Comparison of Gentamicin and Mupirocin in the Prevention of Exit-Site Infection and Peritonitis in Peritoneal Dialysis
|
|
|
- Shanna Freeman
- 6 years ago
- Views:
Transcription
1 Advances in Peritoneal Dialysis, Vol. 25, 2009 Anshinee Mahaldar, Michael Weisz, Pranay Kathuria Comparison of Gentamicin and Mupirocin in the Prevention of Exit-Site Infection and Peritonitis in Peritoneal Dialysis Exit-site infection (ESI) and peritonitis are the most frequent reasons for catheter removal and patient drop-out from peritoneal dialysis (PD). After a randomized double-blind study showed gentamicin to be superior to mupirocin for exit-site prophylaxis, several dialysis centers including ours switched from topical mupirocin to gentamicin. Our study examined whether the change from mupirocin to gentamicin affected ESI and peritonitis rates. We retrospectively reviewed consecutive charts of patients seen at our PD clinic between January 2003 and December We noted the rates of ESI and peritonitis in patients who met the study entry criteria. Chart data for the 100 patients that met study entry criteria were evaluated in depth. The ESI rate was episodes/patient month in the gentamicin and episodes/patient month in the mupirocin (p = 0.45). The peritonitis rate was 0.06 episodes/patient month in the gentamicin and 0.02 episodes/patient month in the mupirocin (p = 0.07). The rate of gram-positive peritonitis was 0.05 episodes/ patient month in the gentamicin and 0.01 episodes/patient month in the mupirocin (p = 0.08). The rate of gram-negative peritonitis was episodes/patient month in the gentamicin and episodes/patient month in the mupirocin (p = 0.83). We observed no statistically significant difference in the rates of ESI between patients using mupirocin and those using gentamicin for exit-site prophylaxis. Both s had a very low ESI rate. A trend toward higher peritonitis rates was noted From: Department of Internal Medicine, University of Oklahoma College of Medicine, Tulsa, Oklahoma, U.S.A. in the gentamicin, largely as a result of grampositive bacteria (p value nonsignificant). Key words Exit-site infection, peritonitis, mupirocin, gentamicin Introduction Infection-related complications such as exit-site infection (ESI) and peritonitis remain the most frequent reasons for catheter removal and patient drop-out from peritoneal dialysis (PD) (1). Prevention of catheter-related infections is the primary goal of exitsite care (2). Topical antibiotics are used to prevent catheter-related infections, which are commonly caused by Staphylococcus aureus, Pseudomonas aeruginosa, and coagulase-negative Staphylococcus (CoNS) (3 5). Multiple studies have shown that mupirocin reduces the risk of S. aureus ESIs and peritonitis (6 10). The application of mupirocin at the exit site has therefore become the standard of care to prevent catheter-related infections (2). Mupirocin, however, is not active against gram-negative organisms (9,11). In 2005, Bernardini et al. (11) reported the results of a randomized double-blind study comparing mupirocin with gentamicin for exit-site prophylaxis. Use of gentamicin reduced the occurrence of ESIs and peritonitis caused by P. aeruginosa and other gram-negative organisms; at the same time, gentamicin was as effective as mupirocin in preventing S. aureus infections. In 2005, based on the results of the Bernardini study, our PD clinic switched from mupirocin to gentamicin for topical exit-site prophylaxis. Our aim in the present study was to determine if the incidence of ESIs and peritonitis in our PD center changed after the switch from mupirocin to gentamicin.
2 Gentamicin and Mupirocin in ESI 57 Methods Our study was conducted in the PD unit at a tertiarycare hospital in Oklahoma. The electronic health records of patients seen in the PD clinic were retrospectively reviewed for study eligibility. Eligible charts were those with encounters involving adult patients 18 years and older on PD from January 2003 to December 2007 who were using topical mupirocin or gentamicin and who had at least 6 months of follow-up data. From the 100 patient charts that met the eligibility criteria, we recorded all infection data from 3 months after catheter insertion (to allow for healing and to exclude surgical factors in an ESI). All patients received surgically placed Kendall single-cuff silicon catheters and standard exit-site care. Patients on continuous ambulatory PD were using the twin-bag system. We defined ESI as the presence of two of the following manifestations: purulent or bloody drainage (or both) from the exit site; swelling surrounding the sinus; or erythema surrounding the sinus. When a diagnosis of ESI was charted, we included the ESI in our analysis only if the documented physical examination met our definition. We defined peritonitis as the presence of cloudy dialysate or abdominal pain (or both), with 100 or more white blood cells per milliliter of dialysate, 50% or more being polymorphonuclear cells. We noted the prophylaxis regimen of the patients, rates of ESI and peritonitis, and the organisms causing the infections. Infection rates are expressed as episodes per patient month. Data were analyzed using the unpaired t-test. A p value of less than 0.05 was considered statistically significant. Results Of 100 patients analyzed, 50 were using topical mupirocin, and 50 were using topical gentamicin. Among the 50 patients on gentamicin, 23 had initially been on mupirocin and were later switched to gentamicin. In the study population, the gentamicin had 713 months of PD experience, and the mupirocin had 590 months of PD experience. Table I details the patient characteristics. The two s were similar in age and sex distribution. Of the patients in the gentamicin, 40% had diabetes mellitus; in mupirocin, 38% of patients had diabetes mellitus. The ESI rate was episodes/patient month in the gentamicin and episodes/patient month TABLE I Patient characteristics Characteristic Patients (n) Sex [n men (%)] 23 (46) 25 (50) Age range (years) With diabetes [n (%)] 19 (38) 20 (40) Modality of PD CAPD CCPD 5 4 NIPD 2 2 PD = peritoneal dialysis; CAPD = continuous ambulatory PD; CCPD = continuous cycling PD; NIPD = nightly intermittent PD. in the mupirocin (p = 0.45). The rate of grampositive ESI was episodes/patient month in the gentamicin and episodes/patient month in the mupirocin (p = 0.75). The rate of gram-negative ESI was zero in the gentamicin and episodes/patient month in the mupirocin (p = 0.22, Table II, Figure 1). We observed no P. aeruginosa infections and 2 S. aureus infections in the gentamicin. We observed no S. aureus infections and 2 P. aeruginosa infections in the mupirocin (Table III). The peritonitis rate was 0.06 episodes/patient month in the gentamicin and 0.02 episodes/ patient month in the mupirocin (p = 0.07). The rate of gram-positive peritonitis was 0.05 episodes/ patient month in the gentamicin and 0.01 episodes/patient month in the mupirocin (p = 0.08). The rate of gram-negative peritonitis was episodes/patient month in the gentamicin and episodes/patient month in the mupirocin ( p = 0.83, Table II, Figure 2). In 2 patients on gentamicin and 3 on mupirocin, peritonitis was polymicrobial. We observed 6 S. aureus infections in the gentamicin, and 3 in the mupirocin. Notably, 12 of the 36 episodes of peritonitis in the gentamicin and 5 of the 16 in the mupirocin were attributable to CoNS (Table IV). Discussion The Bernardini study showed superior results for gentamicin in preventing gram-negative infections, with gram-positive coverage similar to that of mupirocin (11). In contrast, our retrospective study showed a trend toward higher peritonitis rates with gentamicin,
3 58 Mahaldar et al. TABLE II Exit-site infections and peritonitis Infection Gentamicin Mupirocin p type n Rate a 95% CI n Rate a 95% CI Value Exit-site infections (ESIs) to to Gram-positive ESIs to to Gram-negative ESIs to Peritonitis to to Gram-positive peritonitis to to Gram-negative peritonitis to to a Episodes/patient month. CI = confidence interval. FIGURE 1 Exit-site infections per patient month. FIGURE 2 Peritonitis per patient month. TABLE III Microbiology of exit-site infections TABLE IV Microbiology of peritonitis Organism (n=2) (n=4) Staphylococcus aureus 2 0 Pseudomonas aeruginosa 0 2 Other/culture-negative 0 2 mainly as a result of a greater number of gram-positive infections. One third of the gram-positive infections in the gentamicin were attributable to CoNS. It is important to remember that most CoNS peritonitis are the result of touch contamination and not periluminal spread of an ESI (12,13). With both gentamicin and mupirocin, ESIs and gram-negative peritonitis episodes were infrequent. None of the results are statistically significant. Our study has several limitations. One major drawback is that the study was retrospective and therefore Organism (n=36) a (n=16) b Staphylococcus aureus 6 3 Gram-negative 6 5 CoNS 12 5 Streptococci 6 0 Other/culture-negative 8 6 a In the gentamicin, 2 patients had polymicrobial infections. b In the mupirocin, 3 patients had polymicrobial infections. CoNS = coagulase-negative Staphylococcus. not controlled for certain major factors that play a role in catheter infection, such as standardized aseptic exitsite care techniques. Our results are further limited by the small number of patients and relatively low infection rates.when a diagnosis of ESI was charted,
4 Gentamicin and Mupirocin in ESI 59 only instances that met our definition were included in our analysis. However, physicians and nurses may have been inaccurate in their documentation of the physical findings used to diagnose ESIs, and underreporting or overreporting of ESIs may have occurred in this retrospective review. In addition to developing because of pericatheter spread, peritonitis can also develop because of spread of infection by the transluminal, endogenous, and hematogenous routes. Given the nature of the organisms isolated from patients with peritonitis, it is likely that other routes of infection were important in our patients. The selection of patients from a single site may also limit the generalizability of the findings. Conclusions Gentamicin cream was not superior to mupirocin in exit-site prophylaxis. Large prospective studies are needed to determine the best protocols for prevention of ESIs and peritonitis in PD patients. References 1 Churchill DN, Taylor DW, Keshaviah PR, and the CANUSA Peritoneal Dialysis Study Group. Adequacy of dialysis and nutrition in continuous peritoneal dialysis: association with clinical outcomes. J Am Soc Nephrol 1996;7: Piraino B, Bailie GR, Bernardini J, et al. Peritoneal dialysis related infections recommendations: 2005 update. Perit Dial Int 2005;25: Gupta B, Bernardini J, Piraino B. Peritonitis associated with exit site and tunnel infections. Am J Kidney Dis 1996;28: Piraino B, Bernardini J, Sorkin M. The influence of peritoneal catheter exit-site infections on peritonitis, tunnel infections, and catheter loss in patients on continuous ambulatory peritoneal dialysis. Am J Kidney Dis 1986;8: Mujais S. Microbiology and outcomes of peritonitis in North America. Kidney Int Suppl 2006;(103):S Thodis E, Passadakis P, Panagoutsos S, Bacharaki D, Euthimiadou A, Vargemezis V. The effectiveness of mupirocin preventing Staphylococcus aureus in catheter-related infections in peritoneal dialysis. Adv Perit Dial 2000;16: Bernardini J, Piraino B, Holley J, Johnston JR, Lutes R. A randomized trial of Staphylococcus aureus prophylaxis in peritoneal dialysis patients: mupirocin calcium ointment 2% applied to the exit site versus cyclic oral rifampin. Am J Kidney Dis 1996;27: Mahajan S, Tiwari SC, Kalra V, et al. Effect of local mupirocin application on exit-site infection and peritonitis in an Indian peritoneal dialysis population. Perit Dial Int 2005;25: Casey M, Taylor J, Clinard P, et al. Application of mupirocin cream at the catheter exit site reduces exit-site infections and peritonitis in peritoneal dialysis patients. Perit Dial Int 2000;20: Uttley L, Vardhan A, Mahajan S, Smart B, Hutchison A, Gokal R. Decrease in infections with the introduction of mupirocin cream at the peritoneal dialysis catheter exit site. J Nephrol 2004;17: Bernardini J, Bender F, Florio T, et al. Randomized, double-blind trial of antibiotic exit site cream for prevention of exit site infection in peritoneal dialysis patients. J Am Soc Nephrol 2005;16: Vas S. Microbiological aspects of peritonitis. Perit Dial Bull 1981;1:S Holley JL, Bernardini J, Piraino B. Infecting organisms in continuous ambulatory peritoneal dialysis patients on the Y-set. Am J Kidney Dis 1994;23: Corresponding author: Pranay Kathuria, MD, Department of Internal Medicine, University of Oklahoma College of Medicine, 4502 E. 41st Street, Tulsa, Oklahoma U.S.A. Pranay-Kathuria@ouhsc.edu
5
The impact of topical mupirocin on peritoneal dialysis infection in Singapore General Hospital
 NDT Advance Access published July 26, 25 Nephrol Dial Transplant (25) 1 of 5 doi:1.193/ndt/gfi1 Original Article The impact of topical mupirocin on peritoneal dialysis infection in Singapore General Hospital
NDT Advance Access published July 26, 25 Nephrol Dial Transplant (25) 1 of 5 doi:1.193/ndt/gfi1 Original Article The impact of topical mupirocin on peritoneal dialysis infection in Singapore General Hospital
A Randomized, Double-Blinded Study for the Prevention of Exit Site Infections in Pediatric Peritoneal Dialysis Patients
 A Randomized, Double-Blinded Study for the Prevention of Exit Site Infections in Pediatric Peritoneal Dialysis Patients Joshua Zaritsky, MD PhD, Barbara Gales, RN, Georgina Ramos, and Isidro B. Salusky,
A Randomized, Double-Blinded Study for the Prevention of Exit Site Infections in Pediatric Peritoneal Dialysis Patients Joshua Zaritsky, MD PhD, Barbara Gales, RN, Georgina Ramos, and Isidro B. Salusky,
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
ISPD Peritonitis Recommendations: 2016 Update on Prevention and Treatment
 April 6, 2017 Mauro Verrelli, MD ISPD Peritonitis Recommendations: 2016 Update on Prevention and Treatment, Li PK, Szeto CC, Piraino, B et al. Peritoneal Dialysis International, Vol. 36, pp. 481 508 Outline
April 6, 2017 Mauro Verrelli, MD ISPD Peritonitis Recommendations: 2016 Update on Prevention and Treatment, Li PK, Szeto CC, Piraino, B et al. Peritoneal Dialysis International, Vol. 36, pp. 481 508 Outline
The CARI Guidelines Caring for Australians with Renal Impairment. 8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter
 8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: February 2003 Final submission: May 2004 Guidelines (Include recommendations based on level I or II evidence) Antibiotic
8. Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: February 2003 Final submission: May 2004 Guidelines (Include recommendations based on level I or II evidence) Antibiotic
Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CONTROLLED DOCUMENT
 CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
CONTROLLED DOCUMENT Protocol for exit-site care and treatment of exit-site infections in peritoneal dialysis CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Guideline Clinical The purpose
TREATMENT OF PERITONEAL DIALYSIS (PD) RELATED PERITONITIS. General Principles
 WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
Diagnosis: Presenting signs and Symptoms include:
 PERITONITIS TREATMENT PROTOCOL CARI - Caring for Australasians with Renal Impairment - CARI Guidelines complete list ISPD Guidelines: http://www.ispd.org/lang-en/treatmentguidelines/guidelines Objective
PERITONITIS TREATMENT PROTOCOL CARI - Caring for Australasians with Renal Impairment - CARI Guidelines complete list ISPD Guidelines: http://www.ispd.org/lang-en/treatmentguidelines/guidelines Objective
To guide safe and appropriate selection of antibiotic therapy for Peritoneal Dialysis patients.
 Nephrology Directorate Subject: Objective: Prepared by: Aintree Antibiotic Guidelines for Peritoneal Dialysis (PD): Catheter Insertion, and the Diagnosis and Treatment of PD Peritonitis and Exit-Site Infections.
Nephrology Directorate Subject: Objective: Prepared by: Aintree Antibiotic Guidelines for Peritoneal Dialysis (PD): Catheter Insertion, and the Diagnosis and Treatment of PD Peritonitis and Exit-Site Infections.
Prophylactic antibiotics for insertion of peritoneal dialysis catheter
 Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: October 2010 Final submission: September 2012 Author: Maha Yehia GUIDELINES a. Intravenous antibiotic prophylaxis should
Prophylactic antibiotics for insertion of peritoneal dialysis catheter Date written: October 2010 Final submission: September 2012 Author: Maha Yehia GUIDELINES a. Intravenous antibiotic prophylaxis should
Randomized, Double-Blind Trial of Antibiotic Exit Site Cream for Prevention of Exit Site Infection in Peritoneal Dialysis Patients
 Randomized, Double-Blind Trial of Antibiotic Exit Site Cream for Prevention of Exit Site Infection in Peritoneal Dialysis Patients Judith Bernardini,* Filitsa Bender, Tracey Florio,* James Sloand, Linda
Randomized, Double-Blind Trial of Antibiotic Exit Site Cream for Prevention of Exit Site Infection in Peritoneal Dialysis Patients Judith Bernardini,* Filitsa Bender, Tracey Florio,* James Sloand, Linda
The CARI Guidelines Caring for Australians with Renal Impairment. 10. Treatment of peritoneal dialysis associated fungal peritonitis
 10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
In peritoneal dialysis (PD) patients, peritonitis is a serious
 Proceedings of the ISPD 2006 The 11th Congress of the ISPD 0896-8608/07 $3.00 +.00 August 25 29, 2006, Hong Kong Copyright 2007 International Society for Peritoneal Dialysis Peritoneal Dialysis International,
Proceedings of the ISPD 2006 The 11th Congress of the ISPD 0896-8608/07 $3.00 +.00 August 25 29, 2006, Hong Kong Copyright 2007 International Society for Peritoneal Dialysis Peritoneal Dialysis International,
2. Peritoneal dialysis-associated peritonitis in children
 2. Peritoneal dialysis-associated peritonitis in children Date written: February 2003 Final submission: July 2004 Guidelines No recommendations possible based on Level I or II evidence Suggestions for
2. Peritoneal dialysis-associated peritonitis in children Date written: February 2003 Final submission: July 2004 Guidelines No recommendations possible based on Level I or II evidence Suggestions for
Infectious Complications in PD. An De Vriese Division of Nephrology and Infectious Diseases AZ Sint-Jan Brugge
 Infectious Complications in PD An De Vriese Division of Nephrology and Infectious Diseases AZ Sint-Jan Brugge Prevention of Peritonitis Management of Peritonitis EXIT-SITE CARE: STATE OF THE ART Szeto
Infectious Complications in PD An De Vriese Division of Nephrology and Infectious Diseases AZ Sint-Jan Brugge Prevention of Peritonitis Management of Peritonitis EXIT-SITE CARE: STATE OF THE ART Szeto
Intraperitoneal and Subsequent. Intravenous Vancomycin: An Effective Treatment Option for Gram-Positive Peritonitis in Peritoneal Dialysis
 Open Access Journal of Clinical Nephrology Research Article Intraperitoneal and Subsequent ISSN 2576-9529 Intravenous Vancomycin: An Effective Treatment Option for Gram-Positive Peritonitis in Peritoneal
Open Access Journal of Clinical Nephrology Research Article Intraperitoneal and Subsequent ISSN 2576-9529 Intravenous Vancomycin: An Effective Treatment Option for Gram-Positive Peritonitis in Peritoneal
Randomized Controlled Trial on Adjunctive Lavage for Severe Peritoneal Dialysis- Related Peritonitis
 Randomized Controlled Trial on Adjunctive Lavage for Severe Peritoneal Dialysis- Related Peritonitis Steve SM Wong Alice Ho Miu Ling Nethersole Hospital Background PD peritonitis is a major cause of PD
Randomized Controlled Trial on Adjunctive Lavage for Severe Peritoneal Dialysis- Related Peritonitis Steve SM Wong Alice Ho Miu Ling Nethersole Hospital Background PD peritonitis is a major cause of PD
Recurrent or severe exit-site infections (ESIs) and peritonitis
 Peritoneal Dialysis International, Vol. 29, pp. 303 309 Printed in Canada. All rights reserved. 0896-8608/09 $3.00 +.00 Copyright 2009 International Society for Peritoneal Dialysis THE HONEYPOT STUDY PROTOCOL:
Peritoneal Dialysis International, Vol. 29, pp. 303 309 Printed in Canada. All rights reserved. 0896-8608/09 $3.00 +.00 Copyright 2009 International Society for Peritoneal Dialysis THE HONEYPOT STUDY PROTOCOL:
The new ISPD peritonitis guideline
 Szeto Renal Replacement Therapy (2018) 4:7 DOI 10.1186/s41100-018-0150-2 REVIEW The new ISPD peritonitis guideline Cheuk Chun Szeto Open Access Abstract: Peritoneal dialysis (PD)-related infection encompasses
Szeto Renal Replacement Therapy (2018) 4:7 DOI 10.1186/s41100-018-0150-2 REVIEW The new ISPD peritonitis guideline Cheuk Chun Szeto Open Access Abstract: Peritoneal dialysis (PD)-related infection encompasses
ISPD GUIDELINES/RECOMMENDATIONS PERITONEAL DIALYSIS-RELATED INFECTIONS RECOMMENDATIONS: 2005 UPDATE
 Peritoneal Dialysis International, Vol. 25, pp. 107 131 Printed in Canada. All rights reserved. 0896-8608/05 $3.00 +.00 Copyright 2005 International Society for Peritoneal Dialysis ISPD GUIDELINES/RECOMMENDATIONS
Peritoneal Dialysis International, Vol. 25, pp. 107 131 Printed in Canada. All rights reserved. 0896-8608/05 $3.00 +.00 Copyright 2005 International Society for Peritoneal Dialysis ISPD GUIDELINES/RECOMMENDATIONS
INFECTIOUS COMPLICATIONS OF PERITONEAL DIALYSIS
 INFECTIOUS COMPLICATIONS OF PERITONEAL DIALYSIS J. Vande Walle, With special thanks to S. Bakkaloğlu, C Aufricht, A. Edefonti, R.Shroff,W. Van Biesen PD Peritonitis prevention - diagnosis - management
INFECTIOUS COMPLICATIONS OF PERITONEAL DIALYSIS J. Vande Walle, With special thanks to S. Bakkaloğlu, C Aufricht, A. Edefonti, R.Shroff,W. Van Biesen PD Peritonitis prevention - diagnosis - management
St George/Sutherland Hospitals And Health Services (SGSHHS)
 PERITONEAL DIALYSIS (PD) PERITONITIS MANAGEMENT AND TREATMENT Cross References (including NSW Health/ SESLHD policy directives) Medication Handling in NSW Public Health Facilities; NSW Health PD2013_043
PERITONEAL DIALYSIS (PD) PERITONITIS MANAGEMENT AND TREATMENT Cross References (including NSW Health/ SESLHD policy directives) Medication Handling in NSW Public Health Facilities; NSW Health PD2013_043
Guideline for the diagnosis and treatment of PD peritonitis and exit site infections in adults
 Full title of guideline Author Division & Speciality Scope (Target audience, state if Trust wide) Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis)
Full title of guideline Author Division & Speciality Scope (Target audience, state if Trust wide) Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis)
13. Treatment of peritoneal dialysis-associated peritonitis in adults
 13. Treatment of peritoneal dialysis-associated peritonitis in adults Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) In peritoneal
13. Treatment of peritoneal dialysis-associated peritonitis in adults Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) In peritoneal
Peritonitis is a serious complication of peritoneal dialysis
 Staphylococcus aureus Peritonitis Complicates Peritoneal Dialysis: Review of 245 Consecutive Cases Cheuk-Chun Szeto, Kai-Ming Chow, Bonnie Ching-Ha Kwan, Man-Ching Law, Kwok-Yi Chung, Samuel Yu, Chi-Bon
Staphylococcus aureus Peritonitis Complicates Peritoneal Dialysis: Review of 245 Consecutive Cases Cheuk-Chun Szeto, Kai-Ming Chow, Bonnie Ching-Ha Kwan, Man-Ching Law, Kwok-Yi Chung, Samuel Yu, Chi-Bon
Peritoneal dialysis (PD) has been an established treatment
 Peritoneal Dialysis International, Vol. 34, pp. 188 194 doi: 10.3747/pdi.2012.00233 0896-8608/14 $3.00 +.00 Copyright 2014 International Society for Peritoneal Dialysis MICROBIOLOGY AND OUTCOMES OF PERITONITIS
Peritoneal Dialysis International, Vol. 34, pp. 188 194 doi: 10.3747/pdi.2012.00233 0896-8608/14 $3.00 +.00 Copyright 2014 International Society for Peritoneal Dialysis MICROBIOLOGY AND OUTCOMES OF PERITONITIS
Peritonitis is a serious complication of peritoneal dialysis
 Coagulase Negative Staphylococcal Peritonitis in Peritoneal Dialysis Patients: Review of 232 Consecutive Cases Cheuk-Chun Szeto, Bonnie Ching-Ha Kwan, Kai-Ming Chow, Miu-Fong Lau Man-Ching Law, Kwok-Yi
Coagulase Negative Staphylococcal Peritonitis in Peritoneal Dialysis Patients: Review of 232 Consecutive Cases Cheuk-Chun Szeto, Bonnie Ching-Ha Kwan, Kai-Ming Chow, Miu-Fong Lau Man-Ching Law, Kwok-Yi
Empiric antimicrobial use in the treatment of dialysis related infections in RIPAS Hospital
 Original Article Brunei Int Med J. 2013; 9 (6): 372-377 Empiric antimicrobial use in the treatment of dialysis related infections in RIPAS Hospital Lah Kheng CHUA, Department of Pharmacy, RIPAS Hospital,
Original Article Brunei Int Med J. 2013; 9 (6): 372-377 Empiric antimicrobial use in the treatment of dialysis related infections in RIPAS Hospital Lah Kheng CHUA, Department of Pharmacy, RIPAS Hospital,
Treatment of peritonitis in patients receiving peritoneal dialysis Antibiotic Guidelines. Contents
 Treatment of peritonitis in patients receiving Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Jude Allen (Pharmacist) Additional author(s): Dr David Lewis, Dr Dimitrios Poulikakos,
Treatment of peritonitis in patients receiving Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Jude Allen (Pharmacist) Additional author(s): Dr David Lewis, Dr Dimitrios Poulikakos,
Peritonitis Management in Children on PD
 Peritonitis Management in Children on PD Bradley A. Warady, M.D. Professor of Pediatrics University of Missouri - Kansas City Chief, Section of Nephrology Director, Dialysis and Transplantation The Children
Peritonitis Management in Children on PD Bradley A. Warady, M.D. Professor of Pediatrics University of Missouri - Kansas City Chief, Section of Nephrology Director, Dialysis and Transplantation The Children
ORIGINAL ARTICLE. Joanna Kabat Koperska, Edyta Gołembiewska, Kazimierz Ciechanowski
 ORIGINAL ARTICLE Peritoneal dialysis related peritonitis in the years 2005 2007 among patients of the Peritoneal Dialysis Clinic of the Department of Nephrology, Transplantology and Internal Medicine,
ORIGINAL ARTICLE Peritoneal dialysis related peritonitis in the years 2005 2007 among patients of the Peritoneal Dialysis Clinic of the Department of Nephrology, Transplantology and Internal Medicine,
Infectious complications remain the most significant
 Peritoneal Dialysis International, Vol. 32, pp. S32-S86 doi: 10.3747/pdi.2011.00091 0896-8608/12 $3.00 +.00 Copyright 2012 International Society for Peritoneal Dialysis ispd guidelines/recommendations
Peritoneal Dialysis International, Vol. 32, pp. S32-S86 doi: 10.3747/pdi.2011.00091 0896-8608/12 $3.00 +.00 Copyright 2012 International Society for Peritoneal Dialysis ispd guidelines/recommendations
Peritonitis is a serious complication of peritoneal dialysis
 Peritoneal Dialysis International, Vol. 30, pp. 311 319 doi: 10.3747/pdi.2008.00258 0896-8608/10 $3.00 +.00 Copyright 2010 International Society for Peritoneal Dialysis STAPHYLOCOCCUS AUREUS PERITONITIS
Peritoneal Dialysis International, Vol. 30, pp. 311 319 doi: 10.3747/pdi.2008.00258 0896-8608/10 $3.00 +.00 Copyright 2010 International Society for Peritoneal Dialysis STAPHYLOCOCCUS AUREUS PERITONITIS
Enterobacteriaceae peritonitis complicating peritoneal dialysis: A review of 210 consecutive cases
 http://www.kidney-international.org & 26 International Society of Nephrology original article see commentary on page 117 Enterobacteriaceae peritonitis complicating peritoneal dialysis: A review of 21
http://www.kidney-international.org & 26 International Society of Nephrology original article see commentary on page 117 Enterobacteriaceae peritonitis complicating peritoneal dialysis: A review of 21
Cibele Grothe 1*, Mônica Taminato 1, Angélica Belasco 1, Ricardo Sesso 2 and Dulce Barbosa 1
 Grothe et al. BMC Nephrology (2016) 17:115 DOI 10.1186/s12882-016-0329-0 RESEARCH ARTICLE Open Access Prophylactic treatment of chronic renal disease in patients undergoing peritoneal dialysis and colonized
Grothe et al. BMC Nephrology (2016) 17:115 DOI 10.1186/s12882-016-0329-0 RESEARCH ARTICLE Open Access Prophylactic treatment of chronic renal disease in patients undergoing peritoneal dialysis and colonized
Predictors and outcomes of fungal peritonitis in peritoneal dialysis patients
 http://www.kidney-international.org & 2009 International Society of Nephrology Predictors and outcomes of fungal peritonitis in peritoneal dialysis patients Rhianna Miles 1,2, Carmel M. Hawley 1,2, Stephen
http://www.kidney-international.org & 2009 International Society of Nephrology Predictors and outcomes of fungal peritonitis in peritoneal dialysis patients Rhianna Miles 1,2, Carmel M. Hawley 1,2, Stephen
Infectious complications of Peritoneal Dialysis
 Infectious complications of Peritoneal Dialysis Prevention and management ISPD 2005 From 30 years of our experience when confirmed by ISPD Guidelines 2005 Alain Slingeneyer : Montpellier Main concern =
Infectious complications of Peritoneal Dialysis Prevention and management ISPD 2005 From 30 years of our experience when confirmed by ISPD Guidelines 2005 Alain Slingeneyer : Montpellier Main concern =
An Evidence Based Approach to Antibiotic Prophylaxis in Oral Surgery
 An Evidence Based Approach to Antibiotic Prophylaxis in Oral Surgery Nicholas Makhoul DMD. MD. FRCD(C). Dip ABOMS. FACS. Director, Division of Oral and Maxillofacial Surgery Assistant Professor McGill
An Evidence Based Approach to Antibiotic Prophylaxis in Oral Surgery Nicholas Makhoul DMD. MD. FRCD(C). Dip ABOMS. FACS. Director, Division of Oral and Maxillofacial Surgery Assistant Professor McGill
Peritoneal dialysis (PD) possesses advantages, such
 Peritoneal Dialysis International, Vol. 34, pp. 308 316 doi: 10.3747/pdi.2013.00012 0896-8608/14 $3.00 +.00 Copyright 2014 International Society for Peritoneal Dialysis ESCHERICHIA COLI PERITONITIS IN
Peritoneal Dialysis International, Vol. 34, pp. 308 316 doi: 10.3747/pdi.2013.00012 0896-8608/14 $3.00 +.00 Copyright 2014 International Society for Peritoneal Dialysis ESCHERICHIA COLI PERITONITIS IN
Worldwide variation of dialysis-associated peritonitis in children
 original article http://www.kidney-international.org & 2007 International Society of Nephrology see commentary on page 1305 Worldwide variation of dialysis-associated peritonitis in children F Schaefer
original article http://www.kidney-international.org & 2007 International Society of Nephrology see commentary on page 1305 Worldwide variation of dialysis-associated peritonitis in children F Schaefer
General Surgery Small Group Activity (Facilitator Notes) Curriculum for Antimicrobial Stewardship
 General Surgery Small Group Activity (Facilitator Notes) Curriculum for Antimicrobial Stewardship Facilitator instructions: Read through the facilitator notes and make note of discussion points for each
General Surgery Small Group Activity (Facilitator Notes) Curriculum for Antimicrobial Stewardship Facilitator instructions: Read through the facilitator notes and make note of discussion points for each
Introduction. n Ventricular catheter placement one of the most common neurosurgical procedures
 SHUNT INFECTION Introduction n Ventricular catheter placement one of the most common neurosurgical procedures n One of the most common complications associated is infection n Infection: positive CSF culture/
SHUNT INFECTION Introduction n Ventricular catheter placement one of the most common neurosurgical procedures n One of the most common complications associated is infection n Infection: positive CSF culture/
Replaces:04/14/16. Formulated: 1997 SKIN AND SOFT TISSUE INFECTION
 Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Effective Date: 04/13/17 Replaces:04/14/16 Page 1 of 7 POLICY To standardize the clinical management and housing of offenders with skin and soft tissue infections, thereby reducing the transmission and
Treatment of Surgical Site Infection Meeting Quality Statement 6. Prof Peter Wilson University College London Hospitals
 Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Treatment of Surgical Site Infection Meeting Quality Statement 6 Prof Peter Wilson University College London Hospitals TEG Quality Standard 6 Treatment and effective antibiotic prescribing: People with
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE FOR HEALTHCARE ACQUIRED CEREBROSPINAL FLUID SHUNT ASSOCIATED INFECTIONS
 Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE FOR HEALTHCARE ACQUIRED CEREBROSPINAL FLUID SHUNT ASSOCIATED INFECTIONS FINAL November 29, 2017 Working Group: Joanne Langley (Chair),
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE FOR HEALTHCARE ACQUIRED CEREBROSPINAL FLUID SHUNT ASSOCIATED INFECTIONS FINAL November 29, 2017 Working Group: Joanne Langley (Chair),
PERITONEAL DIALYSIS PERITONITIS - DIAGNOSIS AND TREATMENT
 PERITONEAL DIALYSIS PERITONITIS - DIAGNOSIS AND TREATMENT Renal, Respiratory, Cardiac and Vascular CMG 1 BACKGROUND In Leicester the rate of PD peritonitis is on average one episode in 19 months PD treatment.
PERITONEAL DIALYSIS PERITONITIS - DIAGNOSIS AND TREATMENT Renal, Respiratory, Cardiac and Vascular CMG 1 BACKGROUND In Leicester the rate of PD peritonitis is on average one episode in 19 months PD treatment.
For some reason the skin on the inside of both my nostrils continually splits, heals, and splits again. I do have allergies frequently
 12-3-2018 For some reason the skin on the inside of both my nostrils continually splits, heals, and splits again. I do have allergies frequently which may contribute. What is Folliculitis? Folliculitis
12-3-2018 For some reason the skin on the inside of both my nostrils continually splits, heals, and splits again. I do have allergies frequently which may contribute. What is Folliculitis? Folliculitis
Pocket Guide to Diagnosis & Treatment of Cardiovascular Implantable Electronic Device (CIED) Infections
 Pocket Guide to Diagsis & Treatment of Cardiovascular Implantable Electronic Device (CIED) Infections Draft Version : November 208 DEFINITION Pocket infection, if all 4 criteria are fulfilled: Investigation/sign
Pocket Guide to Diagsis & Treatment of Cardiovascular Implantable Electronic Device (CIED) Infections Draft Version : November 208 DEFINITION Pocket infection, if all 4 criteria are fulfilled: Investigation/sign
Post-operative surgical wound infection
 Med. J. Malaysia Vol. 45 No. 4 December 1990 Post-operative surgical wound infection Yasmin Abu Hanifah, MBBS, MSc. (London) Lecturer Department of Medical Microbiology, Faculty of Medicine, University
Med. J. Malaysia Vol. 45 No. 4 December 1990 Post-operative surgical wound infection Yasmin Abu Hanifah, MBBS, MSc. (London) Lecturer Department of Medical Microbiology, Faculty of Medicine, University
Concise Antibiogram Toolkit Background
 Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Pathogens and Antibiotic Sensitivities in Post- Phacoemulsification Endophthalmitis, Kaiser Permanente, California,
 Pathogens and Antibiotic Sensitivities in Post- Phacoemulsification Endophthalmitis, Kaiser Permanente, California, 2007-2012 Geraldine R. Slean, MD, MS 1 ; Neal H. Shorstein, MD 2 ; Liyan Liu, MD, MS
Pathogens and Antibiotic Sensitivities in Post- Phacoemulsification Endophthalmitis, Kaiser Permanente, California, 2007-2012 Geraldine R. Slean, MD, MS 1 ; Neal H. Shorstein, MD 2 ; Liyan Liu, MD, MS
Preventing Surgical Site Infections. Edward L. Goodman, MD September 16, 2013
 Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Preventing Surgical Site Infections Edward L. Goodman, MD September 16, 2013 Outline NHSN Reporting and Definitions Magnitude of the Problem Risk Factors Non Pharmacologic Interventions Pharmacologic Interventions
Antibiotic Stewardship in the LTC Setting
 Antibiotic Stewardship in the LTC Setting Joe Litsey, Director of Consulting Services Pharm.D., Board Certified Geriatric Pharmacist Thrifty White Pharmacy Objectives Describe the Antibiotic Stewardship
Antibiotic Stewardship in the LTC Setting Joe Litsey, Director of Consulting Services Pharm.D., Board Certified Geriatric Pharmacist Thrifty White Pharmacy Objectives Describe the Antibiotic Stewardship
Study of Bacteriological Profile of Corneal Ulcers in Patients Attending VIMS, Ballari, India
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 7 (2016) pp. 200-205 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.507.020
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 7 (2016) pp. 200-205 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.507.020
Nottingham Renal and Transplant Unit
 Nottingham Renal and Transplant Unit Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out
Nottingham Renal and Transplant Unit Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out
Role of the nurse in diagnosing infection: The right sample, every time
 BROUGHT TO YOU BY Role of the nurse in diagnosing infection: The right sample, every time The module has been written by Shanika Anne-Marie Crusz and Amelia Joseph Authors affiliation: Department of Clinical
BROUGHT TO YOU BY Role of the nurse in diagnosing infection: The right sample, every time The module has been written by Shanika Anne-Marie Crusz and Amelia Joseph Authors affiliation: Department of Clinical
Objectives 4/26/2017. Co-Investigators Sadie Giuliani, PharmD, BCPS Claude Tonnerre, MD Jayme Hartzell, PharmD, MS, BCPS
 IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
Clinical course of peritonitis due to Pseudomonas species comtor. complicating peritoneal dialysis: A review of 104 cases
 Kidney International, Vol. 59 (2001), pp. 2309 2315 Clinical course of peritonitis due to Pseudomonas species complicating peritoneal dialysis: A review of 104 cases CHEUK-CHUN SZETO, KAI-MING CHOW, CHI-BON
Kidney International, Vol. 59 (2001), pp. 2309 2315 Clinical course of peritonitis due to Pseudomonas species complicating peritoneal dialysis: A review of 104 cases CHEUK-CHUN SZETO, KAI-MING CHOW, CHI-BON
Antibiotic Treatment of Peritonitis
 Antibiotic Treatment of Peritonitis BC Children s Hospital Step-by-Step Instructions for Parents and Allied Health Professionals February 2012 Developed by C. Prestidge, MD, J. Leechik, BSN, K. Collin,
Antibiotic Treatment of Peritonitis BC Children s Hospital Step-by-Step Instructions for Parents and Allied Health Professionals February 2012 Developed by C. Prestidge, MD, J. Leechik, BSN, K. Collin,
2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY FINAL Working Group: E. Henderson, M. John, I. Davis, S. Dunford,
Canadian Nosocomial Infection Surveillance Program 2017 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING TOTAL HIP AND KNEE ARTHROPLASTY FINAL Working Group: E. Henderson, M. John, I. Davis, S. Dunford,
Treatment of peritoneal dialysis associated fungal peritonitis
 Treatment of peritoneal dialysis associated fungal peritonitis Date written: April 2013 Author: Maureen Lonergan GUIDELINES a. Oral antifungal prophylaxis should be considered when antibiotics are administered
Treatment of peritoneal dialysis associated fungal peritonitis Date written: April 2013 Author: Maureen Lonergan GUIDELINES a. Oral antifungal prophylaxis should be considered when antibiotics are administered
CONFLICT OF INTEREST ANTIMICROBIAL LOCK SOLUTIONS INCREASE BACTEREMIA
 CONFLICT OF INTEREST ANTIMICROBIAL LOCK SOLUTIONS INCREASE BACTEREMIA NONE Vandana Dua Niyyar, MD Associate Professor of Medicine, Division of Nephrology, Emory University. OBJECTIVES Role of biofilm in
CONFLICT OF INTEREST ANTIMICROBIAL LOCK SOLUTIONS INCREASE BACTEREMIA NONE Vandana Dua Niyyar, MD Associate Professor of Medicine, Division of Nephrology, Emory University. OBJECTIVES Role of biofilm in
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY
 Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Canadian Nosocomial Infection Surveillance Program 2018 SURVEILLANCE OF SURGICAL SITES INFECTIONS FOLLOWING HIP AND KNEE ARTHROPLASTY FINAL Working Group: Dominik Mertz (Chair) Elizabeth Henderson, Johan
Antibiotic Prophylaxis Update
 Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
Antibiotic Prophylaxis Update Choosing Surgical Antimicrobial Prophylaxis Peri-Procedural Administration Surgical Prophylaxis and AMS at Epworth HealthCare Mr Glenn Valoppi Dr Trisha Peel Dr Joseph Doyle
Clinical Policy: Clindamycin (Cleocin) Reference Number: CP.HNMC.08 Effective Date: Last Review Date: Line of Business: Medicaid - HNMC
 Clinical Policy: (Cleocin) Reference Number: CP.HNMC.08 Effective Date: 07.01.17 Last Review Date: 02.18 Line of Business: Medicaid - HNMC Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Cleocin) Reference Number: CP.HNMC.08 Effective Date: 07.01.17 Last Review Date: 02.18 Line of Business: Medicaid - HNMC Revision Log See Important Reminder at the end of this policy
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
NEONATAL Point Prevalence Survey. Ward Form
 Appendix 2 NEONATAL Point Prevalence Survey Ward Form Please fill in one form for each ward included in PPS Date of survey Person completing form (Auditor code) Hospital Name Department/Ward Neonatal departments
Appendix 2 NEONATAL Point Prevalence Survey Ward Form Please fill in one form for each ward included in PPS Date of survey Person completing form (Auditor code) Hospital Name Department/Ward Neonatal departments
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM
 UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
C. Ciprofloxacin in peritonitis associated with continuous ambulatory peritoneal dialysis (CAPD)
 C. Ciprofloxacin in peritonitis associated with continuous ambulatory peritoneal dialysis (CAPD) Journal of Antimicrobial Chemotherapy (90) 6, Suppl. F, 63-7 A comparison between oral ciprofloxacin and
C. Ciprofloxacin in peritonitis associated with continuous ambulatory peritoneal dialysis (CAPD) Journal of Antimicrobial Chemotherapy (90) 6, Suppl. F, 63-7 A comparison between oral ciprofloxacin and
Treatment for peritoneal dialysis-associated peritonitis (Review)
 (Review) Wiggins KJ, Craig JC, Johnson DW, Strippoli GFM This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2008, Issue
(Review) Wiggins KJ, Craig JC, Johnson DW, Strippoli GFM This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2008, Issue
Patients. Excludes paediatrics, neonates.
 Full title of guideline Author Division & Speciality Scope Gentamicin Prescribing Guideline For Adult Patients Annette Clarkson, Specialist Clinical Pharmacist Antimicrobials and Infection Control All
Full title of guideline Author Division & Speciality Scope Gentamicin Prescribing Guideline For Adult Patients Annette Clarkson, Specialist Clinical Pharmacist Antimicrobials and Infection Control All
Empiric Management of Peritonitis
 Empiric Management of Peritonitis BC Children s Hospital On-Call Handbook February 2012 Developed by C. Prestidge, MD, J. Leechik, BSN, K. Collin, B.Sc.(Pharm), C. White, MD and the Division of Nephrology,
Empiric Management of Peritonitis BC Children s Hospital On-Call Handbook February 2012 Developed by C. Prestidge, MD, J. Leechik, BSN, K. Collin, B.Sc.(Pharm), C. White, MD and the Division of Nephrology,
Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site:
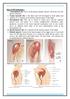 Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site: is the thick and well developed in both adults and children.
Sites of IM injections : 1. Ventrogluteal site: site is in the gluteus medius muscle, which lies over the gluteus minimus. 2. Vastus lateralis site: is the thick and well developed in both adults and children.
Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities
 Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities Introduction As the problem of antibiotic resistance continues to worsen in all healthcare setting, we
Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities Introduction As the problem of antibiotic resistance continues to worsen in all healthcare setting, we
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bennett-Guerrero E, Pappas TN, Koltun WA, et al. Gentamicin
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bennett-Guerrero E, Pappas TN, Koltun WA, et al. Gentamicin
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies
 ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
Rational use of antibiotics
 Rational use of antibiotics Uga Dumpis MD, PhD,, DTM Stradins University Hospital Riga, Latvia ugadumpis@stradini.lv BALTICCARE CONFERENCE, PSKOV, 16-18.03, 18.03, 2006 Why to use antibiotics? Prophylaxis
Rational use of antibiotics Uga Dumpis MD, PhD,, DTM Stradins University Hospital Riga, Latvia ugadumpis@stradini.lv BALTICCARE CONFERENCE, PSKOV, 16-18.03, 18.03, 2006 Why to use antibiotics? Prophylaxis
Intra-Abdominal Infections. Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018
 Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients.
 Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Staph Cases. Case #1
 Staph Cases Lisa Winston University of California, San Francisco San Francisco General Hospital Case #1 A 60 y.o. man with well controlled HIV and DM presents to clinic with ten days of redness and swelling
Staph Cases Lisa Winston University of California, San Francisco San Francisco General Hospital Case #1 A 60 y.o. man with well controlled HIV and DM presents to clinic with ten days of redness and swelling
Peritonitis with Atypical Organisms
 Peritonitis with Atypical Organisms Gurwant Kaur, MD Assistant Professor of Medicine (Nephrology) Co- director for Medical Students Renal block Penn State College of Medicine Penn State Milton S. Hershey
Peritonitis with Atypical Organisms Gurwant Kaur, MD Assistant Professor of Medicine (Nephrology) Co- director for Medical Students Renal block Penn State College of Medicine Penn State Milton S. Hershey
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare
 Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
Felipe N. Gutierrez MD, MPH Chief, Infectious Diseases Phoenix VA Healthcare 100% of all wounds will yield growth If you get a negative culture you something is wrong! Pseudomonas while ubiquitous does
HOSPITAL-ACQUIRED INFECTION/MRSA EYERUSALEM KIFLE AND GIFT IMUETINYAN OMOBOGBE PNURSS15
 HOSPITAL-ACQUIRED INFECTION/MRSA EYERUSALEM KIFLE AND GIFT IMUETINYAN OMOBOGBE PNURSS15 INTRODUCTION DEFINITIONS SIGNS AND SYMPTOMS RISK FACTORS DIAGNOSIS COMPLICATIONS PREVENTIONS TREATMENT PATIENT EDUCATION
HOSPITAL-ACQUIRED INFECTION/MRSA EYERUSALEM KIFLE AND GIFT IMUETINYAN OMOBOGBE PNURSS15 INTRODUCTION DEFINITIONS SIGNS AND SYMPTOMS RISK FACTORS DIAGNOSIS COMPLICATIONS PREVENTIONS TREATMENT PATIENT EDUCATION
Cellulitis. Assoc Prof Mark Thomas. Conference for General Practice Auckland Saturday 28 July 2018
 Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Cellulitis Assoc Prof Mark Thomas Conference for General Practice Auckland Saturday 28 July 2018 Summary Cellulitis Usual treatment flucloxacillin for 5 days Frequent recurrences consider penicillin 250mg
Bacteriological Profile and Antimicrobial Sensitivity of DJ Stents
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 6 (2016) pp. 345-349 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.506.039
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 6 (2016) pp. 345-349 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.506.039
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Antibiotic Stewardship in the Neonatal Intensive Care Unit. Objectives. Background 4/20/2017. Natasha Nakra, MD April 28, 2017
 Antibiotic Stewardship in the Neonatal Intensive Care Unit Natasha Nakra, MD April 28, 2017 Objectives 1. Describe antibiotic use in the NICU 2. Explain the role of antibiotic stewardship in the NICU 3.
Antibiotic Stewardship in the Neonatal Intensive Care Unit Natasha Nakra, MD April 28, 2017 Objectives 1. Describe antibiotic use in the NICU 2. Explain the role of antibiotic stewardship in the NICU 3.
Lessons from the success and failures of peritoneal Dialysis-Related Brucella Peritonitis in the last 16 years: Case report and Literature review
 Open Access Journal of Clinical Nephrology Case Report ISSN 2576-9529 Lessons from the success and failures of peritoneal Dialysis-Related Peritonitis in the last 16 years: Case report and Literature review
Open Access Journal of Clinical Nephrology Case Report ISSN 2576-9529 Lessons from the success and failures of peritoneal Dialysis-Related Peritonitis in the last 16 years: Case report and Literature review
The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection
 THE IRAQI POSTGRADUATE MEDICAL JOURNAL PROPHYLACTIC ANTIBIOTICS ON SURGICAL WOUND INFECTION The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection Ahmed Hamid Jasim*, Nabeel
THE IRAQI POSTGRADUATE MEDICAL JOURNAL PROPHYLACTIC ANTIBIOTICS ON SURGICAL WOUND INFECTION The Effect of Perioperative Use of Prophylactic Antibiotics on Surgical Wound Infection Ahmed Hamid Jasim*, Nabeel
Management of CRBSI Leilani Paitoonpong MD MSc Chusana Suankratay MD PhD Division of Infectious Diseases Chulalongkorn University
 Management of CRBSI Leilani Paitoonpong MD MSc Chusana Suankratay MD PhD Division of Infectious Diseases Chulalongkorn University A 60-year-old man was admitted for CABG surgery due to triple-vessel disease.
Management of CRBSI Leilani Paitoonpong MD MSc Chusana Suankratay MD PhD Division of Infectious Diseases Chulalongkorn University A 60-year-old man was admitted for CABG surgery due to triple-vessel disease.
Prophylactic antibiotic timing and dosage. Dr. Sanjeev Singh AIMS, Kochi
 Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Scottish Medicines Consortium
 Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Your Guide to Managing. Multi Drug-resistant Organisms (MDROs)
 Agency for Integrated Care 5 Maxwell Road #10-00 Tower Block MND Complex Singapore 069110 Singapore Silver Line: 1800-650-6060 Email: enquiries@aic.sg Website: www.silverpages.sg Facebook: www.facebook.com/carerssg
Agency for Integrated Care 5 Maxwell Road #10-00 Tower Block MND Complex Singapore 069110 Singapore Silver Line: 1800-650-6060 Email: enquiries@aic.sg Website: www.silverpages.sg Facebook: www.facebook.com/carerssg
Antibiotic Stewardship Program (ASP) CHRISTUS SETX
 Antibiotic Stewardship Program (ASP) CHRISTUS SETX Program Goals I. Judicious use of antibiotics Decrease use of broad spectrum antibiotics and deescalate use based on clinical symptoms Therapeutic duplication:
Antibiotic Stewardship Program (ASP) CHRISTUS SETX Program Goals I. Judicious use of antibiotics Decrease use of broad spectrum antibiotics and deescalate use based on clinical symptoms Therapeutic duplication:
Surgical prophylaxis for Gram +ve & Gram ve infection
 Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Surgical prophylaxis for Gram +ve & Gram ve infection Professor Mark Wilcox Clinical l Director of Microbiology & Pathology Leeds Teaching Hospitals & University of Leeds, UK Heath Protection Agency Surveillance
Combination vs Monotherapy for Gram Negative Septic Shock
 Combination vs Monotherapy for Gram Negative Septic Shock Critical Care Canada Forum November 8, 2018 Michael Klompas MD, MPH, FIDSA, FSHEA Professor, Harvard Medical School Hospital Epidemiologist, Brigham
Combination vs Monotherapy for Gram Negative Septic Shock Critical Care Canada Forum November 8, 2018 Michael Klompas MD, MPH, FIDSA, FSHEA Professor, Harvard Medical School Hospital Epidemiologist, Brigham
Copyright 2012 Diabetes In Control, Inc. For permission to reprint, please contact Heather Moran, Production Editor, at
 Malignant Otitis Externa Inflammation and damage at the base of the skull due to an untreated outer ear P. aeruginosa most common organism Yellow-green drainage from the ear Odor Fever Deep inner ear pain
Malignant Otitis Externa Inflammation and damage at the base of the skull due to an untreated outer ear P. aeruginosa most common organism Yellow-green drainage from the ear Odor Fever Deep inner ear pain
A retrospective analysis of urine culture results issued by the microbiology department, Teaching Hospital, Karapitiya
 A retrospective analysis of urine culture results issued by the microbiology department, Teaching Hospital, Karapitiya LU Edirisinghe 1, D Vidanagama 2 1 Senior Registrar in Medicine, 2 Consultant Microbiologist,
A retrospective analysis of urine culture results issued by the microbiology department, Teaching Hospital, Karapitiya LU Edirisinghe 1, D Vidanagama 2 1 Senior Registrar in Medicine, 2 Consultant Microbiologist,
S aureus infections: outpatient treatment. Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium
 S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
