Case 1 and Case 2. Case 1 3/23/2016
|
|
|
- Linette Townsend
- 5 years ago
- Views:
Transcription
1 Case 1 and Deidra D. Parrish, MD, MPH&TM Nashville Metro Public Health Dept TB Symposium March 30, 2016 Case 1 27 yo Indian woman came to the US to join her husband three months prior to clinic visit. She initially saw an ob/gyn for an infertility workup and was found to have mild hypothyroidism and a 2 cm X 3 cm lymph node was palpated in the right neck. Pt referred for a lymph node biopsy which showed necrotic debris on path, and a positive AFB smear. Case 1 On evaluation in TB clinic, pt denied cough, fever or night sweats. Denied previous history of TB, but reported lymph node enlargement after an episode of typhoid fever a year before. Reports taking daily meds for the lymph node enlargements for one year, with serial monitoring by CT. During treatment pt gained about 4kg and noted neck nodes enlarged while on treatment. 1
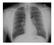
2 PMH/PSH unremarkable Case 1 PE: Well appearing young woman with multiple enlarged, firm anterior cervical nodes bilaterally; PE otherwise negative CXR normal A Google search of the names of the medications she took for a year reveal them to be Isoniazid, Rifampin and Ethambutol Case 1: CT imaging Case 1 Chest CT negative for intrathoracic lymphademopathy or lung parenchymal abnormalities Induced sputums AFB smear negative X 3 HIV negative CBC with slightly low Hgb, normal CMP, slightly elevated TSH with normal free T4 Pt started on RIF 600, INH 300, PZA 1500, EMB 1200 and vit B6 50 2
3 Case 1 After nearly six weeks, M. tb cultures grew from both the lymph node and the initial induced sputum. Resistant to RIF, INH, PZA, EMB and Streptomycin TB meds held and samples sent for MDDR Case 1 In addition to mutations for the first line drugs, a gyra mutation encoding quinolone resistance was detected. No mutations associated with the injectables were detected. Case 1: PreXDR DEFINITIONS Multidrug resistant (MDR) refers to TB caused by Mycobacterium tuberculosis (M. tuberculosis) that is resistant to at least isoniazid (INH) and rifampin (RIF). Pre extensively drug resistant (Pre XDR) refers to MDR TB that is also resistant to either a fluoroquinolone or a second line injectable anti TB drug (kanamycin, capreomycin, or amikacin), but not both. Extensively drug resistant (XDR) refers to MDR TB that is also resistant to both a fluoroquinolone and a secondline injectable anti TB drug. 3
4 Case 1: Pre XDR What are our treatment options? RIF, INH, PZA, EMB, Streptomycin Moxifloxacin Kanamycin/Capreomycin/Amikacin Ethionamide Para aminosalicylate (PAS) Cycloserine Linezolid Clofazimine Carbapenems Amox/Clav, Clarithromycin Bedaquiline QT Prolongation Bedaquiline, Moxifloxacin and Clofazamine all are known to prolong the QT interval, which increases the risk of torsade de pointes. EKG monitoring recommended if treating with bedaquiline plus another drug that prolongs QT No consensus guidelines on the concomittant use of bedaquiline along with moxifloxacin and/or clofazimine Case 1: Pre XDR Pt hospitalized for PICC placement and initiated on DR TB medication regimen: Amikacin 550mg IV qd Bedaquilline 400mg po qd Cycloserine 250mg po bid Para aminosalicylate 4g po bid Clofazimine 200mg po qd Vit B6 100mg po qd 4
5 Clofazimine tx in DR TB Originally developed for TB treatment in 1954; discarded in favor of better TB drugs Currently indicated for treating leprosy Mechanism of action unclear Is a component of the Bangledesh regimen A 9 month regimen shown to be effective in MDR TB treatment using 4 months of kanamycin, prothionamide and INH and 9 months of a quinolone, clofazimine and PZA Clofazimine tx in DR TB Main side effect: skin discoloration Requires investigational new drug (IND) application to FDA for use outside of leprosy Case 1: Pre XDR Final phenotypic susceptibilites confirmed resistance to first line agents and quinolones. Sensitive to Kanamycin, Amikacin, Capreomycin Ethionamide, PAS, Linezolid, Clofazimine No further sputum cultures grew after initial culture. 5
6 Case 1: Pre XDR Pt tolerated regimen well, with minor, tolerable side effects, including moderate even skin darkening and initial lymph node swelling and drainage. QTc 384 (baseline) > 462 (peak) After the 6 month intensive phase, IV amikacin and bedaquiline were discontinued. Low dose linezolid (300mg qd) was added to her continuation phase regimen of PAS, cycloserine and clofazimine. Case 1: Pre XDR After one year on TB meds, pt came in to clinic for a sick visit reporting intermittent abdominal cramps X 10 days. Pt noted clumps of blood when she urinates. No dysuria, normal BMs. LMP was 3 weeks prior. Exam was negative for abdominal tenderness, organomegaly or CVA tenderness. Urine pregnancy test negative, UA trace blood Case 1: Pre XDR Holding clofazimine for two weeks did not improve symptoms. CT abdomen to check for nephrolithiasis revealed no evidence of stones, hydronephrosis or hydroureter. Fat containing masses, likely dermoids, seen in adnexa bilaterally. Upon consultation with SNTC, etiology determined to be hormonal disruption due to PAS. 6
7 Case 1: Pre XDR Followed up with GYN and started OCPs with resolution of symptoms. Pt completed 18 months of therapy with resolution of palpable lymphadenopathy. Will follow up q6 months for two years to evaluate for relapse. 47 yo Nigerian woman came to Nashville to visit family. Within two days, was seen in a clinic for hearing issues, and endorsed wet cough for a couple of weeks with inability to bring up sputum. Also reported night sweats, fatigue and weight loss of an unknown amount. Was treated with Z pack and told to go to the TB clinic. Chest X ray obtained. 7
8 Upon further questioning, the patient admitted to having been treated for TB on two occasions: in 2011 for eight months and in late 2014 for one month, after which she developed hearing loss and discontinued treatment. PMH: DM2 PE: Thin woman, NAD, no palpable LAD, decreased BS in R base Sputums and labs obtained Induced sputum: AFB smear POS (10+) GeneXpert: M.tb DNA Detected rpob mutation Detected HIV negative Normal CBC; creatinine 1.52 (egfr 47); Hep panel Neg; Normal LFTs, Normal TSH, Hgb A1c 7.8 8
9 How to treat? Considerations: Diabetes Renal insufficiency Hearing loss INH??? Pt hospitalized to initiate DR TB regimen of: Amikacin IV at 10 15mg/kg Moxifloxacin 400mg qd EMB 1200mg qd PAS 4g bid INH 300mg qd Peaks and troughs of AMK obtained and titrated in hospital. Peaks up to 45 initially (goal in 20s 30s) Changed to q48h dosing Creatinine rose to 2.2 Pt developed significant nausea, vomitting and diarrhea 9
10 Transaminases normal. PAS discontinued due to GI side effects. Linezolid 600mg po qd started. Pt discharged to home on AMK 650mg IV q48h, moxifloxacin, EMB, INH and linezolid Within one week of discharge, pt developed acute on chronic renal failure with a peak creatinine of 5.8 Amikacin discontinued. All meds held. After supportive treatment and rehydration, pt s creatinine returned to baseline of 1.69 after several days. Phenotypic susceptibilities resulted. 10
11 Additional susceptibilites from National Jewish Sensitive to Linezolid and Cycloserine EKG QTc 442 Pt restarted on DR TB treatment with: Bedaquiline 400mg qd X 2 weeks, then 200mg q M,W,F Moxifloxacin 400mg qd Linezolid 600mg qd Cycloserine 250mg bid Ethionamide 250mg bid Vit B6 150mg po qd Pt tolerated new regimen with symptomatic treatment for nausea. LFTs normal, Cell counts stable QTc 420s 460s Sputum cultures converted to negative at one month of initial treatment. 11
12 At about month 5 of DR TB treatment, pt experienced abrupt onset of witnessed visual hallucinations. Cycloserine was held with rapid resolution of psychotic symptoms. After consultation and discussion with patient and family, cycloserine restarted at lower dose (250mg po qd). Pt is tolerating it without issues. 12
13 Pt currently on continuation phase therapy with Moxifloxacin 400mg qd, Cycloserine 250mg qd, Linezolid 600mg qd and Ethionamide 250mg bid Vit B6 150mg qd Has completed 11 of 18 months of MDR TB treatment. Acknowledgements Staff of MPHD TB Elimination Program (especially case management and outreach) Drs. Tim Sterling, Jon Warkentin, Dave Ashkin and Connie Haley My patients and their families Selected References Francis J. Curry National Tuberculosis Center and California Department of Public Health, 2008: Drug Resistant Tuberculosis: A Survival Guide for Clinicians, Third Edition Hwang et al. Safety and availability of clofazimine in the treatment of multidrug and extensively drugresistant tuberculosis: analysis of published guidance and meta analysis of cohort studies. BMJ Open. 2014;4:e Yoo, JW et al. Clinical experience of using clofazimine to treat multidrug resistant tuberculosis. Int J Tuberc Lung Dis Sep;17(9):
14 Moises A. Huaman, MD MSc University of Kentucky Nashville TB Symposium March 30, year old Male from Mexico with hypertension, diabetes, prior deep venous thrombosis, left below knee amputation, blind left eye, kidney transplant in 2000 Chronic CellCept and prednisone 5 mg daily History of pulmonary TB ~20 years prior treated in Mexico Baseline creatinine 2 mg/dl, albumin 2 g/dl, A1c 9.8%, HIV negative The patient visited the US in 2014 and was diagnosed with pulmonary TB (MTB rifampin resistance and low level isoniazid resistance) and T11 T12 Pott s disease Consultation with SNTC Final TB regimen included isoniazid 900 mg 2X/week, linezolid 300 mg po qdaily, moxifloxacin 400 mg po qdaily and pyrazinamide 1,500 mg po qdaily Plan for 18 months of TB treatment 14
15 TB treatment stopped in Mexico at 4 months Six months later pt developed worsening back pain and decided to come back to the US MRI: worsening T11 T12 Pott s disease with paraspinal phlegmon, mild cord compression Neuro exam without focal deficit Neurosurgery said no surgical intervention IR guided biopsy was performed Consultation with SNTC Restarted isoniazid, moxifloxacin, linezolid and pyrazinamide T11 T12 smear positive, culture grew MTB with same susceptibility pattern as 2014 sputum MTB isolate Discharged on same TB meds and brace 8/2015: MDR Pseudomonas UTI & septicemia 1/2016 (6 months TB treatment): worsening back pain and new onset leg weakness MRI: worsening T11 T12 kyphosis, progression of T12 fracture, edema and cord compression 15
16 TB medications continued Neurosurgery decided to offer spinal decompression and stabilization to protect neurologic function Surgery was performed without immediate major complications, patient was extubated next day, left chest tube placed Vertebral tissue & bone AFB stain negative Vertebral bone MTB PCR positive Spinal tissue & bone cultures finalized negative at 6 weeks Patient developed multiple complications after post operative day 5 ESBL E. coli pneumonia /aspiration MDR Pseudomonas pneumonia x 2 NSTEMI Prolonged respiratory failure requiring trach Graft failure requiring renal replacement therapy Multifactorial shock (septic, cardiogenic, adrenal) After 6 weeks in the ICU the patient expired 16
17 Acknowledgements Kentucky TB Prevention & Control Program UK SNTC CDC Patient and family 17
TB Grand Rounds. MDR-TB: Management of Adverse Drug Reactions. Reynard J. McDonald, M.D. September 18, Patient History
 TB Grand Rounds MDR-TB: Management of Adverse Drug Reactions Reynard J. McDonald, M.D. September 18, 2007 Patient History This 30 y/o H/M was born in Ecuador and immigrated to the US in 2001 On 11-22-05
TB Grand Rounds MDR-TB: Management of Adverse Drug Reactions Reynard J. McDonald, M.D. September 18, 2007 Patient History This 30 y/o H/M was born in Ecuador and immigrated to the US in 2001 On 11-22-05
MDR TB AND CASE STUDIES
 MDR TB AND CASE STUDIES Chris Keh, MD Director, TB Prevention and Control Program, SFDPH HS Assistant Clinical Professor, Infectious Diseases, UCSF Seattle, CITC Clinical Intensive June 15, 2018 Slide
MDR TB AND CASE STUDIES Chris Keh, MD Director, TB Prevention and Control Program, SFDPH HS Assistant Clinical Professor, Infectious Diseases, UCSF Seattle, CITC Clinical Intensive June 15, 2018 Slide
Clinical Management : DR-TB
 Clinical Management : DR-TB Charoen Chuchottaworn MD., Senior Medical Advisor, Central Chest Institute of Thailand, Department of Medical Services, MoPH. Tuberculosis Classification Drug susceptible TB
Clinical Management : DR-TB Charoen Chuchottaworn MD., Senior Medical Advisor, Central Chest Institute of Thailand, Department of Medical Services, MoPH. Tuberculosis Classification Drug susceptible TB
Treatment of Drug Resistant TB
 Treatment of Drug Resistant TB Diana M. Nilsen RN, MD Bureau of TB Control New York City Department of Health & Mental Hygiene Objectives Definition of other drug resistant (ODR), multiple drug resistant
Treatment of Drug Resistant TB Diana M. Nilsen RN, MD Bureau of TB Control New York City Department of Health & Mental Hygiene Objectives Definition of other drug resistant (ODR), multiple drug resistant
DR-TB PATIENT IDENTITY CARD
 Ministry of Health Community Development Gender Elderly and Children National Tuberculosis and Leprosy Programme DR-TB 02 DR-TB Treatment Unit: DR-TB PATIENT IDENTITY CARD DR-TB Reg. Number: Date of registration:
Ministry of Health Community Development Gender Elderly and Children National Tuberculosis and Leprosy Programme DR-TB 02 DR-TB Treatment Unit: DR-TB PATIENT IDENTITY CARD DR-TB Reg. Number: Date of registration:
Multidrug-resistant Tuberculosis. Charles L. Daley, MD National Jewish Health Chair, Global GLC, WHO and Stop TB Partnership
 Multidrug-resistant Tuberculosis Charles L. Daley, MD National Jewish Health Chair, Global GLC, WHO and Stop TB Partnership Disclosures World Health Organization Chair, Global GLC Otsuka Chair, Data Monitoring
Multidrug-resistant Tuberculosis Charles L. Daley, MD National Jewish Health Chair, Global GLC, WHO and Stop TB Partnership Disclosures World Health Organization Chair, Global GLC Otsuka Chair, Data Monitoring
Challenges to treat MDR TB
 Challenges to treat MDR TB Manfred Danilovits Tartu University Hospital, Estonian NTP Program 2nd European Advanced Course in Clinical Tuberculosis 22-24 September 2014, Amsterdam MDR-TB control; WHO Europe,
Challenges to treat MDR TB Manfred Danilovits Tartu University Hospital, Estonian NTP Program 2nd European Advanced Course in Clinical Tuberculosis 22-24 September 2014, Amsterdam MDR-TB control; WHO Europe,
Multi-Drug and Extensively Drug Resistant Tuberculosis
 Multi-Drug and Extensively Drug Resistant Tuberculosis Gwen A. Huitt, M.D., M.S. Professor, Department of Medicine Director, Adult Infectious Disease Care Unit National Jewish Health Disclosures None Tuberculosis
Multi-Drug and Extensively Drug Resistant Tuberculosis Gwen A. Huitt, M.D., M.S. Professor, Department of Medicine Director, Adult Infectious Disease Care Unit National Jewish Health Disclosures None Tuberculosis
TB Intensive San Antonio, Texas
 TB Intensive San Antonio, Texas April 6-8, 2011 Drug Resistant TB Barbara Seaworth, MD Thursday April 7, 2011 Barbara Seaworth, MD has the following disclosures to make: Has received research funding from
TB Intensive San Antonio, Texas April 6-8, 2011 Drug Resistant TB Barbara Seaworth, MD Thursday April 7, 2011 Barbara Seaworth, MD has the following disclosures to make: Has received research funding from
MDR/XDR TB. Barbara Seaworth, MD, FIDSA, FACP October 27, TB Intensive October 24 27, 2017 San Antonio, TX
 MDR/XDR TB Barbara Seaworth, MD, FIDSA, FACP October 27, 2017 TB Intensive October 24 27, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Barbara Seaworth, MD, FIDSA, FACP, has the following disclosures
MDR/XDR TB Barbara Seaworth, MD, FIDSA, FACP October 27, 2017 TB Intensive October 24 27, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Barbara Seaworth, MD, FIDSA, FACP, has the following disclosures
TB Intensive Houston, Texas. Multi-Drug Resistant (MDR) TB Barbara Seaworth, MD
 TB Intensive Houston, Texas November 10-12, 12 2009 Multi-Drug Resistant (MDR) TB Barbara Seaworth, MD November 12, 2009 Multi-Drug Resistant (MDR) TB Updates November 12, 2009 Barbara J. Seaworth Professor
TB Intensive Houston, Texas November 10-12, 12 2009 Multi-Drug Resistant (MDR) TB Barbara Seaworth, MD November 12, 2009 Multi-Drug Resistant (MDR) TB Updates November 12, 2009 Barbara J. Seaworth Professor
Practical. Walk through New Survival Guide
 Many faces of TB: Drug resistant it ttbs Survival lgid Guide v3 P B L Ch G Sh t L T P. Barry, L. Chen, G. Schecter, L. True Curry International TB Center/CTCA April 20, 2016 Real case Practical Walk through
Many faces of TB: Drug resistant it ttbs Survival lgid Guide v3 P B L Ch G Sh t L T P. Barry, L. Chen, G. Schecter, L. True Curry International TB Center/CTCA April 20, 2016 Real case Practical Walk through
THE NEW DR-TB NATIONAL POLICY AND STATE OF IMPLEMENTATION
 1 THE NEW DR-TB NATIONAL POLICY AND STATE OF IMPLEMENTATION Dr. Norbert Ndjeka MD, DHSM (Wits), MMed(Fam Med) (MED), Dip HIV Man (SA) Director Drug-Resistant TB, TB and HIV National Department of Health
1 THE NEW DR-TB NATIONAL POLICY AND STATE OF IMPLEMENTATION Dr. Norbert Ndjeka MD, DHSM (Wits), MMed(Fam Med) (MED), Dip HIV Man (SA) Director Drug-Resistant TB, TB and HIV National Department of Health
Strategies for Successful Treatment of Drug Resistant Tuberculosis in the U.S.
 Strategies for Successful Treatment of Drug Resistant Tuberculosis in the U.S. Barbara J. Seaworth, M.D. Professor of Medicine University of Texas Health Science Center, Tyler Medical Director, Heartland
Strategies for Successful Treatment of Drug Resistant Tuberculosis in the U.S. Barbara J. Seaworth, M.D. Professor of Medicine University of Texas Health Science Center, Tyler Medical Director, Heartland
Treatment of Multidrug-resistant Tuberculosis (MDR-TB)
 Treatment of Multidrug-resistant Tuberculosis (MDR-TB) 2006 2008 2011 2013 2014 2016 2019 Charles L. Daley, MD National Jewish Health University of Colorado Disclosures Research grant Insmed: Phase II
Treatment of Multidrug-resistant Tuberculosis (MDR-TB) 2006 2008 2011 2013 2014 2016 2019 Charles L. Daley, MD National Jewish Health University of Colorado Disclosures Research grant Insmed: Phase II
Drug-resistant TB therapy: the future is now
 Drug-resistant TB therapy: the future is now Gary Maartens Thanks to Francesca Conradie for sharing slides Division of Clinical Pharmacology UNIVERSITY OF CAPE TOWN IYUNIVESITHI YASEKAPA UNIVERSITEIT VAN
Drug-resistant TB therapy: the future is now Gary Maartens Thanks to Francesca Conradie for sharing slides Division of Clinical Pharmacology UNIVERSITY OF CAPE TOWN IYUNIVESITHI YASEKAPA UNIVERSITEIT VAN
XDR TB: The Laboratory s Dilemma vs The Clinician s Dilemma
 XD TB: The Laboratory s Dilemma vs The Clinician s Dilemma Barbara J. Seaworth, MD, FIDSA, FACP, Heartland National TB Center, San Antonio, TX Kenneth Jost, Jr., M(ASCP) Laboratory Services Section, Texas
XD TB: The Laboratory s Dilemma vs The Clinician s Dilemma Barbara J. Seaworth, MD, FIDSA, FACP, Heartland National TB Center, San Antonio, TX Kenneth Jost, Jr., M(ASCP) Laboratory Services Section, Texas
TB Intensive Houston, Texas October 15-17, 2013
 TB Intensive Houston, Texas October 15-17, 2013 MDR/XDR TB Barbara J. Seaworth, MD October 16, 2013 Barbara J. Seaworth, MD has the following disclosures to make: No conflict of interests No relevant financial
TB Intensive Houston, Texas October 15-17, 2013 MDR/XDR TB Barbara J. Seaworth, MD October 16, 2013 Barbara J. Seaworth, MD has the following disclosures to make: No conflict of interests No relevant financial
MDR-TB is a manmade problem..it is costly, deadly, debilitating, and the biggest threat to our current TB control strategies 2
 1 MDR-TB is a manmade problem..it is costly, deadly, debilitating, and the biggest threat to our current TB control strategies 2 1 India has the highest TB burden in the world 3 4 2 5 M. tuberculosis Resistance
1 MDR-TB is a manmade problem..it is costly, deadly, debilitating, and the biggest threat to our current TB control strategies 2 1 India has the highest TB burden in the world 3 4 2 5 M. tuberculosis Resistance
Multidrug resistant Tuberculosis
 Multidrug resistant Tuberculosis Pennan Barry, MD, MPH California MDR TB Consult Service Surveillance and Epidemiology Section Curry International Tuberculosis Center Clinical Intensive October 018 Objectives
Multidrug resistant Tuberculosis Pennan Barry, MD, MPH California MDR TB Consult Service Surveillance and Epidemiology Section Curry International Tuberculosis Center Clinical Intensive October 018 Objectives
Dr Sharanjit Dhoot. Chelsea and Westminster Hospital, London. 18 th Annual Conference of the British HIV Association (BHIVA)
 18 th Annual Conference of the British HIV Association (BHIVA) Dr Sharanjit Dhoot Chelsea and Westminster Hospital, London 18-20 April 2012, The International Convention Centre, Birmingham 18 th Annual
18 th Annual Conference of the British HIV Association (BHIVA) Dr Sharanjit Dhoot Chelsea and Westminster Hospital, London 18-20 April 2012, The International Convention Centre, Birmingham 18 th Annual
Drug Resistant Tuberculosis:
 Drug Resistant Tuberculosis: Pearls and other Considerations John W. Wilson, MD Associate Professor of Medicine Division of Infectious Diseases Mayo Clinic, Rochester MN Mayo Clinic Center for Tuberculosis
Drug Resistant Tuberculosis: Pearls and other Considerations John W. Wilson, MD Associate Professor of Medicine Division of Infectious Diseases Mayo Clinic, Rochester MN Mayo Clinic Center for Tuberculosis
Tb : Recent recommendation. Dr.Ketan Shah
 Tb : Recent recommendation Dr.Ketan Shah Tbc : Clinician If you think It is easy to diagnose : u r not good clinician It is difficult to diagnose :U r not alone doctor to think this 6/22/2015 Ketan Shah
Tb : Recent recommendation Dr.Ketan Shah Tbc : Clinician If you think It is easy to diagnose : u r not good clinician It is difficult to diagnose :U r not alone doctor to think this 6/22/2015 Ketan Shah
Management of MDR and XDR TB Prof. Martin Boeree
 Management of MDR and XDR TB 1, MD, PhD Associate Professor Consultant Respiratory Medicine Department of Lung Diseases Radboud University Nijmegen Medical Centre TB Referral Hospital Dekkerswald Nijmegen,
Management of MDR and XDR TB 1, MD, PhD Associate Professor Consultant Respiratory Medicine Department of Lung Diseases Radboud University Nijmegen Medical Centre TB Referral Hospital Dekkerswald Nijmegen,
TB Intensive San Antonio, Texas
 TB Intensive San Antonio, Texas May 6 9, 2014 MDR/XDR TB Barbara Seaworth, MD May 9, 2014 Barbara Seaworth, MD has the following disclosures to make: No conflict of interests No relevant financial relationships
TB Intensive San Antonio, Texas May 6 9, 2014 MDR/XDR TB Barbara Seaworth, MD May 9, 2014 Barbara Seaworth, MD has the following disclosures to make: No conflict of interests No relevant financial relationships
Multidrug-resistant Tuberculosis
 Multidrug-resistant Tuberculosis Pennan Barry, MD, MPH California MDR TB Consult Service Surveillance and Epidemiology Section Curry International Tuberculosis Center Clinical Intensive September 2016
Multidrug-resistant Tuberculosis Pennan Barry, MD, MPH California MDR TB Consult Service Surveillance and Epidemiology Section Curry International Tuberculosis Center Clinical Intensive September 2016
Treatment of MDR/XDR-TB. Short course chemotherapy for MDR-TB: practical issues. CHIANG Chen-Yuan MD, MPH, DrPhilos
 Treatment of MDR/XDR-TB Short course chemotherapy for MDR-TB: practical issues CHIANG Chen-Yuan MD, MPH, DrPhilos Treatment strategies for MDR-TB Standardized treatment: drug resistance survey data from
Treatment of MDR/XDR-TB Short course chemotherapy for MDR-TB: practical issues CHIANG Chen-Yuan MD, MPH, DrPhilos Treatment strategies for MDR-TB Standardized treatment: drug resistance survey data from
Treatment for NTM: when how.and what next? Pr Claire Andréjak Respiratory and ICU Department University hospital, Amiens, France
 Treatment for NTM: when how.and what next? Pr Claire Andréjak Respiratory and ICU Department University hospital, Amiens, France First step = To diagnose NTM disease One NTM positive sample NTM disease
Treatment for NTM: when how.and what next? Pr Claire Andréjak Respiratory and ICU Department University hospital, Amiens, France First step = To diagnose NTM disease One NTM positive sample NTM disease
Subacute Adenitis. Ann M. Loeffler, MD
 Subacute Adenitis Ann M. Loeffler, MD Lymphadenitis Swelling and hyperplasia of sinusoidal lining cells Infiltration of leukocytes +/- abscess formation Granulomatous or non-granulomatous Pyogenic adenitis
Subacute Adenitis Ann M. Loeffler, MD Lymphadenitis Swelling and hyperplasia of sinusoidal lining cells Infiltration of leukocytes +/- abscess formation Granulomatous or non-granulomatous Pyogenic adenitis
Summary of outcomes from WHO Expert Group Meeting on Drug Susceptibility Testing - PRELIMINARY -
 Summary of outcomes from WHO Expert Group Meeting on Drug Susceptibility Testing PRELIMINARY 4 th Annual GLI meeting 17 April 2012 Fuad Mirzayev Laboratories, Diagnostics and Drug Resistance unit, Stop
Summary of outcomes from WHO Expert Group Meeting on Drug Susceptibility Testing PRELIMINARY 4 th Annual GLI meeting 17 April 2012 Fuad Mirzayev Laboratories, Diagnostics and Drug Resistance unit, Stop
CDC s Molecular Detection of Drug Resistance (MDDR) Service and Mycobacterium tuberculosis DST Model Performance Evaluation Program (MPEP)
 CDC s Molecular Detection of Drug Resistance (MDDR) Service and Mycobacterium tuberculosis DST Model Performance Evaluation Program (MPEP) Beverly Metchock, DrPH, D(ABMM) Mycobacteriology Laboratory Branch/Division
CDC s Molecular Detection of Drug Resistance (MDDR) Service and Mycobacterium tuberculosis DST Model Performance Evaluation Program (MPEP) Beverly Metchock, DrPH, D(ABMM) Mycobacteriology Laboratory Branch/Division
MDR treatment. Shanghai, May 2012 Arnaud Trébucq The Union
 MDR treatment Shanghai, May 2012 Arnaud Trébucq The Union Why to diagnose MDR-TB? Outcome of SS+ new MDR-TB cases, treated with First Line TB (FLD) drugs Setting Success Died Fail LFFU Transf. Corea 20(56)
MDR treatment Shanghai, May 2012 Arnaud Trébucq The Union Why to diagnose MDR-TB? Outcome of SS+ new MDR-TB cases, treated with First Line TB (FLD) drugs Setting Success Died Fail LFFU Transf. Corea 20(56)
TB New Drugs, Shorter Courses
 TB New Drugs, Shorter Courses Brian Chong John Hunter Hospital, Newcastle NSW Talk supervisor: Chris Coulter Disclosures Unfortunately none 1 Current Situation In 2013, Australia had: 1,263 notified TB
TB New Drugs, Shorter Courses Brian Chong John Hunter Hospital, Newcastle NSW Talk supervisor: Chris Coulter Disclosures Unfortunately none 1 Current Situation In 2013, Australia had: 1,263 notified TB
Drug resistant TB: Lisa Chen, MD University of California, San Francisco Curry Interna:onal TB Center Sea=le, June 2016
 Drug resistant TB: Lisa Chen, MD University of California, San Francisco Curry Interna:onal TB Center Sea=le, June 2016 Drug- Resistant TB: De1initions Mono- resistant: Resistance to a single drug Poly-
Drug resistant TB: Lisa Chen, MD University of California, San Francisco Curry Interna:onal TB Center Sea=le, June 2016 Drug- Resistant TB: De1initions Mono- resistant: Resistance to a single drug Poly-
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance
 Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Linezolid: an effective, safe and cheap drug for patients failing multidrug-resistant tuberculosis treatment in India
 Eur Respir J 2012; 39: 956 962 DOI: 10.1183/09031936.00076811 CopyrightßERS 2012 Linezolid: an effective, safe and cheap drug for patients failing multidrug-resistant tuberculosis treatment in India R.
Eur Respir J 2012; 39: 956 962 DOI: 10.1183/09031936.00076811 CopyrightßERS 2012 Linezolid: an effective, safe and cheap drug for patients failing multidrug-resistant tuberculosis treatment in India R.
Drug resistant TB: The role of the laboratory
 Drug resistant TB: The role of the laboratory 26 Oct 2012 Andrew Whitelaw NHSLS / UCT TB lab functions: Outline Resistance testing Genotypic Phenotypic Which tests are done when, and why Reporting of
Drug resistant TB: The role of the laboratory 26 Oct 2012 Andrew Whitelaw NHSLS / UCT TB lab functions: Outline Resistance testing Genotypic Phenotypic Which tests are done when, and why Reporting of
University of Groningen. Tuberculosis and its sequelae Akkerman, Onno
 University of Groningen Tuberculosis and its sequelae Akkerman, Onno IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Tuberculosis and its sequelae Akkerman, Onno IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
ECHO: Management of URIs. Charles Krasner, M.D. Sierra NV Veterans Affairs Hospital University of NV, Reno School of Medicine October 16, 2018
 ECHO: Management of URIs Charles Krasner, M.D. Sierra NV Veterans Affairs Hospital University of NV, Reno School of Medicine October 16, 2018 Infectious causes of URIs change over time Most ARIs are viral
ECHO: Management of URIs Charles Krasner, M.D. Sierra NV Veterans Affairs Hospital University of NV, Reno School of Medicine October 16, 2018 Infectious causes of URIs change over time Most ARIs are viral
Case Presentations: Non Responding TB Dr. Manoj Yadav
 Case Presentations: Non Responding TB Dr. Manoj Yadav mbbs, dtcd, dnb (resp. dis.) Consultant Pulmonologist Kailash Hospital, Kailash Complex Near Mahadev Temple, Productivity Road Vadodara 390007 :: Phone:
Case Presentations: Non Responding TB Dr. Manoj Yadav mbbs, dtcd, dnb (resp. dis.) Consultant Pulmonologist Kailash Hospital, Kailash Complex Near Mahadev Temple, Productivity Road Vadodara 390007 :: Phone:
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus
 Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
Host, Syndrome, Bug, Drug: Introducing 2 Frameworks to Approach Infectious Diseases Cases with an Antimicrobial Stewardship Focus Montana ACP Meeting 2018 September 8, 2018 Staci Lee, MD, MEHP Billings
TRANSPARENCY COMMITTEE
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 29 October 2014 GRANUPAS, gastro-resistant granules 30 sachets with a calibrated measuring spoon (CIP: 34009 278 801
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 29 October 2014 GRANUPAS, gastro-resistant granules 30 sachets with a calibrated measuring spoon (CIP: 34009 278 801
BRUCELLOSIS. Morning report 7/11/05 Andy Bomback
 BRUCELLOSIS Morning report 7/11/05 Andy Bomback Also called undulant, Mediterranean, or Mata fever, brucellosis is an acute and chronic infection of the reticuloendothelial system gram negative facultative
BRUCELLOSIS Morning report 7/11/05 Andy Bomback Also called undulant, Mediterranean, or Mata fever, brucellosis is an acute and chronic infection of the reticuloendothelial system gram negative facultative
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan. Associate Consultant Infectious Disease Centre, PMH
 Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
Clinical Manifestations and Treatment of Plague Dr. Jacky Chan Associate Consultant Infectious Disease Centre, PMH Update of plague outbreak situation in Madagascar A large outbreak since 1 Aug 2017 As
MDR-TB drugs per WHO guidelines
 New antituberculous agents for drug-resistant resistant TB Symposium Belgian Society of Infectiology and Clinical Microbiology November 9 Jens Van Roey, MD - Tibotec Definitions MDR-TB multidrug resistance
New antituberculous agents for drug-resistant resistant TB Symposium Belgian Society of Infectiology and Clinical Microbiology November 9 Jens Van Roey, MD - Tibotec Definitions MDR-TB multidrug resistance
Update on Fluoroquinolones. Charles Krasner, M.D. June 16, 2016 Antibiotic Stewardship Program -ECHO
 Update on Fluoroquinolones Charles Krasner, M.D. June 16, 2016 Antibiotic Stewardship Program -ECHO Potential fluoroquinolone side-effects Increased risk, greater than with most other antibiotics, for
Update on Fluoroquinolones Charles Krasner, M.D. June 16, 2016 Antibiotic Stewardship Program -ECHO Potential fluoroquinolone side-effects Increased risk, greater than with most other antibiotics, for
Acute Pyelonephritis POAC Guideline
 Acute Pyelonephritis POAC Guideline Refer full regional pathway http://aucklandregion.healthpathways.org.nz/33444 EXCLUSION CRITERIA: COMPLICATED PYELONEPHRITIS Discuss with relevant specialist for advice
Acute Pyelonephritis POAC Guideline Refer full regional pathway http://aucklandregion.healthpathways.org.nz/33444 EXCLUSION CRITERIA: COMPLICATED PYELONEPHRITIS Discuss with relevant specialist for advice
The New England Journal of Medicine THE TREATMENT OF MULTIDRUG-RESISTANT TUBERCULOSIS IN TURKEY
 THE TREATMENT OF MULTIDRUG-RESISTANT TUBERCULOSIS IN TURKEY KEMAL TAHAOĞLU, M.D., TÜLAY TÖRÜN, M.D., TÜLIN SEVIM, M.D., GÜLIZ ATAÇ, M.D., ALTAN KIR, M.D., LEVENT KARASULU, M.D., IPEK ÖZMEN, M.D., AND NILÜFER
THE TREATMENT OF MULTIDRUG-RESISTANT TUBERCULOSIS IN TURKEY KEMAL TAHAOĞLU, M.D., TÜLAY TÖRÜN, M.D., TÜLIN SEVIM, M.D., GÜLIZ ATAÇ, M.D., ALTAN KIR, M.D., LEVENT KARASULU, M.D., IPEK ÖZMEN, M.D., AND NILÜFER
Coccidioidomycosis Nothing to disclose
 Coccidioidomycosis Nothing to disclose Disclosure Greg Melcher, M.D. Professor of Clinical Medicine Division of HIV, ID and Global Medicine Zuckerman San Francisco General Hospital University of California,
Coccidioidomycosis Nothing to disclose Disclosure Greg Melcher, M.D. Professor of Clinical Medicine Division of HIV, ID and Global Medicine Zuckerman San Francisco General Hospital University of California,
Exploring Novel Approaches to Shared TB Laboratory Services: California-Wisconsin Shared Services Pilot Study
 Exploring Novel Approaches to Shared TB Laboratory Services: California-Wisconsin Shared Services Pilot Study Julie Tans-Kersten, MS, BS-MT (ASCP) Tuberculosis Laboratory Program Coordinator Wisconsin
Exploring Novel Approaches to Shared TB Laboratory Services: California-Wisconsin Shared Services Pilot Study Julie Tans-Kersten, MS, BS-MT (ASCP) Tuberculosis Laboratory Program Coordinator Wisconsin
Period of study: 12 Nov 2002 to 08 Apr 2004 (first subject s first visit to last subject s last visit)
 Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
Study Synopsis This file is posted on the Bayer HealthCare Clinical Trials Registry and Results website and is provided for patients and healthcare professionals to increase the transparency of Bayer's
10/13/14. Low: not well absorbed. Good: [blood and tissue] < than if given IV. High: > 90% absorption orally
![10/13/14. Low: not well absorbed. Good: [blood and tissue] < than if given IV. High: > 90% absorption orally 10/13/14. Low: not well absorbed. Good: [blood and tissue] < than if given IV. High: > 90% absorption orally](/thumbs/79/80222162.jpg) Low: not well absorbed PO agent not for serious infection nitrofurantoin Good: [blood and tissue] < than if given IV [Therapeutic] in excess of [effective] eg. cephalexin High: > 90% absorption orally
Low: not well absorbed PO agent not for serious infection nitrofurantoin Good: [blood and tissue] < than if given IV [Therapeutic] in excess of [effective] eg. cephalexin High: > 90% absorption orally
Central Nervous System Infections
 Central Nervous System Infections Meningitis Treatment Bacterial meningitis is a MEDICAL EMERGENCY. ANTIBIOTICS SHOULD BE STARTED AS SOON AS THE POSSIBILITY OF BACTERIAL MENINGITIS BECOMES EVIDENT, IDEALLY
Central Nervous System Infections Meningitis Treatment Bacterial meningitis is a MEDICAL EMERGENCY. ANTIBIOTICS SHOULD BE STARTED AS SOON AS THE POSSIBILITY OF BACTERIAL MENINGITIS BECOMES EVIDENT, IDEALLY
Duration of antibiotic therapy:
 Duration of antibiotic therapy: How low can you go? Thomas Holland, MD Hilton Head, SC July 2017 Disclosures Consulting: The Medicines Company, Basilea Pharmaceutica Adjudication committee: Achaogen Grant
Duration of antibiotic therapy: How low can you go? Thomas Holland, MD Hilton Head, SC July 2017 Disclosures Consulting: The Medicines Company, Basilea Pharmaceutica Adjudication committee: Achaogen Grant
SHC Clinical Pathway: HAP/VAP Flowchart
 SHC Clinical Pathway: Hospital-Acquired and Ventilator-Associated Pneumonia SHC Clinical Pathway: HAP/VAP Flowchart v.08-29-2017 Diagnosis Hospitalization (HAP) Pneumonia develops 48 hours following: Endotracheal
SHC Clinical Pathway: Hospital-Acquired and Ventilator-Associated Pneumonia SHC Clinical Pathway: HAP/VAP Flowchart v.08-29-2017 Diagnosis Hospitalization (HAP) Pneumonia develops 48 hours following: Endotracheal
Duke University Hospital Guideline for Empiric Inpatient Treatment of Cancer- Related Neutropenic Fever in Adult Patients
 Duke University Hospital Guideline for Empiric Inpatient Treatment of Cancer- Related Neutropenic Fever in Adult Patients PURPOSE Fever among neutropenic patients is common and a significant cause of morbidity
Duke University Hospital Guideline for Empiric Inpatient Treatment of Cancer- Related Neutropenic Fever in Adult Patients PURPOSE Fever among neutropenic patients is common and a significant cause of morbidity
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings. Carlos Reyes Sacin, MD, AAHIVS
 Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
Antimicrobial Stewardship in the Long Term Care and Outpatient Settings Carlos Reyes Sacin, MD, AAHIVS Disclosure Speaker and consultant in HIV medicine for Gilead and Jansen Pharmaceuticals Objectives
64 year old retired male (former millwright)
 Cheryl Main 2013 None! 64 year old retired male (former millwright) Past medical history Type II Diabetes with Chronic Kidney Disease Sjogren s syndrome treated with plaquenil Autoimmune hemolytic anemia
Cheryl Main 2013 None! 64 year old retired male (former millwright) Past medical history Type II Diabetes with Chronic Kidney Disease Sjogren s syndrome treated with plaquenil Autoimmune hemolytic anemia
Dr. John Rogers. To Whom it May Concern, I have enclosed a cheque for the required $50.00 Hearing Fee. I am T
 ~ Dr. John Rogers 14The Ridgeway London, ON N6C 1Al T 519 432 0822 March 28,2007 To Whom it May Concern, I have enclosed a cheque for the required $50.00 Hearing Fee. I am appealing the dccision re the
~ Dr. John Rogers 14The Ridgeway London, ON N6C 1Al T 519 432 0822 March 28,2007 To Whom it May Concern, I have enclosed a cheque for the required $50.00 Hearing Fee. I am appealing the dccision re the
CLINICAL USE OF AMINOGLYCOSIDES AND FLUOROQUINOLONES
 CLINICAL USE OF AMINOGLYCOSIDES AND FLUOROQUINOLONES Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu THE AMINOGLYCOSIDES: 1944-1975 Drug
CLINICAL USE OF AMINOGLYCOSIDES AND FLUOROQUINOLONES Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu THE AMINOGLYCOSIDES: 1944-1975 Drug
Treatment of Nontuberculous Mycobacterial Infections (NTM)
 Treatment of Nontuberculous Mycobacterial Infections (NTM) Charles L. Daley, MD National Jewish Health University of Colorado, Denver Disclosures Investigator Insmed (inhaled liposomal amikacin) Advisory
Treatment of Nontuberculous Mycobacterial Infections (NTM) Charles L. Daley, MD National Jewish Health University of Colorado, Denver Disclosures Investigator Insmed (inhaled liposomal amikacin) Advisory
Outlines. Introduction Prevalence Resistance Clinical presentation Diagnosis Management Prevention Case presentation Achievements
 Amal Meas Al-Anizi, PharmD Candidate KSU, Infectious Disease Rotation 2014 Outlines Introduction Prevalence Resistance Clinical presentation Diagnosis Management Prevention Case presentation Achievements
Amal Meas Al-Anizi, PharmD Candidate KSU, Infectious Disease Rotation 2014 Outlines Introduction Prevalence Resistance Clinical presentation Diagnosis Management Prevention Case presentation Achievements
OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS
 HTIDE CONFERENCE 2018 OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS FEDERICO PEA INSTITUTE OF CLINICAL PHARMACOLOGY DEPARTMENT OF MEDICINE, UNIVERSITY OF UDINE, ITALY SANTA
HTIDE CONFERENCE 2018 OPTIMIZATION OF PK/PD OF ANTIBIOTICS FOR RESISTANT GRAM-NEGATIVE ORGANISMS FEDERICO PEA INSTITUTE OF CLINICAL PHARMACOLOGY DEPARTMENT OF MEDICINE, UNIVERSITY OF UDINE, ITALY SANTA
Antibiotics in the trenches: An ER Doc s Perspective
 Antibiotics in the trenches: An ER Doc s Perspective Peter Currie, MD Medical Director for Quality Emergency Physicians Professional Association (EPPA) Agenda Emergency Medicine Specific Disease Processes
Antibiotics in the trenches: An ER Doc s Perspective Peter Currie, MD Medical Director for Quality Emergency Physicians Professional Association (EPPA) Agenda Emergency Medicine Specific Disease Processes
M5 MEQs 2016 Session 3: SOB 18/11/16
 M5 MEQs 2016 Session 3: SOB 18/11/16 http://tinyurl.com/hn7qzt3 Question 1 Ms Tan is a 52 year old female with no past medical history. She comes to the emergency department presenting with a fever for
M5 MEQs 2016 Session 3: SOB 18/11/16 http://tinyurl.com/hn7qzt3 Question 1 Ms Tan is a 52 year old female with no past medical history. She comes to the emergency department presenting with a fever for
$100 $200 $300 $400 $500
 Skin is In Runny Noses Got to go! Hear no evil It s in the Lungs $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400 $500 $500 $500 $500 $500 Double Jeopardy
Skin is In Runny Noses Got to go! Hear no evil It s in the Lungs $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400 $500 $500 $500 $500 $500 Double Jeopardy
MINISTRY OF HEALTH, MALAYSIA
 LAMPIRAN C Ref. No : Photo 4 x 6 ( Part I : Personal information ) 1. FULL NAME ( FIRST NAME) : ( FATHER'S NAME) : 2. MALE/FEMALE : 3. AGE : 7. NAME OF EMPLOYER / RECRUITING AGENCY : 8. ADDRESS OF EMPLOYER
LAMPIRAN C Ref. No : Photo 4 x 6 ( Part I : Personal information ) 1. FULL NAME ( FIRST NAME) : ( FATHER'S NAME) : 2. MALE/FEMALE : 3. AGE : 7. NAME OF EMPLOYER / RECRUITING AGENCY : 8. ADDRESS OF EMPLOYER
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections
 Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Optimizing Antibiotic Treatment of Skin and Soft Tissue Infections 15th Annual Rocky Mountain Hospital Medicine Symposium November 6, 2017 Tim Jenkins, MD Director, Antibiotic Stewardship Program Denver
Multidrug resistant tuberculosis. Where next? Professor Peter D O Davies (Liverpool)
 Multidrug resistant tuberculosis. Where next? Professor Peter D O Davies (Liverpool) DOTS + and LTBI New drugs for TB and the challenge of resistance talk plan 1. Epidemiology 2. Treatment 3. The MDRTB
Multidrug resistant tuberculosis. Where next? Professor Peter D O Davies (Liverpool) DOTS + and LTBI New drugs for TB and the challenge of resistance talk plan 1. Epidemiology 2. Treatment 3. The MDRTB
DATA COLLECTION SECTION BY FRONTLINE TEAM. Patient Identifier/ Medical Record number (for facility use only)
 Assessment of Appropriateness of ICU Antibiotics (Patient Level Sheet) **Note this is intended for internal purposes only. Please do not return to PQC.** For this assessment, inappropriate antibiotic use
Assessment of Appropriateness of ICU Antibiotics (Patient Level Sheet) **Note this is intended for internal purposes only. Please do not return to PQC.** For this assessment, inappropriate antibiotic use
Antibiotic stewardship in long term care
 Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
Antibiotic stewardship in long term care Shira Doron, MD Associate Professor of Medicine Division of Geographic Medicine and Infectious Diseases Tufts Medical Center Boston, MA Consultant to Massachusetts
New drugs and regimens for treatment of drug-sensitive TB (DS-TB) Patrick
 New drugs and regimens for treatment of drug-sensitive TB (DS-TB) Patrick Phillips Patrick.Phillips@ucsf.edu @PPJPhillips Outline Overview of regimen development strategies 1-3 year horizon: Ongoing phase
New drugs and regimens for treatment of drug-sensitive TB (DS-TB) Patrick Phillips Patrick.Phillips@ucsf.edu @PPJPhillips Outline Overview of regimen development strategies 1-3 year horizon: Ongoing phase
Effects of Moxifloxacin PK-PD and drug interactions on its use in the Treatment of Tuberculosis(TB)
 Effects of Moxifloxacin PK-PD and drug interactions on its use in the Treatment of Tuberculosis(TB) Session: Fanning the Flames of HIV and TB Cointeraction SA AIDS Conference-Durban ICC 13-15 June 2017
Effects of Moxifloxacin PK-PD and drug interactions on its use in the Treatment of Tuberculosis(TB) Session: Fanning the Flames of HIV and TB Cointeraction SA AIDS Conference-Durban ICC 13-15 June 2017
Risk Factors for Poor Outcomes in Patients with Multi-Drug Resistant Tuberculosis in South Korea
 Hanyang Med Rev 2016;36:262-268 https://doi.org/10.7599/hmr.2016.36.4.262 pissn 1738-429X eissn 2234-4446 Original Article Risk Factors for Poor Outcomes in Patients with Multi-Drug Resistant Tuberculosis
Hanyang Med Rev 2016;36:262-268 https://doi.org/10.7599/hmr.2016.36.4.262 pissn 1738-429X eissn 2234-4446 Original Article Risk Factors for Poor Outcomes in Patients with Multi-Drug Resistant Tuberculosis
PHYSICIAN ORDERS. Page 1 of 6. Provider Initial: Esophagectomy Preoperative [ ] Height Weight Allergies
![PHYSICIAN ORDERS. Page 1 of 6. Provider Initial: Esophagectomy Preoperative [ ] Height Weight Allergies PHYSICIAN ORDERS. Page 1 of 6. Provider Initial: Esophagectomy Preoperative [ ] Height Weight Allergies](/thumbs/93/111492780.jpg) Height Weight Allergies If appropriate for patient condition, please consider the following order sets: Hydration Order for Reducing Risk of Radiocontrast Induced Nephrotoxicity Physician Order #683 In
Height Weight Allergies If appropriate for patient condition, please consider the following order sets: Hydration Order for Reducing Risk of Radiocontrast Induced Nephrotoxicity Physician Order #683 In
The Law of Unintended Consequences
 The Law of Unintended Consequences Tests I Wish You d Never Ordered (Choosing Wisely ) G Blackburn DO, MACOI Moderator, (Infectious Disease) Annual WVOMA CME Conference November, 2017 White Sulphur Springs,
The Law of Unintended Consequences Tests I Wish You d Never Ordered (Choosing Wisely ) G Blackburn DO, MACOI Moderator, (Infectious Disease) Annual WVOMA CME Conference November, 2017 White Sulphur Springs,
Antibiotics & Common Infections: Stewardship, Effectiveness, Safety & Clinical Pearls. Welcome We will begin shortly.
 Antibiotics & Common Infections: Stewardship, Effectiveness, Safety & Clinical Pearls Welcome We will begin shortly. The Canadian Pharmacists Association is pleased to be collaborating with the following
Antibiotics & Common Infections: Stewardship, Effectiveness, Safety & Clinical Pearls Welcome We will begin shortly. The Canadian Pharmacists Association is pleased to be collaborating with the following
Disclosures. Principles of Antimicrobial Therapy. Obtaining an Accurate Diagnosis Obtain specimens PRIOR to initiating antimicrobials
 Disclosures Principles of Antimicrobial Therapy None Lori A. Cox MSN, ACNP-BC, ACNPC, FCCM Penn State Hershey Medical Center Neuroscience Critical Care Unit Obtaining an Accurate Diagnosis Determine site
Disclosures Principles of Antimicrobial Therapy None Lori A. Cox MSN, ACNP-BC, ACNPC, FCCM Penn State Hershey Medical Center Neuroscience Critical Care Unit Obtaining an Accurate Diagnosis Determine site
Northwestern Medicine Central DuPage Hospital Antimicrobial Criteria Updated 11/16/16
 Northwestern Medicine Central DuPage Hospital Antimicrobial Criteria Updated 11/16/16 These criteria are based on national and local susceptibility data as well as Infectious Disease Society of America
Northwestern Medicine Central DuPage Hospital Antimicrobial Criteria Updated 11/16/16 These criteria are based on national and local susceptibility data as well as Infectious Disease Society of America
Inappropriate Use of Antibiotics and Clostridium difficile Infection. Jocelyn Srigley, MD, FRCPC November 1, 2012
 Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Inappropriate Use of Antibiotics and Clostridium difficile Infection Jocelyn Srigley, MD, FRCPC November 1, 2012 Financial Disclosures } No conflicts of interest } The study was supported by a Hamilton
Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults)
 Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults) Community Acquired Pneumonia Community Acquired Pneumonia 1) Is it pneumonia? ie new symptoms and signs of
Guidelines for the Initiation of Empirical Antibiotic therapy in Respiratory Disease (Adults) Community Acquired Pneumonia Community Acquired Pneumonia 1) Is it pneumonia? ie new symptoms and signs of
What is pneumonia? Infection of the lung parenchyma Causative agents include bacteria, viruses, fungi, protozoa.
 Pneumonia What is pneumonia? Infection of the lung parenchyma Causative agents include bacteria, viruses, fungi, protozoa www.netmedicine.com/xray/xr.htm Definition acute infectious disease, etiology usually
Pneumonia What is pneumonia? Infection of the lung parenchyma Causative agents include bacteria, viruses, fungi, protozoa www.netmedicine.com/xray/xr.htm Definition acute infectious disease, etiology usually
Appropriate Management of Common Pediatric Infections. Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases
 Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
Appropriate Management of Common Pediatric Infections Blaise L. Congeni M.D. Akron Children s Hospital Division of Pediatric Infectious Diseases It s all about the microorganism The common pathogens Viruses
Interactive session: adapting to antibiogram. Thong Phe Heng Vengchhun Felix Leclerc Erika Vlieghe
 Interactive session: adapting to antibiogram Thong Phe Heng Vengchhun Felix Leclerc Erika Vlieghe Case 1 63 y old woman Dx: urosepsis? After 2 d: intermediate result: Gram-negative bacilli Empiric antibiotic
Interactive session: adapting to antibiogram Thong Phe Heng Vengchhun Felix Leclerc Erika Vlieghe Case 1 63 y old woman Dx: urosepsis? After 2 d: intermediate result: Gram-negative bacilli Empiric antibiotic
Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC
 Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC APPROVED BY: Policy and Guidelines Committee TRUST REFERENCE: B9/2009 AWP Ref: AWP61 Date (approved): July 2008 REVIEW
Pneumonia Antibiotic Guidance for Adults PAGL Inclusion Approved at January 2017 PGC APPROVED BY: Policy and Guidelines Committee TRUST REFERENCE: B9/2009 AWP Ref: AWP61 Date (approved): July 2008 REVIEW
INCIDENCE OF BACTERIAL COLONISATION IN HOSPITALISED PATIENTS WITH DRUG-RESISTANT TUBERCULOSIS
 INCIDENCE OF BACTERIAL COLONISATION IN HOSPITALISED PATIENTS WITH DRUG-RESISTANT TUBERCULOSIS 1 Research Associate, Drug Utilisation Research Unit, Nelson Mandela University 2 Human Sciences Research Council,
INCIDENCE OF BACTERIAL COLONISATION IN HOSPITALISED PATIENTS WITH DRUG-RESISTANT TUBERCULOSIS 1 Research Associate, Drug Utilisation Research Unit, Nelson Mandela University 2 Human Sciences Research Council,
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Small Animal Medicine Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
ANTIBIOTIC USE GUIDELINES FOR URINARY TRACT AND RESPIRATORY DISEASE
 ANTIBIOTIC USE GUIDELINES FOR URINARY TRACT AND RESPIRATORY DISEASE Jane Sykes, BVSc(Hons), PhD, DACVIM (SAIM) School of Veterinary Medicine Dept. of Medicine & Epidemiology University of California Davis,
ANTIBIOTIC USE GUIDELINES FOR URINARY TRACT AND RESPIRATORY DISEASE Jane Sykes, BVSc(Hons), PhD, DACVIM (SAIM) School of Veterinary Medicine Dept. of Medicine & Epidemiology University of California Davis,
Infection Comments First Line Agents Penicillin Allergy History of multiresistant. line treatment: persist for >7 days they may be
 Gastrointestinal Infections Infection Comments First Line Agents Penicillin Allergy History of multiresistant Campylobacter Antibiotics not recommended. Erythromycin 250mg PO 6 Alternative to first N/A
Gastrointestinal Infections Infection Comments First Line Agents Penicillin Allergy History of multiresistant Campylobacter Antibiotics not recommended. Erythromycin 250mg PO 6 Alternative to first N/A
Creating a global community for clinical drug repurposing and development. Leonard Sacks Center for drug evaluation and research FDA
 Creating a global community for clinical drug repurposing and development Leonard Sacks Center for drug evaluation and research FDA Neglected tropical diseases 1) Repurposing and developing new drugs 2)
Creating a global community for clinical drug repurposing and development Leonard Sacks Center for drug evaluation and research FDA Neglected tropical diseases 1) Repurposing and developing new drugs 2)
Australian College of Veterinary Scientists. Fellowship Examination. Small Animal Surgery Paper 1
 Australian College of Veterinary Scientists Fellowship Examination June 2011 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer your choice
Australian College of Veterinary Scientists Fellowship Examination June 2011 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer your choice
Quality of 2 nd line medicines for tuberculosis. Ms Lisa Hedman World Health Organization Department of Essential Medicines and Health Products
 Quality of 2 nd line medicines for tuberculosis Ms Lisa Hedman World Health Organization Department of Essential Medicines and Health Products Case studies in medicines for tuberculosis Outline: Statistics
Quality of 2 nd line medicines for tuberculosis Ms Lisa Hedman World Health Organization Department of Essential Medicines and Health Products Case studies in medicines for tuberculosis Outline: Statistics
Suitability of Antibiotic Treatment for CAP (CAPTIME) The duration of antibiotic treatment in community acquired pneumonia (CAP)
 STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
STUDY PROTOCOL Suitability of Antibiotic Treatment for CAP (CAPTIME) Purpose The duration of antibiotic treatment in community acquired pneumonia (CAP) lasts about 9 10 days, and is determined empirically.
Tuberculosis infection in an Asian elephant at a Japanese Zoo and its first treatment in Japan
 Tuberculosis infection in an Asian elephant at a Japanese Zoo and its first treatment in Japan Satoshi Ishikawa, Satomi Suga, Yasuhiko Mukai Fukuyama Zoo, Hiroshima Fukuyama Zoo October 22th, 2017 Tuberculosis
Tuberculosis infection in an Asian elephant at a Japanese Zoo and its first treatment in Japan Satoshi Ishikawa, Satomi Suga, Yasuhiko Mukai Fukuyama Zoo, Hiroshima Fukuyama Zoo October 22th, 2017 Tuberculosis
MANAGEMENT OF PELVIC INFLAMMATORY DISEASE
 GYNAECOLOGY SERVICES NORTH CUMBRIA MANAGEMENT OF PELVIC INFLAMMATORY DISEASE Author/Contact DOCUMENT CONTROL Lufti Shamsuddin, ST4 Obs & Gynae Trainee / Nalini Munjuluri, Consultant Gynaecology Tel: 01228
GYNAECOLOGY SERVICES NORTH CUMBRIA MANAGEMENT OF PELVIC INFLAMMATORY DISEASE Author/Contact DOCUMENT CONTROL Lufti Shamsuddin, ST4 Obs & Gynae Trainee / Nalini Munjuluri, Consultant Gynaecology Tel: 01228
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
Levofloxacin induced bilateral achilles tendonitis
 CASE REPORT Levofloxacin induced bilateral achilles tendonitis Muhammad Ishaq, Chand Sudham, Kumar Ajeet, Adnan Baig, Shaikh M. Ishaq Department of Medicine, Authors: 1. Dr. Muhammad Ishaq M.B.B.S., F.C.P.S.
CASE REPORT Levofloxacin induced bilateral achilles tendonitis Muhammad Ishaq, Chand Sudham, Kumar Ajeet, Adnan Baig, Shaikh M. Ishaq Department of Medicine, Authors: 1. Dr. Muhammad Ishaq M.B.B.S., F.C.P.S.
Standing Orders for the Treatment of Outpatient Peritonitis
 Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
Standing Orders for the Treatment of Outpatient Peritonitis 1. Definition of Peritonitis: a. Cloudy effluent. b. WBC > 100 cells/mm3 with >50% polymorphonuclear (PMN) cells with minimum 2 hour dwell. c.
CLINICAL PROTOCOL FOR COMMUNITY ACQUIRED PNEUMONIA. SCOPE: Western Australia. CORB score equal or above 1. All criteria must be met:
 CLINICAL PROTOCOL F COMMUNITY ACQUIRED PNEUMONIA SCOPE: Western Australia All criteria must be met: Inclusion Criteria Exclusion Criteria CB score equal or above 1. Mild/moderate pneumonia confirmed by
CLINICAL PROTOCOL F COMMUNITY ACQUIRED PNEUMONIA SCOPE: Western Australia All criteria must be met: Inclusion Criteria Exclusion Criteria CB score equal or above 1. Mild/moderate pneumonia confirmed by
Nurse Prescribing: Key Principles and Developments. Elissa Ladd, PhD, FNP-BC MGH Institute of Health Professions Boston, Massachusetts USA
 Nurse Prescribing: Key Principles and Developments Elissa Ladd, PhD, FNP-BC MGH Institute of Health Professions Boston, Massachusetts USA No disclosures to report Objectives: 1) To provide an overview
Nurse Prescribing: Key Principles and Developments Elissa Ladd, PhD, FNP-BC MGH Institute of Health Professions Boston, Massachusetts USA No disclosures to report Objectives: 1) To provide an overview
