Adequacy of Early Empiric Antibiotic Treatment and Survival in Severe Sepsis: Experience from the MONARCS Trial
|
|
|
- Beverly Williamson
- 6 years ago
- Views:
Transcription
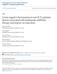
1 BRIEF REPORT Adequacy of Early Empiric Antibiotic Treatment and Survival in Severe Sepsis: Experience from the MONARCS Trial Rodger D. MacArthur, 1 Mark Miller, 2 Timothy Albertson, 3 Edward Panacek, 3 David Johnson, 4 Leah Teoh, 5 and William Barchuk 5 1 Wayne State University, Detroit, Michigan; 5 Abbott Laboratories, Parsippany, New Jersey; 3 University of California, Davis, Sacramento, California; and 2 McGill University, Montreal, and 4 Department of Medicine, Royal University Hospital, Saskatoon, Canada As part of the Monoclonal Anti-TNF: A Randomized Controlled Sepsis (MONARCS) trial, which enrolled patients with suspected sepsis, we sought to determine whether adequate antibiotic therapy was associated with a decreased mortality rate. The study enrolled 2634 patients, 91% of whom received adequate antibiotic therapy. The mortality rate among patients given adequate antibiotic was 33%, versus 43% among patients given inadequate ( P!.001). We conclude that adequate antibiotic therapy results in a significant decrease in the crude mortality rate among patients suspected of sepsis. Sepsis is associated with an in-hospital mortality rate of 30% 40% [1, 2]. The influence of factors such as causative organism, portal of entry, age, or the occurrence of septic shock on the outcome of septicemia has been investigated [3 6]. Early empiric antibiotic of patients suspected of having sepsis is standard practice. Though adequate antibiotic therapy has been shown to reduce mortality rates, this issue has not been studied in detail. By necessity, the association of early empiric antibiotic with mortality in patients with sepsis must be investigated in an observational manner, because ethical considerations preclude a prospective randomized trial. Data from the Monoclonal Anti-TNF: A Randomized Controlled Received 21 March 2003; accepted 11 August 2003; electronically published 22 December Financial support: Abbott Laboratories. Reprints or correspondence to: Dr. Rodger D. MacArthur, Dept. of Medicine, Wayne State University, 4201 St. Antoine, UHC 7D Detroit, MI (rmacarthur@med.wayne.edu). Clinical Infectious Diseases 2004; 38: by the Infectious Diseases Society of America. All rights reserved /2004/ $15.00 Sepsis (MONARCS) trial [7] a double-blind, placebo-controlled trial designed to evaluate the safety and efficacy of afelimomab, an antitumor necrosis factor (TNF) F(ab ) 2 antibody fragment provided the opportunity to determine the relationship between mortality and the adequacy of early empiric antibiotic. In the present study, we analyzed a large group of septic patients for whom detailed data were collected. The aim of the study was to explore the overall association between increased mortality and inadequate empiric. Patients and trial procedures. The MONARCS trial was a multicenter, double-blind, placebo-controlled trial among patients with sepsis. The study included hospitalized adults 118 years old who met criteria for sepsis syndrome [8]. In addition, microbiologic or definitive clinical evidence of acute infection was required for study entry. Neutropenic patients were excluded from enrollment. Patients were randomly allocated to receive either afelimomab or a placebo. Case records for each patient were evaluated in a blinded fashion by a clinical evaluation committee (CEC), using prospectively defined criteria (figure 1). Members of the CEC were blinded to assignment and outcome. There were 7 members of the CEC, of whom 2 were physicians trained in infectious diseases. These 2 physicians (RDM, MM) were primarily responsible for evaluating each case for adequacy of antibiotic therapy. Agreement was obtained by consensus opinion, primarily utilizing the algorithm shown in figure 1. Concordance scoring among evaluators was not performed. Each patient was classified according to primary site of infection, primary causative organism(s), and adequacy of antimicrobial therapy. Therapy was judged to be either adequate or inadequate on the basis of the in vitro susceptibility of an isolated organism and/or the initiation of antibiotic between 24 h before and 72 h after study enrollment. In the absence of sensitivity data for particular organisms and antibiotics utilized, an organism was defined as sensitive if, at that particular institution, 80% of isolates of the relevant pathogen were sensitive to the antibiotic utilized. If data were not listed for the specific antibiotic used, the isolated organism was defined as sensitive if 80% of isolates at the particular institution were susceptible to comparable antibiotics. Organisms reported as intermediate in sensitivity to a particular antibiotic were classified as sensitive for this report. The primary study end point was the 28-day all-cause mortality rate. Data analysis. The Jonckheere-Terpstra test was used to 284 CID 2004:38 (15 January) BRIEF REPORT
2 Figure 1. Algorithm for prospectively determining adequacy of antibiotic therapy. Antibiotics were considered to have expected activity if 180% of clinical isolates were susceptible to them, as determined by published epidemiologic data [16]. evaluate the association between the number of infecting organisms per patient and the adequacy of antibiotic. The Cochran-Mantel-Haenszel test, stratified by, was used to investigate the association between mortality and adequacy of antibiotic therapy for all 2634 patients enrolled. Results. The MONARCS trial was conducted at 157 centers in North America. A total of 2634 patients were enrolled. Details on empiric antibiotic and outcome were ultimately available for all patients. The baseline characteristics of patients who received adequate and inadequate empiric antibiotic therapy are summarized in table 1. Adequate antibiotic was given to 2391 patients (91%). The group receiving adequate antibiotic therapy was slightly younger, but the 2 groups were well balanced for other demographic and baseline characteristics. The most common gram-positive organisms (i.e., those found in 15% of patients) were Staphylococcus aureus and Streptococcus pneumoniae, and the most common gram-negative organisms were Escherichia coli, Klebsiella pneumoniae, and Pseudomonas aeruginosa. In both groups, the most frequent sites of infection were the abdomen, lungs, and blood (i.e., primary bacteremia, in which the blood was the only site of infection identified). Certain isolated organisms (table 1) were associated with inadequate antibiotic s more often than were other organisms. In particular, S. aureus, P. aeruginosa, and fungi were more likely to have been associated with inadequate antibiotic s, which most likely reflects the increase in resistance associated with these organisms in hospitalized patients. The site of infection did not appear to be associated with the adequacy of antibiotic (table 1). However, higher numbers of infecting organisms per patient were significantly associated ( P!.01) with inadequacy of antibiotic (table 2). The mortality rate on day 28 of the study for all randomized patients is summarized in table 3. The overall mortality rate was 34% (898 of 2634 patients). Mortality rates of 33% and 43% were observed among patients receiving adequate and inadequate antibiotic, respectively, and an increased mortality rate was significantly associated with inadequacy of BRIEF REPORT CID 2004:38 (15 January) 285
3 Table 1. Baseline characteristics of 2634 patients with suspected sepsis, according to receipt of adequate or inadequate antibiotic. Variable Patients with adequate Patients with inadequate (n p 243) P a Age in years, mean SD 59.2 (17.0) 61.5 (17.0).05 Sex, % men Clinical evaluation score, mean value APACHE II SAPS II MOD SOFA Septic shock 1564 (65.4) 150 (61.7).25 Pathogen isolated!.01 b Gram-positive bacteria 690 (28.9) 81 (33.3) Staphylococcus aureus 338 (14.1) 47 (19.3) Streptococcus pneumoniae 205 (8.6) 17 (7.0) Gram-negative bacteria 674 (28.2) 59 (24.3) Escherichia coli 369 (15.4) 31 (12.8) Klebsiella pneumoniae 173 (7.2) 19 (7.8) Pseudomonas aeruginosa 116 (4.9) 25 (10.3) Mixed gram-positive and gram-negative bacteria 267 (11.2) 62 (25.5) Other c 45 (1.9) 15 (6.2) None 715 (29.9) 26 (10.7) Site of infection.04 Abdomen 595 (24.9) 67 (27.6) Lung 619 (25.9) 66 (27.2) Blood d 568 (23.8) 68 (28.0) Other or none identified 609 (25.5) 42 (17.3) Positive blood culture result 935 (39.1) 105 (43.2).21 NOTE. Data are no. (%) of patients, unless otherwise indicated. MOD, multiple organ disfunction score; SAPS II, simplified acute physiology score II; SOFA, sequential organ failure assessment score. a P value was calculated using analysis of variance and Pearson s x 2 test. b Gram-positive bacterial infection vs. gram-negative bacterial infection vs. mixed gram-positive and -negative bacterial infection vs. other pathogen vs. no pathogen identified. c E.g., fungus. d Primary bacteremia, in which blood was the only identified site of infection. antibiotic support ( P!.001). Among patients randomized to receive a placebo, those receiving adequate initial empiric antibiotic therapy had a 38% (OR: 1.38) greater chance of being alive on day 28 than did similarly treated patients who were given inadequate antibiotic therapy. The 28-day mortality rate among patients receiving adequate or inadequate antibiotic, stratified by demographic, clinical, and microbiologic variables, is detailed in table 3. With the exception of patients with sepsis that was classified as due to P. aeruginosa or other pathogen, or with sepsis for which no pathogen was isolated, the mortality rate was lower for patients who received adequate empiric antibiotics. Patients with sepsis due to gram-positive bacteria, patients with sepsis due to E. coli, and those with septic shock had the greatest benefit from adequate antibiotic (on the basis of the d for mortality rates between those receiving adequate versus those receiving inadequate antibiotic therapy), with absolute reductions in mortality rates ranging from 22% to 17%. The mortality rate among patients with P. aeruginosa infections who were receiving inadequate antibiotic was slightly lower than that among those given adequate antibiotic, but the number of patients infected by these pathogens was low. The highest mortality rate associated with inadequate antibiotic was observed among patients infected with S. aureus. Discussion. In the MONARCS trial, 91% of enrolled patients received adequate antibiotic support, and the overall mortality rate was 34%, with rates of 33% and 43% for patients 286 CID 2004:38 (15 January) BRIEF REPORT
4 Table 2. No. of infecting organisms per patient in 2634 patients with suspected sepsis, according to receipt of adequate or inadequate antibiotic. No. of organisms isolated With adequate No. (%) of patients With inadequate (n p 243) (29.9) 26 (10.7) (51.1) 113 (46.5) (12.6) 57 (23.5) 3 93 (3.9) 22 (9.1) 4 39 (1.6) 17 (7.0) 5 16 (0.7) 8 (3.3) 6 5 (0.2) 0 (0.0) 7 1 (!0.1) 0 (0.0) receiving adequate and inadequate antibiotic, respectively. Thus, a 10% decrease in the overall crude mortality rate was associated with adequate early empiric antibiotic. With the exception of a small group of patients infected with P. aeruginosa, no subgroup had a prognosis so poor that adequate empiric antibiotic was not beneficial. In fact, reductions in mortality rates were apparent even among patients with septic shock and positive blood culture results, clinical features associated with the highest in-hospital mortality rates [3, 6]. Several factors were associated with a greater likelihood of inadequate antibiotic, including multiple infecting organisms per patient, fungal infection, and P. aeruginosa infection. To the best of our knowledge, the MONARCS trial is the largest prospective, randomized sepsis study yet conducted, and Table 3. Twenty-eight day all-cause mortality rates among 2634 patients with suspected sepsis, according to receipt of adequate or inadequate antibiotic. Variable Mortality rate, proportion (%) of patients With adequate With inadequate (n p 243) Overall mortality 793/2391 (33.2) 105/243 (43.2) Treatment group Afelimomab 364/1174 (31.0) 57/131 (43.5) Placebo 429/1217 (35.3) 48/112 (42.9) Age in years!65 346/1328 (26.1) 42/118 (35.6) /1063 (42.1) 62/124 (50.0) Septic shock 541/1564 (34.6) 77/150 (51.3) Pathogen isolated Gram-positive bacteria 242/690 (35.1) 46/81 (56.8) Staphylococcus aureus 137/338 (40.5) 24/47 (51.1) Streptococcus pneumoniae 65/205 (31.7) 7/17 (41.2) Gram-negative bacteria 207/674 (30.7) 25/59 (42.4) Escherichia coli 104/369 (28.2) 15/31 (48.4) Klebsiella pneumoniae 51/173 (29.5) 8/19 (42.1) Pseudomonas aeruginosa 45/116 (38.8) 9/25 (36.0) Mixed gram-positive and gramnegative bacteria 77/267 (28.8) 22/62 (35.5) Other a 23/45 (51.1) 6/15 (40.0) None 244/715 (34.1) 6/26 (23.1) Site of infection Abdomen 210/595 (35.3) 26/67 (38.8) Lung 222/619 (35.9) 30/66 (45.5) Blood b 204/568 (35.9) 33/68 (48.5) Other or none identified 157/609 (25.8) 16/42 (38.1) Positive blood culture results 321/935 (34.3) 48/105 (45.7) NOTE. Data are no. of patients who died/no. of patients in group or subgroup (%). a E.g., fungus. b Primary bacteremia, in which blood was the only identified site of infection. BRIEF REPORT CID 2004:38 (15 January) 287
5 the detailed data collected on enrolled patients has provided the opportunity to investigate a number of -related questions. Parallel comparison of the results of our study with the results reported by others must be interpreted with caution because of the heterogeneity of patients with sepsis, differences in definitions of adequate antibiotic, and differences in standards of care. Nevertheless, our results are consistent with previous studies [9 13], in which the proportion of patients receiving adequate empiric antibiotic ranged from 63% to 83%. Although our study found that 91% of persons enrolled were treated with adequate antibiotics, the increased rate relative to other studies may have been due to our definition of adequate. In particular, patients for whom no organism was isolated were considered to have received adequate antibiotics if any antibiotic was given during the period between 24 h before and 72 h after study enrollment. In addition, it is likely that classification of organisms that were intermediate in sensitivity as being sensitive increased the number of persons classified as having received adequate antibiotics; the increased use of broader-spectrum antibiotics might also have this effect. Leibovici et al. [14] found that the mortality rate among patients with bacteremia who experienced septic shock was 74.9% for those receiving adequate empiric antibiotic and 84.7% for those receiving inadequate empiric antibiotic. In a separate analysis, these same investigators [15] reported mortality rates for patients with septic bacteremia who did not necessarily experience septic shock: 20% for adequate versus 34% for inadequate antibiotic. Behrendt et al. [11] found similar values, reporting a 15.8% mortality rate for patients with septic bacteremia who received adequate antibiotic and 28.7% for those given inadequate antibiotic. As was the case in the present study, in these analyses [11, 14, 15] there was a decrease of 10% in the mortality rate among patients administered adequate antibiotic compared with that among patients administered inadequate antibiotic. The main limitation on the present investigation is that it was observational and not randomized, and, thus, an unknown risk factor for mortality might have been unequally distributed among the 2 groups. On the other hand, the fact that detailed data were collected in real time for a large group of patients and the fact that the effect of adequate antibiotic trended in one direction support the validity of our interpretation. The present report quantifies the benefit associated with adequate empiric antibiotic therapy. These data suggest that continuing efforts should be aimed at reducing the administration of inadequate empiric antimicrobial to septic patients. References 1. Goldhill DR, Sumner A. Outcome of intensive care patients in a group of British intensive care units. Crit Care Med 1998; 26: Brun-Buisson C, Doyon F, Carlet J, et al. Incidence, risk factors, and outcome of severe sepsis and septic shock in adults. A multicenter prospective study in intensive care units. French ICU Group for Severe Sepsis. JAMA 1995; 274: Roberts F, Geere I, Coldman A. A three-year study of positive blood cultures, with emphasis on prognosis. Rev Infect Dis 1991; 13: McGowan JJ, Barnes M, Finland M. Bacteremia at Boston City Hospital: Occurrence and mortality during 12 selected years ( ), with special reference to hospital-acquired cases. J Infect Dis 1975; 132: Elhanan G, Raz R, Pitlik S, et al. Bacteraemia in a community and a university hospital. J Antimicrob Chemother 1995; 36: Smith R, Meixler S, Simberkoff M. Excess mortality in critically ill patients with nosocomial bloodstream infections. Chest 1991; 100: Panacek E, Marshall JC, Fischkoff S, et al. Neutralization of TNF by a monoclonal antibody improves survival and reduces organ dysfunction in human sepsis: results of the MONARCS trial. Chest 2000; 118: 88S. 8. Bone R, Fisher CJ, Clemmer T, Slotman G, Metz C, Balk R. Sepsis syndrome: a valid clinical entity. Crit Care Med 1989;17: Leibovici L, Samra Z, Konigsberger H, Drucker M, Ashkenazi S, Pitlik S. Long-term survival following bacteremia or fungemia. JAMA 1995; 274: Meyers B, Sherman E, Mendelson M, et al. Bloodstream infections in the elderly. Am J Med 1989; 86: Behrendt G, Schneider S, Brodt H, G J-N, Shah P. Influence of antimicrobial on mortality in septicemia. J Chemother 1999; 11: Byl B, Clevenbergh P, Jacobs F, et al. Impact of infectious diseases specialists and microbiological data on the appropriateness of antimicrobial therapy for bacteremia. Clin Infect Dis 1999; 29: Weinstein M, Towns M, Quartey S, et al. The clinical significance of positive blood cultures in the 1990s: a prospective comprehensive evaluation of the microbiology, epidemiology, and outcome of bacteremia and fungemia in adults. Clin Infect Dis 1997; 24: Leibovici L, Drucker M, Konigsberger H, et al. Septic shock in bacteremic patients: risk factors, features and prognosis. Scand J Infect Dis 1997; 29: Leibovici L, Shraga I, Drucker M, Konigsberger H, Samra Z, Pitlik SD. The benefit of appropriate empirical antibiotic in patients with bloodstream infection. J Intern Med 1998; 244: Lorian V, ed. Antibiotics in laboratory medicine. 4th ed. Baltimore, MD: Williams and Wilkins, CID 2004:38 (15 January) BRIEF REPORT
Received 23 May 2004/Returned for modification 31 August 2004/Accepted 11 October 2004
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2005, p. 760 766 Vol. 49, No. 2 0066-4804/05/$08.00 0 doi:10.1128/aac.49.2.760 766.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 2005, p. 760 766 Vol. 49, No. 2 0066-4804/05/$08.00 0 doi:10.1128/aac.49.2.760 766.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
Bacterial infections complicating cirrhosis
 PHC www.aphc.info Bacterial infections complicating cirrhosis P. Angeli, Dept. of Medicine, Unit of Internal Medicine and Hepatology (), University of Padova (Italy) pangeli@unipd.it Agenda Epidemiology
PHC www.aphc.info Bacterial infections complicating cirrhosis P. Angeli, Dept. of Medicine, Unit of Internal Medicine and Hepatology (), University of Padova (Italy) pangeli@unipd.it Agenda Epidemiology
Combination vs Monotherapy for Gram Negative Septic Shock
 Combination vs Monotherapy for Gram Negative Septic Shock Critical Care Canada Forum November 8, 2018 Michael Klompas MD, MPH, FIDSA, FSHEA Professor, Harvard Medical School Hospital Epidemiologist, Brigham
Combination vs Monotherapy for Gram Negative Septic Shock Critical Care Canada Forum November 8, 2018 Michael Klompas MD, MPH, FIDSA, FSHEA Professor, Harvard Medical School Hospital Epidemiologist, Brigham
Appropriate antimicrobial therapy in HAP: What does this mean?
 Appropriate antimicrobial therapy in HAP: What does this mean? Jaehee Lee, M.D. Kyungpook National University Hospital, Korea KNUH since 1907 Presentation outline Empiric antimicrobial choice: right spectrum,
Appropriate antimicrobial therapy in HAP: What does this mean? Jaehee Lee, M.D. Kyungpook National University Hospital, Korea KNUH since 1907 Presentation outline Empiric antimicrobial choice: right spectrum,
The International Collaborative Conference in Clinical Microbiology & Infectious Diseases
 The International Collaborative Conference in Clinical Microbiology & Infectious Diseases PLUS: Antimicrobial stewardship in hospitals: Improving outcomes through better education and implementation of
The International Collaborative Conference in Clinical Microbiology & Infectious Diseases PLUS: Antimicrobial stewardship in hospitals: Improving outcomes through better education and implementation of
Health Informatics Centre, Division of Community Health Sciences, Dundee, UK
 REVIEW Appropriate vs. inappropriate antimicrobial therapy P. G. Davey and C. Marwick Health Informatics Centre, Division of Community Health Sciences, Dundee, UK ABSTRACT Inappropriate antimicrobial treatment
REVIEW Appropriate vs. inappropriate antimicrobial therapy P. G. Davey and C. Marwick Health Informatics Centre, Division of Community Health Sciences, Dundee, UK ABSTRACT Inappropriate antimicrobial treatment
MAGNITUDE OF ANTIMICROBIAL USE. Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges
 Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control
Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control
Sepsis is the most common cause of death in
 ADDRESSING ANTIMICROBIAL RESISTANCE IN THE INTENSIVE CARE UNIT * John P. Quinn, MD ABSTRACT Two of the more common strategies for optimizing antimicrobial therapy in the intensive care unit (ICU) are antibiotic
ADDRESSING ANTIMICROBIAL RESISTANCE IN THE INTENSIVE CARE UNIT * John P. Quinn, MD ABSTRACT Two of the more common strategies for optimizing antimicrobial therapy in the intensive care unit (ICU) are antibiotic
4/3/2017 CLINICAL PEARLS: UPDATES IN THE MANAGEMENT OF NOSOCOMIAL PNEUMONIA DISCLOSURE LEARNING OBJECTIVES
 CLINICAL PEARLS: UPDATES IN THE MANAGEMENT OF NOSOCOMIAL PNEUMONIA BILLIE BARTEL, PHARMD, BCCCP APRIL 7 TH, 2017 DISCLOSURE I have had no financial relationship over the past 12 months with any commercial
CLINICAL PEARLS: UPDATES IN THE MANAGEMENT OF NOSOCOMIAL PNEUMONIA BILLIE BARTEL, PHARMD, BCCCP APRIL 7 TH, 2017 DISCLOSURE I have had no financial relationship over the past 12 months with any commercial
Konsequenzen für Bevölkerung und Gesundheitssysteme. Stephan Harbarth Infection Control Program
 Konsequenzen für Bevölkerung und Gesundheitssysteme Stephan Harbarth Infection Control Program University of Geneva Hospitals Outline Introduction What data sources are available? AMR-associated outcomes
Konsequenzen für Bevölkerung und Gesundheitssysteme Stephan Harbarth Infection Control Program University of Geneva Hospitals Outline Introduction What data sources are available? AMR-associated outcomes
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs?
 Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Does Screening for MRSA Colonization Have A Role In Healthcare-Associated Infection Prevention Programs? John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control and
Taiwan Crit. Care Med.2009;10: %
 2008 30% 2008 2008 2004 813 386 07-346-8339 E-mail srwann@vghks.gov.tw 66 30% 2008 1 2008 2008 Intensive Care Med (2008)34:17-60 67 2 3 C activated protein C 4 5,6 65% JAMA 1995;273(2):117-23 Circulation,
2008 30% 2008 2008 2004 813 386 07-346-8339 E-mail srwann@vghks.gov.tw 66 30% 2008 1 2008 2008 Intensive Care Med (2008)34:17-60 67 2 3 C activated protein C 4 5,6 65% JAMA 1995;273(2):117-23 Circulation,
Mono- versus Bitherapy for Management of HAP/VAP in the ICU
 Mono- versus Bitherapy for Management of HAP/VAP in the ICU Jean Chastre, www.reamedpitie.com Conflicts of interest: Consulting or Lecture fees: Nektar-Bayer, Pfizer, Brahms, Sanofi- Aventis, Janssen-Cilag,
Mono- versus Bitherapy for Management of HAP/VAP in the ICU Jean Chastre, www.reamedpitie.com Conflicts of interest: Consulting or Lecture fees: Nektar-Bayer, Pfizer, Brahms, Sanofi- Aventis, Janssen-Cilag,
Epidemiology of early-onset bloodstream infection and implications for treatment
 Epidemiology of early-onset bloodstream infection and implications for treatment Richard S. Johannes, MD, MS Marlborough, Massachusetts Health care-associated infections: For over 35 years, infections
Epidemiology of early-onset bloodstream infection and implications for treatment Richard S. Johannes, MD, MS Marlborough, Massachusetts Health care-associated infections: For over 35 years, infections
Antibacterial Resistance: Research Efforts. Henry F. Chambers, MD Professor of Medicine University of California San Francisco
 Antibacterial Resistance: Research Efforts Henry F. Chambers, MD Professor of Medicine University of California San Francisco Resistance Resistance Dose-Response Curve Antibiotic Exposure Anti-Resistance
Antibacterial Resistance: Research Efforts Henry F. Chambers, MD Professor of Medicine University of California San Francisco Resistance Resistance Dose-Response Curve Antibiotic Exposure Anti-Resistance
Barriers to Intravenous Penicillin Use for Treatment of Nonmeningitis
 JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 7 July 2010 J. Clin. Microbiol. doi:10.1128/jcm.01012-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Antimicrobial Stewardship Strategy: Antibiograms
 Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Antimicrobial Cycling. Donald E Low University of Toronto
 Antimicrobial Cycling Donald E Low University of Toronto Bad Bugs, No Drugs 1 The Antimicrobial Availability Task Force of the IDSA 1 identified as particularly problematic pathogens A. baumannii and
Antimicrobial Cycling Donald E Low University of Toronto Bad Bugs, No Drugs 1 The Antimicrobial Availability Task Force of the IDSA 1 identified as particularly problematic pathogens A. baumannii and
An evaluation of the susceptibility patterns of Gram-negative organisms isolated in cancer centres with aminoglycoside usage
 Journal of Antimicrobial Chemotherapy (1991) 27, Suppl. C, 1-7 An evaluation of the susceptibility patterns of Gram-negative organisms isolated in cancer centres with aminoglycoside usage J. J. Muscato",
Journal of Antimicrobial Chemotherapy (1991) 27, Suppl. C, 1-7 An evaluation of the susceptibility patterns of Gram-negative organisms isolated in cancer centres with aminoglycoside usage J. J. Muscato",
Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
 Infect Dis Ther (2014) 3:55 59 DOI 10.1007/s40121-014-0028-8 BRIEF REPORT Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
Infect Dis Ther (2014) 3:55 59 DOI 10.1007/s40121-014-0028-8 BRIEF REPORT Lack of Change in Susceptibility of Pseudomonas aeruginosa in a Pediatric Hospital Despite Marked Changes in Antibiotic Utilization
Development of Drugs for HAP-VAP. Robert Fromtling, MD
 Development of Drugs for HAP-VAP Robert Fromtling, MD Hospital-Acquired & Ventilator- Associated Pneumonia (HAP-VAP) The EMA 2015 roadmap recognizes the need for new antibiotics New drugs for HAP-VAP are
Development of Drugs for HAP-VAP Robert Fromtling, MD Hospital-Acquired & Ventilator- Associated Pneumonia (HAP-VAP) The EMA 2015 roadmap recognizes the need for new antibiotics New drugs for HAP-VAP are
Antibiotic usage in nosocomial infections in hospitals. Dr. Birgit Ross Hospital Hygiene University Hospital Essen
 Antibiotic usage in nosocomial infections in hospitals Dr. Birgit Ross Hospital Hygiene University Hospital Essen Infection control in healthcare settings - Isolation - Hand Hygiene - Environmental Hygiene
Antibiotic usage in nosocomial infections in hospitals Dr. Birgit Ross Hospital Hygiene University Hospital Essen Infection control in healthcare settings - Isolation - Hand Hygiene - Environmental Hygiene
Antimicrobial stewardship in managing septic patients
 Antimicrobial stewardship in managing septic patients November 11, 2017 Samuel L. Aitken, PharmD, BCPS (AQ-ID) Clinical Pharmacy Specialist, Infectious Diseases slaitken@mdanderson.org Conflict of interest
Antimicrobial stewardship in managing septic patients November 11, 2017 Samuel L. Aitken, PharmD, BCPS (AQ-ID) Clinical Pharmacy Specialist, Infectious Diseases slaitken@mdanderson.org Conflict of interest
NUOVE IPOTESI e MODELLI di STEWARDSHIP
 Esperienze di successo di antimicrobial stewardship Bologna, 18 novembre 2014 NUOVE IPOTESI e MODELLI di STEWARDSHIP Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Interventions
Esperienze di successo di antimicrobial stewardship Bologna, 18 novembre 2014 NUOVE IPOTESI e MODELLI di STEWARDSHIP Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Interventions
DETERMINANTS OF TARGET NON- ATTAINMENT IN CRITICALLY ILL PATIENTS RECEIVING β-lactams
 DETERMINANTS OF TARGET NON- ATTAINMENT IN CRITICALLY ILL PATIENTS RECEIVING β-lactams Jan J. De Waele MD PhD Surgical ICU Ghent University Hospital Ghent, Belgium Disclosures Financial: consultancy for
DETERMINANTS OF TARGET NON- ATTAINMENT IN CRITICALLY ILL PATIENTS RECEIVING β-lactams Jan J. De Waele MD PhD Surgical ICU Ghent University Hospital Ghent, Belgium Disclosures Financial: consultancy for
Overview of Nosocomial Infections Caused by Gram-Negative Bacilli
 HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor INVITED ARTICLE Overview of Nosocomial Infections Caused by Gram-Negative Bacilli Robert Gaynes, Jonathan R. Edwards, and the National Nosocomial
HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor INVITED ARTICLE Overview of Nosocomial Infections Caused by Gram-Negative Bacilli Robert Gaynes, Jonathan R. Edwards, and the National Nosocomial
Summary of unmet need guidance and statistical challenges
 Summary of unmet need guidance and statistical challenges Daniel B. Rubin, PhD Statistical Reviewer Division of Biometrics IV Office of Biostatistics, CDER, FDA 1 Disclaimer This presentation reflects
Summary of unmet need guidance and statistical challenges Daniel B. Rubin, PhD Statistical Reviewer Division of Biometrics IV Office of Biostatistics, CDER, FDA 1 Disclaimer This presentation reflects
National Surveillance of Antimicrobial Resistance in Pseudomonas aeruginosa Isolates Obtained from Intensive Care Unit Patients from 1993 to 2002
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Dec. 2004, p. 4606 4610 Vol. 48, No. 12 0066-4804/04/$08.00 0 DOI: 10.1128/AAC.48.12.4606 4610.2004 Copyright 2004, American Society for Microbiology. All Rights
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Dec. 2004, p. 4606 4610 Vol. 48, No. 12 0066-4804/04/$08.00 0 DOI: 10.1128/AAC.48.12.4606 4610.2004 Copyright 2004, American Society for Microbiology. All Rights
Does Early and Appropriate Antibiotic Administration Improve Mortality in Emergency Department Patients with Severe Sepsis or Septic Shock?
 References and Literature Grading Does Early and Appropriate Antibiotic Administration Improve Mortality in Emergency Department Patients with Severe Sepsis or Septic Shock? (9/6/2015) 1. Dellinger, R.P.,
References and Literature Grading Does Early and Appropriate Antibiotic Administration Improve Mortality in Emergency Department Patients with Severe Sepsis or Septic Shock? (9/6/2015) 1. Dellinger, R.P.,
Gram-negative bacteraemia in non-icu patients: factors associated with inadequate antibiotic therapy and impact on outcomes
 Washington University School of Medicine Digital Commons@Becker ICTS Faculty Publications Institute of Clinical and Translational Sciences 2008 Gram-negative bacteraemia in non-icu patients: factors associated
Washington University School of Medicine Digital Commons@Becker ICTS Faculty Publications Institute of Clinical and Translational Sciences 2008 Gram-negative bacteraemia in non-icu patients: factors associated
Treatment Guidelines and Outcomes of Hospital- Acquired and Ventilator-Associated Pneumonia
 SUPPLEMENT ARTICLE Treatment Guidelines and Outcomes of Hospital- Acquired and Ventilator-Associated Pneumonia Antoni Torres, Miquel Ferrer, and Joan Ramón Badia Pneumology Department, Clinic Institute
SUPPLEMENT ARTICLE Treatment Guidelines and Outcomes of Hospital- Acquired and Ventilator-Associated Pneumonia Antoni Torres, Miquel Ferrer, and Joan Ramón Badia Pneumology Department, Clinic Institute
Comparative Clinical Evaluation of the T2Bacteria Panel versus Blood Culture for the Diagnosis of Bacteremia
 Comparative Clinical Evaluation of the T2Bacteria Panel versus Blood Culture for the Diagnosis of Bacteremia MH Nguyen, W Pasculle, PG Pappas, G Alangaden, G Pankey, B Schmitt, M Weinstein, R Widen, D
Comparative Clinical Evaluation of the T2Bacteria Panel versus Blood Culture for the Diagnosis of Bacteremia MH Nguyen, W Pasculle, PG Pappas, G Alangaden, G Pankey, B Schmitt, M Weinstein, R Widen, D
DOES TIMING OF ANTIBIOTICS IMPACT OUTCOME IN SEPSIS? Saravana Kumar MD HEAD,DEPT OF EM,DR MEHTA S HOSPITALS CHENNAI,INDIA
 DOES TIMING OF ANTIBIOTICS IMPACT OUTCOME IN SEPSIS? Saravana Kumar MD HEAD,DEPT OF EM,DR MEHTA S HOSPITALS CHENNAI,INDIA drsaravanakumar.ep@gmail.com JOINT SECRETARY RECOMMENDATIONS: INITIAL RESUSCITATION
DOES TIMING OF ANTIBIOTICS IMPACT OUTCOME IN SEPSIS? Saravana Kumar MD HEAD,DEPT OF EM,DR MEHTA S HOSPITALS CHENNAI,INDIA drsaravanakumar.ep@gmail.com JOINT SECRETARY RECOMMENDATIONS: INITIAL RESUSCITATION
Why should we care about multi-resistant bacteria? Clinical impact and
 Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
Why should we care about multi-resistant bacteria? Clinical impact and public health implications Prof. Stephan Harbarth Infection Control Program Geneva, Switzerland and Ebola (in 2014/2015) Increased
Performance of the TREAT decision support system in an environment with a low prevalence of resistant pathogens
 Journal of Antimicrobial Chemotherapy Advance Access published December 17, 2008 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkn504 Performance of the TREAT decision support system in an environment
Journal of Antimicrobial Chemotherapy Advance Access published December 17, 2008 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkn504 Performance of the TREAT decision support system in an environment
Antimicrobial stewardship: Quick, don t just do something! Stand there!
 Antimicrobial stewardship: Quick, don t just do something! Stand there! Stanley I. Martin, MD, FACP, FIDSA Director, Division of Infectious Diseases Director, Antimicrobial Stewardship Program Geisinger
Antimicrobial stewardship: Quick, don t just do something! Stand there! Stanley I. Martin, MD, FACP, FIDSA Director, Division of Infectious Diseases Director, Antimicrobial Stewardship Program Geisinger
AND MISCONCEPTIONS IN THE MANAGEMENT OF SEPSIS
 MYTHS AND MISCONCEPTIONS IN THE MANAGEMENT OF SEPSIS SEPSISMADE EASY SURVIVINGSEPSIS COOKBOOK SEPSIS ISAPIE MERVYN SINGER BLOOMSBURY INSTITUTE OF INTENSIVE CARE MEDICINE UNIVERSITY COLLEGE LONDON, UK DISCUSSION
MYTHS AND MISCONCEPTIONS IN THE MANAGEMENT OF SEPSIS SEPSISMADE EASY SURVIVINGSEPSIS COOKBOOK SEPSIS ISAPIE MERVYN SINGER BLOOMSBURY INSTITUTE OF INTENSIVE CARE MEDICINE UNIVERSITY COLLEGE LONDON, UK DISCUSSION
Antibiotic treatment in the ICU 1. ICU Fellowship Training Radboudumc
 Antibiotic treatment in the ICU 1 ICU Fellowship Training Radboudumc Main issues Delayed identification of microorganisms Impact of critical illness on Pk/Pd High prevalence of antibiotic resistant strains
Antibiotic treatment in the ICU 1 ICU Fellowship Training Radboudumc Main issues Delayed identification of microorganisms Impact of critical illness on Pk/Pd High prevalence of antibiotic resistant strains
Etiology of blood culture isolates among patients in a multidisciplinary teaching hospital in Kuala Lumpur
 Etiology J Microbiol of blood Immunol culture Infect. isolates in a teaching hospital 2007;40:432-437 Etiology of blood culture isolates among patients in a multidisciplinary teaching hospital in Kuala
Etiology J Microbiol of blood Immunol culture Infect. isolates in a teaching hospital 2007;40:432-437 Etiology of blood culture isolates among patients in a multidisciplinary teaching hospital in Kuala
Collecting and Interpreting Stewardship Data: Breakout Session
 Collecting and Interpreting Stewardship Data: Breakout Session Michael S. Calderwood, MD, MPH Regional Hospital Epidemiologist, Dartmouth-Hitchcock Medical Center March 20, 2019 None Disclosures Outline
Collecting and Interpreting Stewardship Data: Breakout Session Michael S. Calderwood, MD, MPH Regional Hospital Epidemiologist, Dartmouth-Hitchcock Medical Center March 20, 2019 None Disclosures Outline
Duration of antibiotic therapy:
 Duration of antibiotic therapy: How low can you go? Thomas Holland, MD Hilton Head, SC July 2017 Disclosures Consulting: The Medicines Company, Basilea Pharmaceutica Adjudication committee: Achaogen Grant
Duration of antibiotic therapy: How low can you go? Thomas Holland, MD Hilton Head, SC July 2017 Disclosures Consulting: The Medicines Company, Basilea Pharmaceutica Adjudication committee: Achaogen Grant
Successful stewardship in hospital settings
 Successful stewardship in hospital settings Pr Charles-Edouard Luyt Service de Réanimation Institut de Cardiologie Groupe Hospitalier Pitié-Salpêtrière Université Pierre et Marie Curie, Paris 6 www.reamedpitie.com
Successful stewardship in hospital settings Pr Charles-Edouard Luyt Service de Réanimation Institut de Cardiologie Groupe Hospitalier Pitié-Salpêtrière Université Pierre et Marie Curie, Paris 6 www.reamedpitie.com
Source: Portland State University Population Research Center (
 Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Methicillin Resistant Staphylococcus aureus (MRSA) Surveillance Report 2010 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated:
Nosocomial Infections: What Are the Unmet Needs
 Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
Nosocomial Infections: What Are the Unmet Needs Jean Chastre, MD Service de Réanimation Médicale Hôpital Pitié-Salpêtrière, AP-HP, Université Pierre et Marie Curie, Paris 6, France www.reamedpitie.com
Evaluation of a computerized antimicrobial susceptibility system with bacteria isolated from animals
 J Vet Diagn Invest :164 168 (1998) Evaluation of a computerized antimicrobial susceptibility system with bacteria isolated from animals Susannah K. Hubert, Phouc Dinh Nguyen, Robert D. Walker Abstract.
J Vet Diagn Invest :164 168 (1998) Evaluation of a computerized antimicrobial susceptibility system with bacteria isolated from animals Susannah K. Hubert, Phouc Dinh Nguyen, Robert D. Walker Abstract.
Staphylococcus aureus Bacteremia: Comparison of Two Periods and a Predictive Model of Mortality
 288 BJID 2002; 6 (December) Staphylococcus aureus Bacteremia: Comparison of Two Periods and a Predictive Model of Mortality Lucieni de Oliveira Conterno, Sérgio Barsanti Wey and Adauto Castelo Division
288 BJID 2002; 6 (December) Staphylococcus aureus Bacteremia: Comparison of Two Periods and a Predictive Model of Mortality Lucieni de Oliveira Conterno, Sérgio Barsanti Wey and Adauto Castelo Division
Concise Antibiogram Toolkit Background
 Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Background This toolkit is designed to guide nursing homes in creating their own antibiograms, an important tool for guiding empiric antimicrobial therapy. Information about antibiograms and instructions
Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS
 Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care Dell Seton Medical Center at the University of Texas and Seton Healthcare Family Clinical
Give the Right Antibiotics in Trauma Mitchell J Daley, PharmD, BCPS Clinical Pharmacy Specialist, Critical Care Dell Seton Medical Center at the University of Texas and Seton Healthcare Family Clinical
The Impact of meca Gene Testing and Infectious Diseases Pharmacists. Intervention on the Time to Optimal Antimicrobial Therapy for ACCEPTED
 JCM Accepts, published online ahead of print on 7 May 2008 J. Clin. Microbiol. doi:10.1128/jcm.00801-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 7 May 2008 J. Clin. Microbiol. doi:10.1128/jcm.00801-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Period of study: 12 Nov 2002 to 08 Apr 2004 (first subject s first visit to last subject s last visit)
 Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Reply to Fabre et. al
 Reply to Fabre et. al L. Clifford McDonald, 1 Stuart Johnson, 2,3 Johan S. Bakken, 4 Kevin W. Garey, 5 Ciaran Kelly, 6 Dale N. Gerding, 2 1 Centers for Disease Control and Prevention, Atlanta, Georgia;
Reply to Fabre et. al L. Clifford McDonald, 1 Stuart Johnson, 2,3 Johan S. Bakken, 4 Kevin W. Garey, 5 Ciaran Kelly, 6 Dale N. Gerding, 2 1 Centers for Disease Control and Prevention, Atlanta, Georgia;
Guidelines on prescribing antibiotics. For physicians and others in Denmark
 Guidelines on prescribing antibiotics 2013 For physicians and others in Denmark Guidelines on prescribing antibiotics For physicians and others in Denmark 2013 by the Danish Health and Medicines Authority.
Guidelines on prescribing antibiotics 2013 For physicians and others in Denmark Guidelines on prescribing antibiotics For physicians and others in Denmark 2013 by the Danish Health and Medicines Authority.
UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients
 Background/methods: UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients This guideline establishes evidence-based consensus standards for management
Background/methods: UCSF guideline for management of suspected hospital-acquired or ventilatoracquired pneumonia in adult patients This guideline establishes evidence-based consensus standards for management
Surveillance of AMR in PHE: a multidisciplinary,
 Surveillance of AMR in PHE: a multidisciplinary, integrated approach Professor Neil Woodford Antimicrobial Resistance & Healthcare Associated Infections (AMRHAI) Reference Unit Crown copyright International
Surveillance of AMR in PHE: a multidisciplinary, integrated approach Professor Neil Woodford Antimicrobial Resistance & Healthcare Associated Infections (AMRHAI) Reference Unit Crown copyright International
OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS
 HTIDE CONFERENCE 2018 OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS FEDERICO PEA INSTITUTE OF CLINICAL PHARMACOLOGY DEPARTMENT OF MEDICINE, UNIVERSITY OF UDINE, ITALY SANTA
HTIDE CONFERENCE 2018 OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS FEDERICO PEA INSTITUTE OF CLINICAL PHARMACOLOGY DEPARTMENT OF MEDICINE, UNIVERSITY OF UDINE, ITALY SANTA
Summary of the latest data on antibiotic resistance in the European Union
 Summary of the latest data on antibiotic resistance in the European Union EARS-Net surveillance data November 2017 For most bacteria reported to the European Antimicrobial Resistance Surveillance Network
Summary of the latest data on antibiotic resistance in the European Union EARS-Net surveillance data November 2017 For most bacteria reported to the European Antimicrobial Resistance Surveillance Network
Understanding the Hospital Antibiogram
 Understanding the Hospital Antibiogram Sharon Erdman, PharmD Clinical Professor Purdue University College of Pharmacy Infectious Diseases Clinical Pharmacist Eskenazi Health 5 Understanding the Hospital
Understanding the Hospital Antibiogram Sharon Erdman, PharmD Clinical Professor Purdue University College of Pharmacy Infectious Diseases Clinical Pharmacist Eskenazi Health 5 Understanding the Hospital
Urinary Tract Infection Workshop
 Urinary Tract Infection Workshop Diagnosis, sampling, antibiotic selection, recurrence, prophylaxis Nick Francis, Robin Howe, Harry Ahmed Outline Diagnosis and sampling Nick 10 min Choice of antibiotic
Urinary Tract Infection Workshop Diagnosis, sampling, antibiotic selection, recurrence, prophylaxis Nick Francis, Robin Howe, Harry Ahmed Outline Diagnosis and sampling Nick 10 min Choice of antibiotic
10 Golden rules of Antibiotic Stewardship in ICU. Jeroen Schouten, MD PhD intensivist, Nijmegen (Neth) Istanbul, Oct 6th 2017
 10 Golden rules of Antibiotic Stewardship in ICU Jeroen Schouten, MD PhD intensivist, Nijmegen (Neth) Istanbul, Oct 6th 2017 10 golden rules of Antibiotic Stewardship in the ICU ID, Pharma & Micro advice
10 Golden rules of Antibiotic Stewardship in ICU Jeroen Schouten, MD PhD intensivist, Nijmegen (Neth) Istanbul, Oct 6th 2017 10 golden rules of Antibiotic Stewardship in the ICU ID, Pharma & Micro advice
Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts
 Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts Investigational Team: Diane Brideau-Laughlin BSc(Pharm),
Executive Summary: A Point Prevalence Survey of Antimicrobial Use: Benchmarking and Patterns of Use to Support Antimicrobial Stewardship Efforts Investigational Team: Diane Brideau-Laughlin BSc(Pharm),
1/30/ Division of Disease Control and Health Protection. Division of Disease Control and Health Protection
 Surveillance, Outbreaks, and Reportable Diseases, Oh My! Assisted Living Facility, Nursing Home and Surveyor Infection Prevention Training February 2015 A.C. Burke, MA, CIC Health Care-Associated Infection
Surveillance, Outbreaks, and Reportable Diseases, Oh My! Assisted Living Facility, Nursing Home and Surveyor Infection Prevention Training February 2015 A.C. Burke, MA, CIC Health Care-Associated Infection
Critical Appraisal Topic. Antibiotic Duration in Acute Otitis Media in Children. Carissa Schatz, BSN, RN, FNP-s. University of Mary
 Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Running head: ANTIBIOTIC DURATION IN AOM 1 Critical Appraisal Topic Antibiotic Duration in Acute Otitis Media in Children Carissa Schatz, BSN, RN, FNP-s University of Mary 2 Evidence-Based Practice: Critical
Original Articles. K A M S W Gunarathne 1, M Akbar 2, K Karunarathne 3, JRS de Silva 4. Sri Lanka Journal of Child Health, 2011; 40(4):
 Original Articles Analysis of blood/tracheal culture results to assess common pathogens and pattern of antibiotic resistance at medical intensive care unit, Lady Ridgeway Hospital for Children K A M S
Original Articles Analysis of blood/tracheal culture results to assess common pathogens and pattern of antibiotic resistance at medical intensive care unit, Lady Ridgeway Hospital for Children K A M S
Scottish Medicines Consortium
 Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium tigecycline 50mg vial of powder for intravenous infusion (Tygacil ) (277/06) Wyeth 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Suitability of Antibiotic Treatment for CAP (CAPTIME) The duration of antibiotic treatment in community acquired pneumonia (CAP)
 STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship
 Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Methicillin-Resistant Staphylococcus aureus Nasal Swabs as a Tool in Antimicrobial Stewardship Natalie R. Tucker, PharmD Antimicrobial Stewardship Pharmacist Tyson E. Dietrich, PharmD PGY2 Infectious Diseases
Changing trends in clinical characteristics and antibiotic susceptibility of Klebsiella pneumoniae bacteremia
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:595-603 Changing trends in clinical characteristics and antibiotic susceptibility of Klebsiella pneumoniae Miri Hyun, Chang In Noh, Seong Yeol Ryu, and Hyun
ORIGINAL ARTICLE Korean J Intern Med 2018;33:595-603 Changing trends in clinical characteristics and antibiotic susceptibility of Klebsiella pneumoniae Miri Hyun, Chang In Noh, Seong Yeol Ryu, and Hyun
Le infezioni di cute e tessuti molli
 Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Le infezioni di cute e tessuti molli SCELTE e STRATEGIE TERAPEUTICHE Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Treatment of complicated skin and skin structure infections
Int.J.Curr.Microbiol.App.Sci (2017) 6(3):
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 3 (2017) pp. 891-895 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.603.104
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 3 (2017) pp. 891-895 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.603.104
Antibiotic stewardship in long term care
 Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Learning Points. Raymond Blum, M.D. Antimicrobial resistance among gram-negative pathogens is increasing
 Raymond Blum, M.D. Learning Points Antimicrobial resistance among gram-negative pathogens is increasing Infection with antimicrobial-resistant pathogens is associated with increased mortality, length of
Raymond Blum, M.D. Learning Points Antimicrobial resistance among gram-negative pathogens is increasing Infection with antimicrobial-resistant pathogens is associated with increased mortality, length of
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Voluntary Only
 Last Updated: Version 4.4a NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Performance Measure Identifier: Measure Information Form Collected For: CMS Voluntary
Last Updated: Version 4.4a NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Performance Measure Identifier: Measure Information Form Collected For: CMS Voluntary
La sepsi Il ruolo dell antibiotico terapia
 Congresso Nazionale AcEMC Fermo 11-12 Maggio 2017 La sepsi Il ruolo dell antibiotico terapia Michele Bartoletti Infectious Disease Unit - Sant Orsola Hospital, Bologna, Italy Disclosures: none Epidemiology
Congresso Nazionale AcEMC Fermo 11-12 Maggio 2017 La sepsi Il ruolo dell antibiotico terapia Michele Bartoletti Infectious Disease Unit - Sant Orsola Hospital, Bologna, Italy Disclosures: none Epidemiology
College of Medicine, Chang Gung University, Taoyuan, Taiwan. Abstract
 DOI 10.6314/JIMT.2016.27(2).05 2016 27 89-96 Combination Antibiotics for Gram-negative Bacteria in Patients with Healthcare-associated or Hospital-acquired Pneumonia with Severe Sepsis or Septic Shock
DOI 10.6314/JIMT.2016.27(2).05 2016 27 89-96 Combination Antibiotics for Gram-negative Bacteria in Patients with Healthcare-associated or Hospital-acquired Pneumonia with Severe Sepsis or Septic Shock
MDR Acinetobacter baumannii. Has the post antibiotic era arrived? Dr. Michael A. Borg Infection Control Dept Mater Dei Hospital Malta
 MDR Acinetobacter baumannii Has the post antibiotic era arrived? Dr. Michael A. Borg Infection Control Dept Mater Dei Hospital Malta 1 The Armageddon recipe Transmissible organism with prolonged environmental
MDR Acinetobacter baumannii Has the post antibiotic era arrived? Dr. Michael A. Borg Infection Control Dept Mater Dei Hospital Malta 1 The Armageddon recipe Transmissible organism with prolonged environmental
amoxycillin/clavulanate vs placebo in the prevention of infection after animal
 Archives of Emergency Medicine, 1989, 6, 251-256 A comparative double blind study of amoxycillin/clavulanate vs placebo in the prevention of infection after animal bites P. H. BRAKENBURY & C. MUWANGA Accident
Archives of Emergency Medicine, 1989, 6, 251-256 A comparative double blind study of amoxycillin/clavulanate vs placebo in the prevention of infection after animal bites P. H. BRAKENBURY & C. MUWANGA Accident
Objectives. Basic Microbiology. Patient related. Environment related. Organism related 10/12/2017
 Basic Microbiology Vaneet Arora, MD MPH D(ABMM) FCCM Associate Director of Clinical Microbiology, UK HealthCare Assistant Professor, Department of Pathology and Laboratory Medicine University of Kentucky
Basic Microbiology Vaneet Arora, MD MPH D(ABMM) FCCM Associate Director of Clinical Microbiology, UK HealthCare Assistant Professor, Department of Pathology and Laboratory Medicine University of Kentucky
Antimicrobial Stewardship Strategy: Formulary restriction
 Antimicrobial Stewardship Strategy: Formulary restriction Restricted dispensing of targeted antimicrobials on the hospital s formulary, according to approved criteria. The use of restricted antimicrobials
Antimicrobial Stewardship Strategy: Formulary restriction Restricted dispensing of targeted antimicrobials on the hospital s formulary, according to approved criteria. The use of restricted antimicrobials
Recommendations for Implementation of Antimicrobial Stewardship Restrictive Interventions in Acute Hospitals in Ireland
 Recommendations for Implementation of Antimicrobial Stewardship Restrictive Interventions in Acute Hospitals in Ireland A report by the Hospital Antimicrobial Stewardship Working Group, a subgroup of the
Recommendations for Implementation of Antimicrobial Stewardship Restrictive Interventions in Acute Hospitals in Ireland A report by the Hospital Antimicrobial Stewardship Working Group, a subgroup of the
Multi-drug resistant microorganisms
 Multi-drug resistant microorganisms Arzu TOPELI Director of MICU Hacettepe University Faculty of Medicine, Ankara-Turkey Council Member of WFSICCM Deaths in the US declined by 220 per 100,000 with the
Multi-drug resistant microorganisms Arzu TOPELI Director of MICU Hacettepe University Faculty of Medicine, Ankara-Turkey Council Member of WFSICCM Deaths in the US declined by 220 per 100,000 with the
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
TITLE: Recognition and Diagnosis of Sepsis in Rural or Remote Areas: A Review of Clinical and Cost-Effectiveness and Guidelines
 TITLE: Recognition and Diagnosis of Sepsis in Rural or Remote Areas: A Review of Clinical and Cost-Effectiveness and Guidelines DATE: 11 August 2016 CONTEXT AND POLICY ISSUES Sepsis, defined in the 2016
TITLE: Recognition and Diagnosis of Sepsis in Rural or Remote Areas: A Review of Clinical and Cost-Effectiveness and Guidelines DATE: 11 August 2016 CONTEXT AND POLICY ISSUES Sepsis, defined in the 2016
Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days
 Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days Executive Summary National consensus guidelines created jointly by the Infectious Diseases Society of
Treatment Duration for Uncomplicated Community-Acquired Pneumonia: The Evidence in Support of 5 Days Executive Summary National consensus guidelines created jointly by the Infectious Diseases Society of
SHC Clinical Pathway: HAP/VAP Flowchart
 SHC Clinical Pathway: Hospital-Acquired and Ventilator-Associated Pneumonia SHC Clinical Pathway: HAP/VAP Flowchart v.08-29-2017 Diagnosis Hospitalization (HAP) Pneumonia develops 48 hours following: Endotracheal
SHC Clinical Pathway: Hospital-Acquired and Ventilator-Associated Pneumonia SHC Clinical Pathway: HAP/VAP Flowchart v.08-29-2017 Diagnosis Hospitalization (HAP) Pneumonia develops 48 hours following: Endotracheal
S aureus infections: outpatient treatment. Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium
 S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
S aureus infections: outpatient treatment Dirk Vogelaers Dept of Infectious Diseases University Hospital Gent Belgium Intern Med J. 2005 Feb;36(2):142-3 Intern Med J. 2005 Feb;36(2):142-3 Treatment of
Active Bacterial Core Surveillance Site and Epidemiologic Classification, United States, 2005a. Copyright restrictions may apply.
 Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Impact of routine surgical ward and intensive care unit admission surveillance cultures on hospital-wide nosocomial methicillin-resistant Staphylococcus aureus infections in a university hospital: an interrupted
Global Status of Antimicrobial Resistance with a Focus on Nepal
 Global Status of Antimicrobial Resistance with a Focus on Nepal John Ferguson, John Hunter Hospital, University of Newcastle, NSW, Australia Infectious Diseases Physician and Medical Microbiologist SIMON
Global Status of Antimicrobial Resistance with a Focus on Nepal John Ferguson, John Hunter Hospital, University of Newcastle, NSW, Australia Infectious Diseases Physician and Medical Microbiologist SIMON
Jump Starting Antimicrobial Stewardship
 Jump Starting Antimicrobial Stewardship Amanda C. Hansen, PharmD Pharmacy Operations Manager Carilion Roanoke Memorial Hospital Roanoke, Virginia March 16, 2011 Objectives Discuss guidelines for developing
Jump Starting Antimicrobial Stewardship Amanda C. Hansen, PharmD Pharmacy Operations Manager Carilion Roanoke Memorial Hospital Roanoke, Virginia March 16, 2011 Objectives Discuss guidelines for developing
Newsflash: Hospital Medicine JOHN C. CHRISTENSEN, MD FACP AMERICAN COLLEGE OF PHYSICIANS, UTAH CHAPTER SCIENTIFIC MEETING FEBRUARY 10, 2017
 Newsflash: Hospital Medicine JOHN C. CHRISTENSEN, MD FACP AMERICAN COLLEGE OF PHYSICIANS, UTAH CHAPTER SCIENTIFIC MEETING FEBRUARY 10, 2017 Newsflash: Fluoroquinolones Newsflash: Fluoroquinolones Don t
Newsflash: Hospital Medicine JOHN C. CHRISTENSEN, MD FACP AMERICAN COLLEGE OF PHYSICIANS, UTAH CHAPTER SCIENTIFIC MEETING FEBRUARY 10, 2017 Newsflash: Fluoroquinolones Newsflash: Fluoroquinolones Don t
Combating Antibiotic Resistance: New Drugs 4 Bad Bugs (ND4BB) Subtopic 1C. Seamus O Brien and Hasan Jafri Astra Zeneca and MedImmune
 Combating Antibiotic Resistance: New Drugs 4 Bad Bugs (ND4BB) Subtopic 1C Seamus O Brien and Hasan Jafri Astra Zeneca and MedImmune Need for public-private collaboration Challenges of AB R&D: 1. Unique
Combating Antibiotic Resistance: New Drugs 4 Bad Bugs (ND4BB) Subtopic 1C Seamus O Brien and Hasan Jafri Astra Zeneca and MedImmune Need for public-private collaboration Challenges of AB R&D: 1. Unique
Fighting MDR Pathogens in the ICU
 Fighting MDR Pathogens in the ICU Dr. Murat Akova Hacettepe University School of Medicine, Department of Infectious Diseases, Ankara, Turkey 1 50.000 deaths each year in US and Europe due to antimicrobial
Fighting MDR Pathogens in the ICU Dr. Murat Akova Hacettepe University School of Medicine, Department of Infectious Diseases, Ankara, Turkey 1 50.000 deaths each year in US and Europe due to antimicrobial
National Surveillance of Antimicrobial Resistance
 National Surveillance of Antimicrobial Resistance Report to Ministry of Health by Sri Lanka College of Microbiologists SLCM ARSP & NLBSA Technical Committees December 2014 National Surveillance of Antimicrobial
National Surveillance of Antimicrobial Resistance Report to Ministry of Health by Sri Lanka College of Microbiologists SLCM ARSP & NLBSA Technical Committees December 2014 National Surveillance of Antimicrobial
Vaccination as a potential strategy to combat Antimicrobial Resistance in the elderly
 Vaccination as a potential strategy to combat Antimicrobial Resistance in the elderly Wilbur Chen, MD, MS 22-23 March 2017 WHO meeting on Immunization of the Elderly The Problem Increasing consumption
Vaccination as a potential strategy to combat Antimicrobial Resistance in the elderly Wilbur Chen, MD, MS 22-23 March 2017 WHO meeting on Immunization of the Elderly The Problem Increasing consumption
Appropriate Antibiotic Administration in Critically Ill Patients with Pneumonia
 Research Paper Appropriate Antibiotic Administration in Critically Ill Patients with Pneumonia R. A. KHAN, M. M. BAKRY 1 AND F. ISLAHUDIN 1 * Hospital SgBuloh, Jalan Hospital, 47000 SgBuloh, Selangor,
Research Paper Appropriate Antibiotic Administration in Critically Ill Patients with Pneumonia R. A. KHAN, M. M. BAKRY 1 AND F. ISLAHUDIN 1 * Hospital SgBuloh, Jalan Hospital, 47000 SgBuloh, Selangor,
Surveillance of Antimicrobial Resistance among Bacterial Pathogens Isolated from Hospitalized Patients at Chiang Mai University Hospital,
 Original Article Vol. 28 No. 1 Surveillance of Antimicrobial Resistance:- Chaiwarith R, et al. 3 Surveillance of Antimicrobial Resistance among Bacterial Pathogens Isolated from Hospitalized Patients at
Original Article Vol. 28 No. 1 Surveillance of Antimicrobial Resistance:- Chaiwarith R, et al. 3 Surveillance of Antimicrobial Resistance among Bacterial Pathogens Isolated from Hospitalized Patients at
Get Smart For Healthcare
 Get Smart For Healthcare Know When Antibiotics Work Marry Bardin, Quality Improvement Advisor June 9, 2015 Why We Need to Improve In-patient Antibiotic Use Antibiotics are misused in hospitals Antibiotic
Get Smart For Healthcare Know When Antibiotics Work Marry Bardin, Quality Improvement Advisor June 9, 2015 Why We Need to Improve In-patient Antibiotic Use Antibiotics are misused in hospitals Antibiotic
Early Antibiotics for Sepsis and Septic Shock: A Gold Standard
 Early Antibiotics for Sepsis and Septic Shock: A Gold Standard Anand Kumar MD, FRCPC, FCCP, FCCM Professor of Medicine University of Manitoba Health Sciences Centre St. Boniface Hospital Winnipeg, Manitoba
Early Antibiotics for Sepsis and Septic Shock: A Gold Standard Anand Kumar MD, FRCPC, FCCP, FCCM Professor of Medicine University of Manitoba Health Sciences Centre St. Boniface Hospital Winnipeg, Manitoba
Gram-negative bacteraemia; a multi-centre prospective evaluation of empiric antibiotic
 1 2 Gram-negative bacteraemia; a multi-centre prospective evaluation of empiric antibiotic therapy and outcome in English acute hospitals 3 4 5 6 7 8 Jennifer M Fitzpatrick 1, Jason Biswas 2, Jonathan
1 2 Gram-negative bacteraemia; a multi-centre prospective evaluation of empiric antibiotic therapy and outcome in English acute hospitals 3 4 5 6 7 8 Jennifer M Fitzpatrick 1, Jason Biswas 2, Jonathan
Optimize Durations of Antimicrobial Therapy
 Optimize Durations of Antimicrobial Therapy Evidence & Application Jill Cowper, Pharm.D. Division Infectious Diseases Pharmacist Parallon Supply Chain Solutions Richmond, VA P: 607 221 5101 jill.butterfield@parallon.com
Optimize Durations of Antimicrobial Therapy Evidence & Application Jill Cowper, Pharm.D. Division Infectious Diseases Pharmacist Parallon Supply Chain Solutions Richmond, VA P: 607 221 5101 jill.butterfield@parallon.com
Pneumonia considerations Galia Rahav Infectious diseases unit Sheba medical center
 Pneumonia considerations 2017 Galia Rahav Infectious diseases unit Sheba medical center Sir William Osler (1849 1919) "Father of modern medicine Pneumonia: The old man's friend The captain of the men of
Pneumonia considerations 2017 Galia Rahav Infectious diseases unit Sheba medical center Sir William Osler (1849 1919) "Father of modern medicine Pneumonia: The old man's friend The captain of the men of
