Novel avulsion pattern of the left principal bronchus with involvement of the carina and caudal thoracic trachea in a cat
|
|
|
- Elisabeth Higgins
- 5 years ago
- Views:
Transcription
1 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich Year: 2014 Novel avulsion pattern of the left principal bronchus with involvement of the carina and caudal thoracic trachea in a cat Schmierer, Philipp A; Schwarz, Andrea; Bass, Danielle A; Knell, Sebastian Christoph Abstract: A 2-year-old, 4.5 kg, neutered male domestic shorthair cat was presented to the emergency service with dyspnoea, anorexia and apathetic behaviour. Thoracic radiographs showed typical signs for a thoracic trauma and a tracheal lesion in the region of the carina consistent with pseudoairway formation. Computed tomography (CT) was performed in the conscious cat to avoid aggravation of air leakage associated with ventilation. The additional CT findings were consistent with a novel pattern of a traumatic avulsion of the left principal bronchus expanding into the carina and caudal thoracic trachea. Despite the complex avulsion pattern successful treatment was achieved surgically by performing an endto-end anastomosis via a fifth right intercostal lateral thoracotomy. The cat was ventilated with a feeding tube and jet ventilation throughout. The cat showed excellent recovery 6 months after surgery. DOI: Posted at the Zurich Open Repository and Archive, University of Zurich ZORA URL: Journal Article Accepted Version Originally published at: Schmierer, Philipp A; Schwarz, Andrea; Bass, Danielle A; Knell, Sebastian Christoph (2014). Novel avulsion pattern of the left principal bronchus with involvement of the carina and caudal thoracic trachea in a cat. Journal of Feline Medicine and Surgery, 16(8): DOI:
2 1 Case Report A novel avulsion pattern of the left principal bronchus with involvement of the carina and caudal thoracic trachea in a cat Philipp A Schmierer, Andrea Schwarz, Danielle A Bass, Sebastian Christoph Knell Vetsuisse Faculty University of Zurich, Zurich, Switzerland Philipp Schmierer med.vet, Vetsuisse Faculty University of Zurich, Winterthurerstr. 260, Zurich, CH-8057, Switzerland, pschmierer@vetclinics.uzh.ch Summary A two-year-old, 4.5 kg, neutered male domestic shorthair cat was presented to the emergency service with dyspnoea, anorexia and apathetic behaviour. Thoracic radiographs showed typical signs for a thoracic trauma and a tracheal lesion in the region of the carina consistent with pseudoairway formation. CT was performed in the conscious cat to avoid aggravation of air leakage associated with ventilation. The additional CT findings were consistent with a novel pattern of a traumatic avulsion of the left principal bronchus expanding into the carina and caudal thoracic trachea. Despite the complex avulsion pattern successful treatment was achieved surgically by performing an end-to-end anastomosis via a fifth right intercostal lateral thoracotomy. The cat was ventilated with a feeding tube and jet ventilation throughout. The cat showed excellent recovery six months after surgery Keywords Bronchial avulsion, cat, pseudoairway Intrathoracic tracheal avulsion is a rare but well described injury in the cat. 1,2,3,4
3 A blunt trauma with hyperextension of the head and neck is assumed to be the initiating cause typically leading to an avulsion 1 to 4 cm cranial to the bifurcation of the trachea representing its weakest point. In some circumstances avulsion of a principal bronchus is possible. 3,4,5 In the presented case a novel avulsion pattern was observed involving the bifurcation, the carina and the caudal trachea. After an avulsion injury, intact tracheal adventitia as well as thickening of mediastinal tissue is thought to maintain the airway lumen enabling ventilation leading to a condition described as pseudoairway. 3 However the narrowing at both avulsed 34 ends of the injury can result in stenosis. 2,3 Resection of the stenosed ends of the avulsed trachea followed by anastomosis is described as the treatment of choice. 3,4,5,6 This case serves to report a completely novel avulsion pattern including its diagnostic work up on a conscious patient and its subsequent surgical repair. A two-year-old, 4.5 kg, neutered male domestic shorthaired cat was presented to the emergency service with dyspnoea, anorexia and apathetic behaviour for two days. A traumatic history was suspected. Tachypnoea and increased inspiratory lung sounds were present on the right side on auscultation, whereas lung sounds were diminished on the left side. Other vital parameters were within normal limits as well as serum biochemistry and haematology. Initially the cat was treated with intravenous Ringers Lactate solution (Ringer Lactate, Fresenius Medical Care AG&Co.) at maintenance rate (2ml/kg/h) and buprenorphine (20 µg/kg q6h Temgesic, Reckitt Benckiser). Thoracic radiographs revealed moderate pneumothorax, pleural effusion, pneumomediastinum and pneumoretroperitoneum. The base of the left mainstem bronchus appeared spherically enlarged and could not be followed to the periphery, raising the suspicion of an airway laceration (Figure 1). Computed tomography was scheduled for the following day to assess severity and extent of the lesion. Thoracocentesis was performed and examination of the fluid was consistent with the diagnosis of haemothorax. The cat was kept in an oxygen cage with continuous respiratory monitoring.
4 Computed tomography was performed with a multi row helical CT unit (Brilliance16, Philips AG) using 16 detector rows. Due to continuous concern regarding ventilation associated complications in anaesthesia, the study was performed with the animal awake in an appropriately sized conventional cardboard box, allowing oxygen supply and air circulation via small designated holes. The resulting plain scan was only minimally compromised by motion artefacts. Obliquity of patient positioning was corrected by adjusting the multiplanar reconstructions. Scan direction was cranio-caudal using a slice thickness of 1.0mm. Scan parameters were kv 120, ma 183, collimator pitch and 0.75 second tube rotation time. The field of view was adjusted to the cardboard box. The raw data was reconstructed to image series with 1mm slices in a matrix of 512 dpi with an overlap of 33% in a soft tissue, bone and lung algorithm. The images were exported to a work station (OsiriX v bit, DICOM Viewer. See and multiplanar reconstructions were evaluated in appropriate windows (WL/WW): soft tissue (40/350), bone (300/1500) and pulmonary window (- 500/1400). The base of the left mainstembronchus was extensively enlarged over a length of 11.4mm, caudal to which it abruptly decreased in size with ill defined bronchial borders and tapered to the periphery. The left caudal lung lobe was aerated, whereas both parts of the left cranial lung lobe appeared isoattenuating to soft tissue, with only mild volume loss and persistent bronchial aeration. The right caudal mainstem bronchus was normal. Right lung lobe borders were mildly retracted. Moderate gas accumulations were visible around the mediastinal structures, expanding caudally into the retroperitoneal space and into subcutaneous and interfascial planes (Figure 2). The resulting diagnosis was rupture of the left mainstem bronchus, involving the carina, with secondary moderate pneumomediastinum. Following intramuscular ketamine (7 mg/kg, Narketan, Vétoquinol), midazolam (0.1 mg/kg, Dormicum, Roche Pharma) and medetomidine (2 µg/kg; Dorbene), anaesthesia was induced
5 with intravenous alfaxalone (1.3 mg/kg; Alfaxan, Vétoquinol) and maintained with alfaxalone (4.4-8 mg/kg/h), medetomidine (0.5-1 µg/kg/h) and fentanyl (5-10 µg/kg/h, Sintenyl, Sintetica SA) infusions. The trachea was intubated with a cuffed 4.5mm endotracheal tube (Mallinckrodt, Covidien) just beyond the larynx. The cat was allowed to breathe spontaneously. The bifurcation of the trachea was approached through a fifth right intercostal thoracotomy according to the description of White and Milner. 3 A feeding tube (Paediatric Feeding Tube, Mallinckrodt, 5 FR) was advanced through the endotracheal tube lumen and connected to a manual jet ventilator (Manujet III, VBM Medizintechnik). Manual jet ventilation with driving pressures between bar, variable frequency and FiO 2 of 1.0 was initiated thereafter. The effectiveness of ventilation was visually assessed by the degree of lung inflation. The azygos vein was separated by blunt preparation and ligated. The caudal trachea as well as the bifurcation and the principal bronchi were isolated by a combination of sharp and blunt dissection and the oesophagus as well as the cranial vena cava were retracted. A pseudoairway was recognized in the area of the bifurcation. It was entered with a stab incision, which allowed observation of the two avulsed sites. At this state the feeding tube was advanced into the right bronchus under visual control. An oblique avulsion of the left principal bronchus with involvement of the carina and the distal trachea was detected (Figure 3). When a decrease in arterial haemoglobin oxygen saturation and visual lung deflation occurred during opening of the pseudoairway membrane, the injured airway was digitally occluded. The proximal and distal end of the avulsed segment was transected in the cartilage as close as possible to the stenosed ends. Along the laceration the carina had to be resected to achieve proper anastomosis. Single interrupted 4-0 Polydioxanone (PDS, Ethicon, Johnson & Johnson Medical GmbH) sutures were pre-placed in the proximal and distal segment, starting at the dorsal aspect to facilitate best visibility. Most of the sutures were placed around
6 cartilaginous rings. Due to the particular shape of the avulsion some of the sutures had to be placed through the end of cartilaginous rings. Mechanical ventilation was started after tying the last suture and feeding tube removal. Warm sterile Ringers Lactate was used to lavage the surgical site and to check for an airtight seal. A thoracic drain was placed, the thorax was closed routinely and during closure a wound catheter (MILA Diffusion/Wound Catheter, MILA International, Inc.) was placed for local bupivacaine (0.5 mg/kg q6h, Carbostesin 0.5%, AstraZeneca AG) administration. Anaesthetic recovery was uneventful. Medetomidine infusion ( μg/kg/h), buprenorphine (20 μg/kg q6h) and intrapleural bupivacaine (0.5 mg/kg q6h) administration was continued postoperatively. The thoracic drain was removed 36 hours after surgery as thoracic radiographs showed no signs of pneumothorax or persistent pseudoairway. The cat was discharged three days later. Presentation at two weeks and four weeks after surgery showed the patient in a good condition without clinical signs of respiratory abnormalities. At telephone follow up six months after surgery, the owners reported a normal condition of the cat without any signs of respiratory compromise. A traumatic incident is considered to be the most common reason for avulsion injury of the intrathoracic trachea 4 and remains most likely in the presented case. A recent case report described one report of an avulsion injury of a principal bronchus in a cat with a notional traumatic episode, however in that case the bifurcation, the carina and the distal trachea 124 remained unaffected. 5 The reason for the atypical and novel confirmation of the avulsion injury described in this case report remains unclear. Similar injuries are described as avulsion of the main bronchus with stellate tear in human medicine. The reason for this type of injury is unexplained. 7 The cat showed apathetic behaviour for two days prior to the time of presentation. White and Milner described two distinct clinical presentations with the first to be an acute onset dyspnoea and respiratory compromise immediately after the injury and the second a more
7 chronic exertional dyspnoea combined with exercise intolerance appearing several days to weeks after the traumatic episode. 3 Thoracic radiographs initially had raised the suspicion of a discontinuity of the borders of the left mainstem bronchus, resulting in a pseudoairway formation. The latter is described in tracheal lacerations 8, but is expected to develop in a similar manner in bronchial avulsions. 4 Considering the aforementioned, the history of this cat is most consistent with a more chronic avulsion injury. The CT study allowed a distinct characterization of the bronchial lesion, hence facilitating surgical and anaesthetic preparation. Being able to obtain a diagnostic study of a critical patient in an awake state by creating a confined environment by such a simple device as a cardboard box was beneficial. The surgical approach via a right lateral thoracotomy to the tracheal bifurcation gave excellent exposure as previously described. Left lateral thoracotomy would have restricted the exposure by the descending thoracic aorta and the thoracic oesophagus. 5 The authors conclude that avulsion injury of the principal bronchus with involvement of the carina, the bifurcation and the distal trachea is a rare condition, which can be successfully surgically repaired, even in cases with complex avulsion patterns. However it has to be taken into consideration, that anaesthetic management of these patients is unpredictable and challenging. Size and avulsion shape did not allow one-lung ventilation. 9 Selective bronchus intubation with subsequent jet ventilation was a feasible alternative 9, although hypercapnia, hypoxemia and barotrauma can occur References 1. Ryan CO and Smith RA. Seperation of tracheal rings in a cat ( What is your diagnosis?). J Am Vet Med Assoc 1972; 161:
8 Jörger K, Flückiger M and Geret U. Ruptur der Trachea bei drei Katzen. Berl Munch Tierarztl Wochenschr 1988; 101: White RN and Milner HR. Intrathoracic tracheal avulsion in three cats. J Small Anim Pract 1995; 36: White RN and Burton CA. Surgical management of intrathoracic tracheal avulsion in cats: longterm results in 9 consecutive cases. Vet Surg 2000; 29: White RN and Oakley MR. Left principal bronchus rupture in a cat. J Small Anim Pract 2001; 42: Griffiths LG, Sullivan M and Lerche P. Intathoracic tracheal avulsion and pseudodiverticulum following pneumomediastinum in a cat. Vet Rec 1998; 142: Grover FL, Ellestad C, Arom KV, et al. Diagnosis and management of major tracheobronchial injuries. Ann of Thorac Surg 1979; 28: Zerenner DM, Agnello KA and Carberry CA. What is your diagnosis? Gas-filled spherical dilatation of the trachea at the level of T3 through T5 vertebrae and narrowing of the trachea lumen at T5. J Am Vet Med Assoc 2003; 12: Mosing M, Iff I and Moens Y. Endoscopic removal of a bronchial carcinoma in a dog using one-lung ventilation. Vet Surg 2008; 37:
9 Chin JH, Lee EH, Choi DK, et al. High frequency jet ventilation of one lung using a 184 bronchial blocker of Univent during carinal resection. J Korean Med Sci 2010; 25:
Gastric Dilatation-Volvulus
 Gastric Dilatation-Volvulus The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery. Only veterinarians who have successfully completed the certification requirements
Gastric Dilatation-Volvulus The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery. Only veterinarians who have successfully completed the certification requirements
This SOP presents commonly used anesthetic regimes in rabbits.
 Comparative Medicine SOP #: 103. 01 Page: 1 of 7 Rabbit Anaesthesia The intent of this Standard Operating Procedure (SOP) is to describe commonly used methods to anesthetize rabbits at Comparative Medicine
Comparative Medicine SOP #: 103. 01 Page: 1 of 7 Rabbit Anaesthesia The intent of this Standard Operating Procedure (SOP) is to describe commonly used methods to anesthetize rabbits at Comparative Medicine
SEVERE AND EXTENSIVE BITE WOUND ON A FLANK AND ABDOMEN OF AN IRISH WOLF HOUND TREATED WITH DELAYED PRIMARY CLOSURE AND VETGOLD
 SEVERE AND EXTENSIVE BITE WOUND ON A FLANK AND ABDOMEN OF AN IRISH WOLF HOUND TREATED WITH DELAYED PRIMARY CLOSURE AND VETGOLD PRESENTATION & HISTORY A three-year-old male neutered Irish Wolf Hound weighing
SEVERE AND EXTENSIVE BITE WOUND ON A FLANK AND ABDOMEN OF AN IRISH WOLF HOUND TREATED WITH DELAYED PRIMARY CLOSURE AND VETGOLD PRESENTATION & HISTORY A three-year-old male neutered Irish Wolf Hound weighing
Surgery of pulmonary hydatid cystthe Barrett technique
 Surgery of pulmonary hydatid cystthe Barrett technique IVAN LICHTER Department of Surgery, University of Otago Medical School, Dunedin, New Zealand Thorax (1972), 27, 529. A number of methods have been
Surgery of pulmonary hydatid cystthe Barrett technique IVAN LICHTER Department of Surgery, University of Otago Medical School, Dunedin, New Zealand Thorax (1972), 27, 529. A number of methods have been
"Serpent" Sign, "Double Arch" Sign and "Air-Bubble"Sign in a case of Ruptured Hydatid Cyst-A Case Report
 Article ID: WMC004602 ISSN 2046-1690 "Serpent" Sign, "Double Arch" Sign and "Air-Bubble"Sign in a case of Ruptured Hydatid Cyst-A Case Report Peer review status: No Corresponding Author: Dr. Dipti Gothi,
Article ID: WMC004602 ISSN 2046-1690 "Serpent" Sign, "Double Arch" Sign and "Air-Bubble"Sign in a case of Ruptured Hydatid Cyst-A Case Report Peer review status: No Corresponding Author: Dr. Dipti Gothi,
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Small Animal Surgery Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2018 Small Animal Surgery Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2018 Small Animal Surgery Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after perusal Answer
Canine and Feline Foreign Bodies To Cut or Not to Cut? Dr. Jinelle Webb, MSc, DVSc, Diplomate ACVIM
 Canine and Feline Foreign Bodies To Cut or Not to Cut? Dr. Jinelle Webb, MSc, DVSc, Diplomate ACVIM Typical Objects Bones/Rawhide Toys and Balls Greenies Fish hooks Towels, Socks Underwear Nylons Grass
Canine and Feline Foreign Bodies To Cut or Not to Cut? Dr. Jinelle Webb, MSc, DVSc, Diplomate ACVIM Typical Objects Bones/Rawhide Toys and Balls Greenies Fish hooks Towels, Socks Underwear Nylons Grass
Treatment of septic peritonitis
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Treatment of septic peritonitis Author : Andrew Linklater Categories : Companion animal, Vets Date : November 2, 2016 Septic
Intestinal linear foreign body
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Intestinal linear foreign body Author : Sally Birch Categories : Companion animal, Vets Date : February 6, 2017 Your first
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Intestinal linear foreign body Author : Sally Birch Categories : Companion animal, Vets Date : February 6, 2017 Your first
OESOPHAGEAL FOREIGN BODY IN A CAT: CASE REPORT
 Scientific Works. Series C. Veterinary Medicine. Vol. LXII (2) ISSN 2065-1295; ISSN 2343-9394 (CD-ROM); ISSN 2067-3663 (Online); ISSN-L 2065-1295 Abstract OESOPHAGEAL FOREIGN BODY IN A CAT: CASE REPORT
Scientific Works. Series C. Veterinary Medicine. Vol. LXII (2) ISSN 2065-1295; ISSN 2343-9394 (CD-ROM); ISSN 2067-3663 (Online); ISSN-L 2065-1295 Abstract OESOPHAGEAL FOREIGN BODY IN A CAT: CASE REPORT
The Journal of Veterinary Medical Science
 Advance Publication The Journal of Veterinary Medical Science Accepted Date: 25 Jul 2017 J-STAGE Advance Published Date: 7 Aug 2017 1 2 3 Category: Wildlife Science Type of paper: Note Running head: Oophorosalpingectomy
Advance Publication The Journal of Veterinary Medical Science Accepted Date: 25 Jul 2017 J-STAGE Advance Published Date: 7 Aug 2017 1 2 3 Category: Wildlife Science Type of paper: Note Running head: Oophorosalpingectomy
CODING GUIDELINES CODING GUIDELINES - OPCS NEW PAIR CODES...6 ERRATA...7. No. 18 May, 2006
 CODING GUIDELINES No. 18 May, 2006 Please note that the Coding Advisory Service Telephone Number is 0131-275-7283. The number is manned Tuesday to Thursday from 09.00 to 17.00 hrs. The link for previous
CODING GUIDELINES No. 18 May, 2006 Please note that the Coding Advisory Service Telephone Number is 0131-275-7283. The number is manned Tuesday to Thursday from 09.00 to 17.00 hrs. The link for previous
RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS
 RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS I. Purpose/Scope These guidelines apply to all surgical procedures performed on animals at Mississippi State University in which the animals
RESEARCH AND TEACHING SURGERY GUIDELINES FOR MSU-OWNED ANIMALS I. Purpose/Scope These guidelines apply to all surgical procedures performed on animals at Mississippi State University in which the animals
Animal, Plant & Soil Science
 Animal, Plant & Soil Science Lesson C5-9 Veterinary Terminology Interest Approach Gather some common veterinary tools (e.g., scissors, forceps, and scalpels). Ask the students what each item is and for
Animal, Plant & Soil Science Lesson C5-9 Veterinary Terminology Interest Approach Gather some common veterinary tools (e.g., scissors, forceps, and scalpels). Ask the students what each item is and for
Feline blood transfusions: preliminary considerations
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Feline blood transfusions: preliminary considerations Author : Andrea Harvey Categories : RVNs Date : September 1, 2011 ABSTRACT
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Feline blood transfusions: preliminary considerations Author : Andrea Harvey Categories : RVNs Date : September 1, 2011 ABSTRACT
NUMBER: R&C-ARF-10.0
 1. PURPOSE PAGE 1 OF 6 This policy describes the procedures for keeping and maintaining animal medical records. This procedure is approved by the Creighton University Institutional Animal Care and Use
1. PURPOSE PAGE 1 OF 6 This policy describes the procedures for keeping and maintaining animal medical records. This procedure is approved by the Creighton University Institutional Animal Care and Use
Pectus Excavatum (Funnel Chest) Dr Hasan Nugud Consultant Paediatric Surgeon
 Pectus Excavatum (Funnel Chest) Dr Hasan Nugud Consultant Paediatric Surgeon Pectus excavatum Pectus excavatum (PE) is an abnormal development of the rib cage where the breastbone (sternum) caves in,
Pectus Excavatum (Funnel Chest) Dr Hasan Nugud Consultant Paediatric Surgeon Pectus excavatum Pectus excavatum (PE) is an abnormal development of the rib cage where the breastbone (sternum) caves in,
Introduction. Rabbit Respiratory Disease. Lecture Outline. Pre-consult. Initial presentation. History 26/01/2013
 Introduction Rabbit Respiratory Disease Joanna Hedley BVM&S DZooMed (Reptilian) MRCVS Rabbit, Exotic Animal and Wildlife Clinician at R(D)SVS Obligate nasal breathers Small thorax Tendency to mask symptoms
Introduction Rabbit Respiratory Disease Joanna Hedley BVM&S DZooMed (Reptilian) MRCVS Rabbit, Exotic Animal and Wildlife Clinician at R(D)SVS Obligate nasal breathers Small thorax Tendency to mask symptoms
Anaesthesia for exploration of an oro-pharyngeal stick injury in a dog
 SAMPLE CASE REPORT Anaesthesia for exploration of an oro-pharyngeal stick injury in a dog Summary A 3-year-old Border collie dog weighing 17kg was presented for exploration of an oropharyngeal stick injury.
SAMPLE CASE REPORT Anaesthesia for exploration of an oro-pharyngeal stick injury in a dog Summary A 3-year-old Border collie dog weighing 17kg was presented for exploration of an oropharyngeal stick injury.
NUMBER: /2005
 Purpose PAGE 1 OF 7 The purpose of this policy is to describe the procedures for keeping and maintaining animal medical records. This procedure is approved by the Creighton University Institutional Animal
Purpose PAGE 1 OF 7 The purpose of this policy is to describe the procedures for keeping and maintaining animal medical records. This procedure is approved by the Creighton University Institutional Animal
Perioperative Care of Swine
 Swine are widely used in protocols that involve anesthesia and invasive surgical procedures. In order to ensure proper recovery of animals, preoperative, intraoperative and postoperative techniques specific
Swine are widely used in protocols that involve anesthesia and invasive surgical procedures. In order to ensure proper recovery of animals, preoperative, intraoperative and postoperative techniques specific
APPROACHING LIZARD COELIOTOMY
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk APPROACHING LIZARD COELIOTOMY Author : anonymous Categories : Vets Date : March 15, 2010 William Lewis provides a working
Vet Times The website for the veterinary profession https://www.vettimes.co.uk APPROACHING LIZARD COELIOTOMY Author : anonymous Categories : Vets Date : March 15, 2010 William Lewis provides a working
Welcome! 10/26/2015 1
 Welcome! Audio for this event is available via ReadyTalk Internet Streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Welcome! Audio for this event is available via ReadyTalk Internet Streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Companion Animal Fund Research Projects
 Companion Animal Fund Research Projects - 2016 Genomic, Phylogenetic, and Recombinational Characterization of Feline Herpesvirus Field Isolates Using Deep-Sequencing Technology Ellison Bentley, clinical
Companion Animal Fund Research Projects - 2016 Genomic, Phylogenetic, and Recombinational Characterization of Feline Herpesvirus Field Isolates Using Deep-Sequencing Technology Ellison Bentley, clinical
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Veterinary Anaesthesia and Critical Care Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2015 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours
Roundtable Presentation Pectus Excavatum
 Roundtable Presentation Pectus Excavatum Pectus Excavatum Anatomy Laura Saksa, MSN, CPNP Cleveland Clinic Children s Hospital Cleveland, OH Disclosure Information There were no financial interests or Relationships
Roundtable Presentation Pectus Excavatum Pectus Excavatum Anatomy Laura Saksa, MSN, CPNP Cleveland Clinic Children s Hospital Cleveland, OH Disclosure Information There were no financial interests or Relationships
Liver regeneration in dogs after CPSS surgery
 Liver regeneration in dogs after CPSS surgery D.J.E. Vrakking Abstract Background: The purpose of this study was to investigate macroscopic liver regeneration after congenital portosystemic shunt (CPSS)
Liver regeneration in dogs after CPSS surgery D.J.E. Vrakking Abstract Background: The purpose of this study was to investigate macroscopic liver regeneration after congenital portosystemic shunt (CPSS)
SOS EMERGENCY ANIMALS Please note that the following scenario(s) are generalized
 Suggested Tasks for Veterinary Students Volunteering at the VSPCA By Bosmat Gal, DVM Assistant to the President of the Animal Rescue League of Boston for International Programs Member of the VSPCA Advisory
Suggested Tasks for Veterinary Students Volunteering at the VSPCA By Bosmat Gal, DVM Assistant to the President of the Animal Rescue League of Boston for International Programs Member of the VSPCA Advisory
Australian and New Zealand College of Veterinary Scientists. Membership Examination. Veterinary Radiology (Small Animal) Paper 1
 Australian and New Zealand College of Veterinary Scientists Membership Examination June 2016 Veterinary Radiology (Small Animal) Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after
Australian and New Zealand College of Veterinary Scientists Membership Examination June 2016 Veterinary Radiology (Small Animal) Paper 1 Perusal time: Fifteen (15) minutes Time allowed: Two (2) hours after
Advanced Diagnostic Imaging Services
 Advanced Diagnostic Imaging Services 2 Welcome to Moorview Vets Moorview Vets are able to offer many diagnostic services, these include more advanced imaging modalities such as Computed Tomography (CT)
Advanced Diagnostic Imaging Services 2 Welcome to Moorview Vets Moorview Vets are able to offer many diagnostic services, these include more advanced imaging modalities such as Computed Tomography (CT)
DREXEL UNIVERSITY COLLEGE OF MEDICINE ANIMAL CARE AND USE COMMITTEE POLICY FOR PREOPERATIVE AND POSTOPERATIVE CARE FOR NON-RODENT MAMMALS
 DREXEL UNIVERSITY COLLEGE OF MEDICINE ANIMAL CARE AND USE COMMITTEE POLICY FOR PREOPERATIVE AND POSTOPERATIVE CARE FOR NON-RODENT MAMMALS OBJECTIVE: This policy is to ensure that appropriate provisions
DREXEL UNIVERSITY COLLEGE OF MEDICINE ANIMAL CARE AND USE COMMITTEE POLICY FOR PREOPERATIVE AND POSTOPERATIVE CARE FOR NON-RODENT MAMMALS OBJECTIVE: This policy is to ensure that appropriate provisions
T u l a n e U n i v e r s i t y I A C U C Guidelines for Rodent & Rabbit Anesthesia, Analgesia and Tranquilization & Euthanasia Methods
 T u l a n e U n i v e r s i t y I A C U C Guidelines for Rodent & Rabbit Anesthesia, Analgesia and Tranquilization & Euthanasia Methods Abbreviations: General Considerations IV = intravenous SC = subcutaneous
T u l a n e U n i v e r s i t y I A C U C Guidelines for Rodent & Rabbit Anesthesia, Analgesia and Tranquilization & Euthanasia Methods Abbreviations: General Considerations IV = intravenous SC = subcutaneous
CLINICAL ESSENTIAL HUDDLE CARD. All associates must comply with their state practice acts.
 CLINICAL ESSENTIAL HUDDLE CARD All associates must comply with their state practice acts. QUESTIONS FOR DISCUSSION Where can you find information about your state practice acts? If you are unclear of what
CLINICAL ESSENTIAL HUDDLE CARD All associates must comply with their state practice acts. QUESTIONS FOR DISCUSSION Where can you find information about your state practice acts? If you are unclear of what
2011 ASPCA. All Rights Reserved.
 1 Community Cats at the Spay/Neuter Clinic Carolyn R. Brown, DVM Director of Surgery ASPCA Spay/Neuter Operations 2 Defining Community Cats Any cat presenting for spay/neuter surgery in a humane trap with
1 Community Cats at the Spay/Neuter Clinic Carolyn R. Brown, DVM Director of Surgery ASPCA Spay/Neuter Operations 2 Defining Community Cats Any cat presenting for spay/neuter surgery in a humane trap with
Australian and New Zealand College of Veterinary Scientists. Fellowship Examination. Veterinary Anaesthesia and Critical Care Paper 1
 Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2016 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours
Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2016 Veterinary Anaesthesia and Critical Care Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours
Guide to Veterinary Surgery If you are like most people, you want to know what you
 Guide to Veterinary Surgery If you are like most people, you want to know what you are paying for and why things cost what they do. You will find that veterinary providers are all different, and you may
Guide to Veterinary Surgery If you are like most people, you want to know what you are paying for and why things cost what they do. You will find that veterinary providers are all different, and you may
Old Disease New Location Surgeons Be Alerted
 Old Disease New Location Surgeons Be Alerted K. B. Ashok Vol. 3 No. 4 (April 2011) International Journal of Collaborative Research on Internal Medicine & Public Health (IJCRIMPH) ISSN 1840-4529 Journal
Old Disease New Location Surgeons Be Alerted K. B. Ashok Vol. 3 No. 4 (April 2011) International Journal of Collaborative Research on Internal Medicine & Public Health (IJCRIMPH) ISSN 1840-4529 Journal
Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma
 Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma Lucio Petrizzi DVM DECVS Università degli Studi di Teramo Surgical site infections (SSI) Microbial contamination unavoidable Infection
Antimicrobial Selection and Therapy for Equine Musculoskeletal Trauma Lucio Petrizzi DVM DECVS Università degli Studi di Teramo Surgical site infections (SSI) Microbial contamination unavoidable Infection
The Royal College of Veterinary Surgeons DIPLOMA IN EQUINE SOFT TISSUE SURGERY PAPER I. (Basic Sciences) Tuesday 2 May 1995
 The Royal College of Veterinary Surgeons PAPER I (Basic Sciences) Tuesday 2 May 1995 10.00 a.m. to 1.00 p.m. (3 hours) SECTION A Two long answer questions of which a candidate must choose ONE question
The Royal College of Veterinary Surgeons PAPER I (Basic Sciences) Tuesday 2 May 1995 10.00 a.m. to 1.00 p.m. (3 hours) SECTION A Two long answer questions of which a candidate must choose ONE question
EXOTIC SMALL MAMMAL ANESTHETIC TECHNIQUES
 EXOTIC SMALL MAMMAL ANESTHETIC TECHNIQUES Jody Nugent-Deal, RVT, VTS (Anesthesia) and (Clinical Practice Exotic Companion Animal) Veterinary Medical Teaching Hospital University of California, Davis, CA
EXOTIC SMALL MAMMAL ANESTHETIC TECHNIQUES Jody Nugent-Deal, RVT, VTS (Anesthesia) and (Clinical Practice Exotic Companion Animal) Veterinary Medical Teaching Hospital University of California, Davis, CA
Update in Veterinary Medicine. Dr. Maria M. Crane Zoo Atlanta
 Update in Veterinary Medicine Dr. Maria M. Crane Zoo Atlanta Overview of Discussion Medical management of captive orangutans Preventative Medicine Anesthesia Protocols Vaccinations TB testing Current Health
Update in Veterinary Medicine Dr. Maria M. Crane Zoo Atlanta Overview of Discussion Medical management of captive orangutans Preventative Medicine Anesthesia Protocols Vaccinations TB testing Current Health
Proceedings of the International Congress of the Italian Association of Companion Animal Veterinarians
 www.ivis.org Proceedings of the International Congress of the Italian Association of Companion Animal Veterinarians June 8-10, 2012 - Rimini, Italy Next SCIVAC Congress: Mar. 8-10, 2013 Pisa, Italy SCIVAC
www.ivis.org Proceedings of the International Congress of the Italian Association of Companion Animal Veterinarians June 8-10, 2012 - Rimini, Italy Next SCIVAC Congress: Mar. 8-10, 2013 Pisa, Italy SCIVAC
Surgical Site Infections (SSIs)
 Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Surgical Site Infections (SSIs) Postoperative infections presenting at any level Incisional superficial (skin, subcutaneous tissue) Incisional deep (fascial plane and muscles) Organ/space related (anatomic
Anesthesia & analgesia in birds
 Anesthesia and analgesia in birds Yvonne R.A. van Zeeland, DVM, PhD, MVR, Dip. ECZM (avian) Division of Zoological Medicine, Utrecht University Anesthesia & analgesia in birds Yvonne van Zeeland DVM, MVR,
Anesthesia and analgesia in birds Yvonne R.A. van Zeeland, DVM, PhD, MVR, Dip. ECZM (avian) Division of Zoological Medicine, Utrecht University Anesthesia & analgesia in birds Yvonne van Zeeland DVM, MVR,
Jess Weidman, DVM, DACVIM- Cardiology CVCA Cardiac Care for Pets Dogwood Veterinary Emergency and Specialty
 Jess Weidman, DVM, DACVIM- Cardiology CVCA Cardiac Care for Pets Dogwood Veterinary Emergency and Specialty Diagnostics Cardiac auscultation Chest Radiographs BNP Genetic testing Case Scenarios Pre-anesthesia
Jess Weidman, DVM, DACVIM- Cardiology CVCA Cardiac Care for Pets Dogwood Veterinary Emergency and Specialty Diagnostics Cardiac auscultation Chest Radiographs BNP Genetic testing Case Scenarios Pre-anesthesia
AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS. Sample Exam Questions. Veterinary Practice (Small Animal)
 AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS Sample Exam Questions Veterinary Practice (Small Animal) Written Examination (Component 1) Written Paper 1 (two hours): Principles of Veterinary
AUSTRALIAN AND NEW ZEALAND COLLEGE OF VETERINARY SCIENTISTS Sample Exam Questions Veterinary Practice (Small Animal) Written Examination (Component 1) Written Paper 1 (two hours): Principles of Veterinary
SURGICAL MANAGEMENT OF VAGINAL HYPERPLASIA AND PROLAPSE IN A PUG BITCH
 Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN M Gokula 2321 9602 Krishnan www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report SURGICAL MANAGEMENT
Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN M Gokula 2321 9602 Krishnan www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report SURGICAL MANAGEMENT
BY TICKING YES TO ANY RULE ON THIS CHECKLIST YOU AGREE THAT THE FACILITY ALREADY COMPLIES WITH THAT STANDARD.
 Veterinary Facility Evaluated: Rule 25: Mobile animal services for private practitioners practicing from a registered physical veterinary facility and Compulsory Community Services facilities NAME OF THE
Veterinary Facility Evaluated: Rule 25: Mobile animal services for private practitioners practicing from a registered physical veterinary facility and Compulsory Community Services facilities NAME OF THE
BY TICKING YES TO ANY RULE ON THIS CHECKLIST YOU AGREE THAT THE FACILITY ALREADY COMPLIES WITH THAT STANDARD.
 Veterinary Facility Evaluated: Rule 32: Animal Research Facilities NAME OF THE FACILITY: Please note: 32 (1) Application for facility registration must include a detailed description of the work that will
Veterinary Facility Evaluated: Rule 32: Animal Research Facilities NAME OF THE FACILITY: Please note: 32 (1) Application for facility registration must include a detailed description of the work that will
3. ENSURING HUMANE EUTHANASIA OF LABORATORY ANIMALS
 Page 1 of 5 1. DEFINITION Euthanasia is the act of inducing humane death in an animal by a method that induces rapid loss of consciousness and death with a minimum of pain, discomfort, or distress. 2.
Page 1 of 5 1. DEFINITION Euthanasia is the act of inducing humane death in an animal by a method that induces rapid loss of consciousness and death with a minimum of pain, discomfort, or distress. 2.
Bacterial infections in the urinary tract
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Bacterial infections in the urinary tract Gerber, B Posted at the Zurich
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Bacterial infections in the urinary tract Gerber, B Posted at the Zurich
STANDARD OPERATING PROCEDURE #111 RAT ANESTHESIA
 STANDARD OPERATING PROCEDURE #111 RAT ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing rats. 2. RESPONSIBILITY Principal Investigators (PIs) and their research
STANDARD OPERATING PROCEDURE #111 RAT ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing rats. 2. RESPONSIBILITY Principal Investigators (PIs) and their research
UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee
 UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee Policy: Surgical Guidelines EFFECTIVE ISSUE DATE: 2/21/2005 REVISION DATE(s): 2/14/15; 3/19/2018 SCOPE To describe guidelines and considerations
UNIVERSITY OF PITTSBURGH Institutional Animal Care and Use Committee Policy: Surgical Guidelines EFFECTIVE ISSUE DATE: 2/21/2005 REVISION DATE(s): 2/14/15; 3/19/2018 SCOPE To describe guidelines and considerations
STERILIZED NYLON MOSQUITO NET FOR RECONSTRUCTION OF UMBILICAL HERNIA IN BUFFALOES
 Case Report Buffalo Bulletin (March 2014) Vol.33 No.1 STERILIZED NYLON MOSQUITO NET FOR RECONSTRUCTION OF UMBILICAL HERNIA IN BUFFALOES Vineet Kumar*, D.D. Mathew, R.A. Ahmad, M. Hoque, A.C. Saxena, Rekha
Case Report Buffalo Bulletin (March 2014) Vol.33 No.1 STERILIZED NYLON MOSQUITO NET FOR RECONSTRUCTION OF UMBILICAL HERNIA IN BUFFALOES Vineet Kumar*, D.D. Mathew, R.A. Ahmad, M. Hoque, A.C. Saxena, Rekha
Summary of Product Characteristics
 Summary of Product Characteristics 1 NAME OF THE VETERINARY MEDICINAL PRODUCT Narketan-10 100 mg/ml Solution for Injection. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml contains: Active substance
Summary of Product Characteristics 1 NAME OF THE VETERINARY MEDICINAL PRODUCT Narketan-10 100 mg/ml Solution for Injection. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml contains: Active substance
TITLE 9 EQUINE CLINIC
 TITLE 9 EQUIE CLIIC 1.0 General 1.1. The facility, 1.1.1. self-contained, 1.1.2. has a separate and distinct entrance directly from the street or, if the facility is in a building containing more than
TITLE 9 EQUIE CLIIC 1.0 General 1.1. The facility, 1.1.1. self-contained, 1.1.2. has a separate and distinct entrance directly from the street or, if the facility is in a building containing more than
POST-OPERATIVE ANALGESIA AND FORMULARIES
 POST-OPERATIVE ANALGESIA AND FORMULARIES An integral component of any animal protocol is the prevention or alleviation of pain or distress, such as that associated with surgical and other procedures. Pain
POST-OPERATIVE ANALGESIA AND FORMULARIES An integral component of any animal protocol is the prevention or alleviation of pain or distress, such as that associated with surgical and other procedures. Pain
A New Advancement in Anesthesia. Your clear choice for induction.
 A New Advancement in Anesthesia Your clear choice for induction. By Kirby Pasloske When using Alfaxan, patients should be continuously monitored, and facilities for maintenance of a patent airway, artificial
A New Advancement in Anesthesia Your clear choice for induction. By Kirby Pasloske When using Alfaxan, patients should be continuously monitored, and facilities for maintenance of a patent airway, artificial
Proceedings of the International Congress of the Italian Association of Companion Animal Veterinarians
 www.ivis.org Proceedings of the International Congress of the Italian Association of Companion Animal Veterinarians June 8-10, 2012 - Rimini, Italy Next SCIVAC Congress: Mar. 8-10, 2013 Pisa, Italy SCIVAC
www.ivis.org Proceedings of the International Congress of the Italian Association of Companion Animal Veterinarians June 8-10, 2012 - Rimini, Italy Next SCIVAC Congress: Mar. 8-10, 2013 Pisa, Italy SCIVAC
CAT AND DOG ANESTHESIA
 Document: ACUP104.03 Issue Date: 21 SEP 17; Effective Date: 21 SEP 17 Authorization: Dr. N. Place, IACUC Chair Author: E. Silvela (Revision) CAT AND DOG ANESTHESIA 1. PURPOSE 1.1. The purpose of this Animal
Document: ACUP104.03 Issue Date: 21 SEP 17; Effective Date: 21 SEP 17 Authorization: Dr. N. Place, IACUC Chair Author: E. Silvela (Revision) CAT AND DOG ANESTHESIA 1. PURPOSE 1.1. The purpose of this Animal
Leo: linear foreign body in a young cat
 Leo: linear foreign body in a young cat Linear foreign bodies can cause life-threatening illness in cats, with ingestion resulting in plication of the intestine and potentially perforation and peritonitis.
Leo: linear foreign body in a young cat Linear foreign bodies can cause life-threatening illness in cats, with ingestion resulting in plication of the intestine and potentially perforation and peritonitis.
Pedicle ties provide a rapid and safe method for feline ovariohysterectomy
 Pedicle ties provide a rapid and safe method for feline ovariohysterectomy K. Miller 1, W. Rekers 2, K. Ellis 2, K. Ellingsen 2, M. Milovancev 3 1 Oregon State University/Oregon Humane Society 2 Oregon
Pedicle ties provide a rapid and safe method for feline ovariohysterectomy K. Miller 1, W. Rekers 2, K. Ellis 2, K. Ellingsen 2, M. Milovancev 3 1 Oregon State University/Oregon Humane Society 2 Oregon
LOWER EYELID RECONSTRUCTIVE SURGERY AFTER SEBACEOUS GLAND ADENOMA RESECTION IN A GERMAN SHEPHERD DOG: A CASE REPORT
 Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN Rambabu 2321 9602 Kalaka www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report LOWER EYELID RECONSTRUCTIVE
Indo-Am. J. Agric. & Vet. Sci., 2014 ISSN Rambabu 2321 9602 Kalaka www.iajavs.com et al., 2014 Vol. 2, No. 3, September 2014 2014 Meghana Publications. All Rights Reserved Case Report LOWER EYELID RECONSTRUCTIVE
Animal Studies Committee Policy Rodent Survival Surgery
 Animal Studies Committee Policy Rodent Survival Surgery ASC Policy: To optimize animal health and well-being, survival surgery in rodents must be performed using sterile instruments, surgical gloves, masks
Animal Studies Committee Policy Rodent Survival Surgery ASC Policy: To optimize animal health and well-being, survival surgery in rodents must be performed using sterile instruments, surgical gloves, masks
Dexmedetomidine and its Injectable Anesthetic-Pain Management Combinations
 Back to Anesthesia/Pain Management Back to Table of Contents Front Page : Library : ACVC 2009 : Anesthesia/Pain Management : Dexmedetomidine Dexmedetomidine and its Injectable Anesthetic-Pain Management
Back to Anesthesia/Pain Management Back to Table of Contents Front Page : Library : ACVC 2009 : Anesthesia/Pain Management : Dexmedetomidine Dexmedetomidine and its Injectable Anesthetic-Pain Management
International Journal of Science, Environment and Technology, Vol. 7, No 3, 2018,
 International Journal of Science, Environment and Technology, Vol. 7, No 3, 2018, 872 876 ISSN 2278-3687 (O) 2277-663X (P) SURGICAL MANAGEMENT OF INTESTINAL OBSTRUCTION DUE TO BRISTLES OF SWEEP BROOM IN
International Journal of Science, Environment and Technology, Vol. 7, No 3, 2018, 872 876 ISSN 2278-3687 (O) 2277-663X (P) SURGICAL MANAGEMENT OF INTESTINAL OBSTRUCTION DUE TO BRISTLES OF SWEEP BROOM IN
Australian and New Zealand College of Veterinary Scientists. Fellowship Examination. Small Animal Surgery Paper 1
 Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2016 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer
Australian and New Zealand College of Veterinary Scientists Fellowship Examination June 2016 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer
SSI PREVENTION - CORRECT AND SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS
 SSI PREVENTION - CORRECT AN SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS Things you should know! There is wide consensus on specific procedures that warrant antibiotic prophylaxis as well as in which procedures
SSI PREVENTION - CORRECT AN SAFE SURGICAL ANTIBIOTIC PROPHYLAXIS Things you should know! There is wide consensus on specific procedures that warrant antibiotic prophylaxis as well as in which procedures
Patient Preparation. Surgical Team
 January 2019 www.nursingcenter.com Surgical Site Infection Prevention Surgical site infections (SSIs) are one of the most common and costly healthcare-associated infections in the United States (Smith
January 2019 www.nursingcenter.com Surgical Site Infection Prevention Surgical site infections (SSIs) are one of the most common and costly healthcare-associated infections in the United States (Smith
Dog Welfare Assessment App Guidance Document
 Dog Welfare Assessment App Guidance Document Introduction The Dog Welfare Assessment app has been developed to allow you to self-assess the welfare of dogs in your CNR (catch neuter return) programme.
Dog Welfare Assessment App Guidance Document Introduction The Dog Welfare Assessment app has been developed to allow you to self-assess the welfare of dogs in your CNR (catch neuter return) programme.
Wound types and healing part three: classification of injuries
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Wound types and healing part three: classification of injuries Author : Louise O Dwyer Categories : RVNs Date : July 1, 2010
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Wound types and healing part three: classification of injuries Author : Louise O Dwyer Categories : RVNs Date : July 1, 2010
Multiple pulmonary hydatid cysts
 Postgrad. med. J. (December 1967) 43, 774-778. THE LUNG is the second commonest site in man, where the intermediate larval-cysticercal stage of Echinococcus granulosus develops. It is not unusual to find
Postgrad. med. J. (December 1967) 43, 774-778. THE LUNG is the second commonest site in man, where the intermediate larval-cysticercal stage of Echinococcus granulosus develops. It is not unusual to find
Reptile Anesthesia Thomas H. Boyer, DVM, DABVP (Reptile & Amphibian Practice) Pet Hospital of Penasquitos, San Diego, CA, USA This talk will focus on
 Reptile Anesthesia Thomas H. Boyer, DVM, DABVP (Reptile & Amphibian Practice) Pet Hospital of Penasquitos, San Diego, CA, USA This talk will focus on reptile anesthesia by species presentation, excluding
Reptile Anesthesia Thomas H. Boyer, DVM, DABVP (Reptile & Amphibian Practice) Pet Hospital of Penasquitos, San Diego, CA, USA This talk will focus on reptile anesthesia by species presentation, excluding
Heartworm Disease in Dogs
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Heartworm Disease in Dogs Basics OVERVIEW Disease caused by infestation with heartworms
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Heartworm Disease in Dogs Basics OVERVIEW Disease caused by infestation with heartworms
M5 MEQs 2016 Session 3: SOB 18/11/16
 M5 MEQs 2016 Session 3: SOB 18/11/16 http://tinyurl.com/hn7qzt3 Question 1 Ms Tan is a 52 year old female with no past medical history. She comes to the emergency department presenting with a fever for
M5 MEQs 2016 Session 3: SOB 18/11/16 http://tinyurl.com/hn7qzt3 Question 1 Ms Tan is a 52 year old female with no past medical history. She comes to the emergency department presenting with a fever for
Some important information about the fetus and the newborn puppy
 Some important information about the fetus and the newborn puppy Dr. Harmon Rogers Veterinary Teaching Hospital Washington State University Here are a few interesting medical details about fetuses and
Some important information about the fetus and the newborn puppy Dr. Harmon Rogers Veterinary Teaching Hospital Washington State University Here are a few interesting medical details about fetuses and
What s Your Diagnosis?
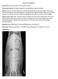 What s Your Diagnosis? Signalment: Maine Coone (8 month old, female intact) Presenting complaint: Lethargy, inappetence, serosanguinous vaginal discharge History: Lives with 11 other Maine Coone cats (males
What s Your Diagnosis? Signalment: Maine Coone (8 month old, female intact) Presenting complaint: Lethargy, inappetence, serosanguinous vaginal discharge History: Lives with 11 other Maine Coone cats (males
Health Products Regulatory Authority
 1 NAME OF THE VETERINARY MEDICINAL PRODUCT Ketamidor 100 mg/ml solution for injection 2 QUALITATIVE AND QUANTITATIVE COMPOSITION 1 ml contains: Active substance: Ketamine (as hydrochloride) Excipient:
1 NAME OF THE VETERINARY MEDICINAL PRODUCT Ketamidor 100 mg/ml solution for injection 2 QUALITATIVE AND QUANTITATIVE COMPOSITION 1 ml contains: Active substance: Ketamine (as hydrochloride) Excipient:
APPLICATION FOR LIVE ANIMAL USE IN TEACHING AT FAULKNER STATE COMMUNITY COLLEGE
 APPLICATION FOR LIVE ANIMAL USE IN TEACHING AT FAULKNER STATE COMMUNITY COLLEGE MARK WITH AN X IN THE BOX FOR ONE OF THE FOLLOWING AND TYPE YOUR CURRENT PROTOCOL NUMBER IF NEEDED: X New application Amendment
APPLICATION FOR LIVE ANIMAL USE IN TEACHING AT FAULKNER STATE COMMUNITY COLLEGE MARK WITH AN X IN THE BOX FOR ONE OF THE FOLLOWING AND TYPE YOUR CURRENT PROTOCOL NUMBER IF NEEDED: X New application Amendment
Certificate in Advanced Veterinary Practice C-VDI.3 Small Animal Diagnostic Imaging (Soft Tissue) Module Outline
 Certificate in Advanced Veterinary Practice C-VDI.3 Small Animal Diagnostic Imaging (Soft Tissue) Module Outline Module Leader: Elizabeth Baines MA VetMB DVR DipECVDI MRCVS Lecturer in Veterinary Radiology
Certificate in Advanced Veterinary Practice C-VDI.3 Small Animal Diagnostic Imaging (Soft Tissue) Module Outline Module Leader: Elizabeth Baines MA VetMB DVR DipECVDI MRCVS Lecturer in Veterinary Radiology
Digital flexor tendon contracture treated by tenectomy: different clinical presentations in three cats
 597237JOR0010.1177/2055116915597237Journal of Feline Medicine and Surgery Open ReportsCabon et al research-article2015 Case Series Digital flexor tendon contracture treated by tenectomy: different clinical
597237JOR0010.1177/2055116915597237Journal of Feline Medicine and Surgery Open ReportsCabon et al research-article2015 Case Series Digital flexor tendon contracture treated by tenectomy: different clinical
Australian College of Veterinary Scientists. Fellowship Examination. Small Animal Surgery Paper 1
 Australian College of Veterinary Scientists Fellowship Examination June 2011 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer your choice
Australian College of Veterinary Scientists Fellowship Examination June 2011 Small Animal Surgery Paper 1 Perusal time: Twenty (20) minutes Time allowed: Three (3) hours after perusal Answer your choice
PROCEEDINGS OF THE NORTH AMERICAN VETERINARY CONFERENCE VOLUME 20 JANUARY 7-11, 2006 ORLANDO, FLORIDA
 PROCEEDINGS OF THE NORTH AMERICAN VETERINARY CONFERENCE VOLUME 20 JANUARY 7-11, 2006 ORLANDO, FLORIDA SMALL ANIMAL EDITION Reprinted in the IVIS website (http://www.ivis.org) with the permission of the
PROCEEDINGS OF THE NORTH AMERICAN VETERINARY CONFERENCE VOLUME 20 JANUARY 7-11, 2006 ORLANDO, FLORIDA SMALL ANIMAL EDITION Reprinted in the IVIS website (http://www.ivis.org) with the permission of the
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS
 VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
VCH PHC SURGICAL PROPHYLAXIS RECOMMENDATIONS CARDIAC Staphylococcus aureus, S. epidermidis, except for For patients with known MRSA colonization, recommend decolonization with Antimicrobial Photodynamic
Who should read this document 2. Key practice points 2. Background/ Scope/ Definitions 2. What is new in this version 3. Policy/Procedure/Guideline 3
 Antibiotic Prophylaxis in Cranial Neurosurgery Antibiotic Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): as above Authors Division: DCSS & Tertiary
Antibiotic Prophylaxis in Cranial Neurosurgery Antibiotic Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): as above Authors Division: DCSS & Tertiary
Surgical Cross Coder. Essential links from CPT codes to ICD-9-CM and HCPCS codes
 Essential links from CPT codes to ICD-9-CM and HCPCS codes 2016 Contents Introduction... iii Cardiovascular System...527 Digestive System...707 General...1 Integumentary System...9 Musculoskeletal System...173
Essential links from CPT codes to ICD-9-CM and HCPCS codes 2016 Contents Introduction... iii Cardiovascular System...527 Digestive System...707 General...1 Integumentary System...9 Musculoskeletal System...173
Perioperative Pain Management in Veterinary Patients
 Perioperative Pain Management in Veterinary Patients Doris H. Dyson, DVM, DVSc KEYWORDS Analgesia Surgical pain Dog Cat As veterinarians in the twenty-first century, we have an ethical responsibility to
Perioperative Pain Management in Veterinary Patients Doris H. Dyson, DVM, DVSc KEYWORDS Analgesia Surgical pain Dog Cat As veterinarians in the twenty-first century, we have an ethical responsibility to
Computed Tomography and 3D Reconstruction of the Respiratory Organs of the Egyptian Tortoise
 Computed Tomography and 3D Reconstruction of the Respiratory Organs of the Egyptian Tortoise (Testudo kleinmanni) A.S. M. Kamal Department of Anatomy and Embryology, Faculty of Veterinary Medicine, Sadat
Computed Tomography and 3D Reconstruction of the Respiratory Organs of the Egyptian Tortoise (Testudo kleinmanni) A.S. M. Kamal Department of Anatomy and Embryology, Faculty of Veterinary Medicine, Sadat
Specialist Referral Service Willows Information Sheets. Rigid endoscopy
 Specialist Referral Service Willows Information Sheets Rigid endoscopy Professor Rob White with a state-of-the-art rigid Karl Storz endoscope. Rigid endoscopy What is endoscopy? Endoscopy involves the
Specialist Referral Service Willows Information Sheets Rigid endoscopy Professor Rob White with a state-of-the-art rigid Karl Storz endoscope. Rigid endoscopy What is endoscopy? Endoscopy involves the
Antimicrobial Prophylaxis for Surgical and Non-surgical Procedures
 Antimicrobial Prophylaxis for Surgical and Non-surgical Procedures Written by: Dr Linda Jewes, Consultant Microbiologist Date: April 2016 Approved by: Drugs & Therapeutics Committee Date: September 2016
Antimicrobial Prophylaxis for Surgical and Non-surgical Procedures Written by: Dr Linda Jewes, Consultant Microbiologist Date: April 2016 Approved by: Drugs & Therapeutics Committee Date: September 2016
POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014
 POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014 The U.S.D.A Animal Welfare Act (9 CFR) requires use of aseptic
POLICY ON ASEPTIC RECOVERY SURGERY ON USDA REGULATED NONRODENT SPECIES Adopted by the University Committee on Animal Resources October 15, 2014 The U.S.D.A Animal Welfare Act (9 CFR) requires use of aseptic
Yosemite Pet Hospital, Inc
 Yosemite Pet Hospital, Inc Exceptional Care for Exceptional Pets Consumer Guide to Elective Surgery and Procedures Thank you for recognizing your pet may need to undergo an elective procedure such as spay
Yosemite Pet Hospital, Inc Exceptional Care for Exceptional Pets Consumer Guide to Elective Surgery and Procedures Thank you for recognizing your pet may need to undergo an elective procedure such as spay
EXAMINATION & ASSESSMENT On presentation, the receptionist should ask the client:
 STEP 1: Comprehensive Overview Overview Bite wounds constitute 10% 15% of acute injuries in dogs and cats admitted to veterinary practices. 1 All bite wounds warrant veterinary attention, regardless of
STEP 1: Comprehensive Overview Overview Bite wounds constitute 10% 15% of acute injuries in dogs and cats admitted to veterinary practices. 1 All bite wounds warrant veterinary attention, regardless of
Competencies for VETCEE Accredited Companion Animal Programmes
 Veterinary Continuous Education in Europe International non-profit association Competencies for VETCEE Accredited Companion Animal Programmes -- Approved by The VETCEE Board -- March 2016 Competences for
Veterinary Continuous Education in Europe International non-profit association Competencies for VETCEE Accredited Companion Animal Programmes -- Approved by The VETCEE Board -- March 2016 Competences for
Proceeding of the SEVC Southern European Veterinary Conference
 Close this window to return to IVIS www.ivis.org Proceeding of the SEVC Southern European Veterinary Conference Oct. 2-4, 2009, Barcelona, Spain http://www.sevc.info Next conference : October 1-3, 2010
Close this window to return to IVIS www.ivis.org Proceeding of the SEVC Southern European Veterinary Conference Oct. 2-4, 2009, Barcelona, Spain http://www.sevc.info Next conference : October 1-3, 2010
Institute of Surgical Research
 Institute of Surgical Research Surgical techniques A5 Practical Module. A1. MODUL - Asepsis and the surgeon A2. MODUL Surgical instrumentation A3. MODUL Operations A4. MODUL Bleedings A5. MODUL sterile
Institute of Surgical Research Surgical techniques A5 Practical Module. A1. MODUL - Asepsis and the surgeon A2. MODUL Surgical instrumentation A3. MODUL Operations A4. MODUL Bleedings A5. MODUL sterile
Prevention of Perioperative Surgical Infections
 Prevention of Perioperative Surgical Infections Michael A. West, MD, PhD, FACS Department of Surgery University California San Francisco San Francisco, CA, USA Surgical Site Infections (SSI) 2-5% of operated
Prevention of Perioperative Surgical Infections Michael A. West, MD, PhD, FACS Department of Surgery University California San Francisco San Francisco, CA, USA Surgical Site Infections (SSI) 2-5% of operated
Proceeding of the SEVC Southern European Veterinary Conference
 www.ivis.org Proceeding of the SEVC Southern European Veterinary Conference Oct. 17-19, 2008 Barcelona, Spain http://www.sevc.info Reprinted in the IVIS website with the permission of the SEVC www.ivis.org
www.ivis.org Proceeding of the SEVC Southern European Veterinary Conference Oct. 17-19, 2008 Barcelona, Spain http://www.sevc.info Reprinted in the IVIS website with the permission of the SEVC www.ivis.org
The sandwich technique for repair of pectus carinatum and excavatum/carinatum complex
 Featured rticle The sandwich technique for repair of pectus carinatum and excavatum/carinatum complex Hyung Joo Park, Kyung Soo Kim Department of Thoracic and Cardiovascular Surgery, Seoul St. Mary s Hospital,
Featured rticle The sandwich technique for repair of pectus carinatum and excavatum/carinatum complex Hyung Joo Park, Kyung Soo Kim Department of Thoracic and Cardiovascular Surgery, Seoul St. Mary s Hospital,
STANDARD OPERATING PROCEDURE #110 MOUSE ANESTHESIA
 STANDARD OPERATING PROCEDURE #110 MOUSE ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing mice. 2. RESPONSIBILITY Principal Investigators (PIs) and their
STANDARD OPERATING PROCEDURE #110 MOUSE ANESTHESIA 1. PURPOSE This Standard Operating Procedure (SOP) describes methods for anesthetizing mice. 2. RESPONSIBILITY Principal Investigators (PIs) and their
