Safety and Efficacy of Dexmedetomidine, Ketofol, and Propofol for Sedation of Mechanically Ventilated Patients
|
|
|
- Allison Pierce
- 5 years ago
- Views:
Transcription
1 Research Article imedpub Journals Journal of Intensive and Critical Care ISSN DOI: / Abstract Safety and Efficacy of Dexmedetomidine, Ketofol, and Propofol for Sedation of Mechanically Ventilated Patients Introduction: The Society of Critical Care Medicine recommended using non -benzodiazepine agents as propofol and dexmedetomidine for sedation of the critically ill patients in intensive care units. Aims and Objectives: This study aimed to evaluate the safety and efficacy of ketofol, dexmedetomidine or propofol for sedation of postoperative mechanically ventilated patients in intensive care unit. Materials and Methods: The study included ninety postoperative mechanically ventilated patients in the intensive care unit divided randomly into three equal groups. Group A: 30 patients received ketofol an initial bolus dose (500 mcg/kg) of ketamine/propofol 1:1 (ketamine 8 mg/ml and propofol 8 mg/ml followed by a maintenance dose of (10 mcg/kg/min). Group B: 30 patients received loading dose infusion of dexmedetomidin diluted in 0.9% sodium chloride 1 mcg/kg/h over 10 min followed by a maintenance infusion of mcg/kg/h. Group C: 30 patients received propofol undiluted as an infusion of 1-3 mg/kg/h, after a loading dose infusion up to 1 mg/kg over 10 min. Sedation level, bispectral index, systolic and diastolic blood pressure, heart rate, recovery time, complications (hypertension, hypotension, bradycardia). Result: RAMSY sedation score was statistically significantly higher in group A than group B at the sixth and twelfth h; it was statistically significantly higher in group A than group C from the first to the twenty-fourth h and was statistically significantly higher in group B than group C at first, the sixth and eighteenth h. The recovery time was longer in group A compared to group B and C, and it was statistically significant, no complications recorded in the three groups. Conclusion: Using ketofol, dexmedetomidine or propofol was effective in maintaining sedation without hemodynamic complications in postoperative mechanically ventilated patients in the intensive care unit. Keywords: Sedation; Ketofol; Dexmedetomidine; Propofol Samaa Rashwan*, Hatem El moutaz Mahmoud and Zeinab Taha Department of Anesthesiology, Surgical ICU and Pain Management, Faculty of Medicine, Beni Suef University, Egypt *Corresponding author: Samaa Rashwan samaarashwan1971@gmail.com Department of Anesthesiology, Surgical ICU and Pain Management, Faculty of Medicine, Beni Suef University, Egypt Tel: Citation: Rashwan S, El moutaz Mahmoud H, Taha Z, et al. Safety and Efficacy of Dexmedetomidine, Ketofol, and Propofol for Sedation of Mechanically Ventilated Patients. J Intensive & Crit Care Vol.4 No.4:16 Received: October 31, ; Accepted: December 13, ; Published: December 20, Introduction The critically ill patients in an intensive care unit are exposed to different noxious stimuli including postoperative pain, multiple venipuncture, invasive monitoring, and endotracheal intubation; therefore they are usually managed using a continuous-infusion of sedative [1]. It has been recommended by the Society of Critical Care Medicine (SCCM) to use non-benzodiazepine agents as propofol and dexmedetomidine for sedation regimen [2]. This change from benzodiazepines to non-benzodiazepines is Under License of Creative Commons Attribution 3.0 License 1
2 based on recent evidence reported that using benzodiazepine was an independent risk factor for the development of delirium, increased hospital Length of Stay (LOS) and increased 6-month mortality [3-7]. Alpha 2 agonist dexmedetomidine has sedative and analgesic effects and has been proved for ICU sedation for up to 24 h. It provides hemodynamic stability without depressing respiration. It produces mild cognitive impairment allowing easy communication between the healthcare provider and the patient in the ICU. It also has the advantages of reducing the costs of ICU stay and more natural liberation from mechanical ventilation [8-10]. It has been reported that intravenous ketamine/propofol combination (ketofol) can be used for sedation for 24 h [11]. This is based on the finding that propofol is recommended for the short-term (<24 h) treatment of anxiety in the critically ill adult patients and continuous infusion doses of ketamine have also been described for 24 h, so ketofol was expected to be given safely as a continuous infusion for 24 h [12], with the advantages of increasing their safety and efficacy and decreases their side effects [13]. In a study by Hamimy et al. continuous intravenous infusion of ketofol provided adequate and safe short-term sedation (less than 24 h) for critically ill patients in the intensive care units, rapid recovery without significant complications but because of the small size of their case series further studies with more significant number of patients were recommended to confirm their finding [14]. This study aimed to evaluate the safety and efficacy of using ketofol compared to dexmedetomidine or propofol for sedation of postoperative patients who required mechanical ventilation in the intensive care unit. Materials and Methods This study was conducted in the Surgical Intensive Care Unit (SICU) of Beni-Suef University hospital; the study was registered at PACRT (trial registration number ) after obtaining approval from the anesthesia department and the local committee of ethics and research (The FM-BSU REC) and obtaining consents from the patients or their guardians. This study was performed from 21 November 2015 to 21 November The study included ninety postoperative adult patients of both sex (aged years old) who required close monitoring and mechanical ventilation and sedation for 24 h after major surgery, excluding pregnant females, history of epilepsy and patients with increased intracranial tension, major renal, hepatic or cardiac diseases, neurosurgical operations or having allergies to the studied drugs. On arrival to the SICU the patients were connected to mechanical ventilator (initial sitting were SIMV mode, FiO 2 40%, PEEP 5-8 cm H 2 O, pressure support Cm H 2 O), monitoring were applied (5 leads ECG, pulse oximetry, capnography, invasive and noninvasive arterial blood pressure, and central venous pressure were monitored), BIS electrodes were applied to the forehead. 12 leads ECG, chest X-ray were done; a blood sample was taken for complete blood count, biochemistry and arterial 2 blood gas analysis. The patients were randomly divided into three equal groups according to closed, opaque envelop technique (30 patients each): Group A: 30 patients received ketofol an initial bolus dose (500 mcg/kg) of ketamine/propofol 1:1 (ketamine 8 mg/ml and propofol 8 mg/ml followed by a maintenance dose of (10 mcg/ kg/min) [14]. Group B: 30 patients received loading dose infusion of dexmedetomidine (precedex, Hospira inc lake forest, IL60045 US) diluted in 0.9% sodium chloride 1 mcg/kg/h over 10 min followed by a maintenance infusion of mcg/kg/h [15]. Group C: 30 patients received propofol (diprivan;fresenius Kabi Astaria GmbH-A8005Gra kz, Austaria) undiluted as an infusion of 1-3 mg/kg/h, after a loading dose infusion up to 1 mg/kg over 10 min. The following data were collected and recorded by SICU staff unaware of the study protocol 1. Demographic data (age, sex, weight) and types of surgeries. 2. Degree of sedation was recorded hourly for 24 h using the Ramsay sedation score (16) and continuously using the bispectral index, and the sedation level was maintained at RSS>2 by adjustment of the drug infusion rate, as a primary outcome. 3. Systolic Blood Pressure (SBP), Diastolic Blood Pressure (DBP) and Heart Rate (HR). 4. Recovery time: the time required for the patient to regain the conscious level before sedation) after discontinuing sedation [16]. 5. Complications including hypotension which is defined as (systolic blood pressure less than 90 mmhg), hypertension which is defined as systolic blood pressure more than 160 mmhg, bradycardia (heart rate less than 60 beats/ minute), and tachycardia (heart rate more than 90 beats/ minute) were also recorded. Hypotension was managed by lowering the infusion rate of sedation and IV bolus of crystalloid fluid; hypertensive events were achieved by increasing the sedation infusion rate till stabilizing the blood pressure then the infusion rate was adjusted according to the study protocol. Inadequate analgesia was expected if the patient experienced tachycardia or hypertension>20% from the baseline reading in spite of adequate sedation level as indicated by BIS value, so fentanyl (25-50 µg IV bolus) was given. Statistical analysis Sample size After a pilot study with five patients in each group, the minimum detectable difference in RSS between groups was 0.8, and a standard deviation of residuals was 0.7. Accordingly, the calculated
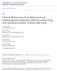
3 minimum sample size was 24 patients in each group with 95% power and α level was 0.05 using F-test (ANOVA), Biostatstics, version3.01.the number was increased to 30 patients in each group in case of the drop in any case. Statistical methods All statistical calculations were done using computer programs Microsoft Excel (Microsoft Corporation, NY, USA) & SPSS (Statistical Package for the social science) statistical programs (SPSS Inc., Chicago, IL, USA). Data were statistically described in terms of mean ± standard deviation (SD), median (range) or number (percentage) as appropriate. Inferential analyses were done for quantitative variables using paired T-test or one way ANOVA. P-values less than 0.05 were considered significant and p values less than 0.01 were considered highly significant. Results All cases completed the study, Figure 1. Table 1 showed the types of surgeries No statistically significant differences in the demographic data between the studied groups (p value>0.05); (Table 2). Systolic Blood Pressure (SBP), diastolic Blood Pressure (DBP) and Heart Rate (HR) were recorded before starting sedation, then after starting sedation by 30 min, then hourly for 24 h, but for statistical analysis the data were averaged and recorded at 6 h interval. The heart rate was higher in group A than group B and C before starting sedation, but it was not statistically significant (p>0.05), the heart rate was statistically significantly higher in group A than both group B and C 30 min after starting sedation and at sixth, twelfth, eighteenth and twenty-fourth h (p 0.001), it was also statistically significantly higher in group C than group B 30 min after starting sedation and at sixth, twelfth, eighteenth and twenty-fourth h (p ) (Table 3). The systolic arterial blood pressure was statistically significantly higher in group A than both group B and C 30 min after starting sedation, and at sixth, twelfth, eighteenth and twenty-fourth h, Enrollment Assessed for eligibility (n=90) Excluded Not meeting inclusion criteria Declined to participate Other reasons Randomized (n=90) Allocation Allocated to Group A (n=30) Received allocated intervention (n=30) Did not receive allocated intervention Allocated to Group B (n=30) Received allocated intervention (n=30) Did not receive allocated intervention Allocated to Group C (n=30) Received allocated intervention (n=30) Did not receive allocated intervention Follow Up Lost to follow-up Discontinued intervention Lost to follow-up Discontinued intervention Lost to follow-up Discontinued intervention Analysis Analyzed (n=30) Excluded from analysis Analyzed (n=30) Excluded from analysis Analyzed (n=30) Excluded from analysis Figure 1 Consort flow participant diagram. Under License of Creative Commons Attribution 3.0 License 3
4 Table 1 Types of surgeries. Data are presented as numbers (%) Types of surgeries (no %) Group A (n=30) Group B (n=30) Group C (n=30) Cesarean hysterectomy 8 (26.6) 9 (30) 8 (26.6) Radical cystectomy 5 (16.6) 3 (10) 5 (16.6) Abdominal Exploration 7 (23.3) 8 (26.6) 4 (13.3) Amputation 8 (26.6) 5 (16.6) 4 (13.3) Embolectomy 0 (0) 2 (6.6) 3 (10) Fixation of fractured femur 2 (6.6) 1 (3.3) 3 (10) Fixation of cervical spine 0 (0) 2 (6.6) 2 (6.6) Fixation of dorsal spine 0 (0) 0 (0) 1 (3.3) Table 2 Demographic data of the three groups. Data were presented as mean ± SD and number (percentage), p<0.05 is considered significant Variable Group A (n=30) Group B (n=30) Group C (n=30) p value Age (year) 34.6 ± ± ± Weight (kg) 67.7 ± ± ± Sex, no. (%) Male 18 (60) 20 (66.7) 19 (63.3) Female 12 (40) 10 (33.3) 11 (36.7) Table 3 Heart rate (Bpm). p value<0.05 were considered significant and P values<0.01 were considered highly significant. Time Group A (n=30) Group B (n=30) Group C (n=30) p value Before sedation ± ± ± min after sedation 90.4 ± ± ± th h after sedation 91.1 ± ± ± th h after sedation 91.1 ± ± ± th h after sedation 92.3 ± ± ± th h after sedation 91.4 ± ± ± 1.6 p 1 =0.419 P 2 =0.192 p 3 =0.616 (p 0.001), it was also statistically significantly higher in group B than C 30 min after starting sedation and at sixth, twelfth, eighteenth and twenty-fourth h (p 0.001) (Table 4). The Diastolic Blood Pressure (DBP) was statistically significantly higher in group A than group B and C from the first to the 24 th h, 4 DBP was statistically significantly higher in group B than C 30 min after starting sedation and at the sixth, twelfth, eighteenth and twenty-fourth h (p 0.001) (Table 5). BIS value was statistically significantly higher in group A than group B at sixth h only (p 0.01). It was statistically significantly
5 Table 4 Systolic arterial blood pressure (mmhg). p values less than 0.05 were considered significant and P values less than 0.01 were considered highly significant. Time Group A (n=30) Group B (n=30) Group C (n=30) p value Before sedation ± ± ± 6.5 p1=0.26 p2=0.33 p3= min after sedation ± ± ± th h after sedation ± ± ± th h after sedation ± ± ± th h after sedation ± ± ± th h after sedation ± ± ± 4.3 Table 5 Diastolic arterial blood pressure (mmhg). p values less than 0.05 were considered significant and P values less than 0.01 were considered highly significant. Time Group A (n=30) Group B (n=30) Group C (n=30) p value Before sedation 79.7 ± ± ± 2 p1=0.16 p2=0.33 p3= min after sedation 74.7 ± ± ± th h after sedation 75.8 ± ± ± th h after sedation 73.5 ± ± ± th h after sedation 73.4 ± ± ± th h after sedation 75.5 ± ± ± 1 higher in group A than group C at first and eighteenth h (p 0.01), and was statistically significantly higher in group B than group C from the first to 24 h (p 0.01) (Table 6). Under License of Creative Commons Attribution 3.0 License RAMSY sedation score was statistically significantly higher in group A than group B at sixth and twelfth h, it was statistically significantly higher in group A than group C in the first, sixth and eighteenth h, it was statistically significantly higher in group B 5
6 Table 6 Bispectral index (BIS). p values<0.05 were considered significant and P values<0.01 were considered highly significant. BIS Group A (n=30) Group B (n=30) Group C (n=30) p-value p1= st h 76.6 ± ± ± th h 74.8 ± ± ± 4.0 p1=0.037 p2= th h 74.7 ± ± ± 3.5 p1=0.059 p2=0.210 p3= th h 75.1 ± ± ± 3.4 p1=0.209 p2= th h 74.4 ± ± ± 4.2 p1=0.196 p2=0.064 p3=0.002 Table 7 Ramsay sedation score. Data were presented as median (range). p values<0.05 were considered significant and P values < 0.01 were considered highly significant. RAMSY scoring system Group A (n=30) Group B (n=30) Group C (n=30) p value 1 st h 3 (2-4) 3 (2-4) 3 (2-5) p1=0.397 p2= p3= th h 3 (2-4) 3 (2-4) 3 (3-5) p1=0.022 p2=0.028 p3= th h 3 (2-4) 3 (2-4) 3 (3-5) p1=0.006 p2= th h 3 (2-4) 3 (2-4) 3 (3-5) p1=0.306 p2= p3= th h 3 (2-4) 3 (2-4) 3 (3-5) p1=0.085 p2=0.120 p3=0.011 than group C from the first to twenty-fourth h (Table 7). The recovery time was longer in group A compared to group B and C, and it was statistically significant (p 0.05) (Table 8). The mean administered dosages of fentanyl was ± 9.7 µg, ± 7.5 µg, ± 12.3 µg for groups A-C respectively, it was statistically significantly higher in group C than group A and B group (p 0.001), and it was statistically significantly higher in group A than in B group (p 0.001) (Table 9). 6 Discussion The current study showed that infusion of ketofol, dexmedetomidine or propofol was effective for sedation of mechanically ventilated patients in SICU as detected by RSS which is maintained in the range of 2-4 for the patients who were sedated by ketofol or dexmedetomidine and 2-5 for the patients who were sedated by propofol without causing hemodynamic complications. Dexmedetomidine group required less fentanyl for postoperative analgesia.
7 Table 8 Recovery time (min). p values<0.05 were considered significant and P values<0.01 were considered highly significant. Group A (n=30) Group B (n=30) Group C (n=30) p value Recovery time (min.) 35.8 ± ± ± 8.6 Table 9 Fentanyl requirement (µg). p values<0.05 were considered significant and P values<0.01 were considered highly significant. p1=0.038 p2=0.038 p3=0.541 Group A (n=30) Group B (n=30) Group C (n=30) P value Fentanyl requirement (µg) ± ± ± 12.3 p p p There are few available data in the scientific literature for using ketofol for sedating the patients in ICUs but there are several trials used ketofol for procedural sedation. The result of this study coincides with those of the study which was performed by Hamimy et al. [14]. They concluded that using ketofol for sedating the mechanically ventilated patients was effective in maintaining Ramsay sedation score of 4 without hemodynamic instability. Willman [17] and Andolfatto [18] concluded that none of the patients developed hypotension when ketofol was administrated in a mean dose of (0.75 mg/kg of ketamine and 0.75 mg/ kg of propofol) but they reported in another study that only 1 patient out of 728 patients became hypotensive when ketofol was used for PSA for orthopedic procedures. Dal et al. [19] concluded that ketofol was effective and safe for sedation during endobronchial ultrasound-guided needle aspiration procedure. Ghadami et al. [20] reported that quality of sedation, the total dose of the drug and respiratory and hemodynamic parameters were comparable when using two different ratios of ketofol in 60 pediatric patients scheduled for lumbar puncture or bone marrow aspiration. David et al. [21] did not report a significant difference in respiratory depression between 98 adults and 93 children. Tosun et al. [22] demonstrated that ketofol was useful for sedation and providing hemodynamic stability in pediatric patients who underwent upper GIE procedures. On the other hand, Loh et al. [23] reported that fewer patients who were given ketofol had a significant hemodynamic compromise, and required active interventions using fluid or vasopressor. They explained their results by the opposite effect of ketamine and propofol on the autonomic nervous system, as ketamine is sympathomimetic, but propofol lessens this effect. 7 One study was done by Venn et al. [24] which included 20 adult patients who required at least 8 h of postoperative mechanical ventilation, the patients who were sedated by dexmedetomidine significantly needed less alfentanil (2.5 vs. 0.8 mg.h -1 ) than those sedated by propofol. RSS for propofol was 5 [4,5], and for dexmedetomidine, RSS was 5 [4-6]. In the current study, RSS was 2-4 for dexmedetomidine and 2-5 for the patients who were sedated by propofol; the difference between this study and the study of Venn et al. may be explained by different time for assessing the BIS value as this study was for 24 h and the study of Venn et al. [24] was for 8 h, also due to different number of the patients between the two studies. In a study by Prerana et al. [25] that included thirty patients who required postoperative mechanical ventilation and sedation; 15 patients received dexmedetomidine, and 15 patients received propofol. The mean pulse-rate, respiratory rate, blood pressure between the groups was not statistically significant. The mean RSS was between 2-4 and 2-3 for dexmedetomidine and propofol groups respectively. In this study, Ramsay sedation score was 2-4 and 2-5 for dexmedetomidine group and propofol group respectively. These results were not in line with the study by Corbett et al. [26] they titrated dexmedetomidine or propofol to a Ramsay sedation score of 3 4. Demiraran et al. [27] did not find a difference in HR, mean arterial pressure, or recovery time in a prospective trial of 50 patients underwent upper endoscopy sedated with dexmedetomidine or midazolam. Stephan et al. [28] reported that ICU patients receiving prolonged mechanical ventilation, dexmedetomidine was comparable
8 to midazolam and propofol in maintaining light to moderate sedation. In the current study the recovery time was 35.8 ± 14.4 min for the patients sedated by ketofol 29.5 ± 10.9 min for the patients sedated by dexmedetomidine and it was 27.7 ± 8.6 min for the patients who were sedated by propofol, while in the study of Hamimy et al. [14] the median recovery time was 30 min (range min) and in the study of Andolfatto et al. [17] the median recovery time was 14 min (range 3 50 min). The different number of patients may explain the difference between this study and other studies, and they used ketofol while in this study included three groups of patients sedated by ketofol, dexmedetomidine or propofol, and Andolfatto et al. [17] used ketofol for procedural sedation. In this study, the patients sedated by dexmedetomidine required less fentanyl than patients sedated by ketofol or propofol. This was also reported by Vinit et al. [29]. References 1 Lonardo NW, Mone MC, Nirula R, Kimball EJ, Ludwig K, et al. (2014) The propofol is associated with favorable outcomes compared with benzodiazepines in ventilated intensive care unit patient. Am J Respir Crit Care Med 189: Barr J, Fraser GL, Puntillo K, Ely EW, Gelinas C, et al. (2013) Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the intensive care unit. Crit Care Med 41: Girard TD, Jackson JC, Pandharipande PP, Pun BT, Thompson JL, et al. (2010) Delirium as a predictor of long-term cognitive impairment in survivors of critical illness. Crit Care Med 38: Ely EW, Shintani A, Truman B, Speroff T, Gordon SM, et al. (2004) Delirium as a predictor of mortalityin mechanically ventilated patients in the intensive care unit. JAMA 291: Pandharipande P, Shintani A, Peterson J, Pun BT, Wilkinson GR, et al. (2006) Lorazepam is an independent risk factor for transitioning to delirium in intensive care unit patients. Anesthesiology 104: Carson SS, Kress JP, Rodgers JE, Vinayak A, Campbell-Bright S, et al. (2006) A randomized trial of intermittent lorazepam versus propofol with daily interruption in mechanically ventilated patients. Crit Care Med 34: Shehabi Y, Riker RR, Bokesch PM, Wisemandle W, Shintani A, et al. (2010) Delirium duration and mortality inlightly sedated, mechanically ventilated intensive care patients. Crit Care Med 38: Singh R, Batra YK, Bharti N, Panda NB (2010) Comparison of propofol versus propofol ketamine combination for sedation during spinal anesthesia in children: Randomized clinical trial of efficacy and safety. Paediatr Anaesth 20: Yamauchi M, Asano M, Watanabe M, Iwasaki S, Furuse S, et al. (2008) Continuous low-dose ketamine improves the analgesic effects of fentanyl patient-controlled analgesia after cervical spine surgery. Anesth Analg 107: Conclusion This study concluded that using ketofol, dexmedetomidine or propofol for sedation of postoperative intubated and mechanically ventilated patients in the surgical ICU for 24 h was effective in maintaining Ramsay sedation score in the range of 2-4 for the patients who were sedated by ketofol or dexmedetomidine and 2-5 for the patients who were sedated by propofol without causing hemodynamic instability. Limitations of the Study More studies are recommended for the longer duration of mechanical ventilation. Conflicts of Interest The authors declare that there are no conflicts of interest. 10 Camu F, Vanlersberghe C (2002) Pharmacology of systemic analgesics. Best Pract Res Clin Anaesthesiol 16: Venn RM, Hell J, Grounds RM (2000) Respiratory effects of dexmedetomidine in the surgical patient requiring intensive care. Crit Care 4: Hall JE, Uhrich TD, Barney JA, Arain SR, Ebert TJ (2000) Sedative, amnestic, and analgesic properties of small-dose dexmedetomidine infusion. Anesth Analg 90: 699: O'Connor M, Bucknall T, Manias E (2010) Sedation Management in Australian and New Zealand Intensive Care Units: Doctors' and Nurses' Practices and Opinions. Am J Crit Care 19: Hamimy IW, Zaghloul A, Mahmoud AAA (2012) The application of a new regimen for short term sedation in the ICU (ketofol) Case series. Egyptian J Anaesthesia 28: American Society of Anesthesiologists Task Force on Sedation Analgesia by Non-Anesthesiologists (2002) Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology 96: Ramsay MA, Savege TM, Simpson BR, Goodwin R (1974) Controlled sedation with alphaxalone-alphadolone. Br Med J 22: Willman EV, Andolfatto G (2007) A Prospective evaluation of ketofol (ketamine/propofol combination for proceduralsedation and analgesia in the emergency department. Ann Emerg Med 49: Andolfatto G, Willman EV (2011) A prospective case series of single syringe ketamine propofol (ketofol) for emergency department procedural sedation and analgesia in adults. Acad Emerg Med 3: Dal T, Sazak H, Tunc M, Sahin S, Yilmaz A (2014) A comparison ofketamine-midazolam and ketamine-propofol combinations used for sedation in the endobronchial ultrasound guided transbronchialneedle aspiration: a prospective, single blind, randomized study. J Thorac Dis 6: Yazdi GA, Ayatollahi V, Hashemi A, Behdad SH, Yazdi GE (2013) Effect of two different concentrations of propofol 8
9 and'ketamine combinations (Ketofol) in pediatric patients under lumbar puncture or bone marrow aspiration. Iran J Ped Hematol Oncol 3: David H, Shipp J (2011) A randomised, controlled trial of ketamine/propofol versus propofol alone for emergency department procedural sedation. Ann Emerg Med 57: Tosun Z, Aksu R, Guler G, Esmaoglu A, Akin A, et al. (2007) Propofol-ketamine vs propofol-fentanyl for sedation during pediatric upper gastrointestinal endoscopy. Pediatr Anesth 17: Loh G, Dalen D (2007) Low-dose ketamine in addition to propofol for procedural sedation and analgesia in the emergency department. Ann Pharmacother 41: Venn RM, Grounds RM (2001) Comparison between dexmedetomidine and propofol for sedation in the intensive care unit: patient and clinician perceptions. Br J Anaesth 87: Shah PN, Dongre V, Patil V, Pandya S, Mungantiwar A, et al. (2014) Comparison of post-operative ICU sedation between dexmedetomidine and propofol in Indian population. Indian J Crit Care Med 18: Corbett SM, Rebuck JA, Greene CM, Callas PW, Neale BW, et al. (2005) Dexmedetomidine does not improve patient satisfaction when compared to propofol during mechanical ventilation. Crit Care Med 33: Demiraran Y, Korkut E, Tamer A, Yorulmaz I, Kocaman B, et al. (2007) The comparison of dexmedetomidine and midazolam used for sedation of patients during upper endoscopy: A prospective, randomized study. Can J Gastroenterol 21: Jakob SM, Ruokonen E, Grounds RM, Sarapohja T, Garratt C, et al. (2012) Dexmedetomidine vs midazolam or propofol for sedation during prolonged mechanical ventilation: Two randomized controlled trials. JAMA 307: Srivastava VK, Agrawal S, Kumar S, Mishra A, Sharma S, et al. (2014) Comparison of dexmedetomidine, propofol and midazolam for short-term sedation in postoperatively mechanically Ventilated neurosurgical patients. J Clin Diagn Res 8: GC04 GC07. 9
A COMPARATIVE STUDY OF MIDAZOLAM, PROPOFOL AND DEXMEDETOMIDINE INFUSIONS FOR SEDATION IN ME- CHANICALLY VENTILATED PATIENTS IN ICU
 ORIGINAL ARTICLE A COMPARATIVE STUDY OF MIDAZOLAM, PROPOFOL AND DEXMEDETOMIDINE INFUSIONS FOR SEDATION IN ME- CHANICALLY VENTILATED PATIENTS IN ICU Suresh Chandra Dulara 1, Pooja Jangid 2, Ashish Kumar
ORIGINAL ARTICLE A COMPARATIVE STUDY OF MIDAZOLAM, PROPOFOL AND DEXMEDETOMIDINE INFUSIONS FOR SEDATION IN ME- CHANICALLY VENTILATED PATIENTS IN ICU Suresh Chandra Dulara 1, Pooja Jangid 2, Ashish Kumar
Appendix: Outcomes when Using Adjunct Dexmedetomidine with Propofol Sedation in
 SUPPLEMENTAL CONTENT Appendix: Outcomes when Using Adjunct Dexmedetomidine with Propofol Sedation in Mechanically Ventilated Surgical Intensive Care Patients Table of Contents Methods Summary of Definitions
SUPPLEMENTAL CONTENT Appendix: Outcomes when Using Adjunct Dexmedetomidine with Propofol Sedation in Mechanically Ventilated Surgical Intensive Care Patients Table of Contents Methods Summary of Definitions
Comparison of dexmedetomidine and propofol in mechanically ventilated patients with sepsis: A pilot study
 Original article Comparison of dexmedetomidine and propofol in mechanically ventilated patients with sepsis: A pilot study Mark B. Sigler MD, Ebtesam A. Islam MD PhD, Kenneth M. Nugent MD Abstract Objective:
Original article Comparison of dexmedetomidine and propofol in mechanically ventilated patients with sepsis: A pilot study Mark B. Sigler MD, Ebtesam A. Islam MD PhD, Kenneth M. Nugent MD Abstract Objective:
Hemodynamic effects of dexmedetomidine-- fentanyl vs. nalbuphine--propofol in plastic surgery
 Hemodynamic effects of dexmedetomidine-- fentanyl vs. nalbuphine--propofol in plastic surgery Juan F. De la Mora-González *, José A. Robles-Cervantes 2,4, José M. Mora-Martínez 3, Francisco Barba-Alvarez
Hemodynamic effects of dexmedetomidine-- fentanyl vs. nalbuphine--propofol in plastic surgery Juan F. De la Mora-González *, José A. Robles-Cervantes 2,4, José M. Mora-Martínez 3, Francisco Barba-Alvarez
DOI /yydb medetomidine a review of clinical applications J. Curr Opin Anaesthesiol
 1573 medetomidine a review of clinical applications J. Curr Opin Anaesthesiol 2008 21 4 457-461. 6 DAHMANI S PARIS A JANNIER V et al. Dexmedetom- 2. α 2 idine increases hippocampal phosphorylated extracellular
1573 medetomidine a review of clinical applications J. Curr Opin Anaesthesiol 2008 21 4 457-461. 6 DAHMANI S PARIS A JANNIER V et al. Dexmedetom- 2. α 2 idine increases hippocampal phosphorylated extracellular
Comparison of Intensive Care Unit Sedation Using Dexmedetomidine, Propofol, and Midazolam
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/24 Comparison of Intensive Care Unit Sedation Using Dexmedetomidine, Propofol, and Midazolam Gajendra Singh, Kakhandki
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/24 Comparison of Intensive Care Unit Sedation Using Dexmedetomidine, Propofol, and Midazolam Gajendra Singh, Kakhandki
Therapeutics and clinical risk management (2011) Vol.7:291~299. Dexmedetomidine hydrochloride as a long-term sedative.
 Therapeutics and clinical risk management (2011) Vol.7:291~299. Dexmedetomidine hydrochloride as a long-term sedative Kunisawa Takayuki Therapeutics and Clinical Risk Management open access to scientific
Therapeutics and clinical risk management (2011) Vol.7:291~299. Dexmedetomidine hydrochloride as a long-term sedative Kunisawa Takayuki Therapeutics and Clinical Risk Management open access to scientific
Propofol vs Dexmedetomidine
 Propofol vs Dexmedetomidine A highlight of similarities & differences Lama Nazer, PharmD, BCPS Critical Care Clinical Pharmacy Specialist King Hussein Cancer Center Outline Highlight similarities and differences
Propofol vs Dexmedetomidine A highlight of similarities & differences Lama Nazer, PharmD, BCPS Critical Care Clinical Pharmacy Specialist King Hussein Cancer Center Outline Highlight similarities and differences
A Clinical Study of Dexmedetomidine under Combined Spinal Epidural Anaesthesia at a Tertiary Care Hospital
 Original Research A Clinical Study of Dexmedetomidine under Combined Spinal Epidural Anaesthesia at a Tertiary Care Hospital Kamala GR 1, Leela GR 2 1 Assistant Professor, Department of Anaesthesiology,
Original Research A Clinical Study of Dexmedetomidine under Combined Spinal Epidural Anaesthesia at a Tertiary Care Hospital Kamala GR 1, Leela GR 2 1 Assistant Professor, Department of Anaesthesiology,
Susan Becker DNP, RN, CNS, CCRN, CCNS Marymount University, Arlington, VA
 Susan Becker DNP, RN, CNS, CCRN, CCNS Marymount University, Arlington, VA Disclosures Study and presentation has no commercial bias or interests No financial relationship with a commercial interest, products,
Susan Becker DNP, RN, CNS, CCRN, CCNS Marymount University, Arlington, VA Disclosures Study and presentation has no commercial bias or interests No financial relationship with a commercial interest, products,
SCIENTIFIC COOPERATIONS MEDICAL WORKSHOPS July, 2015, Istanbul - TURKEY
 21-22 July, 2015, Istanbul - TURKEY PROSPECTIVE EVALUATION OF CORRELATION OF DEPTH OF DEXMEDETOMIDINE SEDATION AND CLINICAL EFFECTS FOR RECONSTRUCTIVE SURGERIES UNDER REGIONAL ANAESTHESIA Alma Jaunmuktane
21-22 July, 2015, Istanbul - TURKEY PROSPECTIVE EVALUATION OF CORRELATION OF DEPTH OF DEXMEDETOMIDINE SEDATION AND CLINICAL EFFECTS FOR RECONSTRUCTIVE SURGERIES UNDER REGIONAL ANAESTHESIA Alma Jaunmuktane
Disclosures. Dexmedetomidine: The Good, The Bad and The Delirious. The Delirious. Objectives. Characteristics of Delirium. Definition of Delirium
 Dexmedetomidine: The Good, The Bad and The Delirious Disclosures! I have no actual or potential conflict of interest in relation to this presentation. By John J. Bon, Pharm.D., BCPS Lead Clinical Pharmacist,
Dexmedetomidine: The Good, The Bad and The Delirious Disclosures! I have no actual or potential conflict of interest in relation to this presentation. By John J. Bon, Pharm.D., BCPS Lead Clinical Pharmacist,
ASMIC 2016 DEXMEDETOMIDINE IN THE INTENSIVE CARE UNIT DR KHOO TIEN MENG
 ASMIC 2016 DEXMEDETOMIDINE IN THE INTENSIVE CARE UNIT DR KHOO TIEN MENG PREAMBLE : EVOLUTION OF SEDATION IN THE ICU 1980s : ICU sedation largely extension of GA No standard approach, highly variable Deep
ASMIC 2016 DEXMEDETOMIDINE IN THE INTENSIVE CARE UNIT DR KHOO TIEN MENG PREAMBLE : EVOLUTION OF SEDATION IN THE ICU 1980s : ICU sedation largely extension of GA No standard approach, highly variable Deep
Use of Dexmedetomidine for Sedation of Children Hospitalized in the Intensive Care Unit
 ORIGINAL RESEARCH Use of Dexmedetomidine for Sedation of Children Hospitalized in the Intensive Care Unit Christopher L. Carroll, MD 1 Diane Krieger, MSN, CPNP 1 Margaret Campbell, PharmD 2 Daniel G. Fisher,
ORIGINAL RESEARCH Use of Dexmedetomidine for Sedation of Children Hospitalized in the Intensive Care Unit Christopher L. Carroll, MD 1 Diane Krieger, MSN, CPNP 1 Margaret Campbell, PharmD 2 Daniel G. Fisher,
NIH Public Access Author Manuscript J Crit Care. Author manuscript; available in PMC 2013 July 28.
 NIH Public Access Author Manuscript Published in final edited form as: J Crit Care. 2009 December ; 24(4): 568 574. doi:10.1016/j.jcrc.2009.05.015. A new dosing protocol reduces dexmedetomidine-associated
NIH Public Access Author Manuscript Published in final edited form as: J Crit Care. 2009 December ; 24(4): 568 574. doi:10.1016/j.jcrc.2009.05.015. A new dosing protocol reduces dexmedetomidine-associated
Corresponding author: V. Dua, Department of Anaesthesia, BJ Wadia Hospital for Children, Parel, Mumbai, India.
 Comparative evaluation of dexmedetomidine as a premedication given intranasally vs orally in children between 1 to 8 years of age undergoing minor surgical procedures V. Dua, P. Sawant, P. Bhadlikar Department
Comparative evaluation of dexmedetomidine as a premedication given intranasally vs orally in children between 1 to 8 years of age undergoing minor surgical procedures V. Dua, P. Sawant, P. Bhadlikar Department
TITLE: Dexmedetomidine for Sedation of Patients in the ICU or PICU: Review of Clinical Effectiveness and Safety
 TITLE: Dexmedetomidine for Sedation of Patients in the ICU or PICU: Review of Clinical Effectiveness and Safety DATE: 16 January 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential
TITLE: Dexmedetomidine for Sedation of Patients in the ICU or PICU: Review of Clinical Effectiveness and Safety DATE: 16 January 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential
Dexmedetomidine. Dr.G.K.Kumar,M.D.,D.A., Assistant Professor, Madras medical college,chennai. History
 Dexmedetomidine Dr.G.K.Kumar,M.D.,D.A., Assistant Professor, Madras medical college,chennai Dexmedetomidine is the most recently released IV anesthetic. It is a highly selective α 2 -adrenergic agonist
Dexmedetomidine Dr.G.K.Kumar,M.D.,D.A., Assistant Professor, Madras medical college,chennai Dexmedetomidine is the most recently released IV anesthetic. It is a highly selective α 2 -adrenergic agonist
Associate Professor, Department of Anaesthesiology, Government Thoothukudi Medical College, Thoothukudi, Tamil Nadu, India, 2
 Original Article DOI: 10.17354/ijss/2016/295 Effect of Intravenous use of Dexmedetomidine on Anesthetic Requirements in Patients Undergoing Elective Spine Surgery: A Double Blinded Randomized Controlled
Original Article DOI: 10.17354/ijss/2016/295 Effect of Intravenous use of Dexmedetomidine on Anesthetic Requirements in Patients Undergoing Elective Spine Surgery: A Double Blinded Randomized Controlled
Comparison of several dosing schedules of intravenous dexmedetomidine in elderly patients under spinal anesthesia
 Anesth Pain Med 2017;12:320-325 https://doi.org/10.17085/apm.2017.12.4.320 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received January 11, 2017 Revised 1st, February 28, 2017 2nd, April 4, 2017
Anesth Pain Med 2017;12:320-325 https://doi.org/10.17085/apm.2017.12.4.320 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received January 11, 2017 Revised 1st, February 28, 2017 2nd, April 4, 2017
Chronic subdural hematoma (CSDH) is one of the most
 CLINICAL INVESTIGATION Comparison of Dexmedetomidine Versus Midazolam-Fentanyl Combination for Monitored Anesthesia Care During Burr-Hole Surgery for Chronic Subdural Hematoma Vinod Bishnoi, MD,* Bhupesh
CLINICAL INVESTIGATION Comparison of Dexmedetomidine Versus Midazolam-Fentanyl Combination for Monitored Anesthesia Care During Burr-Hole Surgery for Chronic Subdural Hematoma Vinod Bishnoi, MD,* Bhupesh
Study the Effect of Dexmedetomidine on Emergence Agitation after Nasal Surgeries
 Original Research Article Study the Effect of Dexmedetomidine on Emergence Agitation after Nasal Surgeries G V Krishna Reddy 1*, S. Kuldeep 2, G. Obulesu 3 1 Assistant Professor, Department of Anaesthesiology,
Original Research Article Study the Effect of Dexmedetomidine on Emergence Agitation after Nasal Surgeries G V Krishna Reddy 1*, S. Kuldeep 2, G. Obulesu 3 1 Assistant Professor, Department of Anaesthesiology,
The evolving approach to sedation in ventilated patients: a real world perspective
 Editorial Page 1 of 5 The evolving approach to sedation in ventilated patients: a real world perspective Annachiara Marra 1,2, Pratik P. Pandharipande 3 1 Department of Medicine, Division of Allergy and
Editorial Page 1 of 5 The evolving approach to sedation in ventilated patients: a real world perspective Annachiara Marra 1,2, Pratik P. Pandharipande 3 1 Department of Medicine, Division of Allergy and
Haemodynamic and anaesthetic advantages of dexmedetomidine
 Haemodynamic and anaesthetic advantages of dexmedetomidine Abstract Rao SH, Assistant Professor Sudhakar B, Associate Professor Subramanyam PK, Professor Department of Anaesthesia and Critical Care, Dr
Haemodynamic and anaesthetic advantages of dexmedetomidine Abstract Rao SH, Assistant Professor Sudhakar B, Associate Professor Subramanyam PK, Professor Department of Anaesthesia and Critical Care, Dr
Dexmedetomidine for Sedation in the Critical Care Setting: An Economic Assessment
 CADTH TECHNOLOGY REVIEW Dexmedetomidine for Sedation in the Critical Care Setting: An Economic Assessment Service Line: Technology Review Issue Number: 6 Version: 1.0 Publication Date: March 2017 Report
CADTH TECHNOLOGY REVIEW Dexmedetomidine for Sedation in the Critical Care Setting: An Economic Assessment Service Line: Technology Review Issue Number: 6 Version: 1.0 Publication Date: March 2017 Report
Invasive and noninvasive procedures
 Feature Review Article Dexmedetomidine and ketamine: An effective alternative for procedural sedation? Joseph D. Tobias, MD Objectives: Although generally effective for sedation during noninvasive procedures,
Feature Review Article Dexmedetomidine and ketamine: An effective alternative for procedural sedation? Joseph D. Tobias, MD Objectives: Although generally effective for sedation during noninvasive procedures,
Comparison of dexmedetomidine and propofol for conscious sedation in inguinal hernia repair: A prospective, randomized, controlled trial
 Research Report Comparison of dexmedetomidine and propofol for conscious sedation in inguinal hernia repair: A prospective, randomized, controlled trial Journal of International Medical Research 2017,
Research Report Comparison of dexmedetomidine and propofol for conscious sedation in inguinal hernia repair: A prospective, randomized, controlled trial Journal of International Medical Research 2017,
Ashraf Darwish, Rehab Sami, Mona Raafat, Rashad Aref and Mohamed Hisham
 Dexmedetomidine versus Propofol for Monitored Anesthesia Care In Patients Undergoing Anterior Segment Ophthalmic Surgery Under Peribulbar Medial Canthus Anesthesia Ashraf Darwish, Rehab Sami, Mona Raafat,
Dexmedetomidine versus Propofol for Monitored Anesthesia Care In Patients Undergoing Anterior Segment Ophthalmic Surgery Under Peribulbar Medial Canthus Anesthesia Ashraf Darwish, Rehab Sami, Mona Raafat,
Study between clonidine and dexmedetomidine in attenuation of pressor response during endotracheal intubation
 Original Research Article Study between clonidine and dexmedetomidine in attenuation of pressor response during endotracheal intubation K. Selvarju 1, Kondreddi Narayana Prasad 2*, Ajay Kumar Reddy Bobba
Original Research Article Study between clonidine and dexmedetomidine in attenuation of pressor response during endotracheal intubation K. Selvarju 1, Kondreddi Narayana Prasad 2*, Ajay Kumar Reddy Bobba
A Comparison of Dexmedetomidine and Midazolam for Sedation in Gynecologic Surgery Under Epidural Anesthesia
 Original Article Elmer Press A Comparison of Dexmedetomidine and Midazolam for Sedation in Gynecologic Surgery Under Epidural Anesthesia Yongxin Liang a, b, Miaoning Gu b, Shiduan Wang a, Haichen Chu a,
Original Article Elmer Press A Comparison of Dexmedetomidine and Midazolam for Sedation in Gynecologic Surgery Under Epidural Anesthesia Yongxin Liang a, b, Miaoning Gu b, Shiduan Wang a, Haichen Chu a,
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Sun, 10 Mar 2019 06:52:14 GMT) CTRI Number Last Modified On 29/07/2016 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Clinical Trial Details (PDF Generation Date :- Sun, 10 Mar 2019 06:52:14 GMT) CTRI Number Last Modified On 29/07/2016 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Dexmedetomidine vs. Propofol for Short-Term Sedation of Postoperative Mechanically Ventilated Patients
 Journal of the Egyptian Nat. Cancer Inst., Vol. 16, No. 3, September: 153-158, 2004 Dexmedetomidine vs. for Short-Term Sedation of Postoperative Mechanically Ventilated Patients SAMIA ELBARADIE, M.D.*;
Journal of the Egyptian Nat. Cancer Inst., Vol. 16, No. 3, September: 153-158, 2004 Dexmedetomidine vs. for Short-Term Sedation of Postoperative Mechanically Ventilated Patients SAMIA ELBARADIE, M.D.*;
Original Article Effects of low dose midazolam on bradycardia and sedation during dexmedetomidine infusion
 Int J Clin Exp Med 2016;9(6):11838-11844 www.ijcem.com /ISSN:1940-5901/IJCEM0020616 Original Article Effects of low dose midazolam on bradycardia and sedation during dexmedetomidine infusion Yun-Sic Bang
Int J Clin Exp Med 2016;9(6):11838-11844 www.ijcem.com /ISSN:1940-5901/IJCEM0020616 Original Article Effects of low dose midazolam on bradycardia and sedation during dexmedetomidine infusion Yun-Sic Bang
Comparison of anesthesia with a morphine lidocaine ketamine infusion or a morphine lidocaine epidural on time to extubation in dogs
 Veterinary Anaesthesia and Analgesia, 2016, 43, 86 90 doi:10.1111/vaa.12273 SHORT COMMUNICATION Comparison of anesthesia with a morphine lidocaine ketamine infusion or a morphine lidocaine epidural on
Veterinary Anaesthesia and Analgesia, 2016, 43, 86 90 doi:10.1111/vaa.12273 SHORT COMMUNICATION Comparison of anesthesia with a morphine lidocaine ketamine infusion or a morphine lidocaine epidural on
Case Report Dexmedetomidine as a Procedural Sedative for Percutaneous Tracheotomy: Case Report and Systematic Literature Review
 Case Reports in Critical Care Volume 2012, Article ID 659415, 4 pages doi:10.1155/2012/659415 Case Report Dexmedetomidine as a Procedural Sedative for Percutaneous Tracheotomy: Case Report and Systematic
Case Reports in Critical Care Volume 2012, Article ID 659415, 4 pages doi:10.1155/2012/659415 Case Report Dexmedetomidine as a Procedural Sedative for Percutaneous Tracheotomy: Case Report and Systematic
Role of Dexmedetomidine as an Anesthetic Adjuvant in Laparoscopic Surgery
 Role of Dexmedetomidine as an Anesthetic Adjuvant in Laparoscopic Surgery Vaishali Waindeskar, Munir Khan, Shankar Agarwal, M R Gaikwad Department of Anesthesiology, People s College of Medical Sciences
Role of Dexmedetomidine as an Anesthetic Adjuvant in Laparoscopic Surgery Vaishali Waindeskar, Munir Khan, Shankar Agarwal, M R Gaikwad Department of Anesthesiology, People s College of Medical Sciences
Original Contributions
 Original Contributions Use of Dexmedetomidine to Facilitate Extubation in Surgical Intensive-Care-Unit Patients Who Failed Previous Weaning Attempts Following Prolonged Mechanical Ventilation: A Pilot
Original Contributions Use of Dexmedetomidine to Facilitate Extubation in Surgical Intensive-Care-Unit Patients Who Failed Previous Weaning Attempts Following Prolonged Mechanical Ventilation: A Pilot
Rajaclimax Kirubahar, Bose Sundari, Vijay Kanna*, Kanakasabai Murugadoss
 International Journal of Research in Medical Sciences Kirubahar R et al. Int J Res Med Sci. 2016 Apr;4(4):1172-1176 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20160804
International Journal of Research in Medical Sciences Kirubahar R et al. Int J Res Med Sci. 2016 Apr;4(4):1172-1176 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20160804
Preliminary UK experience of dexmedetomidine, a novel agent for postoperative sedation in the intensive care unit
 Preliminary UK experience of dexmedetomidine, a novel agent for postoperative sedation in the intensive care unit R. M. Venn, 1 C. J. Bradshaw, 1 R. Spencer, 2 D. Brealey, 3 E. Caudwell, 3 C. Naughton,
Preliminary UK experience of dexmedetomidine, a novel agent for postoperative sedation in the intensive care unit R. M. Venn, 1 C. J. Bradshaw, 1 R. Spencer, 2 D. Brealey, 3 E. Caudwell, 3 C. Naughton,
Egyptian Society of Anesthesiologists. Egyptian Journal of Anaesthesia.
 Egyptian Journal of Anaesthesia (2010) 26, 299 304 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Comparative
Egyptian Journal of Anaesthesia (2010) 26, 299 304 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Comparative
Quality of MRI pediatric sedation: Comparison between intramuscular and intravenous dexmedetomidine
 Egyptian Journal of Anaesthesia (2013) 29, 47 52 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Quality of MRI
Egyptian Journal of Anaesthesia (2013) 29, 47 52 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Quality of MRI
Comparison of Clonidine and Dexmedetomidine on Cardiovascular Stability in Laparoscopic Cholecystectomy
 Original Article DOI: 10.17354/ijss/2016/185 Comparison of Clonidine and Dexmedetomidine on Cardiovascular Stability in Laparoscopic Cholecystectomy Devang Bharti 1, Juhi Saran 2, Chetan Kumar 3, H S Nanda
Original Article DOI: 10.17354/ijss/2016/185 Comparison of Clonidine and Dexmedetomidine on Cardiovascular Stability in Laparoscopic Cholecystectomy Devang Bharti 1, Juhi Saran 2, Chetan Kumar 3, H S Nanda
Dexmedetomidine intravenous sedation using a patient-controlled sedation infusion pump: a case report
 Case Report pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2016;16(1):55-59 http://dx.doi.org/10.17245/jdapm.2016.16.1.55 Dexmedetomidine intravenous sedation using a patient-controlled sedation
Case Report pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2016;16(1):55-59 http://dx.doi.org/10.17245/jdapm.2016.16.1.55 Dexmedetomidine intravenous sedation using a patient-controlled sedation
Clinical effectiveness of a sedation protocol minimizing benzodiazepine infusions and favoring early dexmedetomidine: A before-after study
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Clinical effectiveness of a sedation protocol minimizing benzodiazepine infusions and favoring early dexmedetomidine:
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Clinical effectiveness of a sedation protocol minimizing benzodiazepine infusions and favoring early dexmedetomidine:
Period of study: 12 Nov 2002 to 08 Apr 2004 (first subject s first visit to last subject s last visit)
 Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Safety and efficacy of dexmedetomidine for long-term sedation in critically ill patients
 J Anesth (2014) 28:38 50 DOI 10.1007/s00540-013-1678-5 ORIGINAL ARTICLE Safety and efficacy of dexmedetomidine for long-term sedation in critically ill patients Makoto Ozaki Junzo Takeda Keiji Tanaka Yasuhiro
J Anesth (2014) 28:38 50 DOI 10.1007/s00540-013-1678-5 ORIGINAL ARTICLE Safety and efficacy of dexmedetomidine for long-term sedation in critically ill patients Makoto Ozaki Junzo Takeda Keiji Tanaka Yasuhiro
Alfaxan. (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. TECHNICAL NOTES DESCRIPTION INDICATIONS
 Alfaxan (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. NADA 141-342, Approved by FDA ALFAXAN (Schedule: C-IV) (alfaxalone 10 mg/ml) Intravenous injectable anesthetic
Alfaxan (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. NADA 141-342, Approved by FDA ALFAXAN (Schedule: C-IV) (alfaxalone 10 mg/ml) Intravenous injectable anesthetic
Parthasarathy et al. Sri Lankan Journal of Anaesthesiology: 25(2):76-81(2017)
 Comparison of efficacy of intravenous dexmedetomidine with intravenous ketamine in allaying procedural discomfort during establishment of subarachnoid block S Parthasarathy 1*, AJ Charles 2, DR Singh 1,
Comparison of efficacy of intravenous dexmedetomidine with intravenous ketamine in allaying procedural discomfort during establishment of subarachnoid block S Parthasarathy 1*, AJ Charles 2, DR Singh 1,
A SYSTEMATIC REVIEW ON THE USE OF DEXMEDETOMIDINE AS A SOLE AGENT FOR INTRAVENOUS MODERATE SEDATION
 A SYSTEMATIC REVIEW ON THE USE OF DEXMEDETOMIDINE AS A SOLE AGENT FOR INTRAVENOUS MODERATE SEDATION by Dr. Samuel Y. Toong A thesis submitted in conformity with the requirements for the degree of Master
A SYSTEMATIC REVIEW ON THE USE OF DEXMEDETOMIDINE AS A SOLE AGENT FOR INTRAVENOUS MODERATE SEDATION by Dr. Samuel Y. Toong A thesis submitted in conformity with the requirements for the degree of Master
Over the past 10 years, there has been an increase in
 Dexmedetomidine for Sedation During Noninvasive Ventilation in Pediatric Patients Rasika Venkatraman, MD 1 ; James L. Hungerford, MD 2,3 ; Mark W. Hall, MD 1 ; Melissa Moore-Clingenpeel, MS 1,4 ; Joseph
Dexmedetomidine for Sedation During Noninvasive Ventilation in Pediatric Patients Rasika Venkatraman, MD 1 ; James L. Hungerford, MD 2,3 ; Mark W. Hall, MD 1 ; Melissa Moore-Clingenpeel, MS 1,4 ; Joseph
Dexmedetomidine and its Injectable Anesthetic-Pain Management Combinations
 Back to Anesthesia/Pain Management Back to Table of Contents Front Page : Library : ACVC 2009 : Anesthesia/Pain Management : Dexmedetomidine Dexmedetomidine and its Injectable Anesthetic-Pain Management
Back to Anesthesia/Pain Management Back to Table of Contents Front Page : Library : ACVC 2009 : Anesthesia/Pain Management : Dexmedetomidine Dexmedetomidine and its Injectable Anesthetic-Pain Management
Suitability of Antibiotic Treatment for CAP (CAPTIME) The duration of antibiotic treatment in community acquired pneumonia (CAP)
 STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
Neonates and infants undergoing radiological imaging
 Dexmedetomidine for Pediatric Sedation for Computed Tomography Imaging Studies Keira P. Mason, MD* Steven E. Zgleszewski, MD* Jennifer L. Dearden, MD* Raymond S. Dumont, MD* Michele A. Pirich, RN, BSN
Dexmedetomidine for Pediatric Sedation for Computed Tomography Imaging Studies Keira P. Mason, MD* Steven E. Zgleszewski, MD* Jennifer L. Dearden, MD* Raymond S. Dumont, MD* Michele A. Pirich, RN, BSN
Associate Professor, Department of Anaesthesiology, Rangaraya Medical College, Kakinada, East Godavari, Andhra Pradesh, India, 2
 Original Article Print ISSN: 3-6379 Online ISSN: 3-595X DOI: 0.7354/ijss/07/47 Bolus Doses of Ketofol versus Dexmedetomidine for the Prevention of Emergence Agitation in Children: A Prospective Randomized
Original Article Print ISSN: 3-6379 Online ISSN: 3-595X DOI: 0.7354/ijss/07/47 Bolus Doses of Ketofol versus Dexmedetomidine for the Prevention of Emergence Agitation in Children: A Prospective Randomized
Original Article INTRODUCTION. Abstract
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/305 Comparison between 0.5 µg/kg Dexmedetomidine with 0.5% Lignocaine and 0.5% Lignocaine Alone in Intravenous for
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/305 Comparison between 0.5 µg/kg Dexmedetomidine with 0.5% Lignocaine and 0.5% Lignocaine Alone in Intravenous for
Effective dose of dexmedetomidine to induce adequate sedation in elderly patients under spinal anesthesia
 KJA Korean Journal of Anesthesiology Clinical Research Article pissn 2005-6419 eissn 2005-7563 Effective dose of dexmedetomidine to induce adequate sedation in elderly patients under spinal anesthesia
KJA Korean Journal of Anesthesiology Clinical Research Article pissn 2005-6419 eissn 2005-7563 Effective dose of dexmedetomidine to induce adequate sedation in elderly patients under spinal anesthesia
Study of Dexmedetomidine as intramuscular premedication in outpatient cataract surgery: A placebo controlled study
 Original Research Article Study of Dexmedetomidine as intramuscular premedication in outpatient cataract surgery: A placebo controlled study D. Srinivasa Naik 1, K. Ravi Kumar 1, Surendra Babu 2, R. Pandu
Original Research Article Study of Dexmedetomidine as intramuscular premedication in outpatient cataract surgery: A placebo controlled study D. Srinivasa Naik 1, K. Ravi Kumar 1, Surendra Babu 2, R. Pandu
Dexmedetomidine Versus Midazolam for the Sedation of Patients with Non-invasive Ventilation Failure
 ORIGINAL ARTICLE Dexmedetomidine Versus Midazolam for the Sedation of Patients with Non-invasive Ventilation Failure Zhao Huang, Yu-sheng Chen, Zi-li Yang and Ji-yun Liu Abstract Objective To compare the
ORIGINAL ARTICLE Dexmedetomidine Versus Midazolam for the Sedation of Patients with Non-invasive Ventilation Failure Zhao Huang, Yu-sheng Chen, Zi-li Yang and Ji-yun Liu Abstract Objective To compare the
Comparison of two doses of intranasal dexmedetomidine as premedication in children
 Comparison of two doses of intranasal dexmedetomidine as premedication in children V. Pavithra, M. N. Ramani, S. K. Shah Department of Anaesthesia, B. J. Medical College, Civil Hospital, Ahmedabad, Gujarat,
Comparison of two doses of intranasal dexmedetomidine as premedication in children V. Pavithra, M. N. Ramani, S. K. Shah Department of Anaesthesia, B. J. Medical College, Civil Hospital, Ahmedabad, Gujarat,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Intravenous Dexmedetomidine Premedication on Spinal Anaesthesia with Hyperbaric Bupivacaine
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Intravenous Dexmedetomidine Premedication on Spinal Anaesthesia with Hyperbaric Bupivacaine
Intraoperative Sedation During Epidural Anesthesia: Dexmedetomidine Vs Midazolam
 ISPUB.COM The Internet Journal of Anesthesiology Volume 17 Number 2 Intraoperative Sedation During Epidural Anesthesia: Dexmedetomidine Vs Midazolam M Celik, N Koltka, B Cevik, H Baba Citation M Celik,
ISPUB.COM The Internet Journal of Anesthesiology Volume 17 Number 2 Intraoperative Sedation During Epidural Anesthesia: Dexmedetomidine Vs Midazolam M Celik, N Koltka, B Cevik, H Baba Citation M Celik,
A comparison of dexmedetomidine and midazolam for sedation in third molar surgery*
 doi:10.1111/j.1365-2044.2007.05230.x A comparison of dexmedetomidine and midazolam for sedation in third molar surgery* C. W. Cheung, 1 C. L. A. Ying, 2 W. K. Chiu, 3 G. T. C. Wong, 1 K. F. J. Ng 4 and
doi:10.1111/j.1365-2044.2007.05230.x A comparison of dexmedetomidine and midazolam for sedation in third molar surgery* C. W. Cheung, 1 C. L. A. Ying, 2 W. K. Chiu, 3 G. T. C. Wong, 1 K. F. J. Ng 4 and
Perioperative Pain Management in Veterinary Patients
 Perioperative Pain Management in Veterinary Patients Doris H. Dyson, DVM, DVSc KEYWORDS Analgesia Surgical pain Dog Cat As veterinarians in the twenty-first century, we have an ethical responsibility to
Perioperative Pain Management in Veterinary Patients Doris H. Dyson, DVM, DVSc KEYWORDS Analgesia Surgical pain Dog Cat As veterinarians in the twenty-first century, we have an ethical responsibility to
Pharmacokinetics of dexmedetomidine infusions for sedation of postoperative patients requiring intensive care ²
 British Journal of Anaesthesia 88 (5): 669±75 (2002) Pharmacokinetics of dexmedetomidine infusions for sedation of postoperative patients requiring intensive care ² R. M. Venn 1*, M. D. Karol 2 and R.
British Journal of Anaesthesia 88 (5): 669±75 (2002) Pharmacokinetics of dexmedetomidine infusions for sedation of postoperative patients requiring intensive care ² R. M. Venn 1*, M. D. Karol 2 and R.
Dıfferent Doses Of Dexmedetomidine On Controllıng Haemodynamıc Responses To Tracheal Intubatıon
 ISPUB.COM The Internet Journal of Anesthesiology Volume 27 Number 2 Dıfferent Doses Of Dexmedetomidine On Controllıng Haemodynamıc Responses To Tracheal Intubatıon A Sa??ro?lu, M Celik, Z Orhon, S Yüzer,
ISPUB.COM The Internet Journal of Anesthesiology Volume 27 Number 2 Dıfferent Doses Of Dexmedetomidine On Controllıng Haemodynamıc Responses To Tracheal Intubatıon A Sa??ro?lu, M Celik, Z Orhon, S Yüzer,
Pain Management in Racing Greyhounds
 Pain Management in Racing Greyhounds Pain Pain is a syndrome consisting of multiple organ system responses, and if left untreated will contribute to patient morbidity and mortality. Greyhounds incur a
Pain Management in Racing Greyhounds Pain Pain is a syndrome consisting of multiple organ system responses, and if left untreated will contribute to patient morbidity and mortality. Greyhounds incur a
Dr. PratekKoolwal, Dr.BribalBaj, DrKashif M Madani, Dr.MohitSomani, Dr. Vijay Mathur.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 14, Issue 7 Ver. VIII (July. 215), PP 84-9 www.iosrjournals.org "Dose related prolongation of hyperbaric
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 14, Issue 7 Ver. VIII (July. 215), PP 84-9 www.iosrjournals.org "Dose related prolongation of hyperbaric
Effects of Dexmedetomidine on Serum Interleukin-6, Hemodynamic Stability, and Postoperative Pain Relief in Elderly Patients under Spinal Anesthesia
 - CopyrightC 2016 by Okayama University Medical School. Original Article http ://escholarship.lib.okayama-u.ac.jp/amo/ Effects of Dexmedetomidine on Serum Interleukin-6, Hemodynamic Stability, and Postoperative
- CopyrightC 2016 by Okayama University Medical School. Original Article http ://escholarship.lib.okayama-u.ac.jp/amo/ Effects of Dexmedetomidine on Serum Interleukin-6, Hemodynamic Stability, and Postoperative
TITLE: Dexmedetomidine for Sedation in the ICU or PICU: A Review of Cost- Effectiveness and Guidelines
 TITLE: Dexmedetomidine for Sedation in the ICU or PICU: A Review of Cost- Effectiveness and Guidelines DATE: 17 December 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential for ICU
TITLE: Dexmedetomidine for Sedation in the ICU or PICU: A Review of Cost- Effectiveness and Guidelines DATE: 17 December 2014 CONTEXT AND POLICY ISSUES Sedation of ICU patients is often essential for ICU
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Veterinary Anaesthesia and Critical Care Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
A Comparative Evaluation of Intranasal Dexmedetomidine and Intranasal Midazolam for Premedication in Pediatric Surgery
 Original Research Article A Comparative Evaluation of Intranasal Dexmedetomidine and Intranasal Midazolam for Premedication in Pediatric Surgery Dr. Shweta Nitturi 1*, Dr. Olvyna D souza 2 1 ICU Junior
Original Research Article A Comparative Evaluation of Intranasal Dexmedetomidine and Intranasal Midazolam for Premedication in Pediatric Surgery Dr. Shweta Nitturi 1*, Dr. Olvyna D souza 2 1 ICU Junior
DISSOCIATIVE ANESTHESIA
 DISSOCIATIVE ANESTHESIA Adarsh Kumar Dissociative anesthesia implies dissociation from the surrounding with only superficial sleep mediated by interruption of neuronal transmission from unconscious to
DISSOCIATIVE ANESTHESIA Adarsh Kumar Dissociative anesthesia implies dissociation from the surrounding with only superficial sleep mediated by interruption of neuronal transmission from unconscious to
THE EFFECTS OF MIDAZOLAM AND DEXMEDETOMIDINE INFUSION ON Peri-OPERATIVE ANXIETY IN REGIONAL ANESTHESIA
 THE EFFECTS OF MIDAZOLAM AND DEXMEDETOMIDINE INFUSION ON Peri-OPERATIVE ANXIETY IN REGIONAL ANESTHESIA Elif Şenses *, Alparslan Apan **, Emıne Arzu Köse ***, Gökşen Öz *** and Hatice Rezaki **** Abstract
THE EFFECTS OF MIDAZOLAM AND DEXMEDETOMIDINE INFUSION ON Peri-OPERATIVE ANXIETY IN REGIONAL ANESTHESIA Elif Şenses *, Alparslan Apan **, Emıne Arzu Köse ***, Gökşen Öz *** and Hatice Rezaki **** Abstract
Dexmedetomidine and stress response Madhusudan et al
 Original Article: Effect of intravenous dexmedetomidine on haemodynamic responses to laryngoscopy, tracheal intubation and anaesthetic and analgesic requirements: a randomized double-blind clinical efficacy
Original Article: Effect of intravenous dexmedetomidine on haemodynamic responses to laryngoscopy, tracheal intubation and anaesthetic and analgesic requirements: a randomized double-blind clinical efficacy
Department of Intensive Care Medicine, Austin Hospital and the University of Melbourne, 145 Studley Road, Heidelberg, Victoria, 3084, Australia
 Available online http://ccforum.com/content/13/3/r75 Vol 13 No 3 Research Open Access Dexmedetomidine vs. haloperidol in delirious, agitated, intubated patients: a randomised open-label trial Michael C
Available online http://ccforum.com/content/13/3/r75 Vol 13 No 3 Research Open Access Dexmedetomidine vs. haloperidol in delirious, agitated, intubated patients: a randomised open-label trial Michael C
Mouse Formulary. The maximum recommended volume of a drug given depends on the route of administration (Formulary for Laboratory Animals, 3 rd ed.
 Mouse Formulary The maximum recommended volume of a drug given depends on the route of administration (Formulary for Laboratory Animals, 3 rd ed.): Intraperitoneal (IP) doses should not exceed 80 ml/kg
Mouse Formulary The maximum recommended volume of a drug given depends on the route of administration (Formulary for Laboratory Animals, 3 rd ed.): Intraperitoneal (IP) doses should not exceed 80 ml/kg
Dexmedetomidine use in a pediatric cardiac intensive care unit: Can we use it in infants after cardiac surgery?
 Cardiac Intensive Care Dexmedetomidine use in a pediatric cardiac intensive care unit: Can we use it in infants after cardiac surgery? Constantinos Chrysostomou, MD; Joan Sanchez De Toledo, MD; Tracy Avolio,
Cardiac Intensive Care Dexmedetomidine use in a pediatric cardiac intensive care unit: Can we use it in infants after cardiac surgery? Constantinos Chrysostomou, MD; Joan Sanchez De Toledo, MD; Tracy Avolio,
Australian and New Zealand College of Veterinary Scientists. Fellowship Examination. Veterinary Anaesthesia and Critical Care Paper 1
 Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2016 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours
Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2016 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours
EPAR type II variation for Metacam
 23 June 2011 EMA/674662/2011 International Non-proprietary Name: Meloxicam Procedure No. EMEA/V/C/033/II/084 EU/2/97/004/026, 33-34 Scope: Type II Addition of indication for cats Page 1/6 Table of contents
23 June 2011 EMA/674662/2011 International Non-proprietary Name: Meloxicam Procedure No. EMEA/V/C/033/II/084 EU/2/97/004/026, 33-34 Scope: Type II Addition of indication for cats Page 1/6 Table of contents
Evaluation of efficacy of sedative and analgesic effects of single IV dose of dexmedetomidine in post-operative patients
 www.ijpcs.net ABSTRACT Evaluation of efficacy of sedative and analgesic effects of single IV dose of dexmedetomidine in post-operative patients Manasa CR 1 *, Padma L 2, Shivshankar 3, Ranjani Ramanujam
www.ijpcs.net ABSTRACT Evaluation of efficacy of sedative and analgesic effects of single IV dose of dexmedetomidine in post-operative patients Manasa CR 1 *, Padma L 2, Shivshankar 3, Ranjani Ramanujam
The demand for sedation outside of the operating room for diagnostic or therapeutic procedures
 Focused Issue of This Month 진정요법 http://dx.doi.org/10.5124/jkma.2013.56.4.264 pissn: 1975-8456 eissn: 2093-5951 http://jkma.org 진정요법의현황 박철수 * 가톨릭대학교의과대학서울성모병원마취통증의학과 Chul Soo Park, MD* Department of Anesthesiology
Focused Issue of This Month 진정요법 http://dx.doi.org/10.5124/jkma.2013.56.4.264 pissn: 1975-8456 eissn: 2093-5951 http://jkma.org 진정요법의현황 박철수 * 가톨릭대학교의과대학서울성모병원마취통증의학과 Chul Soo Park, MD* Department of Anesthesiology
What dose of methadone should I use?
 What dose of methadone should I use? Professor Derek Flaherty BVMS, DVA, DipECVAA, MRCA, MRCVS RCVS and European Specialist in Veterinary Anaesthesia SPC dose rates for Comfortan dogs: 0.5-1.0 mg/kg SC,
What dose of methadone should I use? Professor Derek Flaherty BVMS, DVA, DipECVAA, MRCA, MRCVS RCVS and European Specialist in Veterinary Anaesthesia SPC dose rates for Comfortan dogs: 0.5-1.0 mg/kg SC,
The Addition of Dexmedetomidine as an Adjunctive Therapy to Benzodiazepine Use in Alcohol Withdrawal Syndrome
 Original Article Journal of Addictions Nursing & Volume 28 & Number 4, 188Y195 & Copyright B 2017 International Nurses Society on Addictions The Addition of Dexmedetomidine as an Adjunctive Therapy to
Original Article Journal of Addictions Nursing & Volume 28 & Number 4, 188Y195 & Copyright B 2017 International Nurses Society on Addictions The Addition of Dexmedetomidine as an Adjunctive Therapy to
Yuan Han 1,2, Liu Han 1, Mengmeng Dong 1, Qingchun Sun 1, Ke Ding 1, Zhenfeng Zhang 1, Junli Cao 1,2* and Yueying Zhang 1*
 Han et al. BMC Anesthesiology (2018) 18:12 DOI 10.1186/s12871-018-0468-x RESEARCH ARTICLE Open Access Comparison of a loading dose of dexmedetomidine combined with propofol or sevoflurane for hemodynamic
Han et al. BMC Anesthesiology (2018) 18:12 DOI 10.1186/s12871-018-0468-x RESEARCH ARTICLE Open Access Comparison of a loading dose of dexmedetomidine combined with propofol or sevoflurane for hemodynamic
Premedication with alpha-2 agonists procedures for monitoring anaesthetic
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Premedication with alpha-2 agonists procedures for monitoring anaesthetic Author : Lisa Angell, Chris Seymour Categories :
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Premedication with alpha-2 agonists procedures for monitoring anaesthetic Author : Lisa Angell, Chris Seymour Categories :
Int. J. Pharm. Sci. Rev. Res., 36(1), January February 2016; Article No. 38, Pages: *Corresponding author s
 Research Article Comparative Study Betweeen Dexmedetomidine and Remifentanyl for Efficient Pain and Ponv Management in Propofol Based Total Intravenous Anesthesia after Laparoscopic Gynaecological Surgeries
Research Article Comparative Study Betweeen Dexmedetomidine and Remifentanyl for Efficient Pain and Ponv Management in Propofol Based Total Intravenous Anesthesia after Laparoscopic Gynaecological Surgeries
Metacam. The Only NSAID Approved for Cats in the US. John G. Pantalo, VMD Professional Services Veterinarian. Think easy. Think cat. Think METACAM.
 Metacam The Only NSAID Approved for Cats in the US John G. Pantalo, VMD Professional Services Veterinarian Think easy. Think cat. Think METACAM. Today s Agenda New pain management guidelines for cats Only
Metacam The Only NSAID Approved for Cats in the US John G. Pantalo, VMD Professional Services Veterinarian Think easy. Think cat. Think METACAM. Today s Agenda New pain management guidelines for cats Only
Case Report Extended Infusion of Dexmedetomidine to an Infant at Sixty Times the Intended Rate
 International Pediatrics Volume 2010, Article ID 825079, 6 pages doi:10.1155/2010/825079 Case Report Extended Infusion of Dexmedetomidine to an Infant at Sixty Times the Intended Rate Bryan A. Max 1 and
International Pediatrics Volume 2010, Article ID 825079, 6 pages doi:10.1155/2010/825079 Case Report Extended Infusion of Dexmedetomidine to an Infant at Sixty Times the Intended Rate Bryan A. Max 1 and
S Kumar, B B Kushwaha, R Prakash, S Jafa, A Malik, R Wahal, J Aggarwal, R Kapoor
 ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 Comparative Study Of Effects Of Dexmedetomidine And Clonidine Premedication In Perioperative Hemodynamic Stability And Postoperative
ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 Comparative Study Of Effects Of Dexmedetomidine And Clonidine Premedication In Perioperative Hemodynamic Stability And Postoperative
Comparison of dexmedetomidine v/s propofol used as adjuvant with combined spinal epidural anaesthesia for joint replacement surgeries
 Comparison of dexmedetomidine v/s propofol used as adjuvant with combined spinal epidural anaesthesia for joint replacement surgeries Kuldeep Chittora 1 *; Ritu Sharma 2 ; Rajeev LochanTiwari 3 1 Department
Comparison of dexmedetomidine v/s propofol used as adjuvant with combined spinal epidural anaesthesia for joint replacement surgeries Kuldeep Chittora 1 *; Ritu Sharma 2 ; Rajeev LochanTiwari 3 1 Department
Efficacy of dexmedetomidine in reducing postoperative morphine consumption in patients undergoing total abdominal hysterectomy
 Original Article Brunei Int Med J. 2016; 12 (3): 97-103 Efficacy of dexmedetomidine in reducing postoperative morphine consumption in patients undergoing total abdominal hysterectomy Mazlilah ABDUL MALEK
Original Article Brunei Int Med J. 2016; 12 (3): 97-103 Efficacy of dexmedetomidine in reducing postoperative morphine consumption in patients undergoing total abdominal hysterectomy Mazlilah ABDUL MALEK
Original Article Dose-dependent effects of dexmedetomidine during one-lung ventilation in patients undergoing lobectomy
 Int J Clin Exp Med 2017;10(3):5216-5221 www.ijcem.com /ISSN:1940-5901/IJCEM0012317 Original Article Dose-dependent effects of dexmedetomidine during one-lung ventilation in patients undergoing lobectomy
Int J Clin Exp Med 2017;10(3):5216-5221 www.ijcem.com /ISSN:1940-5901/IJCEM0012317 Original Article Dose-dependent effects of dexmedetomidine during one-lung ventilation in patients undergoing lobectomy
COMPARATIVE STUDY OF INTRAVENOUS DEXMEDETOMIDINE PLUS INTRATHECAL BUPIVACAINE VS INTRATHECAL BUPIVACAINE ALONE FOR PROLONGATION OF SPINAL ANALGESIA
 COMPARATIVE STUDY OF INTRAVENOUS DEXMEDETOMIDINE PLUS INTRATHECAL BUPIVACAINE VS INTRATHECAL BUPIVACAINE ALONE FOR PROLONGATION OF SPINAL ANALGESIA H. L. Rani 1, I. Upendranath 2 1Associate Professor,
COMPARATIVE STUDY OF INTRAVENOUS DEXMEDETOMIDINE PLUS INTRATHECAL BUPIVACAINE VS INTRATHECAL BUPIVACAINE ALONE FOR PROLONGATION OF SPINAL ANALGESIA H. L. Rani 1, I. Upendranath 2 1Associate Professor,
12/3/14. Top 10 Tips You Need to Know About for Anesthesia & Analgesia. Sponsorship. Introduction. VETgirl on the RUN!
 Top 10 Tips You Need to Know About for Anesthesia & Analgesia Sponsorship Introduction Introduction Introduction VETgirl on the RUN! 1 Subscription plans Download our podcasts on itunes! Find us on social
Top 10 Tips You Need to Know About for Anesthesia & Analgesia Sponsorship Introduction Introduction Introduction VETgirl on the RUN! 1 Subscription plans Download our podcasts on itunes! Find us on social
Procedure # IBT IACUC Approval: December 11, 2017
 IACUC Procedure: Anesthetics and Analgesics Procedure # IBT-222.04 IACUC Approval: December 11, 2017 Purpose: The purpose is to define the anesthetics and analgesics that may be used in mice and rats.
IACUC Procedure: Anesthetics and Analgesics Procedure # IBT-222.04 IACUC Approval: December 11, 2017 Purpose: The purpose is to define the anesthetics and analgesics that may be used in mice and rats.
EXOTIC SMALL MAMMAL ANESTHETIC TECHNIQUES
 EXOTIC SMALL MAMMAL ANESTHETIC TECHNIQUES Jody Nugent-Deal, RVT, VTS (Anesthesia) and (Clinical Practice Exotic Companion Animal) Veterinary Medical Teaching Hospital University of California, Davis, CA
EXOTIC SMALL MAMMAL ANESTHETIC TECHNIQUES Jody Nugent-Deal, RVT, VTS (Anesthesia) and (Clinical Practice Exotic Companion Animal) Veterinary Medical Teaching Hospital University of California, Davis, CA
Highly variable pharmacokinetics of dexmedetomidine during intensive care: a case report
 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Highly variable pharmacokinetics of dexmedetomidine during intensive care: a case report Timo Iirola 1*, Ruut Laitio 1, Erkki Kentala 1, Riku Aantaa
JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Highly variable pharmacokinetics of dexmedetomidine during intensive care: a case report Timo Iirola 1*, Ruut Laitio 1, Erkki Kentala 1, Riku Aantaa
POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014
 POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014 The U.S.D.A Animal Welfare Act (9 CFR) requires use of aseptic
POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014 The U.S.D.A Animal Welfare Act (9 CFR) requires use of aseptic
A randomized control study of dexmedetomidine versus fentanyl as an anesthetic adjuvant in supratentorial craniotomies
 ORIGINAL ARTICLE ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com A randomized control study of dexmedetomidine versus fentanyl as an anesthetic adjuvant in supratentorial craniotomies Amrita Gupta,
ORIGINAL ARTICLE ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com A randomized control study of dexmedetomidine versus fentanyl as an anesthetic adjuvant in supratentorial craniotomies Amrita Gupta,
Critical appraisal Randomised controlled trial questions
 Critical appraisal Randomised controlled trial questions Korpivaara, M., Laapas, K., Huhtinen, M., Schoning, B., Overall, K. (2017) Dexmedetomidine oromucosal gel for noise-associated acute anxiety and
Critical appraisal Randomised controlled trial questions Korpivaara, M., Laapas, K., Huhtinen, M., Schoning, B., Overall, K. (2017) Dexmedetomidine oromucosal gel for noise-associated acute anxiety and
