Hepatic diseases are relatively common in cats.
|
|
|
- Rosamond Phelps
- 5 years ago
- Views:
Transcription
1 J Vet Intern Med 2006;20: High Complication Rate of an Automatic Tru-Cut Biopsy Gun Device for Liver Biopsy in Cats S.J.M. Proot and J. Rothuizen Background: Liver biopsies taken with an automatic Tru-Cut biopsy gun device caused unexpected fatal shock reactions in cats. The goal of the present study was to determine if this biopsy device caused more frequent fatal complications than did a semiautomatic device. Animals: All cats referred to the Utrecht University, between October 1, 2002, and October 31, 2004, in which ultrasoundguided Tru-Cut liver biopsies were taken. The indications for liver biopsy were increased liver enzyme activity, increased bile acid concentrations, ultrasonographic abnormalities of the liver, ultrasonographic abnormalities of the bile ducts, or some combination of these findings. Coagulation parameters were normal. Methods: From October 1, 2002, until October 31, 2003, 26 cats were biopsied with an automatic biopsy device. Between November 1, 2003, and October 31, 2004, 19 cats underwent liver biopsy with a semiautomatic biopsy device. Results: In the first period, 5 of the 26 cats (19%) developed severe shock within 15 minutes. Resuscitation was not successful. In the second period, none of the 19 cats experienced any major adverse effect. There were no significant differences between the 2 groups with respect to diagnosis, clinical signs, clinicopathologic findings, or the use of anesthetics. Conclusions and Clinical Importance: We conclude that the difference in complication rate is explained by the biopsy technique used. The pressure wave, which occurs when firing the automatic device, may have caused intense vagotonia and shock. Use of this automatic biopsy device should be avoided in cats because of the high risk of fatal complications. Key words: Fatal risk; Cat; Liver disease; Vagal shock. Hepatic diseases are relatively common in cats. Depending on the geographic location, cholangiohepatitis or idiopathic hepatic lipidosis is regarded as the most common hepatic disorder of cats. In the United States, hepatic lipidosis seems to be most common, while in the UK and Europe, neutrophilic or lymphocytic cholangitis is most common. 1 Other hepatic disorders of cats are feline infectious peritonitis (FIP), neoplasia, and amyloidosis. Ultrasonographic findings can be suggestive but are not diagnostic for any of these diseases. Fine needle aspiration biopsies often are helpful in diagnosing lipidosis, steroid-induced hepatopathy, and lymphoma, but histology of liver biopsies is required to diagnose most liver diseases. 2 Biopsies can be performed under ultrasound guidance or during laparoscopy or laparotomy. A surgical approach allows macroscopic evaluation of the liver, yields larger biopsy samples, and enables control of postbiopsy hemorrhage, but these techniques are more invasive. In contrast, ultrasoundguided biopsy is much less invasive and also permits visualization of the liver, bile ducts, biopsy tract, and the occurrence of hemorrhage. At the Companion Animal Clinic of Utrecht University, most liver biopsies in cats are performed under ultrasound guidance unless surgery is warranted for a specific reason. In the past, we used a semiautomatic 16G VET-core biopsy needle a (Fig 1). Because of the high costs, we From the Department of Clinical Sciences of Companion Animals, Faculty of Veterinary Medicine, University Utrecht, Utrecht, The. Reprint requests: Sarah J.M. Proot, DVM, Department of Clinical Sciences of Companion Animals, Faculty of Veterinary Medicine, University Utrecht, P.O. Box , 3508 TD Utrecht, The ; S.J.M.Proot@vet.uu.nl. Submitted March 3, 2003; Revised May 9, 2006; Accepted June 30, Copyright E 2006 by the American College of Veterinary Internal Medicine /06/ /$3.00/0 have replaced this method with a less expensive automatic biopsy device, the Pro-Mag Ultra Automatic Biopsy Instrument b (Fig 2). This device has been used for many years to perform biopsies in dogs and has been a safe and suitable instrument in our experience. The better size and quality of the biopsy samples obtained with this device was another reason to consider this method in cats. 3 However, experience indicated that some cats developed fatal hypotensive shock reactions after biopsies were performed with the16g device, in contrast to the semiautomatic device. The aim of this study was to evaluate whether collection of 16G Tru-Cut biopsy samples with an automatic biopsy device causes more complications than collection of biopsy samples with a semiautomatic device of identical diameter. Materials and Methods Cases We reviewed all cases from October 1, 2002, until October 31, 2004, in which ultrasound-guided Tru-Cut liver biopsies were performed in cats referred to the University of Utrecht. Reasons for referral were liver-related clinical signs (eg, general malaise, lethargy, anorexia, vomiting, weight loss, jaundice), increased liver enzyme activities, increased bile acid concentrations, ultrasonographic abnormalities, or some combination of these findings. Between October 1, 2002, and October 31, 2003, biopsies were performed with an automatic biopsy device b on 26 occasions. One cat underwent biopsy twice with an interval of 1 month. In another cat, a hepatic mass was biopsied, and 3 weeks later other locations within the diffusely abnormal liver also were biopsied. We considered each biopsy as a separate case for statistical analysis. Between November 1, 2003, and October 31, 2004, biopsies were performed with a semiautomatic VET-core biopsy needle a on 19 occasions. During this period, 1 cat underwent biopsy 3 times with intervals of 1 and 2 months, respectively. Clinical Database All cats were examined physically. In most cats, CBC and biochemical analysis (especially liver enzyme activities and bile acid
2 1328 Proot and Rothuizen Fig 2. gun). Pro-Mag Ultra Automatic Biopsy Instrument (biopsy Fig 1. Needle used for hepatic biopsies. Semiautomatic 16-gauge VET-core biopsy needle. concentrations) were performed at the referring practice or at the University. Determination of coagulation parameters (ie, prothrombin time [PT], activated partial thromboplastin time [APTT], and fibrinogen concentration) was always performed before performing Tru-Cut biopsies. In each cat, ultrasonographic examination of the abdomen, with special attention to hepatobiliary structures, was performed. If the cat was not cooperative enough to safely perform the biopsy procedure under local anesthesia, it was anesthetised, usually with propofol c (4 mg/kg IV as the initial dose, with additional dosing depending on the effect). Biopsy Procedures and Devices The biopsy site was surgically prepared. Lidocaine, 2 to 3 ml, was injected SC and into the abdominal wall before a small skin incision was made with a number 11 surgical blade. The biopsy instrument then was introduced through the abdominal wall and advanced into the liver under ultrasound guidance to the location of interest. Before firing the device, the distance between the tip of the needle and important structures, such as blood vessels or bile ducts, was measured. A distance of at least 2 cm always was allowed because inner needle advancement was 2 cm when the device was fired. In general, 2 biopsy samples were taken from each cat. After each attempt, Doppler ultrasonography was used to detect bleeding. Skin incisions did not require suturing. 4 The procedure was performed by the hepatologist (JR) or the resident rotating in the hepatology department at that time. This procedure was followed consistently during the entire study period. If the resident performed the procedure, it was done so after intensive training in the method and always under the direct supervision of the hepatologist. Resuscitation In the first period (when the automatic biopsy device was used), a high incidence of hypotensive or bradycardic shock, occurring within 10 to 15 minutes of taking the biopsy, was observed. Resuscitation was initiated immediately in these cats. Oxygen was supplied, a peripheral venous catheter was placed for fluid therapy, an electrocardiogram was monitored, heart massage was applied, and resuscitative drugs (eg, atropine, d epinephrine, e dobutamine f ) were administered IV as necessary. Statistical Analysis For statistical analysis, SPSS 13.0 software g was used. First, the normality of the different variables was evaluated by the Kolmogorov-Smirnov test. Normally distributed variables were then evaluated with Levene s test for equality of variances and t- test for equality of means (2-tailed). Non normally distributed parameters were evaluated by a 2-tailed Mann-Whitney test. Significant differences between the 2 groups for the different clinical signs, sex, histology, and anesthesia were evaluated by the 2-sided Fisher s exact test. A P value of,.05 was considered significant. Results Forty-five ultrasound-guided liver biopsies were performed. In the first period, biopsy specimens were collected at 26 occasions with the automatic device. Of these cats, 18 were neutered males, 7 were neutered females, and 1 was an intact female. The median age was 10 years (95% confidence interval [CI], 1 13; in 2 instances the age was not available), and median weight was 4.1 kg (95% CI, ; in 3 instances weight was not recorded). This group consisted of 14 mixed breed cats, 8 European shorthairs, 2 British shorthairs, 1 Siamese, and 1 Tonkinese cat. Of the 19 biopsy samples collected in the second period, 15 were taken from neutered males, 1 from an intact male, and 3 from neutered females. During this period, the median age of the cats was 11 years (95% CI, 5 14 years), and the median weight was 3.8 kg (95% CI, ; in 1 instance weight was not recorded). The second group comprised 9 mixed breed cats, 4 European shorthairs, 3 Persians, 1 Burmese, 1 East European Shorthair, and 1 Main Coon. There were no differences between groups in regard to sex, age, breed, or weight. Clinical Signs Clinical information about 2 cats in the first group was limited, likely because the cats were referred only for biopsy and not for full diagnostic evaluation. Similar clinical signs were present in both groups of cats. Jaundice and vomiting were more frequent in cats seen in the first period (Table 1). However, none of the differences was significant. Clinicopathologic Findings In the first period, 6 cats (23%) had anemia, 8 cats (31%) had leukocytosis, and 1 had leukopenia. Bile acid concentrations were increased in 11 cats (42%); alanine aminotransferase (ALT) activity, in 16 cats (62%); total protein concentration, in 16 cats (62%); serum albumin concentration, in 4 cats (15%); and in the 18 cats (of 26) in which serum protein electrophoresis was performed, gamma globulin concentrations were increased in 16 cats. In the second period, 5 cats (26%) had anemia, 4 (21%) had leukocytosis, but no cat had leukopenia. Bile
3 Risks of Biopsy Guns in Cats 1329 Table 1. Clinical signs in cats of both groups. No. with Automatic Biopsy Device No. with Semiautomatic Biopsy Device Clinical Sign n 5 24 n 5 19 P Value Jaundice Anorexia/decreased appetite Weight loss Lethargy Ascites Vomiting PU/PD Fever PU, polyuria; PD, polydipsia. acid concentrations were increased in 8 cats (42%); ALT activity, in 10 cats (53%); total protein concentration, in 6 cats (32%); serum albumin concentration, in 3 cats (16%); and in 8 of the 11 cats in which serum protein electrophoresis was performed, gamma globulin concentrations were increased (Table 2). In all cats of both periods, blood coagulation parameters (ie, PT, APTT, and fibrinogen concentration) were within the reference range. Statistically, there were no differences in PCV, leukocyte counts, bile acid concentrations, ALT activity, albumin, or gamma globulin concentrations between the 2 groups. Only the difference in total protein concentration was statistically significant, with mean total protein concentration being higher in cats of the first period (7.5 g/dl) compared with those of the second period (6.7 g/dl; P,.05). Clinicopathologic findings in surviving and nonsurviving cats in which the automatic biopsy device was used were within comparable ranges (Table 3). It was not possible to statistically evaluate these results because of insufficient numbers. Anesthesia In 25 of the 45 cats, anesthesia was required to safely perform the biopsy procedure. In the period from October 1, 2002, until October 31, 2003, 12 of the 26 (46%) were anesthetized. In 6 of these, propofol was used. Medetomidine h was used in 3 cats. Midazolam i combined with buprenorphine j or ketamine k were used once each. The anesthetics used could not be identified in 1 case. Between November 1, 2003, and October 31, 2004, 13 of the 19 cats (68%) required anesthesia. In 9 of these cats, propofol was used. Medetomidine was used twice, and the combination of acepromazine l with methadone m was used in 1 cat. In 1 cat, the anesthetic used could not be identified. There was no significant difference in the number of cats that needed anesthesia in the first period compared with the second period. In addition, the anesthetic protocol used was not changed between study periods, and the anesthetics used were selected based on the needs of each individual cat. Biopsy Procedure and Outcome Ultrasound-guided biopsies were taken in all 45 cats. Care was taken to avoid bile ducts and large blood vessels in all cats. After completion of the biopsy procedure, ultrasonography was performed and no bleeding could be detected in any of the cats. During the period in which the automatic biopsy device was used, 5 cats developed severe shock within 15 minutes after the biopsy. All of these cats experienced severe bradycardia accompanied by very weak pulse, respiratory impairment, and loss of consciousness (ie, hypotensive shock). None survived despite prompt resuscitation as described previously. Table 2. Clinicopathologic findings in cats of both groups. Automatic Biopsy Device a Semiautomatic Biopsy Device a Value Units Reference Range Median 95% CI Median 95% CI PCV % Leucocytes 10 3 /ml Bile acids mm ALT U/L Total protein* g/dl Albumin g/dl Gamma globulins g/dl CI, confidence interval. a Median values and 95% CI of the 2.5th and 97.5th percentiles. * indicates significant difference between the 2 groups.
4 1330 Proot and Rothuizen Table 3. Clinicopathologic findings in the surviving and deceased cats of the period in which the automatic biopsy gun was used. Survivors a Deceased Cats a Value Units Reference Range Median Range Median Range PCV % Leucocytes 10 3 /ml Bile acids mm ALT U/L Total protein g/dl Albumin g/dl Gamma globulins g/dl ALT, alanine aminotransferase. a Median values with lowest and highest values. Because of this high complication rate, as of November 2003 we stopped using the automatic biopsy device and began using the semiautomatic VET-core biopsy needle. During the next 12 months, 19 liver biopsies were performed in cats. None of them experienced any major adverse effects. The complication rate in the first period in which the automatic biopsy device was used was 19.2%, and the complication rate was 0.0% in the second period during which the semiautomatic biopsy device was used. The difference in complication rates had a P value of.06. Histopathology Lymphocytic and neutrophilic cholangitis was equally distributed between the 2 groups (Table 4). In the group in which the automatic biopsy device was used, there were 2 cats with neoplasia (1 adenocarcinoma and 1 hepatocellular adenoma). In the other group, there were 5 tumors: 1 adenocarcinoma, 1 (likely metastatic) carcinoma, 1 malignant lymphoma, 1 histiocytosis, 1 erythroid myeloma. In 2 of the 3 cats with normal liver histopathology, bile duct dilatation was seen with ultrasonography. However, culture of bile samples from these cats was negative and no bacteria or leukocytes were seen on cytologic examination. Fatal Cases Of the 5 cats that died, 2 were European Shorthairs, 2 were mixed breed, and 1 was a Tonkinese cat. The median age was 11 years (range, 5 months 13 years). Reasons for referral were weight loss (in all cats), jaundice (in 4 cats), decreased appetite or anorexia (in 4 cats), fever and ascites (in 1 cat), and vomiting and abdominal pain (in 1 cat). In 4 cats, the PCV was low with a median of 23% (range, 13 39%). In all but 1 cat, bile acid concentrations were increased (median, 47 mm; range, mm). In 3 cats ALT activity was increased (median, 292 U/L; range, U/L). In 3 cats total protein concentration was increased (median, 8 g/dl; range, g/dl). One cat had high serum albumin concentration (without high PCV), and in all 5 cats gamma globulin concentrations were increased (median, 1.7 g/dl; range, g/dl). Coagulation parameters were normal in all cats. To perform ultrasonography and biopsy, 2 of the 5 nonsurviving cats had required anesthesia. In both instances propofol was used. Two cats were diagnosed with FIP, 1 with lymphocytic cholangitis, 1 with acute local necrotic hepatitis, and 1 with macro-vesicular and micro-vesicular steatosis suggestive of hepatic lipidosis. Of the 2 cats that required anesthesia, 1 had FIP and the other had lymphocytic cholangitis. In 1 cat (with FIP) postmortem examination was performed, confirming the diagnosis and absence of hemorrhage. Discussion Fatal shock reactions were only observed after the use of the automatic biopsy device b and did not occur when using the semiautomatic biopsy device. a The difference in complication rate between the 2 groups had a P value of.06. It is important to evaluate whether factors other than the biopsy device used could explain this difference. Massive bleeding (leading to hypotensive shock) or injury of larger bile ducts could have been complicating factors. However, ultrasound-guidance was used as the standard procedure in all cats in this study. The distance between the tip of the Tru-Cut needle and vital structures (eg, blood vessels, bile ducts, gall bladder) always was measured before taking the biopsy sample, and enough space (minimum of 2 cm) was allowed to avoid such structures. After the biopsy was performed, ultrasonography was used to check for the presence of hemorrhage. Clinically relevant bleeding was not observed in any of the cats in this study. Postmortem examination was performed in 1 of the 5 nonsurviving cats, and no trauma to vital structures or evidence of bile peritonitis was found in this cat. Anesthesia also may have been a factor in the outcome. The number of cats that needed anesthesia for the procedure during the first period was not substantially different from the number requiring anesthesia during the second period. Of the 5 nonsurviving cats, 2 were anesthetized with propofol. The course of anesthesia was smooth and uneventful until the time of biopsy, and fatal shock occurred immediately after taking the biopsy sample. Therefore, there is no indication that anesthesia could explain the difference between the 2 groups.
5 Risks of Biopsy Guns in Cats 1331 Table 4. Histologic diagnosis in cats of both groups. Histologic Diagnosis No. with Automatic Biopsy Device a No. with Semiautomatic Biopsy Device Lymphocytic cholangitis 5 (1) 4 Neutrophilic cholangitis 3 2 Hepatic lipidosis 1 (1) 3 Neoplasia 2 5 Feline infectious peritonitis 2 (2) 0 Steroid-induced Hepatopathy 2 0 Polycystic kidney disease 3 1 Arteriovenous fistula 1 0 Secondary reactive hepatitis 3 1 Local necrotic hepatitis/necropurulent hepatitis 1 (1) 1 Ischemic hepatitis 0 1 Normal 3 1 Total a Number in parentheses indicates the number of cats that died with this diagnosis. Clinical differences existed in the cats before biopsy. Whenever possible potential risks were avoided. Anesthesia was also avoided, unless the biopsy procedure could not be safely performed without it. The number of cats was too small to statistically compare the clinicopathologic features of the survivors to those of the nonsurviving cats during the first period. Table 3 compares the clinicopathologic features of the groups. The PCV of the nonsurviving cats was somewhat lower than that of the survivors. Although the ranges are quite comparable, the median bile acid concentrations differ between the groups. Cats that were more anemic and had more severe hepatic dysfunction may have been more susceptible to complications, which may have contributed to their deaths. Coagulation was evaluated before biopsy and was normal in all 45 cats. Finally, specific subgroups of liver diseases may be associated with specific risk factors during the biopsy procedure. The diagnoses in the 2 groups were comparable, but not identical. Two of the 5 nonsurvivors had FIP, but the clinical relevance of this observation is unknown. In the second group of cats in which the semiautomatic VET-core biopsy needle was used, none had FIP. Fatal complications were not limited to cats with FIP, and other nonsurviving cats in the first group had hepatobiliary diseases that also occurred in the second group in which no complications occurred. We therefore do not believe that the presence of FIP in the first group explains the difference in complication rates. Moreover, no clinically relevant variations were identified with respect to clinical signs or clinicopathologic findings between the groups. Only total protein concentration was significantly different between the 2 groups, which may be explained by the presence of FIP in only 1 group. We conclude that the difference in biopsy procedures between the groups is the only logical explanation for the different occurrence of fatal postbiopsy shock reactions. Thus, the most probable explanation for the occurrence of shock after the automatic biopsy procedure is the occurrence of intense vagotonia leading to shock. All 5 cats that died had developed severe bradycardia with weak pulse, respiratory impairment, and loss of consciousness. All of these cats died because of cardiac arrest despite immediate resuscitation. Such clinical signs may be seen when a strong increase in vagal tone occurs (eg, during surgical procedures in which vagal reflexes occur secondary to visceral traction). 5 Such a reaction may be explained when the 2 biopsy devices are compared. The automatic biopsy needle is put in place under ultrasound guidance. When the device is activated, an inner needle with stylet and specimen notch is advanced 2 cm into the liver and then immediately covered by an outer cannula. This splitsecond event transfers a 14 pound-force (lbf), which equals N, to the tissue which is specifically produced by the stylet (written communication from Inter-V, tjolsen@interv.net, Jan 23, 2006). In the case of the semiautomatic biopsy needle, the stylet (with specimen notch) is manually advanced into the liver under ultrasound guidance. When the plunger is fully depressed, the outer cutting cannula is quickly advanced to cover the stylet. Here the manual advancement of the stylet transfers much less force, and the thin cutting sheath, which is fired automatically, also represents less force than the much quicker movement of the stylet of the automatically driven biopsy needle. It is likely that the strong pressure wave from the automatic biopsy device is not tolerated by cats. Vagotonia after liver biopsy is a reported complication in human patients. In humans, complications of percutaneous liver biopsy are pain; vagal reaction with hypotension; trauma to other abdominal organs; perforation of the diaphragm, gallbladder, or blood vessels; fracture or dislocation of the needle or parts of it; and seeding of microorganisms or tumor cells. 6 Vasovagal episodes and pain are the most common reasons for hospitalization after outpatient liver biopsy. 7 Janes and Lindor 8 found that 3.2% of all patients undergoing outpatient liver biopsy required hospitalization afterwards. In 92% of patients, hospitalization was for pain or hypotension. Piccinino et al 9 analyzed the complications of percutaneous liver biopsy in humans in relation to the type of needle used and the underlying disease in a retrospective study of 68,276 liver biopsies from 1973 to In this study, liver biopsies were performed with
6 1332 Proot and Rothuizen a Menghini needle (60,611 biopsies), a Tru-Cut needle (7,372 biopsies), or a Vim-Silverman needle (293 biopsies). Death, serious hemorrhagic complications, pneumothorax, and biliary peritonitis occurred most frequently when the Tru-Cut needle was used. The use of a semiautomatic device, however, was not evaluated. The underlying disease in human patients who did not survive the procedure was always cirrhosis or hepatic neoplasia. Dupas et al 10 investigated the complications of percutaneous liver biopsy guided by fluoroscopy, ultrasonography, and computed tomography in human patients. Liver biopsy was associated with complications in,2% of patients and consisted of transient hepatic pain and vagal reactions that were not fatal but required treatment with atropine. Unfortunately, none of these studies provided an explanation for the vasovagal episodes or hypotension. In the veterinary literature, similar immediate adverse effects have not been reported. 11,12 Léveillé et al 13 reviewed 233 ultrasound-guided biopsies of abdominal structures in anesthetized cats and dogs in which an automated Biopty biopsy device n with an 18-gauge needle was used. In 177 cases (cats and dogs), the liver was biopsied, and in 2 cats major complications occurred. These cats developed bile peritonitis 24 hours after the procedure, although the gall bladder was not punctured. Both cats were diagnosed with hepatic lipidosis, and the friability of the lipidotic liver was thought possibly to have led to bile duct rupture. Such an event could only explain 1 of the 5 deaths in our study. Furthermore, in the study of Léveillé et al, the cats did not develop complications immediately as was the case in our study. The absence of vagotonic shock in the previous study may have been due to less pronounced forces developed by the Biopty device n ( lbf or N) (written communication from Frank Borremans of CR Bard Inc, Frank.Borremans@ crbard.com, April 19, 2006). An alternative explanation may be the smaller gauge needle used (ie, 18 gauge compared with 16 gauge in this study). However, the bevelled edge of the stylet of the 16-gauge needle does not exceed that of an 18-gauge needle by more than 15%. Consequently, we believe the force exerted by the automatic device is the major factor contributing to the fatal complications in this cat series. Apparently, cats are much more susceptible to developing vagotonia than are dogs, because we have used the same automatic biopsy device for many years in dogs without the complications reported here in cats. As in humans, we have observed discomfort and vagotonic reactions that had to be treated with atropine and IV fluid administration in a few dogs with hepatic carcinomas. These vagotonic reactions were treated successfully and were never fatal. The use of anticholinergic premedication could be considered when using the automatic biopsy device in cats. However, we question whether it would be ethical to expose any other cats, even with anticholinergic premedication, to the high risk of fatal complications. Consequently, we have not pursued this approach. Use of anticholinergics, however, may be a consideration when using other automated devices, because cats appear to be more susceptible to vagotonia than are dogs. We conclude that the use of the automatic biopsy device evaluated in this study (which develops a force of 14 lbf) should be avoided for liver biopsy in cats because of the unacceptably high frequency of severe complications. Instead, semiautomatic or automatic biopsy devices that do not develop such high forces may be employed, taking standard safety precautions for liver biopsy. Footnotes a Vet-Core biopsy needle (16 gauge; length, 9 mm; throw length, 20 mm), Global Veterinary Products Inc, New Buffalo, MI b Pro-Mag Ultra Automatic Biopsy Instrument, Manan Medical Products, PBN Medicals, Stenløse, Denmark. (22-mm stroke, serial no. 6527) c PropoVet, Abbott Laboratories, Queensborough, Kent, UK d Atropinesulfaat, Pharmachemie BV, Haarlem, Noord-Holland, The e Adrenaline, Pharmachemie BV, Haarlem, Noord-Holland, The f Dobutamine, Centrafarm, BV, Etten-Leur, Noord-Brabant, The g SPSS 13.0; SPSS Inc, Chicago, IL h Domitor, Pfizer Animal Health BV, Cappelle a/d IJssel, Zuid- Holland, The i Dormicum, Roche Nederland BV, Woerden, Utrecht, The j Temgesic, Schering-Plough, Utrecht, The k Ketamine HCl, AST farma BV, Oudewater, Utrecht, The l Acepromazine, Apotheek faculteit diergeneeskunde, Utrecht, The m Methadon HCl, Eurovet Animal Health BV, Bladel, Noord- Brabant, The n Bard Urological Division, CR Bard Inc, Covington, GA Acknowledgments We hereby want to thank Dr E. Teske (DVM, PhD, Dipl ECVIM-CA) for his support in the statistical analysis of the data and J. Fama for providing digital images. References 1. Caney SMA, Gruffed-Jones TJ. Feline inflammatory liver disease. In: Ettinger SJ, ed. Textbook of Veterinary Internal Medicine, 6th ed. Philadelphia, PA: WB Saunders; 2005: Webster CRL. History, clinical signs, and physical findings in hepatobiliary disease. In: Ettinger SJ, ed. Textbook of Veterinary Internal Medicine, 6th ed. Philadelphia, PA: WB Saunders; 2005: Hoppe FE, Hager DA, Poulos PW, et al. A comparison of manual and automatic ultrasound-guided biopsy techniques. Vet Radiology 1986;27: Rothuizen J, Desmet VJ, van den Ingh TSGAM, et al. In: WSAVA Standards for Histological and Clinical Diagnosis of
7 Risks of Biopsy Guns in Cats 1333 Canine and Feline Liver Disease. Edinburgh, UK: Churchill Livingstone; 2006: Briggs BA, Cullen DJ. In: Complications in Anaesthesiology. Philadelphia, PA: Lippincott; 1983: Desmet V, Fevery J. Liver biopsy. Bailliere Clin Gastr 1995;9: Flora KD, Ingram K. Diagnostic liver biopsy. Available at: Accessed March 9, Janes CH, Lindor KD. Outcome of patients hospitalized for complications after outpatient liver biopsy. Ann Intern Med 1993;118: Piccinino F, Sagnelli E, Pasquale G. Complications following percutaneous liver biopsy: A multi-centre study. J Hepatol 1986;2: Dupas B, Frampas E, Leaute F, et al. Complications de gestes interventionnels percutanés sous contrôle radioscopique, échographique ou scanographique. J Radiol 2005;86: Bigge LA, Brown DJ, Penninck DG. Correlation between coagulation profile findings and bleeding complications after ultrasound-guided biopsies: 434 cases ( ). J Am Anim Hosp Assoc 2001;37: Cole TL, Center SQ, Shannon NF, et al. Diagnostic comparison of needle and wedge biopsy specimens of the liver in dogs and cats. J Am Vet Med Assoc 2002;220: Léveillé R, Partington BP, Biller DS et al. Complications after ultrasound-guided biopsy of abdominal structures in dogs and cats: 246 cases ( ). J Am Vet Med Assoc 1993; 203:
DIAGNOSIS AND MANAGEMENT OF CHOLECYSTITIS IN DOGS
 Int. J. Agric.Sc & Vet.Med. 2014 K Satish Kumar and D Srikala, 2014 Research Paper ISSN 2320-3730 www.ijasvm.com Vol. 2, No. 3, August 2014 2014 www.ijasvm.com. All Rights Reserved DIAGNOSIS AND MANAGEMENT
Int. J. Agric.Sc & Vet.Med. 2014 K Satish Kumar and D Srikala, 2014 Research Paper ISSN 2320-3730 www.ijasvm.com Vol. 2, No. 3, August 2014 2014 www.ijasvm.com. All Rights Reserved DIAGNOSIS AND MANAGEMENT
Treatment of septic peritonitis
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Copper-Storage Liver Disease Basics
 Copper-Storage Liver Disease Basics OVERVIEW Abnormal accumulation of copper in the liver, causing sudden (acute) inflammation of the liver (hepatitis) or long-term (chronic) hepatitis and eventually progressive
Copper-Storage Liver Disease Basics OVERVIEW Abnormal accumulation of copper in the liver, causing sudden (acute) inflammation of the liver (hepatitis) or long-term (chronic) hepatitis and eventually progressive
The Vet Education Webinar Series Biliary Mucocoeles With Dr Gemma Birnie
 The Vet Education Webinar Series 2016 Biliary Mucocoeles With Dr Gemma Birnie BVSc MACVSc Vet Education is Proudly Supported by Hill s Pet Nutrition Australia Gallbladder Mucocoeles Dr. Gemma Birnie Resident
The Vet Education Webinar Series 2016 Biliary Mucocoeles With Dr Gemma Birnie BVSc MACVSc Vet Education is Proudly Supported by Hill s Pet Nutrition Australia Gallbladder Mucocoeles Dr. Gemma Birnie Resident
Gastric Dilatation-Volvulus
 Gastric Dilatation-Volvulus The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery. Only veterinarians who have successfully completed the certification requirements
Gastric Dilatation-Volvulus The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery. Only veterinarians who have successfully completed the certification requirements
Anesthesia Check-off Form
 Anesthesia Check-off Form 5231 SW 91st Drive Gainesville, FL 32608 (352) 377-6003 The doctors and staff at Haile Plantation Animal Clinic would like to offer the most advanced medical care and services
Anesthesia Check-off Form 5231 SW 91st Drive Gainesville, FL 32608 (352) 377-6003 The doctors and staff at Haile Plantation Animal Clinic would like to offer the most advanced medical care and services
Double-Blind, Placebo-Controlled, Randomized Study of Dipyrone as a Treatment for Pyrexia in Horses
 Double-Blind, Placebo-Controlled, Randomized Study of Dipyrone as a Treatment for Pyrexia in Horses Emily Sundman, DVM Ming Yin, PhD Tianhua Hu, PhD Melinda Poole, DVM Disclosures Sundman, Yin, Hu, and
Double-Blind, Placebo-Controlled, Randomized Study of Dipyrone as a Treatment for Pyrexia in Horses Emily Sundman, DVM Ming Yin, PhD Tianhua Hu, PhD Melinda Poole, DVM Disclosures Sundman, Yin, Hu, and
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Small Animal Medicine Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
POST-OPERATIVE ANALGESIA AND FORMULARIES
 POST-OPERATIVE ANALGESIA AND FORMULARIES An integral component of any animal protocol is the prevention or alleviation of pain or distress, such as that associated with surgical and other procedures. Pain
POST-OPERATIVE ANALGESIA AND FORMULARIES An integral component of any animal protocol is the prevention or alleviation of pain or distress, such as that associated with surgical and other procedures. Pain
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Veterinary Anaesthesia and Critical Care Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
Associated Terms: Breast Cancer, Radical Mastectomy, Mastectomy, Mammectomy, Mammary Adenocarcinoma
 Associated Terms: Breast Cancer, Radical Mastectomy, Mastectomy, Mammectomy, Mammary Adenocarcinoma The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Associated Terms: Breast Cancer, Radical Mastectomy, Mastectomy, Mammectomy, Mammary Adenocarcinoma The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Septic cats are not small septic dogs
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Septic cats are not small septic dogs Author : ROGER WILKINSON Categories : Vets Date : September 29, 2008 ROGER WILKINSON
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Septic cats are not small septic dogs Author : ROGER WILKINSON Categories : Vets Date : September 29, 2008 ROGER WILKINSON
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT DRAFT AS CURRENTLY OUT FOR CONSULTATION BUT CAN BE UTILISED IN PRESENT FORMAT Name & Title Of Author: Date Revised: Approved by Committee/Group:
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT DRAFT AS CURRENTLY OUT FOR CONSULTATION BUT CAN BE UTILISED IN PRESENT FORMAT Name & Title Of Author: Date Revised: Approved by Committee/Group:
Acute Hemorrhagic Diarrhea Syndrome (AHDS) A Cause of Bloody Feces in Dogs
 Acute Hemorrhagic Diarrhea Syndrome (AHDS) A Cause of Bloody Feces in Dogs No dog parent wants to clean up diarrhea. Cleaning up bloody diarrhea is even more unpleasant. Unfortunately, the development
Acute Hemorrhagic Diarrhea Syndrome (AHDS) A Cause of Bloody Feces in Dogs No dog parent wants to clean up diarrhea. Cleaning up bloody diarrhea is even more unpleasant. Unfortunately, the development
Mature lymphocytosis (ie, 7,000/ L) in the blood of
 J Vet Intern Med 2005;19:855 859 Differentiating Benign and Malignant Causes of Lymphocytosis in Feline Bone Marrow Douglas J. Weiss Differentiation of benign and malignant causes of lymphocytosis in blood
J Vet Intern Med 2005;19:855 859 Differentiating Benign and Malignant Causes of Lymphocytosis in Feline Bone Marrow Douglas J. Weiss Differentiation of benign and malignant causes of lymphocytosis in blood
SOS EMERGENCY ANIMALS Please note that the following scenario(s) are generalized
 Suggested Tasks for Veterinary Students Volunteering at the VSPCA By Bosmat Gal, DVM Assistant to the President of the Animal Rescue League of Boston for International Programs Member of the VSPCA Advisory
Suggested Tasks for Veterinary Students Volunteering at the VSPCA By Bosmat Gal, DVM Assistant to the President of the Animal Rescue League of Boston for International Programs Member of the VSPCA Advisory
Dexmedetomidine and its Injectable Anesthetic-Pain Management Combinations
 Back to Anesthesia/Pain Management Back to Table of Contents Front Page : Library : ACVC 2009 : Anesthesia/Pain Management : Dexmedetomidine Dexmedetomidine and its Injectable Anesthetic-Pain Management
Back to Anesthesia/Pain Management Back to Table of Contents Front Page : Library : ACVC 2009 : Anesthesia/Pain Management : Dexmedetomidine Dexmedetomidine and its Injectable Anesthetic-Pain Management
Understanding your pet s LIVER CONDITION
 Understanding your pet s LIVER CONDITION Why is the liver so important? What causes liver disease in dogs and cats? The liver is one of the largest organs in your pet s body, and it s vital for their good
Understanding your pet s LIVER CONDITION Why is the liver so important? What causes liver disease in dogs and cats? The liver is one of the largest organs in your pet s body, and it s vital for their good
Feline blood transfusions: preliminary considerations
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Feline blood transfusions: preliminary considerations Author : Andrea Harvey Categories : RVNs Date : September 1, 2011 ABSTRACT
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Feline blood transfusions: preliminary considerations Author : Andrea Harvey Categories : RVNs Date : September 1, 2011 ABSTRACT
Hydatid Cyst Dr. Nora L. El-Tantawy
 Hydatid Cyst Dr. Nora L. El-Tantawy Ass. Prof. of Parasitology Faculty of Medicine, Mansoura university, Egypt Echinococcus granulosus Geographical Distribution: cosmopolitan especially in sheep raising
Hydatid Cyst Dr. Nora L. El-Tantawy Ass. Prof. of Parasitology Faculty of Medicine, Mansoura university, Egypt Echinococcus granulosus Geographical Distribution: cosmopolitan especially in sheep raising
Overview. Clinical signs. Will you treat? Owner willing to treat? Surgical vs. Medical. Medical options
 Part II (cushing s disease is hard to diagnose) Cushing s Disease Is Easy To Treat Why test? When to test? How to test? Will you treat? How to treat? Overview Thomas Schermerhorn, VMD, DACVIM(SAIM) Kansas
Part II (cushing s disease is hard to diagnose) Cushing s Disease Is Easy To Treat Why test? When to test? How to test? Will you treat? How to treat? Overview Thomas Schermerhorn, VMD, DACVIM(SAIM) Kansas
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS
 VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Medicine of Cats Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2016 Medicine of Cats Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2016 Medicine of Cats Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
CANINE HEARTWORM DISEASE
 ! CANINE HEARTWORM DISEASE What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs. It is caused by a blood-borne parasite called Dirofilaria
! CANINE HEARTWORM DISEASE What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs. It is caused by a blood-borne parasite called Dirofilaria
Non-steroidal anti-inflammatory drugs (NSAIDs) are used widely to relieve pain, with or without
 May 2013 Contents About NSAIDs What about COXselectivity? How effective are NSAIDs? Adverse effects of NSAIDs How frequent are the adverse effects of NSAIDs? General prescribing guidelines for NSAIDs What
May 2013 Contents About NSAIDs What about COXselectivity? How effective are NSAIDs? Adverse effects of NSAIDs How frequent are the adverse effects of NSAIDs? General prescribing guidelines for NSAIDs What
What causes heartworm disease?
 Heartworm Disease: What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs and cats. It is caused by a blood-borne parasite called Dirofilaria
Heartworm Disease: What causes heartworm disease? Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs and cats. It is caused by a blood-borne parasite called Dirofilaria
T u l a n e U n i v e r s i t y I A C U C Guidelines for Rodent & Rabbit Anesthesia, Analgesia and Tranquilization & Euthanasia Methods
 T u l a n e U n i v e r s i t y I A C U C Guidelines for Rodent & Rabbit Anesthesia, Analgesia and Tranquilization & Euthanasia Methods Abbreviations: General Considerations IV = intravenous SC = subcutaneous
T u l a n e U n i v e r s i t y I A C U C Guidelines for Rodent & Rabbit Anesthesia, Analgesia and Tranquilization & Euthanasia Methods Abbreviations: General Considerations IV = intravenous SC = subcutaneous
PHYSICIAN ORDERS. Page 1 of 6. Provider Initial: Esophagectomy Preoperative [ ] Height Weight Allergies
![PHYSICIAN ORDERS. Page 1 of 6. Provider Initial: Esophagectomy Preoperative [ ] Height Weight Allergies PHYSICIAN ORDERS. Page 1 of 6. Provider Initial: Esophagectomy Preoperative [ ] Height Weight Allergies](/thumbs/93/111492780.jpg) Height Weight Allergies If appropriate for patient condition, please consider the following order sets: Hydration Order for Reducing Risk of Radiocontrast Induced Nephrotoxicity Physician Order #683 In
Height Weight Allergies If appropriate for patient condition, please consider the following order sets: Hydration Order for Reducing Risk of Radiocontrast Induced Nephrotoxicity Physician Order #683 In
Hope for Healing Liver Disease in Your Dog. Quick Start Guide. by Cyndi Smasal
 Hope for Healing Liver Disease in Your Dog Quick Start Guide by Cyndi Smasal Copyright 2004 by Cyndi Smasal All Rights Reserved. No part of this book may be reproduced, stored in a retrieval system, or
Hope for Healing Liver Disease in Your Dog Quick Start Guide by Cyndi Smasal Copyright 2004 by Cyndi Smasal All Rights Reserved. No part of this book may be reproduced, stored in a retrieval system, or
What s Your Diagnosis? By Sohaila Jafarian, Class of 2018
 Signalment: Greeley, 3 yo MC DSH Presenting Complaint: ADR History: What s Your Diagnosis? By Sohaila Jafarian, Class of 2018 Patient is an indoor/outdoor cat. Previously healthy and up to date on vaccines
Signalment: Greeley, 3 yo MC DSH Presenting Complaint: ADR History: What s Your Diagnosis? By Sohaila Jafarian, Class of 2018 Patient is an indoor/outdoor cat. Previously healthy and up to date on vaccines
Update on diagnosis of feline infectious peritonitis (FIP)
 Update on diagnosis of feline infectious peritonitis (FIP) Séverine Tasker RCVS Specialist in Feline Medicine The Feline Centre Langford Veterinary Services University of Bristol http://www.felinecentre.co.uk/
Update on diagnosis of feline infectious peritonitis (FIP) Séverine Tasker RCVS Specialist in Feline Medicine The Feline Centre Langford Veterinary Services University of Bristol http://www.felinecentre.co.uk/
Heartworm Disease in Dogs
 Kingsbrook Animal Hospital 5322 New Design Road, Frederick, MD, 21703 Phone: (301) 631-6900 Website: KingsbrookVet.com What causes heartworm disease? Heartworm Disease in Dogs Heartworm disease or dirofilariasis
Kingsbrook Animal Hospital 5322 New Design Road, Frederick, MD, 21703 Phone: (301) 631-6900 Website: KingsbrookVet.com What causes heartworm disease? Heartworm Disease in Dogs Heartworm disease or dirofilariasis
Journal home page:
 Journal home page: http://www.journalijiar.com INTERNATIONAL JOURNAL OF INNOVATIVE AND APPLIED RESEARCH RESEARCH ARTICLE A First Case Report of Feline Infectious Peritonitis in a Domestic Cat in Pakistan
Journal home page: http://www.journalijiar.com INTERNATIONAL JOURNAL OF INNOVATIVE AND APPLIED RESEARCH RESEARCH ARTICLE A First Case Report of Feline Infectious Peritonitis in a Domestic Cat in Pakistan
LOWER EYELID RECONSTRUCTIVE SURGERY AFTER SEBACEOUS GLAND ADENOMA RESECTION IN A GERMAN SHEPHERD DOG: A CASE REPORT
 Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN Rambabu 2321 9602 Kalaka www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report LOWER EYELID RECONSTRUCTIVE
Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN Rambabu 2321 9602 Kalaka www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report LOWER EYELID RECONSTRUCTIVE
Naturally occurring hyperadrenocorticism is a wellrecognized
 Evaluation of twice-daily lower-dose trilostane treatment administered orally in dogs with naturally occurring hyperadrenocorticism Edward C. Feldman, dvm, dacvim Objective To evaluate effectiveness and
Evaluation of twice-daily lower-dose trilostane treatment administered orally in dogs with naturally occurring hyperadrenocorticism Edward C. Feldman, dvm, dacvim Objective To evaluate effectiveness and
ford residence southampton, ny
 P ford residence southampton, ny What bacterial infections cause canine liver disease Causes of Liver Disease. Here are ten causes of liver disease: Poor diet; Bacterial infection; Viral infection; Trauma,
P ford residence southampton, ny What bacterial infections cause canine liver disease Causes of Liver Disease. Here are ten causes of liver disease: Poor diet; Bacterial infection; Viral infection; Trauma,
AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS. Sample Exam Questions. Veterinary Practice (Small Animal)
 AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS Sample Exam Questions Veterinary Practice (Small Animal) Written Examination (Component 1) Written Paper 1 (two hours): Principles of Veterinary
AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS Sample Exam Questions Veterinary Practice (Small Animal) Written Examination (Component 1) Written Paper 1 (two hours): Principles of Veterinary
UNDERSTANDING COLIC: DON T GET IT TWISTED
 UNDERSTANDING COLIC: DON T GET IT TWISTED Today s Topics: What is colic? Anatomy review How to identify colic What to do when you suspect colic What to expect during a colic visit from your veterinarian
UNDERSTANDING COLIC: DON T GET IT TWISTED Today s Topics: What is colic? Anatomy review How to identify colic What to do when you suspect colic What to expect during a colic visit from your veterinarian
Caution: Federal law restricts this drug to use by or on the order of a licensed veterinarian.
 BOEHRINGER INGELHEIM VETMEDICA, INC. USA Product Label http://www.vetdepot.com 2621 NORTH BELT HIGHWAY, ST. JOSEPH, MO, 64506 2002 Telephone: 800 325 9167 Fax: 816 236 2717 Email: www.bi vetmedica.com
BOEHRINGER INGELHEIM VETMEDICA, INC. USA Product Label http://www.vetdepot.com 2621 NORTH BELT HIGHWAY, ST. JOSEPH, MO, 64506 2002 Telephone: 800 325 9167 Fax: 816 236 2717 Email: www.bi vetmedica.com
Anesthesia & analgesia in birds
 Anesthesia and analgesia in birds Yvonne R.A. van Zeeland, DVM, PhD, MVR, Dip. ECZM (avian) Division of Zoological Medicine, Utrecht University Anesthesia & analgesia in birds Yvonne van Zeeland DVM, MVR,
Anesthesia and analgesia in birds Yvonne R.A. van Zeeland, DVM, PhD, MVR, Dip. ECZM (avian) Division of Zoological Medicine, Utrecht University Anesthesia & analgesia in birds Yvonne van Zeeland DVM, MVR,
Australian College of Veterinary Scientists. Fellowship Examination. Small Animal Surgery Paper 1
 Australian College of Veterinary Scientists Fellowship Examination June 2011 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer your choice
Australian College of Veterinary Scientists Fellowship Examination June 2011 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer your choice
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Veterinary Emergency and Critical Care Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2014 Veterinary Emergency and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2014 Veterinary Emergency and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
Feline lower urinary tract disease (FLUTD)
 Feline lower urinary tract disease (FLUTD) Feline lower urinary tract disease (FLUTD) is not a specific disease, but rather is the term used to describe conditions that can affect the urinary bladder and/or
Feline lower urinary tract disease (FLUTD) Feline lower urinary tract disease (FLUTD) is not a specific disease, but rather is the term used to describe conditions that can affect the urinary bladder and/or
COLLEGE OF VETERINARY MEDICINE
 Title: A randomized, masked, placebo controlled field study to determine efficacy and safety of Paccal Vet in dogs with non resectable (or unresected) mammary carcinoma of stage III-V 1. Why is the study
Title: A randomized, masked, placebo controlled field study to determine efficacy and safety of Paccal Vet in dogs with non resectable (or unresected) mammary carcinoma of stage III-V 1. Why is the study
What s Your Diagnosis?
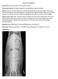 What s Your Diagnosis? Signalment: Maine Coone (8 month old, female intact) Presenting complaint: Lethargy, inappetence, serosanguinous vaginal discharge History: Lives with 11 other Maine Coone cats (males
What s Your Diagnosis? Signalment: Maine Coone (8 month old, female intact) Presenting complaint: Lethargy, inappetence, serosanguinous vaginal discharge History: Lives with 11 other Maine Coone cats (males
Australian College of Veterinary Scientists. Fellowship Examination. Feline Medicine Paper 1
 Australian College of Veterinary Scientists Fellowship Examination June 2011 Feline Medicine Paper 1 Perusal time: Twenty (20) minutes Time allowed: Four (4) hours after perusal In Section A: Answer your
Australian College of Veterinary Scientists Fellowship Examination June 2011 Feline Medicine Paper 1 Perusal time: Twenty (20) minutes Time allowed: Four (4) hours after perusal In Section A: Answer your
Guide to Veterinary Surgery If you are like most people, you want to know what you
 Guide to Veterinary Surgery If you are like most people, you want to know what you are paying for and why things cost what they do. You will find that veterinary providers are all different, and you may
Guide to Veterinary Surgery If you are like most people, you want to know what you are paying for and why things cost what they do. You will find that veterinary providers are all different, and you may
12/3/14. Top 10 Tips You Need to Know About for Anesthesia & Analgesia. Sponsorship. Introduction. VETgirl on the RUN!
 Top 10 Tips You Need to Know About for Anesthesia & Analgesia Sponsorship Introduction Introduction Introduction VETgirl on the RUN! 1 Subscription plans Download our podcasts on itunes! Find us on social
Top 10 Tips You Need to Know About for Anesthesia & Analgesia Sponsorship Introduction Introduction Introduction VETgirl on the RUN! 1 Subscription plans Download our podcasts on itunes! Find us on social
Metacam. The Only NSAID Approved for Cats in the US. John G. Pantalo, VMD Professional Services Veterinarian. Think easy. Think cat. Think METACAM.
 Metacam The Only NSAID Approved for Cats in the US John G. Pantalo, VMD Professional Services Veterinarian Think easy. Think cat. Think METACAM. Today s Agenda New pain management guidelines for cats Only
Metacam The Only NSAID Approved for Cats in the US John G. Pantalo, VMD Professional Services Veterinarian Think easy. Think cat. Think METACAM. Today s Agenda New pain management guidelines for cats Only
Intra-Abdominal Infections. Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018
 Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Intra-Abdominal Infections Jessica Thompson, PharmD, BCPS (AQ-ID) Infectious Diseases Pharmacy Clinical Specialist Renown Health April 19, 2018 Select guidelines Mazuski JE, et al. The Surgical Infection
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients.
 Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Antibiotic prophylaxis guideline for colorectal, hepatobiliary and vascular surgery for adult patients. Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience,
Update in Veterinary Medicine. Dr. Maria M. Crane Zoo Atlanta
 Update in Veterinary Medicine Dr. Maria M. Crane Zoo Atlanta Overview of Discussion Medical management of captive orangutans Preventative Medicine Anesthesia Protocols Vaccinations TB testing Current Health
Update in Veterinary Medicine Dr. Maria M. Crane Zoo Atlanta Overview of Discussion Medical management of captive orangutans Preventative Medicine Anesthesia Protocols Vaccinations TB testing Current Health
At what phone number(s) may we reach you in case of emergency?
 Compassionate Care for Pets 5205 13 th Street Lubbock, TX 79416 Phone: 806-793-2863 Fax: 806-792-0801 www.acresnorthvethospital.com Patient Admission & Consent Form for Dentistry & Anesthesia Patient s
Compassionate Care for Pets 5205 13 th Street Lubbock, TX 79416 Phone: 806-793-2863 Fax: 806-792-0801 www.acresnorthvethospital.com Patient Admission & Consent Form for Dentistry & Anesthesia Patient s
Liver regeneration in dogs after CPSS surgery
 Liver regeneration in dogs after CPSS surgery D.J.E. Vrakking Abstract Background: The purpose of this study was to investigate macroscopic liver regeneration after congenital portosystemic shunt (CPSS)
Liver regeneration in dogs after CPSS surgery D.J.E. Vrakking Abstract Background: The purpose of this study was to investigate macroscopic liver regeneration after congenital portosystemic shunt (CPSS)
Pedicle ties provide a rapid and safe method for feline ovariohysterectomy
 Pedicle ties provide a rapid and safe method for feline ovariohysterectomy K. Miller 1, W. Rekers 2, K. Ellis 2, K. Ellingsen 2, M. Milovancev 3 1 Oregon State University/Oregon Humane Society 2 Oregon
Pedicle ties provide a rapid and safe method for feline ovariohysterectomy K. Miller 1, W. Rekers 2, K. Ellis 2, K. Ellingsen 2, M. Milovancev 3 1 Oregon State University/Oregon Humane Society 2 Oregon
ChroNiC VomitiNG: Should We Ask a Cat to Live with It? CoNtribUtiNG AUthorS
 ChroNiC VomitiNG: Should We Ask a Cat to Live with It? Contributing Author: Gary D. Norsworthy, DVM, DABVP (Feline) Alamo Feline Health Center San Antonio, Texas CoNtribUtiNG AUthorS Case Report 1 S tripes,
ChroNiC VomitiNG: Should We Ask a Cat to Live with It? Contributing Author: Gary D. Norsworthy, DVM, DABVP (Feline) Alamo Feline Health Center San Antonio, Texas CoNtribUtiNG AUthorS Case Report 1 S tripes,
Pain Management in Racing Greyhounds
 Pain Management in Racing Greyhounds Pain Pain is a syndrome consisting of multiple organ system responses, and if left untreated will contribute to patient morbidity and mortality. Greyhounds incur a
Pain Management in Racing Greyhounds Pain Pain is a syndrome consisting of multiple organ system responses, and if left untreated will contribute to patient morbidity and mortality. Greyhounds incur a
Heartworm Disease in Dogs
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Heartworm Disease in Dogs Basics OVERVIEW Disease caused by infestation with heartworms
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Heartworm Disease in Dogs Basics OVERVIEW Disease caused by infestation with heartworms
Australian and New Zealand College of Veterinary Scientists. Fellowship Examination. Small Animal Medicine Paper 1
 Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Twenty (20) minutes Time allowed: Four (4) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2015 Small Animal Medicine Paper 1 Perusal time: Twenty (20) minutes Time allowed: Four (4) hours after perusal Answer
A New Advancement in Anesthesia. Your clear choice for induction.
 A New Advancement in Anesthesia Your clear choice for induction. By Kirby Pasloske When using Alfaxan, patients should be continuously monitored, and facilities for maintenance of a patent airway, artificial
A New Advancement in Anesthesia Your clear choice for induction. By Kirby Pasloske When using Alfaxan, patients should be continuously monitored, and facilities for maintenance of a patent airway, artificial
POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014
 POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014 The U.S.D.A Animal Welfare Act (9 CFR) requires use of aseptic
POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014 The U.S.D.A Animal Welfare Act (9 CFR) requires use of aseptic
The Friends of Nachusa Grasslands 2016 Scientific Research Project Grant Report Due June 30, 2017
 The Friends of Nachusa Grasslands 2016 Scientific Research Project Grant Report Due June 30, 2017 Name: Laura Adamovicz Address: 2001 S Lincoln Ave, Urbana, IL 61802 Phone: 217-333-8056 2016 grant amount:
The Friends of Nachusa Grasslands 2016 Scientific Research Project Grant Report Due June 30, 2017 Name: Laura Adamovicz Address: 2001 S Lincoln Ave, Urbana, IL 61802 Phone: 217-333-8056 2016 grant amount:
COALINGA STATE HOSPITAL. NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF WOUNDS (FIRST AID) 1. PURPOSE: Proper
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 705 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF WOUNDS (FIRST AID) 1. PURPOSE: Proper
EHRLICHIOSIS IN DOGS IMPORTANCE OF TESTING FOR CONTRIBUTING AUTHORS CASE 1: SWIGGLES INTRODUCTION WITH PERSISTENT LYMPHOCYTOSIS
 THE IMPORTANCE OF TESTING FOR EHRLICHIOSIS IN DOGS WITH PERSISTENT LYMPHOCYTOSIS Contributing Authors: Mary Anna Thrall, DVM, MS, DACVP Diana Scorpio, DVM, MS, DACLAM Ross University School of Veterinary
THE IMPORTANCE OF TESTING FOR EHRLICHIOSIS IN DOGS WITH PERSISTENT LYMPHOCYTOSIS Contributing Authors: Mary Anna Thrall, DVM, MS, DACVP Diana Scorpio, DVM, MS, DACLAM Ross University School of Veterinary
Proceedings of the Congreso Ecuatoriano de Especialidades Veterinarias CEEV Nov , 2011 Quito, Ecuador
 Close this window to return to IVIS www.ivis.org Proceedings of the Congreso Ecuatoriano de Especialidades Veterinarias CEEV 2011 Nov. 15-17, 2011 Quito, Ecuador Reprinted in IVIS with the permission of
Close this window to return to IVIS www.ivis.org Proceedings of the Congreso Ecuatoriano de Especialidades Veterinarias CEEV 2011 Nov. 15-17, 2011 Quito, Ecuador Reprinted in IVIS with the permission of
Malignant Mixed Mammary Tumor in a German Shepherd Middle Age Bitch
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 7 (2017) pp. 572-576 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.607.069
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 7 (2017) pp. 572-576 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.607.069
5/3/2018 3:09 AM Approved (Changed Course) ANHLT 151 Course Outline as of Fall 2017
 5/3/2018 3:09 AM Approved (Changed Course) ANHLT 151 Course Outline as of Fall 2017 CATALOG INFORMATION Dept and Nbr: ANHLT 151 Title: VET LAB IMAGING PROC Full Title: Veterinary Laboratory and Imaging
5/3/2018 3:09 AM Approved (Changed Course) ANHLT 151 Course Outline as of Fall 2017 CATALOG INFORMATION Dept and Nbr: ANHLT 151 Title: VET LAB IMAGING PROC Full Title: Veterinary Laboratory and Imaging
Canine Spay and Neuter Services At Manzini Animal Hospital
 Canine Spay and Neuter Services At Manzini Animal Hospital When your dog is booked in for his/her surgical procedure it can be a very anxious time for you, but here at Manzini we strive to ensure every
Canine Spay and Neuter Services At Manzini Animal Hospital When your dog is booked in for his/her surgical procedure it can be a very anxious time for you, but here at Manzini we strive to ensure every
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. Name of the Veterinary Medicinal Product Vetofol 10mg/ml Emulsion for Injection for cats and dogs (AT, CY, EE, FI, DE, EL, LV, PT, ES) Norofol 10mg/ml Emulsion for
SUMMARY OF PRODUCT CHARACTERISTICS 1. Name of the Veterinary Medicinal Product Vetofol 10mg/ml Emulsion for Injection for cats and dogs (AT, CY, EE, FI, DE, EL, LV, PT, ES) Norofol 10mg/ml Emulsion for
Yosemite Pet Hospital, Inc
 Yosemite Pet Hospital, Inc Exceptional Care for Exceptional Pets Consumer Guide to Elective Surgery and Procedures Thank you for recognizing your pet may need to undergo an elective procedure such as spay
Yosemite Pet Hospital, Inc Exceptional Care for Exceptional Pets Consumer Guide to Elective Surgery and Procedures Thank you for recognizing your pet may need to undergo an elective procedure such as spay
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
Hudson, a 10-year-old MC Cocker spaniel, was referred for evaluation of severe polyuria and polydipsia (PU/PD) of 3 months in duration...
 VCAWLAspecialty.com David Bruyette, DVM, DACVIM Hudson, a 10-year-old MC Cocker spaniel, was referred for evaluation of severe polyuria and polydipsia (PU/PD) of 3 months in duration... 1. Physical Examination
VCAWLAspecialty.com David Bruyette, DVM, DACVIM Hudson, a 10-year-old MC Cocker spaniel, was referred for evaluation of severe polyuria and polydipsia (PU/PD) of 3 months in duration... 1. Physical Examination
ANTIBIOTIC USE GUIDELINES FOR URINARY TRACT AND RESPIRATORY DISEASE
 ANTIBIOTIC USE GUIDELINES FOR URINARY TRACT AND RESPIRATORY DISEASE Jane Sykes, BVSc(Hons), PhD, DACVIM (SAIM) School of Veterinary Medicine Dept. of Medicine & Epidemiology University of California Davis,
ANTIBIOTIC USE GUIDELINES FOR URINARY TRACT AND RESPIRATORY DISEASE Jane Sykes, BVSc(Hons), PhD, DACVIM (SAIM) School of Veterinary Medicine Dept. of Medicine & Epidemiology University of California Davis,
Metacam 1.5 mg/ml oral suspension for dogs
 Metacam 1.5 mg/ml oral suspension for dogs Species:Dogs Therapeutic indication:pharmaceuticals: Neurological preparations: Analgesics, Other NSAIDs, Locomotor (including navicular and osteoarthritis) Active
Metacam 1.5 mg/ml oral suspension for dogs Species:Dogs Therapeutic indication:pharmaceuticals: Neurological preparations: Analgesics, Other NSAIDs, Locomotor (including navicular and osteoarthritis) Active
RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS
 RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS I. Purpose/Scope These guidelines apply to all surgical procedures performed on animals at Mississippi State University in which the animals
RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS I. Purpose/Scope These guidelines apply to all surgical procedures performed on animals at Mississippi State University in which the animals
UPEI / AVC Guidelines for Categories of Invasiveness and Rest Periods for Teaching Animals
 UPEI / AVC Guidelines for Categories of Invasiveness and Rest Periods for Teaching Animals Created: 1996 Revised: April 2011 Background The UPEI Animal Care Committee (ACC) recognizes that animals can
UPEI / AVC Guidelines for Categories of Invasiveness and Rest Periods for Teaching Animals Created: 1996 Revised: April 2011 Background The UPEI Animal Care Committee (ACC) recognizes that animals can
Alfaxan. (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. TECHNICAL NOTES DESCRIPTION INDICATIONS
 Alfaxan (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. NADA 141-342, Approved by FDA ALFAXAN (Schedule: C-IV) (alfaxalone 10 mg/ml) Intravenous injectable anesthetic
Alfaxan (alfaxalone 10 mg/ml) Intravenous injectable anesthetic for use in cats and dogs. NADA 141-342, Approved by FDA ALFAXAN (Schedule: C-IV) (alfaxalone 10 mg/ml) Intravenous injectable anesthetic
Veterinary Assistant Course Curriculum
 Semester 1 (32 Hours) Course Prefix & No. VAC100 Course Title: Intro to Veterinary Assistant Course None 5 (5 1-hr classes) Introduction to role of the Veterinary Assistant, client education & communication,
Semester 1 (32 Hours) Course Prefix & No. VAC100 Course Title: Intro to Veterinary Assistant Course None 5 (5 1-hr classes) Introduction to role of the Veterinary Assistant, client education & communication,
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance
 Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Case 2 Synergy satellite event: Good morning pharmacists! Case studies on antimicrobial resistance 22nd Congress of the EAHP "Hospital pharmacists catalysts for change", 22-24 March 2017, Cannes Disclosure
Intestinal linear foreign body
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Intestinal linear foreign body Author : Sally Birch Categories : Companion animal, Vets Date : February 6, 2017 Your first
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Intestinal linear foreign body Author : Sally Birch Categories : Companion animal, Vets Date : February 6, 2017 Your first
Surgical Site Infections (SSIs)
 Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Subjects Beginning with "U"
 Subjects Beginning with "U" SUBJECT: ARTICLE TITLE: JOURNAL DATE: PAGE: Ucatan miniature pigs SWINE UDDER Teat Laceration Repair in Cattle VCONA/FAP JULY 2008 295 UDDER - MICROBIOLOGY GASTROINTESTINAL
Subjects Beginning with "U" SUBJECT: ARTICLE TITLE: JOURNAL DATE: PAGE: Ucatan miniature pigs SWINE UDDER Teat Laceration Repair in Cattle VCONA/FAP JULY 2008 295 UDDER - MICROBIOLOGY GASTROINTESTINAL
Metacam is an anti-inflammatory medicine used in cattle, pigs, horses, dogs, cats and guinea pigs.
 EMA/CVMP/259397/2006 EMEA/V/C/000033 An overview of Metacam and why it is authorised in the EU What is Metacam and what is it used for? Metacam is an anti-inflammatory medicine used in cattle, pigs, horses,
EMA/CVMP/259397/2006 EMEA/V/C/000033 An overview of Metacam and why it is authorised in the EU What is Metacam and what is it used for? Metacam is an anti-inflammatory medicine used in cattle, pigs, horses,
Medical terminology tests. Dr masoud sirati nir
 Circle the term that best completes the meaning of the Following sentences : 1. A physician who specializes in administering anesthetic agents before and during surgery a) anesthetist b) psychologist c)
Circle the term that best completes the meaning of the Following sentences : 1. A physician who specializes in administering anesthetic agents before and during surgery a) anesthetist b) psychologist c)
PREVALENCE OF RENAL DISORDERS IN DOGS A CLINICAL STUDY
 Int. J. Agric.Sc & Vet.Med. 2014 Satish Kumar Karlapudi and Srikanth Kandula, 2014 Research Paper ISSN 2320-3730 www.ijasvm.com Vol. 2, No. 3, August 2014 2014 www.ijasvm.com. All Rights Reserved PREVALENCE
Int. J. Agric.Sc & Vet.Med. 2014 Satish Kumar Karlapudi and Srikanth Kandula, 2014 Research Paper ISSN 2320-3730 www.ijasvm.com Vol. 2, No. 3, August 2014 2014 www.ijasvm.com. All Rights Reserved PREVALENCE
PVMA Veterinary Conference Fall 2018 Craig B. Webb, PhD, DVM, DACVIM. Feline Triaditis: Fact or Philosophy
 PVMA Veterinary Conference Fall 2018 Craig B. Webb, PhD, DVM, DACVIM Feline Triaditis: Fact or Philosophy Learning Objectives 1. To provide clinicians with an up-to-date assessment of the 3 components
PVMA Veterinary Conference Fall 2018 Craig B. Webb, PhD, DVM, DACVIM Feline Triaditis: Fact or Philosophy Learning Objectives 1. To provide clinicians with an up-to-date assessment of the 3 components
Acute Pyelonephritis POAC Guideline
 Acute Pyelonephritis POAC Guideline Refer full regional pathway http://aucklandregion.healthpathways.org.nz/33444 EXCLUSION CRITERIA: COMPLICATED PYELONEPHRITIS Discuss with relevant specialist for advice
Acute Pyelonephritis POAC Guideline Refer full regional pathway http://aucklandregion.healthpathways.org.nz/33444 EXCLUSION CRITERIA: COMPLICATED PYELONEPHRITIS Discuss with relevant specialist for advice
SOP #: Page: 1 of 6 Rodent Analgesia
 Comparative Medicine Page: 1 of 6 Rodent Analgesia The intent of this Standard Operating Procedure (SOP) is to describe commonly used analgesics provided to rodents housed at Comparative Medicine (CM).
Comparative Medicine Page: 1 of 6 Rodent Analgesia The intent of this Standard Operating Procedure (SOP) is to describe commonly used analgesics provided to rodents housed at Comparative Medicine (CM).
Prophylactic antibiotic timing and dosage. Dr. Sanjeev Singh AIMS, Kochi
 Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Prophylactic antibiotic timing and dosage Dr. Sanjeev Singh AIMS, Kochi Meaning - Webster Medical Definition of prophylaxis plural pro phy lax es \-ˈlak-ˌsēz\play : measures designed to preserve health
Australian and New Zealand College of Veterinary Scientists. Fellowship Examination. Small Animal Medicine Paper 1
 Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2014 Small Animal Medicine Paper 1 Perusal time: Twenty (20) minutes Time allowed: Four (4) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2014 Small Animal Medicine Paper 1 Perusal time: Twenty (20) minutes Time allowed: Four (4) hours after perusal Answer
2011 ASPCA. All Rights Reserved.
 1 Community Cats at the Spay/Neuter Clinic Carolyn R. Brown, DVM Director of Surgery ASPCA Spay/Neuter Operations 2 Defining Community Cats Any cat presenting for spay/neuter surgery in a humane trap with
1 Community Cats at the Spay/Neuter Clinic Carolyn R. Brown, DVM Director of Surgery ASPCA Spay/Neuter Operations 2 Defining Community Cats Any cat presenting for spay/neuter surgery in a humane trap with
Rare presentations and Complications of Hepatic Hydatid Cysts
 Rare presentations and Complications of Hepatic Hydatid Cysts Poster No.: C-1926 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Kapoor, A. Arora, N. GUPTA, S. K. Puri ; Delhi/IN, NEW 1 2 3 3
Rare presentations and Complications of Hepatic Hydatid Cysts Poster No.: C-1926 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Kapoor, A. Arora, N. GUPTA, S. K. Puri ; Delhi/IN, NEW 1 2 3 3
Owned Animal Receipt of Service
 Owned Animal Receipt of Service Pet s Name: I understand that my pet must be fully vaccinated and that I must provide proof of vaccinations before my pet can be altered. If I do not have proof, the SPCA
Owned Animal Receipt of Service Pet s Name: I understand that my pet must be fully vaccinated and that I must provide proof of vaccinations before my pet can be altered. If I do not have proof, the SPCA
THERAPY OF ANAEROBIC INFECTIONS LUNG ABSCESS BRAIN ABSCESS
 THERAPY OF ANAEROBIC INFECTIONS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu LUNG ABSCESS A lung abscess is a localized pus cavity in
THERAPY OF ANAEROBIC INFECTIONS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu LUNG ABSCESS A lung abscess is a localized pus cavity in
Small Animal Medicine
 2017 AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS MEMBERSHIP GUIDELINES Small Animal Medicine INTRODUCTION These Membership Guidelines should be read in conjunction with the Membership Candidate
2017 AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS MEMBERSHIP GUIDELINES Small Animal Medicine INTRODUCTION These Membership Guidelines should be read in conjunction with the Membership Candidate
Burn Infection & Laboratory Diagnosis
 Burn Infection & Laboratory Diagnosis Introduction Burns are one the most common forms of trauma. 2 million fires each years 1.2 million people with burn injuries 100000 hospitalization 5000 patients die
Burn Infection & Laboratory Diagnosis Introduction Burns are one the most common forms of trauma. 2 million fires each years 1.2 million people with burn injuries 100000 hospitalization 5000 patients die
SSI PREVENTION - CORRECT AND SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS
 SSI PREVENTION - CORRECT AN SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS Things you should know! There is wide consensus on specific procedures that warrant antibiotic prophylaxis as well as in which procedures
SSI PREVENTION - CORRECT AN SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS Things you should know! There is wide consensus on specific procedures that warrant antibiotic prophylaxis as well as in which procedures
NSAID Toxicity in Dogs & Cats Beware of Ibuprofen!
 NSAID Toxicity in Dogs & Cats Beware of Ibuprofen! One of the most common drug toxicities in companion animal medicine is accidental ingestion of over-the-counter non-steroid anti-inflammatory (NSAID)
NSAID Toxicity in Dogs & Cats Beware of Ibuprofen! One of the most common drug toxicities in companion animal medicine is accidental ingestion of over-the-counter non-steroid anti-inflammatory (NSAID)
Instructions For Completing The Mri Request Form
 Instructions For Completing The Mri Request Form Section I Referring Veterinarian Information Always include YOUR NAME, the HOSPITAL NAME, and a contact TELEPHONE NUMBER. In the event we have questions
Instructions For Completing The Mri Request Form Section I Referring Veterinarian Information Always include YOUR NAME, the HOSPITAL NAME, and a contact TELEPHONE NUMBER. In the event we have questions
