Trends in Prescribing -Lactam Antibiotics for Treatment of Community-Associated Methicillin-Resistant Staphylococcus aureus Infections
|
|
|
- Ada McCoy
- 5 years ago
- Views:
Transcription
1 JOURNAL OF CLINICAL MICROBIOLOGY, Dec. 2007, p Vol. 45, No /07/$ doi: /jcm Copyright 2007, American Society for Microbiology. All Rights Reserved. Trends in Prescribing -Lactam Antibiotics for Treatment of Community-Associated Methicillin-Resistant Staphylococcus aureus Infections Kalpana Gupta, 1,2 * Ann MacIntyre, 2,4 Gary Vanasse, 3 and Louise-Marie Dembry 2,4 Department of Medicine, VA Connecticut Health Care System, West Haven, Connecticut, 1 and Sections of Infectious Diseases 2 and Hematology, 3 Department of Medicine, Yale University School of Medicine, and Quality Improvement Support Services Department, Yale-New Haven Hospital, 4 New Haven, Connecticut Received 27 July 2007/Returned for modification 21 September 2007/Accepted 10 October 2007 Rates of prescribing of -lactam antibiotics as initial empirical therapy for patients with skin and soft tissue infections (SSTIs) caused by molecularly and epidemiologically characterized community-associated methicillin-resistant Staphylococcus aureus (CA-MRSA) isolates were assessed over a 3-year period. A prospectively developed database was used to calculate the prevalence of CA-MRSA SSTIs from 2004 to Molecular characterization of the MRSA isolate and medical record review for assessment of initial antimicrobial therapy were performed on a subset of patients. Among 2,636 patients with S. aureus SSTIs, the prevalence of CA-MRSA was 9% in 2004, 16% in 2005, and 21% in 2006 (P < , chi-square test for trend). Seventy-five percent of CA-MRSA isolates tested were of the USA 300 or 400 clone type. Ninety-two percent of CA-MRSA isolates tested were positive for Panton-Valentine leukocidin, of which 90% carried staphylococcal chromosomal cassette mec type IV. The rate of use of a -lactam antibiotic as initial empirical therapy for patients with CA-MRSA SSTIs was 86%, 77%, and 60% in 2004, 2005, and 2006, respectively (P 0.04, chi-square test for trend). Thirty percent of -lactam-treated patients had a documented risk factor for CA-MRSA infection. The use of a -lactam antibiotic as initial empirical therapy for CA-MRSA SSTIs has decreased significantly over the past 3 years. However, even as the prevalence of CA-MRSA SSTIs approaches 25%, the majority of patients are still receiving inactive antimicrobial therapy. Further evaluation of the outcomes associated with discordant therapy for CA-MRSA SSTIs is needed. Infections due to methicillin-resistant Staphylococcus aureus (MRSA) among patients without recent health-care exposures are increasingly being recognized (8, 10, 19, 23, 28). The primary clinical presentation is in the form of skin and soft tissue infections (SSTIs), but necrotizing pneumonia, endocarditis, bacteremia, central nervous system infections, osteomyelitis, and other invasive diseases have also been reported (4, 10, 11, 16, 19, 23). Community-associated MRSA (CA-MRSA) has been defined both epidemiologically (positive culture results within 48 to 72 h of hospital admission, no hospitalizations within the last year, and no history of MRSA colonization or infection) and molecularly (pulsed-field gel electrophoresis type USA 300 and 400) (7, 10, 18). CA-MRSA typically also has a characteristic antibiotic susceptibility pattern, carries specific virulence toxins such as the Panton-Valentine leukocidin (PVL), and possesses a specific staphylococcal chromosomal cassette (SCCmec type IV) (7, 18, 20, 24, 28). The prevalence of CA-MRSA varies greatly by geographic area. A study from San Diego, CA, noted a 65% CA-MRSA rate over a 15-year period while other regions have reported much lower rates, ranging from 4% to 50% (2, 19, 20, 28). An * Corresponding author. Mailing address: VA Boston HCS, 150 South Huntington Ave., 151 MAV, Boston, MA Present address: Department of Medicine, Division of Hematology, Brigham and Women s Hospital, Harvard Medical School, Boston, MA. Published ahead of print on 17 October appreciation of local CA-MRSA rates is critical to the appropriate prescribing of empirical antimicrobial therapy (7). Guidelines have suggested that alternatives to -lactam antibiotics be used as empirical therapy for patients presenting with SSTIs in areas where the prevalence of CA-MRSA exceeds 10 to 15% (7). An accurate calculation of CA-MRSA rates requires coordination of data from clinicians, microbiology laboratories, and hospital epidemiologists, a system that is not usually available or easily implemented. Thus, clinicians usually rely on individual patient characteristics described in the literature as being associated with CA-MRSA. Appreciation of these risk factors and their incorporation into clinical practice are an evolving process that is likely to improve over time. In the interim, however, -lactam antibiotics continue to be prescribed empirically to a proportion of patients who have an infection with CA-MRSA (22, 25, 28). Although some studies have found that the use of an inactive antimicrobial regimen for CA-MRSA infection is not necessarily associated with adverse outcomes, more-recent data suggest that there is a difference in clinical cure rates based on adequacy of the antibiotic prescribed (3, 5, 12, 17, 18, 22). To our knowledge, no study to date has reported trends over a 3-year period in treatment for MRSA infections that are well characterized both molecularly and epidemiologically as being caused by community-associated strains. The purpose of this study was to assess the prevalence and molecular epidemiology of CA-MRSA at Yale-New Haven Hospital (YNHH) and evaluate changes in prescribing patterns over a 3-year period. 3930
2 VOL. 45, LACTAMS FOR CA-MRSA 3931 FIG. 1. Flow diagram of chart-confirmed CA-MRSA SSTI study population from 2,461 unique MRSA patients. MATERIALS AND METHODS Study population. YNHH is a 944-bed academically affiliated medical center providing primary and tertiary care to residents of the New Haven area and southern Connecticut. In 2006, there were 50,369 hospital discharges and 503,656 outpatient visits, including 113,921 emergency room visits. The YNHH Clinical Microbiology Laboratory receives specimens from inpatients, hospital-affiliated outpatient clinics, and the emergency room. As part of the MRSA Surveillance Program of the YNHH Department of Quality Improvement Support Services, all patients with a clinical or surveillance culture positive for MRSA are prospectively entered into a database by an infection control practitioner and the isolate is banked by the Epidemiology Laboratory. From this database, we obtained information which was routinely recorded for each patient, including the date and site of culture, duration of hospitalization, and previous MRSA history. Separate hospital databases provided information as to whether a patient had been hospitalized at YNHH in the prior year and on the total number of patients with SSTIs (infection of skin, wound, or abscess) due to any S. aureus isolate (including both methicillin susceptible and resistant) by study year. Selection of patients and outcome definitions. The patients eligible for inclusion in this study had a culture positive for MRSA at YNHH between 1 January 2004 and 31 December 2006 and met the epidemiological definition of CA- MRSA, including having the MRSA culture obtained within 48 h of hospital admission, no hospitalizations within the last year, and no history of MRSA colonization or infection. Patients who did not meet this epidemiologic definition were excluded. Duplicate isolates and surveillance cultures were also excluded. Patients with a culture obtained from a wound or abscess were defined as having an SSTI. The prevalence of CA-MRSA SSTIs was calculated by dividing the number of patients with SSTIs due to CA-MRSA by the number of patients with any S. aureus SSTI (including both methicillin-susceptible and -resistant isolate infections). Patients eligible for the medical record review and molecular testing portion of the study had to meet the above epidemiological criteria for CA-MRSA and also have an isolate with a susceptibility pattern suggestive of a USA 300 or 400 strain. Specifically, the MRSA isolate had to be sensitive to trimethoprim-sulfamethoxazole, rifampin, gentamicin, clindamycin, and vancomycin. Because clindamycin susceptibility data were not uniformly available in 2006, a random sample of CA-MRSA isolates was selected via a random number generator from each month and tested. Isolates susceptible to clindamycin and meeting the other antimicrobial susceptibility criteria were included in the study. Laboratory methods. MRSA isolates were identified by disk diffusion criteria defined by the Clinical and Laboratory Standards Institute. The presence of the lukf and luks genes encoding PVL and the staphylococcal chromosome cassette mec (SCCmec) type were assessed using previously described PCR methods (13, 21). Isolates also underwent typing by pulsed-field gel electrophoresis (PFGE) using the restriction enzyme SmaI, as previously described, with controls for USA 100 to 800 PFGE types provided by the Network on Antimicrobial Resistance in Staphylococcus aureus supported under NIAID/NIH contract no. N01- AI (1, 26). Interpretation of laboratory results was performed prior to and without knowledge of the results of the medical record review. Medical record review. Medical records were reviewed for the following information: (i) verification of community-associated epidemiology as recorded in the database (with cases reclassified as health-care-associated infections if there was evidence of surgery, admission to another hospital, or residence in a nonhospital health-care facility in the last year), (ii) identification of putative risk factors for CA-MRSA (having a history of contact sports, incarceration, military duty, illicit drug use, homelessness, or day-care attendance or having family members with MRSA or similar skin infections), (iii) initial antimicrobial agent prescribed, and (iv) whether incision and drainage were performed. This study was approved by the Institutional Review Board of Yale University School of Medicine. Statistical methods. Data were analyzed using EPI Info software (version 3.3.2; CDC). Categorical variables were tested using the chi-square test or Fisher s exact test. Trends over the study period were evaluated with the chisquare test for trend. RESULTS Prevalence of CA-MRSA SSTIs. In the 3-year study period, a total of 2,461 unique patients with a culture positive for MRSA were identified. The proportion of patients meeting our epidemiological definition of having a CA-MRSA infection increased from 165 (22%) to 223 (30%) to 348 (35%) over the 3-year period (Fig. 1). SSTIs were the predominant infections caused by CA-MRSA and accounted for 67 (41%), 123 (55%), and 238 (68%) of the CA-MRSA infections in 2004, 2005, and 2006, respectively (P 0.01, chi-square test for trend). Among the 2,636 unique patients identified as having an S. aureus SSTI (including both methicillin-sensitive and
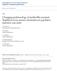
3 3932 GUPTA ET AL. J. CLIN. MICROBIOL. TABLE 2. Characteristics of study patients with a chart-confirmed CA-MRSA SSTI FIG. 2. The proportion of patients with a CA-MRSA SSTI being prescribed a -lactam (solid line) decreased from 2004 to 2006 (P 0.04, chi-square test for trend) as the prevalence of CA-MRSA SSTIs (dashed line) increased over the same time period (P , chisquare test for trend). -resistant isolate infections) at YNHH in the 3-year period, the prevalence of CA-MRSA SSTIs was 67/737 (9%) in 2004, 123/782 (16%) in 2005, and 238/1117 (21%) in 2006 (P , chi-square test for trend) (Fig. 2). Molecular epidemiology of CA-MRSA. From the total group of CA-MRSA isolates meeting our epidemiological criteria for community-associated infection, we identified 183 that also met the antimicrobial susceptibility criteria. Nine isolates were not stored and thus were not available for further testing. The remaining 174 isolates (95%) were available for molecular evaluation (Fig. 1). The molecular characteristics of the MRSA isolates from patients confirmed to have community-associated infection by medical record review are shown in Table 1. Strains consistent with the USA 300 clone type were identified in each year studied and accounted for 38%, 83%, and 69% of all chartconfirmed CA-MRSA isolates in 2004, 2005, and 2006, respectively. The USA 400 clone type was much less frequent but nevertheless present in each year. The only other clone type identified was USA 100 (one or two strains per year; Table 1). In addition, there were a small number of strains in each year that could not be classified as a USA 100 to 800 type. Of this group, there was no prevalent pattern identified, although similarities to the published PFGE pattern of the USA 1000 type were noted (27). No control for USA 1000 type was available for confirmatory testing at the time of the study. The proportion of confirmed CA-MRSA strains positive for PVL was 92% over the 3-year period (Table 1). Among the six TABLE 1. Molecular characteristics of chart-confirmed CA-MRSA isolates Characteristic No. of isolates positive/total no. (%) Total PVL 15/16 (94) 28/29 (97) 30/34 a (88) 73/79 (92) SCCmec type IV 11/15 (73) 28/28 (100) 27/30 (90) 66/73 (90) USA 100 clone 2/16 (13) 1/29 (4) 2/48 (4) 5/93 (5) USA 300 clone 6/16 (38) 24/29 (83) 33/48 (69) 63/93 (68) USA 400 clone 2/16 (13) 2/29 (7) 2/48 (4) 6/93 (7) Non-USA 100 to 800 6/16 (38) 2/29 (7) 11/48 (23) 19/93 (20) a The PVL assay was performed on 34 of 48 isolates confirmed as CA-MRSA in Characteristic Total (n 84) No. of patients positive (%) 2004 (n 14) 2005 (n 27) 2006 (n 43) Age (yr) (15) (23) (49) (13) Male 55 (66) 9 (64) 20 (74) 26 (60) Hospitalized a 39 (46) 11 (79) 8 (30) 20 (47) ß-Lactam therapy b 57 (70) c 12 (86) 20 (77) 25 (60) Risk factor for CA-MRSA d 17 (30) 4 (33) 6 (30) 7 (28) a Cultures were obtained at the time of admission or less than 48 h after admission. b P 0.04, chi-square test for trend for decrease over the 3-year study period. c Data not available for two patients. d Among those receiving -lactams. PVL-negative strains, three were of the USA 100 type, one was a USA 300 strain, and the remaining two isolates could not be classified as a USA 100 to 800 strain. Fourteen confirmed CA-MRSA strains were not available for evaluation of PVL. Among PVL-positive strains, 90% were found to carry SCCmec type IV. Forty-four patients initially designated as having a community-associated infection by epidemiological criteria were reclassified as having a health-care-related MRSA infection after medical record review (further detailed below). Nine of these patients (20%) had a USA 300 clone type compared to 63 (68%) of the 93 patients who were confirmed by record review to have a community-associated infection. Thus, patients with a CA-MRSA infection were eightfold more likely than patients with a health-care-associated MRSA infection to have a USA 300 clone type (odds ratio, 8.2 [95% confidence interval, 3.3 to 21.0]; P ). There were no USA 400 strains found among patients with health-care-associated MRSA. Empirical antimicrobial use. Medical records were requested on all 174 patients whose isolates were molecularly tested. One hundred forty-eight (85%) were available for review and contained information on the visit date of interest. The remaining charts either were not retrievable from the file room or did not contain information about the relevant visit. Of the total group reviewed, 44 (30%) were reclassified as health-care-associated MRSA infections due to documentation of prior hospitalization, residence in a long-term healthcare setting, or a surgical procedure (inpatient and/or outpatient) within the last year. An additional 11 (7%) patients were excluded from further analysis as their isolates were designated as representing colonization rather than infection by the primary providers and no specific therapy was provided. There were only nine infections due to CA-MRSA that were not categorized as an SSTI in the 3-year study period (two urinary tract infections, one bacteremia case, one sinusitis case, and five pneumonia cases). The remaining 84 infections were categorized as SSTIs (i.e., skin, wound, or abscess) and were the focus of the antimicrobial management analyses. As shown in Table 2, more than half of the patients meeting our defini-
4 VOL. 45, LACTAMS FOR CA-MRSA 3933 tion of having a CA-MRSA SSTI were 10 to 50 years of age in each year studied. There was a greater proportion of males than of females identified with CA-MRSA in each year. Approximately half the patients were hospitalized for treatment of their infection. The rate of utilization of a -lactam antibiotic as initial empirical therapy for SSTIs due to CA-MRSA decreased from 86% to 77% to 60% over the years 2004, 2005, and 2006, respectively (P 0.04, chi-square test for trend) (Table 2). As shown in Fig. 2, this decrease was in inverse relationship to the statistically significant increasing prevalence of CA-MRSA SSTIs. Patients were almost threefold less likely to receive a -lactam antibiotic for a CA-MRSA SSTI in 2006 than in 2004 and 2005 (odds ratio, 0.37; P 0.04), the same period in which the prevalence of CA-MRSA SSTIs more than doubled. A putative epidemiological risk factor for CA-MRSA infection was identified in 30% of patients who were treated with a -lactam as initial empirical therapy. Specifically, the percentages of patients prescribed a -lactam who had a risk factor for CA-MRSA were 33% in 2004, 30% in 2005, and 28% in 2006 (Table 2). The majority of patients with SSTIs (67/84, 80%) underwent incision and drainage regardless of antimicrobial therapy. DISCUSSION To our knowledge, this is one of the first studies to evaluate prescribing trends over a 3-year period for infections that are well characterized epidemiologically, clinically, and molecularly as being due to CA-MRSA. Such data are critically important in assisting clinicians to optimize the accuracy of empirical prescribing that is integral to treating these acute infections. The overall rate of CA-MRSA in the YNHH catchment area was moderately high ( 30%) and increased over the 3-year study period. The proportion of patients with SSTIs due to CA-MRSA compared to methicillin-susceptible S. aureus or health-care-associated MRSA also increased significantly, from 9% in 2004 to 21% in An important finding in our study is that empirical -lactam use for CA-MRSA SSTIs decreased significantly over this same 3-year period, suggesting that clinicians are recognizing this emerging infection and modifying their treatment approach as recommended by CDC guidelines (7). However, despite this decrease, nearly 60% of patients presenting with CA-MRSA SSTIs still received -lactams as initial empirical therapy in A similar rate of -lactam use was found among patients treated in 2004 for MRSA SSTIs in 11 emergency rooms throughout the United States (18). Recently, a study from a community-based clinic in Boston, MA, found that the majority of patients with SSTIs were no longer being prescribed a -lactam in 2005 (25). The study differed from ours in that molecular characterization of the strains was not performed and approximately one-quarter of patients had a known previous MRSA infection, decreasing the likelihood of -lactam utilization and distinguishing the study population from ours, in which there was no known history of MRSA. Another important difference is that more than half of the Boston clinic population were men who have sex with men, an exposure that has been associated with increased CA-MRSA risk (14, 25). It may be that smaller clinical sites serving higherrisk populations have more rapidly and uniformly modified their approach to empirical therapy of SSTI. About one-third of the patients in our study had one or more of the factors that have been associated with CA-MRSA, including young age, contact sports, incarceration, illicit drug use, homelessness, and day-care attendance (6, 9, 29). As reported in previous studies, specific risk factor profiles cannot reliably help clinicians distinguish between CA-MRSA and methicillin-susceptible isolate infections (15). Thus, knowledge of local prevalence rates is still critical to appropriate empirical prescribing. Initial classification of our isolates as community associated was performed via a computerized database. Of the subset of patients whose charts were reviewed, only 63% of isolates could be confirmed as community-associated infections by epidemiologic criteria. Prior hospitalization in outside community hospitals, recent outpatient surgical procedures, and residence in long-term care facilities were the main factors that resulted in reclassification of MRSA isolates as health care associated. These variables are rarely available in automated electronic databases, suggesting that studies relying on such databases for identification of CA-MRSA may be hindered by misclassification bias. Interestingly, the utilization of molecular characteristics was very helpful in identifying the isolates that ultimately met our strict definition for being CA-MRSA. The availability of more-rapid methods for typing makes it feasible to use molecular features to further define CA-MRSA when traditional chart review or direct patient interview is not possible (27). The main limitation of our study is the use of chart abstraction for assessment of antimicrobial regimens and risk factors. The utilization of an active, prospectively developed, surveillance database helps to minimize some of the issues of a retrospective study design. Since we cannot assume that the risk factors of interest were uniformly recorded, we limited this part of the analysis to being primarily descriptive. In addition, the unavailability of complete clindamycin susceptibility data in 2006 could have influenced the number of patients selected for medical record review in that year. For this reason, we do not base any of our results on antimicrobial susceptibility criteria alone and used the information only to further identify patients for chart review and molecular characterization of their isolates. Finally, the generalizability of our findings may be limited as the study population was from one hospital, although the catchment area includes both rural and urban settings. To our knowledge, our study is the first to synthesize epidemiologic, clinical, and molecular typing criteria to identify annual trends in empirical -lactam therapy for CA-MRSA SSTIs. The prevalence of CA-MRSA SSTIs has increased significantly and is approaching 25%. Although the use of a -lactam as initial empirical therapy has decreased significantly over the past 3 years, more than half of patients presenting with CA-MRSA SSTIs are still receiving inactive antimicrobial therapy. The findings emphasize the need for individual institutions to identify their CA-MRSA prevalence rates, as this may help optimize empirical antimicrobial choice. Further study of the role of empirical antimicrobial use in outcomes in
5 3934 GUPTA ET AL. J. CLIN. MICROBIOL. patients with CA-MRSA SSTIs is warranted, particularly in light of the high frequency of -lactam use that currently exists. ACKNOWLEDGMENTS We thank Sofya Rodov, Department of Medicine, Section of Hematology, Yale School of Medicine, for performance of PCR assays; Deborah Callan and Patricia Farrel, Department of Quality Improvement Support Services (Epidemiology Laboratory), Yale-New Haven Hospital, for assistance with microbiology and typing; and Helen Schweidler, Yale-New Haven Hospital Laboratory Computer Operations, for assistance with data retrieval. Funding for this work was provided by the Department of Medicine, Section of Infectious Diseases (K.G.), and the Department of Quality Improvement Support Services, Yale-New Haven Hospital (L.-M.D.). We have no conflicts of interest to report. REFERENCES 1. Bannerman, T. L., G. A. Hancock, F. C. Tenover, and J. M. Miller Pulsed-field gel electrophoresis as a replacement for bacteriophage typing of Staphylococcus aureus. J. Clin. Microbiol. 33: Crum, N. F., R. U. Lee, S. A. Thornton, O. C. Stine, M. R. Wallace, C. Barrozo, A. Keefer-Norris, S. Judd, and K. L. Russell Fifteen-year study of the changing epidemiology of methicillin-resistant Staphylococcus aureus. Am. J. Med. 119: Davis, S. L., M. B. Perri, S. M. Donabedian, C. Manierski, A. Singh, D. Vager, N. Z. Haque, K. Speirs, R. R. Muder, B. Robinson-Dunn, M. K. Hayden, and M. J. Zervos Epidemiology and outcomes of communityassociated methicillin-resistant Staphylococcus aureus infection. J. Clin. Microbiol. 45: Francis, J. S., M. C. Doherty, U. Lopatin, C. P. Johnston, G. Sinha, T. Ross, M. Cai, N. N. Hansel, T. Perl, J. R. Ticehurst, K. Carroll, D. L. Thomas, E. Nuermberger, and J. G. Bartlett Severe community-onset pneumonia in healthy adults caused by methicillin-resistant Staphylococcus aureus carrying the Panton-Valentine leukocidin genes. Clin. Infect. Dis. 40: Fridkin, S. K., J. C. Hageman, M. Morrison, L. T. Sanza, K. Como-Sabetti, J. A. Jernigan, K. Harriman, L. H. Harrison, R. Lynfield, and M. M. Farley Methicillin-resistant Staphylococcus aureus disease in three communities. N. Engl. J. Med. 352: Gilbert, M., J. MacDonald, D. Gregson, J. Siushansian, K. Zhang, S. Elsayed, K. Laupland, T. Louie, K. Hope, M. Mulvey, J. Gillespie, D. Nielsen, V. Wheeler, M. Louie, A. Honish, G. Keays, and J. Conly Outbreak in Alberta of community-acquired (USA300) methicillin-resistant Staphylococcus aureus in people with a history of drug use, homelessness or incarceration. CMAJ 175: Gorwitz, R. J., D. B. Jernigan, J. H. Powers, J. A. Jernigan, and Participants Strategies for clinical management of MRSA in the community: summary of an expert s meeting convened by the CDC. Centers for Disease Control and Prevention, Atlanta, GA. 8. Karchmer, A. W From theory to practice: resistance in Staphylococcus aureus and new treatments. Clin. Microbiol. Infect. 12(Suppl. 8): Kazakova, S. V., J. C. Hageman, M. Matava, A. Srinivasan, L. Phelan, B. Garfinkel, T. Boo, S. McAllister, J. Anderson, B. Jensen, D. Dodson, D. Lonsway, L. K. McDougal, M. Arduino, V. J. Fraser, G. Killgore, F. C. Tenover, S. Cody, and D. B. Jernigan A clone of methicillin-resistant Staphylococcus aureus among professional football players. N. Engl. J. Med. 352: King, M. D., B. J. Humphrey, Y. F. Wang, E. V. Kourbatova, S. M. Ray, and H. M. Blumberg Emergence of community-acquired methicillin-resistant Staphylococcus aureus USA 300 clone as the predominant cause of skin and soft-tissue infections. Ann. Intern. Med. 144: Kourbatova, E. V., J. S. Halvosa, M. D. King, S. M. Ray, N. White, and H. M. Blumberg Emergence of community-associated methicillin-resistant Staphylococcus aureus USA 300 clone as a cause of health care-associated infections among patients with prosthetic joint infections. Am. J. Infect Control 33: Lee, M. C., A. M. Rios, M. F. Aten, A. Mejias, D. Cavuoti, G. H. McCracken, Jr., and R. D. Hardy Management and outcome of children with skin and soft tissue abscesses caused by community-acquired methicillin-resistant Staphylococcus aureus. Pediatr. Infect. Dis. J. 23: Lina, G., Y. Piemont, F. Godail-Gamot, M. Bes, M. O. Peter, V. Gauduchon, F. Vandenesch, and J. Etienne Involvement of Panton-Valentine leukocidin-producing Staphylococcus aureus in primary skin infections and pneumonia. Clin. Infect. Dis. 29: Mathews, W. C., J. C. Caperna, R. E. Barber, F. J. Torriani, L. G. Miller, S. May, and J. A. McCutchan Incidence of and risk factors for clinically significant methicillin-resistant Staphylococcus aureus infection in a cohort of HIV-infected adults. J. Acquir. Immune Defic. Syndr. 40: Miller, L. G., F. Perdreau-Remington, A. S. Bayer, B. Diep, N. Tan, K. Bharadwa, J. Tsui, J. Perlroth, A. Shay, G. Tagudar, U. Ibebuogu, and B. Spellberg Clinical and epidemiologic characteristics cannot distinguish community-associated methicillin-resistant Staphylococcus aureus infection from methicillin-susceptible S. aureus infection: a prospective investigation. Clin. Infect. Dis. 44: Miller, L. G., F. Perdreau-Remington, G. Rieg, S. Mehdi, J. Perlroth, A. S. Bayer, A. W. Tang, T. O. Phung, and B. Spellberg Necrotizing fasciitis caused by community-associated methicillin-resistant Staphylococcus aureus in Los Angeles. N. Engl. J. Med. 352: Miller, L. G., C. Quan, A. Shay, K. Mostafaie, K. Bharadwa, N. Tan, K. Matayoshi, J. Cronin, J. Tan, G. Tagudar, and A. S. Bayer A prospective investigation of outcomes after hospital discharge for endemic, community-acquired methicillin-resistant and -susceptible Staphylococcus aureus skin infection. Clin. Infect. Dis. 44: Moran, G. J., A. Krishnadasan, R. J. Gorwitz, G. E. Fosheim, L. K. McDougal, R. B. Carey, and D. A. Talan Methicillin-resistant S. aureus infections among patients in the emergency department. N. Engl. J. Med. 355: Naimi, T. S., K. H. LeDell, D. J. Boxrud, A. V. Groom, C. D. Steward, S. K. Johnson, J. M. Besser, C. O Boyle, R. N. Danila, J. E. Cheek, M. T. Osterholm, K. A. Moore, and K. E. Smith Epidemiology and clonality of community-acquired methicillin-resistant Staphylococcus aureus in Minnesota, Clin. Infect. Dis. 33: Naimi, T. S., K. H. LeDell, K. Como-Sabetti, S. M. Borchardt, D. J. Boxrud, J. Etienne, S. K. Johnson, F. Vandenesch, S. Fridkin, C. O Boyle, R. N. Danila, and R. Lynfield Comparison of community- and health careassociated methicillin-resistant Staphylococcus aureus infection. JAMA 290: Oliveira, D. C., and H. de Lencastre Multiplex PCR strategy for rapid identification of structural types and variants of the mec element in methicillin-resistant Staphylococcus aureus. Antimicrob. Agents Chemother. 46: Ruhe, J. J., N. Smith, R. W. Bradsher, and A. Menon Communityonset methicillin-resistant Staphylococcus aureus skin and soft-tissue infections: impact of antimicrobial therapy on outcome. Clin. Infect. Dis. 44: Seybold, U., E. V. Kourbatova, J. G. Johnson, S. J. Halvosa, Y. F. Wang, M. D. King, S. M. Ray, and H. M. Blumberg Emergence of community-associated methicillin-resistant Staphylococcus aureus USA300 genotype as a major cause of health care-associated blood stream infections. Clin. Infect. Dis. 42: Shukla, S. K., M. E. Stemper, S. V. Ramaswamy, J. M. Conradt, R. Reich, E. A. Graviss, and K. D. Reed Molecular characteristics of nosocomial and Native American community-associated methicillin-resistant Staphylococcus aureus clones from rural Wisconsin. J. Clin. Microbiol. 42: Szumowski, J. D., D. E. Cohen, F. Kanaya, and K. H. Mayer Treatment and outcomes of infections by methicillin-resistant Staphylococcus aureus at an ambulatory clinic. Antimicrob. Agents Chemother. 51: Tenover, F. C., R. D. Arbeit, R. V. Goering, P. A. Mickelsen, B. E. Murray, D. H. Persing, and B. Swaminathan Interpreting chromosomal DNA restriction patterns produced by pulsed-field gel electrophoresis: criteria for bacterial strain typing. J. Clin. Microbiol. 33: Tenover, F. C., R. R. Vaughn, L. K. McDougal, G. E. Fosheim, and J. E. McGowan, Jr Multiple-locus variable-number tandem-repeat assay analysis of methicillin-resistant Staphylococcus aureus strains. J. Clin. Microbiol. 45: Vandenesch, F., T. Naimi, M. C. Enright, G. Lina, G. R. Nimmo, H. Heffernan, N. Liassine, M. Bes, T. Greenland, M. E. Reverdy, and J. Etienne Community-acquired methicillin-resistant Staphylococcus aureus carrying Panton-Valentine leukocidin genes: worldwide emergence. Emerg. Infect. Dis. 9: Zinderman, C. E., B. Conner, M. A. Malakooti, J. E. LaMar, A. Armstrong, and B. K. Bohnker Community-acquired methicillin-resistant Staphylococcus aureus among military recruits. Emerg. Infect. Dis. 10:
Epidemiology and Outcomes of Community-Associated Methicillin-Resistant Staphylococcus aureus Infection
 JOURNAL OF CLINICAL MICROBIOLOGY, June 2007, p. 1705 1711 Vol. 45, No. 6 0095-1137/07/$08.00 0 doi:10.1128/jcm.02311-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Epidemiology
JOURNAL OF CLINICAL MICROBIOLOGY, June 2007, p. 1705 1711 Vol. 45, No. 6 0095-1137/07/$08.00 0 doi:10.1128/jcm.02311-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Epidemiology
Treatment and Outcomes of Infections by Methicillin-Resistant Staphylococcus aureus at an Ambulatory Clinic
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2007, p. 423 428 Vol. 51, No. 2 0066-4804/07/$08.00 0 doi:10.1128/aac.01244-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Treatment
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2007, p. 423 428 Vol. 51, No. 2 0066-4804/07/$08.00 0 doi:10.1128/aac.01244-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Treatment
A Prospective Investigation of Nasal Mupirocin, Hexachlorophene Body Wash, and Systemic
 AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 14 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01608-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
Molecular Characterization of Staphylococcus aureus Isolates from a Contemporary (2005) ACCEPTED
 AAC Accepts, published online ahead of print on 18 June 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.01588-06 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 18 June 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.01588-06 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
Presence and Molecular Epidemiology of Virulence Factors in Methicillin-Resistant Staphylococcus aureus Strains Colonizing and Infecting Soldiers
 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2009, p. 940 945 Vol. 47, No. 4 0095-1137/09/$08.00 0 doi:10.1128/jcm.02352-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Presence and
JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2009, p. 940 945 Vol. 47, No. 4 0095-1137/09/$08.00 0 doi:10.1128/jcm.02352-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Presence and
Hong-Kai Wang 1, Chun-Yen Huang 1 and Yhu-Chering Huang 1,2*
 Wang et al. BMC Infectious Diseases (2017) 17:470 DOI 10.1186/s12879-017-2560-0 RESEARCH ARTICLE Open Access Clinical features and molecular characteristics of childhood communityassociated methicillin-resistant
Wang et al. BMC Infectious Diseases (2017) 17:470 DOI 10.1186/s12879-017-2560-0 RESEARCH ARTICLE Open Access Clinical features and molecular characteristics of childhood communityassociated methicillin-resistant
Received 20 March 2007/Returned for modification 10 July 2007/Accepted 27 August 2007
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome
 MAJOR ARTICLE Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome Jörg J. Ruhe, 1,2 Nathaniel Smith, 1,3 Robert W. Bradsher,
MAJOR ARTICLE Community-Onset Methicillin-Resistant Staphylococcus aureus Skin and Soft-Tissue Infections: Impact of Antimicrobial Therapy on Outcome Jörg J. Ruhe, 1,2 Nathaniel Smith, 1,3 Robert W. Bradsher,
Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care units
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus colonization in paediatric intensive-care
Received 5 June 2008/Returned for modification 5 March 2009/Accepted 12 February 2010
 JOURNAL OF CLINICAL MICROBIOLOGY, May 2010, p. 1753 1757 Vol. 48, No. 5 0095-1137/10/$12.00 doi:10.1128/jcm.01065-08 Copyright 2010, American Society for Microbiology. All Rights Reserved. Staphylococcus
JOURNAL OF CLINICAL MICROBIOLOGY, May 2010, p. 1753 1757 Vol. 48, No. 5 0095-1137/10/$12.00 doi:10.1128/jcm.01065-08 Copyright 2010, American Society for Microbiology. All Rights Reserved. Staphylococcus
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant
 Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Impact of a Standardized Protocol to Address Outbreak of Methicillin-resistant Staphylococcus Aureus Skin Infections at a large, urban County Jail System Earl J. Goldstein, MD* Gladys Hradecky, RN* Gary
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
The past decade has seen a large increase in infections
 Community-associated Methicillin- Resistant Staphylococcus aureus in Outpatients, United States, 1999 2006 Eili Klein, David L. Smith, and Ramanan Laxminarayan CME ACTIVITY MedscapeCME is pleased to provide
Community-associated Methicillin- Resistant Staphylococcus aureus in Outpatients, United States, 1999 2006 Eili Klein, David L. Smith, and Ramanan Laxminarayan CME ACTIVITY MedscapeCME is pleased to provide
A Clone of Methicillin-Resistant Staphylococcus aureus among Professional Football Players
 The new england journal of medicine original article A Clone of Methicillin-Resistant Staphylococcus aureus among Professional Football Players Sophia V. Kazakova, M.D., M.P.H., Ph.D., Jeffrey C. Hageman,
The new england journal of medicine original article A Clone of Methicillin-Resistant Staphylococcus aureus among Professional Football Players Sophia V. Kazakova, M.D., M.P.H., Ph.D., Jeffrey C. Hageman,
Received 21 February 2007/Returned for modification 27 March 2007/Accepted 12 June 2007
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2007, p. 3298 3303 Vol. 51, No. 9 0066-4804/07/$08.00 0 doi:10.1128/aac.00262-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Tetracyclines
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2007, p. 3298 3303 Vol. 51, No. 9 0066-4804/07/$08.00 0 doi:10.1128/aac.00262-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Tetracyclines
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016
 Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillin- Resistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2016 Jessica Spencer and Uzo Chukwuma Approved for public release. Distribution
Since its discovery in the 1960s, methicillinresistant
 CME Community-Acquired Methicillin-Resistant Staphylococcus aureus: Diagnosis and Treatment Update for Plastic Surgeons D. Heath Stacey, M.D. Barry C. Fox, M.D. Samuel O. Poore, M.D., Ph.D. Michael L.
CME Community-Acquired Methicillin-Resistant Staphylococcus aureus: Diagnosis and Treatment Update for Plastic Surgeons D. Heath Stacey, M.D. Barry C. Fox, M.D. Samuel O. Poore, M.D., Ph.D. Michael L.
Epidemiology of community MRSA obtained from the UK West Midlands region.
 Epidemiology of community MRSA obtained from the UK West Midlands region. J. Rollason a, L. Bastin b, A. C. Hilton a, D. G. Pillay c, T. Worthington a, C. Mckeon c, P. De c, K. Burrows c and P. A. Lambert
Epidemiology of community MRSA obtained from the UK West Midlands region. J. Rollason a, L. Bastin b, A. C. Hilton a, D. G. Pillay c, T. Worthington a, C. Mckeon c, P. De c, K. Burrows c and P. A. Lambert
Research Article Genotyping of Methicillin Resistant Staphylococcus aureus Strains Isolated from Hospitalized Children
 International Pediatrics, Article ID 314316, 4 pages http://dx.doi.org/10.1155/2014/314316 Research Article Genotyping of Methicillin Resistant Staphylococcus aureus Strains Isolated from Hospitalized
International Pediatrics, Article ID 314316, 4 pages http://dx.doi.org/10.1155/2014/314316 Research Article Genotyping of Methicillin Resistant Staphylococcus aureus Strains Isolated from Hospitalized
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017
 Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
Annual Surveillance Summary: Methicillinresistant Staphylococcus aureus (MRSA) Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution
Fifteen-Year Study of the Changing Epidemiology of Methicillin-Resistant Staphylococcus aureus
 The American Journal of Medicine (2006) 119, 943-951 CLINICAL RESEARCH STUDY AJM Theme Issue: Infectious Disease Fifteen-Year Study of the Changing Epidemiology of Methicillin-Resistant Staphylococcus
The American Journal of Medicine (2006) 119, 943-951 CLINICAL RESEARCH STUDY AJM Theme Issue: Infectious Disease Fifteen-Year Study of the Changing Epidemiology of Methicillin-Resistant Staphylococcus
Ca-MRSA Update- Hand Infections. Washington Hand Society September 19, 2007
 Ca-MRSA Update- Hand Infections Washington Hand Society September 19, 2007 Resistant Staph. Aureus Late 1940 s -50% S.Aureus resistant to PCN 1957-80/81 strain- of S.A. highly virulent and easily transmissible
Ca-MRSA Update- Hand Infections Washington Hand Society September 19, 2007 Resistant Staph. Aureus Late 1940 s -50% S.Aureus resistant to PCN 1957-80/81 strain- of S.A. highly virulent and easily transmissible
Staphylococcus aureus
 Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins
 Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Staphylococcus aureus Significant human pathogen. SSTI Biomaterial related infections Osteomyelitis Endocarditis Toxin mediated diseases TSST Staphylococcal enterotoxins Quintessential Pathogen? Nizet
Management of Skin and Soft-Tissue Infection
 Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
Clinical Decisions Interactive at www.nejm.org Management of Skin and Soft-Tissue Infection This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed
Clostridium difficile Surveillance Report 2016
 Clostridium difficile Surveillance Report 2016 EMERGING INFECTIONS PROGRAM Clostridium difficile Surveillance Report 2016 Minnesota Department of Health Emerging Infections Program PO Box 64882, St. Paul,
Clostridium difficile Surveillance Report 2016 EMERGING INFECTIONS PROGRAM Clostridium difficile Surveillance Report 2016 Minnesota Department of Health Emerging Infections Program PO Box 64882, St. Paul,
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Community-Associated Methicillin-Resistant Staphylococcus aureus: Review of an Emerging Public Health Concern
 Community-Associated Methicillin-Resistant Staphylococcus aureus: Review of an Emerging Public Health Concern Timothy D. Drews, MD; Jonathan L. Temte, MD, PhD; Barry C. Fox, MD ABSTRACT Methicillin-resistant
Community-Associated Methicillin-Resistant Staphylococcus aureus: Review of an Emerging Public Health Concern Timothy D. Drews, MD; Jonathan L. Temte, MD, PhD; Barry C. Fox, MD ABSTRACT Methicillin-resistant
Yaseen Rafee 1,2, Nahed Abdel-Haq 1,2*, Basim Asmar 1,2, Tanaz Salimnia 3, Celine Vidaillac Pharm 4, Michael J Rybak Pharm 4,5 and Muhammad Amjad 6
 RESEARCH ARTICLE Open Access Increased prevalence of methicillin-resistant Staphylococcus aureus nasal colonization in household contacts of children with community acquired disease Yaseen Rafee 1,2, Nahed
RESEARCH ARTICLE Open Access Increased prevalence of methicillin-resistant Staphylococcus aureus nasal colonization in household contacts of children with community acquired disease Yaseen Rafee 1,2, Nahed
FM - Male, 38YO. MRSA nasal swab (+) Due to positive MRSA nasal swab test, patient will be continued on Vancomycin 1500mg IV q12 for MRSA treatment...
 Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Jillian O Keefe Doctor of Pharmacy Candidate 2016 September 15, 2015 FM - Male, 38YO HPI: Previously healthy male presents to ED febrile (102F) and in moderate distress ~2 weeks after getting a tattoo
Social and healthcare factors of methicillin-resistant Staphylococcus aureus resistance to targeted antibiotics THESIS
 Social and healthcare factors of methicillin-resistant Staphylococcus aureus resistance to targeted antibiotics THESIS Presented in Partial Fulfillment of the Requirements for the Degree Master of Science
Social and healthcare factors of methicillin-resistant Staphylococcus aureus resistance to targeted antibiotics THESIS Presented in Partial Fulfillment of the Requirements for the Degree Master of Science
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Contrasting Pediatric and Adult Methicillin-resistant Staphylococcus aureus Isolates
 Contrasting Pediatric and Adult Methicillin-resistant Staphylococcus aureus Isolates Michael Z. David,* Susan E. Crawford,* Susan Boyle-Vavra,* Mark A. Hostetler,* Daniel C. Kim,* and Robert S. Daum* We
Contrasting Pediatric and Adult Methicillin-resistant Staphylococcus aureus Isolates Michael Z. David,* Susan E. Crawford,* Susan Boyle-Vavra,* Mark A. Hostetler,* Daniel C. Kim,* and Robert S. Daum* We
Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department
 The new england journal of medicine original article Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department Gregory J. Moran, M.D., Anusha Krishnadasan, Ph.D., Rachel J.
The new england journal of medicine original article Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department Gregory J. Moran, M.D., Anusha Krishnadasan, Ph.D., Rachel J.
Methicillin-Resistant Staphylococcus aureus
 Methicillin-Resistant Staphylococcus aureus By Karla Givens Means of Transmission and Usual Reservoirs Staphylococcus aureus is part of normal flora and can be found on the skin and in the noses of one
Methicillin-Resistant Staphylococcus aureus By Karla Givens Means of Transmission and Usual Reservoirs Staphylococcus aureus is part of normal flora and can be found on the skin and in the noses of one
Infections caused by Methicillin-Resistant Staphylococcus
 MRSA infections are no longer limited to hospitals. An infectious disease specialist offers insight on what this means for dermatologists. By Robert S. Jones, DO, Reading, PA Infections caused by Methicillin-Resistant
MRSA infections are no longer limited to hospitals. An infectious disease specialist offers insight on what this means for dermatologists. By Robert S. Jones, DO, Reading, PA Infections caused by Methicillin-Resistant
Methicillin Resistant Staphylococcus aureus:
 Methicillin Resistant Staphylococcus aureus: Action-Oriented Guidance for Community-Based Prevention Jackie Dawson, PhD Public Health Epidemiologist Chelan, Douglas, Grant, Kittitas, & Okanogan Counties
Methicillin Resistant Staphylococcus aureus: Action-Oriented Guidance for Community-Based Prevention Jackie Dawson, PhD Public Health Epidemiologist Chelan, Douglas, Grant, Kittitas, & Okanogan Counties
ACCEPTED. Division of pediatric infectious diseases, Chang Gung Children s Hospital and Chang
 JCM Accepts, published online ahead of print on 1 October 00 J. Clin. Microbiol. doi:./jcm.0-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on 1 October 00 J. Clin. Microbiol. doi:./jcm.0-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
Community-associated methicillin-resistant Staphylococcus aureus infections
 British Medical Bulletin Advance Access published April 1, 2010 Community-associated methicillin-resistant Staphylococcus aureus infections Fiona J. Cooke and Nicholas M. Brown * Clinical Microbiology
British Medical Bulletin Advance Access published April 1, 2010 Community-associated methicillin-resistant Staphylococcus aureus infections Fiona J. Cooke and Nicholas M. Brown * Clinical Microbiology
Methicillin-Resistant Staphylococcus aureus Disease in Three Communities
 The new england journal of medicine original article Methicillin-Resistant Staphylococcus aureus Disease in Three Communities Scott K. Fridkin, M.D., Jeffrey C. Hageman, M.H.S., Melissa Morrison, M.P.H.,
The new england journal of medicine original article Methicillin-Resistant Staphylococcus aureus Disease in Three Communities Scott K. Fridkin, M.D., Jeffrey C. Hageman, M.H.S., Melissa Morrison, M.P.H.,
Antimicrobial Resistance and Molecular Epidemiology of Staphylococcus aureus in Ghana
 Antimicrobial Resistance and Molecular Epidemiology of Staphylococcus aureus in Ghana Beverly Egyir, PhD Noguchi Memorial Institute for Medical Research Bacteriology Department, University of Ghana Background
Antimicrobial Resistance and Molecular Epidemiology of Staphylococcus aureus in Ghana Beverly Egyir, PhD Noguchi Memorial Institute for Medical Research Bacteriology Department, University of Ghana Background
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs?
 Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
MRSA Outbreak in Firefighters
 MRSA Outbreak in Firefighters Angie Carranza Munger, MD Resident, Occupational and Environmental Medicine The University of Colorado, Denver and National Jewish Health Candidate, Masters of Public Health
MRSA Outbreak in Firefighters Angie Carranza Munger, MD Resident, Occupational and Environmental Medicine The University of Colorado, Denver and National Jewish Health Candidate, Masters of Public Health
Community-onset Staphylococcus aureus infections presenting to general practices in South-eastern Australia
 Epidemiol. Infect. (2014), 142, 501 511. Cambridge University Press 2013 doi:10.1017/s0950268813001581 Community-onset Staphylococcus aureus infections presenting to general practices in South-eastern
Epidemiol. Infect. (2014), 142, 501 511. Cambridge University Press 2013 doi:10.1017/s0950268813001581 Community-onset Staphylococcus aureus infections presenting to general practices in South-eastern
Research Article Classification of Epidemic Community-Acquired Methicillin-Resistant Staphylococcus aureus by Anatomical Site of Isolation
 BioMed Research International, Article ID 904283, 6 pages http://dx.doi.org/10.1155/2014/904283 Research Article Classification of Epidemic Community-Acquired Methicillin-Resistant Staphylococcus aureus
BioMed Research International, Article ID 904283, 6 pages http://dx.doi.org/10.1155/2014/904283 Research Article Classification of Epidemic Community-Acquired Methicillin-Resistant Staphylococcus aureus
 This is an author version of the contribution published on: Corcione S,Motta I,Fossati L,Campanile F,Stefani S,Cavallo R,Di Perri G,Ranieri VM,De Rosa FG Molecular epidemiology of methicillin-resistant
This is an author version of the contribution published on: Corcione S,Motta I,Fossati L,Campanile F,Stefani S,Cavallo R,Di Perri G,Ranieri VM,De Rosa FG Molecular epidemiology of methicillin-resistant
GUIDE TO INFECTION CONTROL IN THE HOSPITAL
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
LINEE GUIDA: VALORI E LIMITI
 Ferrara 28 novembre 2014 LINEE GUIDA: VALORI E LIMITI Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi EVIDENCE BIASED GERIATRIC MEDICINE Older patients with comorbid conditions
Ferrara 28 novembre 2014 LINEE GUIDA: VALORI E LIMITI Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi EVIDENCE BIASED GERIATRIC MEDICINE Older patients with comorbid conditions
Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2015
 Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2015 Helen Heffernan and Sarah Bakker Nosocomial Infections Laboratory, Institute of Environmental Science and Research Limited (ESR);
Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2015 Helen Heffernan and Sarah Bakker Nosocomial Infections Laboratory, Institute of Environmental Science and Research Limited (ESR);
JAMA. 2007;298(15):
 ORIGINAL CONTRIBUTION Invasive Methicillin-Resistant Staphylococcus aureus Infections in the United States R. Monina Klevens, DDS, MPH Melissa A. Morrison, MPH Joelle Nadle, MPH Susan Petit, MPH Ken Gershman,
ORIGINAL CONTRIBUTION Invasive Methicillin-Resistant Staphylococcus aureus Infections in the United States R. Monina Klevens, DDS, MPH Melissa A. Morrison, MPH Joelle Nadle, MPH Susan Petit, MPH Ken Gershman,
Summary Report Relating to a Pilot Program to Require Reporting of Methicillin-resistant Staphylococcus aureus
 Summary Report Relating to a Pilot Program to Require Reporting of Methicillin-resistant Staphylococcus aureus Prepared by the Texas Department of State Health Services as required by House Bill 1082,
Summary Report Relating to a Pilot Program to Require Reporting of Methicillin-resistant Staphylococcus aureus Prepared by the Texas Department of State Health Services as required by House Bill 1082,
CA-MRSA. The New Sports Pathogen
 10763-11_ON2605-Kurkowski.qxd 9/13/07 2:25 PM Page 310 CA-MRSA The New Sports Pathogen Christina Kurkowski Skin infections in athletes caused by community-associated (CA-MRSA) have been observed within
10763-11_ON2605-Kurkowski.qxd 9/13/07 2:25 PM Page 310 CA-MRSA The New Sports Pathogen Christina Kurkowski Skin infections in athletes caused by community-associated (CA-MRSA) have been observed within
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update
 EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
EDUCATIONAL COMMENTARY - Methicillin-Resistant Staphylococcus aureus: An Update Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain
Healthcare-associated Infections Annual Report December 2018
 December 2018 Healthcare-associated Infections Annual Report 2011-2017 TABLE OF CONTENTS INTRODUCTION... 1 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS INFECTIONS... 2 MRSA SURVEILLANCE... 3 CLOSTRIDIUM
December 2018 Healthcare-associated Infections Annual Report 2011-2017 TABLE OF CONTENTS INTRODUCTION... 1 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS INFECTIONS... 2 MRSA SURVEILLANCE... 3 CLOSTRIDIUM
TACKLING THE MRSA EPIDEMIC
 TACKLING THE MRSA EPIDEMIC Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine MRSA Trend (HA + CA) in US TSN Database USA (1993-2003) % of MRSA among S. aureus
TACKLING THE MRSA EPIDEMIC Paul D. Holtom, MD Associate Professor of Medicine and Orthopaedics USC Keck School of Medicine MRSA Trend (HA + CA) in US TSN Database USA (1993-2003) % of MRSA among S. aureus
Frequent Carriage of Panton-Valentine Leucocidin Genes by Staphylococcus aureus Isolates from Surgically Drained Abscesses
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2005, p. 3203 3207 Vol. 43, No. 7 0095-1137/05/$08.00 0 doi:10.1128/jcm.43.7.3203 3207.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, July 2005, p. 3203 3207 Vol. 43, No. 7 0095-1137/05/$08.00 0 doi:10.1128/jcm.43.7.3203 3207.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2014
 Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2014 Helen Heffernan, Sarah Bakker, Kristin Dyet, Deborah Williamson Nosocomial Infections Laboratory, Institute of Environmental Science
Annual survey of methicillin-resistant Staphylococcus aureus (MRSA), 2014 Helen Heffernan, Sarah Bakker, Kristin Dyet, Deborah Williamson Nosocomial Infections Laboratory, Institute of Environmental Science
Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital
 Epidemiology J Microbiol Immunol of MRSA Infect. bacteremia 2007;40:310-316 Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital Chih-Yu
Epidemiology J Microbiol Immunol of MRSA Infect. bacteremia 2007;40:310-316 Molecular epidemiology of community-acquired methicillin-resistant Staphylococcus aureus bacteremia in a teaching hospital Chih-Yu
2016 Sabaheta Bektas, Amina Obradovic, Mufida Aljicevic, Fatima Numanovic, Dunja Hodzic, Lutvo Sporisevic
 DOI: 10.5455/msm.2016.28.61-65 Received: 05 December 2015; Accepted: 11 January 2016 2016 Sabaheta Bektas, Amina Obradovic, Mufida Aljicevic, Fatima Numanovic, Dunja Hodzic, Lutvo Sporisevic This is an
DOI: 10.5455/msm.2016.28.61-65 Received: 05 December 2015; Accepted: 11 January 2016 2016 Sabaheta Bektas, Amina Obradovic, Mufida Aljicevic, Fatima Numanovic, Dunja Hodzic, Lutvo Sporisevic This is an
Received 24 July 2008/Accepted 28 July 2008
 JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2008, p. 3222 3227 Vol. 46, No. 10 0095-1137/08/$08.00 0 doi:10.1128/jcm.01423-08 Copyright 2008, American Society for Microbiology. All Rights Reserved. Predominance
JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2008, p. 3222 3227 Vol. 46, No. 10 0095-1137/08/$08.00 0 doi:10.1128/jcm.01423-08 Copyright 2008, American Society for Microbiology. All Rights Reserved. Predominance
Evaluating the Role of MRSA Nasal Swabs
 Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
Evaluating the Role of MRSA Nasal Swabs Josh Arnold, PharmD PGY1 Pharmacy Resident Pharmacy Grand Rounds February 28, 2017 2016 MFMER slide-1 Objectives Identify the pathophysiology of MRSA nasal colonization
*Corresponding Author:
 Original Research Article DOI: 10.18231/2394-5478.2017.0098 Prevalence and factors associated with the nasal colonization of Staphylococcus aureus and Methicillin-Resistant Staphylococcus aureus among
Original Research Article DOI: 10.18231/2394-5478.2017.0098 Prevalence and factors associated with the nasal colonization of Staphylococcus aureus and Methicillin-Resistant Staphylococcus aureus among
Prevalence and Molecular Characteristics of Methicillin-resistant Staphylococcus aureus Isolates in a Neonatal Intensive Care Unit
 Journal of Bacteriology and Virology 2016. Vol. 46, No. 2 p.99 103 http://dx.doi.org/10.4167/jbv.2016.46.2.99 Communication Prevalence and Molecular Characteristics of Methicillin-resistant Staphylococcus
Journal of Bacteriology and Virology 2016. Vol. 46, No. 2 p.99 103 http://dx.doi.org/10.4167/jbv.2016.46.2.99 Communication Prevalence and Molecular Characteristics of Methicillin-resistant Staphylococcus
S aureus infections: outpatient treatment. Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium
 S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
Natural History of Community-Acquired Methicillin-Resistant Staphylococcus aureus Colonization and Infection in Soldiers
 MAJOR ARTICLE Natural History of Community-Acquired Methicillin-Resistant Staphylococcus aureus Colonization and Infection in Soldiers Michael W. Ellis, 1 Duane R. Hospenthal, 1 David P. Dooley, 1 Paula
MAJOR ARTICLE Natural History of Community-Acquired Methicillin-Resistant Staphylococcus aureus Colonization and Infection in Soldiers Michael W. Ellis, 1 Duane R. Hospenthal, 1 David P. Dooley, 1 Paula
Staphylococcus Aureus
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 43: Staphylococcus Aureus Authors J. Pierce, MD M. Edmond, MD, MPH, MPA M.P. Stevens, MD, MPH Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key
Methicillin Resistant Staphylococcus Aureus (MRSA) The drug resistant `Superbug that won t die
 Methicillin Resistant Staphylococcus Aureus (MRSA) The drug resistant `Superbug that won t die Michael A. Miller, MD Assistant Professor of Pediatrics -Jacksonville OBJECTIVES 1. Understand the basic microbiology
Methicillin Resistant Staphylococcus Aureus (MRSA) The drug resistant `Superbug that won t die Michael A. Miller, MD Assistant Professor of Pediatrics -Jacksonville OBJECTIVES 1. Understand the basic microbiology
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust
 PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust Neonatal Case History Neonate born at 26 +2 gestation Spontaneous onset of
PVL Staph aureusjust a skin/soft tissue problem? Layla Mohammadi Lead Pharmacist, Antimicrobials Lewisham Healthcare NHS Trust Neonatal Case History Neonate born at 26 +2 gestation Spontaneous onset of
Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1
 Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Community Onset MRSA Infections in Australia: A Tale of Two Clones Geoffrey Coombs 1, Graeme Nimmo 2, Julie Pearson 1, Samantha Cramer 1 and Keryn Christiansen 1 Community Associated MRSA First isolated
Community-Associated Methicillin-Resistant Staphylococcus aureus: Epidemiology and Clinical Consequences of an Emerging Epidemic
 CLINICAL MICROBIOLOGY REVIEWS, July 2010, p. 616 687 Vol. 23, No. 3 0893-8512/10/$12.00 doi:10.1128/cmr.00081-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Community-Associated
CLINICAL MICROBIOLOGY REVIEWS, July 2010, p. 616 687 Vol. 23, No. 3 0893-8512/10/$12.00 doi:10.1128/cmr.00081-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Community-Associated
The molecular epidemiology of methicillin-resistant Staphylococcus aureus (MRSA) in the major countries of East Asia
 Boston University OpenBU Theses & Dissertations http://open.bu.edu Boston University Theses & Dissertations 2017 The molecular epidemiology of methicillin-resistant Staphylococcus aureus (MRSA) in the
Boston University OpenBU Theses & Dissertations http://open.bu.edu Boston University Theses & Dissertations 2017 The molecular epidemiology of methicillin-resistant Staphylococcus aureus (MRSA) in the
CA-MRSA: How Should We Respond to Outbreaks?
 CA-MRSA: How Should We Respond to Outbreaks? Robert B. Stroube, MD, MPH Medscape Infectious Diseases. 2008; 2008 Medscape Posted 11/05/2008 Introduction to MRSA Methicillin-resistant Staphylococcus aureus
CA-MRSA: How Should We Respond to Outbreaks? Robert B. Stroube, MD, MPH Medscape Infectious Diseases. 2008; 2008 Medscape Posted 11/05/2008 Introduction to MRSA Methicillin-resistant Staphylococcus aureus
ORIGINAL ARTICLE /j x
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01718.x Clonal spread of SCCmec type IV methicillin-resistant Staphylococcus aureus between community and hospital Y. H. Huang 1, S. P. Tseng 1,J.M.Hu 1, J. C.
ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01718.x Clonal spread of SCCmec type IV methicillin-resistant Staphylococcus aureus between community and hospital Y. H. Huang 1, S. P. Tseng 1,J.M.Hu 1, J. C.
Prevalence & Risk Factors For MRSA. For Vets
 For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
For Vets General Information Staphylococcus aureus is a Gram-positive, aerobic commensal bacterium of humans that is carried in the anterior nares of approximately 30% of the general population. It is
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM
 UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
UPDATE ON ANTIMICROBIAL STEWARDSHIP REGULATIONS AND IMPLEMENTATION OF AN AMS PROGRAM Diane Rhee, Pharm.D. Associate Professor of Pharmacy Practice Roseman University of Health Sciences Chair, Valley Health
Epidemiology of Community- Associated (CA) Methicillin-Resistant Staphylococcus aureus (MRSA) in the United States
 Epidemiology of Community- Associated (CA) Methicillin-Resistant Staphylococcus aureus (MRSA) in the United States R. M. Klevens, DDS, MPH Division of Healthcare Quality Promotion Acknowledgements CDC
Epidemiology of Community- Associated (CA) Methicillin-Resistant Staphylococcus aureus (MRSA) in the United States R. M. Klevens, DDS, MPH Division of Healthcare Quality Promotion Acknowledgements CDC
RESEARCH NOTE COMMUNITY-ACQUIRED METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN A MALAYSIAN TERTIARY CENTRE
 RESEARCH NOTE COMMUNITY-ACQUIRED METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN A MALAYSIAN TERTIARY CENTRE Zetti Zainol Rashid 1, Norazlah Bahari 1, Amizah Othman 1, Roslinda Jaafar 1, Nurul Azmawati
RESEARCH NOTE COMMUNITY-ACQUIRED METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS IN A MALAYSIAN TERTIARY CENTRE Zetti Zainol Rashid 1, Norazlah Bahari 1, Amizah Othman 1, Roslinda Jaafar 1, Nurul Azmawati
STAPHYLOCOCCUS AUREUS IS THE
 ORIGINAL INVESTIGATION National Trends in Ambulatory Visits and Antibiotic Prescribing for Skin and Soft-Tissue Infections Adam L. Hersh, MD, PhD; Henry F. Chambers, MD; Judith H. Maselli, MSPH; Ralph
ORIGINAL INVESTIGATION National Trends in Ambulatory Visits and Antibiotic Prescribing for Skin and Soft-Tissue Infections Adam L. Hersh, MD, PhD; Henry F. Chambers, MD; Judith H. Maselli, MSPH; Ralph
Physician Rating: ( 23 Votes ) Rate This Article:
 From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
Typing of Methicillin Resistant Staphylococcus Aureus Using DNA Fingerprints by Pulsed-field Gel Electrophoresis
 Published online: 16/07/2016 Published print:08/2016 ORIGINAL PAPER Typing of Methicillin Resistant Staphylococcus Aureus Using DNA Fingerprints by Pulsed-field Gel Electrophoresis Velma Rebic 1, Ana Budimir
Published online: 16/07/2016 Published print:08/2016 ORIGINAL PAPER Typing of Methicillin Resistant Staphylococcus Aureus Using DNA Fingerprints by Pulsed-field Gel Electrophoresis Velma Rebic 1, Ana Budimir
Community-Associated C. difficile Infection: Think Outside the Hospital. Maria Bye, MPH Epidemiologist May 1, 2018
 Community-Associated C. difficile Infection: Think Outside the Hospital Maria Bye, MPH Epidemiologist Maria.Bye@state.mn.us 651-201-4085 May 1, 2018 Clostridium difficile Clostridium difficile Clostridium
Community-Associated C. difficile Infection: Think Outside the Hospital Maria Bye, MPH Epidemiologist Maria.Bye@state.mn.us 651-201-4085 May 1, 2018 Clostridium difficile Clostridium difficile Clostridium
JAMA. 2003;290:
 ORIGINAL CONTRIBUTION Comparison of Communityand Health Care Associated Methicillin-Resistant Staphylococcus aureus Infection Timothy S. Naimi, MD, MPH Kathleen H. LeDell, MPH, RN Kathryn Como-Sabetti,
ORIGINAL CONTRIBUTION Comparison of Communityand Health Care Associated Methicillin-Resistant Staphylococcus aureus Infection Timothy S. Naimi, MD, MPH Kathleen H. LeDell, MPH, RN Kathryn Como-Sabetti,
Decrease of vancomycin resistance in Enterococcus faecium from bloodstream infections in
 AAC Accepted Manuscript Posted Online 30 March 2015 Antimicrob. Agents Chemother. doi:10.1128/aac.00513-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 Decrease of vancomycin
AAC Accepted Manuscript Posted Online 30 March 2015 Antimicrob. Agents Chemother. doi:10.1128/aac.00513-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 Decrease of vancomycin
Microbiological and Genotypic Analysis of Methicillin-Resistant ACCEPTED. 1. Department of Medicine, New York Medical College, Valhalla, NY
 AAC Accepts, published online ahead of print on 7 July 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00357-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 7 July 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00357-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
Community Associated MRSA Dr. Rachel Gorwitz, CDC A Webber Training Teleclass
 Community-Associated MRSA: What s Up and What s Next? Rachel Gorwitz, MD, MPH Division of Healthcare Quality Promotion Centers for Disease Control and Prevention Learning Objectives Describe the changing
Community-Associated MRSA: What s Up and What s Next? Rachel Gorwitz, MD, MPH Division of Healthcare Quality Promotion Centers for Disease Control and Prevention Learning Objectives Describe the changing
MRSA. ( Staphylococcus aureus; S. aureus ) ( community-associated )
 005 16 190-194 ( Staphylococcus aureus; S. aureus ) ( community-associated ) ( -susceptible Staphylococcus auerus; MSSA ) ( -resistant Staphylococcus auerus; ) ( ) ( -lactam ) ( glycopeptide ) ( Staphylococcus
005 16 190-194 ( Staphylococcus aureus; S. aureus ) ( community-associated ) ( -susceptible Staphylococcus auerus; MSSA ) ( -resistant Staphylococcus auerus; ) ( ) ( -lactam ) ( glycopeptide ) ( Staphylococcus
ORIGINAL ARTICLE /j x
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2008.02064.x Community-associated Staphylococcus aureus infections and nasal carriage among children: molecular microbial data and clinical characteristics G. Sdougkos
ORIGINAL ARTICLE 10.1111/j.1469-0691.2008.02064.x Community-associated Staphylococcus aureus infections and nasal carriage among children: molecular microbial data and clinical characteristics G. Sdougkos
Prevalence and Risk Factor Analysis for Methicillin-Resistant Staphylococcus aureus Nasal Colonization in Children Attending Child Care Centers
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1041 1047 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.02235-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Prevalence
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1041 1047 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.02235-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Prevalence
Rapid Increase of Genetically Diverse Methicillin-Resistant. Staphylococcus aureus, Copenhagen, Denmark
 Rapid Increase of Genetically Diverse Methicillin-Resistant Staphylococcus aureus, Copenhagen, Denmark Mette Damkjær Bartels,* Kit Boye,* Anders Rhod Larsen, Robert Skov, and Henrik Westh* In Copenhagen,
Rapid Increase of Genetically Diverse Methicillin-Resistant Staphylococcus aureus, Copenhagen, Denmark Mette Damkjær Bartels,* Kit Boye,* Anders Rhod Larsen, Robert Skov, and Henrik Westh* In Copenhagen,
Is Cefazolin Inferior to Nafcillin for Treatment of Methicillin-Susceptible Staphylococcus aureus Bacteremia?
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2011, p. 5122 5126 Vol. 55, No. 11 0066-4804/11/$12.00 doi:10.1128/aac.00485-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Is Cefazolin
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2011, p. 5122 5126 Vol. 55, No. 11 0066-4804/11/$12.00 doi:10.1128/aac.00485-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Is Cefazolin
Nasal Carriage Rates of Methicillin Resistant Staphylococcus aureus in Healthy Individuals from a Rural Community in Southeastern United States
 World Journal of Medical Sciences 4 (2): 65-69, 2009 ISSN 1817-3055 IDOSI Publications, 2009 Nasal Carriage Rates of Methicillin Resistant Staphylococcus aureus in Healthy Individuals from a Rural Community
World Journal of Medical Sciences 4 (2): 65-69, 2009 ISSN 1817-3055 IDOSI Publications, 2009 Nasal Carriage Rates of Methicillin Resistant Staphylococcus aureus in Healthy Individuals from a Rural Community
11/22/2016. Antimicrobial Stewardship Update Disclosures. Outline. No conflicts of interest to disclose
 Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices,
 Original Research Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices, 2007-2010 Daniel J. Pallin, MD, MPH Carlos A. Camargo Jr, MD, DrPH Jeremiah D. Schuur,
Original Research Skin Infections and Antibiotic Stewardship: Analysis of Emergency Department Prescribing Practices, 2007-2010 Daniel J. Pallin, MD, MPH Carlos A. Camargo Jr, MD, DrPH Jeremiah D. Schuur,
Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
 Infect Dis Ther (2014) 3:55 59 DOI 10.1007/s40121-014-0028-8 BRIEF REPORT Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
Infect Dis Ther (2014) 3:55 59 DOI 10.1007/s40121-014-0028-8 BRIEF REPORT Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
Resistant Staphylococcus aureus
 Resistant Staphylococcus aureus Infections in the United States: A New Classification, a New Resistance and the Implications for Surveillance, Prevention, and Control by Dawn M. Sievert A dissertation
Resistant Staphylococcus aureus Infections in the United States: A New Classification, a New Resistance and the Implications for Surveillance, Prevention, and Control by Dawn M. Sievert A dissertation
Concise Antibiogram Toolkit Background
 Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Helen Heffernan and Sarah Bakker Nosocomial Infections Laboratory, Institute of Environmental Science and Research Limited (ESR); October 2018
 2017 survey of methicillin-resistant Staphylococcus aureus (MRSA) Helen Heffernan and Sarah Bakker Nosocomial Infections Laboratory, Institute of Environmental Science and Research Limited (ESR); October
2017 survey of methicillin-resistant Staphylococcus aureus (MRSA) Helen Heffernan and Sarah Bakker Nosocomial Infections Laboratory, Institute of Environmental Science and Research Limited (ESR); October
Received 25 July 2006/Returned for modification 29 September 2006/Accepted 11 October 2006
 JOURNAL OF CLINICAL MICROBIOLOGY, Dec. 2006, p. 4436 4440 Vol. 44, 12 0095-1137/06/$08.00 0 doi:10.1128/jcm.01546-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Antimicrobial
JOURNAL OF CLINICAL MICROBIOLOGY, Dec. 2006, p. 4436 4440 Vol. 44, 12 0095-1137/06/$08.00 0 doi:10.1128/jcm.01546-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Antimicrobial
