Primary care clinicians perceptions about antibiotic prescribing for acute bronchitis: a qualitative study
|
|
|
- Harriet Ellis
- 6 years ago
- Views:
Transcription
1 Primary care clinicians perceptions about antibiotic prescribing for acute bronchitis: a qualitative study The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed Citable Link Terms of Use Dempsey, Patrick P, Alexandra C Businger, Lauren E Whaley, Joshua J Gagne, and Jeffrey A Linder Primary care clinicians perceptions about antibiotic prescribing for acute bronchitis: a qualitative study. BMC Family Practice 15 (1): 2. doi: /s doi: /s December 7, :17:44 PM EST This article was downloaded from Harvard University's DASH repository, and is made available under the terms and conditions applicable to Other Posted Material, as set forth at (Article begins on next page)
2 Dempsey et al. BMC Family Practice 2014, 15:194 RESEARCH ARTICLE Open Access Primary care clinicians? perceptions about antibiotic prescribing for acute bronchitis: a qualitative study Patrick P Dempsey 1, Alexandra C Businger 1, Lauren E Whaley 2, Joshua J Gagne 3 and Jeffrey A Linder 1,4* Abstract Background: Clinicians prescribe antibiotics to over 65% of adults with acute bronchitis despite guidelines stating that antibiotics are not indicated. Methods: To identify and understand primary care clinician perceptions about antibiotic prescribing for acute bronchitis, we conducted semi-structured interviews with 13 primary care clinicians in Boston, Massachusetts and used thematic content analysis. Results: All the participants agreed with guidelines that antibiotics are not indicated for acute bronchitis and felt that clinicians other than themselves were responsible for overprescribing. Barriers to guideline adherence included 6 themes: (1) perceived patient demand, which was the main barrier, although some clinicians perceived a recent decrease; (2) lack of accountability for antibiotic prescribing; (3) saving time and money; (4) other clinicians? misconceptions about acute bronchitis; (5) diagnostic uncertainty; and (6) clinician dissatisfaction in failing to meet patient expectations. Strategies to decrease inappropriate antibiotic prescribing included 5 themes: (1) patient educational materials; (2) quality reporting; (3) clinical decision support; (4) use of an over-the-counter prescription pad; and (5) pre-visit triage and education by nurses to prevent visits. Conclusions: Clinicians continued to cite patient demand as the main reason for antibiotic prescribing for acute bronchitis, though some clinicians perceived a recent decrease. Clinicians felt that other clinicians were responsible for inappropriate antibiotic prescribing and that better pre-visit triage by nurses could prevent visits and change patients? expectations. Keywords: Bronchitis, Respiratory tract infections, Anti-bacterial agents, Primary health care, Qualitative research Background Acute bronchitis is a cough-predominant upper respiratory illness, lasting less than three weeks, in a patient without underlying cardiopulmonary disease [1]. National guidelines and performance measures, based on randomized controlled trials and meta-analyses, recommend avoiding antibiotic prescribing for patients with acute cough/acute bronchitis [2-5]. Over the past several decades, the Centers for Disease Control and Prevention and other organizations have continued efforts to discourage * Correspondence: jlinder@partners.org 1 Division of General Medicine and Primary Care, Brigham and Women?s Hospital, 1620 Tremont Street, Boston, MA 02120, USA 4 Harvard Medical School, Boston, MA, USA Full list of author information is available at the end of the article antibiotic prescribing for acute bronchitis [6]. Despite these efforts, physicians in the United States prescribe antibiotics in over 65% of acute cough/acute bronchitis visits [7,8]. Unnecessary antibiotic prescriptions provide no clinical improvement, expose patients to the risk of adverse drug events, increase the prevalence of antibiotic-resistant bacteria, and increase healthcare costs [9]. Prior studies have assessed clinicians? understanding and attitudes towards antibiotic prescribing for acute bronchitis and other respiratory infections. Most of these studies, summarized in two recent systematic reviews, were performed outside the United States or were published over a decade ago [10,11]. In order to understand contemporary reasons for antibiotic prescribing for acute bronchitis in the United? 2014 Dempsey et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
3 Dempsey et al. BMC Family Practice 2014, 15:194 Page 2 of 10 States, clinicians? familiarity with the clinical guidelines for acute bronchitis, barriers to guideline adherence, and clinicians? views on potential solutions for unnecessary antibiotic prescribing, we conducted semi-structured, qualitative interviews with primary care clinicians. Methods Setting and participants Thirteen primary care clinicians? 12 medical doctors and 1 nurse practitioner? were recruited from 3 Brigham and Women?s Primary Care Practice-Based Research Network-clinics in Boston. The clinics consisted of 1 hospital-based practice and 2 urban community health centers with approximately 175 clinicians which all serve a socioeconomically, racially, and ethnically diverse patient population. Clinicians were recruited via s sent by study staff to practice medical directors of the 3 clinics who, in turn, forwarded the request to primary care clinicians. If clinicians expressed interest in participating, study staff contacted the clinicians and obtained consent to participate. Interviews took place during March Clinicians were internal medicine physicians or internal medicine nurse practitioners, 69% female, with a mean age of 43, and an average of 14 years of experience. Clinicians received US$20 for their participation. The Brigham and Women?s Human Research Committee approved the study protocol. Interview guide development The interview guide was developed as part of an iterative process between our team and a consulting Ph.D.-level, qualitative researcher with extensive training and 12 years of research experience in mixed methods design, field methods, and analysis. We used conceptual models of guideline adherence [12] and appropriate antibiotic prescribing [13] to develop the interview guide, ensuring that a range of concepts would be included. The guide focused on the following goals and domains (Appendix 1): 1. Understand clinicians? contemporary views on acute bronchitis guidelines and antibiotic prescribing; 2. Identify what clinicians felt were the main barriers to antibiotic guideline adherence; 3. Seek clinicians? ideas and suggestions for methods of improvement for the management of acute bronchitis, clinic workflow, and patient education materials. Interview conduct Interviews were conducted by a medical anthropologist with a Masters Degree in Applied Socio-Cultural Anthropology and 17 years experience in conducting qualitative research interviews. Interviews were completed over the phone and lasted between 30 and 60 minutes. The interviewer obtained IRB-approved verbal informed consent to conduct and record the interview as well as use the content of the interview for analysis and publication. The interviewer generally followed the interview guide, asked open-ended questions, but also improvised questions to elicit additional responses or clarify prior responses. If the participant did not offer solutions for domain 3, the interviewer mentioned specific potential interventions included in the interview guide. We conducted 13 interviews to collect general assessments of attitudes regarding acute bronchitis, reasons for antibiotic prescribing, and solutions to reduce antibiotic prescribing for acute bronchitis. Preliminary analysis of the interviews suggested we were approaching thematic saturation after 12 interviews. Data collection and analysis Each interview was recorded, transcribed verbatim, and analyzed according to a conventional comprehensive qualitative analysis method [14-17]. We used a two-stage coding process: structural coding (Level 1) and thematic coding (Level 2). Structural coding followed the structure of the interview guide: every question received a structural code that was applied to the appropriate text. Thematic coding was based on themes that arose from the structural coding, and was applied in a second-pass analysis. Thematic analysis was inductive and followed the structure of the interview. The thematic content analysis was at the question level, such that themes emerged from the questions. We resolved differences in interpretation through discussion. We used NVivo (Version 8, QSR International) to code, categorize, search, retrieve, attach analytical memos and create conceptual relationship networks in our textual data that had been taxonomically coded. Once the 2-stage coding process was completed and reviewed by the entire research team, we generated a comprehensive thematic analysis summary report, including exemplary quotes. The analysis was performed and the summary report was written and delivered by the same experienced qualitative researcher that completed the interviews. In this manuscript, we organized themes by decreasing number of participants who discussed each theme. While this provides quantitative impression of the frequency with which participants discussed each theme, we do not mean to imply that themes with a higher number of discussants are necessarily more important. Results Twelve themes emerged from the data within the 3 interview guide domains. Within the first domain,? contemporary views on acute bronchitis guidelines and antibiotic prescribing?, there was only 1 consistent theme. Within the second domain,? barriers to guideline adherence?, there were 6 themes. Within the third domain,? methods to reduce antibiotic prescribing?, there were 5 themes (Table 1).
4 Dempsey et al. BMC Family Practice 2014, 15:194 Page 3 of 10 Table 1 Domains and themes regarding antibiotic prescribing for acute bronchitis Domain Theme Contemporary views on acute bronchitis guidelines and antibiotic prescribing Barriers to guideline adherence Methods to reduce antibiotic prescribing 1. Antibiotics are not indicated for acute bronchitis, but antibiotics are overprescribed 1. Perceived patient demand for antibiotics 2. Lack of accountability or feedback about prescribing 3. Time and money 4. Other clinicians? misconceptions about acute bronchitis 5. Diagnostic uncertainty and defensive practice 6. Clinician dissatisfaction with not meeting patient expectations 1. Patient handouts and other educational materials 2. Quality reports 3. Clinical decision support 4. Pre-visit triage by nurses 5. Over-the-counter prescription pad Domain 1: Contemporary views on acute bronchitis guidelines and antibiotic prescribing The consistent theme that emerged regarding guidelines and antibiotic prescribing for acute bronchitis was that all participants agreed with guidelines stating that antibiotics are not indicated for acute bronchitis and clinicians felt like antibiotics for acute bronchitis were overprescribed by other clinicians, but not by themselves. One participant stated the guidelines were,?fantastic,?cause I think there IS a lot of unnecessary prescribing? for colds, for bronchitis, for viral illnesses. So I think that having a guideline might also be helpful in terms of communicating that to patients, and explaining, you know,?not only do I feel this way, but this is a guideline set up for us? by the people in charge of treating??. (AB013-MD) Well established guidelines allowed clinicians to avoid prescribing antibiotics by having an authoritative norm that states antibiotics are not necessary. Despite the availability of guidelines, clinicians felt that other clinicians overused antibiotics. Domain 2: Barriers to guideline adherence Perceived patient demand for antibiotics (12 participants) All but one participant cited patient demand as a reason for prescribing antibiotics for acute bronchitis. Responses were similar among participants, commonly referring to the clinic visit being the logical next step after the patient has tried everything else:? I think the patient?s expectation? by the time they?ve come to you, they feel they?ve tried everything else and they want antibiotics, so that?s abigdriver?. (AB002-MD) One other participant attributed this to living,?? in an instant gratification society, and I think [patients] have the impression that an antibiotic is the thing that?ll clear it up really quickly?. (AB003-MD) Another clinician stated,?i don?t blame them; I blame us. They?re used to it, so, they feel like? they bother to come in, so we should deliver?. (AB007-MD) Clinicians felt their patients come to the clinic as a final option, expecting the clinician to provide a quick solution. Two clinicians mentioned serving patients from cultures where antibiotics are over-the-counter and frequently used:? Most of my patients are Spanish-speaking; most of them are from other cultures. You know, antibiotics are available over the counter, most places that they live. You can get?em over the counter, down at the little bodega, down at the corner? People go get it, you can buy ampicillin there. You know, and people are used to taking antibiotics all the time, for everything?. (AB013-MD) Differing cultural norms lead clinicians to feel that certain populations have an even greater expectation of receiving antibiotics. Six clinicians indicated patient demand had decreased over the last 5 years:?i think it?s much? lower than it used to be. I think people kind of? get it, at least for colds. I think for bronchitis, they still think a bit differently about bronchitis than they do about colds, and so if we use the word?bronchitis,? they are a bit more set up to expect antibiotics. But, I would say most people are fairly accepting of the fact that these things are caused by viruses, and they don?t respond to antibiotics. So, I would say, you know? a fairly significant majority? are okay with that?. (AB010-MD) Clinicians perceived that public desire for antibiotics for acute bronchitis has decreased. Clinicians attributed this to the public developing a better understanding of
5 Dempsey et al. BMC Family Practice 2014, 15:194 Page 4 of 10 the nature of viruses and antibiotics, but still associated the diagnosis? bronchitis? with a need for an antibiotic. Lack of accountability or feedback about prescribing (10) Eight participants stated that there was no accountability, oversight, or feedback for prescribing antibiotics that they were aware of.?i don?t think I would NOTICE the difference, really, if I? prescribe antibiotics or not? I don?t have any kind of quality measures? that so far I?ve had to? I haven?t really had anyone say anything about it to me?. (AB011-MD) Two participants felt no direct accountability except from their own conscience and their responsibility to the public to not contribute to increases in the prevalence of antibiotic-resistant bacteria. One said,? I think we?re accountable to? the public, to not render certain antibiotics? powerless, because we?re contributing to the development of resistant organisms?. (AB005-MD) Time and money (7) Seven participants acknowledged financial and time-saving incentives that encourage antibiotic prescribing. One participant said that,?if you do it, you can see more patients, because you end the visit quicker instead of having a long discussion, trying to get their buy-in to not prescribe. So, actually, yes, in essence [there are time and financial incentives]; but not in the? we-get-paid-to-use-this-drug-stuff-[way]?. (AB007-MD) Participants felt that simply prescribing an antibiotic rather than educating the patient meant they could end each encounter faster, see more patients, and be more financially productive. All clinicians who cited time or money as a reason for antibiotic prescribing said that they, themselves, do not do this. Other clinicians? misconceptions about acute bronchitis (6) Clinicians felt some of their colleagues did not understand acute bronchitis or were stuck in the habit of prescribing antibiotics for acute bronchitis. Three participants stated that some doctors either do not know or do not believe that acute bronchitis is viral. One participant felt,? many physicians believe that? many of the bronchitises are caused by bacterial infections? especially when the sputum is green, which is not really true?. (AB002-MD) Another clinician stated that it is more common amongst,?doctors that have been practicing for a long time, it?s sort of what they?ve always done. And so, changing behavior is always harder. It?s what they?ve always done and what they?ve seen their colleagues do, and what their patients have asked them to do. And I think changing those behaviors is very challenging?. (AB001-MD) Two participants stated that some clinicians might believe antibiotics are the correct treatment:?i expect there might be some physicians who actually believe that it?s helpful. Not? putting myself in that category. But that they believe that it?s the right treatment?. (AB004-MD) Lastly, one participant felt some clinicians perceive antibiotics as harmless:? I think the other thing that?s probably misinformation on physicians? part is that I think a lot of? and I?m guilty of this, too. I think we think they?re kind of harmless?. what?s the worst that happens if a person was on a course of antibiotics and, they didn?t need it?? (AB008-MD) Participants felt there were three main reasons other clinicians prescribed antibiotics for acute bronchitis: thinking that acute bronchitis is caused by bacteria; the fixed behavior of antibiotic prescribing; and thinking that antibiotic prescribing for acute bronchitis is benign. Diagnostic uncertainty and defensive practice (4) Four participants stated that diagnostic uncertainty influenced their decision to prescribe antibiotics. One clinician stated,?the physician can never be 100% sure it?s not a bacterial infection, so they worry about that. So there?s some clinical uncertainty?. (AB002-MD) Another participant elaborated on practicing defensively:? The guidelines, even though I think they?re wellknown, there?s certainly variation in uptake around the fact that? for those kind of question mark calls, people practice defensively and might want to just?? be on the safe side, give someone antibiotics,? even though it?s not clear to me that that?s actually the safer choice to do?. (AB012-MD)
6 Dempsey et al. BMC Family Practice 2014, 15:194 Page 5 of 10 Participants felt that despite well-established guidelines to avoid antibiotic prescribing for acute bronchitis, there will always be some diagnostic uncertainty and associated risk of undertreating an infection when they do not prescribing antibiotics. Clinician dissatisfaction in not meeting patient expectations (3) Three participants discussed antibiotic prescribing as a response to clinician dissatisfaction in failing to meet perceived patient expectations. One clinician stated,?a person who has? taken off work? come in to urgent care, and then for me to turn?em around and say,?keep doin? what you?re already doing,? I think in some ways doesn?t feel very satisfying as a physician?. (AB003-MD) Another clinician stated,?if somebody is sick enough to come in? they?re expecting something? Ithinkdoctorsliketodosomething.You don?t liketothinkthereisnothingyoucando,andthere?s nothing you can offer?. (AB005-MD) Clinicians felt that once a patient makes the effort to come into the clinic it is unsatisfying to not be able to offer a solution. Domain 3: Methods to reduce inappropriate prescribing Patient handouts and other educational materials (13) All clinicians felt it would be helpful to have educational materials for patients that describe the importance of avoiding unnecessary antibiotic use. The majority of responses stated educational materials? would be really helpful? (AB008-MD) and would impact prescribing in a? huge? way (AB011-MD). Three clinicians felt educational posters are or would be useful in addition to handouts:?i think it would be great? [I have] the one that says,?antibiotics don?t work for colds and flu.? Got that right next to? where my head is, so people, when they?re looking at me, they see the thing saying,?antibiotics are not for you??. (AB009-MD) Clinicians felt that handouts and posters could make for an efficient, established, official-looking means to educate patients about why antibiotics are not needed for acute bronchitis. One clinician felt that mass media coverage of the issue would be more useful than handouts:? I?m always hesitant to hit? with handouts and pamphlets? I don?t think that people really pay attention to that? they?re already kind of in the office. And if they?re in the office, you can just have the conversation? The only way people read about things related to their health is? they?re picking up? magazines, like? Self,orCosmo,orHealth,or, reading The [Boston] Globe, reading The Metro, so? maybe just putting those kind of informational type pieces, in mass media could help?. (AB003-MD) Participants felt that mass media coverage of the issue would be more useful than posters and handouts given in the clinic because they are more attention-getting and have the potential to prevent visits in the first place. Quality reports (10) Ten clinicians felt quality and feedback reports and reviews would be helpful. One clinician stated,? that everyone should get their [upper respiratory infection] dashboard? and they should be compared to all their peers in their clinic? in their system? and that it should be publicly available? to patients and supervisors?. (AB012-MD) Two clinicians thought group feedback would be useful:?[it would be] good at the clinic, then you don?t sort of demonize somebody, and you get to have the education as a group of clinicians in the clinic?. (AB008-MD) One clinician recommended the pharmacy track prescribing:?i knowthepharmacypeople? track what we prescribe? specifically, whether it?s generic or name brand? they track these measures and so? they could track who[is] prescribing?.antibiotics? Having evidence, like? the number of times that you prescribed antibiotics; these are the cases where you did it?. (AB013-MD) Participants responded that ongoing comparison to their peers and pharmacy tracking could provide ongoing encouragement in lowering antibiotic prescribing rates for acute bronchitis. Clinical decision support (8) Six participants recommended prompts against antibiotics through clinical decision support within the electronic health record. One specifically mentioned an earlier documentation-based clinical decision support prototype:?when we had [an earlier form of electronic clinical decision support], that made it really easy, in my opinion, to be able to? more easily flow through these
7 Dempsey et al. BMC Family Practice 2014, 15:194 Page 6 of 10 visits? because it had these prompts? that were a little reminder? not only did it have the reminders, but then it had all the kind of symptomatic treatment stuff that you could just print out with a click of a button, like, give them the cough syrup and the Tylenol and the this and the that and the patient handouts on it? I really liked that form, and I wish it hadn?t gone away?. (AB012-MD) Two clinicians recommended that the system have clinicians click an indication which reviews the antibiotic order before being accepted, both comparing it to the way radiology ordering is done. Participants indicated that clinical decision support had been and could be a useful tool to reduce inappropriate antibiotic prescribing for acute bronchitis. Having an established means of reviewing best practices, receiving alternative prescription options, and ready-to-print patient information packets had been useful in the past. Pre-visit triage and education by nurses (6) Six clinicians suggested having nurses? Registered Nurses or Licensed Practical Nurses? perform pre-visit triage to reduce unnecessary visits. One clinician stated:?i think a lot of people who have respiratory infections automatically think they need to see a doctor because they think they need a prescription. And? really good education from the? nurses on triage, I think, could actually? do a good job of not even bothering to bring these people in?. (AB001-MD) Another clinician added,?there has to be some way of identifying those patients so that you don?t? bring them in to the clinic, because I think that there?s a message in bringing somebody into the clinic that we?re actually going to do something that you couldn?t doathome?. (AB005-MD) Clinicians expressed that having nurses perform previsit triage would be very useful in reducing inappropriate prescribing. Once a patient has made the trip to the clinic it is far more difficult to convince them to simply continue doing the same things. Clinicians thought review and confirmation by triage nurses that the patient was already taking the right steps and did not need to come into the clinic could reduce visits and antibiotic prescribing. However, three clinicians recommended caution and a potential unintended consequence of pre-visit triage.? You don?t wantpeopletofeellikethey?re getting prejudged as not sick, because then they?re going to come in even more defensive about BEING sick? I?m notsurei?d want somebody that sort of primed? to think they?re not going to get antibiotics, because they?re going to get more geared up?. (AB007-MD) Over the counter prescription pad (2) Over-the-counter prescription pads are official-looking, pre-printed forms on which clinicians can quickly recommend non-antibiotic, non-prescription remedies to patients. Two participants endorsed using an over-thecounter prescription pad.? I like having the over-the-counter medication kind of prescription pad? because one nice thing about it is, it shows the different classes of medications. Like, I think people say,?oh, I just took the cold stuff,? but they don?t really know the difference between a pain reliever and a decongestant, and an antibiotic and kind of understanding, well,?did what you picked out, match what your complaints and symptoms are??? (AB003-MD) The second clinician used the over-the-counter prescription pad to put the encounter,?in a positive light. You can spin things anyway,?well, the really good news is, you don?t actually need to take an antibiotic. Your body can fight this off, we can help it, you know, with these ways??. (AB005-MD) The over-the-counter prescription pad provides an established, official-looking means to do something for the patient without having to prescribe antibiotics. Discussion We conducted qualitative, semi-structured interviews of primary care clinicians to learn about clinicians? understanding about acute bronchitis guidelines, barriers to guideline adherence, and thoughts about interventions to decrease antibiotic prescribing for acute bronchitis. All clinicians agreed with guidelines that antibiotics are not indicated for acute bronchitis. Clinicians perceived that patients continued to have a high level of demand for antibiotics, which remained the largest perceived driver of antibiotic prescribing for acute cough/ acute bronchitis. Clinicians wanted to justify patients? efforts and feel satisfied that they are meeting patients? expectations. A novel finding was that clinicians noted less demand for antibiotics and better patient understanding in the past five years. Clinicians generally viewed the problem of antibiotic prescribing for acute bronchitis and solutions
8 Dempsey et al. BMC Family Practice 2014, 15:194 Page 7 of 10 to address the problem as being someone else?s responsibility. Participants felt that other clinicians, especially older clinicians, think antibiotics are harmless. Participants mentioned that better pre-visit triage by nurses to identify patients who do not need to make a visit would save patients money, avoid the inconvenience of an unnecessary visit, and decrease overall antibiotic prescribing. Participants generally did not say that clinicians could do a better job coaching and educating patients themselves. Comparison with prior qualitative studies Prior qualitative studies of clinicians? attitudes towards antibiotic prescribing for respiratory infections were mainly done in Europe or in the United States over 10 years ago. Two recent systematic reviews identified 45 individual studies that examined clinicians? views of antibiotic prescribing for respiratory infections [10,11]. Only 3 reviewed studies examined prescribing for respiratory infections in the United States in the past decade [18-20]. Mangione-Smith and colleagues found that physicians incorrectly perceive patient questioning about whether or not they need antibiotics as indicating a desire for antibiotics, when in fact questioning was not associated with patient desire for antibiotics [18]. Ong and colleagues found that physicians correctly identified only 27% of patients who wanted antibiotics, but that physician perception of patient desire for antibiotics was the main driver of antibiotic prescribing [19]. Hart and colleagues found that physicians try to balance their own individual? best practice? with perceived patient satisfaction by using education, negotiation, holding-firm, or giving-in [20]. Not included in the systematic reviews, was one newer qualitative study by Ackerman and colleagues [21]. Ackerman and colleagues, as part of a randomized controlled trial of print and electronic-delivered decision support to encourage judicious antibiotic prescribing, found improved awareness of antibiotic resistance, but clinicians still cited patient expectations, time pressure, and diagnostic uncertainty as barriers to judicious antibiotic prescribing [22]. Some of the many qualitative studies from Europe highlight similar themes from our study and other studies regarding antibiotic prescribing for acute cough. These studies describe non-medical reasons for antibiotic prescribing such as the physician having previously missed a diagnosis of pneumonia in a different patient, patient expectations, and maintaining patient satisfaction [23-26]. European studies describe clinical reasons for prescribing antibiotics such as diagnostic uncertainty, fear of making an error of omission (i.e., not prescribing an antibiotic when it was indicated), and reliance on certain clinical factors like lung findings, fever, shortness of breath, sputum production, or crackles [26,27]. One multinational European study by Brookes- Howell and colleagues highlighted international variations in guidelines, systems to reduce patients? expectation for antibiotics, and availability of antibiotics without a prescription [25]. Recently, a study by Mustafa and colleagues found that Welsh primary care physicians, rather than directly asking about patient desire for antibiotics, preferred to use a?running commentary? during the physical examination? reviewing findings and implications with the patient as they are examined to reassure, share information, and strategically educate? to set patient expectations that an antibiotic prescription was not necessary without appearing curt or dismissive [18,28,29]. Limitations Our qualitative study has several limitations. First, clinicians were academically-affiliated and those who agreed to participate may have a particular interest in judicious antibiotic prescribing or be less likely to prescribe antibiotics. Second, participants may have been constrained by the content of the interview guide or given socially desirable answers. However, to avoid topic constraint or social desirability, the interviewer asked openended questions and encouraged participants to speak broadly. Third, our sample size was relatively small. However, the low number of emergent themes suggests we approached thematic saturation. Fourth, many of the themes discussed were about participants? views on other clinicians? attitudes and behavior, which may or may not reflect other clinicians? actual attitudes and behavior. Implications for clinical practice and practice improvement If the patient has an acute cough, is not immunosuppressed, does not have a concomitant alternative diagnosis, has normal vital signs and a normal lung exam, antibiotics are not indicated [1]. Despite clinicians? perception that patients are only interested in antibiotics, other studies have shown that clinicians overestimate this desire and poorly predict which patients want antibiotics [19,30,31]. Clinicians should be educated that antibiotic prescribing is, at most, marginally associated with patient satisfaction [19,31-33]. Future guidelines should address the role of explicit and perceived patient demand in antibiotic prescribing. Ongoing education and patient-directed materials such as handouts, posters, and over-the-counter prescription pads may further decrease perceived patient demand for antibiotics [34]. Outside of clinic visits, as suggested by our study, improved quality reports? although prior studies about monitoring and feedback are conflicting [35-37]? and pre-visit interventions should continue to be evaluated to decrease inappropriate antibiotic
9 Dempsey et al. BMC Family Practice 2014, 15:194 Page 8 of 10 prescribing for acute bronchitis [38]. Accurate point of care tests, which were not addressed in our study, might be acceptable to clinicians and patients [39,40]. Clinicians should feel secure in their decision that antibiotics are not indicated, should not assume patients want antibiotics, and consider using the? running commentary? method to educate and reassure as they do the physical examination [28,29,41]. Additionally, as our participants pointed out and as previously described, clinicians might consider using a term other than? acute bronchitis?, like a? chest cold?, which is accurate, but less associated with patient expectation for antibiotics [42,43]. Rather than focusing on antibiotics, clinicians should focus on symptomatic treatment and educating patients at the time of the visit about realistic expectations for the duration of cough, which lasts, on average, three weeks [18,44]. Conclusions In our qualitative study to understand contemporary attitudes regarding acute bronchitis in the United States, we found that clinicians agreed with antibiotic prescribing guidelines for acute bronchitis, felt that patient demand remained the main driver of antibiotic prescribing, but that demand may have lessened recently. Clinicians discussed a range of solutions to decrease antibiotic prescribing. Many of the solutions discussed were done by someone other than the treating clinician, like nurses doing better pre-visit triage and education, or? behind the scenes? solutions, such as clinical decision support and feedback. However, clinicians will continue to address patients with acute bronchitis and are an integral part of implementing solutions to decrease inappropriate antibiotic prescribing. Appendix 1 Interview guide summary Questions for Clinicians? Understanding of Antibiotic Treatment for Acute Cough in Primary Care Guidelines for antibiotic prescribing 1. Do you have any insight into why antibiotics are overprescribed for acute bronchitis? 2. What do you think of the guidelines? 3. What has your experience been in following the guidelines? How rigid or flexible do you feel they are? 4. Is there any accountability for following or not following them? 5. Are there any financial incentives for or against prescribing antibiotics? 6. Are there instances in which clinicians bend the guidelines? Clinicians? perception of patient desire and demand for antibiotics 1. What do clinicians perceive as patients? level of desire for and demand for antibiotics? 2. What steps could clinicians at the clinic level take to reduce the over prescribing of antibiotics? Clinic workflow 1. Can you think of ways that the clinic workflow could be changed to reduce the prescribing rate of antibiotics? a) For example, could changes be made before, during, or after the patient visit? Let me offer a couple of other suggestions for you to discuss as potential solutions 1. Clinician decision support 2. Quality reports 3. Patient education Review of draft education materials 1. What do you think of Additional file 1? 2. What do you think of Additional file 2? 3. What suggestions do you have for improving Additional file 1? 4. What suggestions do you have for improving Additional file 2? 5. Would it be appropriate to educate patients as part of the counseling about the importance of not taking too many antibiotics? Final section 1. How do you feel about having a patient handout to give to patients at the end of a visit that details the symptomatic treatment for cough? Additional files Additional file 1: Clinician Handout for Patients. Additional file 2: The Centers for Disease Control and Prevention Get Smart Owl. Competing interests The authors declare that they have no competing interests. Authors? contributions PPD, ACB, and LEW participated in study design, development of the interview guide, study coordination, data analysis, and drafting of the manuscript. JJG conducted the interviews and the initial data analysis. JAL conceived of the study, supervised all aspects of the study, and drafted the manuscript. All authors read and approved the final manuscript.
10 Dempsey et al. BMC Family Practice 2014, 15:194 Page 9 of 10 Acknowledgements The authors thank Katherine Taylor Haynes (KTH), PhD for her expertise in developing the interview guide. Support This project was funded by the Agency for Healthcare Research and Quality (R18 HS018419). Author details 1 Division of General Medicine and Primary Care, Brigham and Women?s Hospital, 1620 Tremont Street, Boston, MA 02120, USA. 2 Bureau of Infectious Diseases, Massachusetts Department of Public Health, Boston, MA, USA. 3 Survey and Data Management Core, Dana Farber Cancer Institute, Boston, MA, USA. 4 Harvard Medical School, Boston, MA, USA. Received: 20 August 2014 Accepted: 12 November 2014 References 1. Snow V, Mottur-Pilson C, Gonzales R: Principles of appropriate antibiotic use for treatment of acute bronchitis in adults. Ann Intern Med 2001, 134(6):518? Gonzales R, Bartlett JG, Besser RE, Cooper RJ, Hickner JM, Hoffman JR, Sande MA: Principles of appropriate antibiotic use for treatment of uncomplicated acute bronchitis: background. AnnInternMed2001, 134(6):521? Irwin RS, Baumann MH, Bolser DC, Boulet LP, Braman SS, Brightling CE, Brown KK, Canning BJ, Chang AB, Dicpinigaitis PV, Eccles R, Glomb WB, Goldstein LB, Graham LM, Hargreave FE, Kvale PA, Lewis SZ, McCool FD, McCrory DC, Prakash UB, Pratter MR, Rosen MJ, Schulman E, Shannon JJ, Smith Hammond C, Tarlo SM: Diagnosis and management of cough executive summary: ACCP evidence-based clinical practice guidelines. Chest 2006, 129(1 Suppl):1S? 23S. 4. National Committee for Quality Assurance. HEDIS 2012 Measures. aspx. Accessed October 7, Smith SM, Fahey T, Smucny J, Becker LA: Antibiotics for acute bronchitis. Cochrane Database Syst Rev 2014, (3):Art. No.: CD doi: / CD pub3. 6. Centers for Disease Control and Prevention. Get Smart: Know When Antibiotics Work. Accessed October 7, Grijalva CG, Nuorti JP, Griffin MR: Antibiotic prescription rates for acute respiratory tract infections in US ambulatory settings. JAMA 2009, 302(7):758? Barnett ML, Linder JA: Antibiotic prescribing for adults with acute bronchitis in the United States, 1996? JAMA 2014, 311(19):2020? Centers for Disease Control and Prevention: Antibiotic Resistance Threats in the United States, ; Accessed August 25, Tonkin-Crine S, Yardley L, Little P: Antibiotic prescribing for acute respiratory tract infections in primary care: a systematic review and meta-ethnography. J Antimicrob Chemother 2011, 66(10):2215? Teixeira Rodrigues A, Roque F, Falcao A, Figueiras A, Herdeiro MT: Understanding physician antibiotic prescribing behaviour: a systematic review of qualitative studies. Int J Antimicrob Agents 2013, 41(3):203? CabanaMD,RandCS,PoweNR,WuAW,WilsonMH,AbboudP-AC, Rubin HR: Why don?t physicians follow clinical practice guidelines? A framework for improvement. JAMA 1999, 282(15):1458? Ranji SR, Steinman MA, Shojania KG, Sundaram V, Lewis R, Arnold S, Gonzales R: Antibiotic Prescribing Behavior. Closing the Quality Gap: a Critical Analysis of Quality Improvement Strategies. Technical Review 9 (Prepared by the Stanford University-UCSF Evidence-based Practice Center under Contract No ), AHRQ Publication No 04(06) Rockville, MD: Agency for Healthcare Research and Quality; Hsieh HF, Shannon SE: Three approaches to qualitative content analysis. Qual Health Res 2005, 15(9):1277? Kondracki NL, Wellman NS, Amundson DR: Content analysis: review of methods and their applications in nutrition education. J Nutr Educ Behav 2002, 34(4):224? Miles MB, Huberman AM: Qualitative Data Analysis: an Expanded Sourcebook. 2nd edition. Thousand Oaks, CA: Sage; Morse JM, Field PA: Qualitative Research Methods for Health Professionals. 2nd edition. Thousand Oaks, CA: Sage; Mangione-Smith R, Elliott MN, Stivers T, McDonald LL, Heritage J: Ruling out the need for antibiotics: are we sending the right message? Arch Pediatr Adolesc Med 2006, 160(9):945? Ong S, Nakase J, Moran GJ, Karras DJ, Kuehnert MJ, Talan DA: Antibiotic use for emergency department patients with upper respiratory infections: prescribing practices, patient expectations, and patient satisfaction. Ann Emerg Med 2007, 50(3):213? Hart AM, Pepper GA, Gonzales R: Balancing acts: deciding for or against antibiotics in acute respiratory infections. J Fam Pract 2006, 55(4):320? Gonzales R, Anderer T, McCulloch CE, Maselli JH, Bloom FJ, Graf TR, Stahl M, Yefko M, Molecavage J, Metlay JP: A cluster randomized trial of decision support strategies for reducing antibiotic use in acute bronchitis. JAMA Intern Med 2013, 173(4):267? Ackerman SL, Gonzales R, Stahl MS, Metlay JP: One size does not fit all: evaluating an intervention to reduce antibiotic prescribing for acute bronchitis. BMC Health Serv Res 2013, 13: Coenen S, Van Royen P, Vermeire E, Hermann I, Denekens J: Antibiotics for coughing in general practice: a qualitative decision analysis. Fam Pract 2000, 17(5):380? Butler CC, Rollnick S, Pill R, Maggs-Rapport F, Stott N: Understanding the culture of prescribing: qualitative study of general practitioners? and patients? perceptions of antibiotics for sore throats. BMJ 1998, 317(7159):637? Brookes-Howell L, Hood K, Cooper L, Little P, Verheij T, Coenen S, Godycki- Cwirko M, Melbye H, Borras-Santos A, Worby P, Jakobsen K, Goossens H, Butler CC: Understanding variation in primary medical care: a ninecountry qualitative study of clinicians? accounts of the non-clinical factors that shape antibiotic prescribing decisions for lower respiratory tract infection. BMJ Open 2012, 2(4):e Coenen S, Michiels B, Van Royen P, Van der Auwera JC, Denekens J: Antibiotics for coughing in general practice: a questionnaire study to quantify and condense the reasons for prescribing. BMC Fam Pract 2002, 3: Brookes-Howell L, Hood K, Cooper L, Coenen S, Little P, Verheij T, Godycki- Cwirko M, Melbye H, Krawczyk J, Borras-Santos A, Jakobsen K, Worby P, Goossens H, Butler CC: Clinical influences on antibiotic prescribing decisions for lower respiratory tract infection: a nine country qualitative study of variation in care. BMJ Open 2012, 2(3):e Mustafa M, Wood F, Butler CC, Elwyn G: Managing expectations of antibiotics for upper respiratory tract infections: a qualitative study. Ann Fam Med 2014, 12(1):29? Heritage J, Elliott MN, Stivers T, Richardson A, Mangione-Smith R: Reducing inappropriate antibiotics prescribing: the role of online commentary on physical examination findings. Patient Educ Couns 2010, 81(1):119? Linder JA, Singer DE: Desire for antibiotics and antibiotic prescribing for adults with upper respiratory tract infections. J Gen Intern Med 2003, 18(10):795? Brookes-Howell L, Hood K, Cooper L, Coenen S, Little P, Verheij T, Godycki- Cwirko M, Melbye H, Krawczyk J, Borras-Santos A, Jakobsen K, Worby P, Goossens H, Butler CC: Are patient views about antibiotics related to clinician perceptions, management and outcome? A multi-country study in outpatients with acute cough. PLoS ONE 2013, 8(10):e Hamm RM, Hicks RJ, Bemben DA: Antibiotics and respiratory infections: are patients more satisfied when expectations are met? J Fam Pract 1996, 43(1):56? Ray DA, Rohren CH: Characteristics of patients with upper respiratory tract infection presenting to a walk-in clinic. Mayo Clin Proc 2001, 76(2):169? Meeker D, Knight TK, Friedberg MW, Linder JA, Goldstein NJ, Fox CR, Rothfeld A, Diaz G, Doctor JN: Nudging guideline-concordant antibiotic prescribing: a randomized clinical trial. JAMA Intern Med 2014, 174(3):425? LinderJA,SchnipperJL,TsurikovaR,YuDT,VolkLA,MelnikasAJ,PalchukMB, Olsha-Yehiav M, Middleton B: Electronic health record feedback to improve antibiotic prescribing for acute respiratory infections. Am J Manag Care 2010, 16(12 Suppl HIT):e311? e Litvin CB, Ornstein SM, Wessell AM, Nemeth LS, Nietert PJ: Use of an electronic health record clinical decision support tool to improve
11 Dempsey et al. BMC Family Practice 2014, 15:194 Page 10 of 10 antibiotic prescribing for acute respiratory infections: the ABX-TRIP study. J Gen Intern Med 2012, 28(6):810? Litvin CB, Ornstein SM, Wessell AM, Nemeth LS, Nietert PJ: Adoption of a clinical decision support system to promote judicious use of antibiotics for acute respiratory infections in primary care. Int J Med Inform 2012, 81(8):521? Persell SD, Friedberg MW, Meeker D, Linder JA, Fox CR, Goldstein NJ, Shah PD, Knight TK, Doctor JN: Use of behavioral economics and social psychology to improve treatment of acute respiratory infections (BEARI): rationale and design of a cluster randomized controlled trial [1RC4AG039115? 01]? study protocol and baseline practice and provider characteristics. BMC Infect Dis 2013, 13: Wood F, Brookes-Howell L, Hood K, Cooper L, Verheij T, Goossens H, Little P, Godycki-Cwirko M, Adriaenssens N, Jakobsen K, Butler CC: A multi-country qualitative study of clinicians? and patients? views on point of care tests for lower respiratory tract infection. Fam Pract 2011, 28(6):661? Tonkin-Crine S, Yardley L, Coenen S, Fernandez-Vandellos P, Krawczyk J, Touboul P, Verheij T, Little P: GPs? views in five European countries of interventions to promote prudent antibiotic use. Br J Gen Pract 2011, 61(586):e252? e Mangione-Smith R, Stivers T, Elliott M, McDonald L, Heritage J: Online commentary during the physical examination: a communication tool for avoiding inappropriate antibiotic prescribing? Soc Sci Med 2003, 56(2):313? Phillips TG, Hickner J: Calling acute bronchitis a chest cold may improve patient satisfaction with appropriate antibiotic use. J Am Board Fam Pract 2005, 18(6):459? Gonzales R, Wilson A, Crane LA, Barrett PH Jr: What?s in a name? Public knowledge, attitudes, and experiences with antibiotic use for acute bronchitis. Am J Med 2000, 108(1):83? Ebell MH, Lundgren J, Youngpairoj S: How long does a cough last? Comparing patients? expectations with data from a systematic review of the literature. Ann Fam Med 2013, 11(1):5? 13. doi: /s Cite this article as: Dempsey et al.: Primary care clinicians? perceptions about antibiotic prescribing for acute bronchitis: a qualitative study. BMC Family Practice :194. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color gure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Who is the Antimicrobial Steward?
 Who is the Antimicrobial Steward? J. Njeri Wainaina, MD FACP Assistant Professor of Medicine Division of Infectious Diseases and Section of Perioperative Medicine Disclosures None 1 Objectives Highlight
Who is the Antimicrobial Steward? J. Njeri Wainaina, MD FACP Assistant Professor of Medicine Division of Infectious Diseases and Section of Perioperative Medicine Disclosures None 1 Objectives Highlight
Visit complexity, diagnostic uncertainty, and antibiotic prescribing for acute cough in primary care: a retrospective study
 Whaley et al. BMC Family Practice 2013, 14:120 RESEARCH ARTICLE Open Access Visit complexity, diagnostic uncertainty, and antibiotic prescribing for acute cough in primary care: a retrospective study Lauren
Whaley et al. BMC Family Practice 2013, 14:120 RESEARCH ARTICLE Open Access Visit complexity, diagnostic uncertainty, and antibiotic prescribing for acute cough in primary care: a retrospective study Lauren
Outpatient Antimicrobial Stewardship. Jeffrey S Gerber, MD, PhD Division of Infectious Diseases The Children s Hospital of Philadelphia
 Outpatient Antimicrobial Stewardship Jeffrey S Gerber, MD, PhD Division of Infectious Diseases The Children s Hospital of Philadelphia Overview The case for outpatient antimicrobial stewardship Interventions
Outpatient Antimicrobial Stewardship Jeffrey S Gerber, MD, PhD Division of Infectious Diseases The Children s Hospital of Philadelphia Overview The case for outpatient antimicrobial stewardship Interventions
Physician Rating: ( 23 Votes ) Rate This Article:
 From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
From Medscape Infectious Diseases Conquering Antibiotic Overuse An Expert Interview With the CDC Laura A. Stokowski, RN, MS Authors and Disclosures Posted: 11/30/2010 Physician Rating: ( 23 Votes ) Rate
Core Elements of Outpatient Antibiotic Stewardship Implementing Antibiotic Stewardship Into Your Outpatient Practice
 National Center for Emerging and Zoonotic Infectious Diseases Core Elements of Outpatient Antibiotic Stewardship Implementing Antibiotic Stewardship Into Your Outpatient Practice Katherine Fleming-Dutra,
National Center for Emerging and Zoonotic Infectious Diseases Core Elements of Outpatient Antibiotic Stewardship Implementing Antibiotic Stewardship Into Your Outpatient Practice Katherine Fleming-Dutra,
Geriatric Mental Health Partnership
 Geriatric Mental Health Partnership September 8, 2017 First, let s test your knowledge about antibiotics http://www.cdc.gov/getsmart/community/about/quiz.html 2 Get Smart Antibiotics Quiz Antibiotics fight
Geriatric Mental Health Partnership September 8, 2017 First, let s test your knowledge about antibiotics http://www.cdc.gov/getsmart/community/about/quiz.html 2 Get Smart Antibiotics Quiz Antibiotics fight
Behavioral Economic Principles to Understand and Change Physician Behavior
 Behavioral Economic Principles to Understand and Change Physician Behavior NIH Collaboratory Grand Rounds January 12, 2018 Jeffrey A. Linder, MD, MPH, FACP Professor of Medicine and Chief Division of General
Behavioral Economic Principles to Understand and Change Physician Behavior NIH Collaboratory Grand Rounds January 12, 2018 Jeffrey A. Linder, MD, MPH, FACP Professor of Medicine and Chief Division of General
Antimicrobial Stewardship in the Outpatient Setting. ELAINE LADD, PHARMD, ABAAHP, FAARFM OCTOBER 28th, 2016
 Antimicrobial Stewardship in the Outpatient Setting ELAINE LADD, PHARMD, ABAAHP, FAARFM OCTOBER 28th, 2016 Abbreviations AMS - Antimicrobial Stewardship Program OP - Outpatient OPS - Outpatient Setting
Antimicrobial Stewardship in the Outpatient Setting ELAINE LADD, PHARMD, ABAAHP, FAARFM OCTOBER 28th, 2016 Abbreviations AMS - Antimicrobial Stewardship Program OP - Outpatient OPS - Outpatient Setting
5/15/17. Core Elements of Outpatient Antibiotic Stewardship: Implementing Antibiotic Stewardship Into Your Outpatient Practice.
 National Center for Emerging and Zoonotic Infectious Diseases Core Elements of Outpatient Antibiotic Stewardship: Implementing Antibiotic Stewardship Into Your Outpatient Practice Melinda Neuhauser, PharmD,
National Center for Emerging and Zoonotic Infectious Diseases Core Elements of Outpatient Antibiotic Stewardship: Implementing Antibiotic Stewardship Into Your Outpatient Practice Melinda Neuhauser, PharmD,
Education Initiative Improves Antibiotic Prescribing in Respiratory Tract Infections in Rural Primary Care. Erin Chiswell, DNP, APRN, FNP-BC
 Education Initiative Improves Antibiotic Prescribing in Respiratory Tract Infections in Rural Primary Care Erin Chiswell, DNP, APRN, FNP-BC Presentation Information Authors: Erin Chiswell, DNP, APRN, FNP-BC
Education Initiative Improves Antibiotic Prescribing in Respiratory Tract Infections in Rural Primary Care Erin Chiswell, DNP, APRN, FNP-BC Presentation Information Authors: Erin Chiswell, DNP, APRN, FNP-BC
Communicating about AR: It s complicated but not impossible! Mary Beth Wenger Health Communications Specialist New York State Department of Health
 Communicating about AR: It s complicated but not impossible! Mary Beth Wenger Health Communications Specialist New York State Department of Health So, why are antibiotics inappropriately prescribed? 2
Communicating about AR: It s complicated but not impossible! Mary Beth Wenger Health Communications Specialist New York State Department of Health So, why are antibiotics inappropriately prescribed? 2
10/9/2017. Evidence-Based Interventions to Reduce Inappropriate Prescription of Antibiotics. Prescribing for Respiratory Tract Infections
 Evidence-Based Interventions to Reduce Inappropriate Prescription of Antibiotics Ann Thomas, MD, MPH Oregon Public Health Division Prescribing for Respiratory Tract Infections Antibiotic use is primary
Evidence-Based Interventions to Reduce Inappropriate Prescription of Antibiotics Ann Thomas, MD, MPH Oregon Public Health Division Prescribing for Respiratory Tract Infections Antibiotic use is primary
Objective 1/20/2016. Expanding Antimicrobial Stewardship into the Outpatient Setting. Disclosure Statement of Financial Interest
 Expanding Antimicrobial Stewardship into the Outpatient Setting Michael E. Klepser, Pharm.D., FCCP Professor Pharmacy Practice Ferris State University College of Pharmacy Disclosure Statement of Financial
Expanding Antimicrobial Stewardship into the Outpatient Setting Michael E. Klepser, Pharm.D., FCCP Professor Pharmacy Practice Ferris State University College of Pharmacy Disclosure Statement of Financial
Improving patient knowledge of antimicrobial resistance and appropriate antibiotic use in a Rutland county acute care center
 University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2019 Improving patient knowledge of antimicrobial resistance and appropriate antibiotic use in a
University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2019 Improving patient knowledge of antimicrobial resistance and appropriate antibiotic use in a
ANTIMICROBIAL STEWARDSHIP FOR AMBULATORY CARE SETTINGS
 ANTIMICROBIAL STEWARDSHIP FOR AMBULATORY CARE SETTINGS Jeffrey S Gerber, MD, PhD Children s Hospital of Philadelphia University of Pennsylvania School of Medicine DISCLOSURE STATEMENT I have no conflicts
ANTIMICROBIAL STEWARDSHIP FOR AMBULATORY CARE SETTINGS Jeffrey S Gerber, MD, PhD Children s Hospital of Philadelphia University of Pennsylvania School of Medicine DISCLOSURE STATEMENT I have no conflicts
Managing winter illnesses without antibiotics
 CLINICAL AUDIT Managing winter illnesses without antibiotics Valid to June 2023 bpac nz better medicin e Background Over the winter months, thousands of people across New Zealand will present to primary
CLINICAL AUDIT Managing winter illnesses without antibiotics Valid to June 2023 bpac nz better medicin e Background Over the winter months, thousands of people across New Zealand will present to primary
United States Outpatient Antibiotic Prescribing and Goal Setting
 National Center for Emerging and Zoonotic Infectious Diseases United States Outpatient Antibiotic Prescribing and Goal Setting Katherine Fleming-Dutra, MD Office of Antibiotic Stewardship Division of Healthcare
National Center for Emerging and Zoonotic Infectious Diseases United States Outpatient Antibiotic Prescribing and Goal Setting Katherine Fleming-Dutra, MD Office of Antibiotic Stewardship Division of Healthcare
Antibiotic Prescribing for Uncomplicated Acute Bronchitis Is Highest in Younger Adults
 Article Antibiotic Prescribing for Uncomplicated Acute Bronchitis Is Highest in Younger Adults Larissa Grigoryan 1, *, Roger Zoorob 1, Jesal Shah 2, Haijun Wang 1, Monisha Arya 3,4 and Barbara W. Trautner
Article Antibiotic Prescribing for Uncomplicated Acute Bronchitis Is Highest in Younger Adults Larissa Grigoryan 1, *, Roger Zoorob 1, Jesal Shah 2, Haijun Wang 1, Monisha Arya 3,4 and Barbara W. Trautner
Necessity of Office Visits for Acute Respiratory Infections in Primary Care
 Necessity of Office Visits for Acute Respiratory Infections in Primary Care The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation
Necessity of Office Visits for Acute Respiratory Infections in Primary Care The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation
BELIEFS AND PRACTICES OF PARENTS ON THE USE OF ANTIBIOTICS FOR THEIR CHILDREN WITH UPPER RESPIRATORY TRACT INFECTION
 PIDSP Journal 2009 Vol 10No.1 Copyright 2009 BELIEFS AND PRACTICES OF PARENTS ON THE USE OF ANTIBIOTICS FOR THEIR CHILDREN WITH UPPER RESPIRATORY TRACT INFECTION Micheline Joyce C. Salonga, MD* ABSTRACT
PIDSP Journal 2009 Vol 10No.1 Copyright 2009 BELIEFS AND PRACTICES OF PARENTS ON THE USE OF ANTIBIOTICS FOR THEIR CHILDREN WITH UPPER RESPIRATORY TRACT INFECTION Micheline Joyce C. Salonga, MD* ABSTRACT
OUTPATIENT ANTIMICROBIAL STEWARDSHIP. Jeffrey S Gerber, MD, PhD Children s Hospital of Philadelphia University of Pennsylvania School of Medicine
 OUTPATIENT ANTIMICROBIAL STEWARDSHIP Jeffrey S Gerber, MD, PhD Children s Hospital of Philadelphia University of Pennsylvania School of Medicine DISCLOSURE STATEMENT I have no conflicts of interest to
OUTPATIENT ANTIMICROBIAL STEWARDSHIP Jeffrey S Gerber, MD, PhD Children s Hospital of Philadelphia University of Pennsylvania School of Medicine DISCLOSURE STATEMENT I have no conflicts of interest to
Antibiotic resistance has become one of the most pressing
 CLINICAL Variation in US Outpatient Antibiotic Prescribing Quality Measures According to Health Plan and Geography Rebecca M. Roberts, MS; Lauri A. Hicks, DO; and Monina Bartoces, PhD Antibiotic resistance
CLINICAL Variation in US Outpatient Antibiotic Prescribing Quality Measures According to Health Plan and Geography Rebecca M. Roberts, MS; Lauri A. Hicks, DO; and Monina Bartoces, PhD Antibiotic resistance
Antibiotics and acute cough: a pan European study
 WONCA Europe 2007, Paris Antibiotics and acute cough: a pan European study Kerry Hood and the GRACE-01 Study Team Department of Primary Care and Public Health Cardiff University Conflict of Interest: None
WONCA Europe 2007, Paris Antibiotics and acute cough: a pan European study Kerry Hood and the GRACE-01 Study Team Department of Primary Care and Public Health Cardiff University Conflict of Interest: None
EVIDENCE BASED MEDICINE: ANTIBIOTIC RESISTANCE IN THE ELDERLY CHETHANA KAMATH GERIATRIC MEDICINE WEEK
 EVIDENCE BASED MEDICINE: ANTIBIOTIC RESISTANCE IN THE ELDERLY CHETHANA KAMATH GERIATRIC MEDICINE WEEK EPIDEMIOLOGY AND BACKGROUND Every year, more than 2 million people in the United States acquire antibiotic-resistant
EVIDENCE BASED MEDICINE: ANTIBIOTIC RESISTANCE IN THE ELDERLY CHETHANA KAMATH GERIATRIC MEDICINE WEEK EPIDEMIOLOGY AND BACKGROUND Every year, more than 2 million people in the United States acquire antibiotic-resistant
4. The use of antibiotics without a prescription in seven EU Member States
 4. The use of antibiotics without a prescription in seven EU Member States Main findings The results are based upon telephone interviews in seven Member States (Cyprus, Estonia, Greece, Hungary, Italy,
4. The use of antibiotics without a prescription in seven EU Member States Main findings The results are based upon telephone interviews in seven Member States (Cyprus, Estonia, Greece, Hungary, Italy,
Antibiotic stewardship a role for Managed Care. Doug Burgoyne, PharmD. CEO, Veridicus Health
 Antibiotic stewardship a role for Managed Care Doug Burgoyne, PharmD CEO, Veridicus Health GRIP: Global Respiratory Infection Partnership Aim: To decrease inappropriate antibiotic use by developing a consistent
Antibiotic stewardship a role for Managed Care Doug Burgoyne, PharmD CEO, Veridicus Health GRIP: Global Respiratory Infection Partnership Aim: To decrease inappropriate antibiotic use by developing a consistent
Improving Human Antibiotic Use in the Community Get Smart: Know When Antibiotics Work
 Improving Human Antibiotic Use in the Community Get Smart: Know When Antibiotics Work Lauri Hicks, DO Director, Office of Antibiotic Stewardship Medical Director, Get Smart: Know When Antibiotics Work
Improving Human Antibiotic Use in the Community Get Smart: Know When Antibiotics Work Lauri Hicks, DO Director, Office of Antibiotic Stewardship Medical Director, Get Smart: Know When Antibiotics Work
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings. Carlos Reyes Sacin, MD, AAHIVS
 Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Improving Antibiotic Use Across the Continuum of Care: Stewardship Opportunities in the Outpatient Setting
 Improving Antibiotic Use Across the Continuum of Care: Stewardship Opportunities in the Outpatient Setting Chloe Bryson-Cahn, MD Chief Fellow, Infectious Disease University of Washington UW Tele-Antimicrobial
Improving Antibiotic Use Across the Continuum of Care: Stewardship Opportunities in the Outpatient Setting Chloe Bryson-Cahn, MD Chief Fellow, Infectious Disease University of Washington UW Tele-Antimicrobial
Antibiotic Stewardship in Human Health- Progress and Opportunities
 National Center for Emerging and Zoonotic Infectious Diseases Antibiotic Stewardship in Human Health- Progress and Opportunities CAPT Lauri A. Hicks, D.O. Director, Office of Antibiotic Stewardship Division
National Center for Emerging and Zoonotic Infectious Diseases Antibiotic Stewardship in Human Health- Progress and Opportunities CAPT Lauri A. Hicks, D.O. Director, Office of Antibiotic Stewardship Division
Antibiotic Stewardship in Nursing Homes SAM GUREVITZ PHARM D, CGP ASSOCIATE PROFESSOR BUTLER UNIVERSITY COLLEGE OF PHARMACY AND HEALTH SCIENCE
 Antibiotic Stewardship in Nursing Homes SAM GUREVITZ PHARM D, CGP ASSOCIATE PROFESSOR BUTLER UNIVERSITY COLLEGE OF PHARMACY AND HEALTH SCIENCE Crisis: Antibiotic Resistance Success Strategy WWW.optimistic-care.org
Antibiotic Stewardship in Nursing Homes SAM GUREVITZ PHARM D, CGP ASSOCIATE PROFESSOR BUTLER UNIVERSITY COLLEGE OF PHARMACY AND HEALTH SCIENCE Crisis: Antibiotic Resistance Success Strategy WWW.optimistic-care.org
Implementing EBM: the case of antibiotics for sore throat
 Implementing EBM: the case of antibiotics for sore throat Mieke van Driel, Marc De Meyere, Jan De Maeseneer Department of General Practice, Ghent University, Belgium mieke.vandriel@ugent.be Supported by
Implementing EBM: the case of antibiotics for sore throat Mieke van Driel, Marc De Meyere, Jan De Maeseneer Department of General Practice, Ghent University, Belgium mieke.vandriel@ugent.be Supported by
Why Are Antibiotics Prescribed for Patients With Acute Bronchitis? A Postintervention Analysis
 Why Are Antibiotics Prescribed for Patients With Acute Bronchitis? A Postintervention Analysis William j. Hueston, MD, julia E. Hopper, Elizabeth N. Dacus, and Arch G. Mainous Ill, PhD Background: Despite
Why Are Antibiotics Prescribed for Patients With Acute Bronchitis? A Postintervention Analysis William j. Hueston, MD, julia E. Hopper, Elizabeth N. Dacus, and Arch G. Mainous Ill, PhD Background: Despite
Antimicrobial Prescribing for Upper Respiratory Infections and Its Effect on Return Visits
 182 March 2009 Family Medicine Clinical Research and Methods Antimicrobial Prescribing for Upper Respiratory Infections and Its Effect on Return Visits John Li, MPH; Anindya De, PhD; Kathy Ketchum, RPh,
182 March 2009 Family Medicine Clinical Research and Methods Antimicrobial Prescribing for Upper Respiratory Infections and Its Effect on Return Visits John Li, MPH; Anindya De, PhD; Kathy Ketchum, RPh,
Patient-Provider Race and Sex Concordance: New Insights into Antibiotic Prescribing for Acute Bronchitis
 67 Patient-Provider Race and Sex Concordance: New Insights into Antibiotic Prescribing for Journal of Health Disparities Research and Practice Volume 10, Issue 4, Winter 2017, pp 67-76 2011 Center for
67 Patient-Provider Race and Sex Concordance: New Insights into Antibiotic Prescribing for Journal of Health Disparities Research and Practice Volume 10, Issue 4, Winter 2017, pp 67-76 2011 Center for
Antibiotics: Take a Time Out
 Antibiotics: Take a Time Out Christine LaRocca, MD Telligen April 27, 2018 This material was prepared by Telligen, the Medicare Quality Innovation Network Quality Improvement Organization, under contract
Antibiotics: Take a Time Out Christine LaRocca, MD Telligen April 27, 2018 This material was prepared by Telligen, the Medicare Quality Innovation Network Quality Improvement Organization, under contract
ANTIBIOTIC RESISTANCE: MULTI-COUNTRY SURVEY
 ANTIBIOTIC RESISTANCE: MULTI-COUNTRY SURVEY November 2015 CONTENTS 1. Executive Summary Page 3 2. Introduction Page 5 3. Methodology Page 6 3.1 Country selection 3.2 Approach 3.3 Limitations 4. Results
ANTIBIOTIC RESISTANCE: MULTI-COUNTRY SURVEY November 2015 CONTENTS 1. Executive Summary Page 3 2. Introduction Page 5 3. Methodology Page 6 3.1 Country selection 3.2 Approach 3.3 Limitations 4. Results
Tandan, Meera; Duane, Sinead; Vellinga, Akke.
 Provided by the author(s) and NUI Galway in accordance with publisher policies. Please cite the published version when available. Title Do general practitioners prescribe more antimicrobials when the weekend
Provided by the author(s) and NUI Galway in accordance with publisher policies. Please cite the published version when available. Title Do general practitioners prescribe more antimicrobials when the weekend
Core Elements of Antibiotic Stewardship for Nursing Homes
 Core Elements of Antibiotic Stewardship for Nursing Homes Nimalie D. Stone, MD, MS Medical Epidemiologist for LTC Division of Healthcare Quality Promotion Centers for Disease Control and Prevention Antimicrobial
Core Elements of Antibiotic Stewardship for Nursing Homes Nimalie D. Stone, MD, MS Medical Epidemiologist for LTC Division of Healthcare Quality Promotion Centers for Disease Control and Prevention Antimicrobial
Knowledge, attitudes and perceptions of antimicrobial resistance amongst private practice patients and primary care prescribers in South Africa
 Knowledge, attitudes and perceptions of antimicrobial resistance amongst private practice patients and primary care prescribers in South Africa Dena van den Bergh, Elise Farley, Annemie Stewart, Mary-Ann
Knowledge, attitudes and perceptions of antimicrobial resistance amongst private practice patients and primary care prescribers in South Africa Dena van den Bergh, Elise Farley, Annemie Stewart, Mary-Ann
Antibiotic resistance presents a major strategic risk to health services;
 Influence of Clinical Communication on Parents Antibiotic Expectations for Children With Respiratory Tract Infections Christie Cabral, PhD 1 Jenny Ingram, PhD 2 Patricia J. Lucas, PhD 3 Niamh M. Redmond,
Influence of Clinical Communication on Parents Antibiotic Expectations for Children With Respiratory Tract Infections Christie Cabral, PhD 1 Jenny Ingram, PhD 2 Patricia J. Lucas, PhD 3 Niamh M. Redmond,
Delayed Prescribing for Minor Infections Resource Pack for Prescribers
 Delayed Prescribing for Minor Infections Resource Pack for Prescribers Background: Antibiotic resistance is an alarming threat to modern healthcare, and infectious illness remains a major global threat
Delayed Prescribing for Minor Infections Resource Pack for Prescribers Background: Antibiotic resistance is an alarming threat to modern healthcare, and infectious illness remains a major global threat
Antimicrobial Stewardship
 Antimicrobial Stewardship Preventing the Spread of Antibiotic Resistance and Improving Patient Care (Adapted from the Centers for Disease Control and Prevention) What is Stewardship? Antimicrobial stewardship
Antimicrobial Stewardship Preventing the Spread of Antibiotic Resistance and Improving Patient Care (Adapted from the Centers for Disease Control and Prevention) What is Stewardship? Antimicrobial stewardship
Updates in Antimicrobial Stewardship
 Updates in Antimicrobial Stewardship Andrew Hunter, Pharm.D., BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center andrew.hunter@va.gov Disclosures No disclosures
Updates in Antimicrobial Stewardship Andrew Hunter, Pharm.D., BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center andrew.hunter@va.gov Disclosures No disclosures
Using a Delayed Antibiotic-Prescribing Education Intervention to Prevent Antibiotic Overuse in the Treatment of Respiratory Tract Infections
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Doctor of Nursing Practice (DNP) Projects College of Nursing 2016 Using a Delayed Antibiotic-Prescribing Education Intervention to Prevent
University of Massachusetts Amherst ScholarWorks@UMass Amherst Doctor of Nursing Practice (DNP) Projects College of Nursing 2016 Using a Delayed Antibiotic-Prescribing Education Intervention to Prevent
Building Rapid Interventions to reduce antimicrobial resistance and overprescribing of antibiotics (BRIT)
 Greater Manchester Connected Health City (GM CHC) Building Rapid Interventions to reduce antimicrobial resistance and overprescribing of antibiotics (BRIT) BRIT Dashboard Manual Users: General Practitioners
Greater Manchester Connected Health City (GM CHC) Building Rapid Interventions to reduce antimicrobial resistance and overprescribing of antibiotics (BRIT) BRIT Dashboard Manual Users: General Practitioners
The Big Picture: Using Antibiotic Use and Surveillance Data to Better Inform Stewardship in Healthcare Settings
 The Big Picture: Using Antibiotic Use and Surveillance Data to Better Inform Stewardship in Healthcare Settings Becky Roberts, MS Get Smart: Know When Antibiotics Work Office of Antibiotic Stewardship
The Big Picture: Using Antibiotic Use and Surveillance Data to Better Inform Stewardship in Healthcare Settings Becky Roberts, MS Get Smart: Know When Antibiotics Work Office of Antibiotic Stewardship
Nursing Home Online Training Sessions Session 2: Exploring Antibiotics and Their Role in Fighting Bacterial Infections
 National Nursing Home Quality Care Collaborative Nursing Home Online Training Sessions Session 2: Exploring Antibiotics and Their Role in Fighting Bacterial Infections Health Services Advisory Group (HSAG)
National Nursing Home Quality Care Collaborative Nursing Home Online Training Sessions Session 2: Exploring Antibiotics and Their Role in Fighting Bacterial Infections Health Services Advisory Group (HSAG)
Optimizing Clinical Diagnosis and Antibiotic Prescribing for Common Respiratory Tract Infections, Fanara Family Health Center- Rural Egypt
 Sameh F. Ahmed, et al Optimizing Clinical Diagnosis and Antibiotic Prescribing 105 Optimizing Clinical Diagnosis and Antibiotic Prescribing for Common Respiratory Tract Infections, Fanara Family Health
Sameh F. Ahmed, et al Optimizing Clinical Diagnosis and Antibiotic Prescribing 105 Optimizing Clinical Diagnosis and Antibiotic Prescribing for Common Respiratory Tract Infections, Fanara Family Health
3/1/2016. Antibiotics --When Less is More. Most Urgent Threats. Serious Threats
 Antibiotics --When Less is More Ralph Gonzales, MD, MSPH Associate Dean, Clinical Innovation School of Medicine VP, Clinical Innovation, UCSF Health Most Urgent Threats Serious Threats Multidrug-Resistant
Antibiotics --When Less is More Ralph Gonzales, MD, MSPH Associate Dean, Clinical Innovation School of Medicine VP, Clinical Innovation, UCSF Health Most Urgent Threats Serious Threats Multidrug-Resistant
MAGNITUDE OF ANTIMICROBIAL USE. Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges
 Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control
Antimicrobial Stewardship in Acute and Long Term Healthcare Facilities: Design, Implementation and Challenges John A. Jernigan, MD, MS Division of Healthcare Quality Promotion Centers for Disease Control
ANTIMICROBIAL RESISTANCE and causes of non-prudent use of antibiotics in human medicine in the EU
 ANTIMICROBIAL RESISTANCE and causes of non-prudent use of antibiotics in human medicine in the EU Health and Food Safety John Paget (NIVEL) Dominique Lescure (NIVEL) Ann Versporten (University of Antwerp)
ANTIMICROBIAL RESISTANCE and causes of non-prudent use of antibiotics in human medicine in the EU Health and Food Safety John Paget (NIVEL) Dominique Lescure (NIVEL) Ann Versporten (University of Antwerp)
BMJ Open. For peer review only -
 Why do general practitioners prescribe antibiotics for upper respiratory tract infections to meet patient expectations : A mixed methods study Journal: BMJ Open Manuscript ID bmjopen-0-0 Article Type:
Why do general practitioners prescribe antibiotics for upper respiratory tract infections to meet patient expectations : A mixed methods study Journal: BMJ Open Manuscript ID bmjopen-0-0 Article Type:
Development and improvement of diagnostics to improve use of antibiotics and alternatives to antibiotics
 Priority Topic B Diagnostics Development and improvement of diagnostics to improve use of antibiotics and alternatives to antibiotics The overarching goal of this priority topic is to stimulate the design,
Priority Topic B Diagnostics Development and improvement of diagnostics to improve use of antibiotics and alternatives to antibiotics The overarching goal of this priority topic is to stimulate the design,
Nudging Guideline-Concordant Antibiotic Prescribing A Randomized Clinical Trial
 Research Original Investigation Nudging Guideline-Concordant Antibiotic Prescribing A Randomized Clinical Trial Daniella Meeker, PhD; Tara K. Knight, PhD; Mark W. Friedberg, MD, MPP; Jeffrey A. Linder,
Research Original Investigation Nudging Guideline-Concordant Antibiotic Prescribing A Randomized Clinical Trial Daniella Meeker, PhD; Tara K. Knight, PhD; Mark W. Friedberg, MD, MPP; Jeffrey A. Linder,
11/22/2016. Antimicrobial Stewardship Update Disclosures. Outline. No conflicts of interest to disclose
 Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
Antimicrobial Stewardship Update 2016 APIC-CI Conference November 17 th, 2016 Jay R. McDonald, MD Chief, ID Section VA St. Louis Health Care System Assistant Professor of medicine Washington University
STANDARD FOR ANTIMICROBIAL STEWARDSHIP IN HAP, CAH, AND NCC OR ANTIBIOTIC STEWARDSHIP AND YOU
 STANDARD FOR ANTIMICROBIAL STEWARDSHIP IN HAP, CAH, AND NCC OR ANTIBIOTIC STEWARDSHIP AND YOU CLINT ROHNER, PHARMD EIRMC CLINICAL COORDINATOR, FORMER AMP LEAD OCTOBER 28, 2016 TYPES OF FACILITY AFFECTED:
STANDARD FOR ANTIMICROBIAL STEWARDSHIP IN HAP, CAH, AND NCC OR ANTIBIOTIC STEWARDSHIP AND YOU CLINT ROHNER, PHARMD EIRMC CLINICAL COORDINATOR, FORMER AMP LEAD OCTOBER 28, 2016 TYPES OF FACILITY AFFECTED:
The development of antibioticresistant
 Appropriate Antimicrobial Prescribing: Approaches that Limit Antibiotic Resistance RICHARD COLGAN, M.D., University of Maryland School of Medicine, Baltimore, Maryland JOHN H. POWERS, M.D., National Institutes
Appropriate Antimicrobial Prescribing: Approaches that Limit Antibiotic Resistance RICHARD COLGAN, M.D., University of Maryland School of Medicine, Baltimore, Maryland JOHN H. POWERS, M.D., National Institutes
Non-Clinical Benefits of Evidence-Based Veterinary Medicine
 Non-Clinical Benefits of Evidence-Based Veterinary Medicine A Knowledge Summary by Sarah Hauser BSc (Hons) MPA MPP 1* Elizabeth L. Jackson BAg (Hons) MBA PhD SFHEA 1 1 Royal Veterinary College, 4 Royal
Non-Clinical Benefits of Evidence-Based Veterinary Medicine A Knowledge Summary by Sarah Hauser BSc (Hons) MPA MPP 1* Elizabeth L. Jackson BAg (Hons) MBA PhD SFHEA 1 1 Royal Veterinary College, 4 Royal
How long do the Hong Kong Chinese expect their URTI to last? Effects on antibiotic use
 Lam et al. BMC Pulmonary Medicine (2015) 15:23 DOI 10.1186/s12890-015-0018-y RESEARCH ARTICLE Open Access How long do the Hong Kong Chinese expect their URTI to last? Effects on antibiotic use Tai Pong
Lam et al. BMC Pulmonary Medicine (2015) 15:23 DOI 10.1186/s12890-015-0018-y RESEARCH ARTICLE Open Access How long do the Hong Kong Chinese expect their URTI to last? Effects on antibiotic use Tai Pong
Surveys of the Street and Private Dog Population: Kalhaar Bungalows, Gujarat India
 The Humane Society Institute for Science and Policy Animal Studies Repository 11-2017 Surveys of the Street and Private Dog Population: Kalhaar Bungalows, Gujarat India Tamara Kartal Humane Society International
The Humane Society Institute for Science and Policy Animal Studies Repository 11-2017 Surveys of the Street and Private Dog Population: Kalhaar Bungalows, Gujarat India Tamara Kartal Humane Society International
What is an Antibiotic Stewardship Program?
 What is an Antibiotic Stewardship Program? Jane Rogers, R.N. Anne Messer, MPH Learning Session #4 August 15, 2017 National Nursing Home Quality Care Collaborative Change Package Change Bundle: To prevent
What is an Antibiotic Stewardship Program? Jane Rogers, R.N. Anne Messer, MPH Learning Session #4 August 15, 2017 National Nursing Home Quality Care Collaborative Change Package Change Bundle: To prevent
CMS Antibiotic Stewardship Initiative
 CMS Antibiotic Stewardship Initiative Mary Fermazin, MD, MPA Chief Medical Officer Vice President, Health Policy and Quality Measurement Health Services Advisory Group (HSAG) March 11, 2017 Disclosure
CMS Antibiotic Stewardship Initiative Mary Fermazin, MD, MPA Chief Medical Officer Vice President, Health Policy and Quality Measurement Health Services Advisory Group (HSAG) March 11, 2017 Disclosure
Antimicrobial Stewardship in the Hospital Setting
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 12 Antimicrobial Stewardship in the Hospital Setting Authors Dan Markley, DO, MPH, Amy L. Pakyz, PharmD, PhD, Michael Stevens, MD, MPH Chapter Editor
Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities
 Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities Introduction As the problem of antibiotic resistance continues to worsen in all healthcare setting, we
Commonwealth of Kentucky Antibiotic Stewardship Practice Assessment For Long-Term Care Facilities Introduction As the problem of antibiotic resistance continues to worsen in all healthcare setting, we
King Fahd University of Petroleum & Minerals College of Industrial Management
 King Fahd University of Petroleum & Minerals College of Industrial Management CIM COOP PROGRAM POLICIES AND DELIVERABLES The CIM Cooperative Program (COOP) period is an essential and critical part of your
King Fahd University of Petroleum & Minerals College of Industrial Management CIM COOP PROGRAM POLICIES AND DELIVERABLES The CIM Cooperative Program (COOP) period is an essential and critical part of your
Bacteria become resistant to antibiotics- not humans or animals.
 July 2017 Dear Colleague, World Antibiotic Awareness Week - National Community Pharmacy Public Health Campaign 2017 Please find enclosed information and resources for the next contractual national community
July 2017 Dear Colleague, World Antibiotic Awareness Week - National Community Pharmacy Public Health Campaign 2017 Please find enclosed information and resources for the next contractual national community
EDUCATION OF HEALTHCARE PROFESSIONALS ON PRUDENT USE OF ANTIBIOTICS: ROOM FOR IMPROVEMENT
 1 EDUCATION OF HEALTHCARE PROFESSIONALS ON PRUDENT USE OF ANTIBIOTICS: ROOM FOR IMPROVEMENT PROF. CÉLINE PULCINI SERVICE DE MALADIES INFECTIEUSES CHU DE NANCY Déclaration de liens d intérêt (3 dernières
1 EDUCATION OF HEALTHCARE PROFESSIONALS ON PRUDENT USE OF ANTIBIOTICS: ROOM FOR IMPROVEMENT PROF. CÉLINE PULCINI SERVICE DE MALADIES INFECTIEUSES CHU DE NANCY Déclaration de liens d intérêt (3 dernières
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources
 Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
Optimizing Antimicrobial Stewardship Activities Based on Institutional Resources Andrew Hunter, PharmD, BCPS Infectious Diseases Clinical Pharmacy Specialist Michael E. DeBakey VA Medical Center Andrew.hunter@va.gov
The Effect of a Patient and Provider Education Program on Antibiotic Overuse in Respiratory Tract Infections in a Rural Primary Care Population
 University of Kentucky UKnowledge DNP Projects College of Nursing 2017 The Effect of a Patient and Provider Education Program on Antibiotic Overuse in Respiratory Tract Infections in a Rural Primary Care
University of Kentucky UKnowledge DNP Projects College of Nursing 2017 The Effect of a Patient and Provider Education Program on Antibiotic Overuse in Respiratory Tract Infections in a Rural Primary Care
Most acute respiratory tract infections. Acute respiratory tract infection: A practice examines its antibiotic prescribing habits
 Michael L. Grover, DO; Martina Mookadam, MD; Richard H. Rutkowski, MD; Allison M. Cullan, MD; Destin E. Hill, MD; David C. Patchett, DO; Esan O. Simon, MD; MariLynn Mulheron, NP; Brie N. Noble, BS Department
Michael L. Grover, DO; Martina Mookadam, MD; Richard H. Rutkowski, MD; Allison M. Cullan, MD; Destin E. Hill, MD; David C. Patchett, DO; Esan O. Simon, MD; MariLynn Mulheron, NP; Brie N. Noble, BS Department
Challenges and opportunities for rapidly advancing reporting and improving inpatient antibiotic use in the U.S.
 Challenges and opportunities for rapidly advancing reporting and improving inpatient antibiotic use in the U.S. Overview of benchmarking Antibiotic Use Scott Fridkin, MD, Senior Advisor for Antimicrobial
Challenges and opportunities for rapidly advancing reporting and improving inpatient antibiotic use in the U.S. Overview of benchmarking Antibiotic Use Scott Fridkin, MD, Senior Advisor for Antimicrobial
WORLD ANTIBIOTIC AWARENESS WEEK
 # AntibioticResistance WORLD ANTIBIOTIC AWARENESS WEEK 14-20 NOVEMBER 2016 2016 CAMPAIGN TOOLKIT TABLE OF CONTENTS Why we need a global campagin... Campagin objectives... Key messages... Calls to action
# AntibioticResistance WORLD ANTIBIOTIC AWARENESS WEEK 14-20 NOVEMBER 2016 2016 CAMPAIGN TOOLKIT TABLE OF CONTENTS Why we need a global campagin... Campagin objectives... Key messages... Calls to action
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies
 ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
ASCENSION TEXAS Antimicrobial Stewardship: Practical Implementation Strategies Theresa Jaso, PharmD, BCPS (AQ-ID) Network Clinical Pharmacy Specialist Infectious Diseases Seton Healthcare Family Ascension
Comments from The Pew Charitable Trusts re: Consultation on a draft global action plan to address antimicrobial resistance September 1, 2014
 Comments from The Pew Charitable Trusts re: Consultation on a draft global action plan to address antimicrobial resistance September 1, 2014 The Pew Charitable Trusts is an independent, nonprofit organization
Comments from The Pew Charitable Trusts re: Consultation on a draft global action plan to address antimicrobial resistance September 1, 2014 The Pew Charitable Trusts is an independent, nonprofit organization
Antimicrobial Stewardship Strategy: Intravenous to oral conversion
 Antimicrobial Stewardship Strategy: Intravenous to oral conversion Promoting the use of oral antimicrobial agents instead of intravenous administration when clinically indicated. Description This is an
Antimicrobial Stewardship Strategy: Intravenous to oral conversion Promoting the use of oral antimicrobial agents instead of intravenous administration when clinically indicated. Description This is an
ANTIBIOTIC STEWARDSHIP
 ANTIBIOTIC STEWARDSHIP S.A. Dehghan Manshadi M.D. Assistant Professor of Infectious Diseases and Tropical Medicine Tehran University of Medical Sciences Issues associated with use of antibiotics were recognized
ANTIBIOTIC STEWARDSHIP S.A. Dehghan Manshadi M.D. Assistant Professor of Infectious Diseases and Tropical Medicine Tehran University of Medical Sciences Issues associated with use of antibiotics were recognized
Physicians Knowledge of prescribing antibiotics for acute Upper Respiratory Tract Infection.
 Physicians Knowledge of prescribing antibiotics for acute Upper Respiratory Tract Infection Awwad Alenezy 1, Fayez Alenezy 2, Al dhafeeri Obaid Manzel 3 and Basem M.M. Salama 1 1 Family and Community Medicine
Physicians Knowledge of prescribing antibiotics for acute Upper Respiratory Tract Infection Awwad Alenezy 1, Fayez Alenezy 2, Al dhafeeri Obaid Manzel 3 and Basem M.M. Salama 1 1 Family and Community Medicine
Volume 2; Number 16 October 2008
 Volume 2; Number 16 October 2008 What s new this month NHS Lincolnshire have launched a public information campaign designed to raise public awareness of the risks associated with the inappropriate use
Volume 2; Number 16 October 2008 What s new this month NHS Lincolnshire have launched a public information campaign designed to raise public awareness of the risks associated with the inappropriate use
Jump Start Stewardship
 Jump Start Stewardship Webinar 2: Building your Stewardship Team and Selecting Interventions and Targets for your Implementation Welcome Thank you for your time today This webinar will be recorded for
Jump Start Stewardship Webinar 2: Building your Stewardship Team and Selecting Interventions and Targets for your Implementation Welcome Thank you for your time today This webinar will be recorded for
Update on CDC Antibiotic Stewardship Activities
 National Center for Emerging and Zoonotic Infectious Diseases Update on CDC Antibiotic Stewardship Activities CAPT Lauri Hicks, DO CAPT Arjun Srinivasan, MD Division of Healthcare Quality Promotion National
National Center for Emerging and Zoonotic Infectious Diseases Update on CDC Antibiotic Stewardship Activities CAPT Lauri Hicks, DO CAPT Arjun Srinivasan, MD Division of Healthcare Quality Promotion National
An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings?
 An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings? Dr. Andrew Morris Antimicrobial Stewardship ProgramMt. Sinai Hospital University Health Network amorris@mtsinai.on.ca andrew.morris@uhn.ca
An Approach to Appropriate Antibiotic Prescribing in Outpatient and LTC Settings? Dr. Andrew Morris Antimicrobial Stewardship ProgramMt. Sinai Hospital University Health Network amorris@mtsinai.on.ca andrew.morris@uhn.ca
Antimicrobial Resistance Module (ARM) for Population-Based Surveys 1
 Antimicrobial Resistance Module (ARM) for Population-Based Surveys 1 The Antimicrobial Resistance (AMR) Module for the Demographic and Health Survey (DHS) and other population-based surveys generates household-level
Antimicrobial Resistance Module (ARM) for Population-Based Surveys 1 The Antimicrobial Resistance (AMR) Module for the Demographic and Health Survey (DHS) and other population-based surveys generates household-level
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus
 Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Monthly Webinar. Tuesday 16th January 2018, 16:00. That Was The Year That Was : Selections from the 2017 Antimicrobial Stewardship Literature
 Monthly Webinar Tuesday 16th January 2018, 16:00 That Was The Year That Was : Selections from the 2017 Antimicrobial Stewardship Literature Audio dial-in (phone): 01 526 0058 Instructions Interactive Please
Monthly Webinar Tuesday 16th January 2018, 16:00 That Was The Year That Was : Selections from the 2017 Antimicrobial Stewardship Literature Audio dial-in (phone): 01 526 0058 Instructions Interactive Please
Journal of Antimicrobial Chemotherapy Advance Access published July 10, 2007
 Journal of Antimicrobial Chemotherapy Advance Access published July 10, 2007 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkm254 Reducing antibiotic prescriptions for acute cough by motivating
Journal of Antimicrobial Chemotherapy Advance Access published July 10, 2007 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkm254 Reducing antibiotic prescriptions for acute cough by motivating
Telligen Outpatient Antibiotic Stewardship Initiative. The Renal Network March 1, 2017
 Telligen Outpatient Antibiotic Stewardship Initiative The Renal Network March 1, 2017 Who is Telligen? What is the QIN-QIO Program? Telligen: The Medicare Quality Innovation Network (QIN)-Quality Improvement
Telligen Outpatient Antibiotic Stewardship Initiative The Renal Network March 1, 2017 Who is Telligen? What is the QIN-QIO Program? Telligen: The Medicare Quality Innovation Network (QIN)-Quality Improvement
Mutt Mitt Survey Summary Results of surveys of Mutt Mitt station sponsors and users
 Mutt Mitt Survey Summary Results of surveys of Mutt Mitt station sponsors and users January, 2015 Kitsap Public Works Stormwater Division Prepared by: Cammy Mills, cmills@co.kitsap.wa.us Executive Summary
Mutt Mitt Survey Summary Results of surveys of Mutt Mitt station sponsors and users January, 2015 Kitsap Public Works Stormwater Division Prepared by: Cammy Mills, cmills@co.kitsap.wa.us Executive Summary
Members are asked to: Support the uptake and development of the AWMSG National Audit: Focus on Antibiotic Prescribing.
 Enclosure No: Agenda Item No: Author: Contact: 7/AWMSG/0215 11 Review of the AWMSG National Audit: Focus on Antibiotic Prescribing 2013 2015 All Wales Prescribing Advisory Group (AWPAG) Lead: TL Lewis
Enclosure No: Agenda Item No: Author: Contact: 7/AWMSG/0215 11 Review of the AWMSG National Audit: Focus on Antibiotic Prescribing 2013 2015 All Wales Prescribing Advisory Group (AWPAG) Lead: TL Lewis
The Use of Procalcitonin to Improve Antibiotic Stewardship
 The Use of Procalcitonin to Improve Antibiotic Stewardship Disclosures I have no actual or potential conflict of interest in relation to this presentation. Patrick A. Laird, DNP, RN, ACNP-BC Objectives
The Use of Procalcitonin to Improve Antibiotic Stewardship Disclosures I have no actual or potential conflict of interest in relation to this presentation. Patrick A. Laird, DNP, RN, ACNP-BC Objectives
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Antibiotic Stewardship and Critical Access Hospitals. Robert White, BA, PT, CPHQ Program Manager TMF Quality Innovation Network
 Antibiotic Stewardship and Critical Access Hospitals Robert White, BA, PT, CPHQ Program Manager TMF Quality Innovation Network Antibiotic-Resistant Bacteria A serious threat to public health and the economy
Antibiotic Stewardship and Critical Access Hospitals Robert White, BA, PT, CPHQ Program Manager TMF Quality Innovation Network Antibiotic-Resistant Bacteria A serious threat to public health and the economy
Antimicrobial Resistance and Dentistry. LDC Officials Day 4 December 2015 Susie Sanderson
 Antimicrobial Resistance and Dentistry LDC Officials Day 4 December 2015 Susie Sanderson Who am I? Why are we interested in AMR? Where is the leadership? Who is taking action? What is the BDA doing? Is
Antimicrobial Resistance and Dentistry LDC Officials Day 4 December 2015 Susie Sanderson Who am I? Why are we interested in AMR? Where is the leadership? Who is taking action? What is the BDA doing? Is
Antimicrobial Stewardship Strategy:
 Antimicrobial Stewardship Strategy: Prospective audit with intervention and feedback Formal assessment of antimicrobial therapy by trained individuals, who make recommendations to the prescribing service
Antimicrobial Stewardship Strategy: Prospective audit with intervention and feedback Formal assessment of antimicrobial therapy by trained individuals, who make recommendations to the prescribing service
SEASONAL TRENDS IN ANTIBIOTIC USAGE AMONG PAEDIATRIC OUTPATIENTS
 SEASONAL TRENDS IN ANTIBIOTIC USAGE AMONG PAEDIATRIC OUTPATIENTS Edita Alili-Idrizi, Msc Merita Dauti, Msc State University of Tetovo, Faculty of Medicine, Department of Pharmacy, Tetovo, R. of Macedonia
SEASONAL TRENDS IN ANTIBIOTIC USAGE AMONG PAEDIATRIC OUTPATIENTS Edita Alili-Idrizi, Msc Merita Dauti, Msc State University of Tetovo, Faculty of Medicine, Department of Pharmacy, Tetovo, R. of Macedonia
Special Eurobarometer 478. Summary. Antimicrobial Resistance
 Antimicrobial Resistance Survey requested by the European Commission, Directorate-General for Health and Food Safety and co-ordinated by the Directorate-General for Communication This document does not
Antimicrobial Resistance Survey requested by the European Commission, Directorate-General for Health and Food Safety and co-ordinated by the Directorate-General for Communication This document does not
TEACHERS TOPICS A Lecture About Pharmaceuticals Used in Animal Patients
 TEACHERS TOPICS A Lecture About Pharmaceuticals Used in Animal Patients Elaine Blythe Lust, PharmD School of Pharmacy and Health Professions, Creighton University Submitted October 30, 2008; accepted January
TEACHERS TOPICS A Lecture About Pharmaceuticals Used in Animal Patients Elaine Blythe Lust, PharmD School of Pharmacy and Health Professions, Creighton University Submitted October 30, 2008; accepted January
ANTIMICROBIAL STEWARDSHIP IN PRIMARY HEALTH CARE WESTERN CAPE GOVERNMENT: HEALTH METRO DISTRICT FINDINGS 6 MONTHS AFTER INITIATION
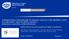 ANTIMICROBIAL STEWARDSHIP IN PRIMARY HEALTH CARE WESTERN CAPE GOVERNMENT: HEALTH METRO DISTRICT FINDINGS 6 MONTHS AFTER INITIATION 2018 IHI Africa Forum for Quality and Safety in Healthcare Bart Willems,
ANTIMICROBIAL STEWARDSHIP IN PRIMARY HEALTH CARE WESTERN CAPE GOVERNMENT: HEALTH METRO DISTRICT FINDINGS 6 MONTHS AFTER INITIATION 2018 IHI Africa Forum for Quality and Safety in Healthcare Bart Willems,
Antimicrobial Stewardship Strategy: Antibiograms
 Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Antimicrobial Stewardship Strategy: Antibiograms A summary of the cumulative susceptibility of bacterial isolates to formulary antibiotics in a given institution or region. Its main functions are to guide
Knowledge, attitude, and behaviour toward antibiotics among Hong Kong people: local-born versus immigrants
 RESEARCH FUND FOR THE CONTROL OF INFECTIOUS DISEASES Knowledge, attitude, and behaviour toward antibiotics among Hong Kong people: local-born versus immigrants TP Lam *, KF Lam, PL Ho, RWH Yung K e y M
RESEARCH FUND FOR THE CONTROL OF INFECTIOUS DISEASES Knowledge, attitude, and behaviour toward antibiotics among Hong Kong people: local-born versus immigrants TP Lam *, KF Lam, PL Ho, RWH Yung K e y M
