Old Disease New Location Surgeons Be Alerted
|
|
|
- Christopher Simon
- 5 years ago
- Views:
Transcription
1 Old Disease New Location Surgeons Be Alerted K. B. Ashok Vol. 3 No. 4 (April 2011) International Journal of Collaborative Research on Internal Medicine & Public Health (IJCRIMPH) ISSN Journal Type: Open Access Volume 3 Number 4 Journal details including published articles and guidelines for authors can be found at: To cite this Article: Ashok KB. Old Disease New Location Surgeons Be Alerted. International Journal of Collaborative Research on Internal Medicine & Public Health. 2011; 3(4): Article URL: Correspondence concerning this article should be addressed to Dr. K. B. Ashok; Midnapore Medical College and Hospital, Midnapore, India / krsnasok@yahoo.co.in Paper publication: 10 May 2011
2 328 Old Disease New Location Surgeons Be Alerted K. B. Ashok * Midnapore Medical College and Hospital, Midnapore, India * Corresponding author; krsnasok@yahoo.co.in ABSTRACT Echinococcus granulosus causes a zoonotic infection called Cystic Echinococcosis (CE). Surgeons meet with hydatid cysts of the liver and lungs with reasonable frequency. However hydatid cyst may appear in other parts of the body too. A 30 yrs old lady presented with a smooth slow-growing subcutaneous nodule on the anteromedial side of the right thigh with no detectable primary site in the liver or lung. The case subsequently diagnosed as hydatid cyst of muscle and radical surgery was done under coverage of anihelminthic drug. The common practice in this type of case is to do FNAC taking the lesion to be a soft tissue neoplasm. The aim of this case presentation is to make aware of the fact that in a case of diffuse non-tender swelling with history of gradual increase in size hydatid cyst also has to be considered in the differential diagnosis. Keywords: Hydatid Cyst, Thigh Muscle, Cystic echinococcosis, Muscular echinococcosis Introduction Cystic echinococcosis (CE) caused by the tape worm Echinococcus granulosus is a zoonotic infection occurring in different parts of world. It is also unusual in northern Europe. The endemic areas include the Mediterranean countries, the Middle East, Iceland, the southern part of South America, New Zealand, Australia, and southern parts of Africa; the latter 5 are intensive endemic areas. The incidence of CE in endemic areas ranges from cases per 100,000 inhabitants, while the incidence of AE ranges from cases per 100,000 inhabitants, making it a much more rare form of echinococcosis. Infestation with E vogeli is the most rare form of echinococcosis and is reported mainly in the southern parts of South America. Surgeons meet with hydatid cysts of the liver and lungs with a reasonable frequency. However when the cyst appears in the unusual sites such as extremities, the clinical suspicion is unlikely. [1] Case Report The patient, a thirty (30) years old lady, presented with a smooth, large swelling on the anteromedial side of her right thigh. There was a history of gradual increase in size for last four years. On clinical examination, a firm mass sized 12cm X 8cm was found to be free from underlying skin and subcutaneous tissue and appeared to arise from the underlying muscles and fascia but not fixed to the bone. Clinically it appeared to be a soft tissue benign tumour. Routine haematological tests show increase (9%) of eosinophil count and no abnormality detected in chest X-ray. MRI of the thigh was done which revealed a hydatid cyst along with some daughter cysts arising from quadriceps muscle of thigh. CT scan of the abdomen and thorax did not reveal any hydatid cyst of liver and lung. The patient was put on oral Albendazole (10-15 mgm/kg/day) for 4 weeks. The area was
3 329 explored and the whole of the cyst along with 1cm rim of the surrounding soft tissue including muscle was removed. The whole area was irrigated with suitably diluted (0.5%) Cetrimide solution. Haemostasis was secured and wound was closed over a drain. [Fig no. 1] Muscular hydatid cyst was confirmed by histological examination. [Fig no. 2] Post operative course of Albendazole for one month was given to the patient to reduce the chance of recurrence. The patient had an uneventful postoperative recovery. No local recurrence or systemic illness was detected during postoperative follow up period within one year. Discussion Cystic echinococcosis (CE) can involve any organ. Organs affected by E. granulosus are the Liver (63%), Lungs (25%), Muscle (5%), Bones (3%), Kidney (2%), Brain (1%) and spleen (1%).[1] Most of the times involvement is usually characterized by a palpable mass. [3,4] Clinical presentation of the hydatid disease depends on the size and site of the lesion. [5] Radical surgery (total pericystectomy or partial affected organ resection), conservative surgery (open cystectomy) or simple tube drainage for infeted communicating cysts are choices of surgical techniques. [6] The more radical the procedure, lower the risk of relapses but higher the risk of complications. [7] Sterilization of the cyst cavity is done by different scolicidal agents and cetrimide solution (0.5%) provides the best protection with least complications. [8] Pre and Postoperative one month course of Albendazole or two weeks of praziquantel should be considered in order to sterilize the cyst and decrease the chance of anaphylaxis, decrease the tension in the cyst wall and to reduce the recurrence rate postoperatively.[9] Conclusion Hydatid cyst of liver and lung is not uncommon in clinical practice. When the cyst is present in the rare site such as in extremities and clinically presents as benign soft tissue tumour the suspicion of hydatid cyst in unlikely. This is further confusing when the patient does not have any primary hydatid cyst in lung or liver. Doctors should also consider the possibility of hydatid cyst in any patient presenting as a soft tissue swelling attending the clinic. As CE can affect any organ of the body, a higher suspicion of the disease is justified in an apparent cystic neoplasm especially in the endemic region. References overview. (Accessed on 29th January, 2011.) 2. Biswas B, Ghosh D, Bhattacharjee R, Patra A, Basuthakur S, Basu R. One stage management of hydatid cyst of lung and liver- by right thoracotomy & phrenotomy. IJTCVS 2004; 20: Marwah S, Shubramainan P, Marwah N, Rattan KN, Krwasra RK. Infested primary intramuscular echinococcosis of thigh. Indian J Pediatr 2005, Sept; 72(9); Erol B, Tetik C, Altun E, Soyal A, Bakir M. Hydatid cyst presenting as a soft tissue calf mass in a child. Eur J Pediatr Surg Feb; 17(1): S.A. ABU-ESHY Case report Some rare presentations of hydatid cyst (Echinococcus granulosus), J R Coll Surg Edinb,43, October 1998,
4 Ates M, Karakapalam M. Hydatid cyst in the biceps and gluteal muscles: case report. Surg Infect (Larchmt), 2007 Aug; 8(4): Kafih M, Ajbal M, Ridia M, Idriss H, Zerualli O. Hydatid cyst of the psoas muscle. Ann Gastroenterol Hepatol (Paris), 1933 May; 29(3): Vicidomini S, Cancrini G, Gabrielli S, Naspetti R, Bartoloni A. Muscular cystic hydatidosis: case report. BMC Infect Dis Mar; 30: 7: Duvqulu F, Karaoqlu S, Erdoqan N, Yildiz O. Primary hydatid cyst of the thigh: a case report of unusual localization. Turk J Pediatr Jul-Sept; 48(3): FIGURES Peroperative picture of excision of the hydatid cyst in thigh
5 331 Post operative picture of muscle, larger cyst wall, smaller cyst wall (Right to left)
6 332 Histopathology of the cyst wall to confirm it as Hydatid Cyst
CRANIAL HYDATID CYST
 Thi-Qar Medical Journal (TQMJ): Vol(6) No(1):2012(48-52) OBJECT: CRANIAL HYDATID CYST Dr. Haitham Handhal* HYDATID disease is caused by infestation by larvae of the tapeworm Echinococcus granulosus. The
Thi-Qar Medical Journal (TQMJ): Vol(6) No(1):2012(48-52) OBJECT: CRANIAL HYDATID CYST Dr. Haitham Handhal* HYDATID disease is caused by infestation by larvae of the tapeworm Echinococcus granulosus. The
An Unusual Presentation of Hydatid Cyst (Echinococcus granulosus)
 Bahrain Medical Bulletin, Vol.23, No.1, March 2001 An Unusual Presentation of Hydatid Cyst (Echinococcus granulosus) Suleiman Jastaniah, FRCS (Ed)* Tarek S Malatani, FRCS* E I Archibong, FRCOG* Abdulhameed
Bahrain Medical Bulletin, Vol.23, No.1, March 2001 An Unusual Presentation of Hydatid Cyst (Echinococcus granulosus) Suleiman Jastaniah, FRCS (Ed)* Tarek S Malatani, FRCS* E I Archibong, FRCOG* Abdulhameed
Multiple Organ Involvement with Hydatid Cysts
 Iranian J Parasitol: Vol. 5, No.2, 2010, pp. 65-70 Tehran University of Medical Sciences Publication http://tums.ac.ir Case Report Iranian J Parasitol Open access Journal at http://ijpa.tums.ac.ir Iranian
Iranian J Parasitol: Vol. 5, No.2, 2010, pp. 65-70 Tehran University of Medical Sciences Publication http://tums.ac.ir Case Report Iranian J Parasitol Open access Journal at http://ijpa.tums.ac.ir Iranian
Isolated primary hydatid cyst of small intestinal mesentery: an exceptional location of hydatid disease
 Case report Open Access Isolated primary hydatid cyst of small intestinal mesentery: an exceptional location of hydatid disease Mohammed Najih 1,&, Ali Chabni 1, Gilles Attoulou 1, Rajae Yamoul 1, Mbarek
Case report Open Access Isolated primary hydatid cyst of small intestinal mesentery: an exceptional location of hydatid disease Mohammed Najih 1,&, Ali Chabni 1, Gilles Attoulou 1, Rajae Yamoul 1, Mbarek
ECHINOCOCCOSIS. By Dr. Ameer kadhim Hussein. M.B.Ch.B. FICMS (Community Medicine).
 ECHINOCOCCOSIS By Dr. Ameer kadhim Hussein. M.B.Ch.B. FICMS (Community Medicine). INTRODUCTION Species under genus Echinococcus are small tapeworms of carnivores with larval stages known as hydatids proliferating
ECHINOCOCCOSIS By Dr. Ameer kadhim Hussein. M.B.Ch.B. FICMS (Community Medicine). INTRODUCTION Species under genus Echinococcus are small tapeworms of carnivores with larval stages known as hydatids proliferating
Hydatid Disease. Overview
 Hydatid Disease Overview Hydatid disease in man is caused principally by infection with the larval stage of the dog tapeworm Echinococcus granulosus. It is an important pathogenic zoonotic parasitic infection
Hydatid Disease Overview Hydatid disease in man is caused principally by infection with the larval stage of the dog tapeworm Echinococcus granulosus. It is an important pathogenic zoonotic parasitic infection
ISPUB.COM. Peritoneal Hydatidosis. F Parray, M Gagloo, A Bhat, N Chowdri, M Noor CASE REPORT
 ISPUB.COM The Internet Journal of Surgery Volume 9 Number 2 Peritoneal Hydatidosis F Parray, M Gagloo, A Bhat, N Chowdri, M Noor Citation F Parray, M Gagloo, A Bhat, N Chowdri, M Noor. Peritoneal Hydatidosis.
ISPUB.COM The Internet Journal of Surgery Volume 9 Number 2 Peritoneal Hydatidosis F Parray, M Gagloo, A Bhat, N Chowdri, M Noor Citation F Parray, M Gagloo, A Bhat, N Chowdri, M Noor. Peritoneal Hydatidosis.
Recurrent Hydatid Cyst of Liver with Asymptomatic Concomitant Hydatid Cyst of Lung: An Unusual Presentation- Case Report
 Iran J Parasitol Tehran University of Medical Sciences Publication http:// tums.ac.ir Open access Journal at http:// ijpa.tums.ac.ir Iranian Society of Parasitology http:// isp.tums.ac.ir Case Report Recurrent
Iran J Parasitol Tehran University of Medical Sciences Publication http:// tums.ac.ir Open access Journal at http:// ijpa.tums.ac.ir Iranian Society of Parasitology http:// isp.tums.ac.ir Case Report Recurrent
The role of multidispinary team in management of Hydatid disease
 The role of multidispinary team in management of Hydatid disease Dr/ Rasheed ALEEZI (JBGS, MHPBS) Departmement of general surgery, USThospital Sana`a-YEMEN 58 years old, female patient, housewif. Complaints
The role of multidispinary team in management of Hydatid disease Dr/ Rasheed ALEEZI (JBGS, MHPBS) Departmement of general surgery, USThospital Sana`a-YEMEN 58 years old, female patient, housewif. Complaints
Unusual Presentation of Hydatid Cyst: A Case Series With Review of Literature
 ISPUB.COM The Internet Journal of Parasitic Diseases Volume 6 Number 1 Unusual Presentation of Hydatid Cyst: A Case Series With Review of Literature S Gole, G Gole, V Satyanarayana Citation S Gole, G Gole,
ISPUB.COM The Internet Journal of Parasitic Diseases Volume 6 Number 1 Unusual Presentation of Hydatid Cyst: A Case Series With Review of Literature S Gole, G Gole, V Satyanarayana Citation S Gole, G Gole,
"Serpent" Sign, "Double Arch" Sign and "Air-Bubble"Sign in a case of Ruptured Hydatid Cyst-A Case Report
 Article ID: WMC004602 ISSN 2046-1690 "Serpent" Sign, "Double Arch" Sign and "Air-Bubble"Sign in a case of Ruptured Hydatid Cyst-A Case Report Peer review status: No Corresponding Author: Dr. Dipti Gothi,
Article ID: WMC004602 ISSN 2046-1690 "Serpent" Sign, "Double Arch" Sign and "Air-Bubble"Sign in a case of Ruptured Hydatid Cyst-A Case Report Peer review status: No Corresponding Author: Dr. Dipti Gothi,
HYDATID CYST DISEASE
 HYDATID CYST DISEASE Hydatid disease, also called hydatidosis or echinococcosis, is a cystforming disease resulting from an infection with the metacestode, or larval form, of parasitic dog tapeworms from
HYDATID CYST DISEASE Hydatid disease, also called hydatidosis or echinococcosis, is a cystforming disease resulting from an infection with the metacestode, or larval form, of parasitic dog tapeworms from
Associated Terms: Breast Cancer, Radical Mastectomy, Mastectomy, Mammectomy, Mammary Adenocarcinoma
 Associated Terms: Breast Cancer, Radical Mastectomy, Mastectomy, Mammectomy, Mammary Adenocarcinoma The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Associated Terms: Breast Cancer, Radical Mastectomy, Mastectomy, Mammectomy, Mammary Adenocarcinoma The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Laparoscopic partial cystectomy for the treatment of hepatic hydatid cysts
 Laparoscopic partial cystectomy for hepatic hydatid cysts Original Research Article ISSN: 2394-0026 (P) Laparoscopic partial cystectomy for the treatment of hepatic hydatid cysts Ilhan Ece 1*, Huseyin
Laparoscopic partial cystectomy for hepatic hydatid cysts Original Research Article ISSN: 2394-0026 (P) Laparoscopic partial cystectomy for the treatment of hepatic hydatid cysts Ilhan Ece 1*, Huseyin
Recurrent giant hydatid cyst in the left axilla: A case report
 www.edoriumjournals.com Case report peer REVIEWED OPEN ACCESS Recurrent giant hydatid cyst in the left axilla: A case report Abbas Alibakhshi, Mehrdad Larry ABSTRACT Introduction: Hydatid disease in the
www.edoriumjournals.com Case report peer REVIEWED OPEN ACCESS Recurrent giant hydatid cyst in the left axilla: A case report Abbas Alibakhshi, Mehrdad Larry ABSTRACT Introduction: Hydatid disease in the
Cystic Hydatid Disease in Southern Sudan
 Original Article Cystic Hydatid Disease in Southern Sudan D.K. Lado, MBBS, FS SMSB, Juba Teaching Hospital, Juba, South Sudan Correspondence and reprint requests to: Dr. D.K. Lado, Juba Teaching Hospital,
Original Article Cystic Hydatid Disease in Southern Sudan D.K. Lado, MBBS, FS SMSB, Juba Teaching Hospital, Juba, South Sudan Correspondence and reprint requests to: Dr. D.K. Lado, Juba Teaching Hospital,
Clinics in diagnostic imaging (102)
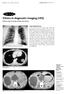 M e d i c a l E d u c a t i o n Singapore Med J 2005; 46(2) : 93 CME Article Clinics in diagnostic imaging (102) M Azeemuddin, T UI-Haq, H Ahsan, W A Memon Fig. 1 Chest radiograph (posteroanterior projection).
M e d i c a l E d u c a t i o n Singapore Med J 2005; 46(2) : 93 CME Article Clinics in diagnostic imaging (102) M Azeemuddin, T UI-Haq, H Ahsan, W A Memon Fig. 1 Chest radiograph (posteroanterior projection).
Multiple pulmonary hydatid cysts
 Postgrad. med. J. (December 1967) 43, 774-778. THE LUNG is the second commonest site in man, where the intermediate larval-cysticercal stage of Echinococcus granulosus develops. It is not unusual to find
Postgrad. med. J. (December 1967) 43, 774-778. THE LUNG is the second commonest site in man, where the intermediate larval-cysticercal stage of Echinococcus granulosus develops. It is not unusual to find
Rare presentations and Complications of Hepatic Hydatid Cysts
 Rare presentations and Complications of Hepatic Hydatid Cysts Poster No.: C-1926 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Kapoor, A. Arora, N. GUPTA, S. K. Puri ; Delhi/IN, NEW 1 2 3 3
Rare presentations and Complications of Hepatic Hydatid Cysts Poster No.: C-1926 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Kapoor, A. Arora, N. GUPTA, S. K. Puri ; Delhi/IN, NEW 1 2 3 3
Laparoscopic versus Open Management of Hydatid Cyst of Liver
 10.5005/jp-journals-10007-1108 ORIGINAL ARTICLE WJOLS Laparoscopic versus Open Management of Hydatid Cyst of Liver Falih Mohssen Ali Consultant Surgeon, Basrah Teaching Hospital, Iraq ABSTRACT Background:
10.5005/jp-journals-10007-1108 ORIGINAL ARTICLE WJOLS Laparoscopic versus Open Management of Hydatid Cyst of Liver Falih Mohssen Ali Consultant Surgeon, Basrah Teaching Hospital, Iraq ABSTRACT Background:
Scientific background concerning Echinococcus multilocularis. Muza Kirjušina, Daugavpils University, Latvia
 Scientific background concerning Echinococcus multilocularis Muza Kirjušina, Daugavpils University, Latvia Echinococcus multilocularis Infection with the larval form causes alveolar echinococcosis (AE).
Scientific background concerning Echinococcus multilocularis Muza Kirjušina, Daugavpils University, Latvia Echinococcus multilocularis Infection with the larval form causes alveolar echinococcosis (AE).
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Clinical Images Title: Huge Echinococcal
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Clinical Images Title: Huge Echinococcal
Understanding the Lifecycle of the Hydatid Tapeworm
 Hydatid Tapeworm The Hydatid Tapeworm (scientific name Echinococcus granulosis) is one of a number of tapeworms that infect dogs. The reason this tapeworm is considered the most significant is that, unlike
Hydatid Tapeworm The Hydatid Tapeworm (scientific name Echinococcus granulosis) is one of a number of tapeworms that infect dogs. The reason this tapeworm is considered the most significant is that, unlike
This is the smallest tapeworm that can affect human being but it s not really proper human tapeworm (the human is not the primary host).
 Echinococcus Granulosus Small Tapeworm (1 cm), Cestode. This is the smallest tapeworm that can affect human being but it s not really proper human tapeworm (the human is not the primary host). The primary
Echinococcus Granulosus Small Tapeworm (1 cm), Cestode. This is the smallest tapeworm that can affect human being but it s not really proper human tapeworm (the human is not the primary host). The primary
Imaging Findings in Liver Hydatidosis: Pictorial Assay
 Imaging Findings in Liver Hydatidosis: Pictorial Assay Poster No.: C-1790 Congress: ECR 2014 Type: Educational Exhibit Authors: A. S. Eksioglu, B. Ucan, E. Çakmakc#, P. S. Öztekin, M. Pala Akdogan; Ankara/TR
Imaging Findings in Liver Hydatidosis: Pictorial Assay Poster No.: C-1790 Congress: ECR 2014 Type: Educational Exhibit Authors: A. S. Eksioglu, B. Ucan, E. Çakmakc#, P. S. Öztekin, M. Pala Akdogan; Ankara/TR
LOWER EYELID RECONSTRUCTIVE SURGERY AFTER SEBACEOUS GLAND ADENOMA RESECTION IN A GERMAN SHEPHERD DOG: A CASE REPORT
 Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN Rambabu 2321 9602 Kalaka www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report LOWER EYELID RECONSTRUCTIVE
Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN Rambabu 2321 9602 Kalaka www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report LOWER EYELID RECONSTRUCTIVE
Case Report Presence of an Isolated Hydatid Cyst in the Left Kidney: Report of a Case of This Rare Condition Managed Surgically
 Case Reports in Urology Volume 2016, Article ID 6902082, 4 pages http://dx.doi.org/10.1155/2016/6902082 Case Report Presence of an Isolated Hydatid Cyst in the Left Kidney: Report of a Case of This Rare
Case Reports in Urology Volume 2016, Article ID 6902082, 4 pages http://dx.doi.org/10.1155/2016/6902082 Case Report Presence of an Isolated Hydatid Cyst in the Left Kidney: Report of a Case of This Rare
Gastric Dilatation-Volvulus
 Gastric Dilatation-Volvulus The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery. Only veterinarians who have successfully completed the certification requirements
Gastric Dilatation-Volvulus The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery. Only veterinarians who have successfully completed the certification requirements
STERILIZED NYLON MOSQUITO NET FOR RECONSTRUCTION OF UMBILICAL HERNIA IN BUFFALOES
 Case Report Buffalo Bulletin (March 2014) Vol.33 No.1 STERILIZED NYLON MOSQUITO NET FOR RECONSTRUCTION OF UMBILICAL HERNIA IN BUFFALOES Vineet Kumar*, D.D. Mathew, R.A. Ahmad, M. Hoque, A.C. Saxena, Rekha
Case Report Buffalo Bulletin (March 2014) Vol.33 No.1 STERILIZED NYLON MOSQUITO NET FOR RECONSTRUCTION OF UMBILICAL HERNIA IN BUFFALOES Vineet Kumar*, D.D. Mathew, R.A. Ahmad, M. Hoque, A.C. Saxena, Rekha
Ovarian Cancer or Hydatidosis? A Case Report
 Iran J Parasitol Tehran University of Medical Sciences Publication http://tums.ac.ir Open access Journal at http://ijpa.tums.ac.ir Iranian Society of Parasitology http://isp.tums.ac.ir Case Report Ovarian
Iran J Parasitol Tehran University of Medical Sciences Publication http://tums.ac.ir Open access Journal at http://ijpa.tums.ac.ir Iranian Society of Parasitology http://isp.tums.ac.ir Case Report Ovarian
General introduction
 Spirometra mansoni General introduction Distributed worldwide, mainly in southeast Asia. Larval infection of S. mansoni may cause serious clinical disease ---Sparganosis Morphology Adult worm measures
Spirometra mansoni General introduction Distributed worldwide, mainly in southeast Asia. Larval infection of S. mansoni may cause serious clinical disease ---Sparganosis Morphology Adult worm measures
International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME)
 International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) CLINICAL STUDY OF HYDATID CYST IN SOUTH RAJASTHAN Dr. Vinod Kumar
International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) CLINICAL STUDY OF HYDATID CYST IN SOUTH RAJASTHAN Dr. Vinod Kumar
Echinococcus multilocularis Diagnosis. Peter Deplazes. Medical Faculty. Swiss TPH Winter Symposium 2017
 Medical Faculty Swiss TPH Winter Symposium 2017 Helminth Infection from Transmission to Control Echinococcus multilocularis Diagnosis Peter Deplazes Global distribution of E. multilocularis Deplazes et
Medical Faculty Swiss TPH Winter Symposium 2017 Helminth Infection from Transmission to Control Echinococcus multilocularis Diagnosis Peter Deplazes Global distribution of E. multilocularis Deplazes et
Eight SH cases were assessed at our Department
 POLSKI PRZEGLĄD CHIRURGICZNY 2011, 83, 5, 271 275 10.2478/v10035-011-0042-4 Jose Manuel Ramia-Angel 1, Andrzej Gasz 2, Roberto de la Plaza-Llamas 1, JoseQuinones-Sampedro 1, Eloy Sancho 2, Jorge Garcia
POLSKI PRZEGLĄD CHIRURGICZNY 2011, 83, 5, 271 275 10.2478/v10035-011-0042-4 Jose Manuel Ramia-Angel 1, Andrzej Gasz 2, Roberto de la Plaza-Llamas 1, JoseQuinones-Sampedro 1, Eloy Sancho 2, Jorge Garcia
Hydatid Cyst Dr. Nora L. El-Tantawy
 Hydatid Cyst Dr. Nora L. El-Tantawy Ass. Prof. of Parasitology Faculty of Medicine, Mansoura university, Egypt Echinococcus granulosus Geographical Distribution: cosmopolitan especially in sheep raising
Hydatid Cyst Dr. Nora L. El-Tantawy Ass. Prof. of Parasitology Faculty of Medicine, Mansoura university, Egypt Echinococcus granulosus Geographical Distribution: cosmopolitan especially in sheep raising
ECHINOCOCCAL DISEASE OF THE LIVER IN PREGNANCY
 HPB Surgery 1990, Vol. 2 pp. 115-119 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom ECHINOCOCCAL
HPB Surgery 1990, Vol. 2 pp. 115-119 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom ECHINOCOCCAL
PERCUTANEOUS CYST DRAINAGE AS A BRIDGE TO SURGERY FOR HYDATID INTESTINAL OBSTRUCTION
 PERCUTANEOUS CYST DRAINAGE AS A BRIDGE TO SURGERY FOR HYDATID INTESTINAL OBSTRUCTION Jaiteh L 1, Benkabbou A 2, Hama Y 1, Hachim H 1, Souadka A 2, El-Malki H. O 1, Chefchaouni M 1, Ifrine L 1, Belkouchi
PERCUTANEOUS CYST DRAINAGE AS A BRIDGE TO SURGERY FOR HYDATID INTESTINAL OBSTRUCTION Jaiteh L 1, Benkabbou A 2, Hama Y 1, Hachim H 1, Souadka A 2, El-Malki H. O 1, Chefchaouni M 1, Ifrine L 1, Belkouchi
Breast Mass on Mammography
 Breast Mass on Mammography Bobbi Pritt, MD 2014 MFMER slide-1 Clinical Presentation 68 year old woman was noted to have 2 adjacent masses in the right breast on screening mammography Well-circumscribed,
Breast Mass on Mammography Bobbi Pritt, MD 2014 MFMER slide-1 Clinical Presentation 68 year old woman was noted to have 2 adjacent masses in the right breast on screening mammography Well-circumscribed,
Presentation of Quiz #85
 Presentation of Quiz #85 ***Reminder: Slides are copyrighted and cannot be copied for publication. A 36 year old male from Columbia was admitted to the hospital with seizures. This patient had previously
Presentation of Quiz #85 ***Reminder: Slides are copyrighted and cannot be copied for publication. A 36 year old male from Columbia was admitted to the hospital with seizures. This patient had previously
Case Report Primary Hydatid Cyst of the Axillary Region: A Case Report
 Case Reports in Medicine Volume 2012, Article ID 362610, 4 pages doi:10.1155/2012/362610 Case Report Primary Hydatid Cyst of the Axillary Region: A Case Report Mehrangiz Zangeneh, 1 Mahmood Amerion, 2
Case Reports in Medicine Volume 2012, Article ID 362610, 4 pages doi:10.1155/2012/362610 Case Report Primary Hydatid Cyst of the Axillary Region: A Case Report Mehrangiz Zangeneh, 1 Mahmood Amerion, 2
3 PG student, Department of General Surgery, B J Medical College, Ahmedabad, India
 surgery in cases of liver hydatid cyst Original Research Article ISSN: 294-0026 (P) ISSN: 294-004 (O) Comparative study of laparoscopicc versus open surgery in 42 cases of liver hydatid cyst K. A. Bhadreshwara,
surgery in cases of liver hydatid cyst Original Research Article ISSN: 294-0026 (P) ISSN: 294-004 (O) Comparative study of laparoscopicc versus open surgery in 42 cases of liver hydatid cyst K. A. Bhadreshwara,
The Role of Wildlife Rehabilitation as Sentinels for One Health Issues at the Wildlife and Public Health Interface:
 The Role of Wildlife Rehabilitation as Sentinels for One Health Issues at the Wildlife and Public Health Interface: Reports of Taenia crassiceps Cysticercosis in Woodchucks (Marmota monax) and Squirrels
The Role of Wildlife Rehabilitation as Sentinels for One Health Issues at the Wildlife and Public Health Interface: Reports of Taenia crassiceps Cysticercosis in Woodchucks (Marmota monax) and Squirrels
Obstructive jaundice secondary to postsurgical persistent residual hydatid ectocyst of left lobe of liver
 www.edoriumjournals.com case REPORT OPEN ACCESS Obstructive jaundice secondary to postsurgical persistent residual hydatid ectocyst of left lobe of liver Maulana M. Ansari, Shahla Haleem, Wasif M. Ali,
www.edoriumjournals.com case REPORT OPEN ACCESS Obstructive jaundice secondary to postsurgical persistent residual hydatid ectocyst of left lobe of liver Maulana M. Ansari, Shahla Haleem, Wasif M. Ali,
Evaluation and comparison of the outcomes of open and laparoscopic surgery of liver hydatid cyst
 Original Research Article Evaluation and comparison of the outcomes of open and laparoscopic surgery of liver hydatid cyst Nilesh J. Patel 1, Hitesh P. Khandra 2*, Shobhit R. Chhabra 3, Chouhan Bhanu Pratap
Original Research Article Evaluation and comparison of the outcomes of open and laparoscopic surgery of liver hydatid cyst Nilesh J. Patel 1, Hitesh P. Khandra 2*, Shobhit R. Chhabra 3, Chouhan Bhanu Pratap
NEPHRON SPARING SURGERY IN RENAL HYDATIDOSIS: AN EXPERIENCE Sajad Ahmad Malik 1, Rouf Khawaja 2, Sahil 3, M. Saleem Wani 4, Arif Hameed 5
 NEPHRON SPARING SURGERY IN RENAL HYDATIDOSIS: AN EXPERIENCE Sajad Ahmad Malik 1, Rouf Khawaja 2, Sahil 3, M. Saleem Wani 4, Arif Hameed 5 HOW TO CITE THIS ARTICLE: Sajad Ahmad Malik, Rouf Khawaja, Sahil,
NEPHRON SPARING SURGERY IN RENAL HYDATIDOSIS: AN EXPERIENCE Sajad Ahmad Malik 1, Rouf Khawaja 2, Sahil 3, M. Saleem Wani 4, Arif Hameed 5 HOW TO CITE THIS ARTICLE: Sajad Ahmad Malik, Rouf Khawaja, Sahil,
Hydatid disease of the liver: A 12 year experience of surgical management
 Hydatid disease of the liver: A 12 year experience of surgical management 54 Hagos Biluts, Mesfin Minas, Abebe Bekele Department of surgery, MF, AAU. Correspondence to: Dr Hagos Biluts, Tikur Anbessa Hospital,
Hydatid disease of the liver: A 12 year experience of surgical management 54 Hagos Biluts, Mesfin Minas, Abebe Bekele Department of surgery, MF, AAU. Correspondence to: Dr Hagos Biluts, Tikur Anbessa Hospital,
Cystic echinococcosis in a domestic cat: an Italian case report
 13th NRL Workshop, Rome, 24-25 May, 2018 Cystic echinococcosis in a domestic cat: an Italian case report Istituto Zooprofilattico Sperimentale (IZS) of Sardinia National Reference Laboratory for Cistic
13th NRL Workshop, Rome, 24-25 May, 2018 Cystic echinococcosis in a domestic cat: an Italian case report Istituto Zooprofilattico Sperimentale (IZS) of Sardinia National Reference Laboratory for Cistic
Surgical Cross Coder. Essential links from CPT codes to ICD-9-CM and HCPCS codes
 Essential links from CPT codes to ICD-9-CM and HCPCS codes 2016 Contents Introduction... iii Cardiovascular System...527 Digestive System...707 General...1 Integumentary System...9 Musculoskeletal System...173
Essential links from CPT codes to ICD-9-CM and HCPCS codes 2016 Contents Introduction... iii Cardiovascular System...527 Digestive System...707 General...1 Integumentary System...9 Musculoskeletal System...173
Intact germinal layer of liver hydatid cysts removed after administration of albendazole
 C a s e r e p o r t Intact germinal layer of liver hydatid cysts removed after administration of albendazole A. Manouras *, M. Genetzakis, E.E. Lagoudianakis, A. Papadima, C. Triantafillou, P.V. Kekis,
C a s e r e p o r t Intact germinal layer of liver hydatid cysts removed after administration of albendazole A. Manouras *, M. Genetzakis, E.E. Lagoudianakis, A. Papadima, C. Triantafillou, P.V. Kekis,
Specialist Referral Service Willows Information Sheets. Rigid endoscopy
 Specialist Referral Service Willows Information Sheets Rigid endoscopy Professor Rob White with a state-of-the-art rigid Karl Storz endoscope. Rigid endoscopy What is endoscopy? Endoscopy involves the
Specialist Referral Service Willows Information Sheets Rigid endoscopy Professor Rob White with a state-of-the-art rigid Karl Storz endoscope. Rigid endoscopy What is endoscopy? Endoscopy involves the
by author Cystic Echinococcosis Rogelio López-Vélez MD, DTM&H, PhD National Referral Unit for Tropical Diseases Infectious Diseases Department
 Cystic Echinococcosis Rogelio López-Vélez MD, DTM&H, PhD National Referral Unit for Tropical Diseases Infectious Diseases Department Ramón y Cajal University Hospital. Madrid. Spain National Referral Unit
Cystic Echinococcosis Rogelio López-Vélez MD, DTM&H, PhD National Referral Unit for Tropical Diseases Infectious Diseases Department Ramón y Cajal University Hospital. Madrid. Spain National Referral Unit
Chronic Hydatid Cyst in Malaysia: A Rare Occurence
 Case Report Chronic Hydatid Cyst in : A Rare Occurence Md Pauzi Suria Hayati 1, Chan Boon Teck Eugene 2, Bong Jan Jin 3, Isa Mohd Rose 4 Submitted: 27 Feb 2014 Accepted: 17 Apr 2014 1 Department of Pathology,
Case Report Chronic Hydatid Cyst in : A Rare Occurence Md Pauzi Suria Hayati 1, Chan Boon Teck Eugene 2, Bong Jan Jin 3, Isa Mohd Rose 4 Submitted: 27 Feb 2014 Accepted: 17 Apr 2014 1 Department of Pathology,
Unusual Presentations of Hydatid Cyst - A Case Study
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/193 Unusual Presentations of Hydatid Cyst - A Case Study Girish K Kullolli 1, Manoj K Vaidya 2, Roshini Patil 2 1 Associate
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/193 Unusual Presentations of Hydatid Cyst - A Case Study Girish K Kullolli 1, Manoj K Vaidya 2, Roshini Patil 2 1 Associate
Bulgarian Journal of Veterinary Medicine (2007), 10, No 1, Summary
 Bulgarian Journal of Veterinary Medicine (2007), 10, No 1, 45 51 IMAGING (ULTRASONOGRAPHY, COMPUTED TOMOGRAPHY) OF PATIENTS WITH HYDATID LIVER DISEASE K. KALINOVA Summary Department of General and Pediatric
Bulgarian Journal of Veterinary Medicine (2007), 10, No 1, 45 51 IMAGING (ULTRASONOGRAPHY, COMPUTED TOMOGRAPHY) OF PATIENTS WITH HYDATID LIVER DISEASE K. KALINOVA Summary Department of General and Pediatric
Primary Hydatid Cyst of the Right Maxillary Sinus: A Case Report
 Case Report Iranian Journal of Otorhinolaryngology, Vol.26(4), Serial No.77, Oct 2014 Abstract Primary Hydatid Cyst of the Right Maxillary Sinus: A Case Report Ali Reza Lotfi 1, * Sina Zarrintan 2, Masoud
Case Report Iranian Journal of Otorhinolaryngology, Vol.26(4), Serial No.77, Oct 2014 Abstract Primary Hydatid Cyst of the Right Maxillary Sinus: A Case Report Ali Reza Lotfi 1, * Sina Zarrintan 2, Masoud
Schistosoma mansoni, S. japonicum, S. haematobium
 Schistosoma mansoni, S. japonicum, S. haematobium The Organisms More than 200 million people are infected worldwide with Schistosoma species. The adult worms are long and slender (males are 6 12 mm in
Schistosoma mansoni, S. japonicum, S. haematobium The Organisms More than 200 million people are infected worldwide with Schistosoma species. The adult worms are long and slender (males are 6 12 mm in
Pectus Excavatum (Funnel Chest) Dr Hasan Nugud Consultant Paediatric Surgeon
 Pectus Excavatum (Funnel Chest) Dr Hasan Nugud Consultant Paediatric Surgeon Pectus excavatum Pectus excavatum (PE) is an abnormal development of the rib cage where the breastbone (sternum) caves in,
Pectus Excavatum (Funnel Chest) Dr Hasan Nugud Consultant Paediatric Surgeon Pectus excavatum Pectus excavatum (PE) is an abnormal development of the rib cage where the breastbone (sternum) caves in,
ON THE TRANSPLANTABILITY OF THE LARVA OF TEh'IA CRASSICOLLIS AND THE PROBABLE R~LE OF THE LIVER IN CYSTICERCUS DISEASE OF RATS
 ON THE TRANSPLANTABILITY OF THE LARVA OF TEh'IA CRASSICOLLIS AND THE PROBABLE R~LE OF THE LIVER IN CYSTICERCUS DISEASE OF RATS E'. 1). BULLOCI< AND M. 1%. CURTIS (Prom Coltil?lhin Uiiroersity, Iiistitute
ON THE TRANSPLANTABILITY OF THE LARVA OF TEh'IA CRASSICOLLIS AND THE PROBABLE R~LE OF THE LIVER IN CYSTICERCUS DISEASE OF RATS E'. 1). BULLOCI< AND M. 1%. CURTIS (Prom Coltil?lhin Uiiroersity, Iiistitute
Malignant Mixed Mammary Tumor in a German Shepherd Middle Age Bitch
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 7 (2017) pp. 572-576 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.607.069
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 7 (2017) pp. 572-576 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.607.069
DISEASE MONITORING AND EXTENSION SYSTEM FOR THE SOUTH AFRICAN DAIRY INDUSTRY
 DISEASE MONITORING AND EXTENSION SYSTEM FOR THE SOUTH AFRICAN DAIRY INDUSTRY Disease Trend Report: July 2014 IN THIS ISSUE: 1. Preface Importance of disease monitoring. 2. Get the vaccination plan in place
DISEASE MONITORING AND EXTENSION SYSTEM FOR THE SOUTH AFRICAN DAIRY INDUSTRY Disease Trend Report: July 2014 IN THIS ISSUE: 1. Preface Importance of disease monitoring. 2. Get the vaccination plan in place
Percutaneous Treatment of a Primary Pancreatic Hydatid Cyst Using a Catheterization Technique
 Case Report http://dx.doi.org/10.3348/kjr.2012.13.2.232 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(2):232-236 Percutaneous Treatment of a Primary Pancreatic Hydatid Cyst Using a Catheterization
Case Report http://dx.doi.org/10.3348/kjr.2012.13.2.232 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(2):232-236 Percutaneous Treatment of a Primary Pancreatic Hydatid Cyst Using a Catheterization
SHORT RESEARCH NOTE. Anca Florea 1. , Liviu Vlad 2, Vasile Cozma 3, Zoe Coroiu 4. Introduction
 Serological diagnosis of cystic echinococcosis by the ELISA technique, in the cases hospitalized in the Surgical Clinic no. III and Internal Medicine no. III of Cluj-Napoca, during October 2006 December
Serological diagnosis of cystic echinococcosis by the ELISA technique, in the cases hospitalized in the Surgical Clinic no. III and Internal Medicine no. III of Cluj-Napoca, during October 2006 December
Laparoscopische chirurgie bij het pancreascarcinoom: wat is de winst voor de patient?
 Laparoscopische chirurgie bij het pancreascarcinoom: wat is de winst voor de patient? Marc Besselink, Thijs de Rooij m.g.besselink@amc.nl www.pancreaskanker.nl Conflict of interest Projects described are
Laparoscopische chirurgie bij het pancreascarcinoom: wat is de winst voor de patient? Marc Besselink, Thijs de Rooij m.g.besselink@amc.nl www.pancreaskanker.nl Conflict of interest Projects described are
Emergence of Echinococcus multilocularis in dogs in Ontario: implications for public and wildlife health?
 Emergence of Echinococcus multilocularis in dogs in Ontario: implications for public and wildlife health? Andrew S. Peregrine 1, Jonathon Kotwa 1, Claire Jardine 1, Benoît Cuq 1, Nicola Mercer 2, Bruno
Emergence of Echinococcus multilocularis in dogs in Ontario: implications for public and wildlife health? Andrew S. Peregrine 1, Jonathon Kotwa 1, Claire Jardine 1, Benoît Cuq 1, Nicola Mercer 2, Bruno
THE STRUCTURE OF ECHINOCOCCAL CYSTS AND HISTOPATHOLOGICAL CHANGES IN LIVER
 THE STRUCTURE OF ECHINOCOCCAL CYSTS AND HISTOPATHOLOGICAL CHANGES IN LIVER Michal Juszynski Helena Palenga, Danuta Cielecka PhD Department of General Biology and Parasitology Medical University of Warsaw
THE STRUCTURE OF ECHINOCOCCAL CYSTS AND HISTOPATHOLOGICAL CHANGES IN LIVER Michal Juszynski Helena Palenga, Danuta Cielecka PhD Department of General Biology and Parasitology Medical University of Warsaw
CASE REPORT CONTROVERSY IN THE MANAGEMENT OF CHOLANGITIS SECONDARY TO HYDATID DAUGHTER CYSTS
 HPB Surgery, 1991, Vol. 4, pp 321-329 Reprints available directly from the publisher Photocopying permitted by license only 1991 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1991, Vol. 4, pp 321-329 Reprints available directly from the publisher Photocopying permitted by license only 1991 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
Modalities Of Treatment Of Hepatic Hydatid Cyst
 International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 3-2018 Research Article DOI: http://dx.doi.org/10.22192/ijamr.2018.05.03.004
International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 3-2018 Research Article DOI: http://dx.doi.org/10.22192/ijamr.2018.05.03.004
Treatment of septic peritonitis
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
New treatments for manges in dogs? Canine demodicosis. Canine demodicosis. Current approved drug in Canada:
 New treatments for manges in dogs? Andrew S. Peregrine, BVMS, PhD, DVM, DipEVPC, DipACVM E-mail: aperegri@ovc.uoguelph.ca; Tel: 519-824-4120 ext 54714 Canine demodicosis Most common = D. canis No difference
New treatments for manges in dogs? Andrew S. Peregrine, BVMS, PhD, DVM, DipEVPC, DipACVM E-mail: aperegri@ovc.uoguelph.ca; Tel: 519-824-4120 ext 54714 Canine demodicosis Most common = D. canis No difference
Clinical Programme. Dermatology
 2018 The diagnosis and management of skin represents a major component of small animal practice. Through lectures, case discussions and practical sessions, this modular programme will enable you to learn
2018 The diagnosis and management of skin represents a major component of small animal practice. Through lectures, case discussions and practical sessions, this modular programme will enable you to learn
On the Occurrence and Significance of Hydatid Cysts in the Ceylon Sambhur Rusa unicolor unicolor.*
 CEYLON J. MBD. SCI. (D) Vol. XI, Pt. 1 (May 1962) On the Occurrence and Significance of Hydatid Cysts in the Ceylon Sambhur Rusa unicolor unicolor.* by A. S. DISSANAIKE AND D. C. PARAMANANTHAN** Department
CEYLON J. MBD. SCI. (D) Vol. XI, Pt. 1 (May 1962) On the Occurrence and Significance of Hydatid Cysts in the Ceylon Sambhur Rusa unicolor unicolor.* by A. S. DISSANAIKE AND D. C. PARAMANANTHAN** Department
Primary splenic echinococcal cyst: a rare presentation
 Case Report Brunei Int Med J. 2013; 9 (5): 345-349 Primary splenic echinococcal cyst: a rare presentation Pinki PANDEY 1, A DIXIT 2, S CHANDRA 1, V CHATURVEDI 1, Anuradha SHARMA 3 1 Departments of Pathology
Case Report Brunei Int Med J. 2013; 9 (5): 345-349 Primary splenic echinococcal cyst: a rare presentation Pinki PANDEY 1, A DIXIT 2, S CHANDRA 1, V CHATURVEDI 1, Anuradha SHARMA 3 1 Departments of Pathology
LEPTOSPIROSIS. Understanding the risk to your dog
 LEPTOSPIROSIS Understanding the risk to your dog What is leptospirosis? Leptospirosis is an infectious disease that causes serious illness in dogs, other animals, and people throughout the US and around
LEPTOSPIROSIS Understanding the risk to your dog What is leptospirosis? Leptospirosis is an infectious disease that causes serious illness in dogs, other animals, and people throughout the US and around
Report and Opinion 2017;9(11) Birara Ayalneh 1, Balemual Abebaw 2
 Major causes of organ condemnation in cattle and sheep slaughtered at Motta abattoir North-West Ethiopia. Birara Ayalneh 1, Balemual Abebaw 2 1. College of Veterinary Medicine and Animal Science, Department
Major causes of organ condemnation in cattle and sheep slaughtered at Motta abattoir North-West Ethiopia. Birara Ayalneh 1, Balemual Abebaw 2 1. College of Veterinary Medicine and Animal Science, Department
Contains most of the medically important tapeworms Scolex has 4 suckers and compact vitelline gland are characteristic Range from mm to >10m
 Cyclophyllidae Contains most of the medically important tapeworms Scolex has 4 suckers and compact vitelline gland are characteristic Range from mm to >10m Family Taeniidae Taenia saginata: beef tapeworm
Cyclophyllidae Contains most of the medically important tapeworms Scolex has 4 suckers and compact vitelline gland are characteristic Range from mm to >10m Family Taeniidae Taenia saginata: beef tapeworm
Surgery of pulmonary hydatid cystthe Barrett technique
 Surgery of pulmonary hydatid cystthe Barrett technique IVAN LICHTER Department of Surgery, University of Otago Medical School, Dunedin, New Zealand Thorax (1972), 27, 529. A number of methods have been
Surgery of pulmonary hydatid cystthe Barrett technique IVAN LICHTER Department of Surgery, University of Otago Medical School, Dunedin, New Zealand Thorax (1972), 27, 529. A number of methods have been
Human Hydatidosis in the Central Andes of Peru: Evolution of the Disease over 3 Years
 807 Human Hydatidosis in the Central Andes of Peru: Evolution of the Disease over 3 Years Pedro L. Moro, Robert H. Gilman, Manuela Verastegui, Caryn Bern, Bernave Silva, and Juan J. Bonilla From the Asociación
807 Human Hydatidosis in the Central Andes of Peru: Evolution of the Disease over 3 Years Pedro L. Moro, Robert H. Gilman, Manuela Verastegui, Caryn Bern, Bernave Silva, and Juan J. Bonilla From the Asociación
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance
 Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Australian and New Zealand College of Veterinary Scientists. Fellowship Examination. Small Animal Surgery Paper 1
 Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2017 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2017 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer
Restore life and vitality in your dog. Feel the same results as an owner.
 Restore life and vitality in your dog. Feel the same results as an owner. Your dog, Cushing s syndrome and you This booklet has been designed to help answer questions that you may have about Cushing s
Restore life and vitality in your dog. Feel the same results as an owner. Your dog, Cushing s syndrome and you This booklet has been designed to help answer questions that you may have about Cushing s
Guard against intestinal worms with Palatable All-wormer
 Guard against intestinal worms with Palatable All-wormer WHIPWORMS HOOKWORMS TAPEWORMS ROUNDWORMS Palatable All-wormer, for superior, flexible protection of dogs and cats. GENTLE ON PETS, TOUGH ON WORMS.
Guard against intestinal worms with Palatable All-wormer WHIPWORMS HOOKWORMS TAPEWORMS ROUNDWORMS Palatable All-wormer, for superior, flexible protection of dogs and cats. GENTLE ON PETS, TOUGH ON WORMS.
Fertility of Hydatid Cysts and Viability of Protoscoleces in Slaughtered Animals in Qazvin, Iran
 Journal of Agricultural Science; Vol. 5, No. 1; 2013 ISSN 1916-9752 E-ISSN 1916-9760 Published by Canadian Center of Science and Education Fertility of Hydatid Cysts and Viability of Protoscoleces in Slaughtered
Journal of Agricultural Science; Vol. 5, No. 1; 2013 ISSN 1916-9752 E-ISSN 1916-9760 Published by Canadian Center of Science and Education Fertility of Hydatid Cysts and Viability of Protoscoleces in Slaughtered
National Research Center
 National Research Center Update of immunodiagnosis of cystic echinococcosis cysts Global distribution of zoonotic strains of Echinococcus granulosus (Adapted from Eckert and Deplazes, 2004) Echinococcus
National Research Center Update of immunodiagnosis of cystic echinococcosis cysts Global distribution of zoonotic strains of Echinococcus granulosus (Adapted from Eckert and Deplazes, 2004) Echinococcus
International Journal of Scientific Research and Reviews
 Case Study Available online www.ijsrr.org ISSN: 2279 0543 International Journal of Scientific Research and Reviews Primary Hydatid Disease of the Uterus A Case Report Iyer Rekha R. *1, Tyagi M. S. 2*,
Case Study Available online www.ijsrr.org ISSN: 2279 0543 International Journal of Scientific Research and Reviews Primary Hydatid Disease of the Uterus A Case Report Iyer Rekha R. *1, Tyagi M. S. 2*,
Restore life and vitality in your dog. Feel the same results as an owner.
 Restore life and vitality in your dog. Feel the same results as an owner. Your dog, Cushing s syndrome and you This booklet has been designed to help answer questions that you may have about Cushing s
Restore life and vitality in your dog. Feel the same results as an owner. Your dog, Cushing s syndrome and you This booklet has been designed to help answer questions that you may have about Cushing s
A placebo controlled study of albendazole in the treatment of pulmonary echinococcosis
 Eur Respir J 1999; 14: 503±507 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 A placebo controlled study of albendazole in the of pulmonary
Eur Respir J 1999; 14: 503±507 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 A placebo controlled study of albendazole in the of pulmonary
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Small Animal Medicine Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
A simple guide to the post mortem examination procedure
 A simple guide to the post mortem examination procedure Crown copyright 2003 Produced by the Department of Health 29770 1p 50k Apr 03 (XXX) CHLORINE FREE PAPER The text of this document may be reproduced
A simple guide to the post mortem examination procedure Crown copyright 2003 Produced by the Department of Health 29770 1p 50k Apr 03 (XXX) CHLORINE FREE PAPER The text of this document may be reproduced
Any Animal. Section G. General Conditions (many different animals) Sicknesses seen on the outside of the animal. Injuries.
 Section G General Conditions (many different animals) Sicknesses seen on the outside of the animal Injuries Photo credit: Dr. M. Cattet See Section G-1.1 Emaciation See Section G-1.2 Photo credit: WCVM
Section G General Conditions (many different animals) Sicknesses seen on the outside of the animal Injuries Photo credit: Dr. M. Cattet See Section G-1.1 Emaciation See Section G-1.2 Photo credit: WCVM
Anesthesia Check-off Form
 Anesthesia Check-off Form 5231 SW 91st Drive Gainesville, FL 32608 (352) 377-6003 The doctors and staff at Haile Plantation Animal Clinic would like to offer the most advanced medical care and services
Anesthesia Check-off Form 5231 SW 91st Drive Gainesville, FL 32608 (352) 377-6003 The doctors and staff at Haile Plantation Animal Clinic would like to offer the most advanced medical care and services
5/17/2012 DISCLOSURES OBJECTIVES CONTEMPORARY PEDIATRICS
 CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
CONTEMPORARY PEDIATRICS Surgical Management of MRSA Soft Tissue Infections John M. Draus, Jr., M.D. Assistant Professor of Surgery and Pediatrics Kentucky Children s Hospital University of Kentucky DISCLOSURES
Understanding your pet s LIVER CONDITION
 Understanding your pet s LIVER CONDITION Why is the liver so important? What causes liver disease in dogs and cats? The liver is one of the largest organs in your pet s body, and it s vital for their good
Understanding your pet s LIVER CONDITION Why is the liver so important? What causes liver disease in dogs and cats? The liver is one of the largest organs in your pet s body, and it s vital for their good
PARASITOLOGICAL EXAMINATIONS CATALOGUE OF SERVICES AND PRICE LIST
 INSTITUTE OF PARASITOLOGY Biomedical Research Center Seltersberg Justus Liebig University Giessen Schubertstrasse 81 35392 Giessen Germany Office: +49 (0) 641 99 38461 Fax: +49 (0) 641 99 38469 Coprological
INSTITUTE OF PARASITOLOGY Biomedical Research Center Seltersberg Justus Liebig University Giessen Schubertstrasse 81 35392 Giessen Germany Office: +49 (0) 641 99 38461 Fax: +49 (0) 641 99 38469 Coprological
Your Pet s Surgery. What happens on the day and follow up care
 Your Pet s Surgery What happens on the day and follow up care Surgery at Coastway We ve produced this short guide for owners of pets who are having a surgical procedure with us, to explain and reassure
Your Pet s Surgery What happens on the day and follow up care Surgery at Coastway We ve produced this short guide for owners of pets who are having a surgical procedure with us, to explain and reassure
Albendazole for pinworms
 Albendazole for pinworms Detailed Albendazole dosage information for adults and TEENren. Includes dosages for Ascariasis, Pinworm Infection (Enterobius vermicularis), Hookworm Infection. Best sale albendazole
Albendazole for pinworms Detailed Albendazole dosage information for adults and TEENren. Includes dosages for Ascariasis, Pinworm Infection (Enterobius vermicularis), Hookworm Infection. Best sale albendazole
INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE
 INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE CYSTIC ECHINOCOCCOSIS OF THE LIVER A CASE REPORT DR. S.VENKATESWARA RAO, 1 DR. BASETTY NAGARAJA, 2 DR. MUCHUKOTA BABU 3 1. Assistant Professor,
INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE CYSTIC ECHINOCOCCOSIS OF THE LIVER A CASE REPORT DR. S.VENKATESWARA RAO, 1 DR. BASETTY NAGARAJA, 2 DR. MUCHUKOTA BABU 3 1. Assistant Professor,
Medical Conditions Questionnaire
 Medical Conditions Questionnaire (to be completed by the member) Member Full Name.Date of birth. Policy number or scheme name. Please complete the appropriate section(s) only after completing the Member
Medical Conditions Questionnaire (to be completed by the member) Member Full Name.Date of birth. Policy number or scheme name. Please complete the appropriate section(s) only after completing the Member
ALBENDAZOLE AND ITS ANALOGUES
 ALBENDAZOLE AND ITS ANALOGUES J. El harti *, M. Ansar, J. Taoufik. Laboratory of Medicinal Chemistry, Faculty of Medicine and Pharmacy, BP 6203, Rabat Institute, University Mohammed V Souissi, Rabat, Morocco.
ALBENDAZOLE AND ITS ANALOGUES J. El harti *, M. Ansar, J. Taoufik. Laboratory of Medicinal Chemistry, Faculty of Medicine and Pharmacy, BP 6203, Rabat Institute, University Mohammed V Souissi, Rabat, Morocco.
Trabajos Originales 75
 Trabajos Originales 75 article_file Click here to download Manuscript: article_file.doc 1 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Title Surveillance of Human Echinococcosis
Trabajos Originales 75 article_file Click here to download Manuscript: article_file.doc 1 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Title Surveillance of Human Echinococcosis
