NIH Public Access Author Manuscript J Crit Care. Author manuscript; available in PMC 2013 July 28.
|
|
|
- Jonathan Eaton
- 5 years ago
- Views:
Transcription
1 NIH Public Access Author Manuscript Published in final edited form as: J Crit Care December ; 24(4): doi: /j.jcrc A new dosing protocol reduces dexmedetomidine-associated hypotension in critically ill surgical patients,,,, Anthony T. Gerlach, PharmD, BCPS a, Joseph F. Dasta, MS, FCCM b,c, Steven Steinberg, MD d, Larry C. Martin, MD e, and Charles H. Cook, MD, FCCM d Anthony T. Gerlach: gerlach.6@osu.edu; Joseph F. Dasta: jdasta@mail.utexas.edu; Steven Steinberg: steven.steinberg@osumc.edu; Larry C. Martin: larry.martin@surgery.ufl.edu; Charles H. Cook: cook.131@osu.edu a Department of Pharmacy, The Ohio State University Medical Center, Columbus, Ohio 43210, USA b The Ohio State University, Columbus, Ohio, USA c University of Texas, Round Rock, TX 78665, USA d Department of Surgery, The Ohio State University Medical Center, Columbus, Ohio 43210, USA e Department of Surgery, University of Florida, P.O. Box , Gainesville, Fl 32610, USA Abstract Background Although no ideal sedative exists, dexmedetomidine is unique because it produces sedation and analgesia without decreasing the respiratory drive. Hemodynamic responses to dexmedetomidine are variable and dependent on the patient population. Our initial experience was associated with an unacceptable incidence of hypotension and bradycardia. We evaluated occurrence of hypotension and bradycardia in critically ill surgical patients receiving dexmedetomidine before and after implementation of a dosing protocol. Methods This is a retrospective chart review of all admissions to a university medical center based, 44-bed surgical intensive care unit pre and post protocol implementation. Results Forty-four patients received dexmedetomidine including 19 historic controls and 25 dosed via protocol. Both groups had comparable demographics and initial and maximum dosages of dexmedetomidine. Use of the dosing protocol resulted in fewer dosage changes (mean ± standard deviation, 4.8 ± 3.8 compared to 7.8 ± 3.9; P =.014) and fewer episodes of hypotension (16% vs 68.4%; P =.0006) but did not influence bradycardic episodes (20% vs 15.5%; P >.99). Conclusion We found that use of a protocol that increases the time interval between dosage adjustments may reduce dexmedetomidine-associated hypotension. Keywords Dexmedetomidine; Intensive care unit; Hypotension Joseph F. Dasta is a consultant and member of the Hospira Speakers Bureau for dexmedetomidine. None of the other authors have anything to disclose. No outside finances were used to fund this study. Author contributions trial design: AG, SS, LM, CC; data collection: AG; data analysis: AG, SS, LM, CC Elsevier Inc. All rights reserved. Correspondence to: Anthony T. Gerlach, gerlach.6@osu.edu. Amneal Pharmaceuticals LLC Exhibit 1020 Page 1
2 Gerlach et al. Page 2 1. Introduction After publication of Too Err is Human: Building a Safer Health System in 1999 by the Institute of Medicine, medication safety has become a top priority in health care [1]. That report focused on the observation that many medical errors involve medications and concluded that health care providers need to design safer systems [2,3]. Because of complexities of critical illness, patients in the intensive care unit (ICU) are considered to be at increased risk of medication errors and adverse drug events, particularly with intravenous medications [2 5]. Proposed strategies to improve medication safety in the ICU include intensivist-lead, multidisciplinary rounds with pharmacist participation; standardized drug preparation and administration; computerized prescriber order entry; bar coding technology; computerized intravenous infusion devices; education; and developing a culture of safety [2,6]. Because most medication errors and many adverse drug events are considered preventable, development of surveillance systems targeting strategies for improvement should help decrease adverse drug events in both the outpatient and the inpatient setting, including the ICU [6]. An essential part of ICU care is to protect patients from themselves during agitation, and this often requires use of sedatives such as propofol or benzodiazepines [7]. In addition, opioids are used to treat pain, a common contributor to agitation in surgical patients. Unfortunately, use of these medications is associated with adverse drug events such as respiratory depression, resulting in increased duration of mechanical ventilation, and development of ventilator-associated pneumonia, all of which increase ICU length of stay [8]. Dexmedetomidine is a sedative with a unique mechanism of action that became available in the United States in 1999 for sedation of critically ill patients [9]. Desirable properties of dexmedetomidine include induction of sedation and analgesia via stimulation of α 2 - receptors without concomitant respiratory depression by γ-aminobutric acid-mimetic properties that accompany use of many other sedatives [9]. Additional advantages of dexmedetomidine include a relatively short half-life and hepatic metabolism [9]. Described adverse drug reactions with dexmedetomidine include altered blood pressure, nausea, and bradycardia [10,11]. Hypotension, which is the most commonly reported adverse effect, results from a sympatholytic effect mediated by activation of central α 2a -receptors causing vasodilation [9,12]. Thus, dexmedetomidine has the desirable characteristic of inducing sedation without causing respiratory depression, but it also has potential side effects that might preclude its use during critical illness. Despite an initial enthusiasm for dexmedetomidine to treat agitation in our surgical ICU, data from our drug surveillance monitoring system suggested an unacceptable incidence of hypotension and bradycardia associated with its use. Closer evaluation revealed that hypotension often occurred when dexmedetomidine dosage was titrated rapidly (more frequently than every 20 minutes) compared with slower rates of titration [13]. Based upon these data, a dosing protocol for dexmedetomidine was developed that allows titration no more frequently than every 30 minutes. In this report, we described reduced occurrence of hypotension associated with dexmedetomidine in our surgical ICU after institution of this dosing protocol. 2. Materials and methods Dexmedetomidine was added to the Formulary of Accepted Medications at The Ohio State University Medical Center in 2001 and was restricted to use in the surgical ICU. We previously reported a medication use evaluation performance improvement project of patients receiving dexmedetomidine in the surgical ICU between October 2001 and December 2004 [13]. These data suggested that hypotension occurred more frequently when Amneal Pharmaceuticals LLC Exhibit 1020 Page 2
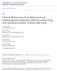
3 Gerlach et al. Page 3 3. Results dexmedetomidine is rapidly titrated. Based on these data, a dosing protocol was developed (Fig. 1). This protocol was reviewed and approved by the surgical ICU quality committee with representation from surgery, nursing, and pharmacy. Between April 2005 and March 2006, patients received dexmedetomidine via this new protocol and were compared with historic controls that received dexmedetomidine rapidly titrated (<20 minutes between dosage adjustments) between October 2001 and December Patients were excluded if they were less than 18 or more than 89 years old, pregnant, incarcerated, or receiving vasopressors before initiation of dexmedetomidine. Data collected included demographics, Acute Physiology and Chronic Health Evaluation II (APACHE II) score on admission, sedation score, indication, dosage titration, length of therapy, time between dosing adjustments, and adverse drug reactions attributed to dexmedetomidine from start of infusion to end of infusion. Data were retrospectively collected from our electronic ICU charting system (CliniComp International, San Diego, Calif). Vitals signs can be automatically imported at the touch of a computer key with this system. The primary outcome was the occurrence of hypotension, defined as a mean arterial blood pressure less than 60 mm Hg attributed to dexmedetomidine, as determined by one of the investigators (AG). Development of bradycardia was also studied and defined as heart rate less than 50 beats per minute attributed to dexmedetomidine. Hemodynamic parameters were monitored for 2 hours before initiation of dexmedetomidine to 12 hours after discontinuation. Sedation scores (Ramsay Sedation Score was collected in the control group and Richmond Agitation Sedation Score [RASS] for the protocol group) were collected between 30 and 120 minutes of initiation and within 2 hours before or after the development of an adverse drug reaction [7,14]. To allow comparison between these different scales, patients are reported to be agitated, calm, or sedated. Our retrospective chart review received institutional review board exemption. Statistical analysis was performed by Fisher exact test for nominal data or Student test for continuous data. The Mann-Whitney U test was used for nonparametric data. Continuous data are presented as mean ± standard deviation or median (25% 75% interquartile range). P values less than.05 were considered significant. Forty-four patients were included in analysis, including 25 patients that received dexmedetomidine after protocol institution and 19 historic controls that received rapidly titrated dexmedetomidine. Both groups had comparable demographics and admitting services (Tables 1 and 2). Median {25% 75% interquartile range} APACHE II scores upon admission were similar between groups (21 {15 25} protocol group vs 22 {15 29} historic control; P =.38). The mean duration of mechanical ventilation (protocol 10.7 ± 11.1 days vs 10.2 ± 12.1 days for controls; P =.89) and ICU length of stay (protocol 14.5 ± 11.1 days, controls 11.8 ± 11.4; P =.48) were similar between groups. Additional sedation was required in 8% of protocol patients (propofol in 1 patient with subarachnoid hemorrhage and lorazepam in 1 patient after trauma). The mean initial dosage of dexmedetomidine (0.24 ± 0.11 μg kg 1 h 1 protocol vs 0.22 ± 0.07 μg kg 1 h 1 controls; P =.42), the maximum dosage (0.43 ± 0.19 μg kg 1 h 1 protocol vs 0.54 ± 0.16 μg kg 1 h 1 controls; P =.08), and time to maximal dosage (259 ± 429 minutes protocol vs 153 ± 150 minutes controls; P =.4) were not statistically different between the groups (Table 2). Patients treated via protocol had significantly fewer dosage adjustments than historic control patients (protocol 4.8 ± 3.8 vs 7.8 ± 3.9 in controls; P =. 014). Median durations of dexmedetomidine infusion were 19.2 { } hours in the protocol group and 16.6 {7 33} hours in historic controls (P =.14). Sixteen patients Amneal Pharmaceuticals LLC Exhibit 1020 Page 3
4 Gerlach et al. Page 4 4. Discussion received dexmedetomidine longer than 24 hours (11/25 [25%] for protocol, 5/19 [26%] for historic controls; P =.34). Two patients received loading infusions of dexmedetomidine, both historic controls (P =.19). Seventeen patients developed hypotension, but this occurred significantly less frequently in protocol patients compared with historic controls (4 [16%] vs 13 [68.4%]; P =.0006). Bradycardia was not significantly different between groups (5 [20%] vs 3 [15.8%]; P >.99). A total of 22 patients developed hypotension and/or bradycardia (6 [24%] in the protocol group vs 16 [84%] in the historic controls; P =.0002) including 3 patients developing both (2 [8%] in the protocol group and 1 [5.3%] of the controls; P >.99). The total number of adverse drug reactions was significantly less in patients treated via protocol (7 [28%] vs 15 [78.9%]; P =.0019) than historic controls. For patients that developed hypotension, there was no statistical difference in mean arterial pressure between groups (mean nadir mean arterial pressure 51.8 ± 2.2 mm Hg protocol group vs 51.1 ± 7.6 mm Hg for historic controls; P =.87), and the mean nadir heart rates were similar for those that developed bradycardia (39.3 ± 9.9 beats per minutes for historic controls vs 37.8 ± 9.9 for controls). Time from initiation of therapy to development of hypotension was similar between protocol and historic control groups (4.2 ± 3.6 vs 3.8 ± 2.8 hours, respectively; P =.84) as was the time from initiation of therapy to bradycardia (12 ± 9.2 vs 5.9 ± 3.6 hours; P =.32). Hypotension (3.9 ±3 hours) tended to occur before bradycardia (9.7 ± 7.9 hours) in all patients, but this difference did not reach significance (P =.059). Only 2 of the 17 patients that developed hypotension had received dexmedetomidine for more than 24 hours (P >.99). For patients developing hypotension or bradycardia, all but 1 case were treated by stopping the dexmedetomidine infusion. In addition, hypotension was treated with administration of intravenous fluids in 5 patients (1 protocol patient and 4 historic controls). Four historic control patients required transient vasopressors, and 2 patients received atropine (1 in each group; P >.99). The level of sedation or agitation 30 to 120 minutes after dexmedetomidine initiation was documented in 41 patients (24 [96%] protocol vs 17 [89.5%] historic controls; P =.57) and within 2 hours of the development of an adverse effect in all but 1 patient in the control group (Table 3). In the first hours of sedation, the median sedation scores {25% 75% interquartile range} for both groups were calm (median RASS was 0 { 2,1} for the protocol group and median Ramsay Sedation Score was 2 {1,3} for the historical controls). Around the time of development of hypotension and bradycardia, the median RASS in the protocol group was lightly sedated ( 1 { 3,1}), and the median Ramsay Sedation Score for the historic controls was calm (2 {1,3}). The mean time from development of an adverse effect and documentation of sedation levels was 0.74 ± 0.7 hours. This study suggests that occurrence of hypotension associated with dexmedetomidine use in postoperative ICU patients can be significantly reduced by implementation of a dosing protocol. Although hypotension is a potential adverse effect of any sedative agent [15 22], our initial experience with dexmedetomidine showed a somewhat higher incidence of hypotension (approximately 69%) than reported by others (Table 4) [16,17,23]. Some have suggested that dexmedetomidine-associated hypotension and bradycardia are consequent to activation of α 2 -receptors resulting in sympatholysis [11,15,17], and others have reported that administration of dexmedetomidine without loading infusions can achieve satisfactory sedation [21,23]. We chose a slightly different approach, which was to slow down the rate of titration, and report that our protocol may reduce dexmedetomidine-associated hypotension to levels lower than previously reported (16%) [13,16,17,23]. Amneal Pharmaceuticals LLC Exhibit 1020 Page 4
5 Gerlach et al. Page 5 Although the cause is not known for certain, there are several possible mechanisms for development of dexmedetomidine-associated hypotension, especially in patients receiving rapid dosage titration. The first is an opposing effect on α 2a and α 2b receptors. Work by others has shown that heart rate, cardiac output, and norepinephrine concentrations decrease progressively with increasing dexmedetomidine concentrations, but dexmedetomidine causes a biphasic change in blood pressure [24]. At low concentrations (<1.9 ng/ml), mean arterial pressure decreases, followed by increasing mean arterial pressures observed with increasing dexmedetomidine concentrations [24]. It is thought that activation of peripheral α 2b -receptors at higher concentrations causes vasoconstriction, thereby offsetting the vasodilation from activation of α 2a -receptors. Critically ill patients receiving a maximum dosage of 0.7 μg kg 1 h 1 have demonstrated peak serum dexmedetomidine concentrations of 1.2 ng/ml with a range of ng/ml [25]. This is below the point where the activation of α 2b starts to predominate and may explain why hypotension is the most common adverse effect. A second possible mechanism contributing to hypotension induced by dexmedetomidine relates to its pharmaco-kinetic properties. Dexmedetomidine requires extensive metabolism by the liver but appears to have minimal interaction with the cytochrome p450 enzymes [10,11]. Dexmedetomidine exhibits linear pharmacokinetics with distribution (α) half-life range of 6.0 to 8.6 minutes and elimination (β) half-life of approximately 2 to 3.1 hours in both healthy volunteers and critically ill patients [10,11,25]. Thus, completion of distribution from the central to peripheral compartments requires approximately 30 to 45 minutes, whereas steady-state drug concentrations do not occur until approximately 10 to 15 hours. Rapid titration (sooner than every minutes) therefore provides additional drug before distribution of the previous dose is complete. This could therefore result in drug accumulation in the central compartment with development of hypotension after completion of distribution. There was a trend toward lower mean maximum dosage in the protocol group (0.43 ± 0.02 vs 0.54 ± 0.16 μg kg 1 h 1 ; P =.08). Because we did not measure dexmedetomidine serum concentrations, this remains a hypothesis consistent with our clinical data that can be tested in future studies. The optimal method to safely titrate dexmedetomidine in critically ill patients has not been definitively established, but available data support the practice of slower titration. Timing of dexmedetomidine titration has only been described in 2 studies of critically ill patients: one in adults and one in children [26,27]. In adult ICU patients receiving dexmedetomidine longer than 24 hours (median, 71.5 hours), dexmedetomidine was titrated no sooner than every 15 minutes [26]. Mean systolic blood pressures decreased approximately 16% within 2 to 4 hours of initiating therapy, and the lowest single systolic blood pressure was reported 12 hours after starting therapy. Beyond 12 hours (presumably at/near steady state), systolic blood pressures showed minimal change (± 10%) during dexmedetomidine infusion. In pediatric ICU patients (median age, 5 months) receiving dexmedetomidine without loading infusions titrated with changes more than 1 hour apart, there were no episodes of dexmedetomidine-associated hypotension [27]. One patient (6%) developed hypotension when dexmedetomidine was titrated less than 1 hour after the previous change. Thus, these studies taken together with the current study suggest that a slow titration may minimize the incidence of hypotension; once again, further studies are needed to confirm. The optimal dosage and dosing titration frequency that balance safety and efficacy are also unknown. Dexmedetomidine was approved for use in the United States, based on 2 randomized, double-blind, placebo-controlled trials with the maximum dosage of 0.7 μg kg 1 h 1 [9,16]. In our study, the maximum dosage of dexmedetomidine was also 0.7 μg kg 1 h 1, although many studies have reported higher dosages [9]. The revised labeling for procedures or surgery in nonintubated patients increases the maximal dosage to 1.0 μg kg 1 Amneal Pharmaceuticals LLC Exhibit 1020 Page 5
6 Gerlach et al. Page 6 h 1 [10]. In a phase II trial in 12 medical patients, Venn et al [28] have reported maximal dosages of 2.5 μg kg 1 h 1 after their first 4 patients required additional sedation. Pandharipande et al [17] compared sedation with dexmedetomidine or lorazepam in 106 critically ill patients and used a maximal dosage of dexmedetomidine of 1.5 μg kg 1 h 1. Hypotension, reported as a systolic blood pressure less than 80 mm Hg, occurred in 25% of those receiving dexmedetomidine and 20% of those receiving lorazepam (P =.51), but significantly more patients receiving dexmedetomidine developed bradycardia (17% vs 4%; P =.03). Riker et al [22] compared dexmedetomidine to midazolam in a randomized trial where 61% of 244 patients received between 0.71 and 1.4 μg kg 1 h 1 of dexmedetomidine. Significantly more patients receiving dexmedetomidine developed bradycardia compared with those receiving midazolam (42.2% vs 18.9%; P <.001), with similar incidence of hypotension (56.1% vs 55.7%; P >.99). In our study, rate of titration did not appear to influence incidence of bradycardia, but we used a lower maximum dosage and our sample size may be too small to detect a change. Further studies are needed to determine if dosages greater than 0.7 μg kg 1 h 1 are associated with a higher rate of hypotension or bradycardia. The time to hypotension and bradycardia was documented in only a few studies [16,18]. Venn et al [16] report 18 of 66 patients receiving dexmedetomidine after general or cardiac surgery developed hypotension and/or bradycardia. Most of these events (11/18) occurred with the loading infusion. The other 7 patients developed hypotension between 1 and 11 hours of initiation. Herr et al [18] reported that hypotension occurred in 24% of 148 patients receiving dexmedetomidine, and 8% developed hypotension within an hour and most during the loading infusion. In 20 critically ill patients, Shehabi et al [26] report that when dexmedetomidine is started without a loading infusion at 0.4 μg kg 1 h 1 and titrated to Ramsay Sedation Score between 2 and 4 for a median of 71.5 hours, mean systolic blood pressure dropped 16% within 2 hours then gradually stabilized. Heart rate decreased gradually over 12 hours by 21% with minimal changes thereafter. This is similar to our results where the mean time to hypotension was 3.9 hours compared to 9.7 hours for bradycardia. It could be that hypotension occurs sooner in critically ill patients than bradycardia, especially if the patients have intravascular volume depletion and are dependent on their adrenergic response, and this was not measured in our study. Use of the protocol did not seem to compromise sedation, but because there were not consistent time points mandated for sedation documentation, this comparison was not perfect. At initiation of therapy, the groups had comparable sedation levels with the median in each group reported as calm (RASS 0, Ramsay Sedation Score 2) (Table 3). Our best surrogates of later sedation were sedation scores around the time of adverse drug effects or need for additional sedation. Sedation scores were documented within 2 hours of the development of hypotension or bradycardia in all but 1 patient, and median scores were similar between the protocol and control groups (protocol group median RASS 1 [light sedation] vs control group median Ramsey sedation score 2 [calm]). Use of additional sedation was allowed in the protocol, but additional sedation was required in only 2 (8%) patients, which is consistent with other comparative studies [17,20,22]. Nonetheless, because the level of sedation was not documented during the occurrence of each adverse drug event, it is unknown if there was truly a difference in this retrospective review. Because of its retrospective nature, this study has several additional limitations. The results are hypothesis generating, and there is a potential for selection bias in our historical control group. Next, there were no predefined clinical criteria to insure that patients in each group had comparable volume status. It is also possible that protocol patients developed less hypotension because they received slightly less dexmedetomidine, but this question will require a larger sample size. Finally, we switched from using the Ramsay Sedation Scale to the Richmond Agitation Sedation Scale during the study period, and as mentioned, Amneal Pharmaceuticals LLC Exhibit 1020 Page 6
7 Gerlach et al. Page 7 5. Conclusions References frequency of documentation for sedation scores was variable between patients. Although we attempted to equate the 2 sedation scores by normalizing the values, this has not been tested. For these reasons, we feel that our results will need to be confirmed independently, taking care to address these issues. Dexmedetomidine is a sedative agent with several unique properties that make it attractive for use in critically ill patients. Although our initial experience demonstrated an unacceptably high incidence of hypotension, use of a dosing protocol was associated with significant reduction in hypotension incidence. Further prospective studies will be required to validate this protocol for use during critical illness and to determine the influence of preadministration volume status upon dexmedetomidine complications. 1. Kohn, LT.; Corrigan, JM.; Donaldson, MS., editors. To err is human: Building a safer health system. Washington. DC: National Academy Press; Hussain E, Kao E. Medication safety and transfusion errors in the ICU and beyond. Crit Care Clin. 2005; 21: [PubMed: ] 3. Pronovost P, Wu AW, Dorman T, Morlock L. Building safety into ICU care. J Crit Care. 2002; 17: [PubMed: ] 4. Calabrese AD, Erstad BL, Brandl K, Barletta J, Kane SL, Sherman D. Medication administration errors in adult patient in the intensive care unit. Intensive Care Med. 2001; 27(15): Cullen DJ, Sweitzer BJ, Bates DW, Burdick E, Edmondson A, Leape LL. Preventable adverse drug events in hospitalized patients: a comparison of intensive care and general care units. Crit Care Med. 1997; 25: [PubMed: ] 6. Kane-Gill SL, Weber RJ. Principles and practices of medication errors in the ICU. Crit Care Clin. 2006; 22: [PubMed: ] 7. Jacobi J, Fraser GL, Coursin DB, Riker RR, Fontaine D, Wittbrodt ET, et al. Clinical practice guidelines for the sustained use of sedatives and analgesics in the critically ill adult. Crit Care Med. 2002; 30: [PubMed: ] 8. Kollef MH, Levy NT, Ahrens TS, Schaiff R, Prentice D, Sherman G. The use of continuous i.v. sedation is associated with prolongation of mechanical ventilation. Chest. 1998; 114: [PubMed: ] 9. Gerlach AT, Dasta JF. Dexmedetomidine: an updated review. Ann Pharmacother. 2007; 41: [PubMed: ] 10. Product Information Precedex (dexmedetomidine). Lake Forrest, IL: Hospira; Bhana N, Goa KL, McClellan K. Dexmedetomidine Drugs. 2000; 59: Pandharipande PP, Ely EW, Maze M. Dexmedetomidine for sedation and perioperative management of critically ill patients. Semin Anesth Periop Med Pain. 2006; 25: Gerlach AT, Dasta JF, Martin LM, Cook CH. Effect of titration methods on adverse reactions to dexmedetomidine (abstr). Crit Care Med. 2005; 33:A Sessler CN, Gosnell MS, Grap MJ, Brophy GM, O Neal PV, Keane KA, et al. The Richmond Agitation-Sedation Scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002; 166: [PubMed: ] 15. Elbaradie S, El Mahalawy FH, Solyman AH. Dexmedetomidine versus propofol for short-term sedation of postoperative mechanically ventilated patients. J Egyptian Nat Cancer Inst. 2004; 16: Venn RM, Bradshaw CJ, Spencer R, Brealey D, Caudwell E, Naughton C, et al. Preliminary UK experience of dexmedetomidine, a novel agent for postoperative sedation in the intensive care unit. Anaesth. 1999; 54: Amneal Pharmaceuticals LLC Exhibit 1020 Page 7
8 Gerlach et al. Page Pandharipande PP, Pun BT, Herr DL, Maze M, Girard TG, Miller R, et al. Effect of sedation with dexmedetomidine vs lorazepam on acute brain dysfunction in mechanically ventilated patients. JAMA. 2007; 298: [PubMed: ] 18. Herr DL, Sum-Ping ST, England M. ICU sedation after coronary artery bypass surgery: dexmedetomidine-based versus propofol-based sedation regimens. J Cardiothor Vasc Anesth. 2003; 17: Venn RM, Grounds RM. Comparison between dexmedetomidine and propofol for sedation in the intensive care unit: patient and clinician perceptions. Br J Anaesth. 2001; 87: Corbett SM, Rebuck JA, Greene CM, Callas PW, Neale BW, Healey MA, et al. Dexmedetomidine does not improve patients satisfaction when compared to propofol during mechanical ventilation. Crit Care Med. 2005; 33: [PubMed: ] 21. Ickeringill M, Shehabi Y, Adamson H, Reuttimann U. Dexmedetomidine infusion without loading infusion in surgical patients requiring mechanical ventilation; hemodynamic effects and efficacy. Anaesth Intensive Care. 2004; 32: [PubMed: ] 22. Riker RR, Shehabi Y, Bokesch PM, Ceraso D, Wisemandle W, Koura F, et al. Dexmedetomidine vs midazolam for sedation of critically ill patients: a randomized trial. JAMA. 2009; 301: [PubMed: ] 23. Dasta JF, Kane-Gill SL, Durtschi AJ. Comparing dexmedetomidine prescribing patterns and safety in the naturalistic setting versus published data. Ann Pharmacother. 2004; 38: [PubMed: ] 24. Ebert TJ, Hall JE, Barney JA, Uhrich TD, Colinco MD. The effects of increasing plasma concentrations of dexmedetomidine in humans. Anesthesiology. 2000; 93: [PubMed: ] 25. Venn RM, Karol MD, Grounds RM. Pharmacokinetics of dexmedetomidine infusion for sedation of postoperative patients requiring intensive care. Br J Anesth. 2002; 88: Shehabi Y, Ruettimann U, Adamson H, Innes R, Ickeringill M. Dexmedetomidine infusion for more than 24 hours in critically ill patients: sedative and cardiovascular effects. Intensive Care Med. 2004; 30: [PubMed: ] 27. Buck ML, Willson DF. Use of dexmedetomidine in the pediatric intensive care unit. Pharmacotherapy. 2008; 28:51 7. [PubMed: ] 28. Venn RM, Newmann PJ, Grounds RM. A phase II study to evaluate the efficacy of dexmedetomidine for sedation in the medical intensive care units. Intensive Care Med. 2003; 29: [PubMed: ] Amneal Pharmaceuticals LLC Exhibit 1020 Page 8
9 Gerlach et al. Page 9 Fig. 1. Dexmedetomidine dosing protocol. Amneal Pharmaceuticals LLC Exhibit 1020 Page 9
10
11
12
13
A COMPARATIVE STUDY OF MIDAZOLAM, PROPOFOL AND DEXMEDETOMIDINE INFUSIONS FOR SEDATION IN ME- CHANICALLY VENTILATED PATIENTS IN ICU
 ORIGINAL ARTICLE A COMPARATIVE STUDY OF MIDAZOLAM, PROPOFOL AND DEXMEDETOMIDINE INFUSIONS FOR SEDATION IN ME- CHANICALLY VENTILATED PATIENTS IN ICU Suresh Chandra Dulara 1, Pooja Jangid 2, Ashish Kumar
ORIGINAL ARTICLE A COMPARATIVE STUDY OF MIDAZOLAM, PROPOFOL AND DEXMEDETOMIDINE INFUSIONS FOR SEDATION IN ME- CHANICALLY VENTILATED PATIENTS IN ICU Suresh Chandra Dulara 1, Pooja Jangid 2, Ashish Kumar
Susan Becker DNP, RN, CNS, CCRN, CCNS Marymount University, Arlington, VA
 Susan Becker DNP, RN, CNS, CCRN, CCNS Marymount University, Arlington, VA Disclosures Study and presentation has no commercial bias or interests No financial relationship with a commercial interest, products,
Susan Becker DNP, RN, CNS, CCRN, CCNS Marymount University, Arlington, VA Disclosures Study and presentation has no commercial bias or interests No financial relationship with a commercial interest, products,
Therapeutics and clinical risk management (2011) Vol.7:291~299. Dexmedetomidine hydrochloride as a long-term sedative.
 Therapeutics and clinical risk management (2011) Vol.7:291~299. Dexmedetomidine hydrochloride as a long-term sedative Kunisawa Takayuki Therapeutics and Clinical Risk Management open access to scientific
Therapeutics and clinical risk management (2011) Vol.7:291~299. Dexmedetomidine hydrochloride as a long-term sedative Kunisawa Takayuki Therapeutics and Clinical Risk Management open access to scientific
Comparison of dexmedetomidine and propofol in mechanically ventilated patients with sepsis: A pilot study
 Original article Comparison of dexmedetomidine and propofol in mechanically ventilated patients with sepsis: A pilot study Mark B. Sigler MD, Ebtesam A. Islam MD PhD, Kenneth M. Nugent MD Abstract Objective:
Original article Comparison of dexmedetomidine and propofol in mechanically ventilated patients with sepsis: A pilot study Mark B. Sigler MD, Ebtesam A. Islam MD PhD, Kenneth M. Nugent MD Abstract Objective:
Use of Dexmedetomidine for Sedation of Children Hospitalized in the Intensive Care Unit
 ORIGINAL RESEARCH Use of Dexmedetomidine for Sedation of Children Hospitalized in the Intensive Care Unit Christopher L. Carroll, MD 1 Diane Krieger, MSN, CPNP 1 Margaret Campbell, PharmD 2 Daniel G. Fisher,
ORIGINAL RESEARCH Use of Dexmedetomidine for Sedation of Children Hospitalized in the Intensive Care Unit Christopher L. Carroll, MD 1 Diane Krieger, MSN, CPNP 1 Margaret Campbell, PharmD 2 Daniel G. Fisher,
Propofol vs Dexmedetomidine
 Propofol vs Dexmedetomidine A highlight of similarities & differences Lama Nazer, PharmD, BCPS Critical Care Clinical Pharmacy Specialist King Hussein Cancer Center Outline Highlight similarities and differences
Propofol vs Dexmedetomidine A highlight of similarities & differences Lama Nazer, PharmD, BCPS Critical Care Clinical Pharmacy Specialist King Hussein Cancer Center Outline Highlight similarities and differences
DOI /yydb medetomidine a review of clinical applications J. Curr Opin Anaesthesiol
 1573 medetomidine a review of clinical applications J. Curr Opin Anaesthesiol 2008 21 4 457-461. 6 DAHMANI S PARIS A JANNIER V et al. Dexmedetom- 2. α 2 idine increases hippocampal phosphorylated extracellular
1573 medetomidine a review of clinical applications J. Curr Opin Anaesthesiol 2008 21 4 457-461. 6 DAHMANI S PARIS A JANNIER V et al. Dexmedetom- 2. α 2 idine increases hippocampal phosphorylated extracellular
Appendix: Outcomes when Using Adjunct Dexmedetomidine with Propofol Sedation in
 SUPPLEMENTAL CONTENT Appendix: Outcomes when Using Adjunct Dexmedetomidine with Propofol Sedation in Mechanically Ventilated Surgical Intensive Care Patients Table of Contents Methods Summary of Definitions
SUPPLEMENTAL CONTENT Appendix: Outcomes when Using Adjunct Dexmedetomidine with Propofol Sedation in Mechanically Ventilated Surgical Intensive Care Patients Table of Contents Methods Summary of Definitions
ASMIC 2016 DEXMEDETOMIDINE IN THE INTENSIVE CARE UNIT DR KHOO TIEN MENG
 ASMIC 2016 DEXMEDETOMIDINE IN THE INTENSIVE CARE UNIT DR KHOO TIEN MENG PREAMBLE : EVOLUTION OF SEDATION IN THE ICU 1980s : ICU sedation largely extension of GA No standard approach, highly variable Deep
ASMIC 2016 DEXMEDETOMIDINE IN THE INTENSIVE CARE UNIT DR KHOO TIEN MENG PREAMBLE : EVOLUTION OF SEDATION IN THE ICU 1980s : ICU sedation largely extension of GA No standard approach, highly variable Deep
Ashraf Darwish, Rehab Sami, Mona Raafat, Rashad Aref and Mohamed Hisham
 Dexmedetomidine versus Propofol for Monitored Anesthesia Care In Patients Undergoing Anterior Segment Ophthalmic Surgery Under Peribulbar Medial Canthus Anesthesia Ashraf Darwish, Rehab Sami, Mona Raafat,
Dexmedetomidine versus Propofol for Monitored Anesthesia Care In Patients Undergoing Anterior Segment Ophthalmic Surgery Under Peribulbar Medial Canthus Anesthesia Ashraf Darwish, Rehab Sami, Mona Raafat,
Disclosures. Dexmedetomidine: The Good, The Bad and The Delirious. The Delirious. Objectives. Characteristics of Delirium. Definition of Delirium
 Dexmedetomidine: The Good, The Bad and The Delirious Disclosures! I have no actual or potential conflict of interest in relation to this presentation. By John J. Bon, Pharm.D., BCPS Lead Clinical Pharmacist,
Dexmedetomidine: The Good, The Bad and The Delirious Disclosures! I have no actual or potential conflict of interest in relation to this presentation. By John J. Bon, Pharm.D., BCPS Lead Clinical Pharmacist,
Original Contributions
 Original Contributions Use of Dexmedetomidine to Facilitate Extubation in Surgical Intensive-Care-Unit Patients Who Failed Previous Weaning Attempts Following Prolonged Mechanical Ventilation: A Pilot
Original Contributions Use of Dexmedetomidine to Facilitate Extubation in Surgical Intensive-Care-Unit Patients Who Failed Previous Weaning Attempts Following Prolonged Mechanical Ventilation: A Pilot
Hemodynamic effects of dexmedetomidine-- fentanyl vs. nalbuphine--propofol in plastic surgery
 Hemodynamic effects of dexmedetomidine-- fentanyl vs. nalbuphine--propofol in plastic surgery Juan F. De la Mora-González *, José A. Robles-Cervantes 2,4, José M. Mora-Martínez 3, Francisco Barba-Alvarez
Hemodynamic effects of dexmedetomidine-- fentanyl vs. nalbuphine--propofol in plastic surgery Juan F. De la Mora-González *, José A. Robles-Cervantes 2,4, José M. Mora-Martínez 3, Francisco Barba-Alvarez
Clinical effectiveness of a sedation protocol minimizing benzodiazepine infusions and favoring early dexmedetomidine: A before-after study
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Clinical effectiveness of a sedation protocol minimizing benzodiazepine infusions and favoring early dexmedetomidine:
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Clinical effectiveness of a sedation protocol minimizing benzodiazepine infusions and favoring early dexmedetomidine:
Dexmedetomidine. Dr.G.K.Kumar,M.D.,D.A., Assistant Professor, Madras medical college,chennai. History
 Dexmedetomidine Dr.G.K.Kumar,M.D.,D.A., Assistant Professor, Madras medical college,chennai Dexmedetomidine is the most recently released IV anesthetic. It is a highly selective α 2 -adrenergic agonist
Dexmedetomidine Dr.G.K.Kumar,M.D.,D.A., Assistant Professor, Madras medical college,chennai Dexmedetomidine is the most recently released IV anesthetic. It is a highly selective α 2 -adrenergic agonist
Comparison of Intensive Care Unit Sedation Using Dexmedetomidine, Propofol, and Midazolam
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/24 Comparison of Intensive Care Unit Sedation Using Dexmedetomidine, Propofol, and Midazolam Gajendra Singh, Kakhandki
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/24 Comparison of Intensive Care Unit Sedation Using Dexmedetomidine, Propofol, and Midazolam Gajendra Singh, Kakhandki
Dexmedetomidine for Sedation in the Critical Care Setting: An Economic Assessment
 CADTH TECHNOLOGY REVIEW Dexmedetomidine for Sedation in the Critical Care Setting: An Economic Assessment Service Line: Technology Review Issue Number: 6 Version: 1.0 Publication Date: March 2017 Report
CADTH TECHNOLOGY REVIEW Dexmedetomidine for Sedation in the Critical Care Setting: An Economic Assessment Service Line: Technology Review Issue Number: 6 Version: 1.0 Publication Date: March 2017 Report
Period of study: 12 Nov 2002 to 08 Apr 2004 (first subject s first visit to last subject s last visit)
 Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Int J Clin Exp Med 2016;9(6): /ISSN: /IJCEM
 Int J Clin Exp Med 2016;9(6):9694-9704 www.ijcem.com /ISSN:1940-5901/IJCEM0024616 Review Article Evaluation of dexmedetomidine versus propofol sedation therapy in mechanically ventilated cardiac surgery
Int J Clin Exp Med 2016;9(6):9694-9704 www.ijcem.com /ISSN:1940-5901/IJCEM0024616 Review Article Evaluation of dexmedetomidine versus propofol sedation therapy in mechanically ventilated cardiac surgery
Department of Intensive Care Medicine, Austin Hospital and the University of Melbourne, 145 Studley Road, Heidelberg, Victoria, 3084, Australia
 Available online http://ccforum.com/content/13/3/r75 Vol 13 No 3 Research Open Access Dexmedetomidine vs. haloperidol in delirious, agitated, intubated patients: a randomised open-label trial Michael C
Available online http://ccforum.com/content/13/3/r75 Vol 13 No 3 Research Open Access Dexmedetomidine vs. haloperidol in delirious, agitated, intubated patients: a randomised open-label trial Michael C
Fujita et al. Journal of Intensive Care 2013, 1:15
 Fujita et al. Journal of Intensive Care 2013, 1:15 RESEARCH Open Access A comparison between dosages and plasma concentrations of dexmedetomidine in clinically ill patients: a prospective, observational,
Fujita et al. Journal of Intensive Care 2013, 1:15 RESEARCH Open Access A comparison between dosages and plasma concentrations of dexmedetomidine in clinically ill patients: a prospective, observational,
The evolving approach to sedation in ventilated patients: a real world perspective
 Editorial Page 1 of 5 The evolving approach to sedation in ventilated patients: a real world perspective Annachiara Marra 1,2, Pratik P. Pandharipande 3 1 Department of Medicine, Division of Allergy and
Editorial Page 1 of 5 The evolving approach to sedation in ventilated patients: a real world perspective Annachiara Marra 1,2, Pratik P. Pandharipande 3 1 Department of Medicine, Division of Allergy and
Evaluation of efficacy of sedative and analgesic effects of single IV dose of dexmedetomidine in post-operative patients
 www.ijpcs.net ABSTRACT Evaluation of efficacy of sedative and analgesic effects of single IV dose of dexmedetomidine in post-operative patients Manasa CR 1 *, Padma L 2, Shivshankar 3, Ranjani Ramanujam
www.ijpcs.net ABSTRACT Evaluation of efficacy of sedative and analgesic effects of single IV dose of dexmedetomidine in post-operative patients Manasa CR 1 *, Padma L 2, Shivshankar 3, Ranjani Ramanujam
RETRACTED. Dexmedetomidine infusion is associated with enhanced renal function after thoracic surgery
 Journal of Clinical Anesthesia (2006) 18, 422 426 Original contribution Dexmedetomidine infusion is associated with enhanced renal function after thoracic surgery Robert J. Frumento MS, MPH, Helene G.
Journal of Clinical Anesthesia (2006) 18, 422 426 Original contribution Dexmedetomidine infusion is associated with enhanced renal function after thoracic surgery Robert J. Frumento MS, MPH, Helene G.
Preliminary UK experience of dexmedetomidine, a novel agent for postoperative sedation in the intensive care unit
 Preliminary UK experience of dexmedetomidine, a novel agent for postoperative sedation in the intensive care unit R. M. Venn, 1 C. J. Bradshaw, 1 R. Spencer, 2 D. Brealey, 3 E. Caudwell, 3 C. Naughton,
Preliminary UK experience of dexmedetomidine, a novel agent for postoperative sedation in the intensive care unit R. M. Venn, 1 C. J. Bradshaw, 1 R. Spencer, 2 D. Brealey, 3 E. Caudwell, 3 C. Naughton,
Over the past 10 years, there has been an increase in
 Dexmedetomidine for Sedation During Noninvasive Ventilation in Pediatric Patients Rasika Venkatraman, MD 1 ; James L. Hungerford, MD 2,3 ; Mark W. Hall, MD 1 ; Melissa Moore-Clingenpeel, MS 1,4 ; Joseph
Dexmedetomidine for Sedation During Noninvasive Ventilation in Pediatric Patients Rasika Venkatraman, MD 1 ; James L. Hungerford, MD 2,3 ; Mark W. Hall, MD 1 ; Melissa Moore-Clingenpeel, MS 1,4 ; Joseph
Dexmedetomidine use in a pediatric cardiac intensive care unit: Can we use it in infants after cardiac surgery?
 Cardiac Intensive Care Dexmedetomidine use in a pediatric cardiac intensive care unit: Can we use it in infants after cardiac surgery? Constantinos Chrysostomou, MD; Joan Sanchez De Toledo, MD; Tracy Avolio,
Cardiac Intensive Care Dexmedetomidine use in a pediatric cardiac intensive care unit: Can we use it in infants after cardiac surgery? Constantinos Chrysostomou, MD; Joan Sanchez De Toledo, MD; Tracy Avolio,
Associate Professor, Department of Anaesthesiology, Government Thoothukudi Medical College, Thoothukudi, Tamil Nadu, India, 2
 Original Article DOI: 10.17354/ijss/2016/295 Effect of Intravenous use of Dexmedetomidine on Anesthetic Requirements in Patients Undergoing Elective Spine Surgery: A Double Blinded Randomized Controlled
Original Article DOI: 10.17354/ijss/2016/295 Effect of Intravenous use of Dexmedetomidine on Anesthetic Requirements in Patients Undergoing Elective Spine Surgery: A Double Blinded Randomized Controlled
Corresponding author: V. Dua, Department of Anaesthesia, BJ Wadia Hospital for Children, Parel, Mumbai, India.
 Comparative evaluation of dexmedetomidine as a premedication given intranasally vs orally in children between 1 to 8 years of age undergoing minor surgical procedures V. Dua, P. Sawant, P. Bhadlikar Department
Comparative evaluation of dexmedetomidine as a premedication given intranasally vs orally in children between 1 to 8 years of age undergoing minor surgical procedures V. Dua, P. Sawant, P. Bhadlikar Department
Study the Effect of Dexmedetomidine on Emergence Agitation after Nasal Surgeries
 Original Research Article Study the Effect of Dexmedetomidine on Emergence Agitation after Nasal Surgeries G V Krishna Reddy 1*, S. Kuldeep 2, G. Obulesu 3 1 Assistant Professor, Department of Anaesthesiology,
Original Research Article Study the Effect of Dexmedetomidine on Emergence Agitation after Nasal Surgeries G V Krishna Reddy 1*, S. Kuldeep 2, G. Obulesu 3 1 Assistant Professor, Department of Anaesthesiology,
Cefazolin vs. Antistaphyloccal Penicillins: The Great Debate
 Cefazolin vs. Antistaphyloccal Penicillins: The Great Debate Annie Heble, PharmD PGY2 Pediatric Pharmacy Resident Children s Hospital Colorado Microbiology Rounds March 22, 2017 Image Source: Buck cartoons
Cefazolin vs. Antistaphyloccal Penicillins: The Great Debate Annie Heble, PharmD PGY2 Pediatric Pharmacy Resident Children s Hospital Colorado Microbiology Rounds March 22, 2017 Image Source: Buck cartoons
Pain Management in Racing Greyhounds
 Pain Management in Racing Greyhounds Pain Pain is a syndrome consisting of multiple organ system responses, and if left untreated will contribute to patient morbidity and mortality. Greyhounds incur a
Pain Management in Racing Greyhounds Pain Pain is a syndrome consisting of multiple organ system responses, and if left untreated will contribute to patient morbidity and mortality. Greyhounds incur a
Quality of MRI pediatric sedation: Comparison between intramuscular and intravenous dexmedetomidine
 Egyptian Journal of Anaesthesia (2013) 29, 47 52 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Quality of MRI
Egyptian Journal of Anaesthesia (2013) 29, 47 52 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Quality of MRI
1. NAME AND ADDRESS OF THE MARKETING AUTHORISATION HOLDER AND OF THE MANUFACTURING AUTHORISATION HOLDER RESPONSIBLE FOR BATCH RELEASE, IF DIFFERENT
 PACKAGE LEAFLET FOR: Dormilan solution for injection for dogs and cats [FR] Dormilan 1 mg/ml solution for injection for dogs and cats [DE, PT, UK] Reanest 1 mg/ml solution for injection for dogs and cats
PACKAGE LEAFLET FOR: Dormilan solution for injection for dogs and cats [FR] Dormilan 1 mg/ml solution for injection for dogs and cats [DE, PT, UK] Reanest 1 mg/ml solution for injection for dogs and cats
SCIENTIFIC COOPERATIONS MEDICAL WORKSHOPS July, 2015, Istanbul - TURKEY
 21-22 July, 2015, Istanbul - TURKEY PROSPECTIVE EVALUATION OF CORRELATION OF DEPTH OF DEXMEDETOMIDINE SEDATION AND CLINICAL EFFECTS FOR RECONSTRUCTIVE SURGERIES UNDER REGIONAL ANAESTHESIA Alma Jaunmuktane
21-22 July, 2015, Istanbul - TURKEY PROSPECTIVE EVALUATION OF CORRELATION OF DEPTH OF DEXMEDETOMIDINE SEDATION AND CLINICAL EFFECTS FOR RECONSTRUCTIVE SURGERIES UNDER REGIONAL ANAESTHESIA Alma Jaunmuktane
The Addition of Dexmedetomidine as an Adjunctive Therapy to Benzodiazepine Use in Alcohol Withdrawal Syndrome
 Original Article Journal of Addictions Nursing & Volume 28 & Number 4, 188Y195 & Copyright B 2017 International Nurses Society on Addictions The Addition of Dexmedetomidine as an Adjunctive Therapy to
Original Article Journal of Addictions Nursing & Volume 28 & Number 4, 188Y195 & Copyright B 2017 International Nurses Society on Addictions The Addition of Dexmedetomidine as an Adjunctive Therapy to
Safety and Efficacy of Dexmedetomidine, Ketofol, and Propofol for Sedation of Mechanically Ventilated Patients
 Research Article imedpub Journals http://www.imedpub.com Journal of Intensive and Critical Care ISSN 2471-8505 DOI: 10.21767/2471-8505.100118 Abstract Safety and Efficacy of Dexmedetomidine, Ketofol, and
Research Article imedpub Journals http://www.imedpub.com Journal of Intensive and Critical Care ISSN 2471-8505 DOI: 10.21767/2471-8505.100118 Abstract Safety and Efficacy of Dexmedetomidine, Ketofol, and
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Sun, 10 Mar 2019 06:52:14 GMT) CTRI Number Last Modified On 29/07/2016 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Clinical Trial Details (PDF Generation Date :- Sun, 10 Mar 2019 06:52:14 GMT) CTRI Number Last Modified On 29/07/2016 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Comparative Study of Dexmedetomidine and Propofol for Intraoperative Sedation During Surgery Under Regional Anaesthesia
 Original Research Article Comparative Study of Dexmedetomidine and Propofol for Intraoperative Sedation During Surgery Under Regional Anaesthesia Ankita Gupta 1, V.K. Parashar 2, Ankur Gupta 3 1Resident,
Original Research Article Comparative Study of Dexmedetomidine and Propofol for Intraoperative Sedation During Surgery Under Regional Anaesthesia Ankita Gupta 1, V.K. Parashar 2, Ankur Gupta 3 1Resident,
Comparison of several dosing schedules of intravenous dexmedetomidine in elderly patients under spinal anesthesia
 Anesth Pain Med 2017;12:320-325 https://doi.org/10.17085/apm.2017.12.4.320 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received January 11, 2017 Revised 1st, February 28, 2017 2nd, April 4, 2017
Anesth Pain Med 2017;12:320-325 https://doi.org/10.17085/apm.2017.12.4.320 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received January 11, 2017 Revised 1st, February 28, 2017 2nd, April 4, 2017
ISMP Canada HYDROmorphone Knowledge Assessment Survey
 ISMP Canada HYDROmorphone Knowledge Assessment Survey Knowledge Assessment Questions 1. In an equipotent dose, HYDROmorphone is more potent than morphine. True False Unsure 2. HYDROmorphone can be given
ISMP Canada HYDROmorphone Knowledge Assessment Survey Knowledge Assessment Questions 1. In an equipotent dose, HYDROmorphone is more potent than morphine. True False Unsure 2. HYDROmorphone can be given
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE VETERINARY MEDICINAL PRODUCT Medeson 1 mg/ml solution for injection for dogs and cats [AT, CY, CZ, DE, EL, ES, HR, IT, LT, LV, PL, PT, RO, SI, SK] Medeson,
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE VETERINARY MEDICINAL PRODUCT Medeson 1 mg/ml solution for injection for dogs and cats [AT, CY, CZ, DE, EL, ES, HR, IT, LT, LV, PL, PT, RO, SI, SK] Medeson,
Sustaining an Antimicrobial Stewardship
 Sustaining an Antimicrobial Stewardship Much needless expense, untoward effect, harm and disappointment can be prevented by better judgment in the use of antimicrobials Whitney A. Jones, PharmD Antimicrobial
Sustaining an Antimicrobial Stewardship Much needless expense, untoward effect, harm and disappointment can be prevented by better judgment in the use of antimicrobials Whitney A. Jones, PharmD Antimicrobial
MAGNITUDE OF ANTIMICROBIAL USE. Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges
 Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control
Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control
What dose of methadone should I use?
 What dose of methadone should I use? Professor Derek Flaherty BVMS, DVA, DipECVAA, MRCA, MRCVS RCVS and European Specialist in Veterinary Anaesthesia SPC dose rates for Comfortan dogs: 0.5-1.0 mg/kg SC,
What dose of methadone should I use? Professor Derek Flaherty BVMS, DVA, DipECVAA, MRCA, MRCVS RCVS and European Specialist in Veterinary Anaesthesia SPC dose rates for Comfortan dogs: 0.5-1.0 mg/kg SC,
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE VETERINARY MEDICINAL PRODUCT Dormilan solution for injection for dogs and cats [FR] Dormilan 1 mg/ml solution for injection for dogs and cats [DE, ES,
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE VETERINARY MEDICINAL PRODUCT Dormilan solution for injection for dogs and cats [FR] Dormilan 1 mg/ml solution for injection for dogs and cats [DE, ES,
Premedication with alpha-2 agonists procedures for monitoring anaesthetic
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Premedication with alpha-2 agonists procedures for monitoring anaesthetic Author : Lisa Angell, Chris Seymour Categories :
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Premedication with alpha-2 agonists procedures for monitoring anaesthetic Author : Lisa Angell, Chris Seymour Categories :
A cost-minimization analysis of dexmedetomidine compared with midazolam for long-term sedation in the intensive care unit*
 A cost-minimization analysis of dexmedetomidine compared with midazolam for long-term sedation in the intensive care unit* Joseph F. Dasta, MSc, FCCM, FCCP; Sandra L. Kane-Gill, PharmD, MSc, FCCM, FCCP;
A cost-minimization analysis of dexmedetomidine compared with midazolam for long-term sedation in the intensive care unit* Joseph F. Dasta, MSc, FCCM, FCCP; Sandra L. Kane-Gill, PharmD, MSc, FCCM, FCCP;
Prophylactic antibiotic timing and dosage. Dr. Sanjeev Singh AIMS, Kochi
 Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
PATIENTS in intensive care units (ICUs) may experience
 CRITICAL CARE MEDICINE Anesthesiology 2010; 113:386 94 Copyright 2010, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins in the Care of Critically Ill Patients from 2001 to
CRITICAL CARE MEDICINE Anesthesiology 2010; 113:386 94 Copyright 2010, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins in the Care of Critically Ill Patients from 2001 to
11/22/2016. Antimicrobial Stewardship Update Disclosures. Outline. No conflicts of interest to disclose
 Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM
 UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
A Clinical Study of Dexmedetomidine under Combined Spinal Epidural Anaesthesia at a Tertiary Care Hospital
 Original Research A Clinical Study of Dexmedetomidine under Combined Spinal Epidural Anaesthesia at a Tertiary Care Hospital Kamala GR 1, Leela GR 2 1 Assistant Professor, Department of Anaesthesiology,
Original Research A Clinical Study of Dexmedetomidine under Combined Spinal Epidural Anaesthesia at a Tertiary Care Hospital Kamala GR 1, Leela GR 2 1 Assistant Professor, Department of Anaesthesiology,
Safety and efficacy of dexmedetomidine for long-term sedation in critically ill patients
 J Anesth (2014) 28:38 50 DOI 10.1007/s00540-013-1678-5 ORIGINAL ARTICLE Safety and efficacy of dexmedetomidine for long-term sedation in critically ill patients Makoto Ozaki Junzo Takeda Keiji Tanaka Yasuhiro
J Anesth (2014) 28:38 50 DOI 10.1007/s00540-013-1678-5 ORIGINAL ARTICLE Safety and efficacy of dexmedetomidine for long-term sedation in critically ill patients Makoto Ozaki Junzo Takeda Keiji Tanaka Yasuhiro
TITLE: Dexmedetomidine for Sedation in the ICU or PICU: A Review of Cost- Effectiveness and Guidelines
 TITLE: Dexmedetomidine for Sedation in the ICU or PICU: A Review of Cost- Effectiveness and Guidelines DATE: 17 December 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential for ICU
TITLE: Dexmedetomidine for Sedation in the ICU or PICU: A Review of Cost- Effectiveness and Guidelines DATE: 17 December 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential for ICU
Original Article Effects of low dose midazolam on bradycardia and sedation during dexmedetomidine infusion
 Int J Clin Exp Med 2016;9(6):11838-11844 www.ijcem.com /ISSN:1940-5901/IJCEM0020616 Original Article Effects of low dose midazolam on bradycardia and sedation during dexmedetomidine infusion Yun-Sic Bang
Int J Clin Exp Med 2016;9(6):11838-11844 www.ijcem.com /ISSN:1940-5901/IJCEM0020616 Original Article Effects of low dose midazolam on bradycardia and sedation during dexmedetomidine infusion Yun-Sic Bang
Alfaxan. (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. TECHNICAL NOTES DESCRIPTION INDICATIONS
 Alfaxan (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. NADA 141-342, Approved by FDA ALFAXAN (Schedule: C-IV) (alfaxalone 10 mg/ml) Intravenous injectable anesthetic
Alfaxan (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. NADA 141-342, Approved by FDA ALFAXAN (Schedule: C-IV) (alfaxalone 10 mg/ml) Intravenous injectable anesthetic
Suitability of Antibiotic Treatment for CAP (CAPTIME) The duration of antibiotic treatment in community acquired pneumonia (CAP)
 STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
Highly variable pharmacokinetics of dexmedetomidine during intensive care: a case report
 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Highly variable pharmacokinetics of dexmedetomidine during intensive care: a case report Timo Iirola 1*, Ruut Laitio 1, Erkki Kentala 1, Riku Aantaa
JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Highly variable pharmacokinetics of dexmedetomidine during intensive care: a case report Timo Iirola 1*, Ruut Laitio 1, Erkki Kentala 1, Riku Aantaa
Haemodynamic and anaesthetic advantages of dexmedetomidine
 Haemodynamic and anaesthetic advantages of dexmedetomidine Abstract Rao SH, Assistant Professor Sudhakar B, Associate Professor Subramanyam PK, Professor Department of Anaesthesia and Critical Care, Dr
Haemodynamic and anaesthetic advantages of dexmedetomidine Abstract Rao SH, Assistant Professor Sudhakar B, Associate Professor Subramanyam PK, Professor Department of Anaesthesia and Critical Care, Dr
Antibiotic Prophylaxis in Spinal Surgery Antibiotic Guidelines. Contents
 Antibiotic Prophylaxis in Spinal Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine Unique
Antibiotic Prophylaxis in Spinal Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine Unique
Objectives 4/26/2017. Co-Investigators Sadie Giuliani, PharmD, BCPS Claude Tonnerre, MD Jayme Hartzell, PharmD, MS, BCPS
 IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources
 Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Jump Starting Antimicrobial Stewardship
 Jump Starting Antimicrobial Stewardship Amanda C. Hansen, PharmD Pharmacy Operations Manager Carilion Roanoke Memorial Hospital Roanoke, Virginia March 16, 2011 Objectives Discuss guidelines for developing
Jump Starting Antimicrobial Stewardship Amanda C. Hansen, PharmD Pharmacy Operations Manager Carilion Roanoke Memorial Hospital Roanoke, Virginia March 16, 2011 Objectives Discuss guidelines for developing
Curricular Components for Infectious Diseases EPA
 Curricular Components for Infectious Diseases EPA 1. EPA Title Promoting antimicrobial stewardship based on microbiological principles 2. Description of the A key role for subspecialists is to utilize
Curricular Components for Infectious Diseases EPA 1. EPA Title Promoting antimicrobial stewardship based on microbiological principles 2. Description of the A key role for subspecialists is to utilize
Current Strategies In ICU Sedation
 This Special Report is supported through an unrestricted educational grant from BROUGHT TO YOU BY THE PUBLISHERS OF CME ACCREDITED MARCH 2001 Current Strategies In ICU Sedation OBJECTIVES After completing
This Special Report is supported through an unrestricted educational grant from BROUGHT TO YOU BY THE PUBLISHERS OF CME ACCREDITED MARCH 2001 Current Strategies In ICU Sedation OBJECTIVES After completing
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings. Carlos Reyes Sacin, MD, AAHIVS
 Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Providing Constant Analgesia with OROS Ò Hydromorphone
 Vol. 33 No. 2S February 2007 Journal of Pain and Symptom Management S19 Advances in the Long-Term Management of Chronic Pain: Recent Evidence with OROS Ò Hydromorphone, a Novel, Once-Daily, Long-Acting
Vol. 33 No. 2S February 2007 Journal of Pain and Symptom Management S19 Advances in the Long-Term Management of Chronic Pain: Recent Evidence with OROS Ò Hydromorphone, a Novel, Once-Daily, Long-Acting
IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP)
 IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
IMPLEMENTATION AND ASSESSMENT OF A GUIDELINE-BASED TREATMENT ALGORITHM FOR COMMUNITY-ACQUIRED PNEUMONIA (CAP) Lucas Schonsberg, PharmD PGY-1 Pharmacy Practice Resident Providence St. Patrick Hospital Missoula,
DETERMINANTS OF TARGET NON- ATTAINMENT IN CRITICALLY ILL PATIENTS RECEIVING β-lactams
 DETERMINANTS OF TARGET NON- ATTAINMENT IN CRITICALLY ILL PATIENTS RECEIVING β-lactams Jan J. De Waele MD PhD Surgical ICU Ghent University Hospital Ghent, Belgium Disclosures Financial: consultancy for
DETERMINANTS OF TARGET NON- ATTAINMENT IN CRITICALLY ILL PATIENTS RECEIVING β-lactams Jan J. De Waele MD PhD Surgical ICU Ghent University Hospital Ghent, Belgium Disclosures Financial: consultancy for
Antimicrobial Stewardship in the Hospital Setting
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
TITLE: Dexmedetomidine for Sedation of Patients in the ICU or PICU: Review of Clinical Effectiveness and Safety
 TITLE: Dexmedetomidine for Sedation of Patients in the ICU or PICU: Review of Clinical Effectiveness and Safety DATE: 16 January 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential
TITLE: Dexmedetomidine for Sedation of Patients in the ICU or PICU: Review of Clinical Effectiveness and Safety DATE: 16 January 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential
Dexmedetomidine vs. Propofol for Short-Term Sedation of Postoperative Mechanically Ventilated Patients
 Journal of the Egyptian Nat. Cancer Inst., Vol. 16, No. 3, September: 153-158, 2004 Dexmedetomidine vs. for Short-Term Sedation of Postoperative Mechanically Ventilated Patients SAMIA ELBARADIE, M.D.*;
Journal of the Egyptian Nat. Cancer Inst., Vol. 16, No. 3, September: 153-158, 2004 Dexmedetomidine vs. for Short-Term Sedation of Postoperative Mechanically Ventilated Patients SAMIA ELBARADIE, M.D.*;
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies
 ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
Bugs, Drugs, and No More Shoulder Shrugs: The Role for Antimicrobial Stewardship in Long-term Care
 Bugs, Drugs, and No More Shoulder Shrugs: The Role for Antimicrobial Stewardship in Long-term Care Molly Curran, PharmD, BCPS Clinical Assistant Professor The University of Texas College of Pharmacy Clinical
Bugs, Drugs, and No More Shoulder Shrugs: The Role for Antimicrobial Stewardship in Long-term Care Molly Curran, PharmD, BCPS Clinical Assistant Professor The University of Texas College of Pharmacy Clinical
Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities
 Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities Introduction As the problem of antibiotic resistance continues to worsen in all healthcare setting, we
Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities Introduction As the problem of antibiotic resistance continues to worsen in all healthcare setting, we
Pharmacokinetics of dexmedetomidine infusions for sedation of postoperative patients requiring intensive care ²
 British Journal of Anaesthesia 88 (5): 669±75 (2002) Pharmacokinetics of dexmedetomidine infusions for sedation of postoperative patients requiring intensive care ² R. M. Venn 1*, M. D. Karol 2 and R.
British Journal of Anaesthesia 88 (5): 669±75 (2002) Pharmacokinetics of dexmedetomidine infusions for sedation of postoperative patients requiring intensive care ² R. M. Venn 1*, M. D. Karol 2 and R.
DISSOCIATIVE ANESTHESIA
 DISSOCIATIVE ANESTHESIA Adarsh Kumar Dissociative anesthesia implies dissociation from the surrounding with only superficial sleep mediated by interruption of neuronal transmission from unconscious to
DISSOCIATIVE ANESTHESIA Adarsh Kumar Dissociative anesthesia implies dissociation from the surrounding with only superficial sleep mediated by interruption of neuronal transmission from unconscious to
A randomized control study of dexmedetomidine versus fentanyl as an anesthetic adjuvant in supratentorial craniotomies
 ORIGINAL ARTICLE ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com A randomized control study of dexmedetomidine versus fentanyl as an anesthetic adjuvant in supratentorial craniotomies Amrita Gupta,
ORIGINAL ARTICLE ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com A randomized control study of dexmedetomidine versus fentanyl as an anesthetic adjuvant in supratentorial craniotomies Amrita Gupta,
SUMMARY OF PRODUCT CHARACTERISTICS. Narcostart 1 mg/ml solution for injection for cats and dogs (NL, AT, BE, CZ, EL, HU, IS, LU, PL, SK)
 SUMMARY OF PRODUCT CHARACTERISTICS Revised: September 2015 1. NAME OF THE VETERINARY MEDICINAL PRODUCT Narcostart 1 mg/ml solution for injection for cats and dogs (NL, AT, BE, CZ, EL, HU, IS, LU, PL, SK)
SUMMARY OF PRODUCT CHARACTERISTICS Revised: September 2015 1. NAME OF THE VETERINARY MEDICINAL PRODUCT Narcostart 1 mg/ml solution for injection for cats and dogs (NL, AT, BE, CZ, EL, HU, IS, LU, PL, SK)
Case Report Dexmedetomidine as a Procedural Sedative for Percutaneous Tracheotomy: Case Report and Systematic Literature Review
 Case Reports in Critical Care Volume 2012, Article ID 659415, 4 pages doi:10.1155/2012/659415 Case Report Dexmedetomidine as a Procedural Sedative for Percutaneous Tracheotomy: Case Report and Systematic
Case Reports in Critical Care Volume 2012, Article ID 659415, 4 pages doi:10.1155/2012/659415 Case Report Dexmedetomidine as a Procedural Sedative for Percutaneous Tracheotomy: Case Report and Systematic
MEASURING ANTIBIOTIC USE IN LTCFS
 MEASURING ANTIBIOTIC USE IN LTCFS ELIZABETH DODDS ASHLEY, PHARMD, MHS LIAISON CLINICAL PHARMACIST ASSOCIATE PROFESSOR OF MEDICINE Objectives - Compare and contrast advantages and disadvantages to various
MEASURING ANTIBIOTIC USE IN LTCFS ELIZABETH DODDS ASHLEY, PHARMD, MHS LIAISON CLINICAL PHARMACIST ASSOCIATE PROFESSOR OF MEDICINE Objectives - Compare and contrast advantages and disadvantages to various
Dr. Omar S. Tabbouche, M.Sc, D.Sc, Pharm.D Head of Pharmacy Department New Mazloum Hospital Tripoli, Lebanon
 Efficacy & Safety of Ketoprofen 25mg vs. Paracetamol 1g intravenous preparations in the management of fever in adults: A pilot, double-blind, parallel-group, randomized controlled trial Dr. Omar S. Tabbouche,
Efficacy & Safety of Ketoprofen 25mg vs. Paracetamol 1g intravenous preparations in the management of fever in adults: A pilot, double-blind, parallel-group, randomized controlled trial Dr. Omar S. Tabbouche,
Antibiotic Stewardship Beyond Hospital Walls
 Antibiotic Stewardship Beyond Hospital Walls Katie Burenheide Foster, PharmD, MS, BCPS, FCCM Pharmacy Clinical Manager & PGY1 Pharmacy Residency Director OBJECTIVES 1. Review what Antibiotic Stewardship
Antibiotic Stewardship Beyond Hospital Walls Katie Burenheide Foster, PharmD, MS, BCPS, FCCM Pharmacy Clinical Manager & PGY1 Pharmacy Residency Director OBJECTIVES 1. Review what Antibiotic Stewardship
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus
 Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Efficacy of dexmedetomidine in reducing postoperative morphine consumption in patients undergoing total abdominal hysterectomy
 Original Article Brunei Int Med J. 2016; 12 (3): 97-103 Efficacy of dexmedetomidine in reducing postoperative morphine consumption in patients undergoing total abdominal hysterectomy Mazlilah ABDUL MALEK
Original Article Brunei Int Med J. 2016; 12 (3): 97-103 Efficacy of dexmedetomidine in reducing postoperative morphine consumption in patients undergoing total abdominal hysterectomy Mazlilah ABDUL MALEK
Endovascular Aortic Repair under the Monitored Anesthesia Care with Dexmedetomidine without Local Anesthesia: A Retrospective Study
 ARC Journal of Anesthesiology Volume 1, Issue 4, 2016, PP 4-10 ISSN No. 2455-9792 (Online) http://dx.doi.org/10.20431/2455-9792.0104002 www.arcjournals.org Endovascular Aortic Repair under the Monitored
ARC Journal of Anesthesiology Volume 1, Issue 4, 2016, PP 4-10 ISSN No. 2455-9792 (Online) http://dx.doi.org/10.20431/2455-9792.0104002 www.arcjournals.org Endovascular Aortic Repair under the Monitored
Dexmedetomidine for prevention of delirium in elderly patients after non-cardiac surgery: a randomised, double-blind, placebo-controlled trial
 Dexmedetomidine for prevention of delirium in elderly patients after non-cardiac surgery: a randomised, double-blind, placebo-controlled trial Xian Su, Zhao-Ting Meng, Xin-Hai Wu, Fan Cui, Hong-Liang Li,
Dexmedetomidine for prevention of delirium in elderly patients after non-cardiac surgery: a randomised, double-blind, placebo-controlled trial Xian Su, Zhao-Ting Meng, Xin-Hai Wu, Fan Cui, Hong-Liang Li,
Study between clonidine and dexmedetomidine in attenuation of pressor response during endotracheal intubation
 Original Research Article Study between clonidine and dexmedetomidine in attenuation of pressor response during endotracheal intubation K. Selvarju 1, Kondreddi Narayana Prasad 2*, Ajay Kumar Reddy Bobba
Original Research Article Study between clonidine and dexmedetomidine in attenuation of pressor response during endotracheal intubation K. Selvarju 1, Kondreddi Narayana Prasad 2*, Ajay Kumar Reddy Bobba
Introduction to Pharmacokinetics and Pharmacodynamics
 Introduction to Pharmacokinetics and Pharmacodynamics Diane M. Cappelletty, Pharm.D. Assistant Professor of Pharmacy Practice Wayne State University August, 2001 Vocabulary Clearance Renal elimination:
Introduction to Pharmacokinetics and Pharmacodynamics Diane M. Cappelletty, Pharm.D. Assistant Professor of Pharmacy Practice Wayne State University August, 2001 Vocabulary Clearance Renal elimination:
Synopsis. Takeda Pharmaceutical Company Limited Name of the finished product UNISIA Combination Tablets LD, UNISIA Combination Tablets
 Synopsis Name of the sponsor Takeda Pharmaceutical Company Limited Name of the finished product UNISIA Combination Tablets LD, UNISIA Combination Tablets Name of active ingredient Title of the study Study
Synopsis Name of the sponsor Takeda Pharmaceutical Company Limited Name of the finished product UNISIA Combination Tablets LD, UNISIA Combination Tablets Name of active ingredient Title of the study Study
Incidence of hospital-acquired Clostridium difficile infection in patients at risk
 Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 5-20-2016 Incidence of hospital-acquired Clostridium difficile infection in patients at risk Christine Ibarra
Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 5-20-2016 Incidence of hospital-acquired Clostridium difficile infection in patients at risk Christine Ibarra
DATA COLLECTION SECTION BY FRONTLINE TEAM. Patient Identifier/ Medical Record number (for facility use only)
 Assessment of Appropriateness of ICU Antibiotics (Patient Level Sheet) **Note this is intended for internal purposes only. Please do not return to PQC.** For this assessment, inappropriate antibiotic use
Assessment of Appropriateness of ICU Antibiotics (Patient Level Sheet) **Note this is intended for internal purposes only. Please do not return to PQC.** For this assessment, inappropriate antibiotic use
Pharmacoeconomic analysis of selected antibiotics in lower respiratory tract infection Quenzer R W, Pettit K G, Arnold R J, Kaniecki D J
 Pharmacoeconomic analysis of selected antibiotics in lower respiratory tract infection Quenzer R W, Pettit K G, Arnold R J, Kaniecki D J Record Status This is a critical abstract of an economic evaluation
Pharmacoeconomic analysis of selected antibiotics in lower respiratory tract infection Quenzer R W, Pettit K G, Arnold R J, Kaniecki D J Record Status This is a critical abstract of an economic evaluation
Pharmacokinetic & Pharmadynamic of Once Daily Aminoglycosides (ODA) and their Monitoring. Janis Chan Pharmacist, UCH 2008
 Pharmacokinetic & Pharmadynamic of Once Daily Aminoglycosides (ODA) and their Monitoring Janis Chan Pharmacist, UCH 25-4-2008 2008 Aminoglycosides (AG) 1. Gentamicin 2. Amikacin 3. Streptomycin 4. Neomycin
Pharmacokinetic & Pharmadynamic of Once Daily Aminoglycosides (ODA) and their Monitoring Janis Chan Pharmacist, UCH 25-4-2008 2008 Aminoglycosides (AG) 1. Gentamicin 2. Amikacin 3. Streptomycin 4. Neomycin
Study of Dexmedetomidine as intramuscular premedication in outpatient cataract surgery: A placebo controlled study
 Original Research Article Study of Dexmedetomidine as intramuscular premedication in outpatient cataract surgery: A placebo controlled study D. Srinivasa Naik 1, K. Ravi Kumar 1, Surendra Babu 2, R. Pandu
Original Research Article Study of Dexmedetomidine as intramuscular premedication in outpatient cataract surgery: A placebo controlled study D. Srinivasa Naik 1, K. Ravi Kumar 1, Surendra Babu 2, R. Pandu
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Invasive and noninvasive procedures
 Feature Review Article Dexmedetomidine and ketamine: An effective alternative for procedural sedation? Joseph D. Tobias, MD Objectives: Although generally effective for sedation during noninvasive procedures,
Feature Review Article Dexmedetomidine and ketamine: An effective alternative for procedural sedation? Joseph D. Tobias, MD Objectives: Although generally effective for sedation during noninvasive procedures,
