REVIEW DATE EXTENDED 2018 Printed copies must not be considered the definitive version DOCUMENT CONTROL POLICY NO. IC-122 Policy Group Infection Control
Please distribute a copy of this information to each provider in your organization.
 HEALTH ADVISORY TO: Physicians and other Healthcare Providers Please distribute a copy of this information to each provider in your organization. Questions regarding this information may be directed to
HEALTH ADVISORY TO: Physicians and other Healthcare Providers Please distribute a copy of this information to each provider in your organization. Questions regarding this information may be directed to
Staphylococcus aureus
 Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins
 Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Antimicrobial Cycling. Donald E Low University of Toronto
 Antimicrobial Cycling Donald E Low University of Toronto Bad Bugs, No Drugs 1 The Antimicrobial Availability Task Force of the IDSA 1 identified as particularly problematic pathogens A. baumannii and
Antimicrobial Cycling Donald E Low University of Toronto Bad Bugs, No Drugs 1 The Antimicrobial Availability Task Force of the IDSA 1 identified as particularly problematic pathogens A. baumannii and
Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2008
 Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2008 Each year ESR conducts a one-month survey of methicillin-resistant Staphylococcus aureus (MRSA) to provide ongoing information
Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2008 Each year ESR conducts a one-month survey of methicillin-resistant Staphylococcus aureus (MRSA) to provide ongoing information
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Prevalence of MRSA, VRE and C. difficile among Adults Hospitalized in Canadian Hospitals
 Prevalence of MRSA, VRE and C. difficile among Adults Hospitalized in Canadian Hospitals Background The emergence of antibiotic-resistant organisms is a major public health concern, particularly in hospitals
Prevalence of MRSA, VRE and C. difficile among Adults Hospitalized in Canadian Hospitals Background The emergence of antibiotic-resistant organisms is a major public health concern, particularly in hospitals
MDRO in LTCF: Forming Networks to Control the Problem
 MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
MDRO in LTCF: Forming Networks to Control the Problem Suzanne F. Bradley, M.D. Professor of Internal Medicine Division of Infectious Disease University of Michigan Medical School VA Ann Arbor Healthcare
Florida Health Care Association District 2 January 13, 2015 A.C. Burke, MA, CIC
 Florida Health Care Association District 2 January 13, 2015 A.C. Burke, MA, CIC 11/20/2014 1 To describe carbapenem-resistant Enterobacteriaceae. To identify laboratory detection standards for carbapenem-resistant
Florida Health Care Association District 2 January 13, 2015 A.C. Burke, MA, CIC 11/20/2014 1 To describe carbapenem-resistant Enterobacteriaceae. To identify laboratory detection standards for carbapenem-resistant
Suspected transmission of methicillin-resistant Staphylococcus aureus between domestic pets and humans in veterinary clinics and in the household
 Veterinary Microbiology 115 (2006) 148 155 www.elsevier.com/locate/vetmic Suspected transmission of methicillin-resistant Staphylococcus aureus between domestic pets and humans in veterinary clinics and
Veterinary Microbiology 115 (2006) 148 155 www.elsevier.com/locate/vetmic Suspected transmission of methicillin-resistant Staphylococcus aureus between domestic pets and humans in veterinary clinics and
Bacterial whole genome sequencing in clinical microbiology, infection control and public health. Julian Parkhill. FIS, Birmingham, November 2013
 Bacterial whole genome sequencing in clinical microbiology, infection control and public health Julian Parkhill FIS, Birmingham, November 2013 Falling costs of genomics 2003 Cost/genome Throughput 60,000
Bacterial whole genome sequencing in clinical microbiology, infection control and public health Julian Parkhill FIS, Birmingham, November 2013 Falling costs of genomics 2003 Cost/genome Throughput 60,000
Antibiotic Stewardship in the Hospital Setting
 Antibiotic Stewardship in the Hospital Setting G. Evans, MD FRCPC Medical Director, Infection Prevention & Control Kingston General Hospital & Hotel Dieu Hospital EOPIC September 26, 2012 Stewardship stew-ard-ship
Antibiotic Stewardship in the Hospital Setting G. Evans, MD FRCPC Medical Director, Infection Prevention & Control Kingston General Hospital & Hotel Dieu Hospital EOPIC September 26, 2012 Stewardship stew-ard-ship
European Antimicrobial Resistance Surveillance System (EARSS) in Scotland: 2004
 European Antimicrobial Resistance Surveillance System (EARSS) in Scotland: 2004 SECOND ANNUAL REPORT MJ Coyne 1, SJ Dancer 1, G Edwards 2, 3, D Morrison 2. 1 Health Protection Scotland, 2 Scottish MRSA
European Antimicrobial Resistance Surveillance System (EARSS) in Scotland: 2004 SECOND ANNUAL REPORT MJ Coyne 1, SJ Dancer 1, G Edwards 2, 3, D Morrison 2. 1 Health Protection Scotland, 2 Scottish MRSA
Tel: Fax:
 CONCISE COMMUNICATION Bactericidal activity and synergy studies of BAL,a novel pyrrolidinone--ylidenemethyl cephem,tested against streptococci, enterococci and methicillin-resistant staphylococci L. M.
CONCISE COMMUNICATION Bactericidal activity and synergy studies of BAL,a novel pyrrolidinone--ylidenemethyl cephem,tested against streptococci, enterococci and methicillin-resistant staphylococci L. M.
Barriers to Intravenous Penicillin Use for Treatment of Nonmeningitis
 JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
1/30/ Division of Disease Control and Health Protection. Division of Disease Control and Health Protection
 Surveillance, Outbreaks, and Reportable Diseases, Oh My! Assisted Living Facility, Nursing Home and Surveyor Infection Prevention Training February 2015 A.C. Burke, MA, CIC Health Care-Associated Infection
Surveillance, Outbreaks, and Reportable Diseases, Oh My! Assisted Living Facility, Nursing Home and Surveyor Infection Prevention Training February 2015 A.C. Burke, MA, CIC Health Care-Associated Infection
Approval Signature: Original signed by Dr. Michel Tetreault Date of Approval: July Review Date: July 2017
 WRHA Infection Prevention and Control Program Operational Directives Admission Screening for Antibiotic Resistant Organisms (AROs): Methicillin Resistant Staphylococcus aureus (MRSA) and Vancomycin Resistant
WRHA Infection Prevention and Control Program Operational Directives Admission Screening for Antibiotic Resistant Organisms (AROs): Methicillin Resistant Staphylococcus aureus (MRSA) and Vancomycin Resistant
Get Smart For Healthcare
 Get Smart For Healthcare Know When Antibiotics Work Marry Bardin, Quality Improvement Advisor June 9, 2015 Why We Need to Improve In-patient Antibiotic Use Antibiotics are misused in hospitals Antibiotic
Get Smart For Healthcare Know When Antibiotics Work Marry Bardin, Quality Improvement Advisor June 9, 2015 Why We Need to Improve In-patient Antibiotic Use Antibiotics are misused in hospitals Antibiotic
